Role of Botulinum Toxin A in Cerebral Palsy - 10yrs Experience
PA Mohammed Kunju1*, Riaz I1, Mary Iype1, Mini S2 and Kalpana D3
1Dept of pediatric neurology, Medical college, India
2Pediatric neurologist, KIMS, India
3Department of Pediatrics, Medical College, India
Submission: December 04, 2017; Published: December 18, 2017
*Corresponding author: PA Mohammed Kunju, Professor & Head, Dept of pediatric neurology, Medical college, Trivandrum 695 011, India, Email: drpamkunju@gmail.com
How to cite this article: PA Mohammed K, Riaz I, Mary I, Mini S, Kalpana D. Role of Botulinum Toxin A in Cerebral Palsy � 10yrs Experience. Ortho & Rheum Open Access 2017;9(3): 555765 DOI: 10.19080/OROAJ.2017.09.555765.
Abstract
Botulinum Toxin has been used for over 20 years to help people with problems like strabismus & blepharospasm [1]. Within the last 15 years, it is being successfully used to treat spasticity in children with cerebral palsy [2]. From 2000-2010 Botulinum toxin A (BT) was tried for spasticity (diplegic & hemiplegic) management in 60 children with cerebral palsy. 48 of them had severe spastic diplegia & 12 had hemiplegia. All were monitored for 6-24 months before BT injection. 48 had calf muscle spasticity with equinus, 40 had scissoring due to adductor spasm. 36 had flexion at knee due to hamstring spasm and 8 had spasm at different levels. Target muscles identified by functional spasticity assessment or by EMG guidance. The mean follow-up time was 36 months. Post injection, intensive physiotherapy was given.
Response parameters included changes in muscle tone, longitudinal gait parameters as well as parental assessments of improvement. The peak effect noticed by 1 to 2 weeks in the majority & lasted for 3 to 10 months. All children except 2 with fixed contractures experienced decreased spasticity scores, scissoring, equinus deformity and improved mobility. 13 non ambulatory children became ambulatory with assistance and five with assisted ambulation became more independently mobile. Remote effect like improvement in drooling & swallowing also noticed. None of the children had any untoward side effects. Post treatment physio and appliances helped in consolidating the results. An attempt is also made to discuss the basics of Botulinum Toxin treatment .
Introduction
Botulinum toxin A (BT) has been used therapeutically in patients for a variety of neurological conditions since 1980. Recently, it has been used successfully more frequently for management of spasticity and other movement abnormalities due to cerebral palsy (CP) [3-5]. However, the long-term results of BT have not yet been determined. In this article the use of BT in general is discussed in relation to our clinical experience.
Materials and Methods
To try botulinum toxin for spasticity (diplegic or hemiplegic) in 60 children with cerebral palsy (CP). Spastic CP was diagnosed by clinical criteria , initial spasticity status and response parameters including changes in muscle tone assessed by the modified Tardieu scale [6], range-of-motion (ROM) measurements , Clinical assessment of selective motor control (Boyd & Graham scale ) [7] at knee and ankle joint, objective analysis of longitudinal gait parameters as well as parental assessment of subjective improvement. Gait evaluation was done on videotape recordings.
Results and Discussion
Botulinum toxin was given for spasticity (diplegic or hemiplegic) in 60 children with cerebral palsy (CP).
48 of these children had severe spastic diplegia and 12 had hemiplegia. All children were undergoing a physiotherapy programme with monitoring of their baseline functional status for 6-24 months before BT injection. 24 of them were ambulatory and 36 were nonambulatory. 48 had an equinus posturing resulting from calf muscle spasticity, 40 had scissoring due to adductor spasm; 36 had flexed knee posture due to hamstring spasm and 8 had spasm at different levels. 2 of them were having very limited range of movement at ankle and knee. They were treated with varying doses of BT depending on the weight and number of muscles affected. The mean follow-up time was 36 months. Post injection, intensive physiotherapy; periodic evaluation and modification of splints and other appliances were done.
Response parameters included changes in muscle tone assessed by the modified Tardieu scale, range-of-motion (ROM) measurements , Clinical assessment of selective motor control (Boyd & Graham scale ) at knee and ankle joint, objective analysis of longitudinal gait parameters as well as parental assessment of subjective improvement. Gait evaluation was done on videotape recordings for 32 patients.
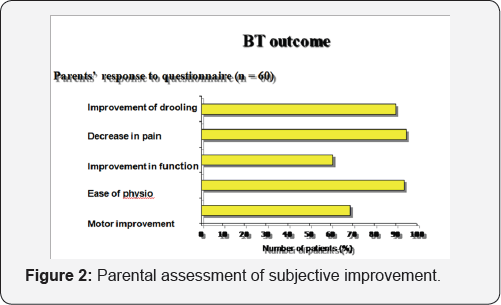
Most of these patients exhibited a progressive improvement in their gait pattern. The effect was evident within 72 hours. The peak effect was noticed by 1 to 2 weeks in the majority; the effect lasted for 3 to 10 months. In 45 of these patients a repeat injection was done during a varying period of 4-9 months. All children experienced decreased spasticity scores. More than 50% reduction has seen in all Figure 1. Their functional status improved, with 13 nonambulatory children becoming ambulatory with assistance and five children with assisted ambulation becoming more independently mobile. Measurement of joint motion showed improvement in the range of motion as compared with baseline. Video analysis of the functional state revealed comparative improvement. Ability to rise from the sitting position to standing also demonstrated improvement. One of the children had increase in weakness of dorsiflexion, 2 had fever for 2 days, and 7 had mild transient pain at the injection site. Parental assessment of subjective improvement and other parameters are given in Figure 2.

Review of Literature
In 1981, the ophthalmologist Alan Scott pioneered treatment with botulinum toxin when he used it to treat strabismus.
Mode of Action of BT
BT interferes with neural transmission by blocking the release of acetylcholine. After synaptic transmission is blocked by botulinum toxin, the muscles become clinically weak and atrophic. The affected nerve terminals do not degenerate, but the blockage of neurotransmitter release is irreversible. The sprouting of nerve terminals and formation of new synaptic contacts can recover function; this usually takes two to three months.
Steps of Action
BT blocks neuromuscular transmission through a three-step process that is followed by the sprouting of new axon terminals, which results in the reestablishment of neuromuscular transmission.
Blockade of Neuromuscular Transmission
i. Binding BT binds to the motor nerve terminal.
ii. Internalization - BT is internalized via receptor- mediated endocytosis, forming a toxin-containing vesicle inside the nerve terminal. After internalization, the light chain of the toxin molecule, released into the cytoplasm of the nerve terminal
iii. Blocking
BT blocks acetylcholine release. The affected terminals are inhibited from stimulating muscle contraction.
Reestablishment of Neuromuscular Transmission
Nerve Sprouting (Figure 3).

Rationale for Treatment with BT
BT induces weakness of striated muscles by inhibiting transmission of alpha motor neurons at the neuromuscular junction. This has led to its use in conditions with muscular over activity, such as dystonia and spasticity. Transmission is also inhibited at gamma neurones in muscle spindles, which may alter reflex over activity. The toxin also inhibits release of acetylcholine in all parasympathetic and cholinergic postganglionic sympathetic neurons [8]. This has fuelled interest in its use as a treatment for overactive smooth muscles -in achalasia or abnormal activity of glands - hyperhidrosis).
Practical aspects of BT injection
BT has to be injected into affected muscles or glands. Doses have to be tailored according to the mode of use and individual patients.
a. Total dose 4-6 U/kg body weight
b. No more than 50 U at any one site
c. Hemiplegia: recommended dose is 4 U/kg body weight in the affected limb
d. Diplegia: recommended dose is 6 U/kg body weight between the affected limbs

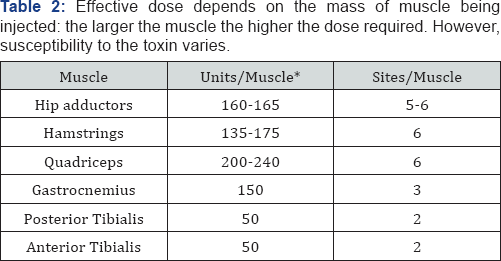
*2 ml dilution = 5 U/0.1 ml.
Overactive muscles are identified by muscular hypertrophy, stiffness, tenderness, and visible abnormal muscular activity. In addition, clinical observation ofabnormal movements or postures may help identify an overactive muscle. Electromyography can also be useful. The weakness induced by injection with BT usually lasts about three months. Patients will then need further injections at regular intervals, although the interval varies widely depending on the dose and individual susceptibility.
Side Effects
Injections with botulinum toxin are generally well tolerated. Development of resistance to BT therapy, characterized by absence of any beneficial effect and by lack of muscle atrophy following the injection, is an important clinical issue. The incidence of antibody-mediated resistance, as determined by the mouse lethality assay, is reported between 3% and 10%. Use of the smallest possible effective dose and longer treatment intervals may reduce the likelihood of antibody development. Other serotypes may benefit those who have developed antibody resistance [9,10].
Role in Spasticity
BT has been evaluated in various spastic disorders. It was shown to improve gait pattern in patients with cerebral palsy with progressive dynamic equinovarus or equinovalgus foot deformities. Treatment of children with cerebral palsy during the key early years when functional skills in walking are being developed improves the outcome and may help to avoid surgery for contracture and bony torsion. However, until very recently, all such use in this indication has been unapproved with no generally accepted treatment protocols, resulting in considerable uncertainty and variation in its use as a therapeutic agent. In view of the increasing awareness of, and interest in, this approach to the treatment of spasticity, and also the recent licensing in a number of countries of a BT preparation for treating equinus deformity in children, it would seem timely to establish a framework of guidelines for the safe and efficacious use of BT for treating spasticity in children. This must include detailed recommendations as to appropriate patient selection and assessment, dosage, injection technique and outcome measurement. The importance of adjunctive physiotherapy, orthoses and casting is also to be stressed [11-13].
A recent cochrane review has not revealed strong controlled evidence to support or refute the use of BA for the treatment of leg spasticity in cerebral palsy [14]. Ongoing randomized controlled trials are likely to provide useful data on the short term effects of BA for leg spasticity. Future research should also assess the longer term use of BA. Ideally studies should be pragmatic in their approach to dose and distribution of toxin to reflect practice. Outcome measures assessing function and disability would give the most useful information [15].
Conclusion
Our limited study demonstrated that BT is useful as an adjunctive therapy in ameliorating spasticity in children with cerebral palsy, along with intensive physiotherapy, timely splinting and usage of corrective appliances. None of them developed new contractures. No significant side effects were also seen. Further randomized controlled trials may help in answering some of confusing issues in BT usage.
References
- Munchau A, Bhatia KP (2000) Uses of botulinum toxin injection in medicine today BMJ 320(7228): 161-165.
- Graham HK, Aoki KR, Autti-Ramo I, Boyd RN, Delgado MR, et al. (2000) Recommendations for the use of botulinum toxin type A in the management of cerebral palsy. Gait Posture 11(1): 67-79.
- Ade-Hall RA, Moore AP (2000) Botulinum toxin type A in the treatment of lower limb spasticity in cerebral palsy. Cochrane Database Syst Rev 2: CD001408.
- DasGupta BR, Sugiyama H (1972) A common subunit structure in Clostridium botulinum type A, B and E toxins. Biochem Biophys Res Comm 48(1): 108-112.
- Coffield JA, Considine RV, Simpson LL (1994) The site and mechanism of action of botulinum neurotoxin. Marcel Dekker, New York, USA, p. 3-13.
- Haugh AB, Pandyan AD, Johnson GR (2006) A systematic review of the Tardieu Scale for the measurement of spasticity. Disabil Rehabil 28(15): 899-907.
- Boyd RN, Graham HK (1999) Objective measurement of clinical findings in the use of botulinum toxin type A for the management of children with cerebral palsy. Eur J Neurol 6(S4): S23-S35.
- Basciani M, Di Rienzo F, Fontana A, Copetti M, Pellegrini F, et al. (2011) Botulinum toxin type B for sialorrhoea in children with cerebral palsy: a randomized trial comparing three doses. Dev Med Child Neurol 53(6): 559-564.
- Hatheway CL, Dang C (1994) Immunogenicity of the neurotoxins of Clostridium botulinum. Therapy with Botulinum Toxin. Marcel Dekker, New York, USA, pp. 93-107.
- Goschel H, Wohlfarth K, Frevert J, Dengler R, Bigalke H (1997) Botulinum A toxin therapy: neutralizing and nonneutralizing antibodies-therapeutic consequences. Exp Neurol 147: 96-102.
- Koman LA, Mooney JF, Smith B, Goodman A, Mulvaney T (1993) Management of cerebral palsy with botulinum-A toxin: preliminary investigation. J Pediatr Orthop 13(4): 489-495.
- Koman LA, Mooney JF, Smith BP, Walker F, Leon JM (2000) Botulinum toxin type A neuromuscular blockade in the treatment of lower extremity spasticity in cerebral palsy: a randomized, double-blind, placebo-controlled trial. BOTOX Study Group. J Pediatr Orthop 20(1): 108-115.
- Molenaers G, Campenhout AV, Fagard K, Cat JD, Desloovere K (2010) The use of botulinum toxin A in children with cerebral palsy, with a focus on the lower limb J Child Orthop 4(3): 183-195.
- Hoare BJ, Wallen MA, Imms C, Villanueva E, Rawicki HB, et al. (2010) Botulinum toxin A as an adjunct to treatment in the management of the upper limb in children with spastic cerebral palsy (UPDATE). Cochrane Database Syst Rev 20(1): CD003469.
- Galli M, Crivellini M, Santambrogio GC, Fazzi E, Motta F (2001) Shortterm effects of 'botulinum toxin A' as treatment for children with cerebral palsy: kinematic and kinetic aspects at the ankle joint. Funct Neurol 16(4): 317-323.






























