Treatment of a Transolecranon Fracture with Acute Osteochondral Bone Loss using Autologous Tricortical Bone Graft - A Case Report
*Dias Carlos Maia, Moita Miguel Brites, Branco Pedro Martins, Martinho Goncalo, Oliveira Manuel Augusto, Silva Antonio Julio
Department of Orthopedics and Traumatology, CUF Santarem Hospital Santarem, Portugal
Submission:February 15, 2017; Published: March 10, 2017
*Corresponding author: Dias Carlos Maia, Department of Orthopedics and Traumatology, CUF Santarem Hospital, Rua Zeferino Brandao, 2005- 321 Santarem, Portugal,Email:carlosmaiadias@gmail.com
How to cite this article: Dias C M, Moita M B, Branco P M, Martinho G, Oliveira M A, et al. Treatment of a Transolecranon Fracture with Acute Osteochondral Bone Loss using Autologous Tricortical Bone Graft - A Case Report. Ortho & Rheum Open Access 2017; 5(2): 555658. DOI: 10.19080/OROAJ.2017.05.555658
Abstract
Transolecranon fractures are complex fractures of the elbow that require adequate stabilization of the fracture fragments and greater sigmoid notch restoration in order to achieve good clinical outcomes. In case of articular osteochondral bone loss there is an increased risk of osteoarthritis and fracture non union which make this goal dif1icult to achieve with simple osteosynthesis. The authors describe the use of an Autologous tricortical pelvic bone graft to address the intra articular bone loss, describing the surgical Technique and showing the end result at 3 years post op.
Keywords: Transolecranon; Fracture; Bone Defect; Autologous Graft
Introduction
Transolecranon fractures are characterized by a subluxation or complete dislocation of the ulno humeral joint and anterior displacement of the radial head relative to the capitellum, while Maintaining proximal radio ulnar congruence and also ulno humeral ligament integrity [1,2], which differentiates them from Monteggia and Monteggia like injuries [1]. Despite simple olecranon Fractures can be expected to have favorable outcomes, with over 96% of good results expected in The long term [3], joint incongruence and poor osteo synthesis are risk factors for arthritis [4], and Can lead to a poor outcome. In transolecranon fractures this pitfalls may pose a serious problem as they are generally highly comminutive fracture dislocations. In order to expect a good outcome, one Should use sound osteosynthesis principles with anatomic reduction of articular fragments and stable Restoration of the greater sigmoid notch [1,5,6], which sometimes is not possible. For those situations fragment excision has been described but literature fails to guarantee good and reproducible outcomes in all patients because proximal ulna shortening, greater sigmoid notch malreduction, instability, osteoarthritis and loss of extension strength can result in patient dissatisfaction, despite that in low demand patients it can be an option [7].
Case Description
.png)

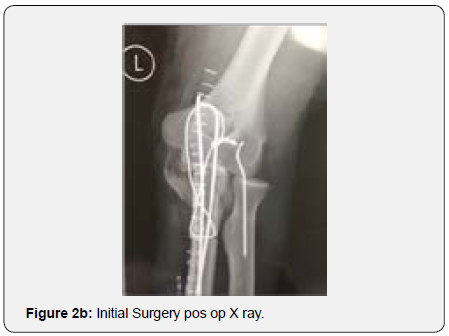
A 59 year old male sustained a working injury after falling from a ladder directly on to his left elbow. He was transported to the ER where he was diagnosed an exposed comminuted olecranon fracture (Figure 1a & 1b) (grade I Gustilo and Anderson/MayoIIIB) (information gathered from the hospital report). The patient had an olecranon surgical debridement and fracture stabilization with a figure of eight tension band construct associated with a trans radiocapitelar k Wire in the same day. Two days later the worker insurance company ordered his referral to our clinic. In the first evaluation the patient had no pain and no signs of neural or vascular injury in his left upper limb. He had a posterior incision and range of motion testing was not possible at that time because of the radiocapitelar fixation. Post operative X rays were performed showing a non reduced transolecranon fracture dislocation, with greater sigmoid notch bone loss but no injury to the coronoid process. He also had a subluxation of the radiocapitelar joint that had been inadequately stabilized with a K wire (Figures 2a & 2b).

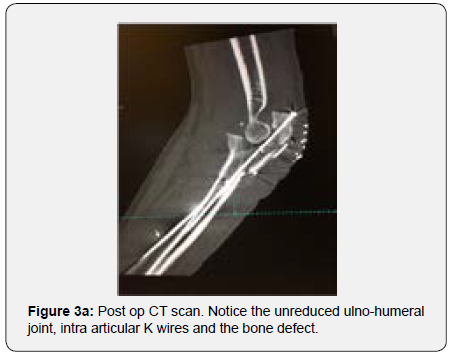
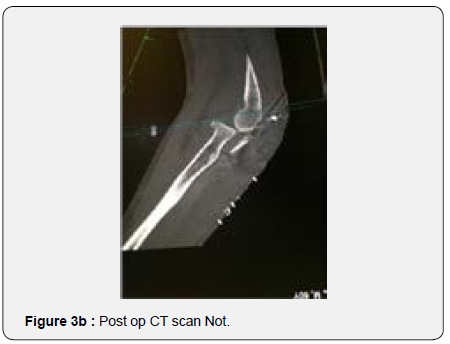
In order to better evaluate the injury and to plan corrective surgery, a CT scan was performed confirming the unreduced comminuted proximal ulna fracture and greater sigmoid notch bone loss with subsequent radio capital subluxation (Figures 3a & 3b) After disussing the case with the patient, decision was made to perform a surgical revision of the osteosynthesis using a tricortical iliac bone graft as the bone gap present seemed to prevent adequate articular stability and bone healing.
Under combined anesthesia (interscalene block + general anesthesia) while using a tourniquet, a posterior elbow approach was made using the previously performed incision. We were able to maintain a thick cutaneous and subcutaneous +lap and elevated the necessary proximal ulna muscle attachments in order to reduce and stabilize the fracture. No lateral ligament injury was noticed. We removed all the osteosynthesis material and confirmed in loco that there was a severe osteochondral bone loss of the greater sigmoid notch. After provisional fixation of the bone fragments with K wires (Figure 4), the ulno humeral and radiocapitelar joint were found to remain stable. We then performed a more rigid stabilization of the proximal ulna combining inter fragmentary screw fixation of the multifragmentary non articular proximal ulna fragments and bridge plating of the entire proximal ulna.
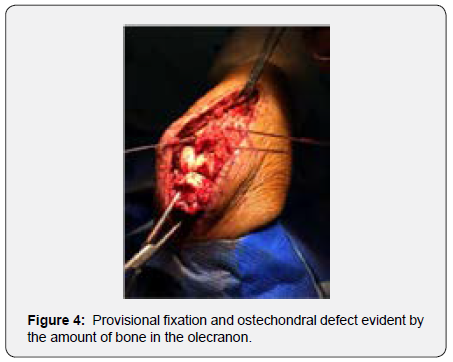
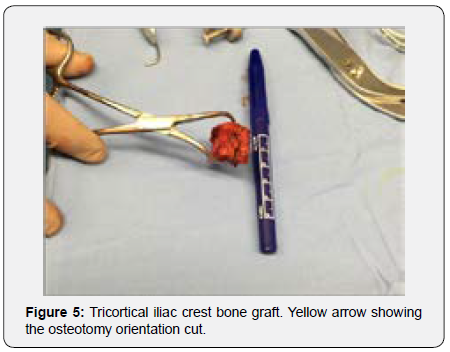
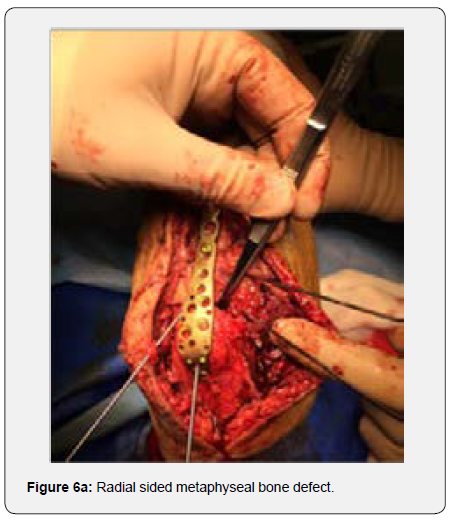

At this stage two bone defects were evident, one in the radial sided metaphyseal cortex and the other in the ulnar sided greater sigmoid notch, exposing a large area of the distal humeral trochlea. Bone contact was possible only at the posterior part of the ulnar fragments. Decision was made to collect atricortical iliac bone graft (Figure 5) and reshape it to fit both bone defects (Figures 6a & 6b). The pelvic sided curvature of the iliac bone graft seemed to adapt perfectly in the osteochondral bone defect (Figure 6C) and (Video1) while providing adequate bone stock to prevent non union. After fine reshaping, the graft was applied to bone defect while testing range of motion and graft stability (Video 2).
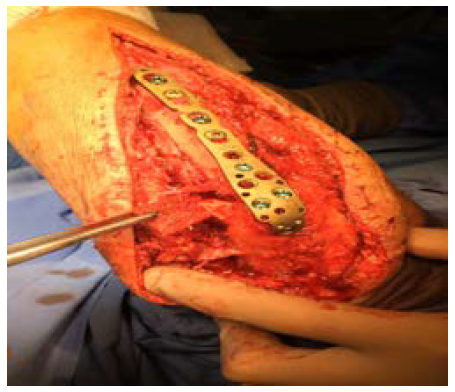

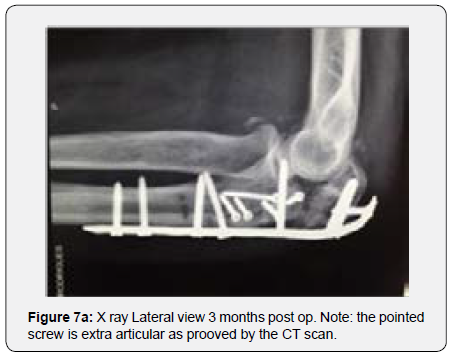
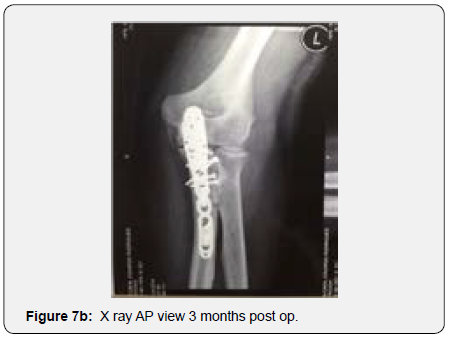
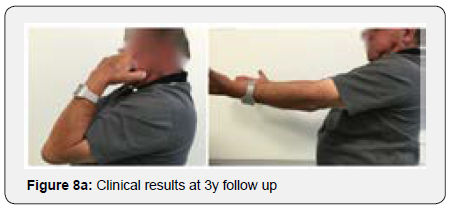
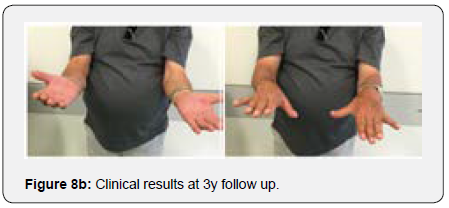
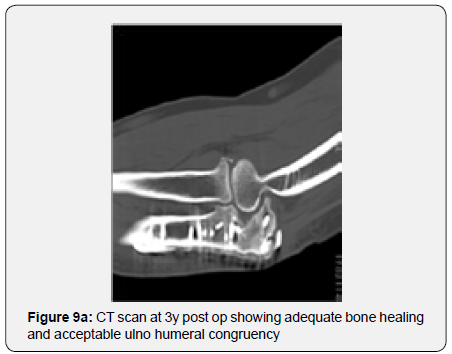
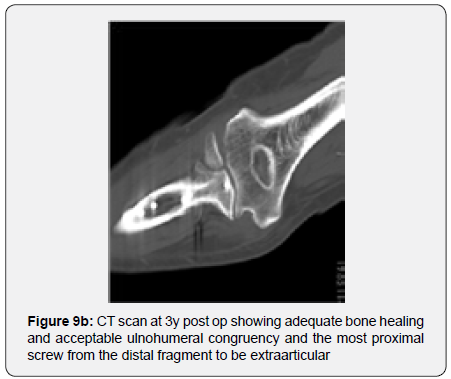
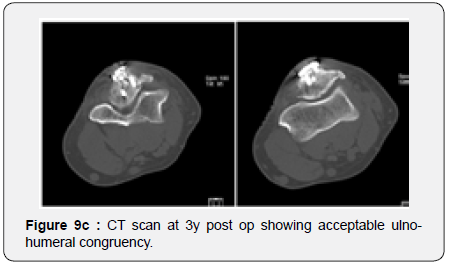
The remaining part of the bone graft was used in the non articular radial sided metaphyseal defect. The wound was then thoroughly irrigated and closed. The Patient was held in a cast for 2 weeks for soft tissue protection and from the 2nd to the 3rd Week he started passive range of motion exercises. After the 3rd Post operative week, the patient enrolled a physical therapy rehabilitation program, not directly controlled by the surgeon. At 3 Months post op the patient had regained adequate range of motion (flexion 120, extension15º, prono supination 90-0- 90º) and the x ray showed a stable elbow with graft integration and greater sigmoid notch articular congruence despite some heterotopic bone ossification/calcification in the olecranon fossa that might preclude full extension (Figures 7a & 7b). The Patient returned to his work 5 Months after surgery. At 3 Years post op he has no pain and has a ROM (Flexion 140º, extension-15º, prono supination 90-0-90) that allows him to do all of his daily living activities (Figures 8a & 8b). His CT Scan shows the healed bone graft and adequate ulno-humeral congruency (Figures 9a & 9b), Despite some degenerative changes are evident. He achieved a Mayo Elbow Performance Score (7) of 100.
Discussion
This is the first Description of an acute proximal ulnar unstable fracture with osteochondral defect managed using tricortical autologous bone graft. This is especially important because the defect involved an articular segment and the authors used a non osteochondral graft, easier to collect and with apparent good clinical and imagiological results. If Local osteochondral fragments are not amenable for reconstruction, using tricortical iliac bone graft seems to be an adequate option as it allows the restoration of ulnar length and articular surface congruency as this case clearly demonstrated. This technique relies on the adaptation of the bone graft to the bone defect by its fine Contouring and adequate stabilization with inter fragmentary positional screws and bridge plating. Other Report [8] Described a similar technique but for a malunited and shortened comminuted proximal ulna fracture with good results. Mortazavi et al. [9] In their case series (8 patients)also mention the use of tricortical iliac bone graft to treat sigmoid notch bone defect in one patient but they don’t describe the technique used nor the specific end result, despite showing performance scores of 88/100(average) .
With our report, along with the previously mentioned ones, we can state that for severely comminuted olecranon or transolecranon fractures, the use of a shaped cortical iliac crest bone graft for parcial or complete defects in association with a stable fixation and early range of motion exercises can yield good results, saving fragment excision with ulnar shortening for salvage procedures in which the described technique can’t be used.
References
- Chan K, King G, Faber K (2016) Treatment of complex elbow fracture dislocations. Curr Rev Musculoskelet Med 9(2): 185-189.
- Ring D, Jupiter JB, Sanders RW, Mast J, Simpson NS (1997) Transolecranon fracture-dislocation of the elbow. J Orthop Trauma 11(8): 545-550.
- Karlsson MK, Hasserius R, Karlsson C, Besjakov J, Josefsson PO (2002) Fractures of the olecranon: a 15- to 25-year followup of 73 patients. Clin Orthop Relat Res (403): 205-212.
- Rommens PM, Kuchle R, Schneider RU, Reuter M (2004) Olecranon fractures in adults: factors influencing outcome. Injury Int J Care Injured 35(11): 1149-1157.
- Doornberg J, Ring D, Jupiter JB (2004) Effective Treatment of Fracture Dislocations of the Olecranon Requires a Stable Trochlear Notch. Clin Orthop Relat Res 429: 292-300.
- Scolaro JA (2014) Treatment of Monteggia and Transolecranon Fracture Dislocations of the Elbow A Critical Analysis Review. JBJS Reviews 2(1): e3.
- Morrey B, Shancez Sotelo J (2009) The Elbow and its disorders. Chapter 25/ Fractures of the Olecranon, USA pp. 389-400.
- Doornberg J, Marti RK (2009) Osteotomy and Autograft Lengthening for Intra Articular Malunion of the Proximal Ulna: A Case Report. Case Reports in Medicine, Hindawi Publishing Corporation, Egypt.
- Mortazavi SMJ, Asadollahi S, Tahririan MA (2006) Functional outcome following treatment of transolecranon fracture dislocation of the elbow. Injury, Int J Care Injured 37: 284-288.






























