- Research Article
- Abstract
- Introduction
- Patients and Methods
- Clinical Examination
- Radiology
- Osteotomy Failure
- Surgical Technique
- Follow-up
- Statistical Analysis
- Results
- KOOS
- Knee stability
- Arthroscopic cartilage evaluation
- Radiological Evaluation
- Body Mass Index
- Range of motion
- Complications
- Survival
- Discussion
- Conclusion
- Funding statement
- Acknowledgement
- References
Similar Functional Results after HTO for Knees with Medial Osteoarthritis with Ruptured or Intact ACL - A prospective study with 10-year follow-up
Arne Ekeland1*, Tor Kjetil Nerhus1, Sigbjorn Dimmen2, Elisabeth Thornes1, and Stig Heir1
1Martina Hansens Hospital, Box 13, N-1342 Gjettum, Norway
2Lovisenberg Diaconal Hospital, Lovisenberggata 17, N-0456 Oslo, Norway
Submission: January 18, 2022; Published: February 07, 2022
*Corresponding author: Arne Ekeland, MD PhD, Martina Hansens Hospital, Box 13, N-1342 Gjettum, Norway
How to cite this article: Arne E, Tor Kjetil N, Sigbjorn D, Elisabeth T, Stig H. Similar Functional Results after HTO for Knees with Medial Osteoarthritis with Ruptured or Intact ACL - A prospective study with 10-year follow-up. Ortho & Rheum Open Access J. 2022; 19(5): 556022. DOI: 10.19080/OROAJ.2022.19.556022
- Research Article
- Abstract
- Introduction
- Patients and Methods
- Clinical Examination
- Radiology
- Osteotomy Failure
- Surgical Technique
- Follow-up
- Statistical Analysis
- Results
- KOOS
- Knee stability
- Arthroscopic cartilage evaluation
- Radiological Evaluation
- Body Mass Index
- Range of motion
- Complications
- Survival
- Discussion
- Conclusion
- Funding statement
- Acknowledgement
- References
Abstract
Aim: To compare time-dependent functional improvement in patients with medial knee osteoarthritis (OA) with ruptured or intact anterior cruciate ligament (ACL) after treatment with high tibial osteotomy (HTO).
Patients and Methods: Forty-nine consecutive patients with medial knee OA were treated with opening wedge HTO stabilized with a Puddu plate and bone grafting. Seventeen patients had suffered anterior cruciate ligament (ACL) rupture mean 17.6 (1-38) years before the osteotomy. The mean age of these was 46 years (31-59 years), compared to 48 years (34-64 years) for the 32 patients (35 knees) with intact ACL. The patients were evaluated by the Knee Injury and Osteoarthritis Outcome Score (KOOS) preoperatively and at 6 months, 1, 2, 5 and 10 years postoperatively. The knee OA was graded radiologically.
Results: The angular correction, the preoperative KOOS and the OA gradings were similar in both groups. KOOS increased far beyond 10 points and clinically relevant compared to preoperative values during the two first postoperative years (P<0.001). This improvement was later sustained with similar KOOS in both groups during the 10-year period, except for higher KOOS subgroup Quality of Life (QoL) score for knees with intact ACL at the 5-year follow-up (P=0.014). The knee stability of the patients with ruptured ACL increased significantly after the HTO (P<0.001), and only two of them required a later ACL reconstruction. The 10-year survival was 84% for the 52 HTOs.
Conclusion: Patients with medial knee OA with ruptured or intact ACL improved with similar KOOS after HTO, but with higher QoL value for patients with intact ACL at the 5-year follow-up. The good functional result was sustained for 10 years for surviving osteotomies. The knee stability increased in patients with chronic ACL rupture, and most of these patients do not seem to require ACL reconstruction after the HTO.
Keywords: Varus knee; Opening wedge osteotomy; Bone transplantation; Knee stability; KOOS
- Research Article
- Abstract
- Introduction
- Patients and Methods
- Clinical Examination
- Radiology
- Osteotomy Failure
- Surgical Technique
- Follow-up
- Statistical Analysis
- Results
- KOOS
- Knee stability
- Arthroscopic cartilage evaluation
- Radiological Evaluation
- Body Mass Index
- Range of motion
- Complications
- Survival
- Discussion
- Conclusion
- Funding statement
- Acknowledgement
- References
Introduction
Rupture of the anterior cruciate ligament (ACL) increases the risk of knee osteoarthritis (OA) [1] and total knee arthroplasty (TKA) [2]. This may be related to increased instability with meniscal [3] and chondral lesions [4]. The increased risk of OA after ACL rupture is also present in ACL reconstructed knees, and this risk increases more than three times if the patients have additional meniscectomy [5]. The medial compartment of the knee carries on average 60-70% of the load during walking [6]. Medial meniscectomy aggravates varus alignment [7], resulting in increasing load and OA development [8,9]. Unloading the medial compartment by a corrective valgus high tibial osteotomy (HTO) will relieve the OA symptoms and destroyed hyaline cartilage may later be replaced by fibrocartilage [10]. HTO is also reported to improve knee stability [11,12]. As ACL rupture may induce or aggravate knee OA [13], the purpose of this study was to compare the time-dependent functional outcome of medial knee OA treated by opening wedge HTO for patients with chronic ACL rupture or intact ACL. The working hypothesis was that the functional outcome after HTO would be lower in patients with ruptured ACL than in those with intact ACL.
- Research Article
- Abstract
- Introduction
- Patients and Methods
- Clinical Examination
- Radiology
- Osteotomy Failure
- Surgical Technique
- Follow-up
- Statistical Analysis
- Results
- KOOS
- Knee stability
- Arthroscopic cartilage evaluation
- Radiological Evaluation
- Body Mass Index
- Range of motion
- Complications
- Survival
- Discussion
- Conclusion
- Funding statement
- Acknowledgement
- References
Patients and Methods
Forty-nine consecutive patients with medial knee OA were treated with opening wedge HTO in the period 2000-2008. Three patients had bilateral operations at different time points, including 52 knees in the study. Seventeen patients (17 knees) had additional ACL rupture and 32 patients (35 knees) had intact ACL. The demographic data of the two groups were similar (Table 1). The OA was mainly due to an open medial meniscal resection performed 20-30 years previously before the arthroscopic era, to several successive arthroscopic meniscal resections, and to the added effect of a ruptured ACL in 17 of the 52 knees. The ACL rupture occurred mean 17.6 (CI 13.1-22.1) (range 1-38) years before the osteotomy. Only three of the 17 ACL injured knees had been ACL reconstructed, but with later graft failure and increasing instability. Inclusion criteria were severe pain in an osteoarthritic knee with varus malalignment which had not responded to conservative treatment and where knee arthroplasty was not the first choice because of relatively young age. Exclusion criteria were patients with severe OA and pain needing a TKA.
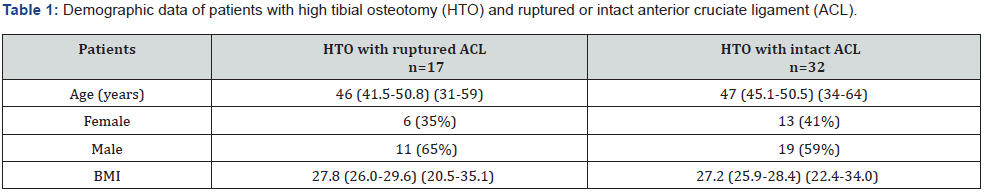
n = number of patients. BMI = Body mass index. Mean with CI 95% and range. No significant difference between HTO patients with ruptured or intact ACL for age (P=0.540), sex distribution (P=0.955) and BMI (P=0.536).
- Research Article
- Abstract
- Introduction
- Patients and Methods
- Clinical Examination
- Radiology
- Osteotomy Failure
- Surgical Technique
- Follow-up
- Statistical Analysis
- Results
- KOOS
- Knee stability
- Arthroscopic cartilage evaluation
- Radiological Evaluation
- Body Mass Index
- Range of motion
- Complications
- Survival
- Discussion
- Conclusion
- Funding statement
- Acknowledgement
- References
Clinical Examination
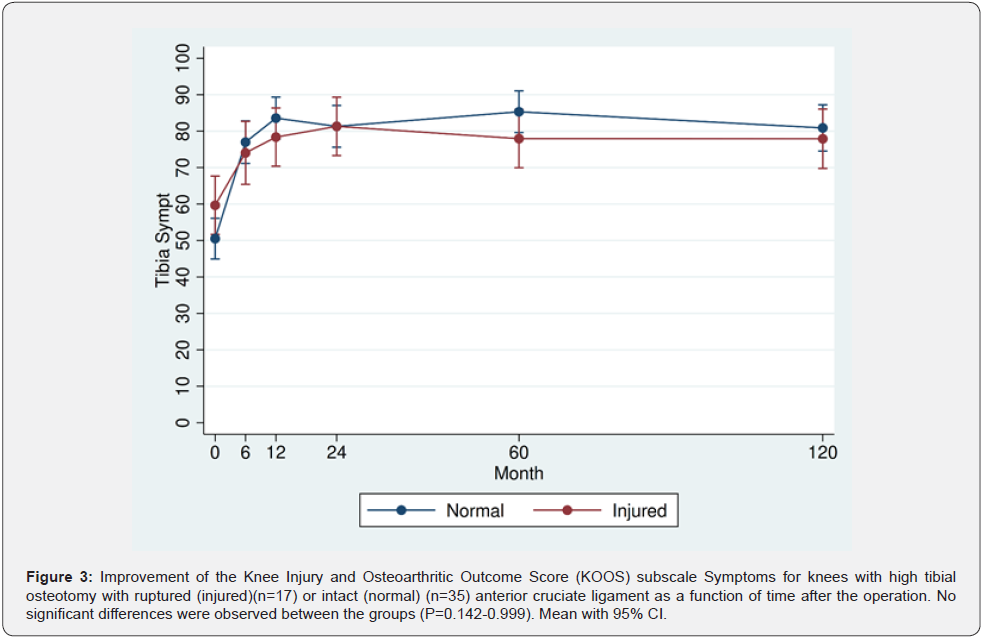
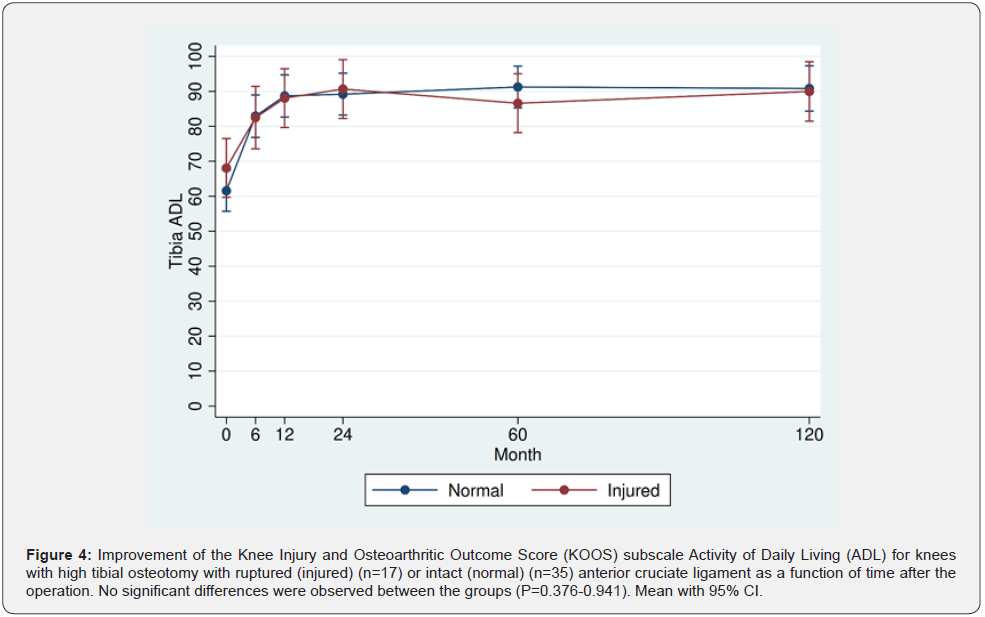
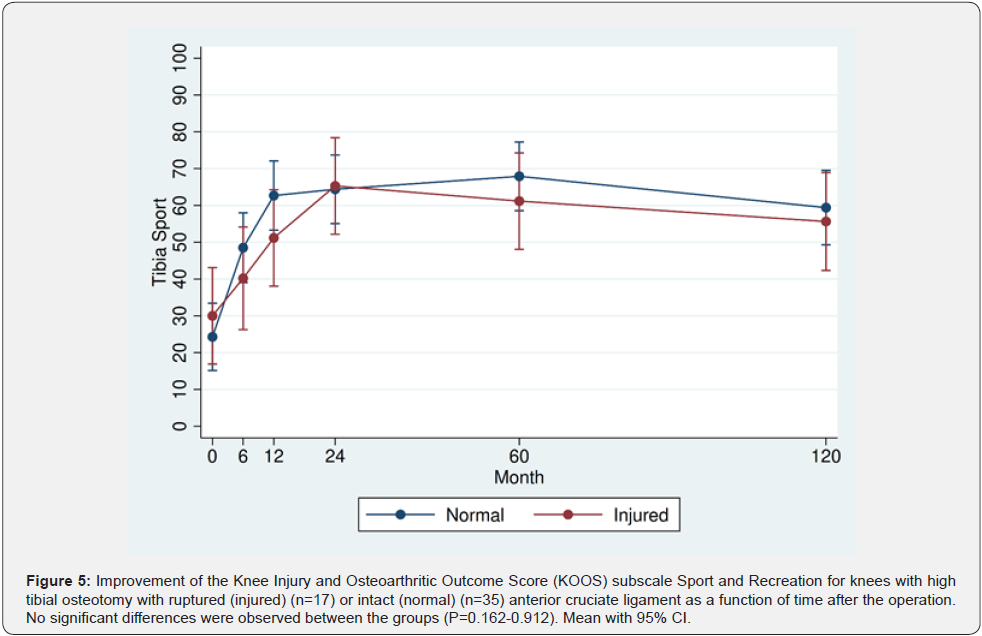
All patients were subjected to a preoperative arthroscopy 6 weeks to 4 months before the HTO where the degree of OA of the medial knee compartment was recorded according to the International Cartilage Repair (ICRS) classification [14]. Any meniscal flaps and loose joint cartilage were removed. It was also considered if the joint surfaces of the lateral compartment could tolerate the increased weight load following a correcting osteotomy. Small cartilage changes with an intact lateral meniscus were accepted. The clinical examination included knee range of motion (ROM) measured with a goniometer, the Lachman stability test, and body weight and height for calculation of body mass index (BMI). The patients also filled in a questionnaire for calculation of the Knee Injury and Osteoarthritic Outcome Score (KOOS) the day before the HTO [15]. KOOS has five subscales: Pain, other Symptoms, Activities of Daily Living (ADL), Sport and Recreational function, and knee related Quality of Life (QoL), and is well recognized to evaluate knee function [16]. A score from 0-100 is calculated for each subscale, with 100 representing the best result. A score improvement of 10 is supposed to have clinical relevance [17].
- Research Article
- Abstract
- Introduction
- Patients and Methods
- Clinical Examination
- Radiology
- Osteotomy Failure
- Surgical Technique
- Follow-up
- Statistical Analysis
- Results
- KOOS
- Knee stability
- Arthroscopic cartilage evaluation
- Radiological Evaluation
- Body Mass Index
- Range of motion
- Complications
- Survival
- Discussion
- Conclusion
- Funding statement
- Acknowledgement
- References
Radiology
Radiological evaluation was made on weight-bearing radiographs with straight knees and on lateral knee radiographs. The radiographs were scored according to the Ahlbäck classification criteria [18] and the Kellgren-Lawrence grading scale [19]. Also, the tibiofemoral anatomical axis was recorded. The angular correction was calculated on standing (full leg length) hip, knee and ankle (HKA) radiographs according to Dugdale [20], aiming for the mechanical axis to pass just lateral to the intercondylar eminence corresponding to 62% of the width of the tibial plateau, measured from the medial side.
- Research Article
- Abstract
- Introduction
- Patients and Methods
- Clinical Examination
- Radiology
- Osteotomy Failure
- Surgical Technique
- Follow-up
- Statistical Analysis
- Results
- KOOS
- Knee stability
- Arthroscopic cartilage evaluation
- Radiological Evaluation
- Body Mass Index
- Range of motion
- Complications
- Survival
- Discussion
- Conclusion
- Funding statement
- Acknowledgement
- References
Osteotomy Failure
Failure was defined as conversion of the osteotomy to total knee arthroplasty (TKA). Data from TKA converted patients were only included in the study until TKA surgery
- Research Article
- Abstract
- Introduction
- Patients and Methods
- Clinical Examination
- Radiology
- Osteotomy Failure
- Surgical Technique
- Follow-up
- Statistical Analysis
- Results
- KOOS
- Knee stability
- Arthroscopic cartilage evaluation
- Radiological Evaluation
- Body Mass Index
- Range of motion
- Complications
- Survival
- Discussion
- Conclusion
- Funding statement
- Acknowledgement
- References
Surgical Technique
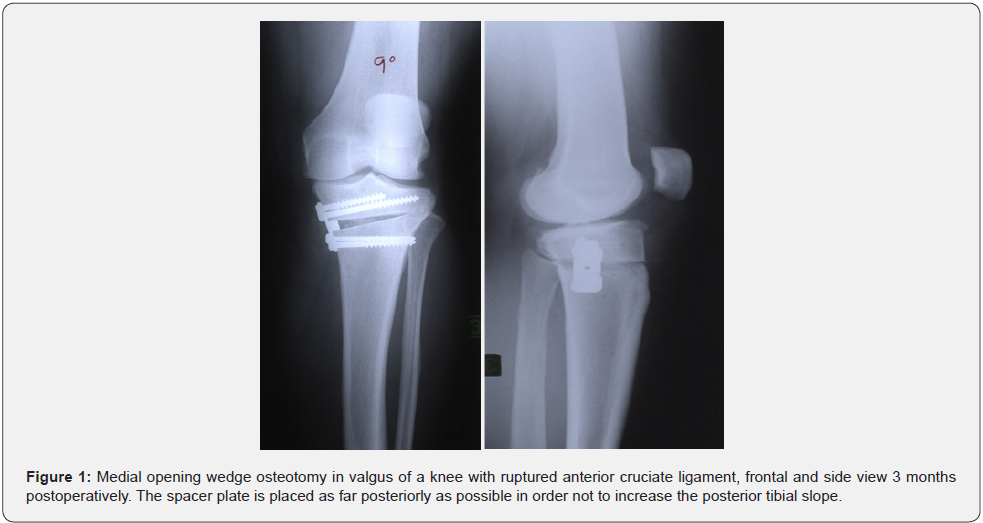
The patients were operated on a traction table with slight flexion of the knee to ease fluoroscopic guidance during the operation and secure rotational control of the leg. The osteotomy was performed as described by Puddu et al. [21]. The proximal part of the tibia was approached through a medial incision. The superficial medial collateral ligament was cut as part of an oblique osteotomy starting from the upper edge of pes anserinus and aiming for the fibular head. The height of the osteotomy cleft was calculated from the length of the osteotomy cut and the planned correcting angle, and the appropriate spacer plate chosen from a table provided by the plate manufacturer (Arthrex, Naples, FL, USA). Puddu plates of the first generation were used. The spacer plate was placed as far posteriorly as possible in order not to increase the tibial slope [9] (Figure 1). The osteotomy cleft was filled with bone from the iliac crest. All patients received antithrombotic prophylaxis with low molecular weight heparin (Fragmin®, Pfizer, New York. USA) for 10 days postoperatively. They were allowed partial weight-bearing (10 kg) postoperatively, and no braces were used. Increasing weight-bearing was allowed after 6 weeks and full weight-bearing a few weeks later depending on the radiological healing of the osteotomy. Healing was defined as ¾ of the osteotomy filled with new bone, and delayed healing as healing beyond 5 months postoperatively.
- Research Article
- Abstract
- Introduction
- Patients and Methods
- Clinical Examination
- Radiology
- Osteotomy Failure
- Surgical Technique
- Follow-up
- Statistical Analysis
- Results
- KOOS
- Knee stability
- Arthroscopic cartilage evaluation
- Radiological Evaluation
- Body Mass Index
- Range of motion
- Complications
- Survival
- Discussion
- Conclusion
- Funding statement
- Acknowledgement
- References
Follow-up
Standing weight-bearing radiographs of both knees were obtained at the 3-month, 5- and 10- year follow-ups, but only supine radiographs of the index knee at the 6-week follow-up. The patients filled in KOOS at the 6-month, 1-, 2-, 5- and 10-year follow-ups. Most of the follow-ups were performed by the first author, and no patients were lost to follow-up. The collection of data was approved by the Norwegian Social Science Data Services (project 22075), and the study was performed in accordance with the Helsinki Declaration with informed patient consent.
- Research Article
- Abstract
- Introduction
- Patients and Methods
- Clinical Examination
- Radiology
- Osteotomy Failure
- Surgical Technique
- Follow-up
- Statistical Analysis
- Results
- KOOS
- Knee stability
- Arthroscopic cartilage evaluation
- Radiological Evaluation
- Body Mass Index
- Range of motion
- Complications
- Survival
- Discussion
- Conclusion
- Funding statement
- Acknowledgement
- References
Statistical Analysis
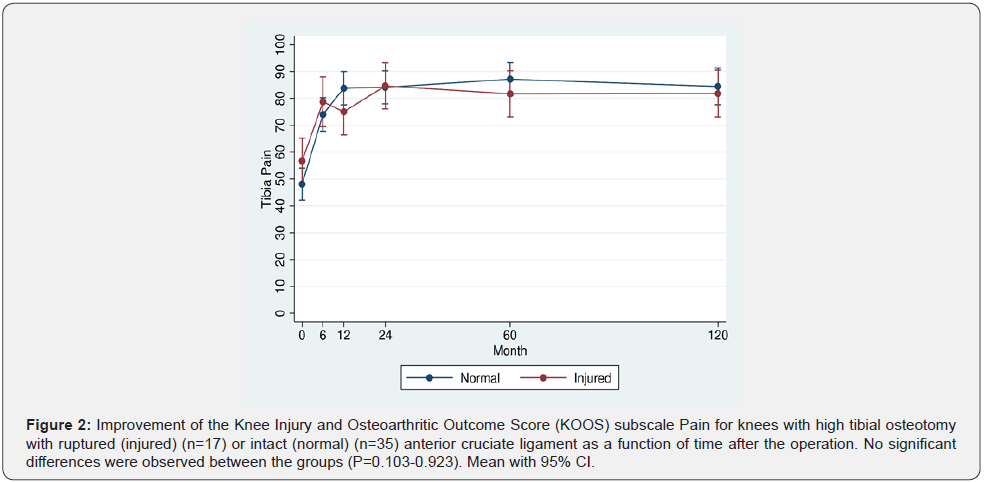
The results are presented as mean with CI 95% and range. Statistical differences were calculated by fitting separate linear mixed models for each of the KOOS subscores (Figures 2-6). Missing data were assumed to be missing at random. Treatment effects of patients with ACL rupture versus patients with intact ACL and the change from baseline to all other points in time were analyzed. The two-tailed T-test were used to calculate differences between the demographic data and for angular correction data (Tables 1 & 2). The Chi square test was used for categorical variables, and the two-tailed Fisher exact test when groups with small numbers were involved (Tables 3-6). The calculations were made with the SPSS software version 22 (IBM, Armonk, New York, USA) and Stata v16 (Stata 2015, College Station, Texas, USA). The level of statistical significance was set to p< 0.05.
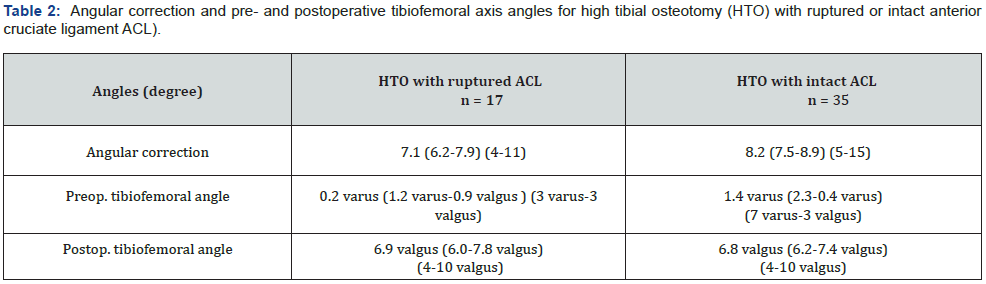
n = Number of osteotomies. Mean with CI 95% and range. No significant difference between HTO patients with ruptured or intact ACL for angular correction (P=0.051), preoperative tibiofemoral angle (P=0.087) and postoperative tibiofemoral angle (P=0.869).
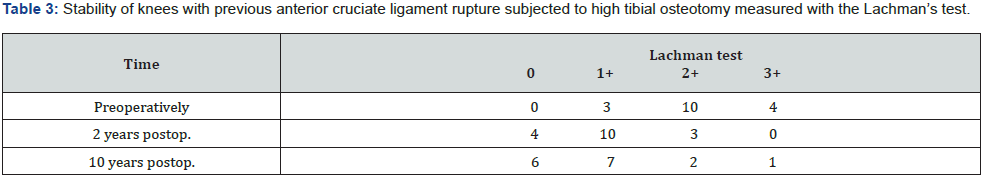
n = 17. Significant difference between preoperative and 2-year and 10-year postoperative knee stability (P<0.001).
No significant difference between the two groups (P = 0.344).
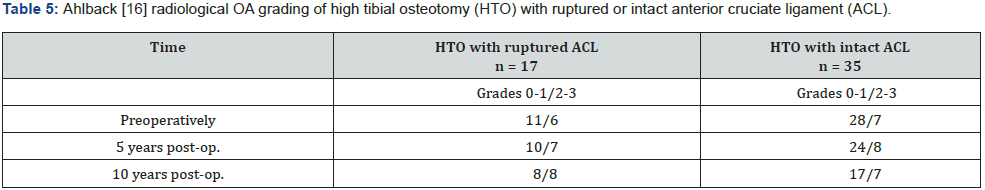
n = Number of osteotomies. No significant difference between the two groups (preoperatively P=0.309, 5-year postop. P=0.399, 10-year post op. P=0.317). Neither significant difference between the preoperative and 10-year postop. gradings (HTO with ruptured ACL P=0.616 or intact ACL P=0.616). Radiographs of three knees are missing at the 10-year follow-up in addition to those converted to TKA and the knee from the person who died in the follow-up period.
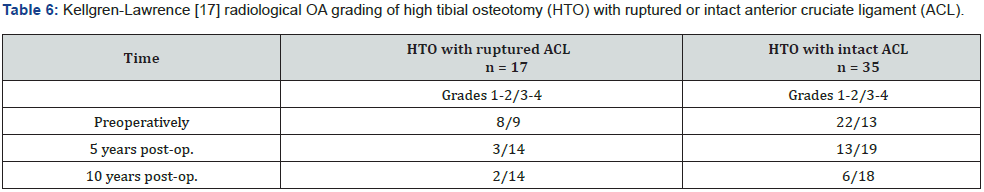
n = Number of osteotomies. No significant difference between the two groups (preoperatively P=0.434, 5-year postop. P=0.189, 10-year post op. P=0.439). The difference between the preoperative and 10-year postop. gradings was only significant for HTO with intact ACL (HTO with ruptured ACL P=0.057, intact ACL P=0.009), but this difference was even more significant when the two groups (HTO with ruptured or intact ACL) were combined (P<0.001). Radiographs of three knees are missing at the 10-year follow-up in addition to those converted to TKA and the knee from the person who died in the follow-up period.
- Research Article
- Abstract
- Introduction
- Patients and Methods
- Clinical Examination
- Radiology
- Osteotomy Failure
- Surgical Technique
- Follow-up
- Statistical Analysis
- Results
- KOOS
- Knee stability
- Arthroscopic cartilage evaluation
- Radiological Evaluation
- Body Mass Index
- Range of motion
- Complications
- Survival
- Discussion
- Conclusion
- Funding statement
- Acknowledgement
- References
Results
The mean angular correction measured from pre- and 3 months postoperative radiographs was 7.1° for knees with previous ACL rupture and 8.2° for those with intact ACL (Table 2). Also, the preoperative and 3 months postoperative tibiofemoral anatomical axis angles were similar for the two groups (Table 2). The angular correction was later sustained with mean tibiofemoral valgus angles of 6.3°/6.0° at the 5-year and 5.4°/5.5° at the 10- year follow-ups for HTOs with ruptured, respectively intact ACL. Fourteen of the 17 HTOs with ruptured ACL (82%) were healed at the 3-month and all at the 6-month follow-up. Of the 35 HTOs with intact ACL, 28 (80%) were healed at the 3-month and all but one with osteosynthetic failure at the 6-month follow-up. One patient in the group with intact ACL died in the follow-up period of causes unrelated to the knee surgery.
- Research Article
- Abstract
- Introduction
- Patients and Methods
- Clinical Examination
- Radiology
- Osteotomy Failure
- Surgical Technique
- Follow-up
- Statistical Analysis
- Results
- KOOS
- Knee stability
- Arthroscopic cartilage evaluation
- Radiological Evaluation
- Body Mass Index
- Range of motion
- Complications
- Survival
- Discussion
- Conclusion
- Funding statement
- Acknowledgement
- References
KOOS
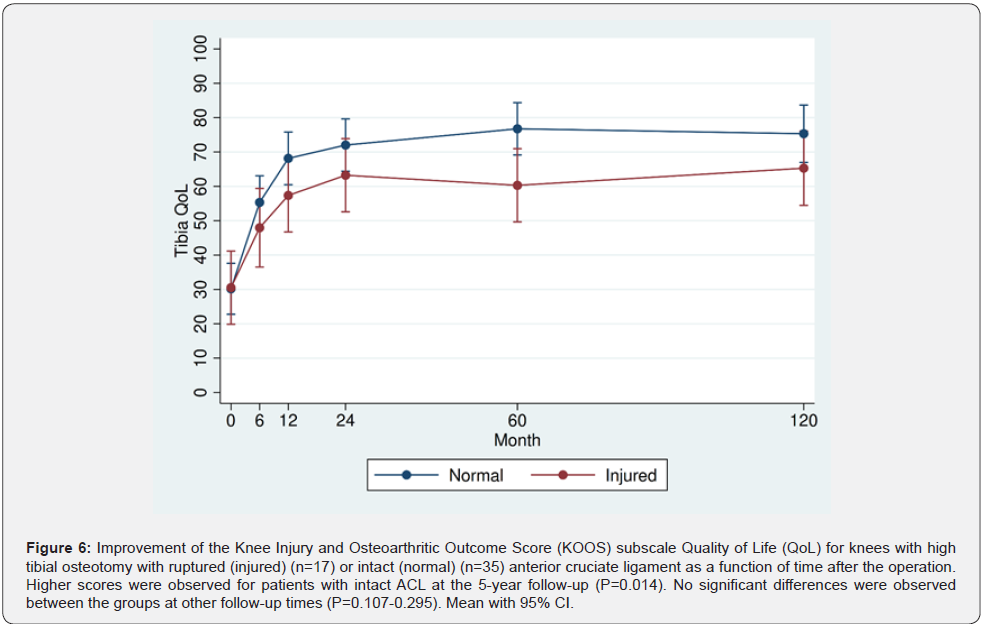
Similar KOOS values were recorded preoperatively for both osteotomy groups. During the two first postoperative years, KOOS improved far beyond 10 points and clinically relevant in both groups compared to the preoperative values (P<0.001). Thereafter the KOOS values plateaued, remaining on that level throughout the 10-year follow-up period for surviving osteotomies Similar KOOS values were recorded at all follow-up times for patients with ruptured or intact ACL, except for higher QoL scoring for patients with intact than those with ruptured ACL at the 5-year follow-up (P=0.014) (Figures 2-6).
- Research Article
- Abstract
- Introduction
- Patients and Methods
- Clinical Examination
- Radiology
- Osteotomy Failure
- Surgical Technique
- Follow-up
- Statistical Analysis
- Results
- KOOS
- Knee stability
- Arthroscopic cartilage evaluation
- Radiological Evaluation
- Body Mass Index
- Range of motion
- Complications
- Survival
- Discussion
- Conclusion
- Funding statement
- Acknowledgement
- References
Knee stability
Most of the patients with ruptured ACL had fewer knee instability symptoms after the osteotomy. The knee stability measured by the Lachman’s test was significantly increased (p<0.001) at the 2- and 10-year follow-ups compared to the preoperative recordings (Table 3). Only two of the 17 patients (12%) required an ACL reconstruction in the 10-year follow-up period. The first patient one year after the osteotomy due to a new knee injury and a previously failed ACL reconstruction, and the second 4 years after the osteotomy after a new knee injury. The knees with intact ACL were stable both pre- and post-osteotomy.
- Research Article
- Abstract
- Introduction
- Patients and Methods
- Clinical Examination
- Radiology
- Osteotomy Failure
- Surgical Technique
- Follow-up
- Statistical Analysis
- Results
- KOOS
- Knee stability
- Arthroscopic cartilage evaluation
- Radiological Evaluation
- Body Mass Index
- Range of motion
- Complications
- Survival
- Discussion
- Conclusion
- Funding statement
- Acknowledgement
- References
Arthroscopic cartilage evaluation
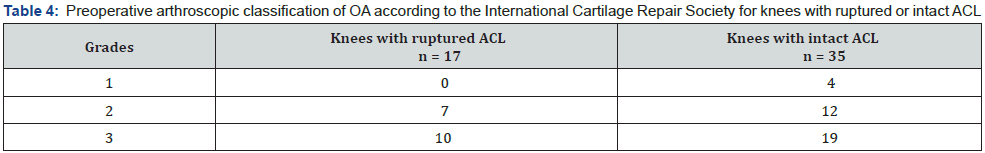
Many of the knees had pronounced OA in the medial compartment with degenerative meniscal ruptures and worn hyaline cartilage with loose flaps down to the subchondral bone plate. The ICRS evaluation of hyaline cartilage in the medial knee compartment was similar for knees with ruptured or intact ACL (Table 4).
- Research Article
- Abstract
- Introduction
- Patients and Methods
- Clinical Examination
- Radiology
- Osteotomy Failure
- Surgical Technique
- Follow-up
- Statistical Analysis
- Results
- KOOS
- Knee stability
- Arthroscopic cartilage evaluation
- Radiological Evaluation
- Body Mass Index
- Range of motion
- Complications
- Survival
- Discussion
- Conclusion
- Funding statement
- Acknowledgement
- References
Radiological Evaluation
The preoperative Ahlbäck scores were similar for knees with ruptured or intact ACL, and so were the scorings at the 5- and 10-year follow-ups (Table 3). Also, the Kellgren-Lawrence classification disclosed similar scorings for the two groups preoperatively and at the 5- and 10-year follow-ups, but a significant increase was observed between the preoperative and the 10-year postoperative scoring for knees with intact ACL. This difference was even more pronounced when the two groups (with ruptured or intact ACL) were combined (Table 4).
- Research Article
- Abstract
- Introduction
- Patients and Methods
- Clinical Examination
- Radiology
- Osteotomy Failure
- Surgical Technique
- Follow-up
- Statistical Analysis
- Results
- KOOS
- Knee stability
- Arthroscopic cartilage evaluation
- Radiological Evaluation
- Body Mass Index
- Range of motion
- Complications
- Survival
- Discussion
- Conclusion
- Funding statement
- Acknowledgement
- References
Body Mass Index
The mean preoperative BMI of the patients with ruptured or intact ACL was similar in both groups and about 27.5 (Table 1).
- Research Article
- Abstract
- Introduction
- Patients and Methods
- Clinical Examination
- Radiology
- Osteotomy Failure
- Surgical Technique
- Follow-up
- Statistical Analysis
- Results
- KOOS
- Knee stability
- Arthroscopic cartilage evaluation
- Radiological Evaluation
- Body Mass Index
- Range of motion
- Complications
- Survival
- Discussion
- Conclusion
- Funding statement
- Acknowledgement
- References
Range of motion
The preoperative ROM was similar in both groups and about 130°. After a small drop at the 3-month follow-up, the ROM was regained at the 6-month follow-up and later remained at the preoperative level.
- Research Article
- Abstract
- Introduction
- Patients and Methods
- Clinical Examination
- Radiology
- Osteotomy Failure
- Surgical Technique
- Follow-up
- Statistical Analysis
- Results
- KOOS
- Knee stability
- Arthroscopic cartilage evaluation
- Radiological Evaluation
- Body Mass Index
- Range of motion
- Complications
- Survival
- Discussion
- Conclusion
- Funding statement
- Acknowledgement
- References
Complications
The postoperative complications were similarly distributed among the two HTO groups (Table 7). The only osteosynthetic failure occurred in a patient with a body weight of 130 kg. He was reoperated with a Tomofix® plate (Synthes, Stratec Medical, Oberdorf, Switzerland) with autologous bone grafting. The osteotomy healed, but the OA deteriorated and the HTO was later converted to TKA.

- Research Article
- Abstract
- Introduction
- Patients and Methods
- Clinical Examination
- Radiology
- Osteotomy Failure
- Surgical Technique
- Follow-up
- Statistical Analysis
- Results
- KOOS
- Knee stability
- Arthroscopic cartilage evaluation
- Radiological Evaluation
- Body Mass Index
- Range of motion
- Complications
- Survival
- Discussion
- Conclusion
- Funding statement
- Acknowledgement
- References
Survival
One of the 17 knees (6%) with ruptured ACL was converted to TKA 9.5 years postoperatively compared to 7 of 35 knees (21%) with intact ACL after mean 6.3 (CI 3.1-9.5, range 2.0- 9.8 years) (P=0.242), giving a 10-year survival of 84% for the HTOs. The angular correction was similar for the patients who ended up with TKA and those where the osteotomy survived.
- Research Article
- Abstract
- Introduction
- Patients and Methods
- Clinical Examination
- Radiology
- Osteotomy Failure
- Surgical Technique
- Follow-up
- Statistical Analysis
- Results
- KOOS
- Knee stability
- Arthroscopic cartilage evaluation
- Radiological Evaluation
- Body Mass Index
- Range of motion
- Complications
- Survival
- Discussion
- Conclusion
- Funding statement
- Acknowledgement
- References
Discussion
This study revealed that opening wedge HTO for medial knee OA resulted in good and similar functional results both for patients with ruptured and intact ACL. The age of the patients, the preoperative KOOS, the degree of preoperative OA, the BMI, the preoperative varus alignment and the angular correction were similar in both groups. The knee function evaluated by the five subgroups of KOOS was similar for the two groups in 24 out of 25 recordings, but with higher subgroup QoL scoring for patients with intact ACL at the 5-year follow-up (Figure 6). The working hypothesis was therefore only partly rejected.
The sagittal knee instability evaluated by the Lachman’s test improved significantly after HTO in patients with chronic ACL rupture. This agrees with the findings of Mehl et al. [22] who reported the same improvement of instability in patients with ACL deficiency subjected to HTO alone or combined single-stage HTO and ACL reconstruction. At mean 5.8 years postoperatively no group differences were found in the KT-2000 examinations or Kellgren-Lawrence radiographic gradings. A systematic review has reported significant improvement of functional subjective outcome after simultaneous HTO and ACL reconstruction (ACLR), but due to the lack of comparative studies, it remains unclear if HTO with ACLR is superior to ACLR or HTO alone according to the authors [23]. The reason for the improvement in knee stability in ACL deficient knees after HTO is unclear. It may be related to better and more training of the stabilizing knee muscles after the post osteotomy pain relief when the medial knee compartment is unloaded, and later to a more fibrotic knee capsule by advancing osteoarthritis.
An increase in the posterior tibial slope will increase ACL tension and may lead to increased anterior tibial translation [9,24]. Opening wedge osteotomies may unintentionally lead to an increase of the posterior tibial slope depending on the location and the design of the osteotomy plate [9,25-27]. The spacer plates in this study were therefore placed far posteriorly in the osteotomy cleft (Figure 1). The preoperative arthroscopy displayed that most of the knees both in patients with ruptured and intact ACL had cartilage damage down to the subchondral bone plate. The HTO was performed to prevent or delay TKA in this middle-aged group of patients [28]. For the patients with additional ACL rupture and instability we were prepared to do a later ACL reconstruction, as some authors recommend doing these two operations during the same surgery [29,30]. But most of the patients with additional ACL rupture recovered so much after the correcting osteotomy (Figures 2-6), that a secondary stabilizing operation was only required in 2 of 17 patients (12%).
Both Ahlback [18] and Kellgren-Lawrence [19] radiological grading systems for OA were used in this study. In the Ahlback system, great importance is attached to obliteration of the joint space and any bone loss, whereas the Kellgren-Lawrence system also consider the presence of osteophytes in addition to narrowing of the joint space. Different descriptions of the Kellgren-Lawrence criteria for knee OA have been published, but we used the original description [31]. The degree of OA was similar in both groups of patients throughout the study, but with a significant increase of the Kellgren-Lawrence scoring at the 10-year follow-up compared to the preoperative scoring (Table 6). This may suggest that the Kellgren-Lawrence grading scale is more sensitive to OA changes over time than the Ahlbäck classification criteria. Kellgren-Lawrence is also the grading system recommended by the International Society of Arthroscopy and Orthopaedic Knee Surgery (ISAKOS).
The 10-year survival of the HTOs in this study was 84%. This agrees with the osteotomy survival reported by Jin et al. [32], but higher than reported by Keenan et al. [33]. The BMI was similar and about 26-28 both for patients with ruptured and intact ACL. Overweight is a risk factor for later conversion of HTO to TKA [34,35], but the number of patients with BMI>30 in this study was small.
All osteotomies healed in this study including the HTO with osteosynthetic failure, where the osteotomy healed after a reoperation. This is probably due to grafting of autologous bone from crista into the osteotomy cleft [36]. Nelissen et al. [37] used Vitoss superficial bone substitute in osteotomies stabilized with the Puddu plate and recorded pseudarthrosis in 11 of 49 patients (22%) and several other complications, claiming the spacer plate provided inadequate stability. The strength of this study is the prospective design with repetitive KOOS recordings enabling functional evaluation of the patients over time, that no patients were lost, and the long follow-up time. The limitations are that the tibial slope angle has not been measured as only short sagittal radiographs of the proximal tibia were available, that the anterior tibial translation was only evaluated by the Lachman test, and not by the instrumental KT-2000 test which is more accurate. Another weakness is the missing of postoperative HKA radiographs since the study started before such radiographs were available at our hospital. The preoperative HKA radiographs of the first included patients were therefore taken at another hospital, making it inconvenient for the patients to visit two hospitals for postoperative follow-ups. A later HTO study with pre- and postoperative HKA radiographs at our hospital disclosed an under correction of about 3° related to the planned correction with Dugdale’s method [20], using the same opening wedge technique for HTO as in the present study [38].
- Research Article
- Abstract
- Introduction
- Patients and Methods
- Clinical Examination
- Radiology
- Osteotomy Failure
- Surgical Technique
- Follow-up
- Statistical Analysis
- Results
- KOOS
- Knee stability
- Arthroscopic cartilage evaluation
- Radiological Evaluation
- Body Mass Index
- Range of motion
- Complications
- Survival
- Discussion
- Conclusion
- Funding statement
- Acknowledgement
- References
Conclusion
The functional results after opening wedge HTO for knees with ruptured or intact ACL were good and similar for 10 years followups, except for a higher KOOS QoL score for patients with intact ACL at the 5-year follow-up. HTO increased the knee stability in ACL deficient knees, and most of these patients do not seem to need an ACL reconstruction in addition to the HTO.
- Research Article
- Abstract
- Introduction
- Patients and Methods
- Clinical Examination
- Radiology
- Osteotomy Failure
- Surgical Technique
- Follow-up
- Statistical Analysis
- Results
- KOOS
- Knee stability
- Arthroscopic cartilage evaluation
- Radiological Evaluation
- Body Mass Index
- Range of motion
- Complications
- Survival
- Discussion
- Conclusion
- Funding statement
- Acknowledgement
- References
Funding statement
No benefits in any form have been received or will be received from a commercial party related directly or indirectly to the subject of this article.
- Research Article
- Abstract
- Introduction
- Patients and Methods
- Clinical Examination
- Radiology
- Osteotomy Failure
- Surgical Technique
- Follow-up
- Statistical Analysis
- Results
- KOOS
- Knee stability
- Arthroscopic cartilage evaluation
- Radiological Evaluation
- Body Mass Index
- Range of motion
- Complications
- Survival
- Discussion
- Conclusion
- Funding statement
- Acknowledgement
- References
Acknowledgement
The authors thank Jonas Ranstam BSc PhD, Lund University, Sweden for valuable statistical help.
- Research Article
- Abstract
- Introduction
- Patients and Methods
- Clinical Examination
- Radiology
- Osteotomy Failure
- Surgical Technique
- Follow-up
- Statistical Analysis
- Results
- KOOS
- Knee stability
- Arthroscopic cartilage evaluation
- Radiological Evaluation
- Body Mass Index
- Range of motion
- Complications
- Survival
- Discussion
- Conclusion
- Funding statement
- Acknowledgement
- References
References
- Gillquist J, Messner K (1999) Anterior cruciate ligament reconstruction and the long-term incidence of gonarthrosis. Sports Med 27(3): 143–156.
- Khan T, Alvand A, Prieto-Alhambra D, David J Culliford, Andrew Judge, et al. (2019) ACL and meniscal injuries increase the risk of primary total knee replacement for osteoarthritis: A matched case-control study using the critical practice research datalink (CPRD). Br J Sports Med 53(15): 965-968.
- Levy AS, Meier SW (2003) Approach to cartilage injury in the anterior cruciate ligament-deficient knee. Orthop Clin North Am 34(1): 149–167.
- Drogset JO, Grontvedt T (2002) Anterior cruciate ligament reconstruction with and without a ligament augmentation device: results at 8-year follow-up. Am J Sports Med 30(6): 851–856.
- Claes S, Hermie L, Verdonk R, Bellemans J, Verdonk P (2013) Is osteoarthritis an inevitable consequence of anterior cruciate ligament reconstruction? A meta-analysis. Knee Surg Sports Traumatol Arthrosc 21(9): 1967–1976.
- Becker R, Kopf S, Karlsson J (2013) Loading conditions of the knee: what does it mean? Knee Surg Sports Traumatol Arthrosc 21: 2659–2660.
- Yoon KH, Lee SH, Bae DK, Park SY, Oh H (2013) Does varus alignment increase after medial meniscectomy? Knee Surg Sports Traumatol Arthrosc 21(9): 2131–2136.
- Teichtahl AJ, Davies-Tuck ML, Wluka AE, Jones G, Cicuttini FM (2009) Change in knee angle influences the rate of medial tibial cartilage volume loss in knee osteoarthritis. Osteoarthr Cartil 17(1): 8–11.
- Amis AA (2013) Biomechanics of high tibial osteotomy. Knee Surg Sports Traumatol Arthrosc 21(1): 197–205.
- Jung WH, Takeuchi R, Chun CW, Lee JS, Ha JM, et al. (2014) Second look arthroscopic assessment of cartilage regeneration after medial opening-wedge high tibial osteotomy. Arthroscopy 30(1): 72-79.
- Naudie DD, Amendola A, Fowler PJ (2004) Opening wedge high tibial osteotomy for symptomatic hyperextension-varus thrust. Am J sports Med 32(1): 60-70.
- Dean CS, Liechti DJ, Chahla, J, Moatsche G. LaPrade, et al. (2016) Clinical outcomes of high tibial osteotomy for knee instability. Orthop J Sports Med 4(3): 2325967116633419.
- Oiestad BE, Engebretsen L, Storheim K, Risberg MA (2009) Knee osteoarthritis after anterior cruciate ligament injury: A systematic review. Am J Sports Med 37(7): 1434-1437.
- Brittberg M, Winalski CS (2003) Evaluation of cartilage injuries and repair. J Bone Joint Surg Am 85(Suppl. 2): 58–69.
- Roos EM, Roos HP, Lohmander LS, Ekdahl C, Beynnon BD (1998) Knee Injury and Osteoarthritis Outcome Score (KOOS)--development of a self-administered outcome measure. J Orthop Sports Phys Ther 28(2): 88–96.
- Tanner SM, Dainty KN, Marx RG, Kirkley A (2007) Knee-specific quality-of-life instruments: which one measure symptoms and disabilities most important to patients? Am J Sports Med 35(9): 1450–1458.
- Roos EM, Lomander LS (2003) Knee injury and Osteoarthritis Outcome Score (KOOS): from joint injury to osteoarthritis. Health Qual Life Outcomes 1: 64.
- Ahlback S (1968) Osteoarthrosis of the knee. A radiographic investigation. Acta Radiol Diagn 7(Suppl 277): 7–72.
- Kellgren JH, Lawrence JS (1957) Radiological assessment of osteo-arthrosis. Ann Rheum Dis 16(4): 494–502.
- Dugdale TW, Noyes FR, Styer D (1992) Preoperative planning for high tibial osteotomy. The effect of lateral tibiofemoral separation and tibiofemoral length. Clin Orthop 274: 248–264.
- Puddu G, Franco V, Cipolla M, Cerullo G, Gianni E (2002) Opening wedge osteotomy: proximal tibia and distal femur. In: Jackson RW, ed. Reconstructive knee surgery. Lippincott, Williams and Wilkins, Philadelphia, USA, pp. 375-390.
- Mehl J, Paul J, Feucht MJ, Bode G, Imhoff AB, et al. (2017) ACL deficiency and varus osteoarthritis: high tibial osteotomy alone or combined with ACL reconstruction? Arch Orthop Trauma Surg 137(2): 233-240.
- Stride D, Wang, J, Horner NS, Alolabi B, Khanna, V, et al. (2019) Indications and outcomes of simultaneous high tibial osteotomy and ACL reconstruction. Knee Surg Sports Traumatol Arthrosc 27(4): 1320-1331.
- Shelburne KB, Kim HJ, Sterett WI, Pandy MG (2011) Effect of posterior tibial slope on knee biomechanics during functional activity. J Orthop Res 29(2): 223-231.
- Marti CB, Gautier E, Wachtl SW, Jakob RP (2004) Accuracy of frontal and sagittal plane correction in open-wedge high tibial osteotomy. Arthroscopy 20(4): 366–372.
- El-Azab H, Glabgly P, Paul J, Imhoff AB, Hinterwimmer S (2010) Patellar height and posterior tibial slope after open- and closed-wedge high tibial osteotomy: a radiological study on 100 patients. Am J Sports Med 38(2): 323–329.
- Laprade RF, Spiridonov SI, Nystrom LM, Jansson KS (2012) Prospective outcomes of young and middle-aged adults with medial compartment osteoarthritis treated with a proximal tibial opening wedge osteotomy. Arthroscopy 28(3): 354–364.
- Ekeland A, Nerhus TK (2020) Editorial commentary: High tibial osteotomy for varus knees with medial osteoarthritis may prevent total knee arthroplasty. Arthroscopy 36(2): 544-545.
- Zaffagnini S, Bonanzinga T, Grassi A, Marcheggiani Muccioli GM, Musiani, C, et al. (2013) Combined ACL reconstruction and closing-wedge HTO for varus angulated ACL-deficient knees. Knee Surg Sports Traumatol Arthrosc 21(4): 934-941.
- McNamara I, Birmingham TB, Fowler PJ, Giffin JR (2013) High tibial osteotomy: evolution of research and clinical applications--a Canadian experience. Knee Surg Sports Traumatol Arthrosc 21(1): 23–31.
- Schiphof D, Boers M, Bierma-Zeinstra SM (2008) Differences in descriptions of Kellgren and Lawrence grades of knee osteoarthritis. Ann Rheum Dis 67(7): 1034–1036.
- Jin C, Song E-K, Santoso A, Ingale PS, Choi I-S, et al. (2020) Survival and risk factor analysis of medial open wedge high tibial osteotomy for unicompartment knee osteoarthritis. Arthroscopy 36(2): 535-543.
- Keenan OJF, Clement ND, Nutton R, Keating JF (2019) Older age and female gender are independent predictors of early conversion to total knee arthroplasty after high tibial osteotomy. Knee 26(1): 207–212.
- Brinkman J-M, Lobenhoffer P, Agneskirchner JD, Staubli AE, Wymenga AB, et al. (2008) Osteotomies around the knee: patient selection, stability of fixation and bone healing in high tibial osteotomies. J Bone Joint Surg Br 90(12): 1548–1557.
- Hui C, Salmon LJ, Kok A, Heidi A Williams, Niels Hockers, et al. (2011) Long-term survival of high tibial osteotomy for medial compartment osteoarthritis of the knee. Am J Sports Med 39(1): 64–70.
- Jung W-H, Takeuchi R, Kim D-H, Nag R (2020) Faster union rate and better clinical outcomes using autologous bone graft after medial opening wedge high tibial osteotomy. Knee Surg Sports Traumatol Arthrosc 28(5): 1380-1387.
- Nelissen EM, van Langelaan EJ, Nelissen RG (2010) Stability of medial opening wedge high tibial osteotomy: a failure analysis. Int Orthop 34(2): 217–223.
- Nerhus TK, Ekeland A, Solberg G, Einar Andreas Sivertsen, Jan Erik Madsen, et al. (2017) Radiological outcomes in a randomized trial comparing opening wedge and closing wedge technique of high tibial osteotomy. Knee Surg sports Traumatol Arthrosc 25(3): 910-917.






























