Postraumatic Pseudoaneurysm of the Superficial Palmar Arch
*Pilar Aparicio, Óscar Izquierdo, Enric Domínguez and Juan Castellanos
Upper Limb and Microsurgery Unit, Orthopaedics Department, Parc Sanitari Sant Joan de Déu de Sant Boi de Llobregat, Spain
Submission: November 19, 2019;Published: November 27, 2019
*Corresponding author: Pilar Aparicio, Upper Limb and Microsurgery Unit, Orthopaedics Department, Parc Sanitari Sant Joan de Déu de Sant Boi de Llobregat, Barcelona, Spain
How to cite this article: Pilar Aparicio, Óscar Izquierdo, Enric Domínguez, Juan Castellanos. Postraumatic Pseudoaneurysm of the Superficial Palmar Arch. Ortho & Rheum Open Access J. 2019; 15(3): 555911. DOI: 10.19080/OROAJ.2019.15.555911
Abstract
We present a successfully treated case of a pseudoaneurysm of the superficial palmar arch after a penetrating wound. Aneurysm and pseudoaneurysm are very infrequent pathologies in the hand. The preferred treatment consists of surgical excision and vascular reconstruction.
Keywords: Microsurgery; Palmar arch; Pseudoaneurysm
Introduction
Aneurysm and pseudoaneurysm are infrequent pathologies found in the hand. Their diagnosis is mainly based on the clinical examination, but a good anamnesis is beneficial. Complementary imaging tests are also useful for the diagnosis and surgical planning, but the diagnosis must be confirmed by histologic examination. A pseudoaneurysm is defined as a dilatation of the artery wall that does not include the three layers of it, in contrast a real aneurysm is a dilatation of the three layers of the artery wall. Aneurysm and pseudoaneurysm of the hand had been described in the radial artery, but the ulnar artery is more frequently affected because as it is more exposed in its anatomical location in Guyon’s canal (as in hypothenar hammer syndrome). The most frequent mechanism of injury is a penetrating wound as in our case.
Case Report
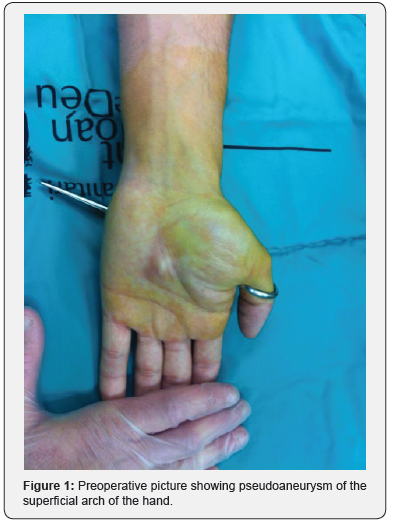
A twenty-five-year-old man, with no history of previous disease, came to the emergency room after cutting himself with a pair of scissors. He presented a puncture wound in the ulnar part of his left hand. After assessing the correct vascularization of the fingers, it was decided not to suture it. After a week, the patient came back to the emergency room because he presented a pulsatile mass of 2x2 cm in the volar part of his left hand, exactly in the place where the former puncture was (Figure 1).
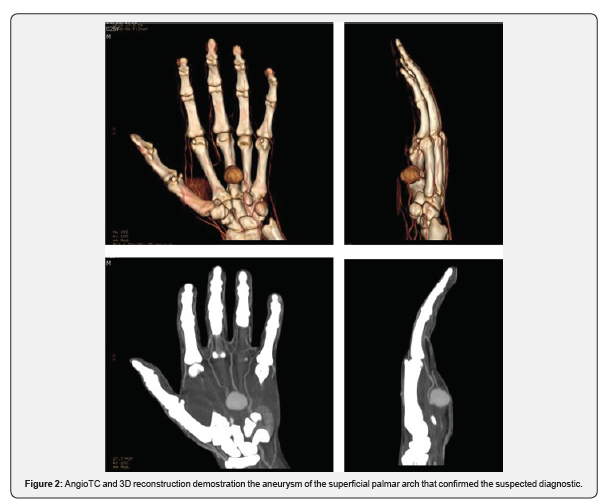
An ECO-Doppler and an angio-CT scan were performed and a pseudoaneurysm of the superficial palmar arch was confirmed (Figure 2). No active bleeding was assessed at this time, and the trophism of the fingers remained normal. Scheduled surgical revision was planned after 48 hours and an excision of the pseudoaneurysm was performed. An end-to-end anastomosis was done with no need for vascular grafts (Figure 3). The piece was sent to histologic examination and the diagnosis was confirmed.

The patient was discharged after two days post-operatively and received anticoagulant therapy with warfarin for four weeks and aspirin for three months. During the post-operative course, the surgical wound presented a dehiscence of the wound that was managed with topical dressings for three weeks until correct healing occurred. After a month an angio CT scan was performed and confirmed the complete removal of the pseudoaneurysm and the correct permeability of the superficial arch. After three months the patient was able to perform his daily life activities including sports. After seven months the patient was still asymptomatic.
Discussion
The difference between aneurysm and pseudoaneurysm lies in the vascular wall architecture. A pseudoaneurysm is defined as a dilatation because of partial tear of the artery wall while a true aneurysm is a dilatation of all three layers of the artery wall. Aneurysm and pseudoaneurysm of the hand have been found in the radial artery, although they are most frequently located in the ulnar artery since its more anatomically exposed. The ulnar artery is the most common site for true and false aneurysms of the upper extremity [1] and fingers are the most common location of aneurysm in the hand [2].
The pseudoaneurysm in the great majority of cases is formed after a penetrating wound, as in our case. The intima layer of the artery is damaged leading to external bleeding and hematoma formation, which allows the artery to repermeabilize and to form a fibrous eccentric evagination without the three artery layers.
However, there are cases of pseudoaneurysm formation of the palmar arch after carpal tunnel syndrome described in the literature [3].
On the other hand, true aneurysms are mainly associated with repetitive micro traumatisms of the tenar eminence, as in ulnar hammer syndrome [4] these micro traumatisms progressively debilitate the artery layers forming the pseudoaneurysm. Angiography is probably the most informative test for diagnosis, it provides information of localization of the tumor as well as the presence of collateral branches that may help with the operative planning, however there is some controversy in its systematic use because of the possibility of distal finger embolism [2]. MRI and ultrasound are not associated with these potential risk factors and have proved to be adequate for surgery planning as well.
We used an Eco-Doppler and angio-CT to confirm the diagnosis. The differential diagnosis between pseudoaneurysm and true aneurysm must be confirmed by histological examination, in our case as no arterial layers were found a pseudoaneurysm was confirmed as the final diagnosis. Regarding different treatments, ultrasound-guided thrombin injection has been shown to be effective in the treatment of peripheral pseudoaneurysms; however, its application in the management of radial or ulnar artery pseudoaneurysms has not been well established [5].
Endovascular techniques such as coil embolization have been employed with success in the treatment of false aneurysms of the superficial palmar arch. This minimally invasive method may be an alternative to open surgery in the management of these lesions, especially in hemodynamically unstable patients[6]. The gold standard treatment is open surgical resection with ligation or arterial reconstruction6, once the mass is resected revision under microscope of the arteries is mandatory for assessment of the intima layer wall, as the presence of any separation in that layer may cause recurrence of the aneurysm.
Cardiac surgery literature supports the use of arterial grafts in preference to venous grafts for long-term patency. These arterial segments are easier to handle than veins, have a more predictable distal branching pattern for multiple distal junctures, and tend not to collapse while being sutured. However, long-term studies of the use of arterial grafts for ulnar artery reconstruction have not been performed to date [1,7]. In our case the extended dissection of the superficial palmar arch and its collaterals allowed the reconstruction with an end-toend anastomosis with no need for grafts.
Anticoagulation with warfarin and antiaggregating with aspirin regimen was administered to the patient after surgery, although some authors do not recommend anticoagulation on a regular basis [2,6]. All the patients undergoing arterial reconstruction in our center are prescribed warfarin and aspirin as, in our opinion, this treatment can decrease thrombotic events. Pseudoaneurysms of the palmar arch are rare entities with only eleven cases described in the English literature, four of them corresponding to pediatric patients two of them were yatrogenic aneurysm after carpal tunnel decompression [2,3] the other four were due to a penetrant wound. Only one of the cases was treated conservatively.
References
- McClinton MA (2011) Reconstruction for Ulnar Artery Aneurysm at the Wrist. Journal of Hand Surgery 36(2): 328-332.
- Sakamoto A, Arai K (2009) False aneurysm of the superficial palmar arch in a child: a case report. Cases J 2(1): 7985–7994.
- Gull S, Spence RAJ, Loan W (2011) Superficial Palmar Arch Aneurysm after Carpal Tunnel Decompression, a Rare Complication: A Case Report. Case Reports in Medicine 2011(2): 1-3.
- Smith HE, Dirks M, Patterson RB (2004) Hypothenar hammer syndrome: Distal ulnar artery reconstruction with autologous inferior epigastric artery. Journal of Vascular Surgery 40(6): 1238-1242.
- Komorowska Timek E, Teruya TH, Abou Zamzam AM Jr, Papa D, Ballard JL (2004) Treatment of radial and ulnar artery pseudoaneurysms using percutaneous thrombin injection. Journal of Hand Surgery 29(5): 936-942.
- Schoretsanitis N, Moustafa E, Beropoulis E, Argyriou C, Georgiadis G, Georgakarakos E (2016) Traumatic Pseudoaneurysm of the Superficial Palmar Arch: A Case Report and Review of the Literature. J Hand Microsurg 07(01): 230-232.
- Fabbrocini M, Fattouch K, Camporini G, DeMicheli G, Bertucci C et al. (2003) The descending branch of lateral femoral circumflex artery in arterial CABG: early and midterm results. Ann Thorac Surg 75(6): 1836-1841.






























