Rare Presentation of Amyotrophic Lateral Sclerosis as Frontotemporal Dementia: A Case Report
Javeria Sahib Din1, Faiza Farooq2, Ali Mahmood Khan3*, Naveed Ahmed Shaikh2 and Abdul Mohit4
1Bergen Regional Medical Center, USA
2Kings County Hospital Center, USA
3Manhattan Psychiatric Center, USA
4Behavioral Health Center, USA
Submission: July 31, 2017; Published: August 16, 2017
*Corresponding author: Ali Mahmood Khan, Manhattan Psychiatric Center, New York, USA, Email: ali_mahmood_khan@hotmail.com
How to cite this article: Javeria S D, Faiza F, Ali M K, Naveed A S, Abdul M. Rare Presentation of Amyotrophic Lateral Sclerosis as Frontotemporal Dementia: A Case Report. Open Acc J of Toxicol. 2017;1(4): 555566. DOI: 10.19080/OAJT.2017.01.555566
Abstract
Amyotrophic Lateral Sclerosis is also known as motor neuron disease or Lou Gehrig's disease. It mainly involves neurons which control voluntary functions. It is characterized by weakness and atrophy of muscles. It can also cause death by respiratory failure. Our case is a 53-years old female with Frontotemporal dementia (FTD), who after two years of stay at a psychiatric facility manifested symptoms of Amyotrophic Lateral Sclerosis (ALS). The patient stayed four and a half years in the hospital, mostly in the psychiatric facility. We have discussed the course of her illness as it progressed, to describe the surprising association between ALS and FTD. A good deal of research has been conducted in this context in the past decades. Genetic, biochemical and clinical associations between the two conditions have been discussed in the later part of this report.
Introduction
This study is aimed is to study the relationship between Amyotrophic Lateral Sclerosis (ALS) and Frontotemporal dementia (FTD). There have been genetic and biochemical linkages found between the two conditions. ALS usually manifests with the symptoms of frontotemporal dysfunction syndromes or preceding them. However, there have been instances where ALS begins in the final stages of frontotemporal dementia.
Case Presentation
Our patient is a 53-year old previously domiciled, unemployed, Caribbean female with no past history of psychiatric illness. The patient was brought to the Comprehensive Psychiatric Emergency Program (CPEP). Patient has been decompensating with symptoms of paranoid delusions, wandering and poor personal hygiene. MMSE (Mini Mental State Examination) of the patient on presentation was 15.
In the unit, the patient was started on Olanzapine for her psychotic symptoms. The dose of Olanzapine was tapered up to 20mg daily dose. MRI (Magnetic Resonance Imaging) report which demonstrated "Bitemporal and Bifrontal atrophy" as shown in the image. Thus, the patient was further diagnosed with "Frontotemporal dementia" by the neurologist. The patient was later kept at a daily dose of 5mg of Olanzapine for irritability and psychosis.
Over the next two years of hospital stay, the patient developed contractures of fingers, a progressive difficulty of moving upper extremities and later became mute. The patient was able to sign her name a year ago but now signs a line usually. Patient has little social support and multiple attempts at transferring the patient to a permanent nursing care facility were futile. During the course of her illness, the patient developed difficulty swallowing. An Electromyography (EMG) was performed by neurology department and the patient was further diagnosed with Amyotrophic Lateral Sclerosis (ALS).
The patient required a percutaneous endoscopic gastrostomy (PEG) tube and ventilator placement during the course of her illness after being diagnosed with ALS. The patient was tapered off Olanzapine and demonstrated no aggression or mood symptoms at baseline. However, the episodes of choking and swallowing difficulty were witnessed which required follow up with speech/swallow pathologist, which en-turn led to a Gastroenterology [GI) consult. GI team after assessing the patient decided to intervene with PEG tubeplacement and keeping the patient nothing per oral (Figure 1).
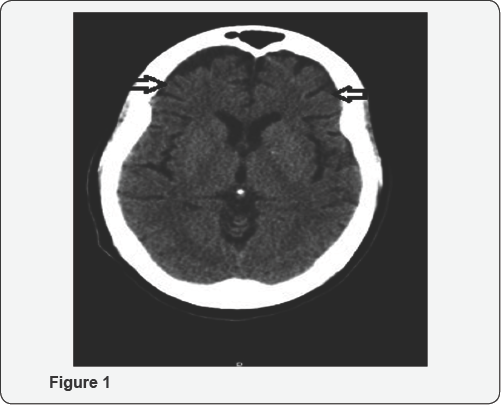
Upon discharge of the patient from the psychiatry unit, the patient did not require any psychiatric medications. The patient was on a clear liquid diet, needed a diaper and complete assistance for activities of daily living. The patient had a calm and blunted affect and was at a risk of aspiration. Apart from FTD and ALS, the patient also carried a diagnosis of dysphagia, mixed incontinence and diabetes mellitus on discharge. The patient was discharged to a nursing care facility.
Discussion
Frontotemporal dementia (FTD) is a neurodegenerative disorder of brain with a prevalence of 15 per 100,000 in the age group 45 to 64 years, a mean age of onset of 52.8 and manifests with a male dominion with a male to female ratio of 14:3 [1]. FTD exhibits in different forms, the most common (around 60% of FTDs) being the Behavioral variant FTD (bvFTD). It reveals itself as mood and behavior changes, social misconduct, apathy, emotional changes etc. 20% of cases constitute the "Temporal variant" named as the "Semantic dementia" in which language difficulty is the foremost issue. Another 20% of FTD comprises of "Progressive non-fluent aphasia" in which patients lose the ability to utter proper sentences and words despite understanding the meaning of the words. 15% of FTD cases evolve into motor neuron disease (FTD-MND). The prevalent cause of FTD-MND is Amyotrophic lateral sclerosis (ALS). It affects the motor neurons in the spinal cord, brainstem and the cerebral cortex and exhibits as slurring of speech, dysphagia, weakness in extremities and wasting of body muscles. Very rarely, about less than 5% of ALS can occur with a motor neuron disease such as an FTD, according to a JAMA report in 2000. ALS is mostly sporadic; however, 10% cases can have a familial disposition [2].
Scientists have studied the eating behavior changes in bvFTD. It was concluded in a report that the overeating behavior in bvFTD patients appears due to atrophy in the right ventral, insula, orbitofrontal cortices and the striatum [3]. Resting-state functional MRI [f MRI) is a diagnostic method used to detect the neural connectivity changes in the brain and can detect the atrophy of the brain at an earlier stage. The diagnostic tests performed in ALS can include EMG, Nerve conduction studies, Magnetic Resonance Imaging, muscle biopsy [to rule out muscle disease), spinal tap etc [4]. The survival ratio of patients with ALS was studied by the research scientists, who found that the 1, 3 and 5 years survival in ALS is 68, 25 and 17 percent. Also, it was determined in the same study that around 40% of patients diagnosed with ALS have generalized and bulbar symptoms in the initial stages of the disease. Those patients with bulbar symptoms will have dysarthria as the chief complaint rather than dysphagia [5].
To determine the association between ALS and FTD, we have discussed a number of researches conducted in the past decade. More than half of the ALS patients have shown affiliation to frontotemporal dysfunction syndromes. These syndromes comprise of cognitive dysfunction, executive dysfunction, and behavioral dysfunction and can include FTD. Typically, these syndromes occur after the manifestation of neuromuscular dysfunction symptoms. However, they can also occur alone or ahead of the appearance of symptoms of neuromuscular dysfunction. Additionally, these syndromes not only correlate clinically to the ALS, they also have a biochemical linkage to the ALS i.e., a variance in the metabolism of tau protein [6]. The presence of these syndromes further cut down the span of ALS to less than one year [7].
ALS involves both upper and lower motor neurons. ALS and FTD both are part of a common disease spectrum. Both are linked to the trans-active response DNA-binding protein 43 (TDP-43), the chief pathologic substrate involved [8]. In a genetic analysis of ALS without frontotemporal dementia cases and age-matched controls, 747 genes were identified in the anterior horn of the spinal cord and 2300 genes identified in the frontal cortex area 8 depicting genetic linkage between the ALS and FTD spectrum complex [9].
An autopsy case report of a woman who developed Pick’s disease at the age of 30, is discussed in the context of our FTD case. In this report, the patient had symptoms of dementia for 14 years and later on exhibited symptoms of ALS, one year after which she died i.e., at the age of 45 [10]. Hence, based on the pathologic and clinical findings of this case, ALS can also appear after long-standing dementia.
Conclusion
We can conclude from our discussion of the latest researches that there is an association between FTD and ALS. ALS can manifest preceding the symptoms of Frontotemporal dysfunction syndromes, along with it or in later stages. There is a clinical, genetic and biochemical association between the two conditions.
References
- Ratnavalli E, Brayne C, Dawson K, Hodges JR (2002) The prevalence of frontotemporal dementia. Neurology 58(11): 1615-1621.
- Hosler BA, Siddique T, Sapp PC, Sailor W, Huang MC, et al. (2000) Linkage of familial amyotrophic lateral sclerosis with frontotemporal dementia to chromosome 9q21-q22. JAMA 284(13): 1664-1669.
- Ahmed RM, Irish M, Henning E, Dermody N, Bartley L, et al. (2016) As-sessment of eating behavior disturbance and associated neural networks in frontotemporal dementia. JAMA Neurology 73(3): 282-290.
- Zhou J, Greicius MD, Gennatas ED, Growdon ME, Jang JY, et al. (2010) Divergent network connectivity changes in behavioral variant fronto- temporal dementia and Alzheimer's disease. Brain 133(Pt 5): 13521367.
- Traynor BJ, Codd MB, Corr B, Forde C, Frost E, et al. (2000) Clinical features of amyotrophic lateral sclerosis according to the el escorial and airlie house diagnostic criteria: A population-based study. Archives 57(8): 1171-1176.
- Strong MJ (2008) The syndromes of frontotemporal dysfunction in amyotrophic lateral sclerosis. Amyotroph Lateral Scler 9(6): 323-338.
- Woolley SC, Strong MJ (2015) Frontotemporal Dysfunction and Dementia in Amyotrophic Lateral Sclerosis. Neurol Clin 33(4): 787-805.
- Couratier P, Corcia P, Lautrette G, Nicol M, Marin B (2017) ALS and frontotemporal dementia belong to a common disease spectrum. Rev Neurol (Paris) 173(5): 273-279.
- Andres BP, Moreno J, Aso E, Povedano M, Ferrer I (2017) Amyotrophic lateral sclerosis, gene deregulation in the anterior horn of the spinal cord and frontal cortex area 8: implications in frontotemporal lobar degeneration. Aging (Albany NY) 9(3): 823-851.
- Tsuchiya K, Ikeda K, Haga C, Kobayashi T, Morimatsu Y, et al. (2001) Atypical amyotrophic lateral sclerosis with dementia mimicking frontal Pick's disease: a report of an autopsy case with a clinical course of 15 years. Acta Neuropathol 101(6): 625-630.






























