Cutaneous Presentation of Xylazine-Associated Wounds
Vrinda Madan and Joel C Sunshine*
Department of Dermatology, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA
Submission:February 22, 2024;Published:March 05, 2024
*Corresponding author: Joel Sunshine, Department of Dermatology, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA
How to cite this article:Vrinda Madan, Joel C Sunshine. Cutaneous Presentation of Xylazine-Associated Wounds. Open Acc J of Toxicol. 2024; 5(5):555675. DOI: 10.19080/OAJT.2024.05.555675.
Abstract
Xylazine, an alpha-2 adrenergic agonist primarily used in veterinary settings, has been increasing prevalent in the illicit drug supply. Recently declared as an emerging threat by the White House, xylazine has been associated with an alarming number of overdose-associated deaths. The use of xylazine has also been associated with a distinct ulceration pattern with necrotic features. The early recognition and treatment of these wounds becomes especially important as xylazine grows in prevalence.
This systematic review aims to summarize published case reports of xylazine-associated skin wounds, highlighting clinical presentation and treatment plans. The majority of patients presented with necrotic ulcerations, some of which extended deep into the fascia and bone. While most of the skin ulcerations occurred at the site of injection, there were also reports of lesions at distant locations. Among patients who received a skin biopsy, histopathological reports showed nonspecific inflammation and necrosis without vasculopathy. Laboratory workup was also ordered to further rule out vasculitis. Treatment plans consisted of antibiotics and local wound care, with surgical debridement required in one case. Wound care included Xeroform, silver impregnated dressing, hypochlorous acid-soaked gauze, and mupirocin followed by biologic dressing. Management required a multidisciplinary approach, including wound care specialists, dermatologists, plastic surgeons, hospitalists, and infectious disease specialists.
Given the relatively recent introduction of xylazine into the illicit drug market, there is currently no established guideline for the treatment and management of associated cutaneous ulcers. This review of the literature summarizes key dermatological findings, clinical workup, and management options to assist with the early detection and treatment of xylazine-associated skin wounds.
Keywords: Xylazine; Xylazine-Associated Skin Wounds; Necrotic Ulcer; Alpha-2 Agonist.
Introduction
Xylazine, a veterinary sedative not approved for human use, has been increasingly prevalent in the illicit drug supply as an additive to fentanyl, heroin, and cocaine [1] Reports of xylazine entering the drug market first emerged in Puerto Rico around the early 2000s [2,3]. A few years later in 2006, xylazine was documented in the continental United States, with Philadelphia and Connecticut appearing as epicenters [3, 4]. It has since spread rapidly across the country, with fentanyl and xylazine mixtures found in 48 states as of March 2023 [1]. The highest prevalence of xylazine-associated overdose deaths has been recorded in Philadelphia (25.8% of all drug-related mortality), Maryland (19.3%), and Connecticut (10.2%) [3]. National data also highlights an increase of 1238% in drug-poisoning deaths involving xylazine between 2018 and 2021 [1]. These alarming trends have prompted xylazine to be declared as an emerging threat by the White House in April 2023 - a designation that has triggered a national plan focused on comprehensive testing, treatment, data collection, supply regulation, and harm reduction strategies.
Clinically, xylazine is an alpha-2 adrenergic receptor agonist that rapidly blocks the release of norepinephrine [1, 5]. This results in hypotension, bradycardia, respiratory depression, and amnesia. Given that xylazine is not an opioid, it is not reversible by naloxone and can be challenging to treat. In addition to these physiologic effects, xylazine has also been associated with non-healing necrotic skin ulcers. A study conducted in Puerto Rico found a higher prevalence of skin ulcers (38.5% vs 6.8%) in those who used xylazine versus those who did not [6]. Additionally, several case reports have been published that highlight the progressive and necrotic nature of xylazine-induced skin wounds [7-12]. The ulcerations have a diffuse distribution, even presenting at sites distant from the injection. Mechanisms for these skin injuries likely involve the direct alpha-2 mediated vasoconstriction, subsequent decreased oxygen perfusion, and increased risk of superinfection [13-15].
With the rising prevalence of xylazine, it becomes increasingly important to appropriately diagnose and treat associated skin wounds. This paper aims to review currently published case reports of xylazine-induced cutaneous lesions to highlight clinical presentation and treatment plans. A PubMed query consisting of “xylazine,” “skin,” “wound,” and “ulcer" was conducted on December 2023, and papers highlighting individual patient cases were included.
Review
Nine patient reports of xylazine-associated skin wounds were identified in the literature. Table 1 summarizes the clinical presentation, imaging, microbiology, skin biopsy, and toxicology results along with treatment plans.
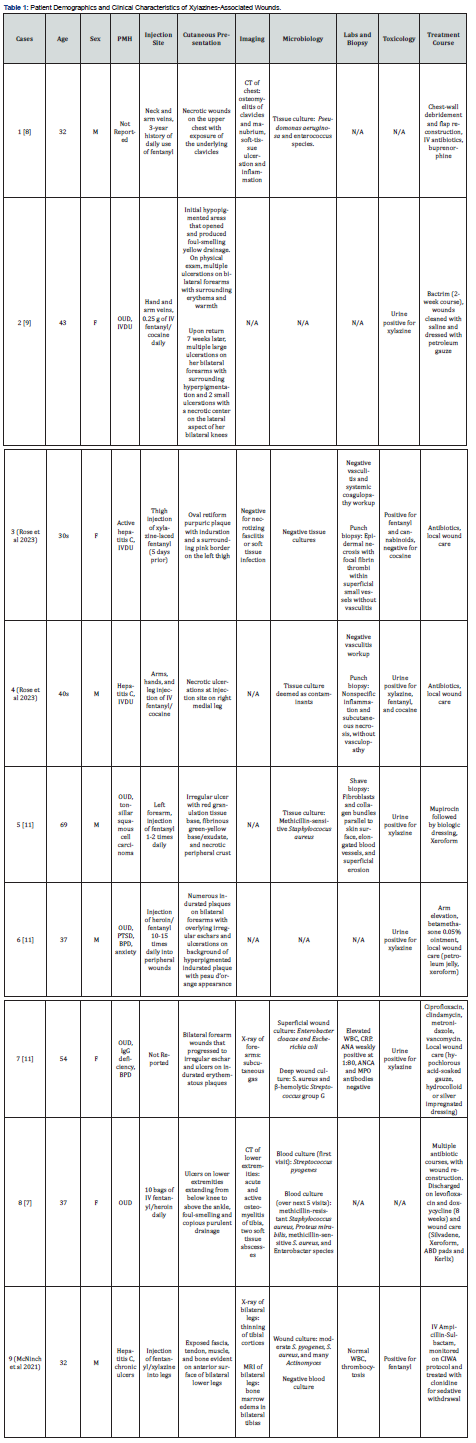
The majority of the patients were diagnosed with either opioid use disorder or IV drug use (7/9, 78%), and three had a history of hepatitis C (3/9, 30%). All reported injections involved fentanyl use (8/8, 100%), with 2 (2/8, 25%) combining it with cocaine, 2 (2/8, 25%) combining it with heroin, and 2 (2/8, 25%) with known xylazine combination. Cutaneous presentation involved necrosis in 6 (6/9, 67%) patients and foul-smelling purulent drainage in 2 (2/9, 22%) patients. The majority of the skin ulcerations occurred near the site of injection, with only 1 (1/9, 11%) report of skin lesions distant to injection site.
Imaging showed signs of definitive osteomyelitis in 2 patients (2/9, 22%) and inconclusive results in 1 patient (1/9, 11%). Additionally, there was 1 (1/9, 11%) report of necrotizing fasciitis on imaging. Bacteria identified in tissue culture included Staphylococcus Aureus (3/9, 33%), Streptococcus pyogenes (2/9, 22%), Pseudomonas aeruginosa (1/9, 11%), Actinomyces (1/9, 11%),and enterococcus species (2/9, 22%). Bacteremia was found in 1 patient (1/9, 11%), positive for Staphylococcus aureus, Proteus mirabilis, methicillin-sensitive S. aureus, and Enterobacter species.
Biopsies were reported in three patients (3/9, 33%), with 2 punch and 1 shave biopsy. Histopathological reports primarily showed necrosis without vasculopathy, superficial erosion, and nonspecific inflammation. To further rule out vasculitis, two patients also had negative laboratory workup that included negative ANA, ANCA, C3/C4, cryoglobulins, cryofibrinogen, fungitell assay, HIV, and RF results. Additional laboratory findings were reported in 2 patients, one of which had elevated WBC, CRP, and a weakly positive ANA (1:80) while the other patient had normal WBC and elevated platelets. While not a part of routine toxicology screening, xylazine was assessed in 5 patients and found to be positive in all (5/5, 100%).
Treatment primarily included antibiotics (8/9, 89%) and local wound care (9/9, 100%), with surgical debridement required in 1 case (1/9, 11%). Wound care included Xeroform (3/9, 33%), silver impregnated dressing (2/9, 22%), mupirocin followed by biologic dressing (1/9, 11%), and hypochlorous acid-soaked gauze (1/9, 11%).
Discussion
This paper summarizes nine recently published case reports of patients who presented with xylazine-associated skin wounds - delineating physical exam findings, imaging, laboratory workup, and treatment plans. The most common clinical characteristics of these wounds included necrotic eschars primarily at the site of injection. Additionally, foul-smelling purulent discharge was also noted. Given the increased risk of infection, the majority of patients had imaging and microbiology workup to assess for osteomyelitis, necrotizing fasciitis, and soft tissue infection. Laboratory workup was also conducted in some patients to rule out underlying vasculitis or coagulopathy. Skin biopsies further corroborated findings pointing to xylazine-induced ulcers, showing necrosis without vasculopathy.
The diagnosis of xylazine cutaneous manifestations can be challenging, especially given that this substance is not currently a part of routine toxicology screening. Xylazine toxicity should be included in the differential of severe ulcers especially in the setting of suspected intravenous drug use, non-response to naloxone, and in regions where xylazine is more prevalent. However, it is also important to rule out other differentials such as ulcers induced by levamisole, pentazocine, and cocaine. Other differentials include vasculitis ulcers, pyoderma gangrenosum, and necrotizing fasciitis. Skin biopsy and laboratory workup can be helpful in narrowing down the diagnosis.
Among the reviewed case reports, treatment options focused largely on local wound care and antibiotics. Given the recent presentation of xylazine-associated skin wounds, there are currently no central guidelines for wound care. Case reports have utilized various options including Xeroform, silver impregnated dressing, mupirocin followed by biologic dressing, and hypochlorous acid-soaked gauze. One report also noted that an intensive outpatient treatment program, along with an increase in methadone dose, enabled the cessation of IVDU and subsequent regression of necrotic ulcers.
Conclusion
The management of xylazine-associated wounds requires a multidisciplinary approach, drawing expertise from wound care specialists, dermatologists, plastic surgeons, infectious disease specialists, and hospitalists, to name a few. Additionally, careful attention must be placed on the social barriers such as dressing affordability, appointment frequency, and other patient-specific factors. Furthermore, this clinical management must occur in concurrence with broader public health initiatives that aim to decrease illicit drug supply and provide support to individuals struggling with opioid use disorder. In summary, this review highlights key clinical characteristics of reported cases of xylazine-associated skin wounds - aiming to increase clinician awareness and call for interdisciplinary management approaches.
References
- Gupta R, Holtgrave DR, Ashburn MA (2023). Xylazine-medical and public health imperatives. New England Journal of Medicine 388(24): 2209-2212.
- Rodríguez N, Vidot JV, Panelli J, Colón H, Ritchie B, et al. (2008) GC-MS confirmation of xylazine (Rompun), a veterinary sedative, in exchanged needles. Drug Alcohol Depend 96(3): 290-293.
- Friedman J, Montero F, Bourgois P, et al. (2022) Xylazine spreads across the US: A growing component of the increasingly synthetic and polysubstance overdose crisis. Drug Alcohol Depend 233: 109380.
- Alexander RS, Canver BR, Sue KL, Morford KL (2022) Xylazine and overdoses: Trends, concerns, and recommendations. Am J Public Health 112(8): 1212-1216.
- Pergolizzi J, Le Quang JAK, Magnusson P, Miller TL, Breve F, et al. (2023) The new stealth drug on the street: A narrative review of xylazine as a street drug. Cureus 15(6): e40983.
- Reyes JC, Negrón JL, Colón HM, et al. (2012) The emerging of xylazine as a new drug of abuse and its health consequences among drug users in puerto rico. J Urban Health 89(3): 519-526.
- Malayala SV, Papudesi BN, Bobb R, Wimbush A (2022) Xylazine-Induced Skin Ulcers in a Person Who Injects Drugs in Philadelphia, Pennsylvania, USA. Cureus 14(8): e28160.
- O Neil J, Kovach S (2023) Xylazine-associated skin injury. N Engl J Med 388(24): 2274-2274.
- Warp PV, Hauschild M, Tookes HE, Ciraldo K, Serota DP, et al. (2023) A confirmed case of xylazine-induced skin ulcers in a person who injects drugs in miami, florida, USA.
- Bishnoi A, Singh V, Khanna U, Vinay K (2023) Skin ulcerations caused by xylazine: A lesser-known entity. J Am Acad Dermatol 89(2): e99-e102.
- Dowton A, Doernberg M, Heiman E, et al. (2023) Recognition and treatment of wounds in persons using xylazine: A case report from New Haven, connecticut. J Addict Med 17(6): 739-741.
- Wallace L (2021) A case of skin necrosis caused by intravenous xylazine abuse. Journal of Hospital Medicine.
- Zwick LS, Patrick DJ, Knupp LC, Ramos MF (2021) Ketamine/xylazine anesthesia-related corneal lesions in rats with surgically implanted venous catheters utilized in nonclinical intravenous studies. Toxicol Pathol 49(3): 598-601.
- Liu C, Chiu M, Fang C, Chen W (2007) Xylazine abuse: A rare cause of syncope. Clin Toxicol (Phila) 45(3): 309-311.
- Greene SA, Thurmon JC. (1988) Xylazine - a review of its pharmacology and use in veterinary medicine. J Vet Pharmacol Ther 11(4): 295-313.






























