Surgical Outcomes and Healthcare Experience in Spinal Surgery: Are They Related
James Thomas Bourne 1*, Charlotte Emily Cross2, Irfan Naveed Yasin2 and Mohammed Naveed Yasin2
1Department of Trauma & Orthopaedic Surgery, Royal Preston Hospital, UK
2Department of Spinal Surgery, Salford Royal NHS Foundation Trust, UK
Submission: April 30, 2017; Published: May 12, 2017
*Corresponding author: James Thomas Bourne, Department of Trauma & Orthopaedic Surgery, Royal Preston Hospital, Sharoe Green Lane, Fulwood, Preston, Lancashire, United Kingdom, Tel: 01772 716565; Email: drjtbourne@gmail.com
How to cite this article: James T B, Charlotte E C, Irfan N Y, Mohammed N Y. Surgical Outcomes and Healthcare Experience in Spinal Surgery: Are They Related. Ortho & Rheum Open Access 2017;7(1): 555701. DOI: 10.19080/OROAJ.2017.07.555701
Abstract
Introduction: Patient healthcare satisfaction and surgical outcome are two important measures. Their complex relationship has not been studied in spinal surgery and the question remains: Are patients with a good surgical outcome satisfied with their healthcare experience?
Method: Patients completed a validated Spine TANGO Core Outcome Measure Index (COMI) questionnaire at 3 months after surgery. Two questions assessing healthcare experience and surgical outcome, both graded from 1-5, were used to measure the two variables for each patient. Statistical analysis was completed to measure any relationship that may exist between the two indices.
Results: 3096 completed questionnaires were analysed. The results demonstrated a weak relationship(correlation coefficient = 0.34, kappa = 0.167)
Conclusion: A weak relationship exists between healthcare experience satisfaction and surgical outcome in spinal surgical patients.
Keywords: Surgical outcomes; Spine; TANGO; Patient reported outcome measures; PROMS
Introduction
There is increasing recognition of the importance of patients’ opinion of the quality of their care. In 2008, The Department of Health (DOH) of Her Majesty’s Government (HMG) stated that quality of care in the NHS should include the following aspects: Patient safety, patient experience and clinical effectiveness [1]. It seems reasonable that these three domains are inter-related but the literature is unclear as to whether there is a relationship, and its nature, between surgical outcome and patient satisfaction.
Patient reported measures have been described as strongly correlated with better outcomes and capture patient evaluation of communication with nurses and physicians rather than noncare aspects [2,3]. However, critics express concerns about patient-reported measures, particularly those assessing "patient satisfaction." They state that patient feedback is not credible, as patients lack formal medical training, and are therefore not able to separate the different domains of healthcare. Following this viewpoint critics believe that patient-satisfaction measures capture an aspect of "happiness," which is influenced by factors unrelated to their hospital stay [4,5]. Given the associations between many spinal pathologies and personality traits and social and psychological inter-relationships, there is an even stronger potential for this in spinal surgery [6,7]. As a result, our aim was to assess whether surgical outcome was related to patient satisfaction and a positive healthcare experience in spinal surgery.
Materials and Methods
Prospectively collected outcome data, Spine TANGO Core Outcome Measure Index (COMI) was utilised. This validated patient questionnaire is routinely collected for all spinal surgery at our institution and is collected at specific time points postoperatively. Analysis was performed upon the 3 month data, to enable accurate recall and reflection of patients’ satisfaction with their healthcare experience. All patients undergoing spinal surgery, excluding therapeutic or diagnostic injections and manipulations are requested to complete the Spine TANGO COMI.
The questionnaire contains data relating to demographics, procedure, complications and outcomes. Two distinct COMI forms exist relating to back and neck surgery, but the questions remain the same except for the terms back and neck being interchanged.
Outcome Data
Within Spine TANGO there are two key questions, assessed by a rating scale, to ascertain surgical outcome and healthcare satisfaction. The question to ascertain surgical outcome: 'Overall, how much did the operation in our hospital help your back/ neck problem?'. Each answer is weighted from 1 being 'very satisfied' or 'helped a lot', to 5 being 'very dissatisfied' or 'made things worse'. The second key question relates to healthcare satisfaction: 'Over the course of treatment for your back/neck problem, how satisfied were you with your overall medical care in our hospital? This is also graded over five answers from 'very satisfied’ to 'very dissatisfied'. Corresponding answers for each patient were tabulated analysed.
Data Analysis
Data analysis was performed with SPSS (IBM Corp. Released 2016. IBM SPSS Statistics for Windows, Version 24.0. Armonk, NY: IBM Corp.) to assess the correlation between two variables using the correlation coefficient, with no analysis of magnitude, direction or linearity of the correlation and the kappa coefficient.
Results
Over the study period a total of 6563 patients underwent surgery and were at least 3 months post-operative. Of these 6563 patients, 3505 replied with their three month COMIdata, giving a response rate of 53%. Patients with incomplete data sets were excluded, leaving 3096patients for statistical analysis (763 Neck COMI, 2333 Back COMI). The average age was 56 years with a slight male preponderance of 52%. 1490 patients (48%) were overweight, as defined by a BMI of greater than 25 (Table 1).

Overall patients were satisfied with their hospital experience, with 89.7% of patients scoring a 1 or 2 on the satisfaction rating scale, regardless of surgical outcome. The correlation coefficient between the two outcomes was 0.34 demonstrating weak correlation between the two variables. The kappa value was 0.167, again demonstrating only slight correlation [8]. The level of correlation was unaffected by gender, age, emergency or elective surgery, level of surgery or main pathology.
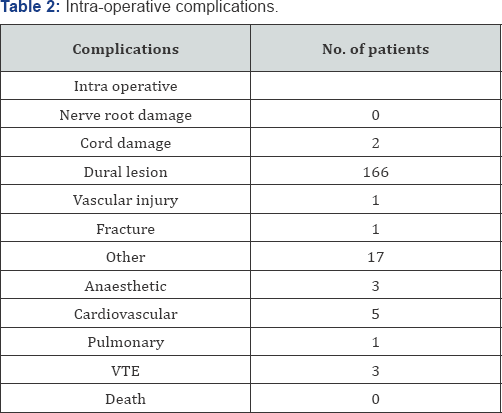
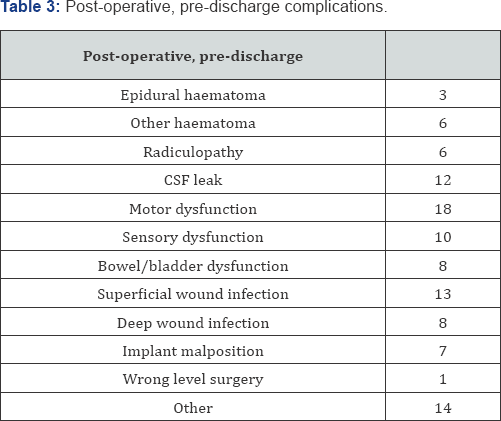
2796 (90%) patients left hospital with no complications.There was no difference in the level of satisfaction experienced between patients with or without a complication, with 90% of patients being satisfied in each group. Types and numbers of peri-operative complications are displayed in (Table 2) (Intraoperative complications) and (Table 3) (Post-operative, predischarge complications).
Discussion
Most of the patients reported a positive hospital experience with 89.7% reporting they were very satisfied or satisfied, regardless of their surgical outcome. There was no difference in satisfaction between male and females, 89% and 90% respectively or between elective and emergency surgeries, 90% satisfaction. Interestingly those patients who had a complication also reported high levels of satisfaction, 90%.
The correlation coefficient and kappa score results show that there is only a very weak relationship between the overall healthcare experience of a patient and their spinal surgical outcome, with results of 0.34 and 0.167 respectively. This is the first study that we are aware of in the UK which looks at the potential relationship between surgical outcome and healthcare experience as reported by the patient in spinal surgery. Previous research studies have looked at a range of non spinal medical conditions and demonstrate similar results to ours with a weakly positive relationship, with correlation coefficients ranging from 0.1-0.33 [9-13].
Strengths and limitations
The strength of this study is the large, prospectively collected dataset, with over 3000 spinal surgery episodes available for analysis. The limitations are the response rate of 53%. Response to post-operative questionnaires vary dependent on gender, age, and socio-economic status [14,15] thus bias may be introduced secondary to this, although our data shows no difference in satisfaction scores dependent on gender and age.
Conclusion
The statistical evidence of over 3000 patients within this study supports that there is only a weak relationship between patient experience and patient reported outcome following spinal surgery. This is an important finding when comparing surgical outcomes between units, surgeons or interventions. The result would suggest that the surgical outcome itself is largely unrelated to other factors that influence healthcare experience of the individual. These include the compassion of nursing staff and medical practitioners, amenities and cleanliness, organisation of procedures and anaesthetic information [16]. Therefore, surgical outcomes cannot be considered as the sole surrogate for the healthcare experience. Furthermore, it would seem justifiable to state that the healthcare experience cannot be considered a significant confounding factor, when comparing outcomes. These results contrast with those stated in the literature [16-18]. However, these involved a different patient group with none in their cohorts having undergone spinal surgery. The relationship, if it does exist, is likely to be complex [16].
As focus increases on publishing surgeon level data and the increasing use of patient reported outcomes, concerns have been raised by clinicians. This unease draws attention to the fact that patient reported measures may reflect the patients' overall level of satisfaction as opposed to the clinicians’ effectiveness or safety [19]. This study does not support these concerns demonstrating only a weak relationship between experience and outcome which is unaffected by surgical complication. Furthermore, regulators and policy-makers believe that patient experience can be used as a surrogate for surgical outcome measures and that it is unnecessary to collect this additional data. This study confirms that patient experience cannot be used as a surrogate maker for surgical outcome and safety.
Acknowledgement
Mr Saeed Mohammad and Mr Rajat Verma for their support.
References
- LoD D (2008) High quality care for all: NHS next stage review final report. Department of Health, London, UK.
- Glickman SW, Boulding W, Manary M, Staelin R, Roe MT, et al. (2010) Patient satisfaction and its relationship with clinical quality and inpatient mortality in acute myocardial infarction. Circ Cardiovasc Qual Outcomes 3(2): 188-195.
- Boulding W, Glickman SW, Manary MP, Schulman KA, Staelin R (2011) Relationship between patient satisfaction with inpatient care and hospital readmission within 30 days. Am J Manag Care 17(1): 41-48.
- Fenton JJ, Jerant AF, Bertakis KD, Franks P (2012) The cost of satisfaction: A national study of patient satisfaction, health care utilization, expenditures, and mortality. Arch Intern Med 172(5): 405411.
- Manary MP, Boulding W, Staelin R, Glickman SW (2013) The patient experience and health outcomes. New England Journal of Medicine 368(3): 201-203.
- Block AR, Ohnmeiss DD, Guyer RD, Rashbaum RF, Hochschuler SH (2001) The use of presurgical psychological screening to predict the outcome of spine surgery. Spine J 1(4): 274-282.
- Waddell G (1987) volvo award in clinical sciences: A new clinical model for the treatment of low-back pain. Spine 12(7): 632-644.
- Landis JR, Koch GG (1977) The measurement of observer agreement for categorical data. Biometrics 1977: 159-174.
- Fremont AM, Cleary PD, Lee Hargraves J, Rowe RM, Jacobson NB, et al. (2001) Patient-centered processes of care and long-term outcomes of myocardial infarction. Journal of General Internal Medicine 16(12): 800-808.
- Larson CO, Nelson EC, Gustafson D (1996) The relationship between meeting patients' information needs and their satisfaction with hospital care and general health status outcomes. International Journal for Quality in Health Care 8(5): 447-456.
- Slatore CG, Cecere LM, Reinke LF, Ganzini L, Udris EM, Moss BR, et al. (2010) Patient-clinician communication: Associations with important health outcomes among veterans with COPD. Chest 138(3): 628-634.
- Lee Y-Y, Lin JL (2009) The effects of trust in physician on self-efficacy, adherence and diabetes outcomes. Social Science & Medicine 68(6): 1060-1068.
- Black N, Varaganum M, Hutchings A (2014) Relationship between patient reported experience (prems) and patient reported outcomes (proms) in elective surgery. BMJ Qual Saf 23(7): 534-542.
- Hutchings A, Neuburger J, Grosse Frie K, Black N, van der Meulen J (2012) Factors associated with non-response in routine use of patient reported outcome measures after elective surgery in england. Health Qual Life Outcomes 10: 34.
- Merrill RM, Allen EW (2002) Racial and ethnic disparities in satisfaction with doctors and health providers in the united states. Ethnicity & Disease 13(4): 492-498.
- Linder-Pelz S (1982) Toward a theory of patient satisfaction. Social Science & Medicine 16(5): 577-582.
- Jackson JL, Chamberlin J, Kroenke K (2001) Predictors of patient satisfaction. Social Science & Medicine 52(4): 609-620.
- Kane RL, Maciejewski M, Finch M (1997) The relationship of patient satisfaction with care and clinical outcomes. Med Care 35(7): 714-730.
- Hildon Z, Allwood D, Black N (2015) Patients’ and clinicians’ views of comparing the performance of providers of surgery: A qualitative study. Health Expect 18(3): 366-378.






























