Diagnosis and Management of Partial Thickness Rotator Cuff Tears
*Saurabh Deore1, Milind Mehta2 and Sunil Garg3*
1Department of Medical, Norwich Medical School, University of East Anglia, UK
2Orthopaedic Surgeon, Isle of Wight NHS Trust, UK
3Consultant Orthopaedic Surgeon, James Paget University Hospital, Great Yarmouth, UK
Submission: November 24, 2016; Published: December 09, 2016
*Corresponding author: Saurabh Deore, Medical Student, Norwich Medical School, University of East Anglia, UK, 40 Dereham Road, Norwich, NR5 0SY, UK Mr Sunil Garg, Consultant Orthopedic Surgeon, James Paget University Hospital NHS Foundation Trust, Lowestoft Road, Great Yarmouth, NR31 6LA , UK
How to cite this article: Saurabh D, Milind M, Sunil G. Diagnosis and Management of Partial Thickness Rotator Cuff Tears. Ortho & Rheum Open Access J. 2016; 4(1): 555626 DOI: 10.19080/OROAJ.2016.04.555626.
Abreviations
PTRCT: Partial-Thickness Rotator Cuff Tears; ATI: Autologous Tenocyte Implantation; ASES: American Shoulder and Elbow Surgeons; UCLA: University of California, Los Angeles.
Introduction
Shoulder pain is a common cause of morbidity in the society with surveys showing that 9-26% of the adult population being affected at a point in time [1]. It is the third most common cause of musculoskeletal pain in community after back and knee pain. Shoulder pain usually indicates an underlying shoulder, neck or nerve pathology. Shoulder conditions causing pain can be broadly divided originating from rotator cuff disease, biceps tendon disease, acromioclavicular joint disease and glenohumeral pathology of adhesive capsulitis or arthritis [2].
In the subtype of rotator cuff disease, rotator cuff tendinopathy, subacromial bursitis, partial-thickness rotator cuff tears (PTRCT) and full thickness tears are the common cause of pain and disability. The major cause of these conditions has been attributed to degenerative changes that come along with ageing. Full thickness rotator cuff tears have been studied, well recognized and managed very effectively. In contrast, the diagnosis and treatment of PTRCTs remains controversial. The purpose of this article is to define partial thickness tears, classify them, and discuss the pathophysiology, diagnosis and their management.
Anatomy
The rotator cuff is made up of 4 tendons - supraspinatus, infraspinatus, subscapularis and teres minor that arise from the scapula. The muscles move towards the humerus and along with ligaments and other muscles help in shoulder stability and mobility. Much like the other tendons majority of the cuff is formed by type 1 collagen with proteoglycans, elastin, glycosaminoglycan and water. The area known as ‘critical zone’ on the supraspinatus insertion has been said to have insufficient blood supply but in contrast Ultrasound Doppler studies have shown a normal supply in this region [3]. The insertion of the rotator cuff follows a consistent pattern. Each tendon attaches to a bony landmark on the humerus to create a footprint. The four tendons of rotator cuff splay out and interdigitateinto one tendon and insert onto the humeral head in a horseshoe shaped pattern. The supraspinatus has its insertion on the greater tuberosity.
Near its insertion the fibers of the supraspinatus and infraspinatus combine. The fibers of the subscapularis and supraspinatus enclose the biceps tendon. The subscapularis arises from the subscapular fossa and has its insertion on the lesser tuberosity beside the bicipital groove near the articular surface. Fibrous tissue originating from the coracohumeral ligament covers the anterior and bursal sides of the supraspinatus tendon. The infraspinatus surfaces from the infraspinatus fossa of the scapula and inserts on the greater tuberosity. Some of its fibers fuse with supraspinatus and some fuse with teres minor [3-5] (Figure 1).
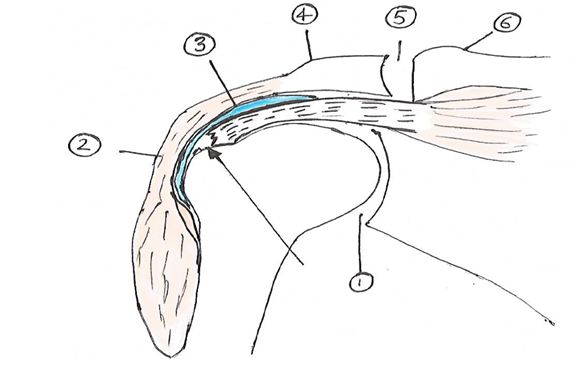
The superior insertion of the rotator cuff called the rotator cable looks like a thickened part of the capsule when seen from the glenohumeral joint. The cable is a deep extension of the coracohumeral ligament and made of fibrous tissue. This surrounds a thinner tissue area, consisting of the distal portions of supraspinatus and infraspinatus, called the crescent region that has its insertion onto the greater tuberosity. This crescent region is contained within an avascular zone [6]. Most partial thickness tears tend to occur in this region. This rotator cablecrescent complex is believed to have stress-shielding properties (Figure 2).

The tendons of the supraspinatus and infraspinatus interdigitate in the posterior half of the supraspinatus tendon [7]. Recent study suggested that the footprint of the supraspinatus was smaller than previously thought. The average maximum lengths reported were 6.9 mm, medial to lateral, and 12.6 mm anteroposterior. It was shown that area of the greater tuberosity was actually occupied by a trapezoidal infraspinatus tendon which was also larger than previously estimated. The average maximum lengths reported were 10.2 mm, medial to lateral, and 32.7 mm anteroposterior. Thus accounting for the high frequency of infraspinatus involvement even in previously thought isolated supraspinatus tear [8].
Classification
- In 1983 the Neer classification described rotator cuff disease in 3 stages of impingement, with rotator cuff tears being classed in the final (3rd) stage. Partial thickness rotator cuff tears can be classified on three different bases - where they are located (articular, bursal or intratendinous), which tendon of the rotator cuff has been affected (supraspinatus, infraspinatus, teres minor or subscapularis) and the size of the tendon tear, calculated as a percentage of the thickness of the tendon [9].
- The Ellman classification is based on arthroscopic intraoperative findings. A grade 1 tear is <3mm deep, a grade 2 tear is 3-6mm deep and not more than 50% the tendon thickness and a grade 3 is >6mm in depth or more than 50% of the tendon thickness [10]. This system has been simplified into two categories, <50% or <6mm and >50% or >6mm. This classification is widely used to determine the treatment regime.
- The Snyder [11] classification described the location, degree and size of the tear. The location being articular, bursal or complete tears. PTRCTs were then further subclassified as normal, grade 1, 2, 3 or 4. Grade 1 representing synovial irritation or capsular fraying in a small localised area usually less than 1 cm. Grade 2 - a lesion with fraying and failure of some rotator cuff fibers along with synovial, bursal or capsular injury in an area of less than 2 cm. Grade 3 - more severe rotator cuff injury with fragmentation of the tendon fibers in an area less than 3cm. Grade 4 - very severe injury with a sizeable flap, usually larger than 3cm, and involves more than one tendon [12].
- The Ellman and Snyder classification both did not cover intratendinous tears and were intended mainly for arthroscopic examination.
- Habermayer proposed a new arthroscopic classification of articular-sided supraspinatus tears which includes determining the tear size, similar to the older classifications, and also includes classification of the tear size and location in the sagittal and coronal plane. This system however does not include bursal sided and intratendinous tears [10,11].
- The Ellman classification is the most widely used and accepted despite other systems being introduced (Figures 3 & 4) (Table 1).
- The Habermayer classification of partial thickness tears in the coronal plane. Longitudinal extension of articular sided supraspinatus tears in coronal plane. Type 1 tear is a small tear at changeover from cartilage to bone. Type 2 tear is a tear in the centre of the footprint and Type 3 is an extension of the tear to the greater tuberosity .
- The Habermayer classification of partial thickness tears in sagittal plane. Sagittal extension of articular supraspinatus tendon tears in transverse plane. The Type A tear is the tear in the coracohumeral ligament that continues into the medial border of the supraspinatus tendon. Type B tear is a tear isolated within the crescent zone. A type C tear is a tear extending from the lateral border of the pulley system over the medial border of supraspinatus tendon up to the area of crescent zone [10,11].



Incidence
It has been known that the true prevalence of partial tears is much more than usually reported as the many of the people who have the tears are asymptomatic [13]. Cadaveric and imaging studies have shown that the prevalence of PTRCTs lies in the range of 13% - 32% and co-relates with the patients age significantly, p < 0.05. This has been supported by a MRI study showing a 20% overall prevalence of partial thickness tears in all age groups. However the prevalence of partial thickness tears in age group more than sixty was 26%, age group forty to sixty was 24% and age group nineteen to thirty-nine years old was only 4% [14].
Reilly et al. [15] reported that 18.5% of the 2553 cadaveric shoulders studied had partial thickness rotator cuff tears. A study of 249 cadaveric supraspinatus tendons revealed that 7% had a full thickness tear whereas 13% had PTRCTs (2.4 % bursal sided, 3.6% articular sided and 7.2% intratendinous tears), suggesting the prevalence of partial thickness tears to be more than that of full thickness tears [8,16] Amongst the three types of partial thickness tears intratendinous tears have been reported to be the commonest, with a cadaveric study reporting 55% of all PTRCTs to be intratendinous tears [17]. Articular sided tears have been reported to be 2-3 times common than bursal sided tears.
It has been proposed that the cause for this in older patients is an area of hypo vascularity on the articular side that runs from the musculotendinous junction to within 5mm of its insertion. The supraspinatus tendon has the highest incidence of tearing amongst the four rotator cuff tendons [18]. Thus tears commonly present on articular side of the supraspinatus tendon [19,20]. A study with senior athletes, aged over 60, showed that the prevalence of partial thickness was greater in the athletes than in the general population of the same age [21]. Overall these results illustrate the importance of age as being an important factor in the prevalence of partial thickness rotator cuff tears.
Pathology
The pathology leading to the formation of PTRCTs is multifactorial. This can be intrinsic, extrinsic or traumatic [8]. Intrinsic factors include age related changes such as hypo cellularity, fascicular disruption, fascicular thinning, granulation tissue formation, dystrophic calcification and decreased vascularity and metabolic changes. Extrinsic factors include subacromial impingement, internal impingement, glenohumeral instability and trauma [22-24]. Many studies have look at changes at a microscopic level as well as the strain patterns. Fukuda et al. [25] looked at 12 specimens with bursal-sided rotator cuff tears. Along with degeneration they noted disruption in the normal layer and increased vascularity at the site of tendon insertion. Whereas the proximal stump was relatively avascular and rich in chondrocytes.
The superior shoulder capsule attaches to a large area (30%-61%) of the greater tuberosity. The capsule lies below the supraspinatus and infraspinatus tendons which also attach to the the superior shoulder capsule and increase the likelihood of joint laxity. Biomechanical studies [17,26-28] have pointed out that that presence of PTRCTs alters the strain patterns within the remaining healthy tendon thus predisposing it to tear propagation [29]. A cadaveric study reported that pathologic and structural changes on the under surface of the acromion were associated with bursal sided tears. The incidence of acromial spurs has been reported to the highest in bursal sided tears. In a study where all patients presenting with impingement signs and sub acromial bursitis had type II or III acromion suggesting that subacromial impingement to be a significant cause for bursal side tears [30].
Majority of strain studies on intact tendons have reported that the strain in greater on the bursal side than on the articular side. It has been contemplated that the difference in the strain patterns contributes to a greater tear propagation in bursal sided infraspinatus tears. This can cause clinical consequences such that the bursal sided tears are harder to treat with physical therapy (conservative). This was tested on sheep tendons. However, in a study in human supraspinatus tendons a similar pattern was observed where the transverse stiffness was greater on the bursal side than the articular side [31]. Many other factors are being proposed in development of PTRCTs as more research is done. A risk factor for a partial thickness tear was suggested to be a tear in the contra lateral shoulder.
The study showed that people with surgically treated rotator cuff tears had a higher prevalence of tears or a lack of functioning of in the contra lateral shoulder [12] Biopsies done on nine PTRCT of the supraspinatus tendon, compared with healthy subscapularis tendon, showed increased density of apoptotic p53+ tendon cells. This may relate to the healing process and has been suggested as a possible therapeutic target in the future [32]. A recent study ruled out any co-relation between macrovascular disease, atherosclerosis, and rotator cuff tears suggesting that vascular pathology is not a cause for rotator cuff disease or if it is then it is likely to be microvascular [33]. Collectively partial thickness rotator cuffs are caused by a combination of many factors. These factors are mostly age related but can also be due to extrinsic factors. It can be noted that conservative treatment may be a factor for poor prognosis of PTRCTs, however recognition of newer factors be of therapeutic significance in the future.
Diagnosis
The diagnosis is based on patient’s presentation, physical examination and the use of diagnostic imaging.
Clinical history and Examination
The patient’s usual presentation is with pain and discomfort. But this can widely vary in every patient with some complaining of chronic pain, shoulder instability and decreased throwing speed [34]. Examination of the shoulder can reveal painful arc syndrome, crepitus, impingement and loss of strength in the affected side [35]. This has a considerable overlap with other shoulder pathologies such as subacromial bursitis and with full thickness rotator cuff tears. Other tests done include the empty can test, full can test and drop arm test. A study found the sub acromial grind test consisting of positive palpable crepitus on passive internal and external rotation of the shoulder while abducted in the scapular plane to be useful in full thickness supraspinatus tears but not in partial thickness tears [36].
There has been a long standing association of rotator cuff pathology with the sub-acromial volume, however, a MRI study with 46 patients found no relationship between the two. Subacromial volume is not yet reliable to help diagnose a rotator cuff tear [37]. Clinical findings should prompt imaging studies to give a better idea of extent of the tear and location. It is also known that many tears can be asymptomatic and thus association with imaging can be decisive.
X-rays
Radiographs were used to look for possible causes for rotator cuff disease in the past. They did not show any abnormalities in acute phases but pointed out presence of subacromial spurs. They can also show degenerative changes in the greater tuberosity of the head of humerus. These can be changes such as osteophytes, subchondral cysts, sclerosis and osteolysis [38]. These could be potential causes for impingement of the rotator cuff.
Ultrasound and MRI scan
2-D sonography or ultrasound is a widely used technique in the diagnosis of rotator cuff tears, with accuracy between 87% and 96%. The use 3-D ultrasound has been reported to have a good inter-observer reliability in full thickness supraspinatus tears but not in partial thickness tears. 3-D ultrasound has also shown to have a 17.4% higher sensitivity than 2-D ultrasound. However, these studies are limited by the number of participants and more data is needed [39]. A study done comparing ultrasound and MRI concluded that there was no difference between the two. The ultrasound detected 68.4% whist MRI detected 63.2% of the partial tears. A meta-analysis done on 65 studies concluded that MR arthrography was more accurate than both MRI and ultrasound, whereas there was no difference between the sensitivity and the specificity for MRI and ultrasound.
Although it was also stated that ultrasound is more costeffective and would be time saving as well. In terms of MR arthrography, the risk of an invasive technique should always be considered [40]. The use of ultrasound in general is cheap and non-invasive however the diagnostic accuracy can be limited by the operator. The diagnosis of intratendinous tears has been pointed out to the most difficult to diagnose amongst the partial thickness tears. Their accuracy of diagnosis has improved with the different MRI sequences and arm positioning. The signals include the linear high signal, within the tendon, that is along the tendon direction and focal defect at tendon insertion that does not communicated with either side of the tendon. A study done diagnosed close to 79% of intratendinous tears [16]. Other techniques used include direct MR arthrography and indirect MR arthrography. Although direct MR arthrography is more accurate in general, it is also more invasive and causes radiation exposure.
Indirect MR arthrography uses paramagnetic contrast media and has shown a sensitivity of diagnosing supraspinatus and infraspinatus partial tears to be 84% and 86% respectively [41]. Some studies have reported better diagnostic accuracy of indirect MR arthrography over the conventional MRI that does not use contrast [42,43]. Another meta-analysis and a systematic review have reported no difference in the sensitivity and specificity of MRI and ultrasound scans, stating that ultrasound would be more cost effective [44]. MR arthrography however was more accurate in the diagnosis of partial and full thickness tears. Thus ultrasound has been recommended as the modality of use to recognize partial thickness tears but MR arthrography can be utilized if no other techniques provide a definitive diagnosis since this has the best sensitivity and specificity [40].
Arthroscopic
This allows a thorough assessment of tears with visualisation of the surrounding tissue and thus is the best known modality for diagnosis of bursal and articular sided tears. Once a diagnosis has been made the extent of the partial thickness tear needs to be determined. This has been done using the estimate of the bone exposed on the rotator cuff footprint with a reference shaver of a known size, which is then compared with existing anatomical, clinical and radiographic data which is used to generate a percentage. As this method is not accurate new methods have been suggested. The intra-articular depth guide is proposed to be used in bursal and articular sided tears.
It is a device made with two parts, an inner probe which measures the size of exposed footprint while the outer sleeve measures the tendon thickness. In a study on 8 cadavers it was found that the intra-articular depth guide was more accurate than the conventional method as it determined the total tendon thickness closer to the true anatomical measurements [45]. Arthroscopy is the gold standard in diagnosis of PTRCTs. However, this invasive procedure and generally performed concurrently with arthroscopic repair. Thus the findings from ultrasound or MRI along with history and examination should be used collectively to make a clinical diagnosis.
Treatment
Conservative management
Partial thickness rotator cuff tears are usually treated similar to those with cuff tendinopathy and subacromial bursitis. Patients are often advised to avoid aggravating activates, rest, apply heat modalities (ultrasound or heat), massage and take NSAIDs. In the early phases the use of steroid injections can be helpful, once the inflammation and pain is under control more exercises can be performed to increase muscle strength. Free weights and rubber bands can be used with progressive increase in resistance to increase strength [8]. A recent study concluded that 91% of patients treated conservatively were content with their treatment at 46 months of follow up. It was also observed that patients without any history of shoulder trauma, nondominant shoulder or tear less than 50% of tendon thickness were more likely to recover [46]. A clinical follow up study was done by Yamanaka and Matsumoto [47] on 40 patients with partial thickness articular sided tears, diagnosed with arthrography and managed conservatively.
Arthrography repeated at a mean of 412 days revealed a disappearance of the tear in 4 patients, reduction in size of the tear in 4 patients, larger tears size in 21 patients and progress to full thickness tears in 11 patients. Recently the use of hyaluronate injections has shown to be beneficial when compared to placebo but RCTs has found its effectiveness to be similar to that of steroids [48,49]. Further research needs to be done to look at the long term success of conservative management within groups with different factors such as age, intrinsic or extrinsic causes. Novel treatments such as ultrasound guided autologous tenocyte implantation (ATI), a bioengineered treatment, and platelet-rich plasma and stem cell injections are being looked into but need more research to be done before these could be implemented [50,51].
Surgical treatment
Usually surgical intervention is indicated if conservative management has failed to control patient symptoms in the past 6 months, however earlier intervention may be necessary if significant functional disability is present. Other factors that are likely to affect decision are the patient age, associated shoulder pathologies, occupation, activity level and the size of the tear [52]. Surgical treatment for PTRCTs includes debridement of the PTRCT with or without acromioplasty, arthroscopic management with trans-tendinous tear repair or conversion of the tear to a full thickness tear to be then repaired.
Debridement +/-Acromioplasty
Debridement with or without acromioplasty is usually performed in low grade tears or tears that are less than 50% the tendon thickness. Acromioplasty has shown to have good outcome in PTRCTs. Studies looking at debridement and sub-acromial decompression in PTRCTs have shown varying data with no clear benefit of one over the other. However the procedure seems to be more likely to be successful in certain types of patients. A study done on 43 athletes under the age of 40 with a follow up of 2 years showed variability in the results. Athletes with acute injuries compared to the athletes who suffered a traumatic partial thickness tears had better outcomes (86% vs 66% respectively) when treated with debridement. The number of athletes who returned to play was also significantly greater (19%) in the acute injuries group of patients [53]. A study in low grade tears showed no difference in bursal-sided and articular sided-tears.
Cordasco et al. [54] revealed good results in a study done on 77 shoulders but concluded that there was a significantly higher rate of failure in bursal-sided tears (29%) compared to articular-sided tears (3%) when treated with acromioplasty. Debridement and acromioplasty did not aid in healing of PTRCTs and the tears could potentially advance to form full thickness tears, this has been supported by Kartus et al where 34.6% of partial thickness tears had progressed to a full thickness tear after a follow up of 8.4 years [55]. This was in contrast to another study with acromioplasty and debridement which reported only 6.5% repairs that progressed into full thickness tears in patient with a mean age of 59.2 years [56]. A systematic review done on 16 studies concluded that debridement with or without acromioplasty had good outcomes in low grade tears but development of a further tear was a possibility [57]. It thus appears that debridement with or without acromioplasty has good outcomes for low grade tears and more likely to be useful in some patients but at the same time it does not prevent tear progression.
Tear conversion followed by repair
A widely used treatment of high grade bursal and articularsided PTRCTs involve its conversion to full-thickness tears followed by tendon repair. However this method is thought to cause a mismatch between the length-tension aspect of the tear and the healthy part of the rotator cuff and thus increase re-tear rate. Studies done to compare tear conversion in bursal and articular sided tears have shown similar results in terms of the outcome, with one study reporting an equal or better outcome in bursal sided tears compared to articular sided tears.
They did not shown any difference in the tear rates on follow ups [58,59]. A study done on 41 patients (42 shoulders) with high grade tears with an average age of 53 years reported 88% of complete repairs at 11 months. At follow up they observed that the average age of patient with progression to full thickness tear (62.6 years) was significantly higher compared to patient who did not have a tear progression (51.8 year) [60].
In situ repair
This involves leaving the bursal sided cuff untouched while just repairing the torn articular sided region and thus theoretically has an advantage over the tear conversion technique as some of the anatomy is preserved. However, it also been reported that the trans-tendon repair might have its flaws as it involves tying the bursal layer down and can cause overtightening of the bursal side. Newer studies have shown an all-inside technique with better post-operative results relating to the stiffness caused by over tightening [61]. Trans-tendon repair-This is a type of in situ repair technique widely used to treat articular sided tears. The trans-tendon repair techniques have shown good improvement in functional outcomes after surgery as well [62]. Castricini et al. treated 33 patients with trans-tendon technique with an average 33 month follow up and reported an increase of more than 100% in the constant score before and after the surgery.
Furthermore no post-operative tears were reported [63]. Procedures performed from the bursal side are without visualisation thus a new trans-tendon repair technique using arthroscopy and bursoscopy at the same time for partial thickness articular surface rotator cuff tears has been presented. It has better visualisation and thus reduces the probability of complications in surgery. However a larger study needs to be done [64]. The trans-tendon repair has been attributed to causing stiffness and thus newer techniques have been suggested. A study done on 20 patients with high grade tears reported high levels of success, only 1 patient not returning to their previous level of activity, when treated with a new allinside repair technique [63]. This high rate of repair has been supported by other studies [65,66] (Table 2).

Trans-tendon vs tear conversion
Many studies have looked at the differences in trans-tendon and tear conversion techniques. Biomechanical studies have shown a higher ultimate load failure in patients with transtendon repair compared to tear conversion in articular sided PTRCTs [15]. Kim et al. [67] compared the in situ repairs versus tear completion for partial thickness tears and concluded that there were increase functional outcomes and visual analogue score regardless of the technique used with no significant difference in the two procedures. However, the re-tear rate for bursal-sided tears was higher in group treated with tear conversion. The re-tear rate for articular sided PTRCTs was not different [67]. This was supported by another RCT that pointed out that both, trans-tendon repair and repair after tear conversion, had similar outcomes clinically and on imaging in articular sided PTRCTs [49].
Another systematic review on arthroscopic management of partial thickness rotator cuff tears concluded that there was no difference in the two techniques. However there was a worse prognosis in bursal sided tears than articular sided tears [59]. A meta-analysis comparing the two techniques in articularsided tears of more than 50% thickness found no difference in the ASES (American Shoulder and Elbow Surgeons) score but noted a lower re-tear rate in the trans-tendon repair. It was also recognised that the patients complained of more pain and had a slower recovery back to functionality after the trans-tendon repair [18]. Repair with tear conversion might have its own flaws as it requires sacrificing tendon that might be healthy. Furthermore, it is harder to restore the native tendon footprint in the anatomical position.
These factors can render this type of repair to fail [49,62]. It was also suggested how trans-tendon may have its flaws, where pulling the retracted tendon onto the footprint can cause tightening in the bursal side and thus cause mechanical changes. This has been attributed to the painful lengthy recovery time of these repairs and might also explain higher chance of developing stiffness in that shoulder [68]. Thus it can be inferred that the trans-tendon technique works better in articular sided tears which are more than 50% thickness, and in general has similar outcomes to tear conversion technique. Although it does appear that trans-tendon has a lower re-tear rate than tear conversion technique.
Double row vs single row repair
Double row suture-bridge rotator cuff repair is another technique that has been shown to be effective when compared to single row repair by many biomechanical studies. The former technique is shown to have more enhanced, pressurized contact area between the tendon and footprint and decreased gap formation. Recently there has been use of modified Mason- Allen single-row technique using triple-load anchors and a cohort study showed this method had similar re-tear rates and functional outcomes as the double-row suture bridge technique in bursal-sided PTRCTs. The benefit of the Mason-Allen singlerow technique being that it used lesser suture anchors [69]. The arthroscopic knotless inverted-mattress technique was shown to have a re-tear rate of 5% in PTRCTs after a retrospective cohort study of 1000 cases. This was however performed by a single surgeon [70].
It is still unsure if single-row or double row repair is better. There has been contrasting evidence as some studies report no difference, anatomically or clinically, whereas other studies suggest that double row repair has improved outcome. A metaanalysis of 7 studies reported no difference in the outcome score however there was a significant increase in imagingdiagnosed re-tear rates in the single-row repair [71]. A review of 6 studies reported lower re-tear incidence after double row repair compared to single row repair in partial thickness tears, however it also stated that the functional outcome (measured using American Shoulder and Elbow Surgeons (ASES) shoulder score, the Constant shoulder score, and the University of California, Los An¬geles (UCLA) score) were not better in any of the techniques [72].
Intratendinous tears
The surgical treatment of intratendinous tears has been rarely studied. They have been reported to be hard to diagnose using either ultrasound or MRI. A study done on intratendinous partial thickness tears which showed a high rate of healing after arthroscopic repair [16]. Uchiyama et al did a study on intratendinous tears and concluded that conservative therapy had no effect on the tear. However, the outcomes were satisfactory (ASES average score 91.0) in 18 out of the 19 patients when surgically treated with anterior acromioplasty, excision and tenorrhaphy of the tear [73].
Conclusion
The presentation of partial thickness rotator cuff is a common shoulder problem prevalent within many age groups.Although new classification systems have been suggested the older Ellman system remains to be used. The diagnostic techniques like ultrasound currently have shown good results and the accuracy is only going to get better with MR arthrography.
Currently, the management of partial thickness tears still remains controversial with the doubts over which patients to be treated conservatively or surgically and which type of surgery would be the most beneficial for the various factors such as age and type of tear. This would need further research with larger groups to establish firmer guidelines.
References
- M Urwin, D Symmons, T Allison, T Brammah, H Busby, et al. (1998) Estimating the burden of musculoskeletal disorders in the community: the comparative prevalence of symptoms at different anatomical sites, and the relation to social deprivation. Ann Rheum Dis 57(11): 649-55.
- Linaker CH, Walker-Bone K (2015) Shoulder disorders and occupation. Best Pract Res Clin Rheumatol 29(3): 405-423.
- Carr A, Harvie P (2005) Rotator cuff tendinopathy. In: Maffulli N, Renstro¨m P, Leadbetter WB, ed. Tendon injuries. London: Springer 101-18.
- Clark JM, Harryman DT (1992). Tendons, ligaments, and capsule of the rotator cuff. Gross and microscopic anatomy. J Bone Joint Surg Am 74(5): 713-725.
- Curtis AS, Burbank KM, Tierney JJ, Scheller AD, Curran AR (2006) The insertional footprint of the rotator cuff: an anatomic study. Arthroscopy 22(6): 609.
- Burkhart SS, Esch JC, Jolson RS (1994) The rotator crescent and rotator cable: an anatomic description of the shoulder’s “suspension bridge”. Arthroscopy 9(6): 611-616.
- Andarawis-Puri N, Ricchetti ET, Soslowsky LJ (2009) Interaction between the supraspinatus and infraspinatus tendons: effect of anterior supraspinatus tendon full-thickness tears on infraspinatus tendon strain. Am J Sports Med 37(9): 1831-1839.
- Mochizuki T, Sugaya H, Uomizu M, Maeda K, Matsuki K, et al. (2008) Humeral insertion of the supraspinatus and infraspinatus. New anatomical indings regarding the footprint of the rotator cuff. J Bone Joint Surg Am 90(5): 962-969.
- Fukuda H (2003) The management of partial-thickness tears of the rotator cuff. J Bone Joint Surg Br 85(1):3-11.
- Ellman H (1990) Diagnosis and treatment of incomplete rotator cuff tears. Clin Orthop Relat Res 254: 64-74.
- Belangero, Paulo Santoro, Benno Ejnisman, Guillermo Arce (2013) “A Review of Rotator Cuff Classifications in Current Use”. Shoulder Concepts: Consensus and Concerns 2013: 5-13.
- Habermeyer P, Krieter C, Tang KL, Lichtenberg S, Magosch P (2008) A new arthroscopic classification of articular-sided supraspinatus footprint lesions: a prospective comparison with Snyder’s and Ellman’s classification. J Shoulder Elbow Surg 17(6): 909-913.
- Liem D, Buschmann VE, Schmidt C, Gosheger G, Vogler T, et al. (2014) The prevalence of rotator cuff tears: is the contralateral shoulder at risk? Am J Sports Med 42(4): 826-830.
- Sher JS, Uribe JW, Posada A, Murphy BJ, Zlatkin MB (1995) Abnormal findings on magnetic resonance images of asymptomatic shoulders. J Bone Joint Surg Am 77(1): 10-15.
- Reilly P, Macleod I, Macfarlane R, Windley J, Emery RJ (2006) Dead men and radiologists don’t lie: a review of cadaveric and radiological studies of rotator cuff tear prevalence. Ann R Coll Surg Engl 88(2): 116-121.
- Graeme Matthewson, Cara J. Beach, Atiba A. Nelson, Jarret M. Woodmass, Yohei Ono, et al. (2015) Partial Thickness Rotator Cuff Tears: Current Concepts. Adv Orthop 2015: 458786.
- Jian Xiao, Guo-Qing Cui (2015) Clinical and Magnetic Resonance Imaging Results of Arthroscopic Repair of Intratendinous Partialthickness Rotator Cuff Tears. Chin Med J (Engl) 128(11): 1496-1501.
- Bey MJ, Ramsey ML, Soslowsky LJ (2002) Intratendinous strain fields of the supraspinatus tendon: Effect of a surgically created articularsurface rotator cuff tear. J Shoulder Elbow Surg 11(6): 562-569.
- Lin Sun, Qiang Zhang, Heng’an Ge, Yeqing Sun, Biao Cheng (2015) Which is the best repair of articular-sided rotator cuff tears: a metaanalysis. J Orthop Surg Res 10: 84.
- Ahmed S. Eid, Amitabh J. Dwyer, Andrew F. W. Chambler (2012) Midterm results of arthroscopic subacromial decompression in patients with or without partial thickness rotator cuff tears. Int J Shoulder Surg 6(3): 86-89.
- McMahon PJ, Prasad A, Francis KA (2014) What is the prevalence of senior-athlete rotator cuff injuries and are they associated with pain and dysfunction? Clin Orthop Relat Res 472(8): 2427-2432.
- Ozaki J, Fujimoto S, Nakagawa Y, Masuhara K, Tamai S (1988) Tears of the rotator cuff of the shoulder associated with pathological changes in the acromion. A study in cadavera. J Bone Joint Surg Am 70(8): 1224- 1230.
- Uhthoff HK, Hammond DI, Sarkar K, Hooper GJ, Papoff WJ (1988) The role of the coracoacromial ligament in the impingement syndrome. A clinical, radiological and histological study. Int Orthop. 12(2): 97-104.
- Ogata S, Uhthoff HK (1990) Acromial enthesopathy and rotator cuff tear. A radiologic and histologic postmortem investigation of the coracoacromial arch. Clin Orthop Relat Res 254: 39-48.
- Fukuda H, Hamada K, Yamanaka K (1990) Pathology and pathogenesis of bursal-side rotator cuff tears viewed from en bloc histologic sections. Clin Orthop Relat Res 254: 75-80.
- Nelly Andarawis-Puri, Eric T. Ricchetti, Louis J. Soslowsky (2009) Rotator cuff tendon strain correlates with tear propagation. J Biomech 42(2): 158-163.
- Mazzocca AD, Rincon LM, O’Connor RW, Obopilwe E, Andersen M, et al. (2008) Intra-articular partial-thickness rotator cuff tears: analysis of injured and repaired strain behavior. Am J Sports Med 36(1): 110-116.
- Reilly P, Amis AA, Wallace AL, Emery RJ (2003) Supraspinatus tears: propagation and strain alteration. J Shoulder Elbow Surg 12(2): 134- 138.
- Mihata T, McGarry MH, Ishihara Y, Bui CN, Alavekios D, et al. (2015) Biomechanical analysis of articular-sided partial-thickness rotator cuff tear and repair. Am J Sports Med 43(2): 439-446.
- Xiao J, Cui G (2015) Clinical and structural results of arthroscopic repair of bursal-side partial-thickness rotator cuff tears. J Shoulder Elbow Surg 24(2): e41-e46.
- Frisch KE, Marcu D, Baer GS, Thelen DG, Vanderby R (2014) The influence of partial and full thickness tears on infraspinatus tendon strain patterns. J Biomech Eng 136(5): 051004.
- Lundgreen K, Lian Ø, Scott A, Engebretsen L (2013) Increased levels of apoptosis and p53 in partial-thickness supraspinatus tendon tears. Knee Surg Sports Traumatol Arthrosc 21(7): 1636-1641.
- Andrea Donovan, Mark Schweitzer, Jenny Bencardino, Catherine Petchprapa, Jodi Cohen, et al. (2011) Correlation between Rotator Cuff Tears and Systemic Atherosclerotic Disease. Radiol Res Pract 2011: 128353.
- Franceschi F, Papalia R, Del Buono A, Maffulli N, Denaro V (2011) Repair of partial tears of the rotator cuff. Sports Med Arthrosc 19(4): 401-408.
- Ponce BA, Kundukulam JA, Sheppard ED, Determann JR, McGwin G, et al. (2014) Rotator cuff crepitus: could Codman really feel a cuff tear? J Shoulder Elbow Surg 23(7): 1017-1022.
- Seif Sawalha, Jochen Fischer (2015) The accuracy of “subacromial grind test” in diagnosis of supraspinatus rotator cuff tears. Int J Shoulder Surg. 9(2): 43-46.
- Anthony Yi, Ioannis A Avramis, Evan H Argintar, Eric R White, Diego C Villacis, et al. (2015) Subacromial volume and rotator cuff tears: Does an association exist? Indian J Orthop 49(3): 300-303.
- Bhagwani S, Peh WC (2013) Clinics in diagnostic imaging. 148. Bursalsided partial-thickness supraspinatus tendon tear. Singapore Med J 54(9): 524-529.
- Hayter CL, Miller TT, Nguyen JT, Adler RS (2012) Comparative analysis of 2- versus 3-dimensional sonography of the supraspinatus tendon. J Ultrasound Med 31(3): 449-453.
- de Jesus JO, Parker L, Frangos AJ, Nazarian LN (2009) Accuracy of MRI, MR arthrography, and ultrasound in the diagnosis of rotator cuff tears: a meta-analysis. AJR Am J Roentgenol 192(6): 1701-1707.
- Lee JH, Yoon YC, Jee S (2015) Diagnostic performance of indirect MR arthrography for the diagnosis of rotator cuff tears at 3.0 T. Acta Radiol 56(6): 720-726.
- Yagci B, Manisali M, Yilmaz E, Ozkan M, Ekin A, et al. (2001) Indirect MR arthrography of the shoulder in detection of rotator cuff ruptures. Eur Radiol 11(2): 258-262.
- Dinauer PA, Flemming DJ, Murphy KP, Doukas WC (2007) Diagnosis of superior labral lesions: comparison of noncontrast MRI with indirect MR arthrography in unexercised shoulders. Skeletal Radiol 36(3): 195- 202.
- Dinnes J, Loveman E, McIntyre L, Waugh N (2003) The effectiveness of diagnostic tests for the assessment of shoulder pain due to soft tissue disorders: a systematic review. Health Technol Assess 7(29): iii, 1-166.
- Michael J. Carroll, Kristie D. More, Stephen Sohmer, Atiba A. Nelson, Paul Sciore, et al. (2013) The use of an intra-articular depth guide in the measurement of partial thickness rotator cuff tears. Adv Orthop 2013: 959305.
- M.Denkers, K. Pletsch, R. Boorman, R.Hollinshead, and I.K. Y (2012) Lo, “Partial thickness rotator cuff tears: observe or operative,” in Proceedings of the American Academy of Orthopaedic Surgeons Annual Meeting, San Francisco, Calif, USA.
- Yamanaka K, Matsumoto T (1994) The joint side tears of the rotator cuff. A follow up study by arthrography. Clin Orthop Relat Res 304: 68- 73.
- Shibata Y, Midorikawa K, Emoto G, Naito M (2001) Clinical evaluation of sodium hyaluronate for the treatment of patients with rotator cuff tear. J Shoulder Elbow Surg 10(3): 209-216.
- Chou WY, Ko JY, Wang FS, Huang CC, Wong T, et al. (2010) Effect of sodium hyaluronate treatment on rotator cuff lesions without complete tears: a randomized, double-blind, placebo-controlled study. J Shoulder Elbow Surg 19(4): 557-563.
- Wang AW, Bauer S, Goonatillake M, Breidahl W, Zheng MH (2013) Autologous tenocyte implantation, a novel treatment for partialthickness rotator cuff tear and tendinopathy in an elite athlete.
- Stefan Bauer, Allan Wang, Rodney Butler, Michael Fallon, Robert Nairn, et al. (2014) Reliability of a 3 T MRI protocol for objective grading of supraspinatus tendonosis and partial thickness tears. J Orthop Surg Res 9: 128.
- Oh LS, Wolf BR, Hall MP, Levy BA, Marx RG (2007) Indications for rotator cuff repair: a systematic review. Clin Orthop Relat Res 455: 52- 63.
- Payne LZ, Altchek DW, Craig EV, Warren RF (1997) Arthroscopic treatment of partial rotator cuff tears in young athletes. A preliminary report. Am J Sports Med 25(3): 299-305.
- Cordasco FA, Backer M, Craig EV, Klein D, Warren RF (2002) The partial-thickness rotator cuff tear: is acromioplasty without repair sufficient? Am J Sports Med 30(2): 257-260.
- Kartus J, Kartus C, Rostgård-Christensen L, Sernert N, Read J, et al. (2006) Long-term clinical and ultrasound evaluation after arthroscopic acromioplasty in patients with partial rotator cuff tears. Arthroscopy 22(1): 44-49.
- Liem D, Alci S, Dedy N, Steinbeck J, Marquardt B, et al. (2008) Clinical and structural results of partial supraspinatus tears treated by subacromial decompression without repair. Knee Surg Sports Traumatol Arthrosc. 16(10): 967-972.
- Strauss EJ, Salata MJ, Kercher J, Barker JU, McGill K, et al. (2011) Multimedia article. The arthroscopic management of partial-thickness rotator cuff tears: a systematic review of the literature. Arthroscopy 27(4): 568-580.
- Kim SJ, Kim SH, Lim SH, Chun YM (2013) Use of magnetic resonance arthrography to compare clinical features and structural integrity after arthroscopic repair of bursal versus articular side partial-thickness rotator cuff tears. Am J Sports Med 41(9): 2041-2047.
- Kim KC, Shin HD, Cha SM, Park JY (2014) Repair integrity and functional outcome after arthroscopic conversion to a full-thickness rotator cuff tear: articular-versus bursal-side partial tears. Am J Sports Med 42(2): 451-456.
- Kamath G, Galatz LM, Keener JD, Teefey S, Middleton W, et al. (2009 ) Tendon integrity and functional outcome after arthroscopic repair of high-grade partial-thickness supraspinatus tears. J Bone Joint Surg Am 91(5): 1055-1062.
- Spencer EE (2010) Partial-thickness articular surface rotator cuff tears: an all-inside repair technique. Clin Orthop Relat Res 468(6): 1514-1520.
- Kyung Cheon Kim, Hyun Dae Shin, Soo Min Cha, Jun Yeong Park (2013) Clinical outcomes after arthroscopic trans-tendon suturebridge technique in partial-thickness articular-side rotator cuff tear. Knee Surgery, Sports Traumatology, Arthroscopy 21(5): 1183-1188.
- R. Castricinir, N. Panfoli, R. NittoliS. Spurio, O. Pirani (2009) Transtendon arthroscopic repair of partial-thickness, articular surface tears of the supraspinatus: results at 2 years. Chir Organi Mov 93(S): 49-54.
- Fukuta S, Amari R, Tsutsui T (2015) Double arthroscopic transtendon repair of partial-thickness articular surface tears of the rotator cuff: a surgical technique. J Orthop Surg (Hong Kong) 23(3): 395-397.
- Castagna A, Delle Rose G, Conti M, Snyder SJ, Borroni M, et al. (2009) Predictive factors of subtle residual shoulder symptoms after transtendinous arthroscopic cuff repair: a clinical study. Am J Sports Med 37(1): 103-108.
- Waibl B, Buess E (2005) Partial-thickness articular surface supraspinatus tears: a new transtendon suture technique. Arthroscopy 21(3): 376-381.
- Kim YS, Lee HJ, Bae SH, Jin H, Song HS (2015) Outcome Comparison Between in Situ Repair Versus Tear Completion Repair for Partial Thickness Rotator Cuff Tears. Arthroscopy 31(11): 2191-2198.
- Huberty DP, Schoolfield JD, Brady PC, Vadala AP, Arrigoni P, et al. (2009) Incidence and treatment of postoperative stiffness following arthroscopic rotator cuff repair. Arthroscopy 25(8): 880-890.
- Shin SJ, Kook SH, Rao N, Seo MJ (2015) Clinical Outcomes of Modified Mason-Allen Single-Row Repair for Bursal-Sided Partial-Thickness Rotator Cuff Tears: Comparison with the Double-Row Suture-Bridge Technique. Am J Sports Med 43(8): 1976-1982.
- Brian T.N. Le, Xiao L. Wu, Patrick H. Lam, George A.C. Murrell (2014) Factors predicting rotator cuff retears: an analysis of 1000 consecutive rotator cuff repairs. Am J Sports Med 42(5): 1134-1142.
- Millett PJ, Warth RJ, Dornan GJ, Lee JT, Spiegl UJ (2014) Clinical and structural outcomes after arthroscopic single-row versus double-row rotator cuff repair: a systematic review and meta-analysis of level I randomized clinical trials. J Shoulder Elbow Surg 23(4): 586-597.
- Shen C, Tang ZH, Hu JZ, Zou GY, Xiao RC (2014) Incidence of retear with double-row versus single-row rotator cuff repair. Orthopedics 37(11): e1006-1013.
- Uchiyama Y, Hamada K, Khruekarnchana P, Handa A, Nakajima T, et al. (2010) Surgical treatment of confirmed intratendinous rotator cuff tears: Retrospective analysis after an average of eight years of follow‑up. J Shoulder Elbow Surg 19(6): 837‑846.






























