Surgical Options for Brachial Plexus Injury in Adults
Ricardo Monreal1*, Damian Gomez2, Giovanni Osinaga3 and Eilen Monreal4
1*Centro Médico MEDEX, República de Panamá, Perú
2Hospital Universitario Madrid Torrelodones, Torrelodones, Spain
3Hospital Obrero No. 3, Caja Nacional de Salud, Bolivia
4School of Medicine, Ricardo Palma University, Perú
Submission: April 14, 2017; Published: April 20, 2017
*Corresponding author: Ricardo Monreal, Centro Médico MEDEX, Republica de Panamá 3065 2do piso, San Isidro-Lima, Perú, Email: rmonreal59@yahoo.es
How to cite this article: Ricardo M, Dami�n G, Giovanni O, Eilen M. Surgical Options for Brachial Plexus Injury in Adults. Ortho & Rheum Open Access 2017; 6(3): 555687. DOI: 10.19080/OROAJ.2017.06.555687
Introduction
A careful analysis of the published literature, however, fails to offer a clear panorama of the functional results of reconstruction. Over the years, opinions concerning the treatment of lesions of the brachial plexus have changed. The first report of successful surgery on a traction injury of the brachial plexus was reported in 1900, by Thoburn [1] but the initial enthusiasm was replaced with pessimism because of the poor subsequent results [2].
The last three decades have witnessed a resurgence of interest in the pathology of the brachial plexus. Seddon [3] demonstrated that continuity of the neural substance can be repaired with auto logous nerve grafts, and surgeons were stimulated to consider reconstruction of traction lesions of the brachial plexus [4-15]. The development of microsurgery and improvements in imaging, electro diagnosis, surgical instruments and suture material renewed interest in surgical reconstruction, and has given rise to more favourable results. Surgical options, such as neurolysis, nerve grafts, nerve transfer, and palliative surgical procedures (tendon transfer or functioning free muscle transplantation and arthrodesis) offer different modalities to improve the clinical outcome of brachial plexus lesions. Evaluating outcomes of reconstructive surgery for lesions of the brachial plexus is extremely complex.
Surgical Treatment
Timing of surgical procedure
The time between accident and surgical intervention is one of the more important factors and may be an important predictor of the final outcome. Narakas and Hentz [16] found a correlation between preoperative duration and recovery. When reconstruction was delayed for more than 8-12 months, the recovery was poor, but if reconstruction was carried out before the fourth month, the functional outcome was better. Bentolila et al. [14] pointed out that the delay between the moment of injury and the surgical intervention presages the final outcome.Monreal [15] found that the preoperative duration inversely influenced the probability of motor recovery.
Indications for emergency operative procedures include vascular injury, open penetrating injuries, and open infected crushing/stretching wounds. In the case of closed BPI wounds and when there are no other emergent injuries, surgical exploration and recovery may not take place immediately. After 3-6 months surgical operation is recommended for traumatic palsy injuries with no clinical sign of functional restoration or electromyography signs of denervation. A delay of more than eight months implied a bad prognosis for functional recovery [7] and nerve reconstruction is not recommended for traumatic lesions more than 9 months after the accident although there have been reports of successful procedures after 9 months [8,9].
Repair priorities
The surgical plan should be individualized and a priority list must be established, based on functional importance and the prognosis after nerve reconstruction.
In our opinion, an ideal sequence of priorities:
A. Elbow flexion against (Figure 1).
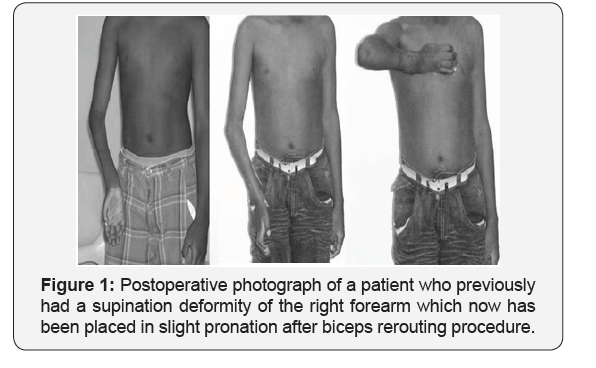
B. Shoulder stabilization and recovery of abduction and external rotation (Figure 1).
C. Elbow extension.
D. Brachio thoracic pinch (abduction of the arm against the chest).
E. Wrist and finger extension.
F. Wrist and finger flexion.
G. The ulnar innervated structures are the last priority because of the poor prognosis for recovery.
Surgical procedure
Neurolysis is indicated when the nerve lesion is in continuity. Anterior epineurectomy is recommended and interfascicular neurolysis should be avoided in order to preserve the intrinsic vascularity of the nerve. Nerve Grafting is the predominant technique for clear cut injuries with a healthy proximal stump and with no axial damage. The sural nerve, the sensory branch of ulnar nerve, and the medial cutaneous nerve of the forearm are the usual donor nerves. The outcome is influenced by the length of the nerve graft, the presence of scar tissue at the wound site, the number of grafts used, and the presence of a healthy proximal stump available. Narakas and Hentz [16] found that the functional outcome was favorable in cases with grafts less than 5 cm but that it was less favorable in those with grafts longer than 10 cm and Monreal [15] found that graft length inversely influenced the motor results after surgical treatment. A significant positive correlation was found between the number of grafts and muscular strength [15].
Neurotization: This type of procedure is used for preganglionic root injury in BPI to achieve motor reinnervation. The nerve transfer may be extraplexus or intraplexus. Intraplexus transfer options include intact nerve roots and extraplexus transfer options include the use of intercostal [17], spinal accessory nerve [18], phrenic nerve [19], and deep motor branches of the cervical plexus [20]. More recently, fascicles from a functioning ulnar and/or median nerve [21-23] have started, as well as branches of the radial nerve that go to the triceps muscle [24], and the contra lateral C7 [25]. Surgeons should always include sensory transfers in the surgical plan, in an attempt to recover protective sensation of the hand (median nerve area).
Reimplantation of brachial plexus: Carlstedt et al. [26,27] reported the first successful spinal cord implantation of an avulsed spinal nerve root [26,27]. Many questions remain about this type of procedure and further research is needed to bring conclusions.
Secondary Reconstruction
Restorative procedures for upper extremity functions after brachial plexus injuries are principally determined according to their pathological conditions. Repair of the brachial plexus is only one part of the treatment [15]. In the absence of spontaneous recovery or when the first surgical procedure does not provide satisfactory outcomes then a second palliative surgery may be required. Tendon and muscular transfers, arthrodesis, tenodesis, and functional free muscle transplantation should be done in order to improve the functional results.
Arthrodesis
Shoulder: Arthrodesis of the shoulder has stood the test of time, mainly to improve upper-limb function after paralysis. The optimum position for arthrodesis of the shoulder is debateable610 and the recommended positions are: 20 degrees of abduction, 30 degrees flexion, and 30 degrees of internal rotation to allow the patient to be independent in his daily life with a mean range of 60 degrees abduction and flexion through the scapulothoracic joint [28].
Wrist: In cases where the hand has some function, wrist arthrodesis may stabilize the joint and provide motor units for tendon transfers (i.e. flexor carpi radialis to extensor digitorum communis transfer) so as to enhance finger function. Wrist arthrodesis may stabilize the joint and increase grip strength. Arthrodesis places the wrist in a stable functional position, and subsequent tendon transfers can improve movement and power in the elbow when Steindler flexorplasty is done [29].
Tendon transfer
Tendon transfers are useful in restoring upper extremity function after BPI. An absolute indication for tendon transfer is in partial upper or lower brachial plexus paralysis.
Shoulder: Flail shoulder secondary to a brachial plexus injury is difficult to treat. After neurosurgical treatment and adequate physiotherapy, reconstructive surgery may be needed to improve the stability and function of the shoulder. Many tendon transfer techniques have been described for treating partial shoulder paralysis.
Several muscle transfers have been advocated to restore movement and stability of the shoulder after brachial plexus palsy [30-33]. Passive shoulder abduction of 80° is an important prerequisite, and requires intensive physiotherapy before transfer. If 80° is not obtained, shoulder arthrodesis is recommended [29].
Among the most common procedures are the following:
A. Trapezius to deltoid transfer to restore abduction of the shoulder.
B. Latissimus dorsi transfer as described by L' Episcopo,to improve external rotation.
C. Anterior transfer of the posterior branch of the deltoid muscle to restore nonfunctional anterior segment.
Trapezius transfer can provide satisfactory functional improvement and it is better than arthrodesis for paralysis of the shoulder after brachial plexus injury [34-38] (Figure 2).
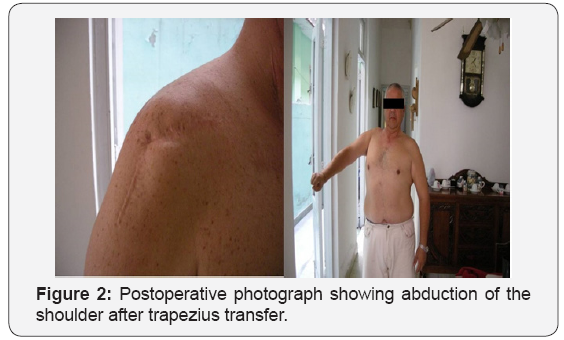
Elbow: Loss of elbow flexion due to traumatic palsy of the brachial plexus represents a major functional handicap. Then, the first goal in the treatment of the flail arm is to restore elbow flexion by primary direct nerve surgery or secondary reconstructive surgery. The surgical goal is to restore good muscle strength through a range of elbow motion (30 to 130 degrees).
There are various methods to restore elbow flexion which are well documented in the medical literature. One of the earliest procedures for restoring function to the elbow, Steindler flexorplasty first reported in 1918 [39] is still preferred by many surgeons.
A. transfer of the common origin of the flexor forearm muscles to a proximal section
B. transfer of latissimus dorsi muscle to the tendon of the biceps brachialis
C. transfer of pectoralis major brachial branch tendon to brachial biceps but a fused shoulder is required
D. transfer of triceps tendon to biceps (Figure 3).
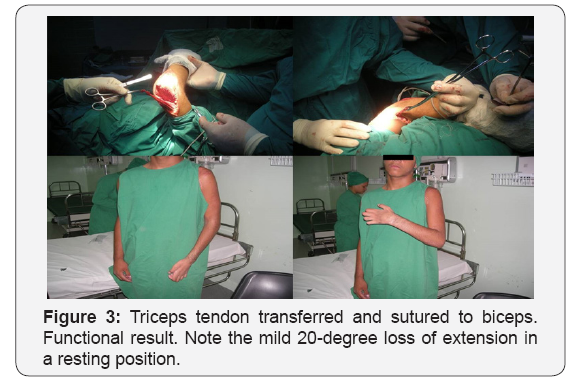
In patients with C5-C6-C7 palsy where the wrist and finger extensors are paralyzed or weaked, the flexor-pronators muscles of the forearm are strong but the triceps is not available for transfer; Monreal [29] proposed Steindler flexorplasty to restore elbow flexion should be complemented with wrist arthrodesis.
Forearm:Forearm rotation depends on the integrity of the proximal and distal radioulnar joints and utilizes four muscles: two pronators (pronator teres and) and two supinators (the biceps and the supinator). In severe brachial plexus palsy in children and adults, supination contracture results from muscle imbalance and shrinkage of inter osseous membrane. The surgical correction of a supination deformity may involve tendon transfers or correction of the axis of rotation by derotation osteotomies which may be open or closed. The biceps then becomes a pronator which provides a dynamic correction [40] (Figure 1).
Wrist and hand: The functional deficits of the hand in the brachial plexus injured patient are badly tolerated when the patient notices recovery of the shoulder and elbow function after surgical procedure. Most patients respond to classical transfers [41,42]. Tendon transfers are a routine procedure used to improve hand function in brachial plexus injuries; however, muscles from forearm donors are not always available for transfer. In this situation a distant muscle may be used.
Wrist extension is the first priority, even if all other muscles are paralyzed; it provides automatic finger flexion by tenodesis effect when the wrist is extended. Monreal [43] proposed an effective and simple procedure (extensor dynamic tenodesis) to restore grip function in patients with C5, 6, 7, and 8 nerve root lesions (Figure 4).
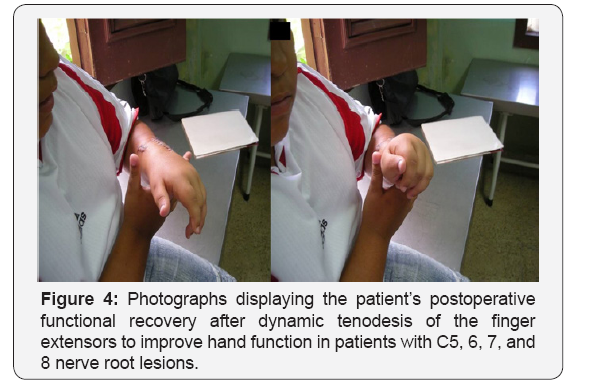
A valid strategy in the reconstruction of finger and thumb flexion and wrist extension after brachial plexus injury when forearm donor muscles are not available is to transfer the brachialis muscle to the forearm muscles [44]. In residual paralysis involving the C7-C8 and T1 nerve roots, the recovery of finger flexion is always incomplete or absent. Restoring active finger flexion is useful for finger flexion grasp. The pronator teres transfer is a good and reliable method for restoring finger flexion in a paralyzed hand after brachial plexus palsy when others options are not available [45] (Figure 5).

Conclusion
Neurolysis, nerve graft or nerve transfer in the early stage or tendon transfer and arthrodesis in the late stage after brachial plexus injury may result in a significant improvement of motor function of the upper limb.
References
- Thoburn W (1900) Secondary suture of the brachial plexus. Br Med J 1(2053): 1073-1075.
- Bonney G (1995) Prognosis in traction lesions of the brachial plexus. J Bone Joint Surg 41(1): 4-35.
- Seddon HJ (1963) Nerve grafting. J Bone Joint Surg Br 45: 447-461.
- Barnes R (1949) Traction injuries of the brachial plexus in adults. J Bone Joint Surg Br 31: 10-12.
- Allieu Y (1975) Exploration et traitement direct des lesions nerveuses dans les paralysies traumatiques par elongation du plexus brachial chez l'adulte. Rev Surg Orthop 63:107-122.
- Millesi H (1977) Surgical management of brachial plexus injuries. J Hand Surg Am 2: 367-378.
- Narakas AO (1978) Surgical treatment of traction injuries of the brachial plexus. Clin Orthop 133: 71-90.
- Jamieson A, Hugues S (1980) The role of surgery in the management of closed injuries of the brachial plexus. Clin Orthop Relat Res 147: 210215.
- Alnot JY, Jolly A, Frot B (1981) Direct treatment of nerve lesions in brachial plexus injuries in adults: a series of 100 operated cases. Int Orthop 5(2): 151-168.
- Sedel L (1982) The results of surgical repair of brachial plexus injuries. J Bone Joint Surg Br 64: 54-66.
- Narakas AO (1985) The treatment of brachial plexus injuries. Int Orthop 9: 29-36.
- Comtet JJ, Sedel L, Fredenucci JF, Herzberg G (1988) Duchenne-Erb palsy. Experience with direct surgery. Clin Orthop 237: 17-23.
- Sedel L (1988) Repair of severe traction lesion of the brachial plexus. Clin Orthop Relat Res 237: 62-63.
- Bentolila V, Nizard R, Bizot P, Sedel L (1999) Complete traumatic brachial plexus palsy. Treatment and outcome after repair. J Bone Joint Surg Am 81: 20-28.
- Monreal R (2005) Surgical treatment of brachial plexus injuries in adults. International Orthopaedics 29: 351-354.
- Narakas A, Hentz V (1988) Neurotization in brachial plexus injuries. Indications and results. Clin Orthop 237: 43-56.
- Tsuyama N, Hara T (1973) Intercostal nerve transfer in the treatment of brachial plexus injury of root avulsion type. In: Delchef J, de Marneffe R, Vander Elst E, (Eds.), Orthopaedic surgery and traumatology. International Congress Series No. 291. Amsterdam: Excerpta Medica, pp. 351-353.
- Allieu Y, Cenac P (1988) Neurotization via the spinal accessory nerve in complete paralysis due to multiple avulsion injuries of the brachial plexus. Clin Orthop 237:67-74.
- Monreal R (2007) Restoration of Elbow Flexion by Transfer of the Phrenic Nerve to Musculocutaneous Nerve after Brachial Plexus Injuries. HAND 2: 206-211.
- Yamada S, Peterson GW, Soloniuk DS (1991) Coaptation of the anterior rami of C-3 and C-4 to the upper trunk of the brachial plexus for cervical nerve root avulsion. J Neurosurg 74(2): 171-177.
- Oberlin C, Beal D, Leechavengvongs S, Salon A, Dauge MC, et al. (1994) Nerve transfer to biceps muscle using a part of ulnar nerve for C5-C6 avulsion of the brachial plexus: Anatomical study and report of four cases. J Hand Surg 19: 232-237.
- Hou Z, Xu Z (2002) Nerve transfer for treatment of brachial plexus injury: Comparison study between the transfer of partial median and ulnar nerves and that of phrenic and spinal accessory nerves. Chin J Traumatol 2002: 263-266.
- Weber RV, Mackinnon SE (2004) Nerve transfers in the upper extremity. J Am Soc Surg Hand 4: 200-213.
- Leechavengvongs S, Witoonchart K, Uerpairojkit C, Thuvasethakul P (2003) Nerve transfer to deltoid muscle using the nerve to the long head of the triceps, part 2: a report of 7 cases. J Hand Surg 28(4): 633638.
- T Carlstedt, P Grane, RG Hallin, G Noren (1995) Return of function after spinal cord implantation of avulsed spinal nerve roots. The Lancet 346: 1323-1325.
- T Carlstedt, P Grane, RG Hallin, G Noren (1995) Return of function after spinal cord implantation of avulsed spinal nerve roots. The Lancet 346: 1323-1325.
- T Carlstedt, P Anand, R Hallin, PV Misra, G Nor'en, et al. (2000) Spinal nerve root repair and reimplantation of avulsed ventral roots into the spinal cord after brachial plexus injury. Journal of Neurosurgery 93: 237-247.?
- E Rouholamin, JR Wootton, AM Jamieson (1991) Arthrodesis of the shoulder following brachial plexus injury. Injury 22(4): 271-274.
- B Elhassan, A Bishop, A Shin, R Spinner (2010) Shoulder tendon transfer options for adult patients with brachial plexus injury. J Hand Surg Am 35(7): 1211-1219.
- B Elhassan, A Bishop, A Shin, R Spinner (2010) Shoulder tendon transfer options for adult patients with brachial plexus injury. J Hand Surg Am 35(7): 1211-1219.
- AM Hendry (1949) The treatment of residual paralysis after brachial plexus injuries. J Bone Joint Surg Br 31(1): 42-49.
- RR Richards (1991) Operative treatment for irreparable lesions of the brachial plexus, in Operative Nerve Repair and Reconstruction. In: RH Gelberman, (Ed.), J. B. Lippincott & Company, Philadelphia, Pa, USA, pp. 1303-1327.
- Rühmann O, Wirth CJ, Gossé F, Schmolke S (1998) Trapezius transfer after brachial plexus palsy: Indications, difficulties and complications. J Bone Join Surg (Br) 80(1): 109-113.
- Karev A (1986) Trapezius transfer for paralysis of the deltoid. J Hand Surg (Br) 11: 81-83.
- Aziz W, Singer RM, Wolff TW (1990) Transfer of the trapezius for flail shoulder after brachial plexus injury. J Bone Joint Surg Br 72(4): 701704.
- Ruhmann O, Wirth CJ, Gosse F, Schmolke S (1998) Trapezius transfer after brachial plexus palsy: Indications, difficulties and complications. J Bone Join Surg (Br) 80(1): 109-113.
- Kotwal PP, Mittal R, Malhotra R (1998) Trapezius transfer for deltoid paralysis. J Bone Join Surg (Br) 80: 114-116.
- Monreal R, Paredes L, Díaz H, León P (2007) Trapezius transfer to treat flail shoulder after brachial plexus palsy. J Brachial Plex Peripher Nerve Inj 2:2.
- Steindler A (1918) A Muscle Plasty for the Relief of Flail Elbow in Infantile Paralysis. Interstate Med J 25: 235-241.
- Zancolli EA (1967) Paralytic supination contracture of the forearm. Journal of Bone and Joint Surgery 49(7): 1275-1284.
- Jones R (1916) On suture of nerves and alternative methods of treatment by transplantation of tendon. Br Med J 1(2888): 641-643.
- Merle d'Aubigne R, Deburge A (1967) Traitement des Paralysies du Plexus Brachial. Rev Chir Orthop 53: 199-215.
- Monreal R (2010) Dynamic Tenodesis of the Finger Extensors to Improve Hand Function after Brachial Plexus Injury. HAND 5: 256-260.
- Bertelli JA, Ghizoni MF (2006) Brachialis Muscle Transfer to Reconstruct Finger Flexion or Wrist Extension in Brachial Plexus Palsy. J Hand Surg am 31(2): 190-196.
- Monreal R, Navarro A (2013) Restoration of finger flexion by pronator teres muscle transfer after brachial plexus injury: a case report. HAND 8(3): 334-338.






























