- Review Article
- Abstract
- Introduction
- Definition of Diabetes And Their Clinical Profiles
- Gestational Diabetes Mellitus (GMD)
- Diabetes Due to Other Causes (e.g. Genetic Factors or Induced by Medication)
- Combination Therapeutics Regime
- Proposed Terminology and Types of Combination Drug Therapeutics
- Knowledge-Gained In the Mechanisms (Signaling Pathways) of Combinations Drugs
- Adverse Effects Observed In Some Combination Drug Therapies
- Combination of Metformin Hydrochloride With Other Agents For the Treatment of Diabetes
- Methods
- Chronological Apperarence of Patents Filed
- Current & Future Developments
- Conclusion
- Conflicts of Interests
- Acknowledgment
- References
Combination Therapy Including Metformin hydrochloride for the Treatment of Diabetes and Related Comorbidity: A Patent Filed Survey
Juan Manuel Germán Acacio1 * and David Morales-Morales2*
1Red de Apoyo a la Investigación, Instituto Nacional de Ciencias Médicas y Nutrición SZ Universidad Nacional Autónoma de México (CIC-UNAM), México
2Instituto de Química. Universidad Nacional Autónoma de México. Circuito Exterior S/N. Ciudad Universitaria. Coyoacán. C. P 04510. México CDMX
Submission: February 11, 2017; Published: March 02, 2017
*Corresponding author: Juan Manuel Germán Acacio, David Morales Morales, Instituto de Química. Universidad Nacional Autónoma de México. Circuito Exterior S/N. Ciudad Universitaria. Coyoacán. C. P. 04510. México, CDMX. Email: domor@unam.mx(D.Morales);jmga@cic.unam.mx(J.M.German-Acacio)
How to cite this article: Juan M G A, David M M. Combination Therapy Including Metformin hydrochloride for the Treatment of Diabetes and Related Comorbidity: A Patent Filed Survey. Organic & Medicinal Chem IJ. 2017; 1(4): 555569.DOI:10.19080/OMCIJ.2017.01.555569
- Review Article
- Abstract
- Introduction
- Definition of Diabetes And Their Clinical Profiles
- Gestational Diabetes Mellitus (GMD)
- Diabetes Due to Other Causes (e.g. Genetic Factors or Induced by Medication)
- Combination Therapeutics Regime
- Proposed Terminology and Types of Combination Drug Therapeutics
- Knowledge-Gained In the Mechanisms (Signaling Pathways) of Combinations Drugs
- Adverse Effects Observed In Some Combination Drug Therapies
- Combination of Metformin Hydrochloride With Other Agents For the Treatment of Diabetes
- Methods
- Chronological Apperarence of Patents Filed
- Current & Future Developments
- Conclusion
- Conflicts of Interests
- Acknowledgment
- References
Abstract
Diabetes is a group of metabolic dysfunctions/disorders and specifically type 2 diabetes (T2D) constitutes ~90-95% of all diabetic patients. For its treatment, Metformin hydrochloride is the most preferred anti-hyperglycemic oral agent. Due to the complexity of T2D, the use of Metformin hydrochloride alone (monotherapy) as the first-line drug has resulted to be inadequate and the addition of a second or multiple agents is necessary. Thus, in the last years there has been an enormous interest in the development of new therapeutic agents, leading to a large number of inventions (patents) regarding alternative therapies involving the use of Metformin hydrochloride in the presence of a second or more agents for the treatment and care of T2D.
Thus, this revision deals with the chronological appearance of patents filed related with combination therapy for the treatment of diabetes or any other related comorbidity with special emphasis in the utilization of Metformin hydrochloride or any related Metformin salt (used equally as first-line or as a second-line of choice), administered simultaneously, separately or sequentially with one or more agents (e.g. drugs, natural products, hormones, peptides, proteins, etc.). In addition, this work highlights some important issues related with combination therapeutic regimes, such as: proposed terminology, the importance of gaining knowledge about the potential mechanisms by which these treatments operate as well as adverse effects observed and so on.
Keywords: Diabetes; Combination therapy; Metformin hydrochloride; Patent; Monotherapy; Fixed dose tablets/pills; Metabolic syndrome
Abbreviations: ADA: American Diabetes Association; AMPK: AMP-Activated Protein Kinase; CVD: Cardiovascular Disease; DDIs: Drug Drug Interaction; DNA: Deoxyribonucleic Acid; FDA: Food and Drug Administration; GIP: Glucose Dependent Insulin tropic Peptide; GLP- 1: Glucagon-Like Peptide-1; GMD: Gestational Diabetes Mellitus; HIV/AIDS: Human Immunodeficiency Virus Infection/Acquired Immune Deficiency Syndrome; IDDM: Insulin Dependent Diabetes Mellitus; mRNA: Messenger Ribonucleic Acid; NIDDM: Non-Insulin Dependent Diabetes Mellitus; NPH: Insulin Isophane; PhRMA: Pharmaceutical Research and Manufacturers of America; RNA: Ribonucleic Acid; SPIDDM: Slowly Progressive Insulin-Dependent Diabetes Mellitus; SU: Sulfonylurea; TZD: Thiazolidinediones; T1D: Type 1 Diabetes; T2D: Type 2 Diabetes
- Review Article
- Abstract
- Introduction
- Definition of Diabetes And Their Clinical Profiles
- Gestational Diabetes Mellitus (GMD)
- Diabetes Due to Other Causes (e.g. Genetic Factors or Induced by Medication)
- Combination Therapeutics Regime
- Proposed Terminology and Types of Combination Drug Therapeutics
- Knowledge-Gained In the Mechanisms (Signaling Pathways) of Combinations Drugs
- Adverse Effects Observed In Some Combination Drug Therapies
- Combination of Metformin Hydrochloride With Other Agents For the Treatment of Diabetes
- Methods
- Chronological Apperarence of Patents Filed
- Current & Future Developments
- Conclusion
- Conflicts of Interests
- Acknowledgment
- References
Introduction
The worldwide impact in our society related with diabetes mellitus is an alarming issue. According with a recent study, the prevalence of diabetic patients around the world (aged 20-79 years) was estimated in 2010 as 285 million adults affected and this number is expected to increase to almost double in 2030 (439 million of diabetic persons) [1]. The predictions indicate there will be an increase of 69% of diabetic adults in developing countries (over-populated most of them) and 20% of incidence in developed countries [1]. Thus, the development of new, more effective, easily available and cheap pharmaceutical agents for the treatment of this illness becomes a priority.
- Review Article
- Abstract
- Introduction
- Definition of Diabetes And Their Clinical Profiles
- Gestational Diabetes Mellitus (GMD)
- Diabetes Due to Other Causes (e.g. Genetic Factors or Induced by Medication)
- Combination Therapeutics Regime
- Proposed Terminology and Types of Combination Drug Therapeutics
- Knowledge-Gained In the Mechanisms (Signaling Pathways) of Combinations Drugs
- Adverse Effects Observed In Some Combination Drug Therapies
- Combination of Metformin Hydrochloride With Other Agents For the Treatment of Diabetes
- Methods
- Chronological Apperarence of Patents Filed
- Current & Future Developments
- Conclusion
- Conflicts of Interests
- Acknowledgment
- References
Definition of Diabetes And Their Clinical Profiles
The American Diabetes Association (ADA), defines diabetes as a chronic condition that requires continuous pharmacologic and non-pharmacologic treatment [2]. Diabetes is a complex and chronic condition associated with a group of metabolic dysfunctions mainly due to hyperglycemia disorders associated with insulin secretion, insulin action or both. Long-term episodes of hyperglycemia in diabetic patients derived in different cardiovascular damages and dysfunctions in multiple organs, e.g. eyes, kidneys, nerves, heart and blood vessels [2c].
According with the ADA “Standards of Medical Care in Diabetes-2012”, diabetes has been classified in four groups: gestational diabetes mellitus (GDM), other types of diabetes due to other causes, type 1 diabetes (T1D) and type 2 diabetes (T2D) [2b]. Although, the Expert Committee on the Diagnosis and Classification of Diabetes Mellitus in 2003 formerly had considered ill nutrition-related diabetes as the fifth clinical profile in this classification[2a]. In 1980[2a], the World Health Organization (WHO) Expert Committee on Diabetes and later the WHO Study Group on Diabetes Mellitus, recognized diabetes in only two main groups and termed as: insulin dependent diabetes mellitus (IDDM, nowadays known as T1D) and non-insulin dependent diabetes mellitus (NIDDM, known today as T2D). Both terms have been eliminated to avoid confusions [2a].
- Review Article
- Abstract
- Introduction
- Definition of Diabetes And Their Clinical Profiles
- Gestational Diabetes Mellitus (GMD)
- Diabetes Due to Other Causes (e.g. Genetic Factors or Induced by Medication)
- Combination Therapeutics Regime
- Proposed Terminology and Types of Combination Drug Therapeutics
- Knowledge-Gained In the Mechanisms (Signaling Pathways) of Combinations Drugs
- Adverse Effects Observed In Some Combination Drug Therapies
- Combination of Metformin Hydrochloride With Other Agents For the Treatment of Diabetes
- Methods
- Chronological Apperarence of Patents Filed
- Current & Future Developments
- Conclusion
- Conflicts of Interests
- Acknowledgment
- References
Gestational Diabetes Mellitus (GMD)
Gestational diabetes mellitus (GMD) is a condition detected during pregnancy, and is characterized as glucose intolerance [3] having an incidence in the USA of 3-5% of cases per year (about the 135,000 pregnancies reported) [4,5]. During pregnancy, insulin resistance episodes can occur naturally often triggering diabetes, another common scenario occurs when the insulin secretory capacity is compromised due to impaired insulin action and secretion thus resulting in developing of T2D. In this regard, women with a GMD history are more likely to develop T2D at some point of their life [6] even when the glucose levels, after delivery, are restored to normal. Thus, the incidence to develop T2D in the future is still possible, but the risk to develop T1D is less likely [5].
- Review Article
- Abstract
- Introduction
- Definition of Diabetes And Their Clinical Profiles
- Gestational Diabetes Mellitus (GMD)
- Diabetes Due to Other Causes (e.g. Genetic Factors or Induced by Medication)
- Combination Therapeutics Regime
- Proposed Terminology and Types of Combination Drug Therapeutics
- Knowledge-Gained In the Mechanisms (Signaling Pathways) of Combinations Drugs
- Adverse Effects Observed In Some Combination Drug Therapies
- Combination of Metformin Hydrochloride With Other Agents For the Treatment of Diabetes
- Methods
- Chronological Apperarence of Patents Filed
- Current & Future Developments
- Conclusion
- Conflicts of Interests
- Acknowledgment
- References
Diabetes Due to Other Causes (e.g. Genetic Factors or Induced by Medication)
Although lifestyle and excess nutrient intake are considered the principal triggers for the development of T2D, genetic factors (heredity) can also play a fundamental role. Thus, families with a diabetes history exhibit a 2 to 4 fold increased probability to develop T2D during their lifetime. And, 15-25% of first-degree relatives of T2D patients are prone to develop impaired glucose tolerance or diabetes [7]. Thus, lifetime risk (at age 80 years) for T2D has been calculated to be 38% when one parent had T2D, and this probability increases to almost double when both parents had diabetes, estimating the prevalence of T2D in the offspring to approach to 60% by the age of 60 years [7].
The genetic etiology of T1D and T2D is very complex and no conclusive data have determined their origins, however predisposition and environmental factors are considered to be associated with these conditions [8]. For example, very low incidence of T1D is seen in several Asian countries [9], but Finland shows the highest rates (35 cases per 100,000) [10]. In contrast, only one third of incidence is observed in the Baltic population [11](e.g. Estonia) [12] despite the ethnical similarity with Finland's population, this being indicative of environmental factors playing an important role [8]. However, T2D is more manifest in certain specific ethnicities and significant disparities are observed. For instance, among the diverse ethnic groups in American population the risk to develop T2D is less prone in non-Hispanic white adults compared with Asian Americans (9%), Hispanics (12.8 %) and non-Hispanic blacks (13.2 %) exhibit a higher incidence [13].
On the other hand, different chemical agents or medications, such as: pentamidine, nicotinic acid, glucocorticoids, thyroid hormone, beta-adrenergic agonists, thiazides or Alfa- interferon can induce the development of diabetes [14]. Whilst conditions such as pancreatitis, pancreatectomy, neoplasia, cystic fibrosis, fibro calculus and pancreatopathy, can also trigger diabetes [14].
T1D
Beta-cell destruction usually leads to absolute insulin deficiency. T1D is a condition associated by the endogenous insufficiency of insulin in the body, and this defect is due to autoimmune destruction of the beta-cells of the endocrine pancreas, as a consequence patients with T1D must receive insulin injections permanently [15].
Since the beta-cells destruction is quite rapid in infants and children, the prevalence of T1D in children and young compared with adults is greater [16]. Besides, after several years it tends to be a very common episode for patients diagnosed with T2D to be re-diagnosed with T1D due to gradual exhaustion of insulin secretion [17]. This process is known as slowly progressive insulin-dependent diabetes mellitus (SPIDDM), condition that is different from typical T2D patients that frequently are obese and insulin resistant [17]. T1D represents 5-10% of diabetic patients [2c].
T2D
T2D is a chronic condition that manifests by disorders of insulin action and/or insulin secretion [18]. This clinical profile accounts for ~90-95% of diabetic patients, and the patients are characterized to have insulin resistance and usually have relative (rather than absolute) insulin deficiency [2b]. Surprisingly, from the people who suffer T2D, at least half, have never been diagnosed, and thus this population have no knowledge of their condition [18]. As mentioned above, T2D is related with family history, age, ethnicity, previous history of gestational diabetes and physical inactivity. According with the WHO, evidence indicates that sedentary lifestyle (lack of physical activity, obesity or overweigh), tobacco and alcohol abuse, family diabetes history and unhealthy dietary regimen contribute to the development of T2D in young adults, children or adolescents [18,19]. Hence, T2D can be prevented encouraging people to make lifestyle changes on diet and promoting the practice of physical exercise. However these actions do not seem to be enough to attack the problem mainly due to people's apathy. Thus, T2D prevention is the key and may save money, for instance Mexico in 2006 spent about US $ 1,164.8 million dollars on the treatment of diabetic patients, situation that can become unsustainable given the accelerated rates of cases [20].
In addition, cardiovascular diseases (CVD), such as myocardial infarction or stroke are the major causes of death in patients with T2D [21]. Hence, a combination of a balanced diet, moderate physical activity and the use of an appropriate pharmacological and/or non-pharmacological agent reduce substantially the risk to develop this and other long-term conditions: retinopathy, nephropathy, CVD, etc [2a]. In addition, recent discoveries indicate that agents such as, hormones, drugs, natural products, etc. may activate physiologically or pharmacology AMP-activated protein kinase (AMPK) considered the therapeutic target for the treatment of T2D [22]. In this sense, the most common pharmacological agents used for the treatment of hyperglycemia in T2D are: biguanides, sulfonylurea's (SUs, 2nd generation), meglitinides, thiazolidinediones (TZDs), Alfa-glucosidase inhibitors, GLP-1 receptor agonists (incretin mimetics), DPP- 4 inhibitors (incretin enhancers), bile acid sequestrants and dopamine-2 agonists [2b] (Table 1).
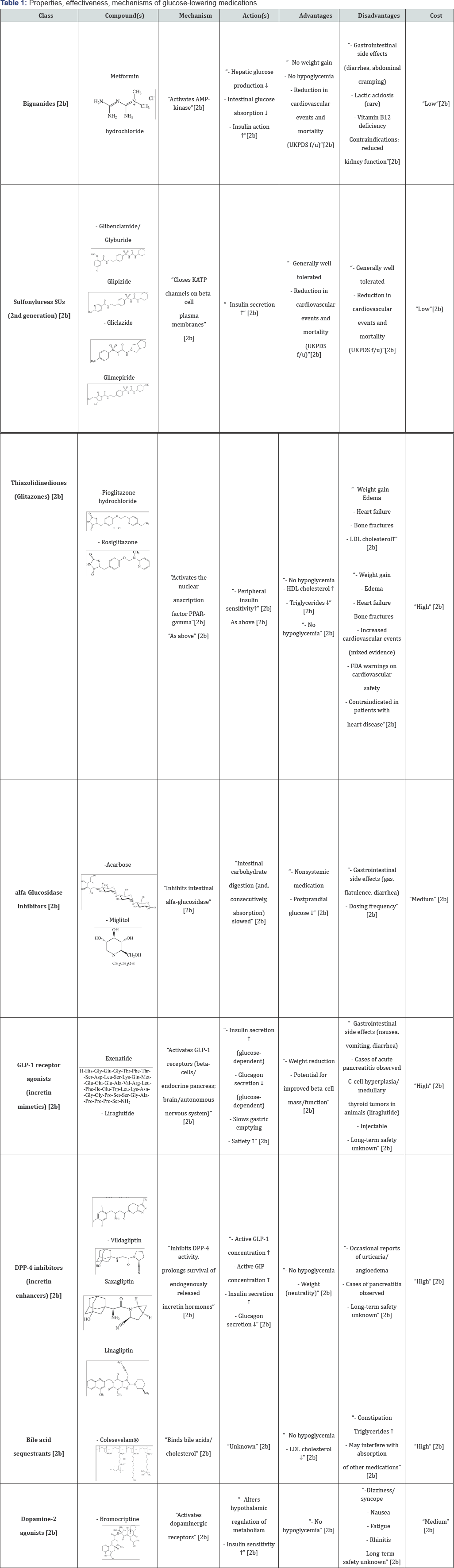
Adapted from: [2b] Position Statement. Standards of Medical Care in Diabetes-2012. Diabetes Care 2012; 35(1): S11-S63.
There is a wide dossier of drugs or chemical agents, depending on the clinical profile of the patient, for the treatment and management of T2D. However, most of these medications have some disadvantages, e.g: elevated cost, limited pharmacological action, after prolonged use some patients develop progressive detrimental pharmacological effectiveness until obsolescence (e.g. SUs) [23] and the appearance of other long-term risk factors (e.g. reduced kidney function, CVD). Due to the nature and complexity of T2D, at this moment there is no efficient pharmacotherapy for the control of hyperglycemia and the efficiency of new drugs is continuously evaluated. As a matter of fact, before 1995 management of diabetes was limited to the use of SUs, isophane (also known as NPH), insulin and regular insulin's were the most prescribed anti-diabetic agents [24]. Since then, in the last 15 years lots of pharmacotherapy options have appeared in an attempt to improve the effectiveness and safety for the management of diabetes [24]. The patients diagnosed with diabetes, only 14% are co-administrated simultaneously with insulin and other medication and 58% only consume oral medications [25].
Thus, the problem is, that due to the complexity in the treatment of T2D, monotherapy does not seem to be the most appropriate strategy in the glycemic control, since the use of a single pharmaceutical agent is likely to target only a single defect, causing in a long-term lapse, the appearance of other inconveniences (vide supra). Hence, today Metformin hydrochloride represents the first choice drug for glycemic control, since: it is cheap compared to other related drugs, their toxicological profile is more innocuous (during monotherapeutic administration less adverse effects where observed) and Metformin hydrochloride is better adapted to the lifestyle even in overweighed patients [25].
Sadly, it is likely that Metformin hydrochloride-glycemic controlled T2D patients, will eventually require the administration of a second drug, being this the main problem in the treatment of T2D and motif for the present review, that comprehensively accounts and describes the chronological appearance of the so far known, inventions/patents filed involving the use of Metformin hydrochloride or any Metformin analogue in the presence of a second or more agents for the efficient treatment of T2D patients. This paper also reviews, important aspects related with combination therapeutic regimes, such as: proposed terminology, clinical in vitro and in vivo studies in an attempt to elucidate the potential mechanisms related with drug-drug interactions (DDls), etc., to hopefully reach, in time, not a proper and efficient treatment but a real cure for this pandemic illness.
- Review Article
- Abstract
- Introduction
- Definition of Diabetes And Their Clinical Profiles
- Gestational Diabetes Mellitus (GMD)
- Diabetes Due to Other Causes (e.g. Genetic Factors or Induced by Medication)
- Combination Therapeutics Regime
- Proposed Terminology and Types of Combination Drug Therapeutics
- Knowledge-Gained In the Mechanisms (Signaling Pathways) of Combinations Drugs
- Adverse Effects Observed In Some Combination Drug Therapies
- Combination of Metformin Hydrochloride With Other Agents For the Treatment of Diabetes
- Methods
- Chronological Apperarence of Patents Filed
- Current & Future Developments
- Conclusion
- Conflicts of Interests
- Acknowledgment
- References
Combination Therapeutics Regime
Due to the complexity of many diseases such as diabetes, cancer, HIV/AIDS, etc., administration of a single drug regimen (monotherapy) to target a single defect, is no longer the most appropriate treatment, due to the fact that prolonged exposure results in the development of other complications [26,27]. Alternatively to monotherapy, administration of multiple agents is therapeutic option, based on the premise that combination of the agents can be more effective than the sum of the effectiveness of the individual agents [2,7].
Combination drug therapeutics (also known as multicomponent therapeutics) might lead to new medication strategies showing mutually interdependent activities required to improve clinical efficacy and understanding the side effects and toxicity involved during the treatment [28]. In fact, the action of a single drug activates/modulates multiple proteins rather than single targets and this may limit its therapeutic effect [28,29]. The combination of multiple drugs may target, multiple subpopulations, or multiple diseases simultaneously, since every drug can work through different mechanisms or modes of action improving efficacy of the therapeutic effect, lowering the dose administration but increasing or maintaining the same efficacy, minimizing or slowing down the development of drug resistance, and giving different types of synergism (additive or antagonist effect; potentiate or reduce effect) [30].
For instance, when patients with severe hyperglycemia are prescribed with one pharmacological agent and glycemic levels are not controlled, is mandatory the administration of another agent to control the hyperglycemia [31]. Some years ago combination drug regimens were prescribed as separated tablets, but today fixed-dose single tablet combinations are available, based on the bio-equivalence of the separate tablets and giving similar efficacy, reducing the pill burden and simplifying the administration regimen of the patient [31]. Fixed- dose single tablets/pills is also a current tendency embraced by the Pharmaceutical companies since may have some important implications in the drug commercialization (cost/effectiveness), lowering the price in the treatment of some diseases by using combination drug therapies rather than single drug treatment and helping the duration of the treatment to be shortened [32].
In 2013 the Food and Drug Administration (FDA) established some recommendations for the combination of two or more drugs as therapeutic regime [33].
i.The combination is intended to treat a serious disease or condition”
ii. There is a strong biological rationale for the use of the combination (e.g., the agents inhibit distinct targets in the same molecular pathway or steps in disease pathogenesis, provide inhibition of both a primary and compensatory pathway, or inhibit the same target at different binding sites to decrease resistance or allow use of lower doses to minimize toxicity).
iii.A full non-clinical characterization of the activity of both the combination and the individual new investigational drugs, or a short-term clinical study on an established biomarker, suggests that the combination may provide a significant therapeutic advance over available therapy and is superior to the individual agents. A non-clinical model should demonstrate that the combination has substantial activity and provides greater activity, a more durable response (e.g., delayed resistance), or a better toxicity profile than the individual agents.
iv.There is a compelling reason why the new investigational drugs cannot be developed independently (e.g., monotherapy for the disease of interest leads to resistance, one or both of the agents would be expected to have very limited activity when used as monotherapy).
ln this regard, some pharmaceutical companies, such as Glaxo-Smith-Kline (Advair for the treatment of asthma and Combivir for HIV) and Kos Pharmaceuticals (Advicor for hypercholesterolemia) have combined the above-mentioned drugs with other pharmaceutical agents on the basis of clinical rationale (comprising two or more drugs), showing therapeutic success [28].
- Review Article
- Abstract
- Introduction
- Definition of Diabetes And Their Clinical Profiles
- Gestational Diabetes Mellitus (GMD)
- Diabetes Due to Other Causes (e.g. Genetic Factors or Induced by Medication)
- Combination Therapeutics Regime
- Proposed Terminology and Types of Combination Drug Therapeutics
- Knowledge-Gained In the Mechanisms (Signaling Pathways) of Combinations Drugs
- Adverse Effects Observed In Some Combination Drug Therapies
- Combination of Metformin Hydrochloride With Other Agents For the Treatment of Diabetes
- Methods
- Chronological Apperarence of Patents Filed
- Current & Future Developments
- Conclusion
- Conflicts of Interests
- Acknowledgment
- References
Proposed Terminology and Types of Combination Drug Therapeutics
The syncretism given by the combination of two drugs may arise a fundamental question: what is the expected effect of the combination? In the spirit to give an answer for the meaning and relevance of this, we must reformulated the question as: these combinations are syncretic or congruous? [28,30]. In this case an appropriate terminology is proposed by Stockwell et al. [28] to differentiate the kind of combination.
Syncretic combination drug
"It is used to denote a drug that is composed of two or more active ingredients, at least one of which is not used individually to treat the target disease indication".
Congruous combination drug
"A drug that is composed of two or more active ingredients, each of which has been individually used to treat the target disease indication".
Multicomponent therapeutic
"An optimized combination and formulation of multiple active ingredients. This category includes both syncretic and congruous drugs". Based on this, in attempt to categorize what type of cooperation is observed in these combinations, depending the synergism presented can be classified as is indicated by several authors as: Chou, Tallarida, Jia, etcetera [30,34,35].
Additive or antagonist effect
Is when the combination is pharmacodynamically additive or antagonist if the effect is greater than, equal to, or less than the summed effects of the partner drugs.
Potentiative or reductive effect
"Is when the therapeutic effect of one drug is augmented or reduced and this can be modulated or regulated by the action of another drug."
Coalistic combination
"This is when the activity of all the drugs involved is inactive separately but is active in combination."
In this sense, extensive and rigorous analyses must be done to decipher the mechanisms circumscribed behind the combination, contrasting the type of cooperation involved (additive, antagonistic and reductive synergism). And, to determine what type of cooperation is observed, experimental data can reveal valuable information. Many of these analyses are: "checkerboard, combination index, fractional effect analysis, isobolographic analysis, interaction index, median drug effect analysis, and response surface approaches" [35].
- Review Article
- Abstract
- Introduction
- Definition of Diabetes And Their Clinical Profiles
- Gestational Diabetes Mellitus (GMD)
- Diabetes Due to Other Causes (e.g. Genetic Factors or Induced by Medication)
- Combination Therapeutics Regime
- Proposed Terminology and Types of Combination Drug Therapeutics
- Knowledge-Gained In the Mechanisms (Signaling Pathways) of Combinations Drugs
- Adverse Effects Observed In Some Combination Drug Therapies
- Combination of Metformin Hydrochloride With Other Agents For the Treatment of Diabetes
- Methods
- Chronological Apperarence of Patents Filed
- Current & Future Developments
- Conclusion
- Conflicts of Interests
- Acknowledgment
- References
Knowledge-Gained In the Mechanisms (Signaling Pathways) of Combinations Drugs
The manifestation and origins of different diseases are determined by different potential factors: environmental factors, tissue type, hormone levels, aging, etc. Thus, in order to gain knowledge in the dynamics and on how different constituents within the cell are integrated and interconnected (e.g. proteins, DNA, RNA and small molecules) in a complex signaling network, it is important to correlate diverse interactions (metabolic, regulatory, spatial, etc) [36]. Thus, a great number of studies including: genomics, proteomics and phosphoproteomics have been carried out in order to discover gene expressions signatures and protein signaling pathways associated with a particular disease [37].
Chemicals agents, hormones, protein receptors, ligands, enzymes, transcription factors, ions or DNA/RNA are responsible to modulate biochemical reactions, electrical signals, mRNA transcription and protein translation in a complex machinery of signaling network [37]. Gaining knowledge at the molecular level of how this complicated network of signals is functioning and/or how is perturbed, is fundamental for the development of drugs. In this regard, systematic studies have been done using a rationale combination of drugs exploring the connectivity of biological pathways, entailing how these small molecules activate or perturb cellular signaling networks in a desired fashion [28-29,35-36,38-43].
Most of the molecular targets of specific drugs have been elucidated or identified serendipitously after studying the mechanisms of action by naive mechanistic assumptions [39]. In fact, many of the US FDA-approved drugs for the treatment of specific diseases are used by clinicians without a previous knowledge of the molecular mechanisms of action [44].
The way of how a drug interacts with a specific target interfering or perturbing the cellular signaling networks is a complicated job, because most of the drugs interact with more than one target and in most cases this assumption is not linearly deducible from single effects [42]. Therefore, one of the largest problems to solve is: once is identified and validated a disease- specific target or once is identified a drug like molecule that can modify this target, how this could be correlated in a way that makes therapeutic sense? This represents a major challenge to confront [45].
The complexity is greater trying to determine the perturbation in the signaling network when combination drug therapy is used, due to the fact that mechanisms of drug-drug interactions (DDIs) must be considered, since therapeutic response and effectiveness of combination pharmacotherapy depends of the pharmacodynamics interaction between the drugs involved, and in addition to that, the potential synergism concerted is strongly influenced with the dose and concentration of the pharmaceutical agents involved, and most of the time these assertions are based on trial and error [46,47].
- Review Article
- Abstract
- Introduction
- Definition of Diabetes And Their Clinical Profiles
- Gestational Diabetes Mellitus (GMD)
- Diabetes Due to Other Causes (e.g. Genetic Factors or Induced by Medication)
- Combination Therapeutics Regime
- Proposed Terminology and Types of Combination Drug Therapeutics
- Knowledge-Gained In the Mechanisms (Signaling Pathways) of Combinations Drugs
- Adverse Effects Observed In Some Combination Drug Therapies
- Combination of Metformin Hydrochloride With Other Agents For the Treatment of Diabetes
- Methods
- Chronological Apperarence of Patents Filed
- Current & Future Developments
- Conclusion
- Conflicts of Interests
- Acknowledgment
- References
Adverse Effects Observed In Some Combination Drug Therapies
Adverse episodes related with DDIs are considered the major cause of morbidity worldwide and several medicaments have been withdrawn of the market after fatal events were reported after their administration for a period of time [47], for instance the case of cerivastatin-gemfibrozil syncretism can be mentioned [48]. These adverse events may occur when the drugs shared metabolic and pharmacological pathways provoking diminution in effectiveness and safety profile [46].
Currently, before a drug can be entered in the marketplace extensive in vitro and in vivo pharmacokinetic DDIs studies must be carried out, emphasizing that combination drug toxicity is null or minimal [47]. An excellent compendium prepared by the Pharmaceutical Research and Manufacturers of America (PhRMA) can be taken as guidance where the best practice for the design of in vitro and in vivo DDIs studies is outlined [49]. Nowadays some of the endeavors currently used for the establishment of DDIs are based on in Silico Approaches (e.g. molecular fingerprints), which have produced uplifting and expeditious results [47,50].
- Review Article
- Abstract
- Introduction
- Definition of Diabetes And Their Clinical Profiles
- Gestational Diabetes Mellitus (GMD)
- Diabetes Due to Other Causes (e.g. Genetic Factors or Induced by Medication)
- Combination Therapeutics Regime
- Proposed Terminology and Types of Combination Drug Therapeutics
- Knowledge-Gained In the Mechanisms (Signaling Pathways) of Combinations Drugs
- Adverse Effects Observed In Some Combination Drug Therapies
- Combination of Metformin Hydrochloride With Other Agents For the Treatment of Diabetes
- Methods
- Chronological Apperarence of Patents Filed
- Current & Future Developments
- Conclusion
- Conflicts of Interests
- Acknowledgment
- References
Combination of Metformin Hydrochloride With Other Agents For the Treatment of Diabetes
Diabetes is a conjunction of systemic diseases and specifically T2D constitutes ~90-95% of diabetic patients [18] and its treatment usually requires the utilization of multiple oral agents (mainly drugs) since monotherapy for maintaining glycemic control may be overcame in some patients affording this approach inadequate. Thus, when monotherapy is no longer efficient, to improve the glycemic control in the patient can be achieved administrating the combination of diverse drugs with different mechanisms of action, [51] despite of some reports stating that long-termed combination therapy coadministrating oral pharmaceutical agents may result obsolete and the co-administration of incretin hormones (e.g. glucagonlike peptide-1 GLP1, glucose dependent insulin tropic peptide GIP, etc) stimulate insulin synthesis and secretion in a glucose- dependent manner and do not produce hyperglycemia [52].
Metformin hydrochloride has been established as the drug of choice for the first-line treatment of T2D [53]. Metformin hydrochloride is considered as one of the safest oral hypoglycemic agents [53], characterized by insulin resistance in overweighed patients and is the only anti-diabetic drug that have conclusively shown prevention in CVD and provide beneficial effects on dyslipidemia and hypofibrinolysis [25]. Besides, its low cost compared with other pharmaceutical agents makes it even more attractive. In specific, it has been pointed out that Metformin hydrochloride is a very efficacious medication used in monotherapy compared with another medications [25].
In practice, Metformin hydrochloride can be combined with any other medication (unless contraindications exist) [31], for instance combination of Metformin hydrochloride with some pharmacological agents may trigger hypoglycemia (e.g. TDZs and SUs) [25], although is pointed out that combination with SUs is associated with 6 times more risk for hypoglycemia than with TDZs [25]. Nevertheless, in the case of the fixed-dose single tablet of Metformin hydrochloride/glyburide shows similar bioequivalence compared with combined therapy of the components, and this tablet allows to have a better glycemic control with lower dosage [54]. On the other hand, Metformin hydrochloride and any other TZDs, can be combined on the treatment of T2D due to their different cellular mechanisms, showing additive syncretism and improving anti-hyperglycemic efficacy [31]. Also, Metformin hydrochloride may be combined with an insulin secretagogue, for instance a dipeptidylpeptidase-4 (DPP-4) inhibitor or an injectable GLP-1 agonist, and this syncretism exhibit reducing insulin resistance [31]. In addition, when Metformin hydrochloride monotherapy fails, the use of SUs, TZDs, insulin, alfa-glucosidase agents must be considered as adjuvants in combination therapy [25,31,55]. Nevertheless, their choice as hypoglycemic adjuvants is dependent on the profile of the patient [25,31,55].
Moreover, recently it has been published that canagliflozin- metformin (Invokament®) approved by the FDA in 2014 as fixed- dose combination is a promising option for the treatment of T2D [56]. The first fixed-dose combination approved for the treatment of diabetes by the FDA was Glucovance® in 2000 combining glyburide and Metformin [57]. The combination of canagliflozin- metformin at this moment seems to be safe and effective as an option when Metformin hydrochloride monotherapy is no longer effective [56]. However this combination must be cautioned in patients with history in genital mycotic infections, hypotension and poor renal function [56].
In this review a survey was made to circumscribe inventions (patents) which claim the development of diverse formulations/ compositions where the presence of Metformin hydrochloride or any Metformin salt is included combined or co-administrated with other agents (e.g. drug/nutraceutical or molecule with antidiabetic activity, hormone, natural product, peptide, protein, etc.), for the treatment, prevention or amelioration of TD2 and in some cases T1D and/or any related complication considered within the metabolic syndrome, for instance: lipid disorders, hypertriglyceridemia, hyperinsulinemia and insulin resistance or any other related CVD, or any comorbidity associated.
- Review Article
- Abstract
- Introduction
- Definition of Diabetes And Their Clinical Profiles
- Gestational Diabetes Mellitus (GMD)
- Diabetes Due to Other Causes (e.g. Genetic Factors or Induced by Medication)
- Combination Therapeutics Regime
- Proposed Terminology and Types of Combination Drug Therapeutics
- Knowledge-Gained In the Mechanisms (Signaling Pathways) of Combinations Drugs
- Adverse Effects Observed In Some Combination Drug Therapies
- Combination of Metformin Hydrochloride With Other Agents For the Treatment of Diabetes
- Methods
- Chronological Apperarence of Patents Filed
- Current & Future Developments
- Conclusion
- Conflicts of Interests
- Acknowledgment
- References
Methods
The survey was made using Scifinder® (in addition with Espacenet® and Google Patent Search® for the reviewing of the original documents) under the restriction search ("Metformin Diabetes”) retrieving only patents. The survey was made for the period of November 29th, 2015 to January 25th, 2016. From the total number of hits found and after a careful and thorough revision, only patents that covered combination therapy using Metformin hydrochloride or any related Metformin salt in the presence of one or more agents in a single composition or separately being administrated by different routes were considered. These combinations include simultaneously, separately or sequentially administration of Metformin hydrochloride or any other Metformin salt in addition to any other agent.
Inventions that include the administration of Metformin hydrochloride or any other Metformin analogues and one or more agents in a fixed-dose as a single pill/tablet were also selected. The inventions related with combination therapy including Metformin hydrochloride or any other Metformin analogues and one or more agents for the exclusively treatment of obesity were excluded. The inventions related with formulations/compositions where Metformin or any related Metformin salt that is not used as the main therapeutic agent or is optionally suggested as an adjuvant are also included. Patents where is suggested the utilization of Metformin hydrochloride or any Metformin salt as a conjugate with another agent also were included. Patents where the original language was other than English were excluded; unless the translated document was found in English language.Table 2 shows these results.
- Review Article
- Abstract
- Introduction
- Definition of Diabetes And Their Clinical Profiles
- Gestational Diabetes Mellitus (GMD)
- Diabetes Due to Other Causes (e.g. Genetic Factors or Induced by Medication)
- Combination Therapeutics Regime
- Proposed Terminology and Types of Combination Drug Therapeutics
- Knowledge-Gained In the Mechanisms (Signaling Pathways) of Combinations Drugs
- Adverse Effects Observed In Some Combination Drug Therapies
- Combination of Metformin Hydrochloride With Other Agents For the Treatment of Diabetes
- Methods
- Chronological Apperarence of Patents Filed
- Current & Future Developments
- Conclusion
- Conflicts of Interests
- Acknowledgment
- References
Chronological Apperarence of Patents Filed


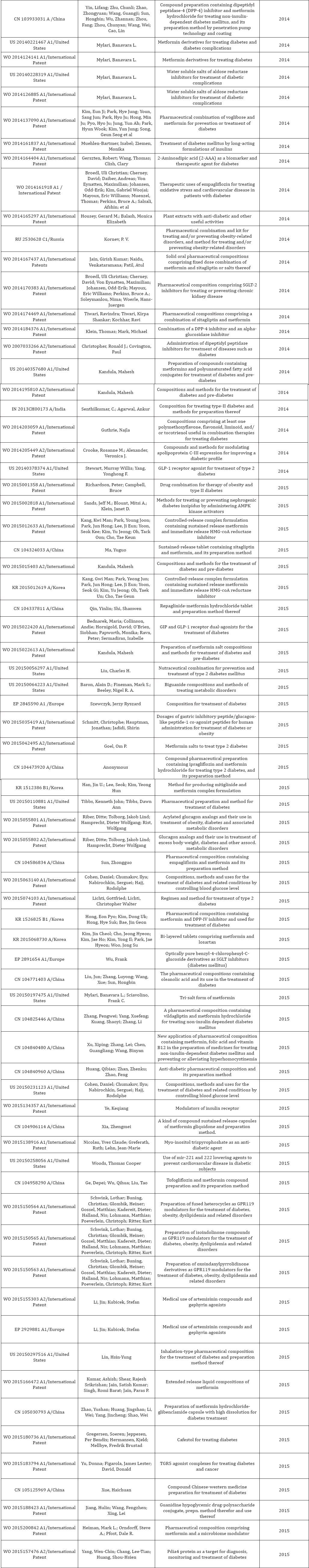
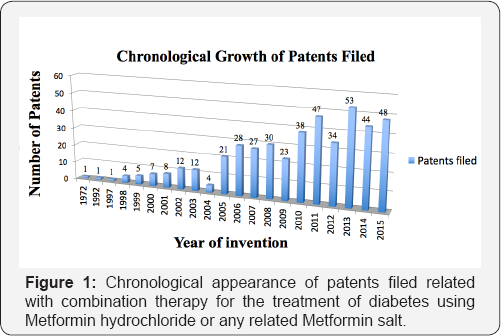
The chronological survey made (Table 2) reflects an exponential growth (Figure 1) from the first patent claimed in 1972 (JP 47032644 B4, Hypoglycemic tolbutamide-metformin salt). It is noteworthy that it took twenty years for the appearance of a second patent in 1992 (WO 9203148 A1, Method and compounds for treating type 2 diabetes mellitus) after the first patent was filed. This absence and sudden outbreak is apparently related with the approval and distribution of Metformin hydrochloride in USA in 1994, despite the fact that Metformin hydrochloride was first introduced in France in 1968 [58]. Moreover, from the period from 1992 to 1997 there were no patent related, however from 1997 a large number of patents have appeared, marking the beginning of an exponential growth in the register of inventions related to Metformin hydrochloride.
- Review Article
- Abstract
- Introduction
- Definition of Diabetes And Their Clinical Profiles
- Gestational Diabetes Mellitus (GMD)
- Diabetes Due to Other Causes (e.g. Genetic Factors or Induced by Medication)
- Combination Therapeutics Regime
- Proposed Terminology and Types of Combination Drug Therapeutics
- Knowledge-Gained In the Mechanisms (Signaling Pathways) of Combinations Drugs
- Adverse Effects Observed In Some Combination Drug Therapies
- Combination of Metformin Hydrochloride With Other Agents For the Treatment of Diabetes
- Methods
- Chronological Apperarence of Patents Filed
- Current & Future Developments
- Conclusion
- Conflicts of Interests
- Acknowledgment
- References
Current & Future Developments
Diabetes is a very complex condition consisting in a group of metabolic dysregulations with no effective treatment up to date. As a consequence of its worldwide incidence an astonishing number of patents have appeared in the recent years claiming the development of new formulations/compositions where Metformin hydrochloride or Metformin analogues is included in the presence of two or more agents for the treatment, prevention or amelioration of diabetes, and this number is still increasing rapidly.
Despite the appearance of new drugs and therapies for the treatment of diabetes specifically T2D, Metformin hydrochloride remains as the agent of choice, [58] due to the multiple benefits provided (low cost, is one of the most efficacious hypoglycemic agents showing prevention in CVD and provide beneficial effects on Dyslipidemia and hypofibrinolysis) [25]. However, it has been pointed out that its utilization in monotherapy after prolonged exposure, results in the development of other complications and the administration of Metformin hydrochloride in the presence of one or multiple agents (e.g. drugs, natural products, hormones, peptides, etc.) becomes necessary, resulting this procedure the treatment of choice. This phenomenon being clearly exemplified in Figure 1, where the trend observed proves the incessant appearance of patents related with combination therapy in 7 recent years.
- Review Article
- Abstract
- Introduction
- Definition of Diabetes And Their Clinical Profiles
- Gestational Diabetes Mellitus (GMD)
- Diabetes Due to Other Causes (e.g. Genetic Factors or Induced by Medication)
- Combination Therapeutics Regime
- Proposed Terminology and Types of Combination Drug Therapeutics
- Knowledge-Gained In the Mechanisms (Signaling Pathways) of Combinations Drugs
- Adverse Effects Observed In Some Combination Drug Therapies
- Combination of Metformin Hydrochloride With Other Agents For the Treatment of Diabetes
- Methods
- Chronological Apperarence of Patents Filed
- Current & Future Developments
- Conclusion
- Conflicts of Interests
- Acknowledgment
- References
Conclusion
Thus, these paper overviews the chronological appearance of patents related with combination therapy including Metformin hydrochloride or any Metformin analogue in the presence of one of more agents for the treatment of T2D. Due to its importance, Metformin hydrochloride is the preferred drug in the management of glycemic levels in T2D patients, and thus a considerable number of patents have been claimed in the last six years (2010-2015, with an average of 44 patents filed per year) demonstrating the importance of administration of Metformin hydrochloride for the treatment of diabetes, mainly in T2D.
Although the number of filed patents cannot be directly related to the growing number of patients with this condition, the statistics are not very promising and the number of patients is expected to increase in the years to come. However, the efforts devoted to the design and synthesis of new drugs based on combination therapy may lead to improving the glycemic controland thus the standard of life of those having T2D. The further understanding of the mechanisms through which thesedrugs work, may shed further light in the design of more efficient therapies ultimately leading not only to a proper control of the illness but to a potential cure of it.
- Review Article
- Abstract
- Introduction
- Definition of Diabetes And Their Clinical Profiles
- Gestational Diabetes Mellitus (GMD)
- Diabetes Due to Other Causes (e.g. Genetic Factors or Induced by Medication)
- Combination Therapeutics Regime
- Proposed Terminology and Types of Combination Drug Therapeutics
- Knowledge-Gained In the Mechanisms (Signaling Pathways) of Combinations Drugs
- Adverse Effects Observed In Some Combination Drug Therapies
- Combination of Metformin Hydrochloride With Other Agents For the Treatment of Diabetes
- Methods
- Chronological Apperarence of Patents Filed
- Current & Future Developments
- Conclusion
- Conflicts of Interests
- Acknowledgment
- References
Conflicts of Interests
The authors declare that they have no competing interests or conflict in the financial contribution.
- Review Article
- Abstract
- Introduction
- Definition of Diabetes And Their Clinical Profiles
- Gestational Diabetes Mellitus (GMD)
- Diabetes Due to Other Causes (e.g. Genetic Factors or Induced by Medication)
- Combination Therapeutics Regime
- Proposed Terminology and Types of Combination Drug Therapeutics
- Knowledge-Gained In the Mechanisms (Signaling Pathways) of Combinations Drugs
- Adverse Effects Observed In Some Combination Drug Therapies
- Combination of Metformin Hydrochloride With Other Agents For the Treatment of Diabetes
- Methods
- Chronological Apperarence of Patents Filed
- Current & Future Developments
- Conclusion
- Conflicts of Interests
- Acknowledgment
- References
Acknowledgment
The financial support of our research by CONACYT (PDCPN-247089) and DGAPA-UNAM (PAPIIT-IA202315) is gratefully acknowledged.
- Review Article
- Abstract
- Introduction
- Definition of Diabetes And Their Clinical Profiles
- Gestational Diabetes Mellitus (GMD)
- Diabetes Due to Other Causes (e.g. Genetic Factors or Induced by Medication)
- Combination Therapeutics Regime
- Proposed Terminology and Types of Combination Drug Therapeutics
- Knowledge-Gained In the Mechanisms (Signaling Pathways) of Combinations Drugs
- Adverse Effects Observed In Some Combination Drug Therapies
- Combination of Metformin Hydrochloride With Other Agents For the Treatment of Diabetes
- Methods
- Chronological Apperarence of Patents Filed
- Current & Future Developments
- Conclusion
- Conflicts of Interests
- Acknowledgment
- References
References
- Shaw J, Sicree R, Zimmet P (2010) Global estimates of the prevalence of diabetes for 2010 and 2030. Diabetes Res Clin Pract 87(1): 4-14.
- a. The Expert Committe on the Diagnosis Classification of Diabetes Mellitus (2003) Report of the Expert Committee on the Diagnosis and Classification of Diabetes mellitus. Diabetes Care 26(1): S5-S20.
American Diabetes Association. (2012) Standards of Medical Care in Diabetes-2012. Diabetes Care 35(1): S11-S63.
American Diabetes Association (2012) Diagnosis and Classification of Diabetes Mellitus. Diabetes Care 35(1): S64-S71. - American Diabetes Association (2003) Gestational Diabetes Mellitus. Diabetes Care 26(1): S103-S105.
- Kim C, Newton KM, Knopp RH (2002) Gestational diabetes and the incidence of type 2 diabetes. Diabetes Care 25(10): 1862-1868.
- Bellamy L, Casas JP, Hingorani AD, Williams D (2009) Type 2 diabetes mellitus after gestational diabetes: a systematic review and metaanalysis. Lancet 373(9677): 1773-1779."
- Jarvela IY, Juutinen J, Koskela P, Hartikainen AL, Kulmala P, et al. (2006) Gestational diabetes identifies women at risk for permanent type 1 and type 2 diabetes in fertile age. Predictive role of auto-antibodies. Diabetes Care 29(3): 607-612.
- Stumvoll M, Goldstein BJ, van Haeften, TW (2005) Type 2 diabetes: principles of pathogenesis and therapy. Lancet 365(9467): 1333-1346.
- Zimmet P, Alberti KGMM, Shaw J (2001) Global and societal implications of the diabetes epidemic. Nature 414(6865): 782-787.
- Atkinson MA, Maclaren NK (1994) The pathogenesis of insulindependent diabetes mellitus. N Engl J Med 331(21): 1428-1436.
- Tuomilehto J, Lounamaa R, Tuomilehto Wolf E, Reunanen A, Virtala E, et al. (1992) Epidemiology of childhood diabetes mellitus in Finland-background of a nationwide study of type 1 diabetes (insulin dependent) diabetes mellitus. The Childhood Diabetes in Finland (DiMe) Study Group. Diabetologia 1 35(1): 70-76.
- Tuomilehto J, Podar T, Brigis G, Urbonaite B, Rewers M, et al. (1992) Comparison of the incidence of insulin dependent diabetes mellitus among five Baltic populations during 1983-1988. Int J Epidemiol 21(3): 518-527.
- Tuomilehto J, Podar T, Reunanen A, Kalits I, Lounamaa R, et al. (1991) Comparison of incidence of IDDM in childhood between Estonia and Finland, 1980-1988. Diabetes Care 14: 982-988.
- Dagogo Jack S (2003) Ethnic disparities in type 2 diabetes: pathophysiology and implications for prevention and management. J Natl Med Assoc 95(9): 774-789.
- Kumar Tiwari B, Ahmad Sheikh B, Abidi AB (2013) A review on complication of Diabetes Mellitus and its Therapy. Int J Pharm Bio Sci 3(3): 56-66.
- Jacobsen IB, Henriksen JE, Hother-Nielsen O, Vach W, Beck-Nielsen H (2009) Evidence-based insulin treatment in type 1 diabetes mellitus. Diabetes Res Clin Pract 86(1): 1-10.
- Shoaib Akhtar M, Irshad N, Malik A, Kamal Y (2013) Need for new hypoglycemic agents: An overview. Int J Pharm Sci Rev Res 4(1): 77-82.
- Suehiro T, Osaki F, Ikeda Y, Arii K, Nakayama F, et al. (2005) Type 1 diabetes developed in a type 2 diabetic patient with severe insulin resistance. Diabetes Res Clin Pract 70(3): 298-302.
- World Health Organization (2003) Department of Noncommunicable Disease Management. Screening for Type 2 Diabetes. Report of a World Health Organization and International Diabetes Federation meeting. Geneva, Switzerland.
- World Health Organization 2011. Global status report on noncommunicable diseases 2010. Italy.
- A. Barquera S, Campos-Nonato I, Aguilar-Salinas C, López-Ridaura R, Arredondo, A, et al. (2013) Diabetes in Mexico: cost and management of diabetes and its complications and challenges for health policy. Global Health 9: 3.
Diabetes en números. Available at http://www.fmdiabetes.org/fmd/ pag/diabetes_numeros.php (accesed on: November 2nd, 2015). - Giorgino F, Leonardini A, Laviola, L (2013) Cardiovascular disease and glycemic control in type 2 diabetes: now that the dust is settling from large clinical trials. Ann NY Acad Sci 1281: 36-50.
- Coughlan KA, Valentine RJ, Ruderman NB, Saha AK (2014) AMPK activation: a therapeutic target for type 2 diabetes? Diabetes Metab Syndr Obes 7: 241-253.
- Rendell M (2004) The Role of Sulphonylureas in the Management of Type 2 Diabetes Mellitus. Drugs 64 (12): 1339-1358.
- Alexander GC, Sehgal NL, Moloney RM, Stafford RS (2008) National Trends in Treatment of Type 2 Diabetes Mellitus, 1994-2007. Arch Intern Med 168(19): 2088-2094.
- Qaseem A, Humphrey LL, Sweet DE, Starkey M, Shekelle P (2012) Oral Pharmacologic Treatment of Type 2 Diabetes Mellitus: A Clinical Practice Guideline From the American College of Physicians. Ann Intern Med 156(3): 218-231.
- Pourkavoos N (2012) Unique Risks, Benefits, and Challenges of Developing Drug-Drug Combination Products in a Pharmaceutical Industrial Setting. Comb Prod Ther 2(1): 1-31.
- Zimmermann GR, Lehar J, Keith CT (2007) Multi-target therapeutics: when the whole is greater than the sum of the parts. Drug Discov Today 12(1-2): 34-42.
- Keith CT, Borisy AA, Stockwell BR (2005) Multicomponent therapeutics for networked systems. Nat Rev Drug Discov 4(1): 71-78.
- Hopkins AL (2008) Network pharmacology: the next paradigm in drug discovery. Nat Chem Biol. 4: 682-690.
- Chou TC (2006) Theoretical Basis, Experimental Design, and Computerized Simulation of Synergism and Antagonism in Drug Combination Studies. Pharmacol Rev 58(3): 621-681.
- Bailey CJ, Day C (2009) Fixed-dose single tablet antidiabetic combinations. Diabetes Obes Metab 11(6): 527-533.
- Greber D, Vaidyanathan S (2014) The Challenge of Pricing Combination Therapies. BCG Perspectives by The Boston Consulting Group.
- Guidance for Industry (2010) Codevelopment of Two or More New Investigational Drugs for Use in Combination. U.S. Department of Health and Human Services Food and Drug Administration. Center for Drug Evaluation and Research (CDER).
- Tallarida RJ (2001) Drug Synergism: Its Detection and Applications. J Pharmacol Exp Ther 298(3): 865-872.
- Jia J, Zhu F, Ma X, Cao Z, Li Y, et al. (2009) Mechanisms of drug combinations: Interaction and Network Perspectives. Nat Rev Drug Discov 8(2): 111-128.
- Barabasi AL, Oltvai ZN (2004) Network biology: understanding the cell's functional organization. Nat Rev Genet 5(2): 101-113.
- Boran AD, Iyengar R (2010) Systems approaches to polypharmacology and drug discovery. Curr Opin Drug Discov Devel; 13(3): 297-309.
- Spiro Z, Kovacs IA, Csermely P (2008) Drug-therapy networks and the prediction of novel drug targets. J Biol 7(6): 20.
- Huang S (2002) Rational drug discovery: what can we learn from regulatory networks? Drug Discov Today 7(Suppl 20): S163-S169.
- Csermely P, Agoston V, Pongor S (2005) The efficiency of multitarget drugs: the network approach might help drug design. Trends Pharmacol Sci 26(4): 178-82.
- Borisy AA, Elliott PJ, Hurst NW, Lee MS, Lehar J, et al. (2003) Systematic discovery of Multicomponent therapeutics. Proc Natl Acad Sci USA 100(13): 7977-7982.
- Imming P, Sinning C, Meyer A (2006) Drugs, their targets and the nature and number of drug targets. Nature Rev Drug Discov 5(10): 821-834.
- Paolini GV, Shapland RH, van Hoorn WP, Mason JS, Hopkins AL (2006) Global mapping of pharmacological space. Nat Biotechnol 24(7): 805815.
- Yildirim MA, Goh KI, Cusick ME, Barabasi AL, Vidal M (2007) Drug- target network. Nat Biotechnol 25(10): 1119-1126.
- Jürgen D (2003) Strategic trends in the drug industry. Drug Discov Today 8(9): 411-420.
- Jonker DM, Visser SA, van der Graaf PH, Voskuyl RA, Danhof M (2005) Towards a mechanism based analysis of pharmacodynamic drug-drug interactions in vivo. Pharmacol Therapeut 106(1): 1-18.
- Vilar S, Uriarte E, Santana L, Tatonetti NP, Friedman C (2013) Detection of Drug-Drug Interactions by Modeling Interaction Profile Fingerprints. PLOS One 8(3): e58321.
- Vilar S, Harpaz R, Uriarte E, Santana L, Rabadan R, et al. (2012) Drug- drug interaction through molecular structure similarity analysis. 2012. J Am Med Inform Assoc 19(6):1066-1074.
- Bjornsson TD, Callaghan JT, Einolf HJ, Fischer V, Gan L, et al. (2003) The conduct of in vitro and in vivo drug-drug interaction studies: A Pharmaceutical Research and Manufacturers of America (PhRMA) perspective. Drug Metab Dispos 31(7): 815-832.
- A. Akihiko Konagaya (2012) Towards an In Silico Approach to Personalized Pharmacokinetics, Molecular Interactions.
B. Zakharov AV, Varlamova EV, LaguninAA, Dmitriev AV, Muratov EN, et al. (2015) QSAR Modeling and Prediction of Drug-Drug Interactions. Mol Pharm 13(2): 545-556. - Charpentier G (2002) Oral combination therapy for type 2 diabetes. Diabetes Metab Res Rev 18(Suppl 3): S70-S6.
- Schmitt C, Hauptman J, Jadidi S (2015) Dosages of GIP/GLP-1 coagonist peptides for human administration. W02015035419 A1.
- McIntosh B, Cameron C, Singh S R, Yu C, Ahuja T, Welton NJ, et al. (2011) Second-line therapy in patients with type 2 diabetes inadequately controlled with metformin monotherapy: a systematic review and mixed-treatment comparison meta-analysis. Open Med 5(1): e35-e48.
- Setter SM, Iltz JL, Pharm D, Thams J, Campbell RK (2003) Metformin Hydrochloride in the Treatment of Type 2 Diabetes Mellitus: A Clinical Review with a Focus on Dual Therapy. Clin Ther 25(12): 2991-3026.
- Monami M, Lamanna C, Marchionni N, Mannucci E (2008) Comparison of different drugs as add-on treatments to metformin in type 2 diabetes: A meta-analysis. Diabetes Res Clin Pr 79(2): 196-203.
- Fleming JW, Fleming LW, Davis CS (2015) Fixed-dose combinations in type 2 diabetes - role of the canagliflozin metformin combination. Diabetes Metab Syndr Obes Target Ther 8: 287-294.
- Marathe PH, Arnold ME, Meeker J, Greene DS, Barbhaiya RH (2000) Pharmacokinetics and Bioavailability of a Metformin/Glyburide Tablet Administered Alone and with Food. J Clin Pharmacol 40: 1494-1502.
- Hauber A, Gale EAM (2006) The market in diabetes. Diabetologia 49(2): 247-252.






























