The Application of Mechanical Diagnosis and Therapy in Failed Anterior Cervical Discectomy and Fusion: a Case Report
Lindsay Carlton*, Joseph R Maccio, Jaime Handford and Pinal Patel
Maccio Physical Therapy, USA
Submission: December 07, 2017; Published: December 19, 2017
*Corresponding author: Lindsay Carlton, Maccio Physical Therapy, 1 New Hampshire Ave, Troy, NY, 12180, USA, Email: lindsaycarltonl5@gmail.com
How to cite this article: Lindsay C, Joseph R M, Jaime H, Pinal P. The Application of Mechanical Diagnosis and Therapy in Failed Anterior Cervical Discectomy and Fusion: a Case Report. Ortho &338; Rheum Open Access 2017;9(4): 555766. DOI: 10.19080/OROAJ.2017.09.555766.
Abstract
The prevalence of neck pain is estimated to be 30-50 % in the general population, the second leading source of reported pain in the United States. There is limited research on the use of mechanical diagnosis and therapy (MDT) on patients with cervical pain. The effects and safety of MDT assessment and treatment for failed anterior cervical discectomy and fusion (ACDF) has yet to be established. This case report presents a 42-year-old female with a complaint of worsening neck pain with intermittent radiculopathy after an ACDF to address cervical radiculopathy. The patient received a MDT evaluation and was classified as a thoracic spine derangement. The patient was treated based on mechanical and symptomatic responses to repeated movements and mobilizations using principles of MDT. Short- and long-term outcomes were excellent, demonstrating rapid abolishment of symptoms and improvement of function in 6 visits over 4 weeks. The patient reported no pain or functional disability and had returned to all work and recreational activities. The patient demonstrated the ability to prevent and manage recurrence of symptoms independently at one-year follow-up. This case report confirms the efficacy and safety of MDT evaluation after a failed ACDF. The patient was successfully managed using MDT with full resolution of symptoms. This case report provides preliminary evidence that MDT may provide effective short- and long-term outcomes after failed ACDF. Less invasive, conservative methods, such as MDT, may be more effective at resolving cervical radiculopathy. Level of evidence 4.
Keywords: Anterior Cervical Discectomy and Fusion (ACDF); Cervical Fusion Surgery; Mechanical Diagnosis and Therapy; Derangement; Thoracic; Stenosis; Magnetic Resonance Imaging (MRI)
Abbreviations: ACDF: Anterior Cervical Discectomy and Fusion; MRI: Magnetic Resonance Imaging; MDT: Mechanical Diagnosis and Therapy; NPRS: Numeric Pain Rating Scale; NDI: Neck Disability Index
Introduction
The estimated prevalence of cervical spine pain in the general population is reported between 30% and 50% [1]. Anterior cervical discectomy and fusion (ACDF) is a commonly utilized surgical procedure for radicular neck pain. One study reported the average cost was 16,162 US dollars and calculated a quality-adjusted life years cost of 43,681 US dollars at 2 years, based on neck disability index scores [2]. Regardless of expense, as with any other invasive surgical intervention, the ACDF procedure has serious health risks including, but not limited to, dysphagia, hematoma, laryngeal nerve palsy, dural penetration, and death [3-5].
In 1,211 asymptomatic subjects, 87.6% had significant disc bulging on magnetic resonance imaging (MRI) [6], implying that MRI is not an accurate tool. Physical examination procedures for cervical radiculopathy have demonstrated poor reliability [7] . The faults in diagnostic tests attempting to identify tissue specific pathology, have led to the creation and use of nonspecific classification based assessment and treatment systems [8] . An assessment following the Mechanical Diagnosis and Therapy (MDT) methodology has proven to be a more accurate, less invasive, and more cost-effective means of identifying spinal lesions [9].
MDT has shown acceptable reliability among well trained MDT clinicians [10-13]. By Bee et al. [14] found MDT-trained physical therapist students to be as reliable as experienced clinicians trained in MDT for diagnosis and treatment of patients with neck pain. MDT evaluation has shown that 92% of 297 consecutive patients with neck pain were classified into the MDT syndrome derangement, indicating it is an applicable assessment system for the majority of patients with cervical spine pain [14].
MDT assessment and treatment has demonstrated the ability to abolish symptoms associated with cervical radiculopathy, even in the presence of positive MRI findings [15]. Spanos et al. [15] showed repeated movements used by the clinician not only resolved the patient’s symptoms, but altered the size of disc herniation on MRI by more than 50%. Recent case reports [16-18] have confirmed that end-range loading strategies based on MDT principles, including extension which is known to physiologically narrow the spinal canal, are safe for patients with an MRI confirmed radiculopathy. MDT has been shown to rapidly abolish pain and restore motor function, leading to improved recovery times [16-18]. Following this line of reasoning, it seems logical that MDT-based evaluation and treatment could be of benefit for patients with a diagnosis of cervical radiculopathy before more invasive intervention measures, such as an ACDF, are considered.
There has been no publication reporting the MDT management for continuing, or worsening, cervical radiculopathy following ACDF. Current literature disputing the reliability of special tests [19-22] and utility of diagnostic tests [15] warrants consideration for other diagnostic and prognostic treatments, such as MDT The aim of this case report was to demonstrate a MDT evaluation, classification, and management of a patient with worsening cervical radiculopathy following ACDF.
Methods
Two examiners were used for data collection, evaluation, and treatment. The lead examiner, a third-year doctoral student of physical therapy, had taken the introductory lumbar (Part A) MDT course. The student was trained by the co-examiner (JRM), who holds a doctorate in physical therapy and Diploma in MDT, for 6 weeks as part of an 8-week clinical affiliation during data collection. All patient management was overseen by the co-examiner. The patient was recruited through the normal business operations of a private Certified McKenzie spine and extremity outpatient clinic.
The patient was evaluated using a mechanical assessment based on the principles of MDT [23]. This involved the use of repetitive movements and mobilizations while monitoring symptomatic (e.g., pain) and mechanical responses (e.g., strength, range of motion, and functional improvement) to classify the patient's musculoskeletal disorder into the following syndromes: derangement, dysfunction, posture, and other. Derangement is defined as an internal dislocation of articular tissue of unknown origin which causes a disturbance in the normal resting position of the affected joint surface, resulting in pain and restriction to movement. Treatment of derangement involves repeated or sustained movement in one direction, known as directional preference [23]. Centralization, a hallmark of spinal derangement, is characterized by the abolishment of referred spinal pain in a distal to proximal manner and can also be associated with mechanical improvement (e.g., range of motion, strength, etc.). When symptoms are fully resolved and mobility is completely restored, for several consecutive days, recovery of function is begun to ensure full reduction of the derangement. To do so, the patient is asked to move in the opposite direction of the reductive exercise while monitoring for reproduction of symptoms or loss of mobility. Should this occur, the patient is considered not to be fully reduced and is returned to the reductive exercise only.
Dysfunction syndrome is defined as mechanical deformation of structurally impaired soft tissue which results in pain and limited range of motion. Treatment of dysfunction involves progressive tissue loading to remodel the articular tissue. Postural syndrome is defined as mechanical deformation of normal soft tissues or vascular insufficiency arising from prolonged positional stresses resulting in pain. The primary intervention for postural syndrome is patient education and avoidance of the offensive position. The classification of other refers to neck pain of non-mechanical origin. Examples of conditions classified as other include, but are not limited to, cancer, upper motor neuron lesion, fracture, vascular pathology, chronic pain syndrome, trauma, soft tissue pathology, post- surgical, and inflammatory conditions [23].
Cervical and thoracic spinal range of motion was established before beginning repeated movement testing. A categorical range of motion scale advocated by McKenzie & May [23] was implemented, where nil, minimal, moderate, and major are used to designate relative range of motion loss. Outcome measures were collected at the initial evaluation and discharge, with follow-up phone interviews conducted 3 weeks and 1 year after discharge. The primary outcome measures were the Numeric Pain Rating Scale (NPRS), where 0 indicates "No pain" and 10 indicates "The worst pain imaginable" [24], and the Neck Disability Index (NDI) which is a validated functional measure [25]. The NDI measures functional disability from 0-100, where 0 indicates no functional limitation and 100 indicates complete functional disability.
Case Description and Outcomes
Prior to attending our clinic, the patient initially reported left-sided neck pain with radicular symptoms in both arms and hands for one year with no mechanism of injury. The patient attended traditional physical therapy where the treatment consisted of stretching and strengthening activities, traction, and ultrasound. This form of conservative treatment was unsuccessful and the patient was referred to a neurosurgeon who performed an ACDF at C5-C6 and C6-C7 with interval discectomy at these levels. After the surgical intervention, the patient no longer had bilateral radicular symptoms but her left-sided neck pain continued to worsen. The patient saw a chiropractor three times a week for approximately one month. The treatment primarily consisted of rib manipulation and taping for postural education. The patient found the tape helpful in maintaining good posture, but the treatment overall provided no pain relief. She consulted a Certified McKenzie Spine and Extremity Clinic for a mechanical evaluation and second opinion of her cervical condition.
Patient Characteristics
A 42 year-old female presented 4 months after ACDF with the primary complaint of constant, worsening neck and scapular pain, and intermittent anterior chest pain as far as the sternum, the latter which began after the procedure without a mechanism of injury. This newer symptom was not of cardiovascular origin,as confirmed by radiograph, electrocardiogram, blood work, and stress. A MRI of her neck after ACDF indicated resolution of the foraminal stenosis found prior to surgical intervention; however, symptoms were still present and had worsened. Her average pain score was 8/10 on the NPRS and her NDI score was 54, indicating severe disability [25].
Her typical work day required extended periods of sitting which had become increasingly difficult as her neck, scapular and chest pain worsened. The patient was no longer able to perform recreational exercise due to the pain and complained of difficulty driving. She consistently had trouble sleeping at night due to constant pain, which led to adverse effects on her day-to- day functioning and social life. On the intake form, in reference to the question, "How does this condition affect your livelihood?", she responded with, 'At my wits end, so stressed and depressed over it".
Examination and Classification
Visit 1
At the time of evaluation, the patient only reported leftsided neck and scapular pain. Assessment revealed major loss of bilateral lateral flexion, moderate loss of bilateral rotation, and minimal loss of flexion, retraction, and extension. Cervical rotation was used as a baseline reference throughout treatment due to the significant loss and importance of the movement while driving. Upon repeated movement testing, the patient performed 10 repetitions of cervical flexion in sitting which increased her symptoms during the movement, but did not remain worse after testing [23]. Following MDT principles, an increase of symptoms during testing with no lasting effect afterward suggests testing of another movement. Ten repetitions of cervical retraction extension in sitting also increased symptoms during the movement, but did not remain worse after.
When there is no favorable response in the sagittal plane, MDT principles advocate for assessment in the frontal or transverse planes [23]. Being that the thoracic spine can refer pain to the anterior chest wall [23], thoracic extension was tested to further exhaust the sagittal plane prior to assessing lateral cervical movements. Ten repetitions of thoracic extension in sitting with overpressure from a chair back (Figure 1) deceased symptoms from 8/10 to 3/10 on the NPRS and when cervical motion was re-examined she displayed a positive mechanical change in cervical rotation. Due to rapid symptomatic and mechanical response to thoracic extension, the patient was classified as a thoracic spine derangement with a directional preference of thoracic extension. The patient was prescribed 10 repetitions of thoracic extension in sitting with overpressure from a chair back every 1-2 hours for 48 hours.
Re-evaluation and Outcome
Visit 2
The patient was re-evaluated in 48 hours. She reported good compliance with the home exercise program at work, but reported poor compliance when at home. Despite the lack of compliance, she reported a 50% perceived improvement in her condition. She described less discomfort driving and improved quality of sleep. The patient displayed only minimal loss of cervical rotation and less pain with cervical flexion. Repeated thoracic extension in sitting with overpressure from a chair back (Figure 1) decreased her NPRS from 2/10 to 1/10. This confirmed thoracic derangement with directional preference for thoracic extension. She was instructed to continue her previously prescribed directional preference until next reassessment.

Visit 3
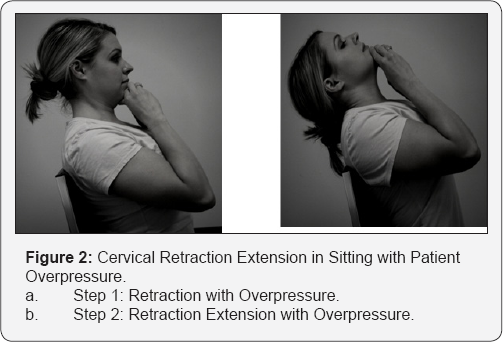
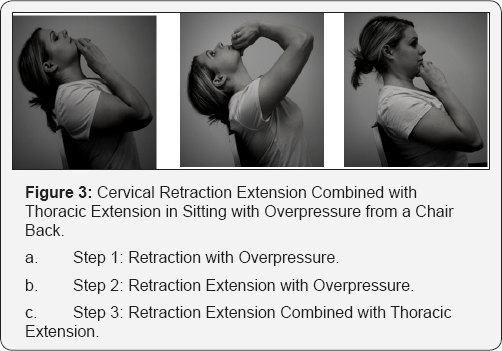
The patient was seen 9 days later after she returned from vacation. She reported inability to adhere to her home exercise program while traveling, but was compliant upon returning home. The patient described her pain as 6/10 on the NPRS which was localized to her left scapula. The scapular region is a common referral location for the cervical spine so cervical motions were re-examined [23,26]. There was no longer any limitation in cervical motion, but some discomfort with cervical retraction and extension still remained. The patient performed 10 repetitions of cervical retraction extension, and with patient overpressure (Figure 2), both had no effect on her pain. To further progress the patient's directional preference for extension, 10 repetitions of cervical retraction extension combined with thoracic extension (Figure 3) was tested which increased pain during movement, but it was no worse afterward. This response warrants the progression of forces further into the same direction [23]. The therapist performed a posterior to anterior mobilization at the cervical thoracic junction to further increase extension mobility [27].
After the mobilization was performed, the patient was able to perform 10 repetitions of cervical retraction extension combined with thoracic extension in sitting with overpressure from a chair back (Figure 3) without discomfort and reported her pain decreased to 3/10 on the NPRS. The significant reduction [24] in symptoms confirmed derangement at the cervicothoracic junction. The patient's home exercise program and directional preference was altered, 10 repetitions of cervical retraction and extension combined with thoracic extension in sitting (Figure 3) every 1-2 hours.
Visit 4
The patient was seen 3 days later. She reported 85% perceived improvement in her condition. She rarely experienced scapular pain, therefore, decided to return to the gym and did so without provocation of pain or loss of motion. There was no change made to her home exercise program.
Visit 5
The patient was seen 4 days later. The patient reported she no longer experienced pain. She had no difficulty sitting at work and continued to work out at the gym without incident. Recovery of function was tested without provocation of symptoms or loss of motion and functional strengthening activities were performed without any complications. The patient was instructed to continue recovery of function via 10 repetitions of cervical flexion followed by 10 repetitions of cervical retraction extension combined with thoracic extension as her home exercise program.
Visit 6
The patient was seen 4 days later. The patient reported the recovery of function exercises had not reproduced her neck or scapular pain and she was completely symptom-free. The patient’s score on the NDI was now 0/100 and 0/10 on the NPRS. The patient's cervical and thoracic range of motion was within normal limits. She reported no difficulty performing a full day’s work, continued to go to the gym, and had resumed a more fulfilling social life.
Follow-up
Three weeks after discharge, the patient reported that she had a minor re-occurrence of pain when she was unable to perform her corrective exercises for 3 days, but upon resuming performance she was able to independently abolish her pain. One year after discharge she reported continued successful selfmanagement. She reported occasionally stopping her exercises which would ultimately lead to "slight stiffness" which would immediately abolish once she began performance of corrective self-mobilizations. She stated she has not sought any further medical treatment for her spine or upper extremity since receiving MDT treatment. She continues to perform her exercises at least two times per day to prevent stiffness from returning.
Discussion
To our knowledge, this is the first paper that has studied the use of MDT on a patient with worsening pain after a failed ACDF, and showed self-maintenance of long-term results. This case study presents a woman who originally was diagnosed with cervical radiculopathy and managed surgically using an ACDF procedure. Post-surgically, she continued to have worsening cervical and scapular pain with limited cervical range of motion, and new onset of anterior chest pain. She was treated for 6 visits over a period of 4weeks using MDT with full resolution of symptoms and return to full physical and reactional activities. The patient was managed solely using MDT assessment and treatment, which relies on the recognition of pain referral patterns and clinical reasoning, and allowed the patient to fully reduce and maintain the reduction of her thoracic derangement.
The treatment period may have been shorter had the patient not been on vacation, which did not allow prompt re-assessment between visit 2 and 3, when her clinical presentation changed and her loading strategy was no longer effective. She required therapist mobilizations at the cervicothoracic junction, as well as repeated movements at the cervicothoracic junction to decrease, and eventually abolish, symptoms. This is a technique the co- treating Diplomate (JRM) has used through clinical experience when he suspects the derangement lies within/near the levels surrounding the cervicothoracic junction. The theory is that this maneuver encourages fluid, sequential, segmental movement, effectively achieving end-range motion at all cervicothoracic spinal segments. There is no literature supporting superior effects utilizing this technique; however, the patient is this case report did have significant (≥ 2-point change on the NPRS [24]) decrease in pain following this procedure, indicating it was appropriate and safe for treatment.
The patient's unresponsiveness to a generalized physical therapy treatment protocol should be noted since this led to a consult with a neurosurgeon, and ultimately resulted in surgical intervention with worsening of symptoms afterward. When generalized physical therapy treatment is compared to MDT management of neck pain, MDT has been shown to have greater improvement in pain intensity scores, NDI scores, Distress and Risk Assessment Method scores, and a tendency toward fewer visits for additional healthcare [28]. This confirms the importance of a patient receiving a MDT assessment and treatment prior to engaging in discussion of surgical interventions. Not only is MDT a reliable assessment tool to determine a patient's need for invasive measures [29], it is a far safer, and more cost effective, road to recovery of function for the patient.
There are two possible explanations for the lack of full resolution of pain after the patient’s ACDF procedure. One scenario is that due to the fusion of two levels ofthe cervical spine, adjacent segment disease occurred. In a recent biomechanical study performed on cadavers, the researchers found that when an in situ fusion across segments C4-C6 was performed a cervical sagittal imbalance occurred due to malalignment and this helped exacerbate the adjacent segment mechanics as well as increased intra-discal pressure below the fusion [30]. Cervical fusions were associated with an increased incidence of radiographically confirmed adjacent level disc disease and a greater number of medical treatments related to episodic neck, shoulder, and arm pain [31]. Maintaining motion, rather than performing a fusion, is the best option to prevent further cervical spine deterioration [31].
The other explanation could be that foraminal stenosis, confirmed by MRI at the levels that were fused, is not the pain generator.6 Follow-up MRI performed, due to this patient's continuingly worsening chest pain, revealed the previous stenosis had been resolved after the ACDF procedure. Had this anatomical abnormality been the true source of the patient’s symptoms, the pain would have abolished after the surgical intervention, not worsened. The treating therapist, not only used repeated movements in the thoracic spine to target the symptoms, but also needed to mobilize the thoracic spine and cervicothoracic junction to fully abolish the patient's symptoms. MDT allows for the treatment to adapt as patient presentation changes. MDT also follows referral patterns and symptomatic and mechanical responses to repeated movements to confirm findings in a safe and more reliable manner [10-13,32-34]. Without an initial MDT evaluation prior to surgery, it is difficult to say if the appropriate level received the surgical intervention with only MRI results dictating treatment. Regardless, symptoms were worse afterward, strongly suggesting that this procedure was not necessary or appropriate.
Conclusion
This case report demonstrates that MDT can be an effective and safe assessment and treatment method after a failed ACDF procedure, showing maintenance of long-term results. The patient presented with worsening cervical and radicular pain after a failed ACDF. Her symptoms were successfully treated and resolved using MDT principles with positive long-term management success one year later. Further research is required to study larger sample sizes to establish better generalizability. MDT assessment prior to an ACDF procedure may be a more effective treatment approach for cervical radiculopathy, allowing for better individualized, proper treatment. Less invasive methods such as MDT, as demonstrated by this case report, are safer and more cost-effective and may even be more effective at resolving cervical radiculopathy.
Conflict of Interest
All named authors have none to disclose.
References
- Hogg Johnson S, van der Velde G, Carroll LJ, Holmd LW, Cassidy JD, et al. (2008) The burden and determinants of neck pain in the general population: results of the Bone and Joint Decade 2000-2010 Task Force on Neck Pain and Its Associated Disorders. Spine 33(4): S39-S51.
- Warren D, Andres T, Hoelscher C, Ricart-Hoffiz P, Bendo J, et al. (2013) Cost-utility analysis modeling at 2-year follow-up for cervical disc arthroplasty versus anterior cervical discectomy and fusion: a singlecenter contribution to the randomized controlled trial. Int J spine Surg 7(1): e58-e66.
- Fountas KN, Kapsalaki EZ, Nikolakakos LG, Smisson HF, Johnston KW, et al. (2007) Anterior cervical discectomy and fusion associated complications. Spine 32(21): 2310-2317.
- Apfelbaum RI, Kriskovich MD, Haller JR (2000) On the incidence, cause, and prevention of recurrent laryngeal nerve palsies during anterior cervical spine surgery. Spine 25(22): 2906-2912.
- Olsson EC, Jobson M, Lim MR (2015) Risk factors for persistent dysphagia after anterior cervical spine surgery. Orthopedics 38(4): e319-e323.
- Nakashima H, Yukawa Y, Suda K, Yamagata M, Ueta T, et al. (2015) Abnormal findings on magnetic resonance images of the cervical spines in 1,211 asymptomatic subjects. Spine 40(6): 392-398.
- Rubinstein SM, Pool JJM, van Tulder MW, Riphagen II, de Vet HCW (2007) A systematic review of the diagnostic accuracy of provocative tests of the neck for diagnosing cervical radiculopathy. Eur Spine J 16(3): 307-319.
- Cook C, Hegedus EJ, Ramey K (2005) Physical therapy exercise intervention based on classification using the patient response method: a systematic review of the literature. J Man Manip Ther 13(3):152-162.
- Donelson R, Aprill C, Medcalf R, Grant W (1997) A prospective study of centralization of lumbar and referred pain. A predictor of symptomatic discs and anular competence. Spine 22(10): 1115-1122.
- Dionne C, Bybee RF, Tomaka J (2007) Correspondence of diagnosis to initial treatment for neck pain. Physiotherapy 93(1): 62-68.
- Clare HA, Adams R, Maher CG (2005) Reliability of McKenzie Classification of Patients with Cervical or Lumbar Pain. J Man Manip Ther 28(2): 122-127.
- Clare HA, Adams R, Maher CG (2004) Reliability of the McKenzie spinal pain classification using patient assessment forms. Physiotherapy 90(3): 114-119.
- Dionne CP, Bybee RF, Tomaka J, Angelo S (2006) Inter-rater reliability of McKenzie assessment in patients with neck pain 92(2): 75-82.?
- Otero J, Bonnet F (2016) Neck pain: prevelance of McKenzie's syndrome and directional preference. Kinesither Rev 16(169): 2-10.
- Spanos G, Zounis M, Natsika M, May S (2013) The application of Mechanical Diagnosis and Therapy and changes on MRI findings in a patient with cervical radiculopathy. Man Ther 18(6): 606-610.
- Murphy DR, Beres JL (2008) Is treatment in extension contraindicated in the presence of cervical spinal cord compression without myelopathy? A case report. Man Ther 13(5): 468-472.
- Schenk R, Bhaidani T, Melissa B, Kelley J, Kruchowsky T (2008) Inclusion of Mechanical Diagnosis and Therapy (MDT) in the management of cervical radiculopathy: a case report. J Man Manip Ther 16(1): e1-e8.
- Takasaki H, Herbowy S (2016) Immediate improvement in the cranio- cervical flexion test associated with MDT-based interventions: a case report. J Man Manip Ther 24(5): 285-292.
- Abady AH, Rosedale R, Chesworth BM, Rotondi MA, Overend J (2018) Consistency of commonly used orthopedic special tests of the shoulder when used with the McKenzie system of mechanical diagnosis and therapy. Musculoskelet Sci Pract 33: 11-17.
- Maccio JR, Fink S, Yarznbowicz R, May S (2016) The application of mechanical diagnosis and therapy in lateral epicondylalgia. J Man Manip Ther 24(3): 158-165.
- Lynch G, May S (2013) Directional preference at the knee: a case report using mechanical diagnosis and therapy. J Man Manip Ther 21(1): 6066.
- Kidd J (2013) Treatment of shoulder pain utilizing mechanical diagnosis and therapy principles. J Man Manip Ther 21(3): 168-173.
- McKenzie R, May S (2006) The Cervical and Thoracic Spine: Mechanical Diagnosis and Therapy. (2nd edn), Spinal Publications, Waikanae, New Zealand.
- Stratford P, Spadoni G (2001) The reliability, consistency, and clinical application of a numeric pain rating scale. Physiother Canada 53(2): 88-91.
- Vernon H (2008) The Neck Disability Index: state-of-the-art, 19912008. J Manipulative Physiol Ther 31(7): 491-502.
- Cloward RB (1959) Cervical diskography: a contribution to the etiology and mechanism of neck, shoulder and arm pain. Ann Surg 150(6): 1052-1064.
- McKenzie RA (1990) The Cervical and Thoracic Spine: Mechanical Diagnosis and Therapy. (1st edn), Spinal Publications Limited, Waikanae, New Zealand.
- Kjellman G, Oberg B (2002) A randomized clinical trial comparing general exercise, McKenzie treatment and a control group in patients with neck pain. J Rehabil Med 34(4): 183-190.
- Rosedale R, Rastogi R, May S, Chesworth BM, Filice F, et al. (2014) Efficacy of exercise intervention as determined by the McKenzie system of mechanical diagnosis and therapy for knee osteoarthritis: a randomized controlled trial. J Orthop Sport Phys Ther 44(3): 173-181.
- Patwardhan AG, Khayatzadeh S, Nguyen N-L, Havey RM, Voronov LI, et al. (2016) Is cervical sagittal imbalance a risk factor for adjacent segment pathomechanics after multilevel fusion? Spine 41(10): E580-E588.
- Robertson JT, Papadopoulos SM, Traynelis VC (2005) Assessment of adjacent-segment disease in patients treated with cervical fusion or arthroplasty: a prospective 2-year study. J Neurosurg Spine 3(6): 417423.
- Bybee R, Dionne C (2007) Interrater agreement on assessment, diagnosis, and treatment for neck pain by trained physical therapist students. J Phys Ther Educ 21(2): 39-47.
- Elenburg JL, Foley BS, Roberts K, Bayliss AJ (2016) Utilization of mechanical diagnosis and therapy (MDT) for the treatment of lumbar pain in the presence of known lumbar transverse process fractures: a case study. J Man Manip Ther 24(2): 74-79.
- Peterson S, Hodges C (2015) Lumbar lateral shift in a patient with interspinous device implantation: a case report. J Man Manip Ther 24(4): 215-222.






























