Comparative Study of PRP Versus NSAIDS Single Injection for Management of Long Head of Biceps Tendinitis: Clinical & Laboratory
Ashraf Elazab1* and Ahmed Sonbol2
1Knee & Shoulder and sport Traumatology center, Mansoura, Egypt
2Pain management unit, Mansoura university hospitals, Faculty of medicine, Mansoura, Egypt
Submission: November 25, 2021; Published: December 08, 2021
*Corresponding author: Ashraf Elazab, Knee & Shoulder and Sport Traumatology Center, Dr. Ashraf Elazab, Al mahata square, Mansoura, Egypt
How to cite this article: Ashraf E, Ahmed S. Comparative Study of PRP Versus NSAIDS Single Injection for Management of Long Head of Biceps 002 Tendinitis: Clinical & Laboratory. Ortho & Rheum Open Access J. 2021; 19(3): 556015. DOI: 10.19080/OROAJ.2021.19.556015
Abstract
Background: Both platelet rich plasma (PRP) and non-steroidal anti-inflammatory drugs (NSAIDs) have proven their efficacy in the management of soft tissue inflammatory disorders. This study was conducted aiming to compare between PRP and NSIAD injections in the management of long head of biceps tendinitis (LHBT).
Patients and methods: We included a total of 88 cases, who were divided into two equal groups; PRP group (44 cases), and NSAIDs group (44 cases). All cases were subjected to history taking, examination, and routine investigations (including IL-6). Ultrasound guided injection of PRP and meloxicam 15 mg inside the biceps sheath was performed in both groups respectively
Results: No significant difference was detected regarding demographic or clinical parameters. Il-6 showed early increase in the PRP group, and then it decreased to significantly lower levels compared to the NSAIDs group after 2 weeks. Likewise, VAS score showed mild increase during the initial 3 days in the PRP group, but it improved significantly in the subsequent visits. Although Oxford score improved in both groups, the improvement was significantly better in the PRP group on the later follow up assessment.
Conclusion: Ultrasound guided injection of PRP and NSAIDs is effective in managing LHBT symptoms. However, a more significant improvement is achieved with PRP.
Introduction
Bicep’s tendinitis is an inflammatory disorder of the tendon around the long head of biceps muscle. Primary tendinitis, which means inflammation of the tendon within the bicipital groove, accounts for 5% of these cases [1]. Most cases usually have a concomitant lesion [2]. Such cases are typically complaining of deep throbbing pain located at the anterior shoulder (mainly at the site of bicipital groove) and radiating to deltoid muscle insertion or down to the hand with radial distribution. Pain usually becomes worse at night, especially if the subject slept over the affected shoulder [3,4]. The management of this disorder include conservative methods (rehabilitation, stretch therapy, and rest), medications (oral NSIADs, paracetamol), local injections (steroids), and surgery if all the previous measures have failed [5,6].
Multiple studies have reported the efficacy of local steroid injection in painful musculoskeletal conditions [7,8]. However,there is still an increased risk for tendon atrophy, rupture, or decreases bone strength [9]. Moreover, changes in blood glucose could be problematic in diabetic persons [10]. Due to these side effects, it was recommended to seek an effective alternative to steroids in managing these conditions [11]. Non-steroidal anti-inflammatory drugs are commonly prescribed for pain resulting from soft tissue injury or tendinopathy [12]. Although it has multiple side effects (e.g., peptic ulceration and bleeding), this risk of adverse events is decreased significantly when these medications are injected locally. Even if systemic these rare effects are encountered, it will be less severe compared to steroid effects [11]. Furthermore, local NSAIDs injection is not associated with significant cartilaginous of soft tissue changes [13,14].
Multiple reports have stated that Platelet rich plasma (PRP) has an accelerating role in response to injury. Cellular response to injurious agent is composed of four stages; hemostasis, inflammation, proliferation, as well as remodeling [15,16].
Mos and his associates reported that in vivo application of PRP in tendon injuries resulted in angiogenesis and fibrovascular callus formation, which in turn may have a beneficial effect on the catabolic demarcation of injured tendon matrix [17]. This study was conducted at Mansoura University Hospitals and Knee &Shoulder orthopedic center in Mansoura, Egypt aiming to compare between PRP and NSIAD injections in the management of biceps tendinitis.
Patients and Methods
This is a prospective randomized study that was conducted at pain clinics, Mansoura University Hospitals and Knee &Shoulder orthopedic center in Mansoura, Egypt during the period between January 2019 and January 2020. This study was designed for cases diagnosed with LHBT who are prepared for local injections. We included a total of 88 cases who were divided into two equal groups; the first group (PRP group) included 44 cases who underwent PRP injection, whereas the other group included the remaining 44 cases who underwent NSAIDs (meloxicam) injection.
Cases older than 18 years, who reported no improvement with physical therapy, oral pain killers, or local steroid injection were included in the study. On the other hand, cases with rheumatoid arthritis, uncontrolled systemic comorbidity, previous shoulder surgery, pregnancy, or steroid injection within the last 3 months were excluded. An informed written consent was obtained from all cases before participating in the study, after complete explanation of the benefits and drawbacks of each treatment method. In addition, the study was approved by the local ethical committee of Mansoura university. All cases were subjected to complete history taking, thorough shoulder examination, and routine radiological investigations. Moreover, visual analogue scale (VAS) [18], and Oxford Shoulder Score [19] were determined before intervention. Plain shoulder radiography was ordered for all cases to exclude the primary causes of impingement. Moreover, shoulder ultrasonography (US) and/or magnetic resonance imaging (MRI) were used to confirm the diagnosis.
Enzyme-linked immunosorbent assay (ELISA) was used to measure the levels of interleukin-6 (IL-6) according to manufacturers’ instructions (RayBio Eliza Kits, RayBiotech Life, Georgia, USA). It was measures before the procedure, then 36 hours, 1 week, and 2 weeks following the procedure.
Ultrasound guided technique
The procedure was performed using Toshiba Xario device. The linear transducer was placed over the bicipital groove, and the biceps tendon was identified. Then, a 25-gauge needle was introduced into the biceps tendon sheath. Care was taken not to inject the medication inside the tendon itself to avoid rupture. Lidocaine was initially injected to confirm the presence of peritendinous flow. After that, 2 ml of PRP was injected in the PRP group, while meloxicam 15 ml was injected in the NSAIDs group.
Atechnically successful procedure was identified by distention of the biceps tendon sheath and circumferential coating of the biceps tendon by the injectate. After procedure, patient was advised to rest for at least 3 days, and to apply a plastic bandage for 10 hours. Both VAS and Oxford scores were assessed 3 days, 1, and 4 weeks after injection.
Sample size calculation
Sample size was calculated using Power Analysis and Sample Size software program (PASS) version 15.0.5 for windows (2017) using data obtained from a pilot study conducted on 10 patients at Mansoura university hospital with short term effect of PRP on biceps tendinitis one week after treatment measured by interlukin-6 levels as the primary outcome. Patients were allocated into two groups: PRP Group and control Group.
Interlukin-6 levels at one week was 7.81 ± 1.039 for the PRP group and 8.39 ± 0.782 for the control group. A sample size of 41 patients in each group is needed to achieve 80% power (1-β or the probability of rejecting the null hypothesis when it is false) in the proposed study using two-sided two-sample unequal-variance t-test with a significance level (α or the probability of rejecting the null hypothesis when it is true) of 5%. 10% drop-out is expected, so 44 patients will be enrolled to each group.
Statistical Analysis
IBM’s SPSS statistics (Statistical Package for the Social Sciences) for windows (version 25, 2017) was used for statistical analysis of the collected data. Shapiro-Wilk test was used to check the normality of the data distribution. Quantitative variables were expressed as mean and standard deviation while categorical variables were expressed as frequency and percentage. Independent sample T and Mann Whitney tests were used for inter-group (between subjects) comparison of parametric and non-parametric continuous data with no follow up readings respectively. Fisher exact and Chi square tests were used for inter-group comparison of nominal data using the crosstabs’ function. All tests were conducted with 95% confidence interval. P (probability) value < 0.05 was considered statistically significant.
Results
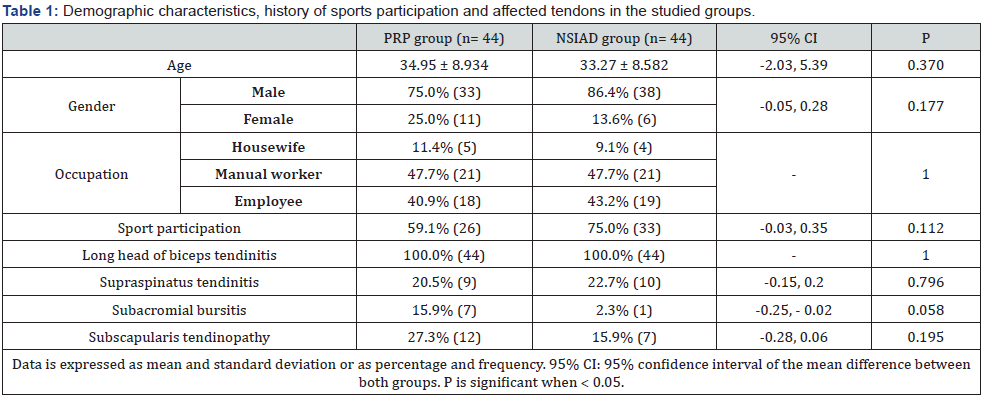
The mean age of the included cases was 34.95 and 33.27 years for PRP and NSIADs group respectively. Males represented 75 and 86.4% of cases in both groups respectively. As regard occupation, most of the included cases were manual workers (47.7% of cases in both groups), followed by employee (40.9 and 43.2% of cases respectively), and housewives (11.4 and 9.1% of cases in both groups respectively). Participation in sports was reported by 59.1 and 75% of cases in both groups respectively. Although all cases had tendonitis affecting the long head of biceps, some cases had concomitant supraspinatus, subacromial, or subscapularis tendinitis. All the previous parameters did not differ significantly between the two study groups (p > 0.05). These data are illustrated at table 1.
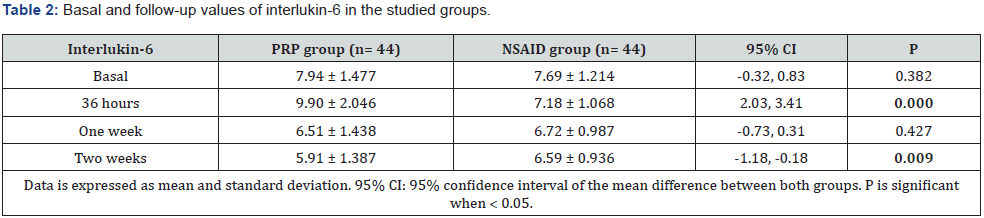
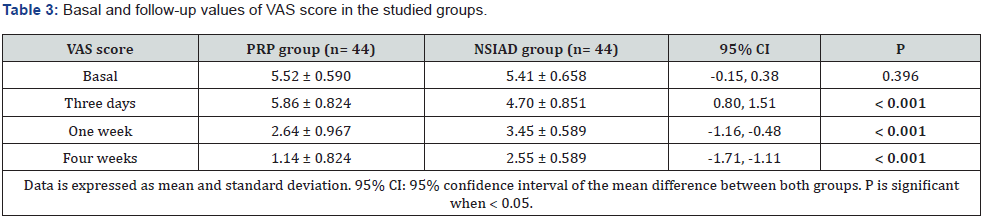
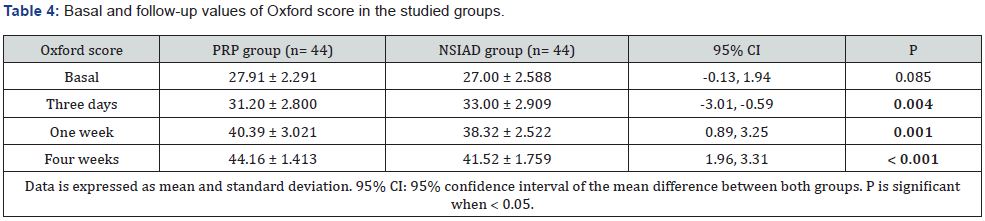
Basal IL-6 levels did not differ significantly between the two groups. After 36 hours, there was a significant increase in IL-6 levels in the PRP compared to the NSAIDs group (p < 0.001). However, after 2 weeks, IL-6 levels decreased significantly in the PRP group compared to the other group. Table 2 illustrated these data. Regarding VAS score, it did not differ between the two groups before intervention. Nevertheless, the NSAIDs group showed significant improvement regarding pain relief compared to the PRP group within the early three days after injection. On the subsequent visits, there was more significant pain improvement in the PRP group. These data are illustrated at table 3. Oxford shoulder score showed the same improvement changes like VAS. It did not differ between the two groups before intervention. Although the NSIADs group showed a significant improvement in the early three days, the PRP group had the upper hand on the subsequent follow up visits. Table 4 illustrates these data.
Discussion
This study was conducted at Mansoura University Hospitals and Knee &Shoulder orthopedic center in Mansoura, Egypt aiming to compare between PRP and NSIADs injections in the management of LHBT. We included a total of 88 cases who were randomly divided into two groups; the first group included 44 cases who underwent PRP injection, while the other 44 cases who underwent NSAIDs (meloxicam) injection were included in the second group. To the best of our knowledge, there is a paucity of studies comparing the efficacy of these two injections in the current literature. In the current study, the mean age of the included cases was 34.95 and 33.27 years for PRP and NSIADs group respectively, without significant difference between the two groups. As regard occupation, most of the included cases were manual workers (47.7% of cases in both groups). It was previously reported that biceps tendon pathologies are often encountered in patients whose age between 18 and 35 years, who are subjected to hard manual work or high impact sports [6].
In the current study, basal IL-6 levels did not differ significantly between the two groups. After36 hours, there was a significant increase in IL-6 levels in the PRP compared to the NSAIDs group (p < 0.001). However, after 2 weeks, IL-6 levels decreased significantly in the PRP group compared to the other group (Figure 1). A previous study has reported that PRP decreased both gene expression and production of IL-6 in tendon cells [20]. Interleukin 6 (IL-6), promptly and transiently produced in response to infections and tissue injuries, contributes to host defense through the stimulation of acute phase responses, hematopoiesis, and immune reactions [21].
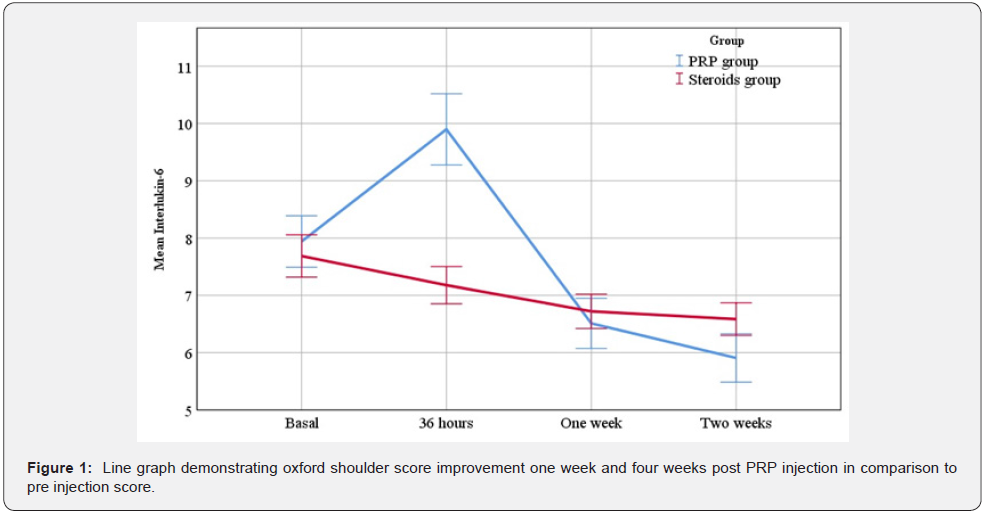
Unlike the information provided by the presence of inflammatory cells, current evidence on the inflammation markers shown in tendinopathic tendons do not show a consistent picture [22]. A previous study has reported that IL-6 expression is significantly increased in the synovium cases with supraspinatus tear [23]. The initial increase in IL-6 levels in the PRP group could be attributed to immunological reaction or the initial inflammatory tissue response to PRP. This elevation was settled as local inflammation subsides. Also, the leucocytes present in the PRP preparation may cause IL-6 over expression, and that may explain the initial increase encountered in our results [24]. Further studies handling the molecular levels need to be conducted to clarify the exact changes of serum IL-6 after PRP injections.
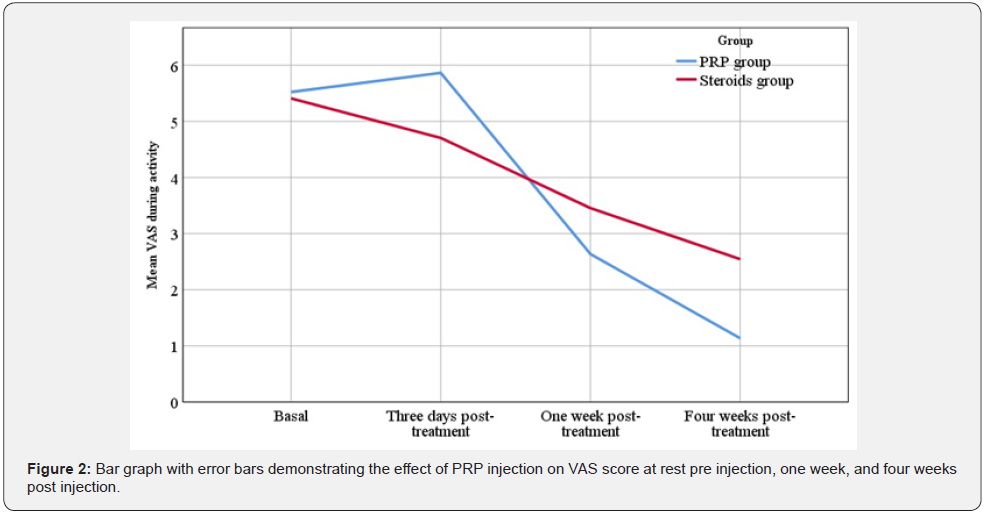
In the current study, VAS score did not differ between the two groups before intervention. Nevertheless, the NSAIDs group showed significant improvement regarding pain relief compared to the PRP group within the early three days after injection. On the subsequent visits, there was more significant pain improvement in the PRP group (Figure 2). Oxford shoulder score also did not differ between the two groups before intervention. Although the NSAIDs group showed a significant improvement in the early three days, the PRP group had the upper hand on the subsequent follow up visits (Figure 3). Our results imply that NSAIDs can achieve more rapid response, whereas PRP causes a delayed but more effective relief.
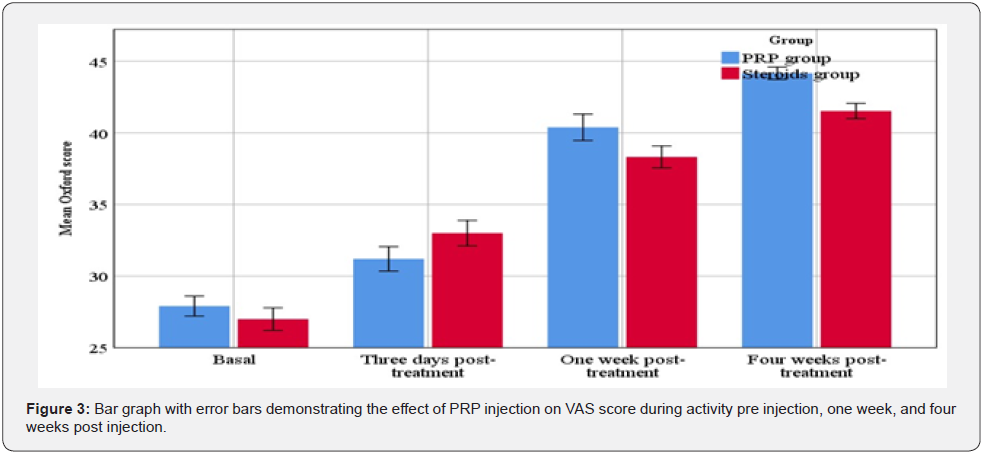
Oral NSIADs are considered the main treatment prescribed for musculoskeletal pain due to its strong anti-inflammatory properties [25]. Besides, multiple studies have confirmed the efficacy of local application of these medications for multiple musculoskeletal conditions [7,26,27]. However, other authors reported that the response was more rapid in steroid injection compared to NSAIDs. They attributed that finding to the fact that steroid, along with its anti-inflammatory effect, can inhibit collagen, granulation tissue, and extracellular matrix formation, whereas NSAIDs do not [28]. Min and his colleagues reported conducted a study to compare between subacromial injection of steroids (triamcinolone 40 mg) versus NSIAD (ketorolac 60 mg) in the management of shoulder impingement syndrome. After 1 month, there was significant improvement of pain and motion range in both groups. Nevertheless, University of California at Los Angeles shoulder scale showed better improvement in the NSAIDs group (7.15 vs. 2.13 in steroids and NSIAD groups respectively - p = 0.03). Other outcome parameters did not differ significantly between steroids and NSIAD [29].
Another study also confirmed the efficacy of NSIADs in musculoskeletal conditions. Shakeel et al. compared triamcinolone and diclofenac injections in relieving symptoms of trigger finger. Complete symptomatic resolution was achieved in 70 and 53% of cases in steroid and NSIAD groups respectively. Moreover, no significant difference was detected between the two groups regarding Quinnell score 3 months after injection [28]. Furthermore, another study compared intraarticular steroids versus NSAIDs injections in knee osteoarthritis. VAS score showed significant decrease in both groups for 24 weeks (from 6.3 to 4.6 in the NSAIDs group, and from 5.2 to 3.6 in the steroid group). The difference between the two groups was statistically insignificant. Nevertheless, NSAIDs were found to save much financial costs compared to steroids [30].
All the previous three studies confirmed that local NSAIDs injection is effective in relieving pain, and that agrees with our findings. Regarding PRP application in tendinopathies in the literature, another study has reported the effectiveness of PRP in the management of biceps tendinitis. VAS score decreased from 6 before intervention down to 0.5 at the final follow up (p < 0.002). In addition, elbow functional assessment score increased from 63 before intervention up to 90 after it (p < 0.004). Authors concluded that PRP injection may be a promising modality for biceps tendinitis resistant to the standard therapy [31].
Another study compared the efficacy of PRP injection versus physical therapy (PT) in partial supraspinatus tears. Both VAS, Disabilities of Arm, Shoulder and Hand questionnaire (DASH), and range of motion were improved significantly in both groups. However, DASH score showed significant better improvement in the PRP compared to PT group [32]. Moreover, another study reported that PRP was significantly better than the dry needling from six weeks to six months after initial injection (P < 0.05). The mean Shoulder Pain and Disability Index was 17.7 in the plateletrich plasma group while it was 29.5 in the dry needling group (p< 0.05) after 6 months [33]. Furthermore, PRP was found to be as good as steroid injections in patients with rotator cuff tear [34]. Conversely, other authors investigated the role of PRP in cases with chronic rotator cuff tendinopathy, and they reported that PRP injection was not effective in improving quality of life, pain, disability, and range of movement. VAS and other functional scores did not differ between the two groups at 1-year follow up [35]. This study has multiple limitations; first, it is only a two centers trial. Besides, the follow up period was limited to 4 weeks with single injection. Therefore, more studies from different centers with longer follow up periods should be conducted soon.
Conclusion
Based on our findings, ultrasound guided injection of PRP and NSAIDs is effective in managing LHBT symptoms. However, a more significant improvement is achieved with PRP.
References
- Patton WC, McCluskey III GM (2001) Biceps tendinitis and subluxation. Clinics in sports medicine. 20(3): 505-529.
- Kibler W (2006) Scapular involvement in impingement: signs and symptoms. Instr Course Lect 55: 35-43.
- Harwood MI, Smith CT (2004) Superior labrum, anterior–posterior lesions and biceps injuries: diagnostic and treatment considerations. Primary Care: Clinics in Office Practice 31(4): 831-855.
- Ahrens P, Boileau P (2007) The long head of biceps and associated tendinopathy. J Bone Joint Surg Br 89(8): 1001-1009.
- Hassan S, Patel V (2019) Biceps tenodesis versus biceps tenotomy for biceps tendinitis without rotator cuff tears. J Clin Orthop Trauma 10(2): 248-256.
- Churgay CA (2009) Diagnosis and treatment of biceps tendinitis and tendinosis. American family physician 80(5): 470-476.
- Bhattacharjee DP, Biswas C, Haldar P, Ghosh S, Piplai G, et al. (2014) Efficacy of intraarticular dexamethasone for postoperative analgesia after arthroscopic knee surgery. J Anaesthesiol Clin Pharmacol 30(3): 387-390.
- Jones A, Doherty M (1996) Intra-articular corticosteroids are effective in osteoarthritis but there are no clinical predictors of response. Ann Rheum Dis 55(11): 829-832.
- Paavola M, Kannus P, Jarvinen TA, Jarvinen TL, Jozsa L, et al. (2002) Treatment of tendon disorders. Foot and ankle clinics 7(3): 501-513.
- Cole BJ, Schumacher Jr RH (2005) Injectable corticosteroids in modern practice. J Am Acad Orthop Surg 13(1): 37-46.
- Sardana V, Burzynski J, Hasan K, Zalzal P (2018) Are non-steroidal anti-inflammatory drug injections an alternative to steroid injections for musculoskeletal pain?: A systematic review. J Orthop 15(3): 812-826.
- Bitterman A, Gao S, Trella K, Li J, Galante J, et al. (2017) Time related effects of non-steroidal anti-inflammatory drugs on Achilles tendinopathy in a murine model. Foot & Ankle Orthopaedics 2(2): 2473011416S00002.
- Dogan N, Erdem AF, Gundogdu C, Kursad H, Kizilkaya M (2004) The effects of ketorolac and morphine on articular cartilage and synovium in the rabbit knee joint. Canadian journal of physiology and pharmacology 82(7): 502-505.
- Wong C, Jean Y, Wen Z, Chang Y (2006) Intraarticular injection of the cyclooxygenase-2 inhibitor parecoxib attenuates osteoarthritis after anterior cruciate ligament transection: role of excitatory amino acids: A-882. European Journal of Anaesthesiology (EJA) 23: 228.
- Martinez‐Zapata MJ, Marti‐Carvajal AJ, Sola I, Exposito JA, Bolibar I, et al. (2016) Autologous platelet‐rich plasma for treating chronic wounds. Cochrane Database of Systematic Reviews (5): CD006899.
- Wasterlain AS, Braun HJ, Dragoo JL (2016) Contents and formulations of platelet rich plasma. In: Maffulli N, editor. Platelet Rich Plasma in Musculoskeletal Practice: Springer p. 1-29.
- de Mos M, van der Windt AE, Jahr H, van Schie HT, Weinans H, et al. (2008) Can platelet-rich plasma enhance tendon repair? A cell culture study. The American journal of sports medicine 36(6): 1171-1178.
- Lesage F-X, Berjot S, Deschamps F (2012) Clinical stress assessment using a visual analogue scale. Occupational medicine 62(8): 600-605.
- Dawson J, Rogers K, Fitzpatrick R, Carr A (2009) The Oxford shoulder score revisited. Arch Orthop Trauma Surg 129(1): 119-123.
- Andia I, Rubio-Azpeitia E, Maffulli N (2015) Platelet-rich plasma modulates the secretion of inflammatory/angiogenic proteins by inflamed tenocytes. Clin Orthop Relat Res 473(5): 1624-1634.
- Tanaka T, Narazaki M, Kishimoto T (2014) IL-6 in inflammation, immunity, and disease. Cold Spring Harbor perspectives in biology 6(10): a016295.
- Jomaa G, Kwan C-K, Fu S-C, Ling SK-K, Chan K-M, et al. (2020) A systematic review of inflammatory cells and markers in human tendinopathy. BMC Musculoskelet Disord 21(1): 78.
- Shindle MK, Chen CC, Robertson C, DiTullio AE, Paulus MC, et al. (2011) Full-thickness supraspinatus tears are associated with more synovial inflammation and tissue degeneration than partial-thickness tears. Journal of shoulder and elbow surgery 20(6): 917-927.
- Zhou Y, Wang JH (2016) PRP treatment efficacy for tendinopathy: a review of basic science studies. Biomed Res Int 2016: 9103792.
- Nelson AE, Allen KD, Golightly YM, Goode AP, Jordan JM, et al. (2014) A systematic review of recommendations and guidelines for the management of osteoarthritis: the chronic osteoarthritis management initiative of the US bone and joint initiative. Semin Arthritis Rheum 43(6): 701-712.
- Convery P, Milligan K, Quinn P, Scott K, Clarke R (1998) Low‐dose intra‐articular ketorolac for pain relief following arthroscopy of the knee joint. Anaesthesia 53(11): 1125-1129.
- Gupta A, Axelsson K, Allvin R, Liszka-Hackzell J, Rawal N, et al. (1999) Postoperative pain following knee arthroscopy: the effects of intra-articular ketorolac and/or morphine. Regional anesthesia and pain medicine 24(3): 225-230.
- Shakeel H, Ahmad TS (2012) Steroid injection versus NSAID injection for trigger finger: a comparative study of early outcomes. The Journal of hand surgery 37(7): 1319-1323.
- Min KS, Pierre PS, Ryan PM, Marchant BG, Wilson CJ, et al. (2013) A double-blind randomized controlled trial comparing the effects of subacromial injection with corticosteroid versus NSAID in patients with shoulder impingement syndrome. J Shoulder Elbow Surg 22(5): 595-601.
- Bellamy JL, Goff BJ, Sayeed SA (2016) Economic impact of ketorolac vs corticosteroid intra-articular knee injections for osteoarthritis: a randomized, double-blind, prospective study. The Journal of arthroplasty 31(9): 293-297.
- Sanli I, Morgan B, van Tilborg F, Funk L, Gosens T (2016) Single injection of platelet-rich plasma (PRP) for the treatment of refractory distal biceps tendonitis: long-term results of a prospective multicenter cohort study. Knee Surgery, Sports Traumatology, Arthroscopy 24(7): 2308-2312.
- Ilhanli I, Guder N, Gul M (2015) Platelet-rich plasma treatment with physical therapy in chronic partial supraspinatus tears. Iran Red Crescent Med J 17(9).
- Rha D-w, Park G-Y, Kim Y-K, Kim MT, Lee SC (2013) Comparison of the therapeutic effects of ultrasound-guided platelet-rich plasma injection and dry needling in rotator cuff disease: a randomized controlled trial. Clinical rehabilitation 27(2): 113-122.
- Von Wehren L, Blanke F, Todorov A, Heisterbach P, Sailer J, et al. (2016) The effect of subacromial injections of autologous conditioned plasma versus cortisone for the treatment of symptomatic partial rotator cuff tears. Knee Surgery, Sports Traumatology, Arthroscopy 24(12): 3787-3792.
- Kesikburun S, Tan AK, Yılmaz B, Yaşar E, Yazıcıoglu K, et al. (2013) Platelet-rich plasma injections in the treatment of chronic rotator cuff tendinopathy: a randomized controlled trial with 1-year follow-up. Am J Sports Med 41(11): 2609-2616.






























