Endoscopic Treatment of Iliopsoas Tendinitis after Hip Resurfacing
Hugo Aleixo1*, S0ren R Jakobsen2 and Marcus VL Oliveira3
1Department of Orthopaedic Surgery, Hospital Pedro Hispano, Portugal
2Department of Orthopaedic Surgery, Aarhus University Hospital, Denmark
3Department of Health Technology and Biology, Federal Institute of Bahia, Brasil
Submission: September 08, 2017; Published: September 11, 2017
*Corresponding author: Hugo Aleixo, Department of Orthopaedic Surgery, Hospital Pedro Hispano, Matosinhos, Portugal, Email: humimoal@hotmail.com
How to cite this article: Hugo A, S�ren R J, Marcus V L O. Endoscopic Treatment of Iliopsoas Tendinitis after Hip Resurfacing. Ortho & Rheum Open Access 2017; 8(3): 555740. DOI: 10.19080/OROAJ.2017.08.555740
Abstract
Introduction: Coxa saltans interna, also known as internal snapping hip, presents as groin pain associated with a catching sensation caused by the iliopsoas tendon when bringing from a position of flexed abduction to extended adduction. We describe what we consider to be the current indications for surgical lengthening or release, the pertinent physical findings, and imaging and describe a case of iliopsoas irritation after a hip resurfacing and the arthroscopic treatment performed. The results are reproducible and weakness of flexion is not expected after surgery.
Methods: We describe a case of iliopsoas tendinitis after a hip resurfacing. The pain was refractory to medical management who was submitted to an arthroscopic lengthening with success.
Results: The pain subsided after 10 weeks without any loss in hip motion. The VAS is now 9/10 and UCLA 9. No difference leg flexion or extension was noted and the patient is able to perform is daily activities without crutches.
Discussion: Iliopsoas tendinitis can be successfully managed with rest and NSAIDs in most cases. However, it is our experience that in case of need for surgical treatment, the arthroscopic management is possible with an accurate technique.
Introduction
Painful snapping hips are due to external, internal, and intra- articular causes [1-3]. The external snapping hip, also the most common type of snapping hip [4], is the result of the iliotibial band snapping across the greater trochanter as the hip moves from flexion to extension and is evident on clinical examination. The intra-articular variety is due to labral tears, loose bodies, and articular cartilage flaps within the hip joint itself. However, the term "intra-articular snapping hip" is rarely used in current literature because a snapping mechanism is not really involved, and diagnosis of intraarticular pathology is now more accurate with other exams. The third type or internal snapping hip was first described in 1951 [5], which is the focus of this case- report, is the result of three possible situations: either a tendon catching at the iliopectineal eminence, or snapping across the femoral head, or flipping over the iliac muscle when the hip is brought from a flexed-abducted-externally rotated position into extension during athletic activities [6]. This happens mostly during activities of daily living, with the associated pain [7].
Although there is a debate whether the tendon’s path is exactly obstructed, it is generally accepted that anatomic factors are the main cause for a tight musculotendinous unit. Whereas a painless, internal snapping hip is normal in the population in up to 10% [4], a painful snapping hip is due to intrinsic iliopsoas tendon pathology or is secondary to other factors, such as native or arthroplasty hip joint pathology, instability or high femoral antetorsion [8].
Treating the Iliopsoas Tendinitis
The internal snapping hip syndrome is characterized by an audible or palpable snap in the anterior area of the hip. In asymptomatic individuals, no treatment is required [4]. Symptomatic individuals with this problem typically report a painful snapping in their hip, localized to the anterior and medial groin area [9]. Their pain is usually exacerbated by active hip flexion and activities that require extension of the flexed, abducted, and externally rotated hip. For this reason, painful snapping iliopsoas tendons most often occur in young, physically active individuals and are common in sports that demand repeated abduction of the leg above waist level [10].
The initial treatment consists inrest, stretching exercises, oral anti-inflammatory medications, and focal treatment including iontophoresis and ultrasound. These will resolve most iliopsoas tendinitis [11]. It is very important to explain the pathology to the patient, so that he can easily cope with this treatment and avoid recurrence of the tendinitis. It is mandatory to be certain that a nonoperative treatment has failed before offering the surgical release. In the setting of primary intrinsic tendon pathology and some secondary pathologies, surgical lengthening or release may be considered [9]. Nevertheless, some will maintain pain, usually being the ones with impingement across the anterior acetabulum, irritation after hip arthroplasty or a refractory tendinitis.
Methods
We present a case of an active man, 54 year-old, submitted to a left Hip Resurfacing (Birmingham Hip Resurfacing - Wright Medical ®) in the last year; the post-operative X-ray is presented in Figure 1. In the post-operative period, his main complaints from osteoarthritis subsided. However, he gradually started complaining about a medial and anterior pain when he flexed the hip above de 70°, with no differences with internal or external rotation. It is possible to say that the acetabular implant (Figure 1) is more anteverted comparing o the contralateral side, and we considered this as a possible cause for the clinical iliopsoas tendinitis. After trying the recommended initial course of rest and NSAIDs, the pain didn't subside. He was then indicated for physiotherapy, with no pain relief. To confirm the source of pain objectively, we proposed an anterior bursa injection with ultra-sound guidance [12]. The patient's left iliopsoas was injected with 5 ml of lidocaine 1% and he referred immediate relief of pain and increase range of motion. After the initial effect of lidocaine, pain came again. A surgical iliopsoas tendon lengthening was needed, either open or arthroscopic. Our option was the arthroscopic release.

Material
We decided to propose an arthroscopic release via peripheral compartment. As an option, and if it wasn't possible to perform due to technical difficulties, we would perform the procedure in an open fashion. The patient was placed in a traditional femoral fracture table. Commercially distraction systems are also available, according to surgeon’s preference. Special equipment is not necessary - the same positioning devices and instruments that are routinely used for hip arthroscopy are needed: 70° arthroscope, arthroscopic beaver blade, nitilol guidewire, blunt switching stick, radiofrequency device, shaver and a slotted cannula. The decision of whether to use lateral or supine positive is more a matter of individual training and habit of use - the supine approach was used in this case. As in every hip arthroscopy, it is of most importance to protect appropriately the bony prominences. Every point of contact must be well padded to avoid potential complications. Also, the operative hip must maintain the possibility of having to be mobilized during surgery.
Technique and Results
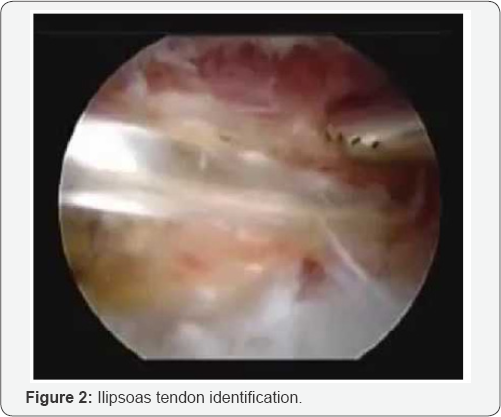
Endoscopic release can be made in essentially two ways: approaching the hip central and peripheral compartment or through an extra-articular release. In both, traction can or cannot be applied [13]. We used the antero-lateral and the anterior portals to be able to triangulate and have direct access to the tendon. As the patient had already been submitted to a HR through an antero-lateral approach, the path to find the tendon was facilitated. However, the authors recognize that it's of paramount importance to perform it in external rotation, so that the lesser trochanter comes to anterior, bringing the insertion of the muscle in a more accessible anatomy. As the tendon was identified (Figure 2), shaver and radiofrequency devices were used, and the lengthening was performed at the level of the lesser trochanter [14]. Cutting the tendon at this level preserves 40% of the musculo-tendinous unit and does not result in a complete detachment of the iliopsoas.
The patient was discharged the day after with crutches and permitted to do partial weight bearing [15]. On the follow-up, he showed loss of muscle power in flexion, which was expected. According to the literature, this happens in the first 8-10 weeks. Approximately at 10 weeks, he no longer felt loss in ROM in flexion, as expected as well. The pain subsided after 10 weeks without any loss in hip motion. The VAS is now 9/10 and UCLA 9. No difference leg flexion or extension was noted and the patient is able to perform is daily activities without crutches.
Conclusion
We found the ultrasound-guided anaesthetic injection of the psoas bursa useful to confirm snapping of the iliopsoas tendon as the cause of a patient's hip pain. Arthroscopic management of iliopsoas management is a safe outpatient procedure that provides effective relief of the snapping and pain.
References
- Allen WC, Cope R (1995) Coxa saltans: the snapping hiprevisited. J Am Acad Orthop Surg 3(5): 303-308.
- Dobbs MB, Gordon JE, Luhmann SJ, Szymanski DA, Schoenecker PL (2002) Surgical correction of the snapping iliopsoas tendon in adolescents, J Bone Joint Surg Am 84(3): 420-424.
- Flanum ME, Keene JS, Blankenbaker DG, DeSmet AA (2007) Arthroscopic treatment of the painful "internal” snapping hip: results of a new endoscopic technique and imaging protocol. Am J Sports Med 35(5): 770-779.
- Potalivo G, W Bugiantella (2017) Snapping hip syndrome: systematic review of surgical treatment. Hip Int 27(2): 111-121.
- Nunziata A, Blumenfeld I (1951) Snapping hip: note on a variety. Prensa Med Argent. 38(2): 1997-2001.
- Musick SR (2017) Snapping Hip Syndrome. StatPearls Publishing LLC. Treasure Island (FL), USA.
- Yen YM, CL Lewis, YJ Kim (2015) Understanding and Treating the Snapping Hip. Sports Med Arthrosc, 23(4): 194-199.
- Capogna BM, Shenoy K, Youm T, Stuchin SA (2017) Tendon Disorders After Total Hip Arthroplasty: Evaluation and Management. J Arthroplasty pii: S0883-5403(17)30337-30360.
- Via AG, Basile A, Wainer M, Musa C, Padulo J, et al. (2016) Endoscopic release of internal snapping hip: a review of literature. Muscles Ligaments Tendons J 6(3): 372-377.
- Henning PT (2014) The running athlete: stress fractures, osteitis pubis, and snapping hips. Sports Health 6(2): 122-127.
- Macke C, C Krettek, S Brand (2017) Tendinopathies of the hip: Treatment recommendations according to evidence-based medicine. Unfallchirurg 120(3): 192-198.
- Flanum ME, Keene JS, Blankenbaker DG, Desmet AA (2007) Arthroscopic treatment of the painful "internal” snapping hip: results of a new endoscopic technique and imaging protocol. Am J Sports Med 35(5): 770-779.
- Ilizaliturri VM Jr, C Suarez-Ahedo, M Acuna (2015) Internal Snapping Hip Syndrome: Incidence of Multiple-Tendon Existence and Outcome After Endoscopic Transcapsular Release. Arthroscopy 31(10): 19911995.
- Blomberg JR, BS Zellner, JS Keene (2011) Cross-sectional analysis of iliopsoas muscle-tendon units at the sites of arthroscopic tenotomies: an anatomic study. Am J Sports Med 39: 58s-63s.
- El Bitar YF, Stake CE, Dunne KF, Botser IB, Domb BG (2014) Arthroscopic Iliopsoas Fractional Lengthening for Internal Snapping of the Hip: Clinical Outcomes With a Minimum 2-Year Follow-up. Am J Sports Med 42(7): 1696-1703.






























