Repair and Rehabilitation of Zone Five Tendon Injuries of the Wrist
Galal Hegazy*1, Ahmed Akar1, Emad Zayed1, Mohamed Ellabad2 and Ahmed Mosalam3
1Orthopedic Department, Al-Azhar University, Egypt
2Nurosurgery Department, Al-Azhar University, Egypt
3physical medicine Rheumatology and Rehabilitation Department
Submission: August 05, 2016; Published: August 16, 2016
*Corresponding author: Galal Hegazy, Orthopedic Department, Al-Azhar University, Cairo, Egypt
How to cite this article: Galal H, Ahmed A, Emad Z, Mohamed E, Ahmed M. Repair and Rehabilitation of Zone Five Tendon Injuries of the Wrist. Ortho & Rheum Open Access J. 2016; 2(4): 555591. DOI: 10.19080/OROAJ.2016.02.555591
Abstract
Background: Volar cut wrist injuries represent a challenge for most hand surgeons as the anatomical complexity of the hand mirrors its functional efficiency. A specialized management approach is often necessary to treat such injuries which are variables and multidisciplinary team can decrease the morbidity rate.
Purpose: To evaluate the clinical outcome of early repair and rehabilitation of zone 5 tendon injuries of the wrist and return to work after trauma.
Patients and Methods: This study included thirteen patients with volar cut wrist injuries. Ten patients were males and three patients were females. the age ranged from 18 to 46 years (average 30 years). All injuries were single sharp cut wound in flexor zone five. Injury was accidental in all patients without skeletal involvement. Neurovascular examinations were done, the sensory and motor components of the nerve tested clinically while assessment of the hand and fingers vascularity carried out by clinical study and hand held Doppler. The surgeries were done by a team of surgeons consists of orthopedic surgeon and neurosurgeon. All patients were subjected to an intensive rehabilitation program under supervision of a specialist in physiotherapy medicine. All cases were followed up for vascularity, sensation and functions of the hand, the average follow up was 8 months (range from 6 - 12).
Results: For thirteen patients over the period of clinical follow up, there was marked reduction in morbidity with satisfactory significant hand functions and no ischemia, neuroma or tendon ruptures were observed during the follow-up period.
Conclusion: Early and technically proper evaluation, exploration and repair of volar cut wrist injuries with programmed intensive rehabilitation protocol result in good functional outcome.
Keywords: Wrist injuries; Flexor tendons; Median nerve; Ulnar nerve; Functional disability
Abbreviations: PL: Palmaris Longus; FCR: Flexor Carpi radialis; FCU: Flexor Carpi ulnaris; FPL: Flexor Pollicis Longus; FDS Flexor Digitorum Superficialis; FDP: Flexor Digitorum Profundus; RT: Right; LT: Left; ED: Emergency department
Introduction
Hand injuries are common and account for 5-10% of emergency department (ED) injuries and 4.7% of all trauma patients [1]. Various mechanisms of injury can lead to volar wrist injuries, and the most common are; machine injuries, glass lacerations, knife wounds, and suicide attempts [2]. Flexor Zone five extends from distal wrist crease to the flexor musculotendinous junction as described by Verdan in 1959 [3].This is the most exposed and so the most vulnerable zone for injuries. Extensive injuries to flexor tendons and surrounding structures are sometimes referred to as spaghetti wrist [4]. The functional importance of the closely packed structures, blood vessels, nerves and flexor tendons, makes the injuries in this zone very hazardous and the carful management of paramount importance [5,6]. The aim of this study was to determine the clinical outcome for early repair and programmed rehabilitation of acute cut injuries in Flexor Zone five. Also to evaluate of the efficacy of multidisciplinary team in evaluation and management of acute volar wrist injuries.
Patients and Methods
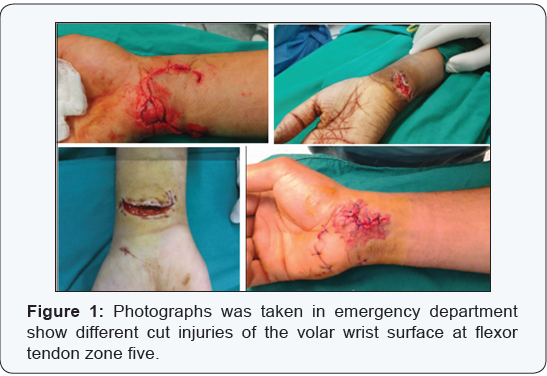
The study includes thirteen patients with average age 30 years (range from 18 to 46). All patients with single sharp cut wound in Flexor Zone five (eight patients with knife cut and five patients with glass cut) presented within 12 hours from injury to emergency department (Figure 1). Patients with all other kind of injuries and patients with associated skeletal injuries were excluded from the study. Informed written consent was taken from all patients.
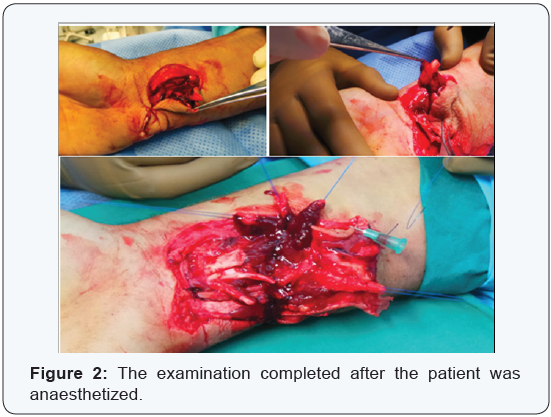
After resuscitation, pain management and tetanus prophylaxis, complete examination of the limb was done including proximal and distal neurovascular evaluation and musculoskeletal examination as thoroughly as could be done without causing pain and discomfort to patient. Rest of examination was with held till the patient was anaesthetized (Figure 2).
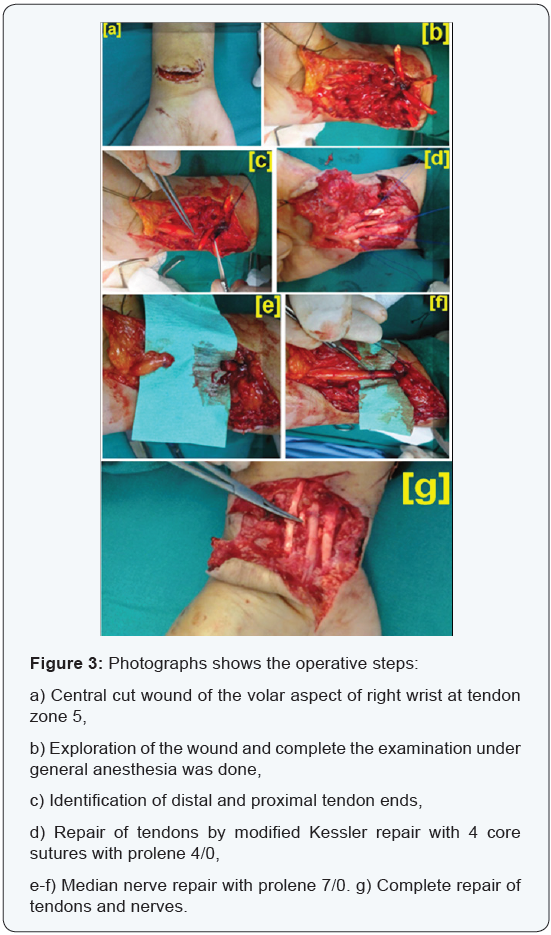
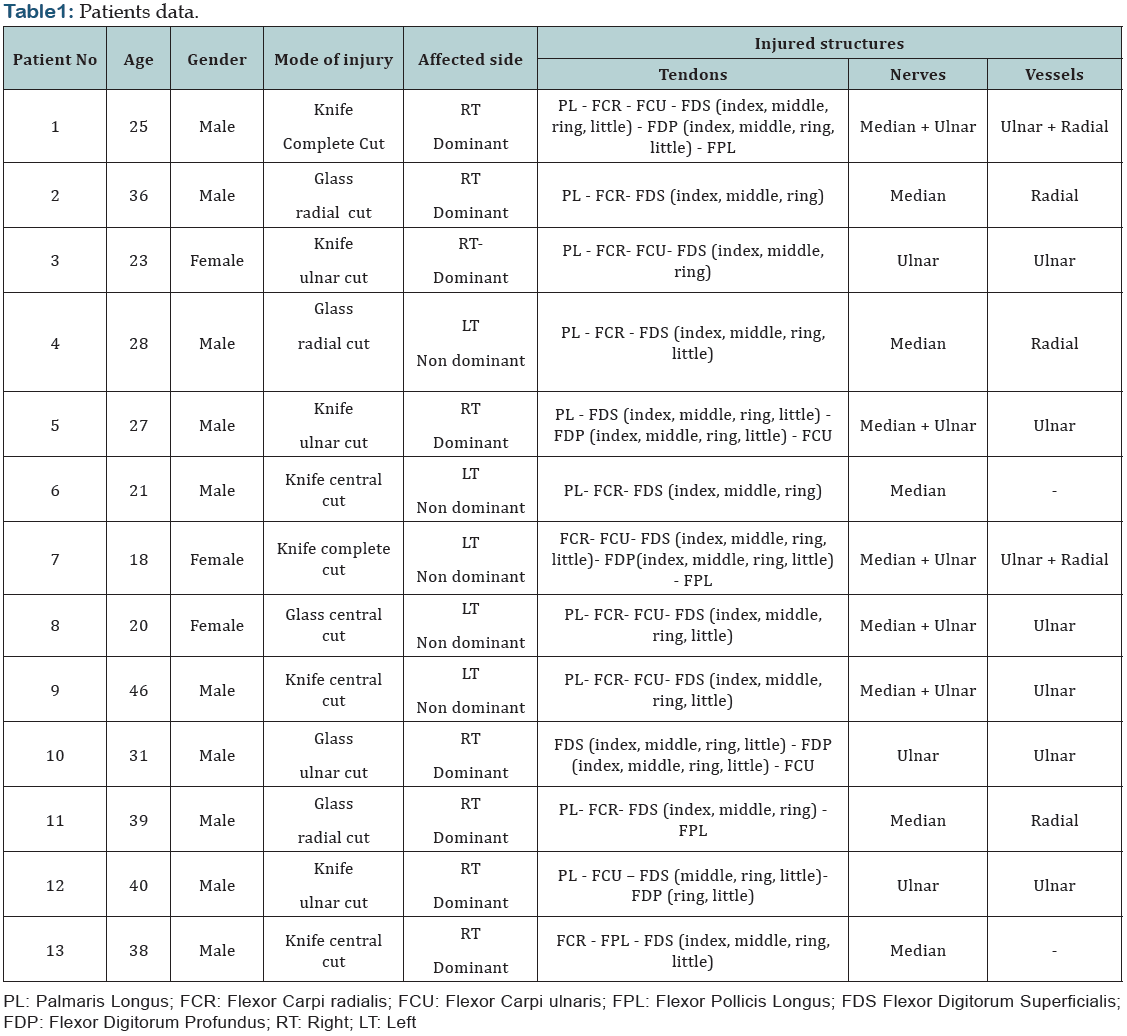
Investigations included baseline blood tests mainly complete blood count and radiological studies. The four most commonly involved structures included flexor carpi ulnaris, ulnar artery, ulnar nerve and flexor digitorum superficialis. Ulnar aspect of the wrist had more propensity for involvement followed by central cuts of wrist. Ulnar artery alone was involved in six cases, radial artery alone in three cases while both ulnar and radial arteries were involved in two cases and no vascular injury in two cases. Ulnar nerve alone was involved in three cases, median nerve alone in five cases while both median and ulnar nerves were involved in five cases. Superficial and deep flexor tendons of fingers were involved in all cases with a total of 65 tendons injured. Flexor carpi ulnaris was involved in eight cases and Flexor pollicis longus was involved in four cases. Flexor carpi radialis was involved in nine cases while palmaris longus was involved in ten cases (Table 1). The surgeries were done by a team of surgeons consists of orthopedic surgeon and neurosurgeon. All patients were operated under general anesthesia, tourniquet control and loupe magnification. In all cases, tendons were repaired first followed by nerves and finally vessels except in two cases where both ulnar and radial arteries were severed, hand needed revascularization and time since injury was approaching 6 hours, in which case ulnar artery was repaired first followed by the above sequence. All flexor tendons were repaired by modified Kessler repair with 4 core sutures with prolene 4/0 with knots in the centre followed by paratenon running suture circumferentially with prolene 6/0. Median and ulnar nerves were repaired with prolene 7/0. Ulnar and radial arteries were repaired with prolene 8/0. Postoperatively, hand was kept in a splint and elevated (Figure 3).
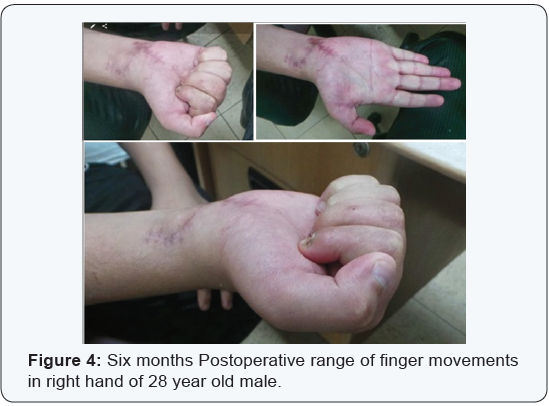
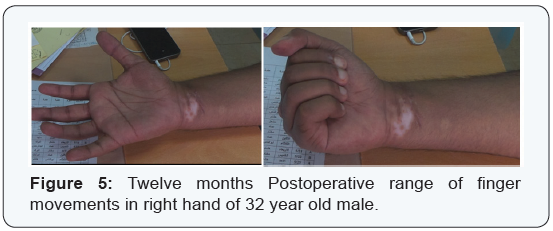
Postoperative physiotherapy rehabilitation program was started after 24 hours under supervision of specialist in physical medicine rheumatology and rehabilitation removing the splint during physiotherapy, initially with active extension and controlled passive flexion and passive range of motion exercises. After two weeks activity was progressed to placing objects but not holding and after 4 weeks holding objects but not exerting force. After 6 weeks holding and lifting light weights was allowed with progressively increasing resistance to flexion. After 6 weeks splint was worn only at night for another 2 weeks (Figures 4 & 5). Progressively increased activity was allowed from 8 weeks onwards. Patients were followed-up with evaluation of:
- Patency of arterial repair
- Nerve repair results (sensory and motor)
- Active range of motion for fingers and wrist joint,
- Grip strength was evaluated. Functional recovery was also evaluated by the duration of return to work.
Results
Thirteen cases with sharp cut wounds in Zone five of Flexor Tendons fulfilled the inclusion criteria during the study period. The average follow up period was eight months (range from 6 - 12).
A: Patency of arterial repair
The patients followed for patency of arterial repair by hand held Doppler. None of the patients required re-exploration for ischemia of distal limb. Doppler showed nine out of the eleven vascular anastomoses remained patent over follow-up period. One showed loss of anastomotic patency on the first postoperative day while another on second post-operative day, both in cases of isolated radial artery injury. Vascularity of hand was not found to be compromised in either case so reexploration was not carried out.
B: Nerve repair results (sensory and motor)
Nerve repair results were evaluated serially by advancing Tinnel’s sign, electrophysiological studies (nerve conduction study and electromyography) and sensory perception scored from (S0 to S4) compared to normal opposite upper limb. Seven cases out of eight repaired ulnar nerves showed sensory perception score (S4) level sensory return and one case had (S3). On the other hand, seven cases out of ten median nerves repaired showed sensory perception score (S4) level of sensory return, two cases showed (S3) level of sensory return and one case had (S2) level of sensory return. Power of intrinsic muscles of the hand was evaluated from (Grade 0 to Grade 5). Three Opponens pollicis had (Grade 5), six cases showed (Grade 4) while one case showed (Grade 3), out of 10 cases of median nerve repair. The other intrinsic muscles of the hand showed (Grade 5) in five cases, (Grade 4) in two cases and (Grade 3) in one case of ulnar nerve repair. Nerve conduction studies showed regenerative changes in all repaired nerves but the results of these studies did not always correlate exactly with clinical findings (Table 2).
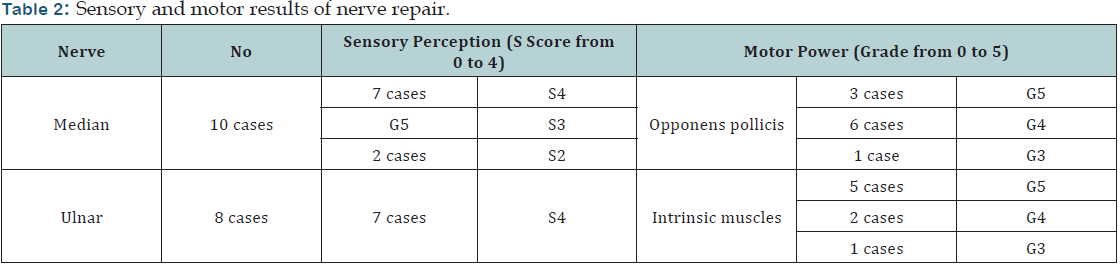
C: Active range of motion for fingers and wrist joint
The average wrist flexion was 77 degrees (range from 60 - 85) and average wrist extension was 75 degrees (range from 65 - 85). Active range of motion for fingers was evaluated by Strickland’s Adjusted Formula [(DIP + PIP) flexion - extension deficit x 100/175 degrees = % normal] with excellent from (75 - 100%), good from (50 - 74%), fair from (25 - 49%) and poor less than (25%). There were eight cases had excellent results, three cases had good results and two cases had fair results. Poor excursion was not found in any of the repaired flexor pollicis longus.
D: Grip strength
The power of grip strength was evaluated by using of Jamar dynamometer compared to normal side. The average grip strength was 75% of normal side (range from 60% to 90%). All patients returned to their previous work and recreational activities without disability. The patients returned to work in average 12 weeks (range from 10 - 16). One patient had superficial infection treated with oral antibiotics and daily dressing. Mild occasional wrist pain was recorded in two patients. The pain did not affect work status or daily activities and no need for medical treatment. Neuroma, tendon rupture or tendon adhesions did not recorded in any one of our patients but one patient had painful hypertrophic volar wrist scar treated with local corticosteroids injection and Silicone sheets for 12 weeks, the hypertrophic scar gradually regress.
Discussion
Injuries to the volar wrist surface have the potential to be severely debilitating, mainly due to the superficial location and high density of tendons, nerves and arteries in that area [1]. Extensive injuries to flexor tendons and surrounding structures are sometimes referred to as spaghetti wrist [4- 6]. The tendons have pretty less inherent tendency of healing. The functional integrity of hand requires intact neurovascular units and a stable platform in the form of a normal wrist joint [7]. Per-operatively, close proximity of structures poses a great challenge in identification of structures. Repair of structures is highly demanding especially in combined neural and tendon injuries [8]. Postoperatively, inter-structural adhesions are a major problem. Prolonged rest postoperatively increases the propensity for adhesions while early mobility impairs healing of nerves [8]. It was found that Zone five Flexor tendon injury is much more common in younger and manually working people. Tuncali et al. [2] studied a total of 228 patients with various types of upper extremity structures injuries. They concluded that tendon and nerve repair are far superior in the younger age group people [2].
This further supports the findings of Yrjana et al. [9] who studied the tendon repair in pediatric age group in 28 patients with 45 injured structures in upper extremity. Accidental injuries are far more common than suicidal and homicidal cases. So most of these patients are co-operative and motivated and have a high intent of recovery and return to work [10,11]. This further stresses on the need for early repair in these patients. This study shows that primary repair of flexor tendons has superior results as far as postoperative functional recovery is concerned compared to results of studies with delayed repairs. Chan et al. [10] came to same conclusion in their study of 31 zone 2 flexor tendon injuries. Strickland also agreed on an early primary repair of flexor tendons [11]. Primary repair of nerves also has a superior outcome [12]. In the present study the results of primary repair of ulnar and median nerves are comparable. This is shown by the improvement in sensation, which is comparable in patients post-ulnar and median nerve repairs.
Motor return in both groups of nerve repairs, shown by recovery of Opponens pollicis and adductors, is also comparable. This is in accordance with the Karaberg et al. [13] comparison of Ulnar and Median nerve repairs, in which they studied 55 patients post-ulnar and/or median nerve repair. This study also concludes that electrophysiological studies do not always co relate accurately with clinical assessment and so they should only be considered in conjunction with clinical evaluation rather than alone as a diagnostic tool as shown by Dutelli et al. [14] in their study as well. This study also implies that the increasing number of core sutures is directly proportional to the strength of repair and it does not hamper the healing or gliding of tendons. It did not have an impact on the adhesion formation as well which is in accord with a number of other studies.
An additional advantage of multiple core sutures, four in case of this study is that early mobilization and physiotherapy can be carried out which has beneficial effects in both promotion of healing and prevention of adhesion formation, as stated by Morya et al. [15] in their study of various suture techniques for flexor tendon repair. There has always been a debate on early versus late mobilization post-tendon repair. Some believe in commencement of early physiotherapy while others believe in prolonged rest post-tendon repair. In this study it was seen that with proper technique of repair, early mobilization and therapy is safe and indeed beneficial. It has been proposed as the stress theory that controlled early stress promotes the healing process of tendons. Prolonged rest post-tendon repair may be responsible for adhesion formation which is an important limiting factor in the final recovery and return of function after tendon repair. This was also shown in an elaborate study by Hung et al. [16]. Some of these studies were characterized by the variation of settings in which the injuries occurred including domestic neat blade cuts to industrial machine injuries with grossly contaminated wounds. Also some patients were more motivated in rehabilitation therapy than others. It is beyond the scope of this study to achieve all these standardizations.
Conclusion
Care of patients with acute hand injury begins with a focused history and physical examination. In most clinical scenarios, a diagnosis is achieved clinically. While most patients require straight forward treatment, the emergency clinician must rapidly identify limb-threatening injuries and obtain critical clinical information. From all results reported in the present study, it can be said that, multidisciplinary team can evaluate and manage acute volar wrist injuries saving time and decreasing post-operative functional disability with short time to return to patient’s daily activity due to accurate repair of injured structures, early movement and appropriate rehabilitation program which need patient co-operation.
Institutional Review Board Statement
The study was reviewed and approved by the Faculty of Medicine – Al-Azhar University Institutional Review Board.
Statement of Informed Consent
All study participants provided informed written consent prior to study enrollment.
Statement of Human Rights
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2008. Informed consent was obtained from all patients for being included in the study.
References
- Pucket GL, Meyer VH (1985) Results of treatment of extensive volar wrist lacerations: the Spaghetti wrist. Plast Reconstr Surg 75(5): 714- 721.
- Tuncali D, Yavuz N, Terzioglu A, Aslan G (2005) The rate of upper extremity deep-structure injuries through small penetrating lacerations. Ann Plast Surg 55(2):146-148.
- Verdan CE (1960) Primary repair of flexor tendons. J Bone Joint Surg 42(2): 647-657.
- Yüksel F, Pecker F, Acikel C, Cellkoz B (2002) Second hand management of Spaghetti wrist: do not hesitate to explore. Ann Plast Surg 49(5): 500-504.
- Weinzweg N, Chin G, Mead M, Gonzalez M (1998) Spaghetti wrist: management and results. Plast Renonst Surg 102(1): 96-102.
- Kabak S, Hallici M, Baktir A, Türk CY, Avsarogullari L (2002) Results of treatment of extensive volar wrist lacerations: the Spaghetti wrist. Eur J Med 9(1): 71-76.
- Sharma P, Maffulli N (2006) Biology of tendon injury: healing, modeling and remodeling. J Musculoskelet Neuronal Interac 6(2): 181-190.
- Bukhari AJ, Saleem M, Bhutta AR, Khan AZ, Abid KJ (2004) Spaghetti wrist; management and outcome. J Coll Physicians Surg Pak 14(10): 608-611.
- Nietosvaara Y, Lindfors NC, Palmu S, Rautakorpi S, Ristaniemi N (2007) Flexor tendon injuries in pediatric patients. J Hand Sur Am 32(10):1549-1557.
- Chan TK, Ho Co, Lee WK, Fung YK, Law YF, et al. (2006) Functional outcome of the hand following flexor tendon repair at the ‘no man’s land’. J Orthopaed Surg (Hong Kong) 14(2):178-183.
- Strickland JW (2001) Development of flexor tendon surgery: twenty five years of progress. J Hand Surg Am 25(2): 214-235.
- Yiltok SJ, Misauno MA (2007) Primary repair of ‘Speghetti wrist” with good functional outcome. Niger J Plast Surg 3(2): 42-46.
- Karabeg R, Jakirlic M, Dujso V (2009) Sensory recovery after forearm median and ulnar nerve grafting. Med Arh 63(2): 97-99
- Duteilli F, Petry D, Poure L, Dautel G, Merle M (2001) A comparative clinical and electromyographic study of median and ulnar nerve injuries at the wrist in children and adults. J Hand Surg Br 26(1): 58- 60.
- Moriya T, Larson MC, Zhao C, An KN, Amadio PC (2012) The effect of core suture flexor tendon repair techniques on gliding resistance during static cycle motion and load to failure: a human cadaver study. J Hand Surg Eur Vol 37(4): 316-322.
- Hung LK, Pang KW, Yeung PLC, Cheung L, Wong JM, et al. (2005) Active mobilisation after flexor tendon repair following injuries in zone 2 and other zones: comparison of results. J Orthopaed Surg 13(2): 158-163.






























