Investigation of the Mechanical Rigidity of First and Second-Order External Fixation Modules Assembled Using the Extracortical Clamp Device
Solomin L1,3*, Sabirov F1, and Fletcher M2
1Vreden Russian Research Institute of Traumatology and Orthopedics, St Petersburg, Russia
2Dawson Creek & District Hospital, Canada
3Saint-Petersburg State University, Russia
Submission: August 14, 2017; Published: September 08, 2017
*Corresponding author: Leonid Solomin, Department of orthopedic, St. Petersburg State University, Russia, Email: solomin.leonid@gmail.com
How to cite this article: Solomin L, Sabirov F, Fletcher M. Investigation of the Mechanical Rigidity of First and Second-Order External Fixation Modules Assembled Using the Extracortical Clamp Device. Nov Tech Arthritis Bone Res. 2017; 1(5) : 555575 DOI: 10.19080/NTAB.2017.01.555575
Abstract
Introduction: The Extra cortical Clamp Device (ECD) is a novel element used in external fixation. Unlike standard transosseous fixation elements, the ECD avoids the intra medullary canal and is rigidly secured to the external periosteal surface of diaphyseal bone. External fixation offers a solution to the management of periprosthetic fractures with well fixed prostheses; however, infection and implant loosening may be troublesome complications. The ECD has direct potential for utility in their management by avoiding these complications. We postulated that in addition to a favorable mechanism of fixation, the ECD would show equal or superior rigidity compared to standard transosseous external fixation.
Methods: Mechanical analysis of the rigidity of the ECD was studied in first and second order external fixation modules using a standardized and accepted testing protocol and compared to accepted fixation techniques in a Sawbones model.
Results: Two parallel ECDs inserted at an angle of 60 degrees to each other with an intercalary distance of 10cm showed greater rigidity in both first and second order modules than alternate configurations. This ECD configuration showed improved stiffness compared to standard Schanz screw fixation.
Conclusion: The ECD shows favorable rigidity in frame construction compared to standard external fixation elements. This study demonstrates the optimal configuration of the ECD when applied to diaphyseal external fixator assemblies for maximal rigidity, and can therefore be utilized as a standard in ECD application in further studies of periprosthetic fracture stabilization, diaphyseal lengthening and bone transport over nail techniques.
Keywords: Extra cortical Clamp Device; External fixation; Periprosthetic fracture; Rigidity
Introduction
The Extra cortical Clamp Device (ECD) is a novel fixation element designed for use in external fixation assemblies. Unlike standard transosseous fixation elements such as fine wires or the Schanz screw, the ECD avoids the intramedullary canal by obtaining capture of the bone segment external to the periosteal surface of diaphyseal bone. The prime advantage of this is to avoid disruption of, and to reduce the risk of introduction of infection into the prosthetic bed and prevent component loosening. Furthermore, whilst transosseous fixation can be performed in the presence of endostea prostheses, this typically requires predominantly cortical fixation with significant heat generation, and if the transosseous element does penetrate the intramedullary canal, fretting wear debris can be generated.
The main disadvantage of the ECD is the increased size of the skin incision and thus the potential to act as a larger conduit to bacterial penetration of the extraosseous space.The ECD comprises two components, a hollow threaded portion, with a curved, hooked clamp to maximize hold on the far side of the diaphysis, and an inner threaded segment to engage the near cortex and via compression of the device, to obtain secure capture of the bone segment (Figure 1a/b). The design of the implant facilitates capture of a bone segment in which there is an intramedullary prosthesis, and as such, offers a potentially valuable addition to the management of periprosthetic fractures and deformity by allowing secure capture of the endoprosthetic segment.

Periprosthetic fractures in relation to total hip replacements are not uncommon, with an incidence of 4% quoted in the literature [1,2]. Surgical management of periprosthetic fractures and deformities is typically associated with significant blood loss, lengthy operative times and risk of deep infection, with a high frequency of complications, and poor long-term outcome [3,4]. Surgery is often complex and expensive [2]. The magnitude of the operative intervention may be precluded by comorbidities, and the preoperative risks are significant, with a high mortality rate [3]. Complications have been reported to have occurred in 3352%, with a re-operation rate of 33%, highest in Vancouver type C fractures with a 52% re-operation rate [4-6]. Complications were associated with poorer clinical outcome [4,6]. Previous studies have described the use of external fixation in the management of periprosthetic fractures [7]. With refinements in design and technique of fixator assembly the indications for femoral frame construction have been expanded, to include Lengthening over Nail (LON) [8-12], Bone Transport over Nail (BTON) [12-15] and correction of periprosthetic femoral deformity and malunion [16]. The ECD, due to its novel concept, permits easy application to the femur without disrupting the endosteal space and any intramedullary device.
In order to determine the usefulness of the application of frames for periprosthetic bone fragment stabilization, it was deemed important to measure the rigidity of different external fixation modules to ensure optimal stability and efficacy of the fixator assembly in a reproducible manner. A mechanical laboratory study was thus devised to compare the stiffness of bone fragment modules fixation provided by standard screws and with the ECD in varying configuration.
Material and Methods
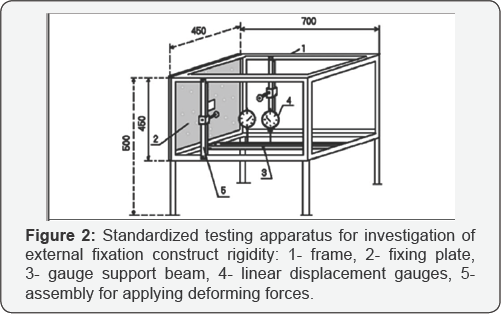
The study design was constructed according to the “Method of investigation of stiffness of transosseous osteosynthesis in planning operations” [17]. A standardized testing frame was used (Figure 2), with linear displacement gauges with a scale of 0. 01 mm, Sawbones models (Pacific Research Laboratories, WA, USA), calibrated loads, Ilizarov external fixation components (Smith & Nephew, Memphis TN) and extra cortical clamp devices.
According to this method, the building blocks of an external fixation assembly constitute a First Order Figure 1 consisting of a single external ring with associated transosseous elements, a Second OrderFigure 2 namely two M1 modules connected together. The Third Order Module consisting of the full fixator assembly incorporating two M1 or M2 modules was not investigated in this initial study.
The standard algorithm for the investigation of stiffness in transosseous modules comparises(Figure 3a-3c)
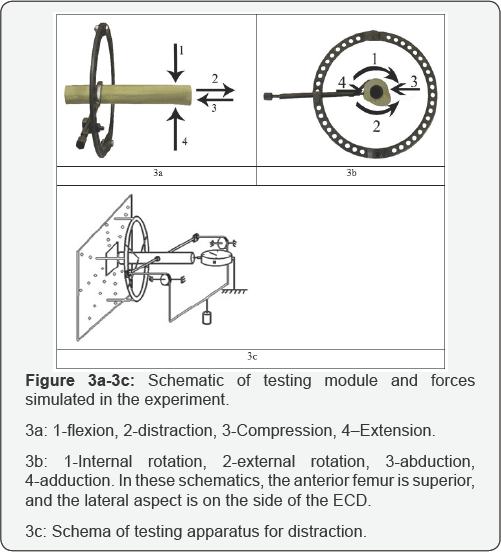
i. Longitudinal stiffness i.e. distraction and compression
ii. Frontal plane stiffness, i.e. abduction and adduction
iii. Sagittal plane stiffness, i.e. flexion and extension
iv. Rotational stiffness, i.e. internal and external rotation
For example, in the study of longitudinal stiffness, the external support of the test module is secured to the testing frame. The bone. Calibrated 5N loads are applied and construct deformation is measured (Figure 3c). Each experiment was concluded when the displacement of the loaded bone reached 1mm or 1 °C with the load achieving this deformation recorded. The coefficient of stiffness (K) for each parameter was determined according to the following formulae:
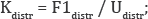
where Kdistr= stiffness coefficient of osteosynthesis in distraction; F1distr, = the value of the axial force of distraction, Udistr,= distance moved (in mm);
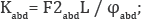
where Kabd = stiffness coefficient of osteosynthesis in abduction, F2abd = value of the force creating frontal plane angular displacement, L = distance from the point of application of force to the position of osseous fixation, φabd = Angle of fragment deformation under load;

where Kflex = stiffness coefficient of osteosynthesis in flexion,F3flex=value of the force creating saggital plane angular displacement, L= distance from the point of application of force to the position of osseous fixation, φflex= angle of fragment deformation under load;
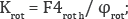
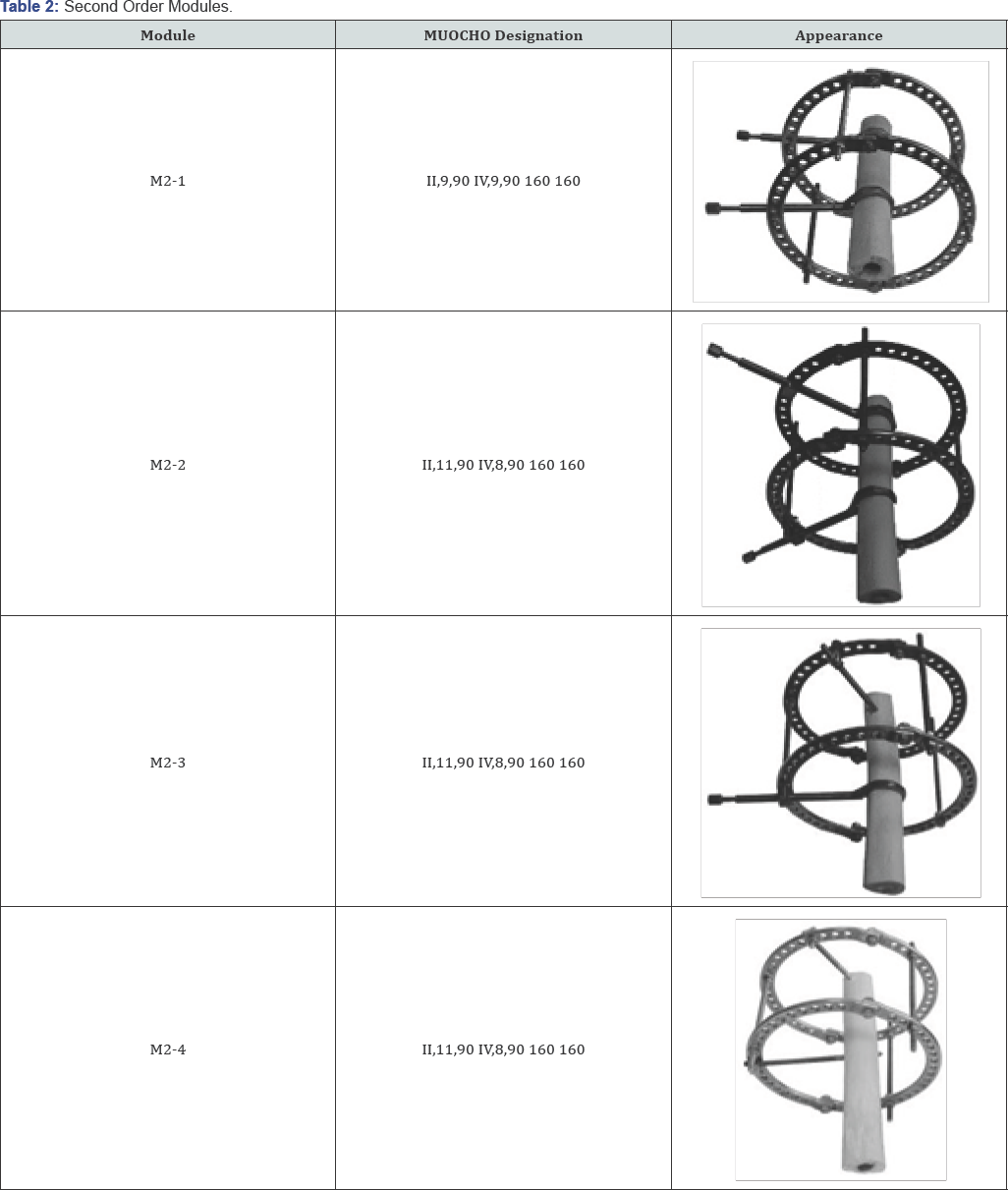
where Krot = stiffness coefficient of osteosynthesis in internal rotation, F4rot = value of the force creating rotational displacement in the transverse plane, h = twice the distance from the point of application of force to the center of the simulated bone, φrot = angle of torsional deformation.
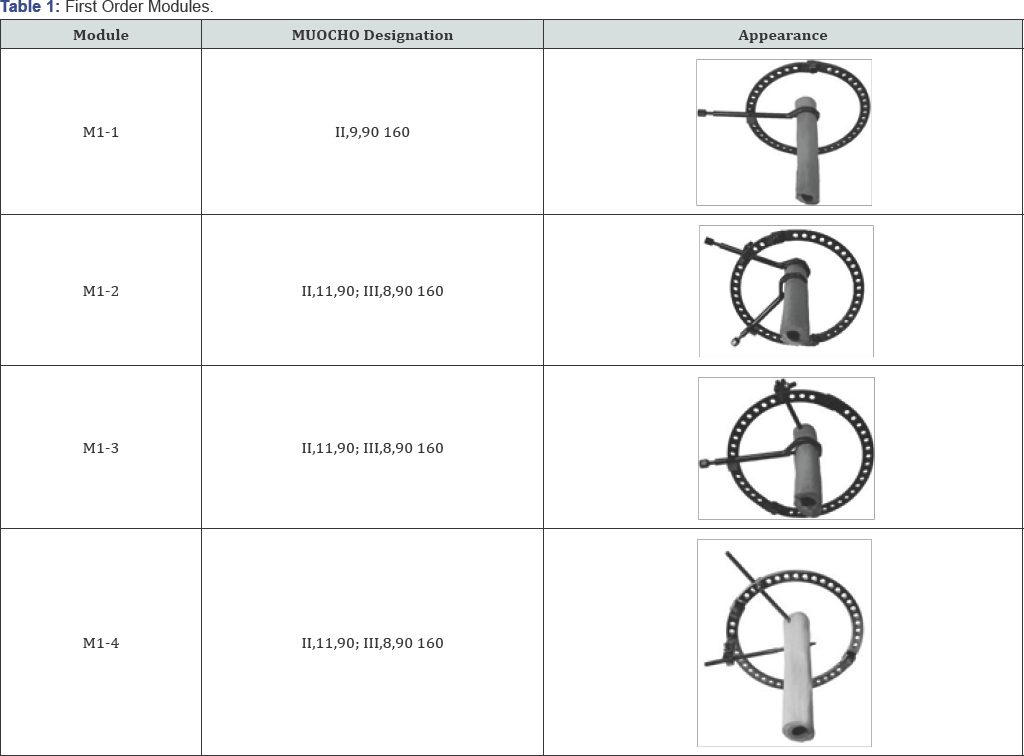
First and second order module assemblies were investigated with varying transosseous elements as shown in Tables 1 & 2. The module and transfixion element position nomenclature was described using the "Method of transosseous osteosynthesis unified notation" (MUOCHO) [18]. According to this method, each limb segment can be divided into eight equidistant levels (Roman numerals). Each level is divided into 12 equal positions, from 1 to 12. The angle of insertion is then given. Each element therefore has a level, position and angle of insertion; the denominator describes order modules.
Results
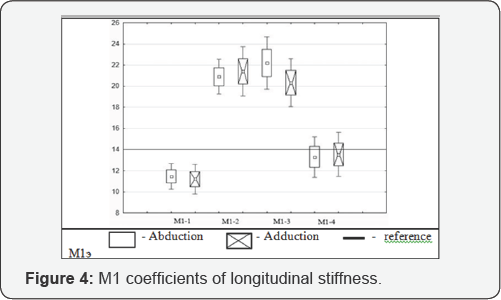
First order module (Ml) coefficients of stiffness are plotted in Figure 4-7.
Results are displayed in box & whisker plots, showing media, 25th and 65th percentile values. Ml coefficients
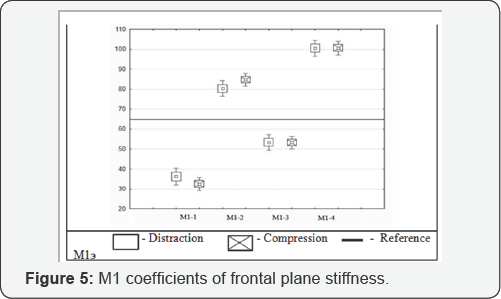
of longitudinal stiffness range from 32.5100.7N/mm with modules M1-2 and M1-4 providing rigidity superior to the value of the reference module (M1e). In the study of Ml frontal plane stiffness (Figure 5)
it was apparent that M1-1 and M1-2 had superior stability in abduction and adduction than M1-1 and M1-4 which approximated the reference standard. Sagittal plane coefficients of stiffness (Figure 6) revealed superior performance by all modules compared to the reference standard, the hybrid module M1-3 showed the greatest improvement, followed by the homologous M1-2 and M1-4 modules.

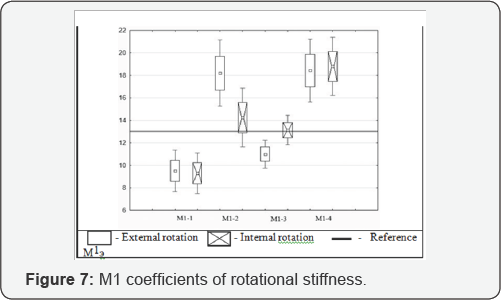
M1 stiffness in internal and external rotation (Figure 7) showed coefficient ranges from 9.3Nmm / deg to 18.8Nmm/ degree. The lowest stiffness was seen in M1-1, with modules M1-2 and M1-4 providing stiffness greater than the reference standard method, each limb segment can be divided into eight equidistant levels (Roman numerals). Each level is divided into 12 equal positions, from 1 to 12. The angle of insertion is then given. Each element therefore has a level, position and angle of insertion; the denominator describes the ring size. First order modules are joined with a hyphen to produce second order modules. Across all planes, M1-2 showed the most consistent improvement in stiffness, with the hybrid M1-3 providing superior sagittal and frontal plane stiffness, and the traditional M1-4 module the best performance in longitudinal rigidity.

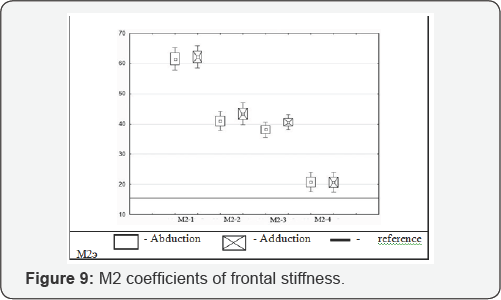
The resulting stiffness coefficients of the second order osteosynthesis modules are shown in Figure 8-11. In longitudinal stiffness testing of second order modules (Figure 8), a range of 70.7N/mm to 137.4N/mm was observed. All M2 values exceed that of the reference module (M2e), however the modules containing at least one ECD demonstrated far superior stiffness than that consisting of two Schanz screws (M2-4). M2 frontal plane stiffness (Figure 9) was noted to be maximal in M2-1 at 66nmm/deg, where the two ECDs are parallel, reduced as the angle between ECDs increased, as would be expected due to the maximal resistance to deformation with parallel devices applied in the plane of deformation, and was least where two Schanz screws were used. Sagittal plane stiffness of all M2 modules exceeded that of the reference module (Figure 10). Stiffness was greatest in M2-4, and least in M21. M2 rotational stiffness was greatest in M2-2, the two other M2 modules containing an ECD also showed greater stiffness than the reference module, with the M2-4 module showing performance similar to the reference (Figure 11).


Discussion & Conclusions
This study demonstrates that the ECD provides superior rigidity in both first and second order modules of external fixation to many types of external force as compared to traditional methods of transosseous fixation in diaphyseal bone. In M1 modules maximal rigidity is seen with two ECDs inserted with a 50mm distance and an angle of 60 degrees between points of insertion. When comparing the results of M1 and M2 modules incorporating ECDs, the numeric values show a definite increase in the coefficient of stiffness in M2 modules. This suggests that the ECD is ideally suited to application in the femur on the basis of the definite increase in the coefficient of stiffness when compared to Schanz screws, and by extrapolation, the utility of this device applies to femoral stabilisation regardless of modality of treatment i.e. periprosthetic fracture management, LON, BTON; where marginal fixation of Schanz screws into unicortical bone to avoid an intramedullary device would reduce the coefficient of stiffness and risk screw cut-out.
It can be postulated that in M1 modules, the reason for the superior performance of traditional Schanz screw fixation in pure compression and distraction can be inferred from the method of capture of the bone fragment by the ECD, as the coefficient of sliding friction of the clamp design would be least in the axis of the long bone due to the alignment of the teeth of the clamp. However, in angular and rotational stress, the clamp design provides a more rigid construct than that obtained by Schanz screw fixation. This has a potential advantage of permitting some desirable compression whilst reducing translational, angular and rotation deflection of fragments.
Options for the management of femoral periprosthetic fractures currently include revision to a long stem end prosthesis, rigid internal fixation with us without allogeneic cortical strut grafting, and external fixation, dependent on site of the periprosthetic fracture and fixity of the femoral component. In the management of a well fixed component with the fracture occurring at the tip of the component or below (Vancouver types B1 & C), typically internal fixation with or without grafting or external fixation are the most typically performed interventions [2,7,19]. Non-union of periprosthetic femoral fractures following rigid osteosynthesis is not an uncommon problem; the incidence of this complication has been reported to be as high as 30-33%, with an overall complication rate of 34-52% in the management of periprosthetic fractures [3,4,6].
Management of type B1 & C fractures by external fixation offers an attractive option by reducing the degree of soft tissue insult, blood loss, further devitalisation of an already compromised fracture site and thus the likelihood of atrophic non-union [2,12,19]. These options are limited in part due to the potential disadvantages of attempting transosseous osteosynthesis in the fragment containing a well fixed endo prosthesis, with potential for disruption of the endo prosthetic bed and subsequent loosening, fretting wear and wear debris generated by transosseous element contact with the prosthesis, and risk of introducing infection into the sterile implant zone. Extra cortical clamps have been successfully used in association with plates in a limited series, however these implants are bulky, and do not avoid the risks of formal open osteosynthesis [20].
Theoretically, the axial compression afforded by a frame construct incorporating ECDs would further reduce the likelihood of these complications and risks, just as circular external fixation is a successful method of obtaining union in the presence of diaphyseal non-union. These non-unions are typically atrophic or oligotrophic, and thus result from a failure of sufficient compression or reduced biological activity in the fracture site, which may have an iatrogenic component secondary to periosteal stripping and dissection. The application of the ECD does not circumferentially compress the periosteum, not is periosteal stripping necessary for its application, and thus this result in a more tissue-friendly approach without circumferential interruption of periosteal blood supply. The use of an external fixator with capture of the bone segments distant to the fracture site avoids further insult to the fracture envelope and so does not add further vascular compromise; likewise, the desirable biomechanical properties of an external fixator help avoid the likelihood of an oligotrophic non-union [21].
This study demonstrates the optimal configuration of modular frame construction in the femur, the data permits a customized approach to frame application dependent on the precise personality of the fracture and its inherent instability, such that transosseous element orientation can be accurately planned and matched to provide maximal rigidity within the plane of greatest instability. The apparent advantages of the ECD appear to have particular application in femoral external fixation where the transosseous element position has a narrow corridor of application due to impingement on soft tissues and bulkiness of the frame and thus may provide a superior frame construct than that currently achievable with standard transosseous fixation and limitations of frame design due to individual patient anatomy and location of pathology within the limb segment. This study has concentrated on the potential utility of the device in femoral applications, further studies will be performed to assess the suitability of the device in tibial and humeral applications.
The ECD is a novel device with attractive biomechanical characteristics which lends itself to the management of diaphyseal limb reconstruction and management of periprosthetic pathology. Further studies are necessary to investigate clinical efficacy, however the utility of the device across multiple applications is of the most potential value in the management of periprosthetic femoral fractures, where violation of the endoprosthetic bed is of the greatest significance.
References
- Marsland D, Mears SC (2012) A review of periprosthetic femoral fractures associated with total hip arthroplasty. Geriatr Orthop Surg Rehabil 3(3): 107-20.
- Giannoudis PV, Kanakaris NK, Tsiridis E (2007) Principles of internal fixation and selection of implants for periprosthetic femoral fractures. Injury 38(6): 669-687.
- Lindahl H, Malchau H, Herberts P, Garellick G (2005) Periprosthetic femoral fractures classification and demographics of 1049 periprosthetic femoral fractures from the Swedish National Hip Arthroplasty Register. J Arthroplasty 20(7): 857-865.
- Crockarell JR Jr, Berry DJ, Lewallen DG (1999) Nonunion after periprosthetic femoral fracture associated with total hip arthroplasty. J Bone Joint Surg Am 81(8): 1073-1079.
- Laurer HL, Wutzler S, Possner S, Geiger EV, El Saman A, et al. (2011) Outcome after operative treatment of Vancouver type B1 and C periprosthetic femoral fractures: open reduction and internal fixation versus revision arthroplasty. Arch Orthop Trauma Surg 131(7): 983989.
- Zuurmond RG, van Wijhe W, van Raay JJ, Bulstra SK (2010) High incidence of complications and poor clinical outcome in the operative treatment of periprosthetic femoral fractures: An analysis of 71 cases. Injury 41(6): 629-633.
- Solomin LN, Vilensky VA (2007) Treatment of periprosthetic femoral fractures by the method of transosseous osteosynthesis with the use of extracortical fixation. Traumatology & Orthopedics of Russia 44(2): 78-83.
- Kim HJ, Fragomen AT, Reinhardt K, Hutson JJ, Rozbruch SR (2011) Lengthening of the Femur Over an Existing Intramedullary Nail. J Orthop Trauma 25(11): 681-684
- Kocaoglu M, Eralp L, Kilicoglu O, Cakmak HBM (2004) Complications Encountered During Lengthening Over an Intramedullary Nail. J Bone Joint Surg Am 86(11): 2406-2411
- Mahboubian S, Seah M, Fragomen AT, Rozbruch SR (2012) Femoral lengthening with lengthening over a nail has fewer complications than intramedullary skeletal kinetic distraction. Clin Orthop Relat Res 470(4): 1221-1231.
- Paley D, Herzenberg JE, Paremain G, Bhave A (1997) Femoral lengthening over an intramedullary nail. A matched case comparison with Ilizarov femoral lengthening. J Bone Joint Surg Am 79(10):1464- 1480.
- Solomin L (2012) The basic principles of external skeletal fixation using the Ilizarov and other devices. Milan. Springer-Verlag Itali pp15- 93
- Eralp L, Kocaoglu M, Polat G, Bas A, Irican A, et al. (2012) A comparison of external fixation alone or combined with intramedullary nailing in the treatment of segmental tibial defects. Acta Orthop Belg 78: 652659.
- Karargyris O, Romoudis P, Morassi LG, Zafeiris C, Mavrogenis AF, et al. (2012) Distraction over nail using circular external fixation for septic pseudarthrosis of the tibia. J Long Term Eff Med Implants 22(2): 137143.
- Oh CW, Song HR, Roh JY, Oh JK, Min WK, et al. (2007) Bone transport over an intramedullary nail for reconstruction of long bone defects in tibia. Arch Orth Traum Surg 128(8): 801-808.
- Kendoff DO, Fragomen AT, Pearle AD, Citak M, Rozbruch SR (2010) Computer navigation and fixator-assisted femoral osteotomy for correction of malunion after periprosthetic femur fracture. J Arthroplasty 25(2): 333.e13-19.
- Kornilov NV (2005) Method of investigation of stiffness of transosseous osteosynthesis in planning operations. RNIITO RR Vreden Rec, Russia.
- Solomin LN (2014) Basics of transosseous osteosynthesis. BINOM 1(2e): 328.
- Moscow Sakai T, Ohzono K, Nakase T, Lee SB, Manaka T, et al. (2007) Treatment of periprosthetic femoral fracture after cementless total hip arthroplasty with Ilizarov external fixation. J Arthroplasty 22(4): 61720.
- Pleva L, Sir M, Madeja R (2004) Our experiences with the treatment of periprosthetic fractures of femur. Biomed Pap Med Fac Univ Palacky Olomouc Czech Repub 148(1):75-79.
- Fletcher MDA, Solomin LN (2015) Solomin LN. Definitive management of significant soft tissue loss associated with open diaphyseal fractures utilising circular external fixation without free tissue transfer, a comprehensive review of the literature and illustrative case. Eur J Orthop Surg Traumatol. 25(1): 65-75.






























