The Effect of Patient Positioning During Radiographs on The Resulting Cobb Angle Measurements
Matthew Siljander1, KadeMcQuivey2, Sapan Gandhi1 and *Patrick Knott3
1Department of Orthopaedic Surgery, Beaumont Health System, USA
2Oakland University William Beaumont School of Medicine, USA
3Rosalind Franklin University of Medicine and Science, USA
Submission: April 30, 2017; Published: May 23, 2017
*Corresponding author: Patrick Knott, Rosalind Franklin University of Medicine and Science, 3333 Green Bay Road, North Chicago, USA, Tel: (847) 578-8689; Email: patrick.knott@rosalindfranklin.edu
How to cite this article: Matthew S, KadeMcQuivey, Sapan G, Patrick K. The Effect of Patient Positioning During Radiographs on The Resulting Cobb Angle Measurements. Ortho & Rheum Open Access J 2017; 7(1): 555705. DOI: 10.19080/OROAJ.2017.07.555705
Abstract
Background: Standing spinal radiographs are the primary method of spinal deformity evaluation in patients with scoliosis. During periods of patient surveillance, the clinician compares serial radiographs to assess progression of the deformity. One of the potential problems in comparing sequential radiographs is variation in patient positioning.
Methods: Computed tomography (CT) scans of seven patients with AIS were used retrospectively. Three dimensional (3D) reconstructions of the images were created by CT scan software. Cobb angles were drawn for scoliosis curves in the coronal plane. The 3D image was then rotated two degrees clockwise and Cobb angle measurements were repeated. This procedure was repeated through 14 degrees of clockwise and counterclockwise rotation. To evaluate variability in patient positioning for standing radiographs, 10 volunteers were positioned in front of a wall. A positional sensor was used to measure axial rotation.
Results: Patients were positioned in front of a radiographic cassette in a reproducible way, but had a standard offset of +/- 3.2 degrees. A two degree rotation of the patient’s trunk resulted in a one degree change in the measured Cobb angle (in patients with larger scoliosis curves, and in the first six degrees of trunk rotation).
Conclusion: Patient positioning needs to be considered when evaluating the progression of spinal deformity, as it can influence the calculation of scoliosis measurements.
Keywords: Scoliosis; Radiographs; Cobb angle
Abbreviations: AIS: Adolescent Idiopathic Scoliosis; CW: Clock Wise; CCW: Counter-Clock Wise;
Introduction
Adolescent idiopathic scoliosis (AIS) is the most common type of idiopathic scoliosis [1], and occurs between ages 10 and maturity [2]. The Scoliosis Research Society has defined scoliosis as ateral curvature of the spine greater than 10 degrees as measured by the Cobb method in a standing coronal plane radiograph [3], and can present as curvature of thoracic and lumbar spine [4]. Treatment recommendations for patients with scoliosis are based on curve magnitudes. Bracing is initiated when the Cobb angles reach 25 degrees, and surgery may be recommended for curves greater than 40 degrees. However, with a margin of error that approaches 10 degrees in measuring Cobb angles, it is difficult to make clinical decisions based on these measurements alone. Only 10% of adolescents with diagnosed scoliosis require medical intervention[5] . Thus, proper evaluation of treatment is necessary to avoid unnecessary exposure to radiation.
Curve patterns in AIS often use the Lenke classification system [6] . Inter-examiner consistency of Cobb angle measurement has been evaluated, and a variability of 4.9 percent was present in a study using four examiners and 50 radiographs [7]. The effects of patient positioning errors have not been well described in the literature, but could theoretically account for up to 20-30 degrees of variation [8]. In vivo patient positioning errors have largely not been studied due to ethical conflicts that exist from exposing patients to unnecessary doses of radiation [9]. Radiation from diagnostic x-rays in patients with AIS has been shown to influence cancer rates. Data from 1925 to 1965 reported a 2-fold increase in the risk of breast cancer for women treated for scoliosis [10]. Advancements in reliability and accuracy of measurements could potentially result in improved treatment plans with decreased radiation exposure.
Materials and Methods
This study was divided into 2 separate phases. Phase 1 analyzed average axial trunk rotation in patients positioned for standing radiographs, and phase 2 analyzed the measurement of thoracic and lumbar Cobb angles from three-dimensional (3D) computed tomography (CT) reconstructions.
Phase 1: Accuracy of Patient Positioning
In phase one of the study, ten volunteer students were recruited after approval by the university IRB committee. The first ten volunteers were selected without exclusion criteria. Each student had a small electronic position sensor placed on his or her back, held in place by a belt. The students were instructed to stand with the sensor pressed up to the wall, and this point was calibrated to zero. The student was then instructed to step forward away from the wall. Subsequently they were instructed to step back and positioned in front of a wall, with the goal to position parallel with the wall. Position sensor readings were then taken to evaluate trunk angle of rotation from parallel. This was repeated 10 times for each of the 10 subjects. The purpose of this positioning analysis was to quantify the average axial trunk rotation in patients positioned for standing radiographs. A reading of zero degrees is desired, and represents a patient's trunk positioned perfectly parallel to the imaging surface, represented by a wall in this study. The results of this analysis were then used to determine the range that would be used to quantify a relationship between axial trunk rotation and change in Cobb angle scoliosis.
Phase 2: Thoracic and Lumbar Cobb Angle Measurements
After approval by the university IRB committee, CT scans of seven patients with adolescent idiopathic scoliosis were used retrospectively. Some of these patients exhibited both right thoracic and left lumbar curves. Of these seven patients, six patients had measurable right thoracic curves and four had measurable left lumbar curves, for a total of 10 curves that were measured. 3D reconstructions of the images were created by the CT scan software, and displayed at a workstation that allowed for rotation of the image. Using the viewing software, Cobb angles were drawn for the thoracic and lumbar scoliosis curves in the coronal plane. The 3D image was then rotated two degrees to the right, and the Cobb angle measurements were repeated. This procedure was repeated through 14 degrees of right rotation, and then subsequently through 14 degrees of left rotation. These measurements were repeated six times for each angle position. The Cobb angles were measured by a single operator to eliminate inter-operator error. Kyphosis angles were measured for right thoracic curves and lordosis angles were measured for left lumbar curves. These measurements were repeated six times. For each curve the following parameters were obtained: coronal Cobb angle and sagittal thoracic kyphosis and lumbar lordosis.
These scans represented larger curve sizes (between 41 - 54 degrees), however, two smaller curves were measured as they appeared as a secondary curve in patients with a larger primary curve (18 and 25 degrees). CT scans were used instead of radiographs, because of the capability of rotating the spine by defined degrees in either direction. Additionally, by using CT scans instead of radiographs, the inherent error associated with standing radiographic positioning was eliminated.
ANOVA testing was conducted (SPSS version 9.0) to determine significant differences in Cob bangle as compared to zero degrees of rotation. Additionally, as the patients' CT models were rotated both counterclockwise and clockwise, two values were achieved for each of the measured set points. Clockwise (CW) rotation is represented by negative values (-2, -4, -6 degrees) and counter-clockwise (CCW) rotation is represented by positive values (+2, +4, +6 degrees). ANOVA analysis was also conducted for significant differences in Cobb angles between CW and CCW positions and magnitude of kyphosis and lordosis.
Results
Phase 1: Accuracy of Patient Positioning
The average Angle of axial rotation was 3.2 degrees with a standard deviation of 2.1 degrees. As a result of the position study, the range used for the Cobb angle model was set to 0-6 degrees.
Phase 2A: Measurement of Thoracic Cobb Angles
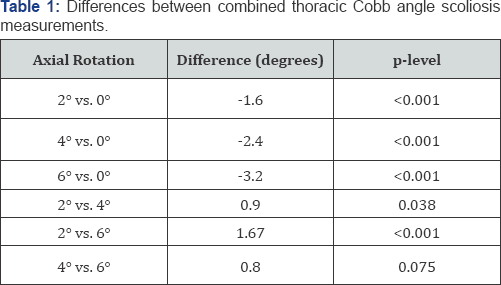
ANOVA testing showed significant differences (p < 0.05) in thoracic Cobb angles between all levels of axial rotation and zero in the 0-6 degree range. The CCW/CW groups (+2/-2, +4/-4, +6/6) did not show statistical differences, thus, it became possible to combine the measurements into a single range from zero to six degrees, irrespective of direction of rotation (Table 1). For the combined range, all values were statistically different from each other (p< 0.05) with the exception of the 4 versus (vs.) 6-degree parameter (p = 0.075). The range of thoracic kyphosis in this study was from 17 to 47 degrees. The magnitude of kyphosis did not have a statistically significant impact on change in Cobb angle magnitude in the 0-6 degree range of axial rotation for thoracic scoliosis curves. For magnitudes of rotation greater than six degrees, the extent of kyphosis curves would likely begin to show a significant effect, as a higher proportion of the curve is progressively rotated into or out of the plane of view.
A model was created to demonstrate the change in thoracic Cobb angle as a function of axial trunk rotation (patient positioning) in the 0-6 degree range. This is a representative model for the calculation of a true (or more accurate) Cobb angle (Figure 1). Refer to Equation 1 (AR = axial rotation).

(Equation 1) TRUE COBB ANGLE = Measured Cobb Angle - (0.05xAR2 - 0.84xAR)
Phase 2B: Measurement of Thoracic Cobb Angles
The analysis of left lumbar scoliosis curves was conducted in the same fashion as for right thoracic curves. There were significant differences in lumbar Cobb angles for all magnitudes of axial rotation in the 0-6 degree range. The CCW/CW groups (+2/-2, +4/4, +6/-6) did not show statistical differences, thus, similarly to the thoracic curves, it was possible to combine the measurements into a single range from 0 - 6 degrees (Table 2). For the combined range, all values were statistically different from each other (p< 0.05) with the exception of the 2 vs. 4 degree (p = 0.9) and 4 vs. 6-degree parameters (p = 0.1).

The range of lumbar lordosis in this study was from 50-70 degrees. There was no statistical difference between any of the lordosis groups on change in Cobb angle magnitude, in the 0-6 degree range of axial rotation for lumbar scoliosis curves. Similarly to thoracic angles, a model was created to demonstrate the change in lumbar Cobb angle as a function of axial trunk rotation (patient positioning) in the 0-6 degree range. This representative model allows for the calculation of a true (or more accurate) Cobb angle (Figure 2). Refer to Equation 2 (AR = Axial rotation).
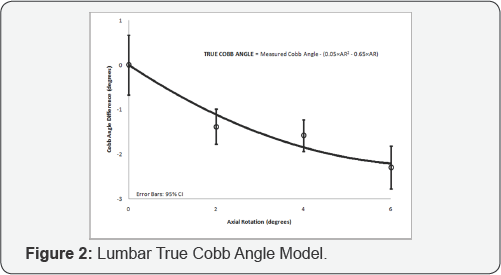
(Equation 2) TRUE COBB ANGLE = Measured Cobb Angle - (0.05xAR2 - 0.65xAR)
Discussion
Progressive increase of curve size is a factor used to develop treatment plans for patients with adolescent idiopathic scoliosis. Important surgical decisions are made based on standing spinal radiographs, yet it is not known how accurate these radiographs are. Additionally, Cobb angle progression over time as measured from a series of standing spinal radiographs can be influenced by patient positioning. Given a series of images taken over several years, there is not a good method to quantify what portion of Cobb angle change is due to physiological change in spine curvature, as opposed to error associated with measurement technique, including axial positioning of the patient. The variation in patient positioning from image to image would be significantly improved with a method that would allow clinicians to account for this positioning effect.
Phase one of this study showed that the average angle of axial rotation with standing radiographs is three degrees. The next step was to determine what effect this level of rotation would have on measured Cobb angles. Phase two of this study demonstrated and quantified statistically significant changes in Cobb angle, even at these small degrees of rotation. In general, a two degree rotation of the patient’s trunk resulted in a one degree change in the measured Cobb angle in the first size degrees of trunk rotation. Clinically, it is difficult appreciate the significance of such small changes in Cobb angle. Ultimately the goal is to create a more reliable method for measuring radiographs to insure accuracy, and to allow clinician to make decisions with better clinical information. At the same time, the number of radiographs taken should be minimized to reduce the level of cumulative radiation exposure.
The models that have been provided in this study quantify a statistically significant relationship between Cobb angle changes with patient positioning, in a small patient population. Once a method has been established to quantify axial rotation during standing radiographs, an algorithm such as this one, obtained from a larger patient population, can be applied either automatically to correct Cob bangle as part of the radiograph measuring software, or can be manually calculated. As a result, Cobb angle measurement will be improved for that specific radiograph and will also allow more accurate comparisons between radiographs.
Conclusion
This study demonstrated that patient positioning contributes to error in Cobb angle measurement. Although statistically significant, these small changes in Cobb angle may not be clinically significant, given the large variability in Cobb angle measurements. Patient positioning should be considered when making important management decisions. Further studies are warranted.
References
- Edery P, Margaritte-Jeannin P, Biot B, Labalme A, Bernard JC, et al. (2011) New disease gene location and high genetic heterogeneity in idiopathic scoliosis. Eur J Hum Genet 19(8): 865-869.
- Dobb MB, Weinstein ML (1999) Infantile and Juvenile Scoliosis. Orthop Clin North Am 30(3): 331-341.
- Reamy BV, Slakey JB (2001) Adolescent idiopathic scoliosis: review and current concepts. Am Fam Phys 64(1):111-116.
- Asher MA, Burton DC (2006) Adolescent idiopathic scoliosis: natural history and long termtreatment effects. Scoliosis 1(1): 2.
- Miller NH (1999) Cause and natural history of adolescent idiopathic scoliosis. Orthop Clin North Am 30: 343-352.
- Lenke LG (2007) The Lenke classification system of operative adolescent idiopathic scoliosis. Neurosurg Clin N Am 18(2): 199-206.
- Morrissy RT, Goldsmith GS, Hall EC, Kehl D, Cowie GH (1990) Measurement of the Cobb angle onradiographs of patients who have scoliosis. Evaluation of intrinsic error. J Bone Joint Surg Am72(3): 320327.
- Schmid SL, Buck FM, Boni T, Farshad M (2016) Radiographic measurement error of the scoliotic curve angle depending on positioning of the patient and the side of scoliotic curve. Eur Spine J 25(2): 379-384.
- Enriquez G, Piqueras J, Catala A, Oliva G, Ruiz A, et al. (2014) Optimization of radiological scoliosis assessment. Med Clin (Barc)143(Suppl. 1): 62-67.
- Levy AR, Goldberg MS, Mayo NE, Hanley JA, Poitras B (1996) Reducing the lifetime risk of cancer from spinal radiographs among people with adolescent idiopathic scoliosis. Spine 21(13): 1540-1547.






























