Initial Assessment of the Minamata Convention on Mercury in Dentistry in Senegal
Touré Aminata1,2*, Lam Absa1,2, Bah Fatoumata1,2, Diop Cheikh1, Aminata Sarr2, Mbaye Diaw Dioum1, Aida Kanouté3, Fall Mamadou1,2 and Cabral Mathilde1,2
1Department of Toxicology and Hydrology, Cheikh Anta Diop University of Dakar, Senegal
2Poison Control Centre, Ministry of Health and Social Action, Senegal
3Department of Oral Health, Ministry of Health and Social Action, Senegal
Submission: August 30, 2021; Published: September 23, 2021
*Corresponding author: Aminata Toure, Department of Toxicology and Hydrology, Faculty of Medicine, Pharmacy and Dentistry, Cheikh Anta Diop University of Dakar, Senegal
How to cite this article: Touré A, Lam A, Bah Fa, Diop C, Aminata S, et al. Initial Assessment of the Minamata Convention on Mercury in Dentistry in Senegal. Open Acc J of Toxicol. 2021; 5(2):555656. DOI: 10.19080/OAJT.2021.05.555656.
Abstract
Mercury is a heavy metal widely distributed in the world. Its impact on the environment and on human health is an ongoing concern. Despite its high toxicity, mercury is subject of several uses. It is in particular the main component of dental amalgam used for more than a century to fill decayed teeth. In order to protect human health and the environment against anthropogenic emissions and discharges of mercury and mercury compounds, international organizations have established the Minamata Convention on Mercury. This convention is an international instrument with provisions relating to the entire life cycle of mercury and its level of use around the world. The present work, which aimed to study levels of use and conditions of management and elimination of mercury in dental practices in Dakar, falls within the framework of the initial assessment of the Minamata Convention in Senegal.
The study was carried out in 30 public and private dental offices in Dakar region, chosen from a reasoned sampling. A semi-structured interview made it possible to administer questions relating to the levels of use of dental amalgams, the production of waste contaminated by mercury, the management of this waste and the knowledge of the dangers, the risks, and procedures for taking into account burden and prevention of exposure.
The results obtained showed that dental amalgam remains the most used material, with 93.33% of dental offices using pre-dosed 2g mercury capsules. A total of 132.74 amalgams are performed on average per practice per year. The total amount of mercury used by dental offices in Senegal is estimated to be around 106.192kg per year. The management of waste containing mercury in the dental offices studied is problematic insofar as the professionals of these structures do not have a specific plan and that only 3.33% of these dental offices have a manual for the management of waste containing mercury. Among the health personnel met, 60% said they were aware of the effects of mercury on health.
These results show a still significant use of mercury and problems of management of amalgam waste in dentistry in Senegal. The plan for implementing the Minamata Convention in Senegal should include training and awareness-raising for dentists for better adoption of the guidelines.
Keywords: Mercury; Toxicity; Minamata convention; Dental offices; Dental amalgam; Waste management
Context
Nowadays, human activities of all kinds have led to widespread pollution. Pollution caused by the release of harmful substances such as metals found in the environment and or in processed food is an ongoing health concern. Some of these released metals have a known biological role whereas others such as cadmium (cd), mercury (Hg), arsenic (As) and lead (Pb) have no known biological role and cause harmful effects even at low doses.
Mercury (Hg) is an element naturally present in the environment, mainly resulting from volcanic actions, weathering of rocks, forest fires, etc. [1]. The problem of the toxicity of Hg is mainly justified by human activities resulting in the release of large amounts of mercury into the environment, which can then circulate freely for thousands of years [2-5]. Mercury pollution is of international concern because of its considerable potential danger to the environment and public health [6-8]. The circumstances of exposure and toxicity in humans are closely related to the state of mercury, which exists in three chemical forms: elemental or metallic mercury, inorganic mercury derivatives and organic derivatives [9].
Worldwide regulation since 1980 of mercury consumption and the efforts focusing on prevention, particularly in the workplace, resulted in almost complete elimination of serious mercury poisoning [10,11]. Exposure levels are certainly lower, but the impact on health is debated and necessitates local and global measures to reduce mercury releases and limit its in raw or processed products [12]. In 2007, the World Health Organization (WHO) recognized that the safety and sustainable management of health care waste is an imperative public health issue and a responsibility of all. However, in many developing countries around the world, this alarm seems to be ignored [13].
Senegal is a country that neither produces or process mercury. However, the presence of this metal in certain instruments and materials in health structures (such as thermometers, tensiometers) and its use in dentistry for the fillings of decayed teeth, explain the possible risks of exposure and mercury poisoning in healthcare settings.
Senegal is one of the countries that have signed and ratified the Minamata Convention on Mercury. This global treaty aims to protect human health and environment from the negative effects of mercury. Thus, it benefited from funding from the Global Environment Facility (GEF) for an Initial Assessment of the Minamata Convention (MIA) in order to enable political and strategic decision-making and to prioritize areas for future interventions.
This work is part of this program, which aimed to study levels of use and conditions for the management and elimination of mercury in dental offices in Dakar (Senegal).
Methodology
Type and duration of the study
This was a retrospective descriptive study conducted on data recorded in the period July 15, 2017, to August 10, 2017.
Study setting and population
Thirty dental practices (public and private) distributed in the 4 departments of the Dakar region (Dakar, Pikine, Guédiawaye and Rufisque) participated in the study.
Selection criteria, sampling, and sample size
The main criterion used for the selection of dental practices was registration in the database of the Oral Health Division (Division de la Santé Bucco-Dentaire) and obtaining the authorization to practice for private individuals, granted by the ministry in charge of health. Reasoned choice sampling made it possible to select the most frequented services in the region. Finally, thirty (30) dental practices (public and private) were selected in collaboration with the Oral Health Division (Division de la Santé Bucco-Dentaire) of the ministry in charge of health.
Variables studied, measurements and data collection
Variables relating to the use of mercury, the generation of mercury-contaminated wastes and the management of these wastes were studied. To do this, we inspired from the validated WHO-Brazzaville Team’s questionnaire with sections collecting data on type of selected practice, the level of mercury used (or other metal), mercury-contaminated waste management, knowledge, and training on mercury-waste management. At the level of each dental office, a semi-structured interview targeted the head of office, which allowed the investigator to directly fill in the questionnaire in order to measure the level of mercury use employed in dental offices in Dakar at the initial stage of the Minamata convention.
Ethical issues
This study did not involve any direct risk neither for the research team nor for the establishments’ personals appointed by the authorities to answer the questions. In addition, the data collected, although not concerning private life, were used by the team within the framework of this study only or for any other scientific use aimed at achieving the objectives of the Minamata Convention, signed Senegal. A circular letter from the Minister of Health and Social Action served as a passport to the authorities of the various structures identified and to introduce the investigators to the heads of the dental offices visited.
Data analysis
The EPI Info software, version 7.2 was used for the statistical analyzes. Means and standard deviations were calculated for each quantitative variable. The Mann-Whitney test was used to compare groups; the significance level was set at p <0.05. The use of the completed questionnaires made it possible to present results on the distribution of dental offices visited, the health personnel encountered, the type of dental restoration carried out, the use and management of dental amalgam waste by health personnel, mercury knowledge and training level on the management of mercury-containing wastes.
Results
Distribution of dental offices visited
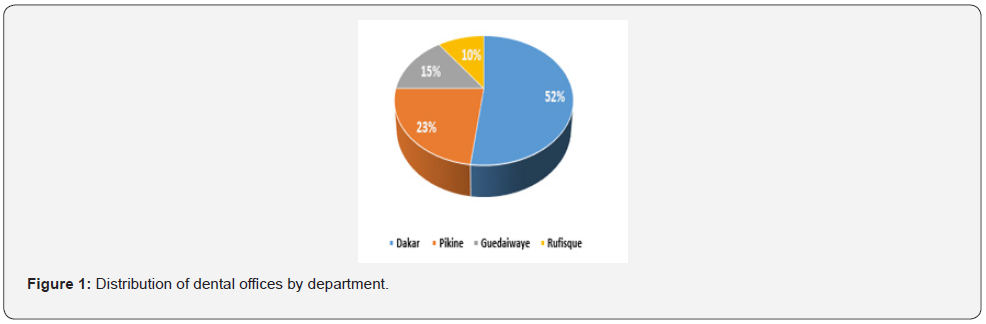
The distribution of dental offices of the study in Dakar departments of is presented in (Figure 1). Of these offices, thirtythree percent (33%) are private and 67% are public.
Health personnel encountered
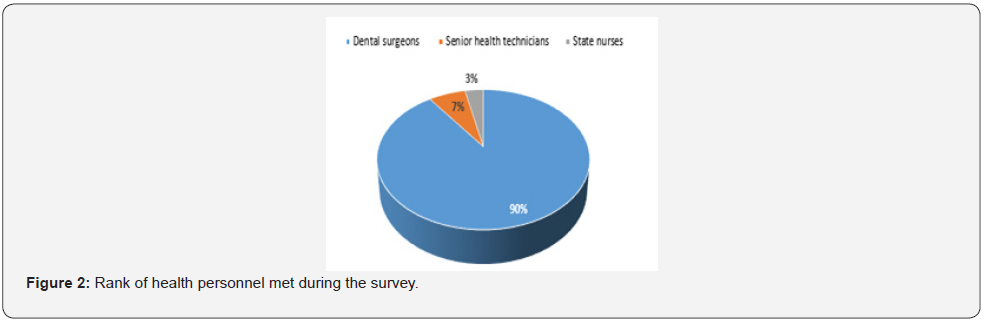
The majority of health professionals met in dental offices were dental surgeons (27/30). Senior health technicians (2/30) and state nurses (1/30) were also found (Figure 2).
Type of dental restoration performed
Several types of dental restorations were performed in the dental offices of the study. Dental amalgams used are most often in the form of pre-dosed capsules of 2g of mercury, suitable for use for a single dental restoration. Twenty-eight (28) of 30 dental offices (93.33%) used these types of dental amalgams. Almost all these structures used other types of materials such as glass ionomer cements and composites in addition to dental amalgam. Indeed, 90% of private structures used these associations against 80% of public structures (without significant difference).
Use and management of dental amalgam waste by health personnel
Amount of mercury used for dental amalgam
It was noted that dental offices perform an average of 34.42 restorations per month, or a little more than one restoration per day. Public structures, with a monthly average of 42.00, achieved much more than the private ones, which totaled an average of 30.22 (p ˂ 0.05).
In form of pre-dosed capsules, an average of 132.74 amalgams were used per practice per year (private and public combined). This value does not take into account the use of bulk mercury for restorations, the amount of which is not estimated by users. Thus, when the quantities of pre-dosed capsules used are taken into account, an average quantity of 265.48 g of mercury is used per dental office and per year. By extending it to the number of dentists officially registered with the Order and authorized to practice in Senegal, which was 400, the total quantity of mercury used by dental offices would be of the order of 106,192g, i.e., 106,192kg per year for all dental offices in Senegal.
Collection and storage of dental amalgam waste
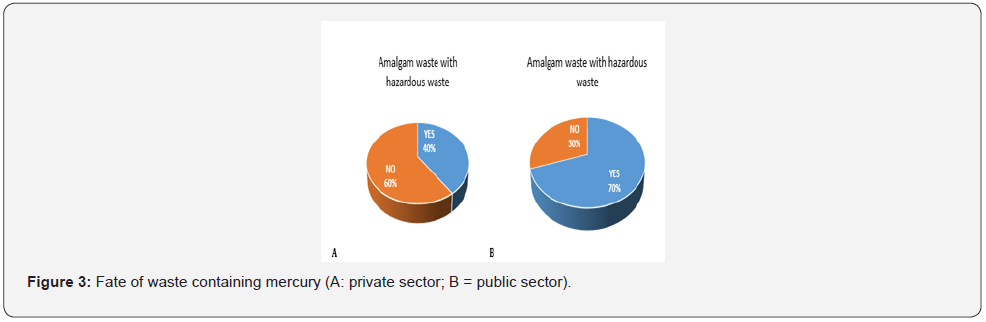
The waste found consists of mercury from old amalgams, predosed capsules, remaining liquid and amalgam powder. Half of dental offices throw away amalgam waste with hazardous waste, known as infectious waste. Public dental structures carry out this practice more (70% of them) than private structures (40%) (Figure 3). Study shows that 10% of public dental offices and 35% of private dental offices eliminate mercury-contaminated waste in bulk waste. Five percent (5%) of private dental practices and 50% of public dental practices place amalgam waste in a specific container or container (Figure 4). All these differences in private and public sector were significant (p ˂ 0.05). But in all cases, all the waste ends up in a wild landfill behind the buildings of the dental offices or in the Mbeubeuss landfill (open dump).
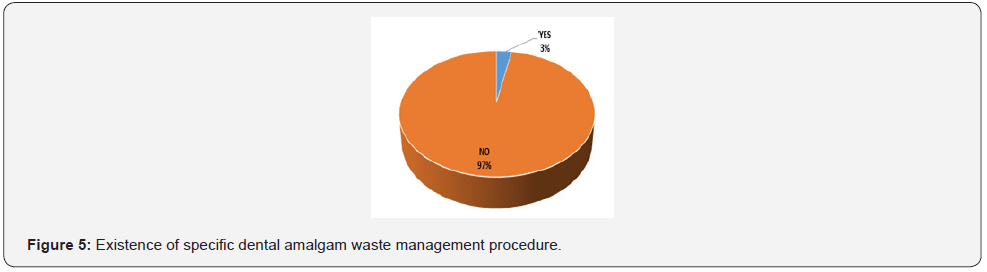
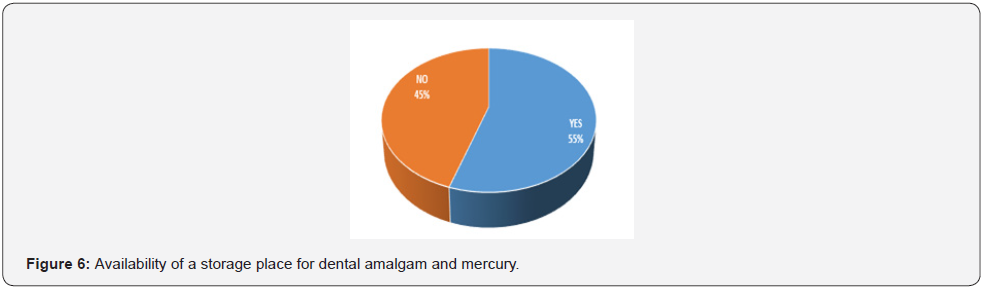
Dental office staff were questioned about the existence of specific procedures for managing dental amalgam waste and about the existence of a place to store these amalgams. Only 3% of the dental offices surveyed claimed to have specific procedures for the management of amalgam waste; they were all public cabinets (Figure 5). Private dental offices do not have specific procedures for the management of amalgam waste but 55% of them said they have a storage place for dental amalgam and mercury (Figure 6) compared to only 10% of public offices with a significant difference (p ˂ 0.05).

Mercury knowledge and training on the management of mercury-containing waste
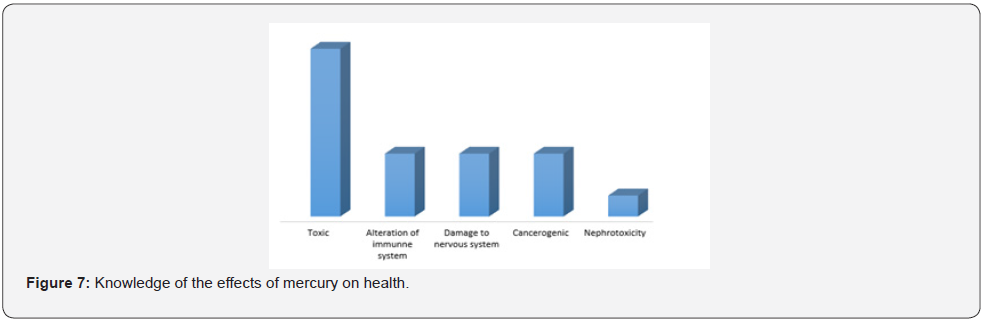
Knowledge of the different sources of mercury exposure was also assessed and 53.33% of health staff in dental offices had a notion of the different sources of exposure to mercury (16 out of 30 surveyed). Among the 20 private dentists, 65% answered yes to the question (therefore have knowledge) while among dental staff in the public sector, only 30% (3/10) had an idea about the sources of exposure to mercury. These sources of mercury exposure included the release of mercury from dental amalgams into the oral mucosa, energy-saving lamps, and atmospheric exposure through deposition on food crops. Dentists are generally aware of the effects of mercury on the health of humans. Indeed, 60% of the practitioners questioned answered yes to this question and the various ailments on human health mentioned are presented (Figure 7).
Most dentists (81%) state that they have never received training in the management of waste contaminated by mercury and the various stages of this management are not always known or mastered. However, half of private dentists want to limit the use of instruments containing mercury by adopting alternative methods, while in the public, this project does not exist.
Discussion
The objective of this work was to study the levels of use and the conditions of management and elimination of mercury in dental offices in Dakar (Senegal).
Validity of results
It is possible that the results obtained suffer from some selection and information bias due to the reasoned choice of dental practices retained and the declarative data of health personnel. However, these minimized biases cannot invalidate these results obtained from data from sworn people (27 dental surgeons, 2 senior technicians, 1 state nurse) invited by a circular letter from their supervisory ministry. These results have enabled us to note a still significant use of mercury in dental offices in the Dakar region. This significant use of mercury has been observed in Tunisia and Cameroon where dental amalgam constitutes one of the main sources of biomedical waste from hospitals [14,15].
Waste management
The management of mercury-based materials has been ensured mainly by dental surgeons. However, in three structures out of thirty, senior health technicians and nurses were responsible of management of the stock of material and waste, as was the case in India [16]. The number of dental amalgam restorations performed differs depending on the private or public status of the dental offices visited. Estimate of the total amount of mercury consumed or generated in terms of waste could not be performed because values obtained do not consider use of bulk mercury in restorations.
Dental amalgams generate waste that is managed in several ways. Half of dental offices throw out amalgam waste with hazardous waste. The concept of risky waste is relative, especially since sorting at source, collection and transport are steps in waste management that do not always take place correctly. Our study shows that mercury-contaminated waste was, in certain case, eliminated in bulk waste to be then transported to open dumps. These practices were especially recurrent in public structures.
In addition, only 17% of the dental offices visited have a biomedical waste management procedure manual and only 3.33% have a waste amalgam and mercury-containing waste management procedure manual. A small percentage of staff have received training in waste management in dental offices. De facto, the dangers associated with the use of materials and instruments containing mercury are not identified or assimilated by professionals in dental offices.
Exposure and risk to humans and the environment
The most common risk of occupational exposure to mercury is inhalation of vapors given off by liquid mercury. The lack of proper cleaning of mercury spilled even in very small quantities, particularly because of dispersion of vapors and dust of metallic mercury is often observed at the time of preparation for the laying of amalgam, thus constituting a very important source of exposure to this metal. Indeed, this air contamination exceeds the recommended limit and can have serious health consequences [17]. Because mercury vapor is odorless and colorless, it can be inhaled insidiously and over long periods of time without any immediate effects detected. However, it can happen that mercury beads get lodged in cracks or adhere to porous materials such as carpets, fabrics or wood and then be extremely difficult to remove. When mercury has been spilled, traces may remain under the shoes. If these soils are poorly cleaned and disposed of, patients who are already debilitated and caregivers risk a dangerous exposure [18].
As long as the mercury is trapped in the original material (amalgam, thermometer, etc.), toxicity is reduced, and mercury only becomes dangerous when it is released. Particular attention has been paid in recent years to the risk of mercury poisoning in the general population, linked to the wearing of dental amalgam containing mercury, but also silver, copper, tin, and zinc. Indeed, several studies have shown a release of mercury from dental amalgams into the oral cavity, which is then inhaled and then absorbed [19,20]. The disposal practices used are most often: open burning, discharge into drains, routing, and burial of waste in Mbeubeuss Lindfil, collection and storage with household waste among many others. All these practices expose the general population in addition to health professionals to the dangers associated with mercury but also expose the environment.
When these releases reach the level of environmental matrices, in particular water and soil, the methylation of Hg2 + into methylmercury (MeHg) takes place by sulfato-reducing bacteria. This organic form is subsequently bioaccumulated especially by fish and biomagnified along the trophic chain with high concentrations in large predatory fish. Thus, the piscivorous fish located at the top of the food chain have a high concentration of methylmercury. The general population consuming such fish is then exposed to this organomercurial compound [21-23]. Improper disposal of mercury-containing wastes is tantamount to exposing the general population to mercury through the food chain. This participates in, animates, and even strengthens the mercury cycle in the environment.
Level of application of the Minamata Convention
The goal of Minamata Convention is to protect human health and environment from anthropogenic emissions and releases of mercury. So, to this end, its provisions cover the entire mercury life cycle, including controlling and reducing a wide range of products, processes and industries that use, release, or emit mercury. This is the reason why Minamata Convention prohibited any country having ratified the said convention, control and use of mercury-based devices (thermometers, tensiometers, etc.) from 2020. But this rule does not yet take dental amalgam into account. WHO expert consultation held in 2009 [24] concluded that a short-term global ban on dental amalgam would pose a problem for public health and the dental sector. In contrast, phasing out should be considered through the promotion of preventive measures and alternatives to amalgam, research and development of inexpensive alternatives, education of dental professionals and public awareness.
In this dynamic, our study showed that majority of dentists (60%) in Dakar have a plan to replace dental amalgam with their alternatives (examples: glass-ionomers and composites). Currently, there is no longer any doubt about the toxicity of mercury because it has caused a lot of damage, especially in all the continents [25,26]. But debate on dangers of dental amalgam remains mixed as there is not yet unanimity on whether dental amalgam represents a danger to human health or not. For reasons of operating budget and technical resources, substitution of mercury-based instruments has not yet been integrated into the technical and administrative management plan of public dental offices in Senegal.
On the other hand, in the general population, it is a chronic exposure to very low-level mercury and the only demonstrated effects of dental amalgam are local with inflammatory reactions (pulpitis, lichen planus), disappearing within a few months after removal of the dental fillings [10,27]. In some studies, no effect on renal or neuropsychological function has been demonstrated in children with dental amalgam [17,28]. In 2003, Afssaps set up a working group with an exhaustive bibliographic analysis on the state of knowledge on dental amalgam fillings. In a report published in 2005 [10], no evidence of a causal relationship between the presence of amalgams in the mouth and systemic symptoms or pathologies could be provided. Nevertheless, Afssaps recommends only based on the precautionary principle that the insertion or removal of amalgam fillings be avoided during pregnancy or breastfeeding [21]. Several epidemiological studies have raised the hypothesis of a link between the wearing of dental amalgams and the occurrence of neurodegenerative diseases, such as amyotrophic lateral sclerosis, Parkinson’s disease, and Alzheimer’s disease without providing epidemiological or experimental evidence sufficient to demonstrate a causal link [10,29]. But, given that mercury is undoubtedly toxic and that it is contained in dental amalgams, the ideal is to avoid its use as a precaution as recommended by Afssaps [10].
Minamata Convention was therefore drawn up with the aim of limiting or even abandoning the use of mercury-based products. However, for the limitation of the use of the latter to be effective, it is necessary to have good information and awareness on the risks of contamination of mercury-based devices among all health workers (doctors, dental surgeons, pharmacists, …). In this regard, it is one of the objectives of the Minamata Convention, information, public awareness, and education on the dangers associated with mercury but also the training of health personnel on the identification of poisoning, symptoms of mercury poisoning and possibly principles of treatment. According to our study, the handling of amalgam is mostly done by dental surgeons. Thus, the risk of mercury contamination is higher among them. However, the risk to maintenance workers, patients and others who work in the dental office environment should not be minimized. These results are in line with what other studies have shown [12,15,16].
Conclusion
The mercury in dental amalgams combined with poor management can be the source of intoxication, especially for dental surgeons and their employees. The tendency for these health professionals would be to replace dental amalgams with alternative materials in the long or short term, which would join the recommendation of the Minamata Convention to abandon their use in favor of alternative materials. In public sector, we noted more compliance with the guidelines of the Minamata Convention, compared to private structures. This could be explained by the fact that public dental offices are housed in health structures (health center, hospitals) which generally receive training in waste management. Management of mercurycontaminated waste, adoption of an amalgam substitution plan, acquisition of knowledge about mercury and its effects on health and environment are elements that are better integrated in the public sector than in the private sector. This observation suggests a better harmonization of axes of awareness and communication on Minamata Convention but also a more effective involvement of private sector in adoption and implementation of the conventions in different countries. This present work should therefore be continued to see the evolution of the practices of dental surgeons according to the recommendations of the Minamata Convention.
References
- Sheu GR, Lin NH (2011) Mercury in cloud water collected on Mt. Bamboo in northern Taiwan during the northeast monsoon season. Atmos Environ 45(26): 4454-4462.
- Bernhoft RA (2012) Mercury toxicity and treatment: a review of the literature. J Approx Public Health 2012: 460508.
- Focus E, Rwiza MJ, Mohammed NK, Banzi FP (2021) Health Risk Assessment of Trace Elements in Soil for People Living and Working in a Mining Area. J Environ Public Health 2021: 9976048.
- Bradl HB (2005) Heavy metals in the environment: origin, interaction and remediation. Elsevier Academic Press 6: 282.
- Howard D, Nelson PF, Edwards GC, Morrison AL, Fisher JA, et al. (2017) Atmospheric mercury in the southern hemisphere tropics: seasonal and diurnal variations and influence of inter-hemispheric transport. Atmos Chem Phys 17: 11623-11636.
- Zheng L, Tang Q, Fan J, Huang X, Jiang C, et al. (2015) Distribution and health risk assessment of mercury in urban street dust from coal energy dominant Huainan City, China. Environ Sci Pollut Res Int 22(12): 9316-9322.
- Tucaliuc OM, Cretescu I, Nemtoi G, Breaban IG, Soreanu G, et al. (2014) Monitoring of mercury from air and urban dust in the industrial area of Iasi municipality. Environ Eng Manag J 13(8): 2051-2061.
- RAIS (2018) RAIS (The Risk Assessment Information System, Toxicity Profiles, Condensed Toxicity Summary for Mercury.
- Bensefa Colas L, Andujar P, Descatha A (2011) Mercury poisoning. Rev Med Interne 32(7): 416-424.
- United Nation Environment Program (UNEP) - Chemicals. Global Mercury Assessment. Geneva, 2002. 266 pages.
- Lauwerys RR, Haufroid V, Hoet P, Lison D (2007) Mercury. In: Industrial toxicology and occupational poisoning. Paris, Elsevier Masson pp 309-363.
- Clarkson TW (2002) The three modern faces of mercury. Environ Health Perspect 110(1): 11-23.
- Georgescu C (2011) Report of the Special Rapporteur on the adverse effects of the movement and dumping of toxic and dangerous products and wastes on the enjoyment of human rights. Humans Rights Council 25.
- Kuepouo G (2013) Estimating environmental release of mercury from medical-thermometers and potential “hot spot” development: Case study of need for improved waste management capacity in Cameroon. Resour Conserv Recycl 71: 48-52.
- Chadli Debbiche A, Allani R, Jouini R, Abidi Emna, Nouri A, et al. (2018) Mercurial hospital waste: management, becoming and recommendations. Tunis Med 96(5): 273-280.
- Viragi PS, Ankola AV, Hebbal M (2013) Occupational hazards in dentistry-Knowledge attitudes and practices of dental practitioners in Belgaum city. J Pierre Fauchard Acad 27(3): 90-94.
- Magos L, Clarkson TW (2006) Overview of the clinical toxicity of mercury. Ann Clin Biochem 43(4): 257-268.
- Mason RP (2008) Mercury Emissions from Natural Sources and their Importance in the Global Mercury cycle, Mercury fate and transport in the Global atmosphere: Measurements, models and policy implications In: Pirrone N, Mason R, UNEP 19: 173-191.
- Bose OReilly S, Lettmeier B, Shoko D, Roider G, Drasch G, et al. (2020) Infants and mothers levels of mercury in breast milk, urine and hair, data from an artisanal and small-scale gold mining area in Kadoma/Zimbabwe. Environ Res 184: 109266.
- Sahakyan L, Tepanosyan G, Maghakyan N, Kafyan M, Melkonyan G, et al. (2018) Contamination levels and human health risk assessment of mercury in dust and soils of the urban environment, Vanadzor, Armenia. Atmos Pollut Res 10(3): 808-816.
- Schmeltz D, Evers DC, Driscoll CT, Artz R, Cohen M, et al. (2011) MercNet: a national monitoring network to assess responses to changing mercury emissions in the United States. Ecotoxicology 20(7): 1713-1725.
- Horvat M, Gibicar D (2005) Speciation of Mercury: Environment, Food, Clinical, and Occupational Health in “Handbook of Elemental Speciation II”, John Wiley and Sons, LTD, England pp 737.
- UNEP (2002) Chemicals. Global Mercury Assessment, Geneva: 372.
- National Order of Dental Surgeons (ONCD, France) (2010) Dental amalgam: the European Court of Justice in favor of free movement pp 116.
- Suvda D, Davaadorj R, Baatartsol D, Unursaikhan S, Tsengelmaa M, et al. (2015) Toxicity assessment in artisanal miners from low-level mercury exposure in Bornuur and Jargalant soums of Mongolia. Procedia Environ Sci 30: 97-102.
- Tseng CF, Chen KH, Yu HC, Huang FM, Chang Y (2020) Dental Amalgam Fillings and Multiple Sclerosis: A Nationwide Population-Based Case - Control Study in Taiwan. Int J Environ Res Public Health 17(8): 2637.
- McParland H, Warnakulasuriya S (2012) Oral Lichenoid Contact Lesions to Mercury and Dental Amalgam - A Review. J Biomed Biotechnol 2012: 589569.
- DE Rouen TA, Martin MD, Leroux BG, Townes BD, Woods JS, et al. (2006) Neurobehavioral effects of dental amalgam in children: a randomized clinical trial. JAMA 295(15): 1784-1792.
- Cilliers K (2021) Trace element alterations in Alzheimer's disease: A review. Clinical anatomy 34(5): 766-773.






























