Kienböck’s Disease: Diagnosis and the Different Ways of Management
Elalfy M Mohamed1* and Nour A Khaled2
1Orthopaedic surgery resident at Mansoura University Hospital, Faculty of medicine, Egypt
2Orthopedic surgery lecturer at Mansoura University Hospital, Faculty of medicine, Egypt
Submission: October 27, 2017; Published: November 13, 2017
*Corresponding author: Mohamed Mohsen El Alfy, Faculty of Medicine, Orthopaedic surgery resident at Mansoura University Hospitals, Egypt, Email: elalfy2299@gmail.com
Nour A Khaled, Faculty of medicine, Orthopedic surgery lecturer at Mansoura University Hospital, Egypt.
How to cite this article: Elalfy M M, Nour A K. Kienböck's Disease: Diagnosis and the Different Ways of Management. Ortho & Rheum Open Access 2017;9(1): 555755. DOI: 10.19080/OROAJ.2017.09.555755.
Abbreviations
Abbreviations: MRI: Magnetic Resonance Imaging; STT: Scapho Trapezio Trapezoid; SC: Scapho Capitate (SC); PRC: Proximal Row Carpectomy; CH: Capito Hamate
Background
Kienböck's disease is a condition of uncertain etiology that results in osteonecrosis of the carpal lunate. It usually affects the dominant wrist of men aged 20-40 years [1,2] (Figure 1).
Etiology
The etiology of Kienbock’s disease is not clear. Most likely, it occurs as a result of repeated loads to a "lunate at risk" by virtue of its unique vascular or mechanical environment. Although the underlying etiology of this condition is not known, the final results of fragmentation and collapse are secondary to osteonecrosis.
Pathophysiology
Thought to be caused by multiple factors:
i. Biomechanical factors,
ii. Ulnar negative variance (leads to increased radial- lunate contact stress)[3],
iii. Decreased radial inclination,
iv. Repetitive trauma [4],
v. Anatomic factors,
vi. Geometry of lunate,
vii. Vascular supply to lunate (patterns of arterial blood supply have differential incidences of AVN or disruption of venous outflow leading to increased intraosseous pressure) [5,6].
Pathology
The pathologic changes are equivalent to those of avascular necrosis of other bones. There is disruption of critical blood supply leading to bone infarction, central necrosis and surrounding hyperaemia. Microfractures ensue resulting in flattening and deformity of the bone surface. In 70% of lunates there is vascular supply multiple vessels either volarly or dorsally. In the remaining 30% only a single vessel is present volarly and dorsally, which may explain some of the vulnerability of the lunate to avascular necrosis.
Clinical Manifestations
a. Wrist pain that radiates up the forearm and stiffness, tenderness, and swelling over lunate.
b. Passive dorsiflexion of middle finger produces characteristic pain.
c. Limitation of wrist motion, usually dorsiflexion.
d. Weakness of grip.
e. Pain and weakness increase as the lunate collapses and degenerative changes develop, making the disability both severe and chronic [2].
Radiological Findings
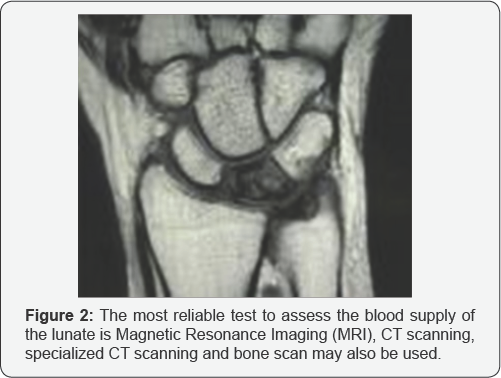
In early stages of this disease, the x-rays may be normal and other tests are needed to confirm the diagnosis. Most likely, the most reliable test to assess the blood supply of the lunate is Magnetic Resonance Imaging (MRI), CT scanning, specialized CT scanning and bone scan may also be used (Figure 2). The Stahl classification of Kienböck's disease, modified by Lichtman, is the most commonly used staging system and is useful in the treatment of Kienböck's disease (avascular necrosis of the lunate) [7]. This system divides the disease into four stages (Figures 3-6):
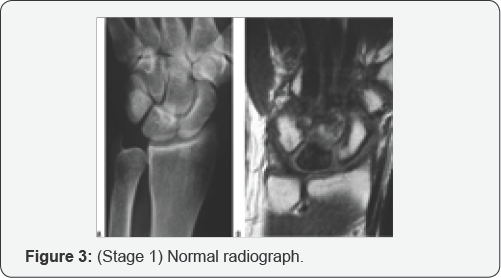
i. Stage I: normal radiograph.
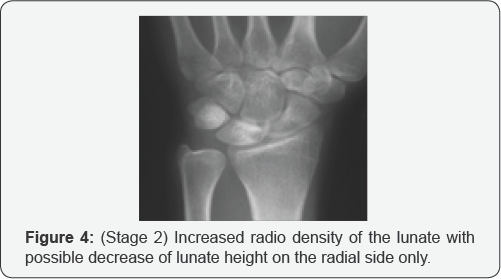
ii. Stage II: increased radiodensity of the lunate with possible decrease of lunate height on the radial side only.
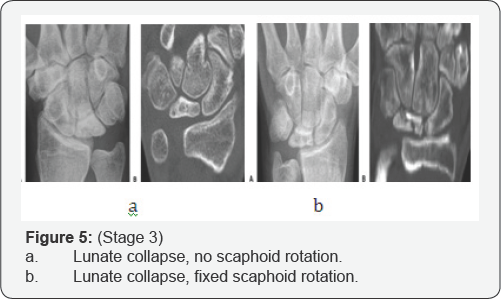
iii. Stage III:
a. Lunate collapse, no scaphoid rotation.
b. Lunate collapse, fixed scaphoid rotation.
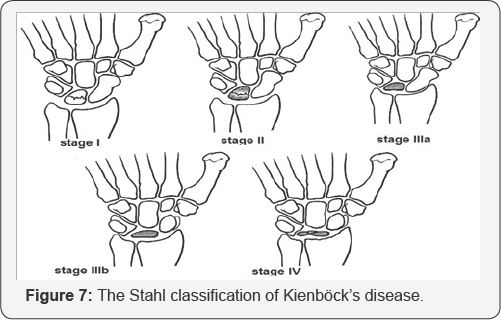
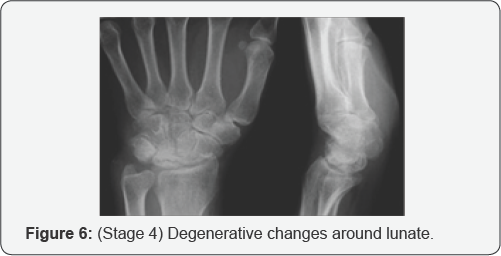
iv. Stage IV: degenerative changes around lunate (Figure 7).
Arthroscopic Classification [8,9]
Bain and Begg first described their arthroscopic classification in 2006 .This is based on the number of nonfunctional articular surfaces.
a. Grade 0: All articular surfaces are functional.
b. Grade 1: One nonfunctional articular surface, usually the proximal articular surface of the lunate.
c. Grade 2: Two nonfunctional articular surfaces. Divided into types A and B.
Grade 2A: The proximal lunate and the lunate facet of the radius.
Grade 2B: Proximal articular surface of the lunate, and distal articular surface of the lunate.
d. Grade 3: Three nonfunctional articular surfaces (the lunate facet of the radius, proximal and distal articular surfaces of the lunate), with a preserved head of capitate.
e. Grade 4: All four articular surfaces are nonfunctional (Figure 8).
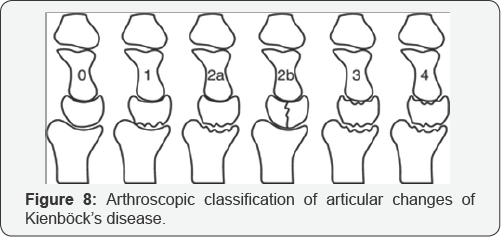
The authors have noted the following observations:
a. The degree of synovitis correlates with the degree of articular damage.
b. The severity of articular changes is underestimated by plain radiographs.
c. Findings at arthroscopy commonly change the initial treatment plan.
d. In certain cases the articular cartilage envelope remains intact with collapse of the subchondral bone plate. This is an important subgroup where the lunate has probably revascularized. In these patients, particularly if they are young, conservative treatment may be considered, as there is potential to heal and stabilize [9].
Management
Nonoperative
Observation, immobilization and NSAIDS.
Certainly, a very young patient, though an unusual presentation of Kienbock disease, should be given an adequate trial of immobilization in hopes of allowing revascularization of the lunate and preventing disease progression. Usually it acts as initial management for Stage I disease.
Operative
A number of options are available for surgical management of Kienbock disease. The two most important pieces of information are the stage of the disease and the presence or absence of ulnar variance.
Operative management can be classified into:
a. Lunate excision with or without replacement.
b. Joint-leveling procedures.
c. Intercarpal fusions.
d. Revascularization.
e. Salvage procedures.
f. Others:
Cancellous bone grafting plus external fixation, Arthroscopic debridement, Wrist denervation, Metaphyseal decompression and Lunate core decompression [10].
Lunate excision with or without replacement
Simple lunate excision, Excision with soft-tissue (fascial or palmarislongus tendon graft) replacement and Silicone replacement arthroplasty [11].
Joint-leveling procedures
Radial shortening and ulnar lengthening are the two options for leveling the joint. The goal is to produce a wrist with neutral ulnar variance. Strains at the lunate can be reduced by 70% with an appropriate radial shortening or ulnar lengthening. Currently, radial shortening with a volar distal radius locking plate is preferred to ulnar lengthening because there is a lower complication rate with the volar-shortening procedure and because the two procedures have shown similarly good outcomes. In patients with neutral or positive ulnar variance, shortening the radius is contraindicated. In this clinical situation, radial wedge osteotomies designed to decrease the radial inclination have been proposed [12,13].
Intercarpal Fusions
The goal is to reduce lunate strain and to correct and maintain proper scaphoid position in procedures that involve the scaphoid. Of the limited intercarpal fusions reported, the greatest experience has been with scapho trapezio trapezoid (STT) fusion. STT arthrodesis does decrease lunate strain but merely by shifting it to the radioscaphoid joint. STT fusion in a cadaver model was found to provide strain reduction similar to that of joint-leveling procedures but with greater loss of motion.
The use of STT fusion has waned in recent years because of complications and longer-term follow-up that has revealed decreased success rates [14] (Figure 9). Several authors have reported scapho capitate (SC) fusion. Biomechanically, this fusion has been shown to reduce strain at the radiolunate joint by about 10%. Some authors prefer this fusion because it requires only one fusion site and is technically easier to perform.
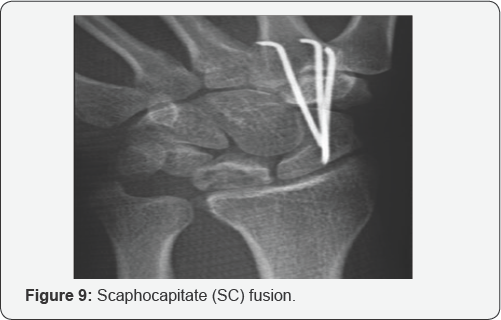
Finally, capitohamate fusion has been reported in some studies but a long follow-up is still not available.
At present, intercarpal fusions are more likely to be reserved for patients with neutral or positive ulnar variance in whom a joint-leveling procedure is contraindicated.
Revascularization
There are several sources for the pedicles, including the distal radius, pisiform, and pronator quadrates [15-18]. Results with the use of pedicled distal radius grafts have shown improved grip strengths and progressive evidence of revascularization on magnetic resonance imaging (MRI) over an 18- to 36-month period [19]. Revascularization techniques may also be combined with other previously mentioned approaches. Revascularization is especially attractive for the young patient with ulnar-neutral or ulnar-positive variance in whom a radial shortening is not an option and for the patient who wishes to avoid an intercarpal fusion and resultant loss of motion.
Salvage Procedures
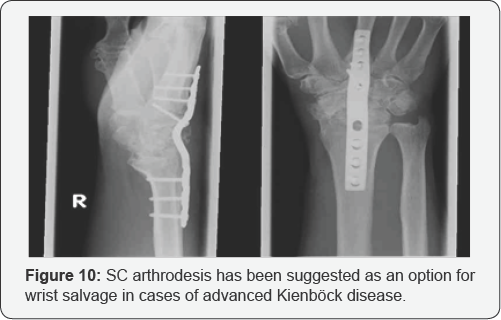
Salvage procedures are reserved for later stages of disease and for failures of other treatments. Proximal row carpectomy (PRC) has been shown to provide relatively good results for Kienbock disease, as well as for other wrist problems [20].Wrist arthrodesis is the final option for patients with global wrist degeneration. Arthrodesis can be achieved successfully following a failed PRC. SC arthrodesis has been suggested as an option for wrist salvage in cases of advanced Kienbock disease [21] (Figure 10). A reasonable approach to determining the surgical treatment of Kienbock disease based on stage is as follows:
i. Stage 0, I, II, or IIIa with ulnar-negative variance: Radial shortening, revascularization and denervation
ii. Stage 0, I, II, or IIIa with ulnar-neutral or positive variance: Revascularization, capitohamate (CH) fusion with capitate shortening, distal radius wedge osteotomy and denervation.
iii. Stage IIIb: SC fusion, radial shortening and denervation.
iv. Stage IV: PRC, total wrist arthrodesis and denervation.
References
- Lutsky K, Beredjiklian PK (2012) Kienbock disease. J Hand Surg Am 37(9): 1942-1952.
- Bain GI, Yeo CJ, Morse LP (2015) Kienbock Disease: Recent Advances in the Basic Science, Assessment and Treatment. Hand Surg 20(3): 352365.
- De Smet L (1994) Ulnar variance: facts and fiction review article. Acta Orthop Belg 60(1): 1-9.
- Stahl S, Stahl AS, Meisner C, Rahmanian Schwarz A (2012) A systematic review of the etiopathogenesis of Kienböck's disease and a critical appraisal of its recognition as an occupational disease related to hand- arm vibration. BMC Musculoskelet Disord 13: 225.
- Gelberman RH, Salamon PB, Jurist JM (1975) Ulnar variance in Kienböck's disease. J Bone Joint Surg 57(5): 674-676.
- Gelberman RH, Bauman TD, Menon J (1980) The vascularity of the lunate bone and Kienböck's disease. J Hand Surg 5(3): 272-278.
- Kulhawik D, Szaiaj T, Grabowska M (2014) A vascular necrosis of the lunate bone (Kienböck's disease) secondary to scapholunate ligament tear as a consequence of trauma - a case study. Pol J Radiol 79: 24-26.
- Bain GI, Begg M (2006) Arthroscopic assessment and classification of Kienböck's disease. Tech Hand Up Extrem Surg 10(1): 8-13.
- Keith PPA, Nuttall D, Trail I (2004) Long-term outcome of nonsurgically managed Kienböck's disease. J Hand Surg Am 29(1): 63-67.
- Mehrpour SR, Kamrani RS, Aghamirsalim MR, Sorbi R, Kaya A (2011) Treatment of kienbock disease by lunate core decompression. J Hand Surg Am 36(10): 1675-1677.
- Ueba Y, Nosaka K, Ikeda N, Seto Y, Nakamura T (1999) An operative procedure for advanced Kienböck's disease. Excision of the lunate and subsequent replacement with a tendon-ball implant. Journal of orthopaedic science 4(3): 207-215.
- Illarramendi AA, De Carli P (2003) Radius decompression for treatment of Kienbock disease. Tech Hand Up Extrem Surg 7(3): 110-113.
- Iwasaki N, Minami A, Ishikawa J, Kato H, Minami M (2005) Radial osteotomies for teenage patients with Kienbock disease. Clin Orthop Relat Res 439: 116-122.
- Lee JS, Park MJ, Kang HJ (2012) Scaphotrapeziotrapezoid arthrodesis and lunate excision for advanced Kienbock disease. J Hand Surg Am 37(11): 2226-2232.
- Elhassan BT, Shin AY (2009) Vascularized bone grafting for treatment of Kienböck's disease. J Hand Surg Am 34(1): 146-154.
- Simmons SP, Tobias B, Lichtman DM (2009) Lunate revascularization with artery implantation and bone grafting. J Hand Surg Am 34(1): 155-160.
- Mathoulin C, Wahegaonkar AL (2009) Revascularization of the lunate by a volar vascularized bone graft and an osteotomy of the radius in treatment of the Kienböck's disease. Microsurgery 29(5): 373-378.
- Sheetz KK, Bishop AT, Berger RA (1995) The arterial blood supply of the distal radius and ulna and its potential use in vascularized pedicled bone grafts. J Hand Surg Am 20(6): 902-914.
- Mazur KU, Bishop AT, Berger RA (1997) Vascularized metaphyseal bone grafts from the distal radius in the treatment of Kienböck's disease. Orthopaedic Transactions 21: 244.
- Kremer T, Sauerbier M, Trankle M, Dragu A, Baumeister S, et al. (2008) Functional results after proximal row carpectomy to salvage a wrist. Scand J Plast Reconstr Surg Hand Surg 42(6): 308-312.
- Iorio ML, Kennedy CD, Huang JI (2015) Limited intercarpal fusion as a salvage procedure for advanced Kienbock disease. Hand (N Y) 10(3): 472-476.






























