Heat Treatment of Metal Implants Significantly Increases Their Osseointegration with the Host Bone
Roni Hazan1, *Uri Oron1 and Amir Oron2
1Department of Zoology, The George S. Wise Faculty of Life Sciences, Tel-Aviv University, Israel
2Department of Orthopedics, Kaplan Medical Center, Rehovot, Israel affiliated with the Hebrew University Jerusalem, Israel
Submission: March 17, 2017; Published: March 24, 2017
*Corresponding author: Uri Oron Ph. D, Department of Zoology, Tel –Aviv University, Tel-Aviv 69978, Israel, Tel:+972544303012; Fax:+97239503871;Email:oronu@post.tau.ac.il
How to cite this article: Roni H, Uri O, Amir O. Heat Treatment of Metal Implants Significantly Increases Their Osseointegration with the Host Bone. Ortho & Rheum Open Access 2017; 5(3): 555665. DOI: 10.19080/OROAJ.2017.05.555665
Abstract
Aim: To investigate whether heat treatment of Ti-Al-Va screw type implants prior to their insertion enhances the extent of osseointegration into the femur bone of rats.
Method: Heat- treated implants (incubation in 280 C in air prior to implantation were inserted in all rats into one femur while non-heat treated implants were inserted into the contralateral femur in the same rat. Femurs bearing the implant were fixed, embedded and sectioned longitudinally through the metal implant and the bone. The extent of osseointegration was evaluated using quantitative histological methods.
Results: It was found that the extent of osseointegration was significantly (3.5, 2.2 and 1.8 -fold ) higher at 6, 10, and 35 days, respectively around the heat treated implants as compared to the non-heat treated ones. At 35 days the osseointegration was 72 % of the implant surface length compared to only 41 % of the non-heat treated implants.
Conclusion: It is concluded that the heat treatment of implants prior to their insertion significantly enhances implant osseointegration with the host bone and thus may be of value in improving implant function in many clinical indication following trauma.
Introduction
Joint replacement by metal implants and the use of metal implants in general have become a mainstream in the fields of dentistry and orthopedics. The use of metal implants enables reconstructive surgery which in turn facilitates for better healing and rehabilitation. As the life span of the patients increases the use of these implants is constantly growing [1-4].
One of the major factors determining the long term functional success of the implants is their osseointegration with the host bone. In those implants that are inserted into long bones or jaws without the use of cement the osseointegration is dependent on the rapid bony in growth to the metal implant surface. Despite the high success rate of the implants conditions of limited- bone healing potential and immediate implant loading have stimulated research into various approaches by which to improve osseointegration. Implant surface modifications stimulating premature osteogenic cells may lead to enhanced peri-implant bone formation and implant osseointegration [1-5]. Experimental evidence has shown that surface roughness and functional surfaces affect the bony ingrowth to metal implants [3]. Other studies have demonstrated that nanofiberous hydroxyapatite made the implant surface osseoinductive [4]. Recently quantitative evidence was reported for the biochemical bond theory of osseointegration with bioactive surface oxide chemistry [6]. The growth of connective tissue as an interface layer between the metal implant and the host bone is bound to fail over time due to the reduction in bonding strength of the implant into the host bone and hence the imminent failure of load transfer leading to implant loosening and eventual failure. We have previously found that heat treatment of implants in an oxygenated environment increases the metal oxide surface layer of the treated implants and led to a swifter integration process of the metal implant into the host bone [7-9]. It was found that the thicker oxide layer over the heat treated implants enhances alkaline phosphate enzymatic activity in the osteoblasts adjacent to these metal implants as compared to the non-heat treated metal implants [7,8]). In addition, calcium accumulation and kinetics of bone formation were enhanced around the heattreated implants as revealed by histology following implant removal. Recently, we have shown that heat treatment in combination with partial deposition of hydroxyapatite onto the implants prior to their insertion caused a significantly better anchorage between the implant and the bone than heat treatment or hydroxyapatite deposition alone [10].
However, the direct osseointegration, bone formation, and interface characteristics between the implant and bone and the heat- treated (HT) implants compared to the non- heat treated (NHT) ones was not explored. The aim of the present study was to quantitatively measure osseointegration and interface characteristics of NHT and HT implants over time post insertion to the bone marrow of the femur in the rat.
Materials and Methods
Experimental procedure
Eighteen Sprague Dawley rats (Harlan Inc, Rehovot, Israel) (3-4 months old, 250-300 grams in weight) were utilized for this study. The rats were kept under 12hrs/12hrs day/night regime and 60% humidity. Water and food was given ad libitum. The experiment was approved by Internal Committee of Faculty of Life Sciences, Tel Aviv University.
Six rats were used for each time interval (6, 10 and 35 days) post implant insertion. Screw implants made of Ti-Al-Va alloy underwent through passivation and were HT or NHT as described by us previously [7.8]. Following passivation and washing in distilled water implants were placed in a temperature controlled glass tube covered by heating pad. The tube was heated to 280 C for 3 hrs in air. Temperature was constantly recorded and kept stable. Following cooling to room temperature the implants were then sterilized with gas and were kept sterilized until surgical procedure. The implants were inserted into the bone marrow cavity of rat femurs as described by us previously (8). Conscious rats were anesthetize with Avertine (1ml/100 gr body weight) using an 18 gauge 1 inch long needle to by intraperitoneal approach. A small entry hole was made in the distal part of the femur in the knee joint. This was followed by slight widening of the intracondylar groove of the joint in the distal femur. The screw was inserted in a retrograde fashion along the axis of the femur. The screw head was situated in the intracondylar groove of the distal femur [8,9] at the end of surgical procedure so that the motion in the knee joint was not be disturbed. In each rat the HT screw implant and NHT implant were inserted randomly in the same rat in regard to which side was chosen as HT vs. NHT in order to minimize variability in bone growth capacity to implants between rats. At one and four days prior to sacrifice the rats received an intraperitoneal injection of tetracycline in saline.
Six rats per each time interval (6, 10 and 30 days post implant insertion) were euthanized by overdose of barbiturates (150mg/Kg) and the femurs with the implants were transferred to a 70% alcohol solution for 10 days. The femurs were then washed and embedded in methylmetacrylate. Both femurs were then carefully cut in the medial plane longitudinally (bone and metal) using a diamond power saw.
The osseointegration in each metal implant was analyzed by observation of the histology-metal integration of each screw implant. The extent of osseointegration was analyzed in each screw at a X20 objective magnification. The length of complete osseointegration out of the total length of the surface in each screw cross section interface (16 threads) was calculated using SigmaScan software (Sigma, St. Louis, USA). This procedure was performed on all screws in the HT and NHT groups. The extent of osseointegration of all screws (HT or NHT) at each time interval was then statistically analyzed using ANOVA SigmaStat software (Sigma, St. Louis, USA).
Results
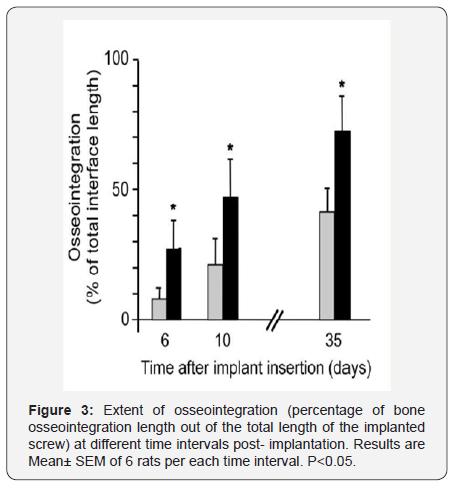
There was a gradual increase in the extent of osseointegration with time in both NHT and HT implants. However, at each time interval post- implant insertion into the femurs there was a significantly higher extent of osseointegration in the HT implants relative to the NHT implants.
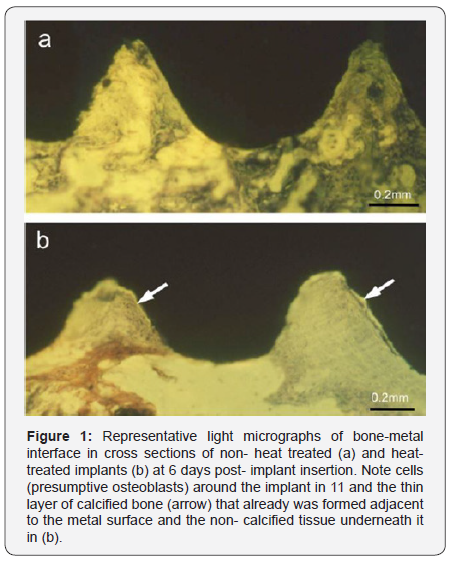
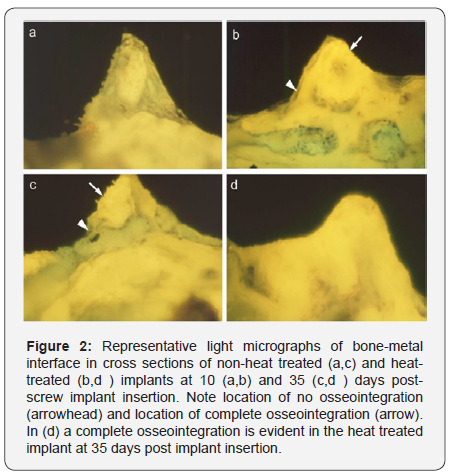
The histological sections demonstrated infiltration of cells with minimal calcified matrix in the groves between the threads of the screw implant at 6 days post implant insertion. However, a thin layer of calcified tissue was present in close contact with the metal implant surface already at this time interval in the HT implants (Figure 1). At 10 and then at 35 days postimplant insertion further calcification was evident with greater calcification and osseointegration in the HT implants than in the control ones. The histology revealed a thin bony line in closed contact to the metal implant surface at 6 days post implantation in the HT implants but not in the NHT implants where connective tissue was present. In the 10days time interval there was a progressive bony growth to a higher extent to the metal surface in the HT than in the NHT implants. At the 35 day time interval a newly formed bone was evident in the grooves of the screw like implant and an almost complete osseointegration in the HT implants relative to partial osseointergration in the NHT implants (Figure 2). The extent of osseointegration ( as defined in the Materials and Methods section) was significantly (p.>0.05 ) 3.5, 2.2, and 1.8- fold higher at 6, 10, and 35 days respectively, around the HT implants as compared to the NHT ones (Figure 3).
Discussion
Demography
The results of the present study indicate that at all time intervals post implant insertion there was a significantly higher extent of osseointegration between the bone and inserted implant. It can be seen that the extent of osseointegration increased between 6 and 10 days post- implantation and then continued toincrease to a lesser extent up to 35 days post implant insertion. Our results corroborate previous results that demonstrated that heat treatment prior to insertion significantly enhances the pull- out force of screw implants in the same rat model as compared to NHT screw implants [7,8]. The results are also in accordance with our previous study that indicated there was a higher alkaline phosphatase activity (indicating osteoblastic activity) and calcium content in the newly- formed tissue adjacent to the metal implants [8]. The results also corroborate our previous publication regarding the significant increase in shear strength in the rat femur of stainless steel and Ti-Al-Va screw implants when the implants were HT prior to their insertion, as compared to NHT implants. The results of the present study indicate that enhanced bone growth to the implants indeed contributes to their osseointegration with into host bone. Thus it can be postulated that heat treatment not only affects the growth rate and maturation of bone around the implant but also the consequent result of this process which is the osseointegration of the host bone with the metal surface with no connective tissue or collagen in the interface between bone and the implant . It may be postulated that the change in the surface chemical characteristics of the HT implant (increase in titanium oxide layer) [7,8] also affects the response of the adjacent tissues to it by enhancing osteoblasts activity and bone deposition onto the metal implant. Furthermore it may be assumed that the change in the surface layer of the implants by the heat treatment [7,8] causes a more rapid bone deposition onto them and prevents connective tissue deposition in the interface between implant and host bone. This is indeed evident in the histology of the interface presented in this study. Indeed, it was postulated previously that connective tissue deposition at the interface may eventually contribute to the functional failure of the metal implants.
The results of the present study have also direct clinical relevance. In orthopedics, dentistry and trauma the need for fast bonding between implants and host bone is crucial for reconstruction of the injured organs with the aid of various metal implants. Thus the simple procedure suggested here of heat treatment prior to insertion may give an added value to the functional performance of the skeleton following trauma. In conclusion, heat treatment of metal implants prior to their insertion causes a better bonding between the metal implants and the host bone, in correlation with our previous studies [7-9] indicating enhanced bone growth to the HT implants inserted into host bone.
Acknowledgement
The authors wish to thank Ms Varda Wexler for help with micrographs and drawings and Ms Naomi Paz for editing the manuscript.
Comments
Background
The use of metal implants for reconstructive surgery have become a mainstream in the fields of dentistry and orthopedics. One of the major factors determining the long term functional success of the implants is their osseointegration with the host bone in those implants that are inserted into long bones or jaws without the use of cement. Osseointegration depends on the rapid bony in growth to the metal implant surface .It was shown that one of the factors affecting the bony in growth to metal implants is the implants surface chemical characteristics. Heat treatment that alters the thickness of the oxide layer on the surface of the metal implant was found to enhance bony in growth to the implants and increase the bonding strength between the host bone and the implant.
Research frontiers
The current study demonstrate the actual enhanced osseointegration between HT implants and host long bone in hind leg of the rats as compared to NHT implants using histological methods.
Innovations and breakthroughs
The current study demonstrates a novel approach in the field of implant –bone interaction by simple treatment of the metal implants that affect their surface oxide layer rather than trying to affect the bone growth using drugs or other means to enhance the bony in growth to the implant. In the current study we show for the first time direct significant improved osseointegration by heat treatment using histological methods.
Applications
The novel approach to heat treat the metal implants prior to implantation in order to increase their bonding strength to host bone has a very significant broad impact in orthopedics and dentistry. The process of the heat treatment is simple and does not alter the biomechanical characteristics of the implant andseem to be safe. Thus the current study is valuable in clinical studies to implement the novel approach and improve the functional performance of the skeleton following implantation of metal implants.
Study Approval
The experiment was approved by internal Committee of Faculty of Life Sciences, Tel Aviv University
Author Contribution
R.H. and U.O designed and performed the study, A.O. designed and performed the study and wrote the manuscript.
References
- Sul Y-TH, Kwon D, Kang BS, Oh SJ, Johansson C (2013) Experimental evidence for interfacial biochemical bonding in osseointegrated titanium implants. Clin Oral Impl Res 24 Suppl A 100: 8-19.
- Hench LL (1998) Biomaterials: a forecast for the future. Biomaterials 19(16): 1419-1423.
- Wennerberg AI, Albrektsson T (2009) Effects of titanium surface topography on bone integration: a systematic review. Clin Oral Implants Res 20 Suppl 4: 172-184.
- Ma XY, Feng YF, Ma ZS, Li X, Wang J, et al. (2014 ) The promotion of osteointegration under diabetic conditions using chitosan/ hydroxyapatite composite coating on porous titanium surfaces. Biomaterials 35(26): 7259-7270.
- Chaudhari A, Duyck J, Braem A, Vleugels J, Petite H, et al. (2013) Modified titanium surface-mediated effects on human bone marrow stromal cell response. Materials 6(12): 5533-5548.
- Albrektsson T, Branemark PI, Hansson HA, Lindstrom J (1981) Osseointegrated titanium implants. Requirements for ensuring a longlasting, direct bone-to-implant anchorage in man. Acta Orthop Scand 52(2): 155-170.
- Hazan R, Brener R, Oron U (1993) Bone growth to metal implants is regulated by their surface chemical characteristics. Biomaterials 14(8): 570- 574.
- Hazan R, Oron U (1993) Enhancement of bone growth to metal implants inserted to the medullary canal of the femur in rats. J Orthop Res 11(5): 655-663.
- Hazan R, Oron U (1991) Bone growth around a metal implant inserted to the medullary canal: a new experimental model in the rat. Clin Mater 7(1): 45-49.
- Oron A, Agar G, Oron U, Stein A (2012) Enhancement of bony in-growth to metal implants by combining controlled hydroxyapatite coating and heat treatment. J Biomed Mater Res A 100(7): 1668-1672.






























