Relationship Among Body Adiposity Index, Skinfold Thickness and Bioelectric Impedance in Estimating Body Fat in Patients with Knee Osteoarthritis
Jeneviv Nene John1,2*, Rufus Sunday Akinbo1, Bankole C Aiyejusunle1, Davidson Okwudili John3 and Obinna Chinedu Okezue2
1Department of physiotherapy, University of Lagos, Nigeria
2Department of medical rehabilitation, University of Nigeria
3Department of physiotherapy, Federal Teaching Hospital, Abakaliki, Nigeria
Submission: December 16, 2018; Published: January 16, 2019
*Corresponding author: Jeneviv Nene John, Department of Medical Rehabilitation, University of Nigeria, P.M.B 01129 Enugu State, Nigeria
How to cite this article: Jeneviv Nene John, Rufus Sunday Akinbo, Bankole C Aiyejusunle, Davidson Okwudili John, Obinna Chinedu Okezue. Relationship Among Body Adiposity Index, Skinfold Thickness and Bioelectric Impedance in Estimating Body Fat in Patients with Knee Osteoarthritis. Nov Tech Arthritis Bone Res. 2019; 3(3): 555614. DOI: 10.19080/NTAB.2019.03.555614
Abstract
Background: Overweight and obesity are strongly associated with the development and progression of knee osteoarthritis (OA). It has been reported that the fat mass rather than the muscle mass determines the health risk. It is uncertain whether the field methods of estimating body fat will give similar values considering the variations in their methodology.
Objectives: To determine the relationship among body adiposity index (BAI), skinfold thickness (SFT) and bioelectric impedance (BIM) in estimating body fat in patients with knee OA.
Methods: This cross-sectional survey involved one hundred participants recruited from the orthopedic clinic of two tertiary hospitals. Measurements of percentage body fat were obtained for each participant using the three field methods. Descriptive statistics was used to summarize the demographic data while inferential statistics of Pearson product moment correlation coefficient was used to test the hypotheses. Alpha level was set at p < 0.05.
Results: There was significant correlations between percentage body fat scores obtained for BAI and SFT (r = 0.71, p = 0.001), BAI and BIM (r = 0.69, p = 0.001) and SFT and BIM (r = 0.98, p = 0.001). Females had significantly higher percentage body fat than males (p = 0.001).
Conclusion: The three field methods could be used for the clinical estimation of body fat in patients with knee OA. However, this suggests that in clinical settings where BIA machine and skinfold caliper are not readily available, the BAI which simply uses tape measurements can be used to estimate percentage body fat.
Keywords: Body Adiposity Index; Skinfold Thickness; Bioelectric Impedance; Knee OA
Introduction
Osteoarthritis (OA) is a degenerative disease that commonly affects the weight bearing joints [1-2]. Of all the risk factors known, overweight and obesity are strongly associated with the development and progression of knee osteoarthritis [2]. Previous studies have reported that it is the fat mass that determines the health risk of individuals [3-4]. Consequently, this has aroused the increased interest of scientists, clinicians and researchers in body fat measurement in order to determine whether an individual is free from health risks or not [3-4] Body fat percentage can be measured using laboratory methods such as hydrostatic weighing (HYW), air displacement plethysmography (ADP), dual-energy x-ray absorptiometry (DXA) and neuron activation techniques (NAT) [5] or field methods such as body adiposity index (BAI), bioelectric impedance analysis (BIM), skinfold thickness (SFT), and anthropometric methods [6].
Hydrostatic weighing is a laboratory method of measurement that determines the body fat to lean mass that make up the total body density [7-8]. Air displacement plethysmography is similar to HYW but uses air displacement instead of water, while neutron activation technique involves high level of neutron radiation exposure. Another laboratory method of measurement is DXA which measures three body compartments of fat mass, lean mass and bone content [9]. These laboratory methods give reliable body composition measurements but are not feasible for clinical use because of their cost and complexity.
Body Adiposity Index (BAI), bioelectric impedance analysis (BIM), skinfold thickness (SFT) and anthropometric methods have been widely used in developing countries due to their relatively low cost, speed of administration and availability compared to the complex and expensive laboratory methods. Body adiposity index was proposed by Bergman et al. [10] in a study to determine the fat contents of one thousand, seven hundred Mexican Americans and it depends on measurements of the hip circumference and height. The BIM measures the impedance of the body tissues to the flow of electric current while the SFT measurement is based on a skinfold or pinch test, whereby a pinch of skin is precisely measured by calipers at several standardized points on the body to determine the subcutaneous fat layer thickness [4]. The SFT is measured at various body locations using a hand-held caliper and the body fat percentage is derived based on the sum of the measurements [11].
Several studies have linked body fat accumulation to a higher risk of progression of knee OA [9-12], Christensen et al. [13] also reported that the reduction of body fat improved aerobic capacity and functional activity of patients with knee OA by 28% while Toda et al. [14] reported that loss of body fat is more effective than the loss of body weight in the management of patients with knee OA. This therefore underlies the importance of body fat measurement for patients with knee OA. Controversies exist on how closely related these field methods of estimating body fat are because each of them has their strengths and weaknesses [15]. A comparison among these field methods of measurement has been made in healthy populations of children and adults to determine how closely related they are [4,7,16].
However, despite the fact that studies have linked reduction of body fat to improved quality of life of patients with knee OA, there is paucity of data comparing these field methods of estimating body fat in patients with knee OA. Also, it is unknown if the body composition changes associated with knee OA will affect the accuracy of these field methods of measurement. Therefore, this study was aimed at determining the relationship among body adiposity index, skinfold thickness and bioelectric impedance in estimating body fat among patients with knee osteoarthritis.
Materials and Methods
This cross-sectional survey involved one hundred patients diagnosed with knee OA in two tertiary hospitals. The participants were recruited from the orthopedic clinic of the hospitals using a convenience sampling technique. All the patients diagnosed of OA at time of the study were invited to participate. The inclusion criteria for participation in this study were patients clinically diagnosed with either unilateral or bilateral knee OA while the exclusion criteria were female patients with knee OA who are pregnant, patients who have significant cognitive impairment, inability to follow instructions or who have other significant pathology of the lower limb.
Ethical approval for this study was obtained from the Health Research and Ethics Committee of the institutions where the research was carried out. The aim of the study, procedure and precautions were explained to the participants who met the inclusion criteria after they read, filled and signed the informed consent form. The demographic data and measurements of height, weight, hip circumference, skinfold thickness and bioelectric impedance were obtained for each participant. The measurements of the height and weight were taken using the International Standards for Anthropometric Assessment protocol [11]. The height was measured in centimeters (cm) using a stadiometer (Secca, Germany). The participants were instructed to stand barefooted in an upright position on the platform of the stadiometer. The horizontal projection of the stadiometer was brought in contact with the head of the participants and the readings were read off to the nearest 0.1 centimeter.
A weighing scale (Secca, Germany) was used to measure the weight, with the participants bare-footed and in light clothing. The weighing scale was reading zero and the participants were instructed to stand on the platform of the weighing scale with their weight evenly distributed on both feet. The readings were read off to the nearest 0.1kg. A non-elastic tape measure (Butterfly, China) was used to measure the hip circumference with the participants in standing position, the arms folded across the thorax, the feet together and the gluteal muscles relaxed. The researcher passed the tape around the hips from the side. The stub of the tape and the housing were held with the researcher’s right hand while the left hand was used to adjust the tape at the back to the level of the greatest posterior protuberance of the buttocks.
The tape was adjusted with the researcher ensuring that
it does not excessively indent the skin, and then the readings
were read off to the nearest 0.1cm. The measurements of the hip
circumference and height were imputed into the body adiposity
index equation (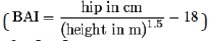 ) in order to derive the
percentage body fat [10].
) in order to derive the
percentage body fat [10].
The skinfold thickness measurements were taken using a Lange skinfold caliper (Beta technology, Inc, USA) on the right side of the body with the subjects in standing position and with the muscles relaxed. The skinfold sites that were measured included the biceps, triceps, subscapular and suprailiac region. A tape measure was used to find the exact points which were marked using a temporary marker. The skinfold was pulled with the tip of the thumb and the index finger of the examiners left hand and held firmly till the readings were taken. The examiner held the caliper with the right hand and placed the jaws of the caliper perpendicular to the skinfold on the site marked. While maintaining the grasp of the skinfold, the caliper was released so that the entire force of the jaws was on the skinfold. The measurements were taken to the nearest millimeter. Two sets of measurement were averaged for one skinfold site and the percentage body fat was estimated from the sum of the skinfold measurements at the four sites using the table developed by Durnin and Womersley [17].
The bioelectric impedance measurement using the OMRON BF511 body composition monitor was carried out according to the manufacturer’s instruction manual with the participants in light clothing and without shoes. The feet were placed on the foot electrodes with the weight evenly distributed. The knees and back were maintained in a straightened position and the arms were extended at right angles to the body while maintaining a slight arch at the back. The grip electrodes were pulled up until both upper limbs were at right angles to the body. The readings were then taken from the display unit. Two sets of measurement were taken for each participant and the average percentage body fat was determined. All measurements were completed on the same day within 25 to 40 minutes for each participant.
Precautions
Participants were asked not to eat at least three hours before the measurements were taken and to abstain from exercise and alcohol twelve and twenty-four hours respectively before the measurements were taken. The researcher also ensured that female participants were not given appointment dates within their menstrual period. These factors have been reported to affect the accuracy of the bioelectric impedance measurement. Descriptive statistics was used to present the demographic and physical characteristics while inferential statistics of Pearson product moment correlation coefficient was used to determine the relationship among the three field methods of estimating percentage fat. An independent t-test was used to compare the gender distribution of percentage body fat scores obtained by the three field methods. All the data were analyzed using SPSS version 20.0 and significance was set at an α - level of p<0.05.
Results
The study population comprised of twenty-four (24.0%) and seventy-six (76.0%) males and females respectively. Seventyseven of the participants (77.0%) presented with bilateral knee OA while the remaining twenty-three (23.0%) presented with unilateral knee OA. [Table 1] shows the demographic and physical characteristics of the participants. Three (3.0%) of the participants had a normal body mass index, seventeen (17.0%) were overweight and eighty (80.0%) were obese. The percentage body fat scores obtained by the three-field method classified according to the age group adjusted body fat percentage recommendations is shown in [Table 2] [18]. The mean percentage body fat scores obtained for body adiposity index, skinfold thickness and bioelectric impedance analysis are presented in [Table 3]. The female participants had significantly higher percentage body fat scores than their male counterparts in all the three methods of estimating body fat [Table 4]. The correlation coefficient among the three field methods of estimating body fat is shown in [Table 5].

X= mean, SD= standard deviation
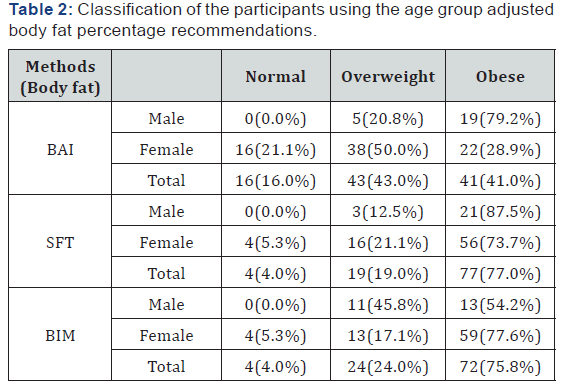
Keys: BAI: Body adiposity index; SFT: Skinfold Thickness; BIM: Bioelectric Impedance Analysis.
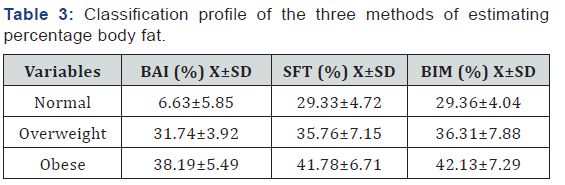
X= mean, SD= standard deviation
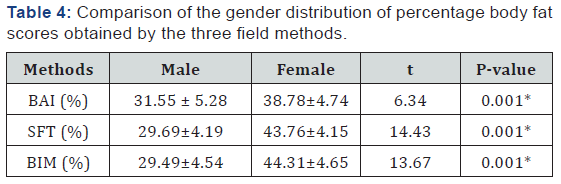
Keys: BAI-Body adiposity index, SFT- Skinfold thickness, BIMBioelectric impedance analysis
*significant at p<0.05.
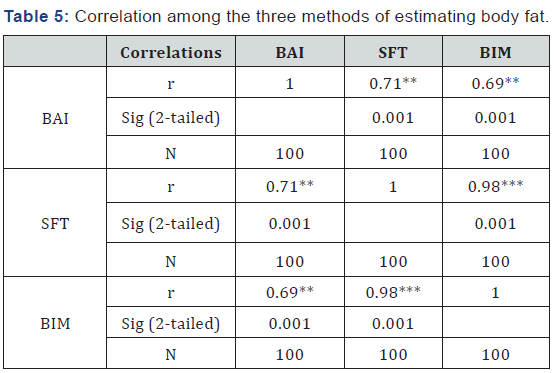
*low correlation (<0.50), **Moderate correlation (0.50-0.80), ***High correlation (˃0.80)
Keys: BAI-Body adiposity index, SFT-Skinfold thickness, BIMBioelectric impedance analysis, r = Pearson’s correlation, N- Total number of participants.
Discussion
A significant correlation was observed among these methods of estimating body fat with the highest correlation observed between skinfold thickness and bioelectric impedance. Previous studies have investigated BAI as a predictor of body fat but only in comparison to BIM, ADP, DXA and body mass index yielding inconsistent results. Geliebter et al. [19] reported that BAI correlated significantly with BIM and ADP but did not correlate with DXA. On the other hand, Johnson et al. [20] reported that BAI and DXA showed a high level of correlation than body mass index (BMI) and DXA in sex-pooled analyses but in sexstratified analyses, BAI and BMI showed similar correlations with DXA. Godoy-Matos et al. [21] also reported that BAI showed a higher correlation with DXA than other laboratory methods of measurement in women with familial partial lipodystrophy. However, despite the fact that this study reported a significant relationship among BAI, SFT and BIM in the estimation of body fat in patients with knee osteoarthritis, the BAI index should be used with some caution when applied in other populations because of these observed inconsistencies.
The correlation observed between BIM and SFT in this study is in agreement with previous studies [22]. Mariana et al. [4] observed a significant correlation between BIM and SFT but concluded that BIM appears to present better results considering its high correlation with anthropometric indicators used in their study. Akinpelu et al [16] and D’Alonzo et al [22] reported that either BIM or SFT are acceptable for the clinical estimation of body fat in apparently healthy adults and sedentary women respectively. Although BIM and SFT rely on different assumptions, it is remarkable that they have a high correlation. While the BIM method has an advantage of minimal inter- or intra- observer variability, it requires adequate participant instruction and strict adherence to the protocol recommendations to ensure that the technique is applied appropriately [23]. On the other hand, SFT which is based on the assumption that a strong relationship exists between the total body fat and subcutaneous fat has high inter- or intra- observer variability [4].
The validity of skinfold thickness measurement has been questioned in overweight and obese population because of the difficulty in finding the landmarks and in sampling the correct layers of skin and underlying fat in this group of people. Despite the fact that majority of the participants in this study were overweight and obese, a strong relationship still existed between SFT and other methods of measurement. Hence, this justifies the use of skinfold measurement in assessing body fat in overweight and obese population of patients with knee OA.
This study found out that females had significantly higher body fat percentage values than males in all the methods of measurement. This finding is in accordance with previous findings and can be attributed to the hormonal differences in male and female gender which predisposes females to increased fat deposition [6,24]. In conclusion, reports of this study justify the use of Lange skinfold caliper, OMRON BF-511 body composition monitor or body adiposity index equation to derive the body fat percentage of patients with knee OA. However, this suggests that in clinical settings where BIA machine and skinfold caliper are not readily available, the BAI which simply uses tape measurements can be used to estimate percentage body fat. Hence, it is advocated that future works should include the laboratory methods of assessing percentage body fat as a reference point to these field methods of measurement.
References
- Akinbo SRA, Aiyejusunle CB, Akinyemi OAK, Adesegun SA, Danesi MA, et al. (2007) Comparison of the Therapeutic Efficacy of Phonophoresis and Iontophoresis using Dexamethasone Sodium Phosphate in the Management of Patients with knee osteoarthritis. NPMJ 14(3): 190- 194.
- Vanmanen MD, Nace J, Mont MA (2012) Management of primary knee osteoarthritis and indications for total knee arthroplasty for general practitioners. JAOA 112(11): 709-715.
- Abate LM, Stevens J, Schwartz TA, Renner JB, Helmick CG, et al. (2006) Anthropometric measures, body composition, body fat distribution and knee osteoarthritis in women. Obesity 14(7): 1274-1281.
- Mariana CD, Aline CSL, lorena PC, Ann KJ, Luana C, et al. (2012) An optimal method for measuring body fat in overweight individuals in clinical practice. J Endocrinol Metab 18: 2161-1017.
- Jordan RM, Sarah ET, Abbie ES, Michael DR, Eric DR, et al. (2007) Percent body fat estimations in college men using field and laboratory methods: a three-compartment model approach. Am J ClinNutr 8: 14- 17.
- Fahey T, Insel P, Roth W (2010) Body composition, Fitness and wellness, core concepts and labs in physical fitness and wellness. (5th ed), Mcgraw-hill, USA. pp. 96-154.
- Moon JR, Hull HR, Tobkin SE, Teramoto M, Karabulut, et al. (2007) Percent body fat estimations in college women using field and laboratory methods: a three-compartment model approach. JISSN 4: 16-24.
- Ojoawo AO, Onigbinde TA, Adeyanju S (2013) Skinfold parameter as predictor of body density for undergraduate female students in a Nigerian university community. TNHJ 13(1): 40-47.
- Wang Z, Heymsfield SB, Chen S (2010) Estimation of percentage body fat by dual-energy x-ray absorptiometry: evaluation by in vivo human elemental composition. Phys Med Biol 55: 2619-2635.
- Bergman RN, Stefanovski D, Buchanan TA, Sumner AE, Reynolds JC, et al. (2011) A better index of body adiposity. Obesity 19: 1083-1089.
- International Society for the Advancement of Kinathropometry International standards for anthropometric assessment (2001).
- Berry PA, Wluka AE, Davies Tuck ML, Wang Y, Strauss BJ et al. (2010) The relationship between body composition and structural changes at the knee. J Rheumatol 49(12): 2362-2369.
- Christensen R, Astrup A, Bliddal H (2005) Weight loss: The treatment choice for knee osteoarthritis? A randomized control trial .J Osteo cartilage 13(1): 20-27.
- Toda Y, Toda T, Takemura S, Wada T, Morimoto T, et al. (1998) Change in body fat but not body weight or metabolic correlates of obesity, is related to symptomatic relief of obessed patients with knee osteoarthritis after a weight control program. J Rheumatol 25(11): 2181-2186.
- Rezende F, Rosado I, Franceschinni S, Rosado G, Ribeiro R (2007) Critical revision of the available methods for evaluating the body composition in population based and clinical studies. Nutr J 57(4): 327-334.
- Akinpelu AO, Gbiri CA, Banks YO, Oyeyemi AL (2011) Relationship among three field methods of estimating percent body fat in young adults. JNSP 18(1-2): 24-35.
- Durnin JVGA, Womersley J (1974) Body fat assessed from total body density and its estimation from skinfold thickness: measurements on 481 men and women aged from 16 to 72 years. Brit J Nutr 32(1): 77- 97.
- Gallagher D, Heymsfield SB, Heo M, Jebb SA, Murgatroyd PR et al. (2000) Healthy percentage body fat ranges: an approach for developing guidelines based on body mass index. Am J ClinNutr 72(3): 694-701.
- Geliebter A, Atalayer D, Flancbaum L, Gibson CD (2013) Comparison of body adiposity index (BAI) and BMI with estimations of percentage body fat in clinically severe obese women. Obesity 21(3): 493-498.
- Johnson W, Chumlea WC, Czerwinski SA, Demerath EW (2012) Concordance of the recently published body adiposity index with measured body fat percent in European-American adults. Obesity 20(4): 900-903.
- Godoy-Matos AF, Moreira RO, Valerio CM, Mory PB, MoisesRS, et al. (2012) A new method for body fat evaluation, body adiposity index, is useful in women with familial partial lipodystrophy. Obesity 20(2): 440-443.
- D Alonzo K, Aluf A, Vincent L, Cooper K (2009) A Comparison of field methods to assess body composition in a diverse group of sedentary women. Biol Res Nurs 10(3): 274-283.
- Horie LM, Barbosa silva MC, Torrinhas RS, Demello MT, Cecconello I, et al. (2008) New body fat prediction equations for severely obese patients. J Clin Nutr 27(3): 350-356.
- Power ML, Schulkin J (2008) Sex differences in fat storage, fat metabolism and the health risks from obesity: possible evolutionary origins. Brit J Nutr 99(5): 931-940.






























