Conventional Open Reduction and Internal Fixation (ORIF) Compared to Minimally Invasive Plate Osteosynthesis (MIPO) for Treatment of Extra-Articular Distal Tibia Fractures - A Prospective Randomized Trial
Ahmed A Khalifa1*, Tarek A Abdel-Daym1, Hamdy Tammam1, ElSayed Said1 and Hesham Refae2
1Qena faculty of medicine and its university hospital, South Valley University, Egypt
2Aswan faculty of medicine, Aswan University, Egypt
Submission: January 20, 2019;Published: February 12, 2019
*Corresponding author: Ahmed A KhalifaFRCS (Tr. & Ortho), Assistant Lecturer, Orthopaedic and Traumatology Department, Qena faculty of medicine and its University hospital, South Valley University, Qena, Egypt
How to cite this article: Ahmed A K, Tarek A A D, Hamdy T, ElSayed S, Hesham R. Conventional Open Reduction and Internal Fixation (ORIF) Compared to Minimally Invasive Plate Osteosynthesis (MIPO) for Treatment of Extra-Articular Distal Tibia Fractures - A Prospective Randomized Trial. Ortho & Rheum Open Access J 2019; 13(4): 555867.DOI: 10.19080/OROAJ.2019.13.555867
Abstract
Introduction/Objective: Extra-articular distal tibia fracture considered one of the most common fracture faced by a trauma surgeon with a diversity of treating techniques with no consensus regarding the best option for management, the objective of this study was to prospectively compare our results of 2 groups of extra-articular distal tibia fracture treated by ORIF or MIPO technique.
Patient and Methods: 40 patients included in the study, 20 patients randomly allocated to each group, including closed or open GI fractures in patients older than 18 years, both pre, post-operative and last follow up AP and Lat. radiographs was assessed, incidence of wound complications, fracture union, blood loss, operative time and fluoroscopy time were reported.
Results: There were no significant differences between the two groups in terms of age, sex, type of fracture, distribution of infection, operative time, bone union time, and Teeny & Wiss score (p>0.05). Nevertheless, skin infection was more in the ORIF group 5 cases against 1 in MIPO group. fluoroscopy time was significantly longer in the MIPO group than in the ORIF group: 87.25±24.52 seconds for, and 41.25±10.37 seconds respectively (p<0.05). Amount of blood loss in the ORIF group was significantly larger than the MIPO group: 46.75±12.16 cc, and 79.1±21.48 cc respectively (p<0.05).
Conclusion: From our results we believe that both ORIF and MIPO techniques are valid in treating extra-articular distal tibia fracture, although MIPO may have a longer operating and fluoroscopy time, but it has the advantage of less bleeding and minimal wound complications.
Keywords: Extra-Articular; Distal Tibia Fracture; ORIF; MIPO
Background/Introduction
The (AO-43A) extra-articular distal tibia facture considered to be one of the most common fracture types, which mainly can result from simple falls, traffic accidents, or sports-related injuries as a result of axial compression and/or rotational forces [1-3]. The decision to treat these fractures conservatively or operatively depends mainly on the fracture pattern and soft tissue status, usually conservative treatment leads to unacceptable results [4]. intramedullary nailing, plate osteosynthesis and external fixation considered the main lines of operative intervention [5,6]. However, there is no consensus for the optimal surgical technique [7]. With the advancement of internal fixation techniques, minimally invasive plate osteosynthesis (MIPO) designed as a new approach for a biological friendly osteosynthesis, which rapidly gained superiority over conventional open reduction and internal fixation (ORIF) especially in treating distal tibia extra-articular fractures (AO-43A) [8-12]. The objective of this study was to prospectively compare the results of 2 groups of extraarticular distal tibia fracture treated by ORIF or MIPO at Qena university Hospital (a new tertiary referral centre in upper Egypt).
Patients and Methods
This is a prospective randomized study of (40) patients diagnosed with extra-articular distal tibia fracture(AO-43A) according to AO classification system, presented to trauma unit at Qena University hospital (a new tertiary referral hospital in upper Egypt) in the period between July 2017 to April 2018. Patients aged 18 years and older diagnosed with closed or open GI (according to Gastillo classification) extra-articular distal tibial fracture with or without fibular fracture were included in the study. patients with pathological fracture, open Gǁ or above, fracture of the proximal two thirds of the tibia and intra-articular fracture extension were excluded. patients were randomized into two groups 20 patients in each group.
Preoperative Management Protocol
Following ATLS protocol for initial assessment and after following careful history taking including (occupation, special habits of medical importance, pre-fracture walking ability, history of trauma and duration of fracture), local clinical examination was performed for all patients mainly for assessment of skin condition, evaluation of distal neurovascular structures and to detect any signs suggesting compartment syndrome.
Radiological Assessment
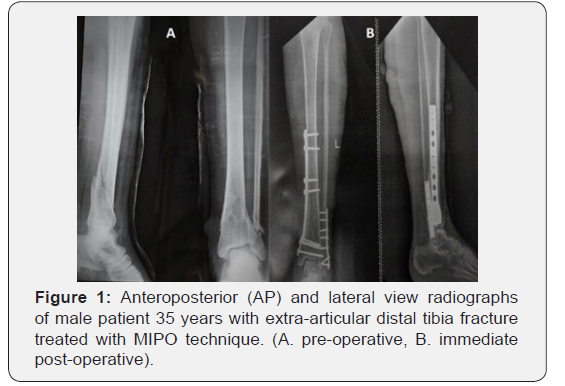
Apart from radiographs needed for the ATLS protocol, Plain radiographs (pre- and immediate post-operative) including an anteroposterior (AP) and lateral views (Figure 1) of tibia including knee and ankle joints and an ankle mortise view whenever needed. Verbal and written informed consent was taken prior to surgery, all patients were consulted about type of surgery and possible complications.
Surgical Procedure
All cases were operated upon or supervised by a senior trauma surgeon and under spinal anesthesia for all cases with a tourniquet used and inflated to 150 above systolic blood pressure, the patient was positioned supine on a radiolucent operative table to ease intraoperative fluoroscopy usage, draping was done in the usual manner to above the knee level, if the fibula fracture was comminuted or involving the syndesmosis it was managed first by ORIF using plate and screws followed by fixation of the tibia fracture.
In ORIF group, the standard anteromedial approach was performed. The distal tibia Fracture was fixed using anatomical distal tibia plate (The choice to use a locked versus non-locked plate in both groups was determined according to the patient bone quality and the surgeon preference, where locked plate was preferred in osteoporotic patients) with at least 3 screws (6 cortices) for each main fragment. In MIPO group, an indirect reduction technique was carried out manually and alignment checked under fluoroscopy.
A distal longitudinal incision was performed at the medial side of the distal tibia approximately 2 cm in length cantered over the medial malleolus to allow insertion of the plate. The saphenous vein and nerve were identified and protected. After choosing an appropriate plate length (according to the configuration and extension of the fracture, taking in consideration that at least 3 screws can be inserted in the proximal fragment), A proximal incision was made under fluoroscope for delivery of the plate. A subcutaneous extra-periosteal tunnel was created by a dissection forceps and followed by the insertion of a plate from the distal to proximal incision. The plate position was checked under fluoroscopy until proper positioning was achieved. screws were inserted with at least 3 screws in each main fragment, wound closure done in layers with no suction drain used in either group.
Postoperative Evaluation and Care
Immediate postoperative plain radiograph (AP and lateral) to assess the reduction and plate position, all patients were encouraged to move the ankle joint starting from day 1 postoperative, and ambulation with crutches at day 2 with Strict non- weight bearing on the operated side, leg was elevated to reduce swelling using elastic bandage, with close monitoring for any signs suggesting development of compartment syndrome. Patients follow up protocol was as follows: after 2 weeks for stitch removal, then at 6 weeks, 3 months and after 6 months for assessment of skin condition and for clinical and radiological evaluation.

At 6 months follow up Visit: The functional outcome was evaluated with the clinical rating for the ankle by Teeny and Wiss criteria [13] and radiographs (AP and lateral views) were obtained to assess fracture union according to Apley and Solomon’s criteria [14] complete bone union according to these criteria defined as the time at which there is no pain upon local palpation, no swelling in the limb, an ability to walk without support and pain free, and an evidence of a radiographic bridging callus or trabecula between fragments (Figure 2).
Statistical analysis was performed using SPSS statistical software (version 22.0). Independent samples t-test or Mann- Whitney U test were used to compare the quantitative variables. The qualitative variables were compared using the chi-square test. P < 0.05 was considered statistically significant.
Results
All patients were available for the last follow up, the groups were compared with respect to gender, age, fracture type, operating time, type of plate used, amount of blood loss, fluoroscopy time, bone healing time, incidence of skin infection (in the first 2 weeks), gait and functional ankle outcome.
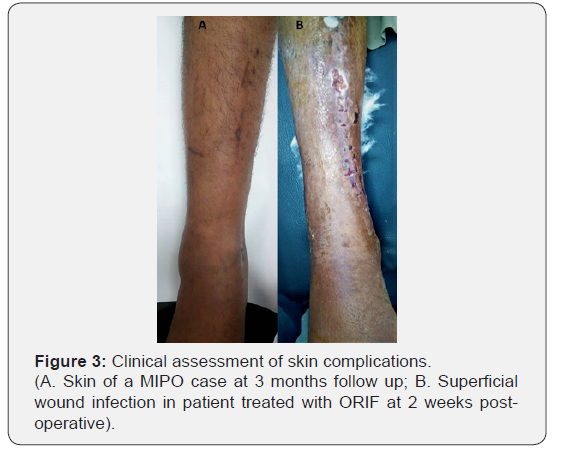
Table 1 presents the demographic data and all outcomes for the two groups that were cross-matched. As is shown, there were no significant differences between the two groups in terms of age, sex, and type of fracture. The time of surgery was shorter in the ORIF group; however, the difference was not statistically significant (p>0.05). There were no significant differences in the distribution of infection, bone union time, gait or Teeny & Wiss score (p>0.05). Nevertheless, the difference in skin infection is considered clinically relevant (Figure 3), being more in the ORIF group, of the 5 cases that had superficial wound infection in the ORIF group, 4 were diagnosed as open GI fracture. Our results indicated that the fluoroscopy time was significantly longer in the MIPO group than in the ORIF group: 87.25±24.52 seconds for the MIPO, and 41.25±10.37 seconds for the ORIF group (p<0.05); but the amount of blood loss in the ORIF group was significantly larger than in the MIPO group: 46.75±12.16 cc, and 79.1±21.48 cc respectively (p<0.05). 30 patients (75%) had associated fibula fracture, 23 patients needed ORIF. At the last follow up, we didn’t encounter any cases with skin problems especially sloughing or necrosis.
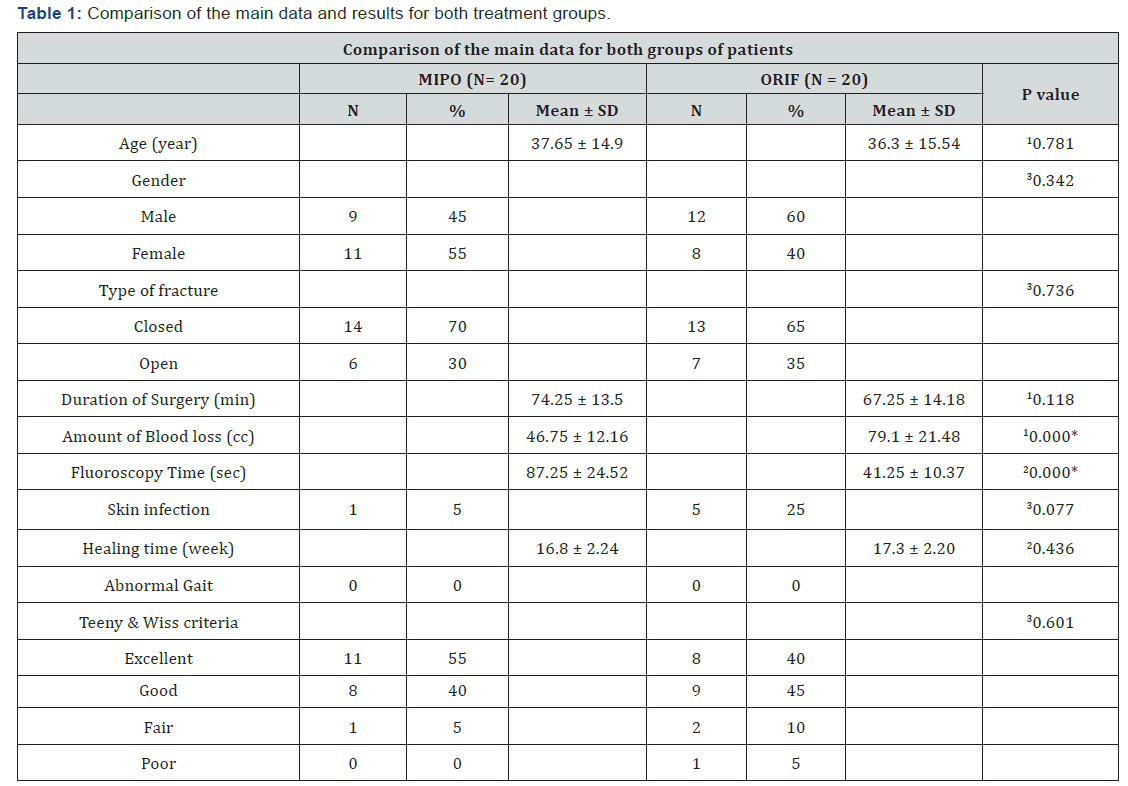
1Independent t-test; 2Mann-Whitney U test; 3Chi-square test; *p<0.05.
MIPO: Minimally Invasive Plate Osteosynthesis; ORIF: Open Reduction And Internal Fixation; SD: standard Deviation.
Discussion
Extra-articular distal tibia fracture (AO- 43A) represents a challenging situation for the trauma surgeon, insufficient blood supply, proximity to the ankle joint and often poor bone quality of the distal fragment contributes to this situation [2,3]. The main goals in treating distal tibia fractures are: anatomical reduction, restoration of axial alignment, maintenance of joint stability, achievement of fracture union, pain free weight baring, and minimal wound complications [15], Although these goals can be achieved by different lines of management, but each carries its own deficiency, non-operative treatment may be complicated by loss of reduction and subsequent malunion; external fixation may result in insufficient reduction, malunion, and pin tract infection; there is some concern about the use of IMN with a short distal segment and lastly ORIF necessities extensive soft tissue dissection which may increase the incidence of wound complications and infections [16].
To minimize disruption of the particularly delicate softtissue envelope and periosteal blood supply, minimally invasive plate osteosynthesis (MIPO) was developed [17] to maintain a more biologically favourable environment for fracture healing [18]. In this study we focused mainly on comparing ORIF to MIPO prospectively in randomised matched 2 groups of patients presented at our trauma unit, which is considered as a new tertiary referral centre in upper Egypt.
According to clinical rating for the ankle by Teeny and Wiss, 90 % of patients in our series had excellent and good results while 10 % had a fair or poor results, with no significant difference between both treatment groups, our results were comparable to Mahajan who reported 91 % excellent and good clinical results with MIPO technique in 20 patients with distal tibia fractures while 9% had a fair results [19]. Webb et al. reported a functional outcome following MIPO in distal tibia fractures which did not significantly differ from that of the general population [20]. Wound problems considered to be one of the most annoying complication to the trauma surgeon while treating this type of fracture, mainly infection and skin necrosis [3,21-23]. Extensive soft tissue dissection accompanied with ORIF increases the risk of wound complications [21,24,25]. Overall wound complications (mainly infection) in our series in both groups were 15 %, distributed as five cases in the ORIF group against one only in the MIPO group, although there was no statistically significant difference in the incidence between both groups, but we consider this a clinical significant finding, apart from soft tissue dissection needed for exposure and fixation in ORIF group, four of the five cases had an open fracture, both factors may contribute to increase incidence of infection in ORIF group.
Our results in the ORIF which was 12.5 % of overall infection incidence were comparable to what was reported by Yih-Shiunn Lee et al. who had a superficial infection rate of 8% in distal tibia fracture treated by ORIF technique [26] also Jensen et al. [27] reported 9% superficial infections in a case series of one hundred and five patients treated with ORIF. Guo et al. [9] and Yong chuan Li et al. [11] reported a rate of wound complications of 14.6% and 19% respectively using MIPO technique, which considered higher than the reported incidence in our MIPO group which was only 2.5%.
At the last follow up, fracture union was observed in all study cases in both groups, although at 3 months follow up, three patients didn’t show signs of union, but they did show bone healing at the last follow up after advising the patients to strictly stop smoking, up to 12% non-union incidence among patients treated for distal tibia fracture had been reported in some series [28-30]. while MIPO with the idea of biological osteosynthesis was popularized with the advantage of minimizing the trauma to the already injured zone and preserve the circulation around the fracture site which preserves the biological environment for optimum fracture healing [31], Hasenboehler et al. [28] reported that prolonged healing times were observed in simple fracture patterns treated with MPIO, also other studies reported a rate of delayed union or non-union to be 5 to17% [32].
Although, operative time was not statistically different between both groups, but it was relatively longer in the MIPO group which can be attributed to the longer time of fluoroscopy usage (which was significantly longer than the ORIF group), but we did find a comparable operative time in MIPO group to what had been reported by Guo et al. [9], Wang Cheng et al. [16] and Jun Shen et al. [31] where they reported a mean operative time with MIPO technique to be 97.9 min, 113.33 min and 56.0 min respectively. Even with the use of tourniquet in both groups, we did find a significant difference in blood loss between both groups, being more in the ORIF group, while the mean blood loss in MIPO group was comparable to the results by Jun Shen et al. [31] where they had a mean blood loss of 20 ml with MIPO technique for distal tibia fracture. Surprisingly, blood loss with a MIPO technique can even reach to a mean of 350 ml as had been reported by Wang Cheng et al. [16].
23 patients underwent ORIF out of total 30 patients with a concomitant fracture fibula in our series, according to Bonnevialle et al. [33], the decision to fix the fibula was made when instability of the inferior tibio-fibular syndesmosis is diagnosed or if the fracture was comminuted and this offers restoration of the lateral column which may help in indirect reduction of a comminuted distal tibia fracture, also it prevents fracture collapse [34].
Limitations
Being a single centre study with a small sample size may affect the significance of the results, also the short term follow up which couldn’t pick late complications
Conclusion
From our results we believe that both ORIF and MIPO techniques are valid in treating extra-articular distal tibia fracture, although MIPO may have a longer operating and fluoroscopy time, but it has the advantage of less bleeding and minimal wound complications.
Acknowledgement
I would like to acknowledge the great effort done for the statistical analysis of the data by Dr. Ahmed Ahmed, an intern in orthopaedic and traumatology department, Qena university hospital. All authors declare no conflict of interest and no funding.
References
- Achten J, Parsons NR, McGuinness KR, Petrou S, Lamb SE, et al. (2015) UK Fixation of Distal Tibia Fractures (UK FixDT): protocol for a randomised controlled trial of ‘locking’plate fixation versus intramedullary nail fixation in the treatment of adult patients with a displaced fracture of the distal tibia. BMJ open 5(9).
- Ma H, Zhao J, Yu B, Ye B (2014) A gross anatomic study of distal tibia and fibula for single-incision approach. J Orthop Surg Res 9(1): 1.
- Lau T, Leung F, Chan C, Chow S (2008) Wound complication of minimally invasive plate osteosynthesis in distal tibia fractures. International orthopaedics 32(5): 697.
- Digby JM, Holloway GM, Webb JK (1983) A study of function after tibial cast bracing. Injury 14(5): 432-439.
- Richard RD, Kubiak E, Horwitz DS (2014) Techniques for the surgical treatment of distal tibia fractures. Orthop Clin North Am 45(3): 295-312.
- Duan X, Al Qwbani M, Zeng Y, Zhang W, Xiang Z (2012) Intramedullary nailing for tibial shaft fractures in adults. Cochrane Database Syst Rev 1.
- Kuo LT, Chi CC, Chuang CH (2015) Surgical interventions for treating distal tibial metaphyseal fractures in adults. Cochrane Database Syst Rev 3.
- Mauffrey C, McGuinness K, Parsons N, Achten J, Costa M (2012) A randomised pilot trial of “locking plate” fixation versus intramedullary nailing for extra-articular fractures of the distal tibia. J Bone Joint Surg Br 94(5): 704-708.
- Guo J, Tang N, Yang H, Tang T (2010) A prospective, randomised trial comparing closed intramedullary nailing with percutaneous plating in the treatment of distal metaphyseal fractures of the tibia. J Bone Joint Surg Br 92(7): 984-988.
- Rijal L, Sagar G, Mani K, Joshi KN, Joshi A (2013) Minimizing radiation and incision in minimally invasive percutaneous plate osteosynthesis (MIPPO) of distal tibial fractures. Eur J Orthop Surg Traumatol 23(3): 361-365.
- Li Y, Jiang X, Guo Q, Zhu L, Ye T, et al. (2014) Treatment of distal tibial shaft fractures by three different surgical methods: a randomized, prospective study. Int Orthop 38(6): 1261-1267.
- Paluvadi SV, Lal H, Mittal D, Vidyarthi K (2014) Management of fractures of the distal third tibia by minimally invasive plate osteosynthesis-A prospective series of 50 patients. J Clin Orthop Trauma 5(3): 129-136.
- Teeny SM, Wiss DA (1993) Open reduction and internal fixation of tibial plafond fractures. Variables contributing to poor results and complications. Clin Orthop Relat Res 292: 108-117.
- Solomon L, Warwick D, Nayagam S (2010) Apley's system of orthopaedics and fractures. CRC press, United States.
- Yang SW, Tzeng HM, Chou YJ, Teng HP, Liu HH, et al. (2006) Treatment of distal tibial metaphyseal fractures: plating versus shortened intramedullary nailing. Injury 37(6): 531-535.
- Cheng W, Li Y, Manyi W (2011) Comparison study of two surgical options for distal tibia fracture-minimally invasive plate osteosynthesis vs. open reduction and internal fixation. Int Orthop 35(5): 737-742.
- Farouk O, Krettek C, Miclau T, Schandelmaier P, Guy P (1999) Minimally invasive plate osteosynthesis: does percutaneous plating disrupt femoral blood supply less than the traditional technique? J Orthop Trauma 13(6): 401-406.
- Ronga M, Longo UG, Maffulli N (2010) Minimally invasive locked plating of distal tibia fractures is safe and effective. Clin Orthop Relat Res 468(4): 975-982.
- Mahajan N (2008) Minimally invasive techniques in distal tibial fractures. JK science 10(2): 78-80.
- Janssen KW, Biert J, van Kampen A (2007) Treatment of distal tibial fractures: plate versus nail: a retrospective outcome analysis of matched pairs of patients. Int Orthop 31(5): 709-714.
- Joveniaux P, Ohl X, Harisboure A, Berrichi A, Labatut L, et al. (2010) Distal tibia fractures: management and complications of 101 cases. International orthopaedics 34(4): 583-588.
- Koval KJ, Clapper MF, Brumback RJ, Ellison JP, Poka A, et al. (1991) Complications of reamed intramedullary nailing of the tibia. J Orthop Trauma 5(2): 184-189.
- Borg T, Larsson S, Lindsjö U (2004) Percutaneous plating of distal tibial fractures: preliminary results in 21 patients. Injury 35(6): 608-614.
- Zou J, Zhang W, Zhang CQ (2013) Comparison of minimally invasive percutaneous plate osteosynthesis with open reduction and internal fixation for treatment of extra-articular distal tibia fractures. Injury 44(8): 1102-1106.
- Im GI, Tae SK (2005) Distal metaphyseal fractures of tibia: a prospective randomized trial of closed reduction and intramedullary nail versus open reduction and plate and screws fixation. J Trauma 59(5): 1219-1223.
- Lee YS, Chen SH, Lin JC, Chen YO, Huang CR, (2009) Surgical treatment of distal tibia fractures: a comparison of medial and lateral plating. Orthopedics 32(3).
- Jensen JS, Hansen FW, Johansen J (1977) Tibial shaft fractures: a comparison of conservative treatment and internal fixation with conventional plates or AO compression plates. Acta Orthop Scand 48(2): 204-212.
- Hasenboehler E, Rikli D, Babst R (2007) Locking compression plate with minimally invasive plate osteosynthesis in diaphyseal and distal tibial fracture: a retrospective study of 32 patients. Injury 38(3): 365-370.
- Horn C, Döbele S, Vester H, Schäffler A, Lucke M, et al. (2011) Combination of interfragmentary screws and locking plates in distal meta-diaphyseal fractures of the tibia: a retrospective, single-centre pilot study. Injury 42(10): 1031-1037.
- Li Q, Zeng B, Luo C, Song S, Zhang C, et al. (2014) Limited open reduction is better for simple-distal tibial shaft fractures than minimally invasive plate osteosynthesis. Genet Mol Res 13(3): 5361-5368.
- Shen J, Xu J, Tang MJ, Luo Cf, Zhang CQ (2016) Extra-articular distal tibia facture (AO-43A): A retrospective study comparing modified MIPPO with IMN. Injury 47(10): 2352-2359.
- Hazarika S, Chakravarthy J, Cooper J (2010) Minimally invasive locking plate osteosynthesis for fractures of the distal tibia-results in 20 patients. Injury 37(9): 877-887.
- Bonnevialle P, Lafosse JM, Pidhorz L, Poichotte A, Asencio G, et al. (2010) Distal leg fractures: How critical is the fibular fracture and its fixation? Orthop Traumatol Surg Res 96(6): 667-673.
- Gupta RK, Rohilla RK, Sangwan K, Singh V, Walia S (2010) Locking plate fixation in distal metaphyseal tibial fractures: series of 79 patients. Int Orthop 34(8): 1285-1290.






























