Some Haemostatic Indicators among Malaria Infected Adolescents Attending a Nigerian University Teaching Hospital
Benjamin Onyema Eledo1,2, Dennis Oju Allagoa3, Comfort Tochukwu Egwuagha2, Kingsley Excel Dunga2 and Sylvester Chibueze Izah4*
1 Departments of Haematology and Blood Transfusion, Federal Medical Centre, Yenagoa Bayelsa State Nigeria
2Department of Medical Laboratory Science, Faculty of Health Sciences, Madonna University, Elele, Nigeria
3 Department of Gynecology and Obstetrics, Federal Medical Centre Yenagoa, Bayelsa state, Nigeria
4 Department of Biological Sciences, Faculty of Science, Niger Delta University, Wilberforce Island, Bayelsa state, Nigeria
Submission: October 17, 2018; Published: March 18, 2019
*Corresponding author: Sylvester Chibueze Izah, Department of Biological Sciences, Faculty of Science, Niger Delta University, Wilberforce Island, Bayelsa state, Nigeria
How to cite this article: Eledo B O, Allagoa D O, Egwugha C T, Dunga K E, Izah S C. Some Haemostatic Indicators among Malaria Infected Adolescents Attending a Nigerian University Teaching Hospital. Open Acc Blood Res Trans J. 2019; 3(1): 555602. DOI: 10.19080/OABTJ.2019.02.555602
Abstract
This study evaluated some haemostatic indicators among malaria infected adolescents attending a University Teaching Hospital in Nigeria. Blood samples were collected from 60 malaria infected patients attending Madonna University Teaching Hospital and another 40 malaria negative students within the same age grade of (18 - 27) were analyzed as control. The haemostatic parameters (viz: Prothrombin time, activated partial thromboplastin time and platelets counts) were analyzed following standard procedures. The results revealed that malaria infected patients and control subjects had prothrombin time of 18.08 seconds and 15.05 seconds respectively; activated partial thromboplastin time of 39.67 seconds and 32.88 seconds, respectively; and blood platelets counts of 238.58x109/L and 328.25 x109/L respectively. There was significant difference (P<0.001) between the malaria infected and control subjects for each of the haemostatic parameters under study. Furthermore, the results showed significant increase, though within normal range in prothrombin time and activated partial thromboplastin time among the malaria infected adolescents, when compared with the control subjects. But the platelets count was slightly lower among the malaria infected adolescents when compared with the control subjects. The values are within normal reference range, but caution should be exercised during acute malaria infections so as to avoid other health conditions that could predispose the body to coagulation and thrombotic abnormalities.
Keywords: Haemostatic System; Malaria; Thrombocytopenia
Introduction
Malaria is included among the major public health problems in Sub-Sahara Africa [1-3] including Nigeria [4]. In many developing nations of the world especially in Sub-Sahara Africa malaria infection causes several deaths on annual basis across all age grades (infants, children, adolescents and elderly). The endemicity of malaria infections tends to vary from country to country [5] based on demographics and nutritional status. Over 50% of the world population is at risk of malaria infection in about 106 nations and territories [4]. Of these, 15 countries account for about 80% and 78% of malaria cases and deaths respectively in the world [6]. In African, Nigeria, Democratic Republic of Congo, Ethiopia, and Uganda account for substantial malaria cases [7].
Malaria is caused by plasmodium species (a protozoan) [8]. Studies have indicated most of the global malaria infections are mainly caused by P. ovale, P. vivax, P. falciparum and P. malariae [3]; [9-11]. Of these species of plasmodium, falciparum causes a substantial malaria infection in West Africa [12].
Malaria is transmitted by Mosquito, an iniquitous dipteran fly [13]; [8]. Typically, several diseases are transmitted by Mosquito depending on the species. Some of the common genera of mosquito that cause diseases include Aedes, Culex, Anopheles and Mansonia etc. According to Ndiok et al. [13] some of the diseases that are transmitted by mosquioto include filariasis, yellow fever, dengue fever, encephalitis, chikungunya, and lymphatic filariasis. Malaria is basically transmitted by anopheles mosquitoes when they bite human and inject sporozoites, the invasive forms of plasmodium into blood stream [4]. The sporozoites often invade the liver and the red blood cells which then predispose the body to periodic shivering, pyrexia and sweating with spleen enlargement [4]; [1]; [8]. Several species of Anopheles transmit malaria parasite but the commonly encountered species are gambiae, funestus, arabiensis and melas [8]; [14]. In the many endemic zone of malaria such as Nigeria, Anopheles gambiae is the most regularly encountered species [8].
Blood is among diagnostic tissue that is easily accessible [15]. Studies have widely showed that changes in physiological condition of the body due to age and/ or disease condition are often detected in the blood. To this effect, malaria has the tendency to affect the host homeostasis in human which could lead to myriad of clinical presentation [15].
During malaria infections, several haematological parameters are altered [4]; [8]. For instance, Eledo & Izah [8] reported significant higher white blood cells, erythrocytes sedimentation rate, Neutrophil, Eosinophils and a lower packed cells volume, haemoglobin, platelets, Lymphocytes, Monocytes counts in malaria infected patients attending out-patient unit of Federal Medical Centre Yenagoa, Bayelsa state Nigeria. Kotepui et al. [4] also reported significant higher white blood cells, erythrocytes sedimentation rate, Lymphocytes, Monocytes and a lower packed cells volume, Neutrophil, Eosinophils and platelets among hospital admission students in a Nigeria tertiary educational health centre within age grade of 5 to 70. The authors further reported that the variation in haematological parameters involves some essential cell lines such as red blood cells, leukocytes and thrombocytes. Haematological alterations (viz: anaemia, thrombocytopaenia and leukocytosis or leukopaenia) among malaria infected patients have been established [4]. Authors have variously reported that malaria prevalence depends on several factors including endemicity, immunity level, nutritional status, demographic factors, among other factors [3]; [4]; [16-18].
According to Kotepui et al. [4], haematological aberrations are seen as hallmark of malaria infection. Several studies have been carried out with regard to malaria infection on haematological parameters [8,19-22]. But this study focused on malaria infection among adolescent patients attending a health centre of a tertiary educational institution in the Niger Delta region, to compare results with existing literature.
Materials and Methods
Study setting
This study was conducted at Madonna University Teaching Hospital. Typically, the area is located in Elele in Rivers state. Like other Niger Delta region, the area is a sedimentary basin. Farming and petty business are the major occupation of some communities around the Teaching hospital location. Based on climatic condition, the temperature and relative humidity of the area is 28 ± 6ºC and 50 - 95% respectively all year around.
Selection criteria for subjects
Inclusion Criteria: Participants of this research were adolescents that sought for treatment at Madonna University Teaching Hospital within the age of 18-27 years. A total of 60 patients participated in this study and another 40-age match group were also taken as control. For the test subjects only individuals that blood samples were confirmed positive for the presence of malaria antigen using rapid diagnostic test kit supplied by ACCESS BIO, while the control samples were confirmed negative using the same procedure.
Exclusion criteria: Individuals with their age above 30 years; pregnant women, lactating mothers, and individuals with known cases of HIV/AIDs, hepatitis, B and C, tuberculosis, diabetics and cardiovascular diseases.
Blood Collection
A standard venipuncture technique was used to collect the blood samples. Approximately 5ml of blood was collected from each subjects from the dorsal vein and was dispensed into plastic tube containing 0.25ml of trisodium citrate for prothrombin time and activated partial thromboplasting analysis (approximately 2.25ml), while the remain sample meant for platelets analysis was dispensed into dipotassium EDTA bottles containing 1.5mg/ml of blood of the anhydrous salt.
Laboratory Analysis
The techniques previously described by Eledo et al. [23-27] was adopted for the determination of prothrombin time and activated partial thromboplastin time. Kits used were supplied by Agappe Diagnostics Switzerland with Lot number: 52601009 for prothrombin time and Lot number: 52602007 for activated partial thromboplastin time. The platelets counts were analysed using Cronkit’s ammonium oxalate method.
Statistical Analysis
SPSS version 20 was used to carry out the statistical analysis. Data were presented as mean ± standard deviation. t-test was used to show significant difference at P<0.05 among test and control subjects.
Results and Discussion
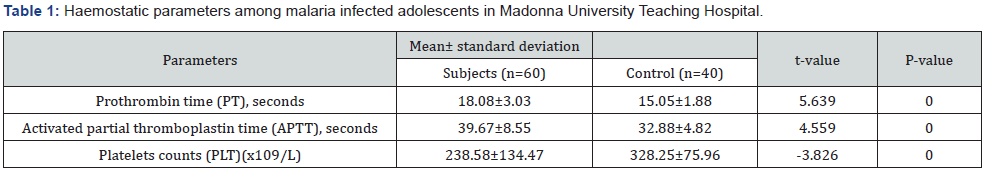
The haemostatic blood indicators among malaria infected adolescents in Madonna University Teaching Hospital Elele, Rivers state, Nigeria is presented in Table 1. The malaria infected patients and control subject’s prothrombin time was 18.08 seconds and 15.05 seconds respectively; the activated partial thromboplastin time was 39.67 seconds and 32.88 seconds, respectively; and blood platelets was 238.58x109/L and 328.25 x109/L respectively. There was a significant difference (P<0.001) between the malaria infected and control subjects for each of the haemostatic parameters under study. The prothrombin time and activated partial thromboplastin time were slightly higher among the test subjects while the platelets count was slightly lower when compared with the control subjects. The values obtained were within the normal reference range which suggests no risk of coagulation or thrombotic disorders among the subjects.
The trend of prothrombin time and activated partial thromboplastin time in this study is comparable to the results in different health conditions including hypertension [26], Helicobacter pylori infected patients [25], aged (elderly) [28], before exercise [23] but not in consonance with the trend in different stages of pregnancy [27], and diabetes condition [24].
Typically, both prothrombin time and activated partial thromboplastin time are essential blood coagulation indicators, hence a higher value in the malaria infected patients may suggest possible risk of vascular complications over a prolonged period of time [25]. The mean platelets for test subjects (malaria infected patients) in this study were slightly lower among the test than the control subjects, though statistically significant. The trend of platelets were not in consonance with the work of Eledo et al. [26] on hypertension, Eledo et al. [25] on Helicobacter pylori infected patients, Eledo et al. [23] before exercise, Eledo et al. [27] at different stages of pregnancy, but comparable to the work of [24] on diabetes patients. Based on malaria infected patients, the findings of this study is at variance with the study of Kotepui et al. [4] in Calabar, Nigeria, Maina et al. [15] in Kisumu West District, Western Kenya. Again, this variation could also be attributed to immunity level of the patients, nutritional status, demographic factors, background haemoglobinopathy [3,4]; [16-18]. Basically, platelet is vital for the initiation and propagation of thrombosis [25]. The significant decrease in the platelets counts among malaria infected patients suggests probable risk of platelets dysfunctioning which could predispose the patients to vascular complications. According to Kotepui et al. [4], thrombocytopenia usually occur when the platelets count is less than 150,000/μL.
Conclusion
This study investigated some haemostatic among malaria infected adolescent attending a tertiary educational institution teaching hospital in Nigeria. The study showed that malaria significantly increases activated partial prothrombin time, prothrombin time and decreases platelets counts. Though, the values were within the normal range, and no risk of thrombocytopenia based on platelets counts, and hypercoagulability or clotting disorder based on activated partial prothrombin time and prothrombin time. But caution should be exercised during acute malaria infections, and treatment should be sorted out immediately after diagnosis to avoid other health conditions that could predispose the body to thrombocytopenia and other coagulation disorders.
References
- Francis U, Isaac Z, Yakubu A, Enosakhare A, Felix E (2014) Haematological Parameters of Malaria Infected Patients in the University of Calabar Teaching Hospital, Calabar, Nigeria. J Hematol Thrombo Dis 2: 171.
- Bassey SE, Izah SC (2017a). Nigerian plants with insecticidal potentials against various stages of mosquito development. ASIO Journal of Medical and Health Sciences Research 2(1): 7-18.
- Bassey SE, Izah SC (2017b) Some determinant factors of Malaria Prevalence in Nigeria. Journal of Mosquito Research 7(7): 48-58.
- Kotepui M, Piwkham D, PhunPhuech B, Phiwklam N, Chupeerach C, et al. (2015) Effects of Malaria Parasite Density on Blood Cell Parameters. PLoS ONE 10(3): e0121057.
- Okoroiwu IL, Obeagu EI, Elemchukwu Q, Ochei KC (2014) Some Hematological Parameters in Malaria Parasitaemia. IOSR Journal of Dental and Medical Sciences 13(9): 74-77.
- Aju-Ameh CO, Awolola ST, Mwansat GS, Mafuyai HB (2016) Malaria transmission indices of two dominant anopheles species in selected rural and urban communities in Benue state North Central, Nigeria. International Journal of Mosquito Research 3(5): 31-35.
- Nigeria Malaria Fact Sheet (2011).
- Eledo BO, Izah SC (2018) Studies on Some Haematological Parameters among Malaria Infected Patients Attending a Tertiary Hospital in Nigeria. Open Access Blood Research and Transfusion Journal 2(3): 555586.
- Tela IA, Modibbo MH, Adamu LH, Taura MG (2015) Prevalence of Malaria Infection Among ABO Blood Groups In Jama’are, Nigeria. RA Journal of Applied Research 1(7): 255-262.
- Unata IM, Bunza NM, Ashcroft OF, Abubakar A, Faruk N (2015) Prevalence of Malaria Parasites among HIV/AIDS Patients Attending HIV Clinic in Usmanu Danfodiyo University Teaching Hospital and Sokoto State Specialist Hospital, Sokoto, Nigeria, International Journal of Novel Research in Life Sciences 2(2): 39-43.
- Pam VA, Landan S, Pam DD, Gullek JF, Okoro J, et al. (2015) The prevalence of malaria and typhoid co-infection in pregnant women attending antenatal in Wuse general hospital Abuja, Nigeria, Scientific Journal of Veterinary Advances 4(6): 39-50.
- Idowu AP, Okoronkwo N, Adagunodo RE (2009) Spatial Predictive Model for Malaria in Nigeria. Journal of Health Informatics in Developing Countries 3(2): 30-36.
- Ndiok EO, Ohimain EI, Izah SC (2016) Incidence of Malaria in Type 2 Diabetic patients and the effect on the liver: a case study of Bayelsa state. J Mosq Res 6(15): 1-8.
- Nmadu PM, Peter E, Alexander P, Koggie AZ, Maikenti JI (2015) The Prevalence of Malaria in Children between the Ages 2-15 Visiting Gwarinpa General Hospital Life-Camp, Abuja, Nigeria. Journal of Health Science 5(3): 47-51.
- Maina RN, Walsh D, Gaddy C, Hongo G, Waitumbi J, et al. (2010) Impact of Plasmodium falciparum infection on haematological parameters in children living in Western Kenya. Malar J 9(Suppl 3): S4.
- Wickramasinghe SN, Abdalla SH (2000) Blood and bone marrow changes in malaria. Baillieres Best Pract Res Clin Haematol 13(2): 277-299.
- Erhart LM, Yingyuen K, Chuanak N, Buathong N, Laoboonchai A, et al. (2004) Hematologic and clinical indices of malaria in a semi-immune population of western Thailand. Am J Trop Med Hyg 70(1): 8-14.
- Price RN, Simpson JA, Nosten F, Luxemburger C, Hkirjaroen L, et al. (2001) Factors contributing to anemia after uncomplicated falciparum malaria. Am J Trop Med Hyg 65(5): 614-622.
- Gondaliya S, Makwana H, Lakum N, Agnihotri A (2015) Study of prevalence of different species of malarial parasites and comparison of hematological parameters in different malarial parasite species. Int J Med Sci Public Health 4: 1697-1701.
- Hamid TAM, Eldin FA, Elnasri HA (2016) Effect of Malaria Parasite Infection on Platelet Parameters (Platelets count, mean platelets volume and platelets distribution width) among Malaria Patients in Khartoum State. Annals of Biological Research 7(5): 18-23.
- Chukwuanukwu RC, Ukaejiofo EO, Ele PU, Onyenekwe CC, Chukwuanukwu TO, et al. (2016) Evaluation of some haemostatic parameters in falciparum malaria and HIV co-infection. Br J Biomed Sci 73(4): 168-173.
- Kotepui M, Phunphuech B, Phiwklam N, Chupeerach C, Duangmano S (2014) Effect of malarial infection on haematological parameters in population near Thailand-Myanmar border. Malar J 13: 218.
- Eledo BO, Igwe R, Okamgba OC, Izah SC (2017a) Effect of Exercise on Some Haemostatic Parameters Among Students in a Tertiary Educational Institution in Nigeria. American Journal of Health Research 5(5): 145-148.
- Eledo BO, Nwoga MI, Okamgba OC, Izah SC (2017b) Assessment of Some Haemostatic Parameters Among Diabetes Mellitus Patients in Bayelsa State: A Case Study at the Federal Medical Centre, Yenagoa. European Journal of Clinical and Biomedical Sciences 3(5): 91-96.
- Eledo BO, Allagoa DO, Onuoha EC, Okamgba OC, Ihedioha AU, et al. (2017c) Effect of Helicobacter Pylori on Some Haemostatic Parameters among Students of a Tertiary Institution in Nigeria. Clinical Biotechnology and Microbiology 1(5): 219-224.
- Eledo BO, Izah SC, Okamgba OC (2018a) Prothrombin Time Activated Partial Thromboplastin Time and Platelets Count among Hypertensive Patients Attending a Tertiary Health Institution in Yenagoa, Nigeria. J Blood Res Vol.1 No. 1:3.
- Eledo BO, Izah SC, Okamgba OC, Onuoha EC (2018b) Assessment of some haemostatic parameters at different stages of pregnancy. Hematol Transfus Int J 6(3): 98-101.
- Eledo BO, Izah SC, Okamgba OC (2018c) Assessment of Some Haemostasis System Blood Indicators among the Elderly Attending a tertiary Health Institution in Nigeria. Arch Blood Transfus Disord 1(4).






























