Knee Osteoarthritis Psychological Complications: An Important Overlooked Disease Correlate
Marks Ray*
Department of Health, Physical Education, Gerontological Studies and Services, York College, CUNY; Teachers College, Health and Behavior Studies, Columbia University, New York, USA
Submission: July 17, 2017; Published: July 26, 2017
*Corresponding author: Marks R, Department of Health and Behavior Studies, Teachers College, Columbia University Box 114, 525W, 120th Street, New York, NY 10027, USA, Tel: 1-212-678-3445; Fax: 1-212-678-8259; Email: rm226@columbia.edu
How to cite this article: Marks R. Knee Osteoarthritis Psychological Complications: An Important Overlooked Disease Correlate. Nov Tech Arthritis Bone Res. 2017; 1(4) : 555568 DOI: 10.19080/NTAB.2017.01.555568
Abstract
Background: Knee osteoarthritis, a highly common progressively disabling health condition affecting many older adults is commonly examined and treated on the basis of its physical and biomechanical correlates.
Objective: This paper was designed to draw attention to the key psychological complications that can prevail in knee osteoarthritis, plus the link of these attributes to pain.
Method: Using the key words: knee osteoarthritis, as well as depression and anxiety, publications located in PUBMED and Web of Science data bases over the past twenty years were sought. Specifically documented were facts concerning the prevalence of depression and anxiety among this group, and the association of these conditions with pain.
Results: The evidence base clearly shows a significant number of adults diagnosed with knee osteoarthritis may be suffering from symptoms of either depression or anxiety or both. Cases that exhibit depressive symptoms and anxiety appear toexperience more pain than those who do not.
Conclusion: Clinicians seeking to reduce the immense burden of painful knee osteoarthritis will find efforts to identify and treat the psychological correlates of depression and anxiety of benefit at all disease stages.
Keywords: Anxiety; Depression; Disability; Knee osteoarthritis; Pain; Treatment
Introduction
Osteoarthritis, the most common joint disease, causes appreciable disability among large numbers of older adults [1-5]. Commonly attributed to progressive disruption of the particular cartilage lining of one or more freely moving joints, plus underlying bone pathology [6-8] this oftentimes produces incapacitating dysfunction [9-10] that may be accompanied by varying degrees of unrelenting pain, joint stiffness and swelling, physical de conditioning, and multiple functional, social, occupational challenges and restrictions. In addition, individuals affected by osteoarthritis may suffer from the presence of one or more debilitating chronic health conditions, such as cardiovascular diseases and obesity, negative self perceptions, heightened fear, obesity, disfigurement, and a low life quality and earnings capacity.
Unfortunately, despite its prevalence, and significant physical, economic, psychological, and social impact, there is presently no known cure for osteoarthritis, and those treatments that are available are not always efficacious, or indicated for a particular patient [5]. Moreover, a number of medications used to ameliorate the condition may prove harmful to the joint tissues [7,8], foster toxic side effects [11], and/or excess mortality due to their gastrointestinal effects.
There is however, a great need to minimize the extent of osteoarthritis disability, and thus factors that can offset or delay predictable consequences of excess morbidity and possibly of excess or premature mortality are of great interest to both the clinician and the patient.
To this end, this report outlines some recent observations concerning knee osteoarthritis, the most common form of osteoarthritis, and the extent and impact of depression and anxiety that can prevail among adults with this condition. Some suggestions for treatment based on this information are included as well. The topic of depression and anxiety is specifically investigated due to the potential prevalence of these conditions among patients with chronically painful disabling knee joint osteoarthritis, as well as their potential for clinical detection, prevention and/or remediation.
In addition, emerging evidence suggests the disability experienced by adults with osteoarthritis is not wholly explained by radiograph measures, and that some of the complaints experienced by affected individuals seeking medical help for painful symptomatic osteoarthritis may be related to psychological factors [12]. In addition, the presence of one or more chronic comorbid conditions, found in knee osteoarthritis, makes it likely depression and/or anxiety will prevail in this group as the disease progresses.
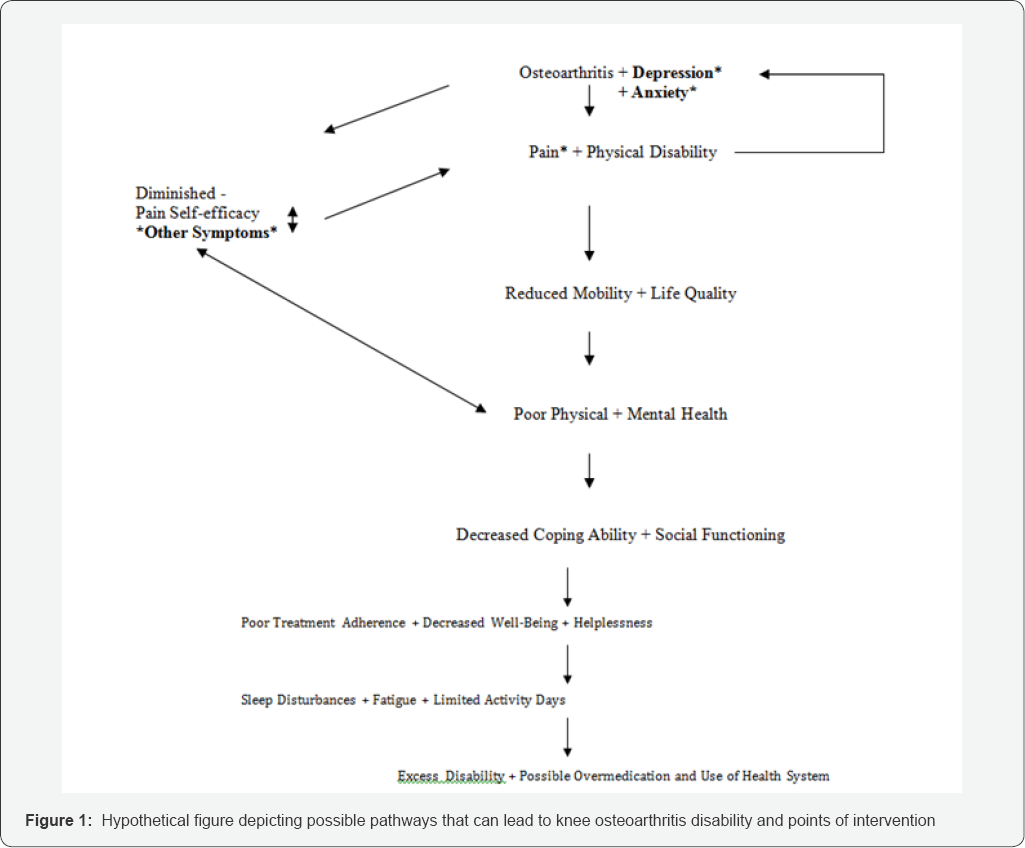
Based on many years of research in the realm of chronic pain and other chronically painful health conditions, it was assumed depression and/or anxiety would be found to be quite common among knee osteoarthritis cases, and where present would be expected to significantly exacerbate the overall pain experience, and resultant disability of the individual [13-17], including feelings of helplessness, fear, reduced coping ability, personal efficacy, and sleep hygiene [18-22]. In turn, this negative spiral of feedback responses would be expected to foster varying degrees of negative affect [22], and a sedentary lifestyle, regardless of the prevailing degree of osteoarthritic damage [23] as outlined in Figure 1. To obtain support for these ideas, the author conducted an in depth scan of the literature as outlined below.
Methods
First, relevant information housed in the major data bases on this topic was sought and examined. After careful analysis, only those articles that addressed the current themes and referred to these topics specifically were retrieved, read and analyzed. No systematic data synthesis was undertaken however, due to the variation in research questions and assessment approaches observed in the available literature. Instead data on prevalence, as well as linkages between depression, anxiety and osteoarthritis of the knee were examined and relevant emergent issues and themes are specifically discussed. Finally some challenges as well as recommendations for clinicians and researchers are presented. Since the topic is very sparsely addressed in the literature all types of research articles were deemed acceptable, unless the form of arthritis studied was unclear. In both cases it was decided to examine these two key correlates relative to pain, the complaint of most relevance to patients, as opposed to other outcome variables. This focus was also chosen because in the case of both data bases employed, so many diverse topics were forthcoming when using the key words listed above emerged, but few were pertinent to the present discussion.
Results
Using the key words depression and knee osteoarthritis or anxiety and knee osteoarthritis the Web of Science Composite data base, yielded 837 and 335 contributions respectively, between 2002 and July 2017; there were 368 articles on depression and 198 on anxiety listed in PUBMED from 1980- July 2017. Articles that discussed both depression and anxiety commonly did so in the context of total knee joint arthroplasty surgery, mental health, sleep health, and quality of life issues.
Prevalence of depression
The precise prevalence of depression among people suffering from knee osteoarthritis, while theoretically important, appears hard to establish. Not only is this topic very sparsely documented, when compared to other more commonly reported topics, such as biomechanical disease correlates, but even when it is mentioned, the methods of assessment, and differing approaches employed are highly inconsistent, and do not necessarily provide definitive depression data, but rather evidence of symptomatic depression. Moreover, even when methods of assessing depression are reasonably similar, and have been consistently applied, published results tend to vary considerably. For example, Gandhi et al. [24] estimated this to be 12.2% among individuals undergoing either hip or knee surgery for osteoarthritis. They also reported higher rates of depression relative to the numbers of affected joints, but the exact prevalence of the depressive symptoms in the knee osteoarthritis sample could not be accurately determined in this mixed sample. Similarly, although Wong et al. [25] found 39% of a group of 115 knee osteoarthritis cases to have a psychiatric disorder after screening for both anxiety and depression, and conducting psychiatric interviews, the precise number of cases suffering from depression was not forthcoming. While it can be assumed that the frequency of depression was quite high in the study by Wong et al., Smith et al. [26] found only 8% of cases undergoing hip or knee arthroplasty to have a diagnosis of depression, but again, how many of these cases with knee osteoarthritis were impacted by depression was uncertain. Although these data are thus challenging to reconcile, das Nair et al. [27] stated one third of cases with osteoarthritis are likely to have mood problems.
More recently, Khatib et al. [28] who assessed psychological traits in patients waiting for total knee arthrovplasty, did observe that 26.8% of these individuals reported psychological distress. However, this group may have included subjects with rheumatoid arthritis, a more serious joint condition, and while the data by Castano Carou et al. [29] support this latter observation to some degree, the specific prevalence among cases with knee osteoarthritis alone and for depression alone could again not be delineated with any degree of confidence.
In other related research efforts, Howard et al. [30] found 38% of patients with severe knee osteoarthritis were distressed psychologically before surgery. This and the aforementioned studies are important to note, even if depression itself was not documented specifically as a correlate because it has been shown that psychological distress, possibly including depression, can occur both before and following knee replacement surgery as outlined by Creamons-Smith et al. [31]. This latter group found up to 20% of 110 patients reported noteworthy levels of distress, which is generally consistent with observations. Tonelli et al. [32] who found depression rates of approximately 15% in men and women prior to total knee replacement, while Duivenvoorden et al. [33] observed a pre surgical prevalence rate of depression of 22%
Even higher rates were observed however, in a crosssectional analysis of 100 community dwelling adults diagnosed as having knee osteoarthritis of one or both knees [see reference 33] where symptoms of depression occurred in 52% of cases and of these 52 cases, 27 had moderate or severe signs of depression. Individuals younger than 60 years of age who had a higher prevalence of unilateral rather than bilateral knee osteoarthritis, reported higher mean pain scores as well as depression scores than those over age 60, suggesting this sub group is highly vulnerable to psychological distress. Males with knee osteoarthritis reported higher levels of depression than females, suggesting that gender may be an important mediating or moderating correlate underpinning the extent of knee osteoarthritis disability.
Based on these data, even though healthy controls have not been studied in most of these studies, and samples have been mixed or highly variable, with no precise validation of the actual comorbid condition of depression, it can be deduced that depressive symptoms can occur at modest to high rates among knee osteoarthritis sufferers, especially those with advanced disease, those who are younger than 60 years of age, and those who are undergoing joint replacement surgery, either as a comorbid preexisting condition or as a reactive response.
Prevalence of anxiety
Among studies that have examined rates of anxiety symptoms among knee osteoarthritis sufferers, similar measurement challenges arise. Nonetheless, Axford et al. [34] found rates of clinically significant anxiety and/or depression of 40.7% in cases of knee osteoarthritis, suggesting anxiety should not be overlooked as a psychological complication. Duivenvoorden et al. [35] too found modest anxiety prevalence rates of 20.3% among that awaiting knee replacement surgery. High rates of anxiety were also noted by Ferreira et al. [36], and Tonelli et al. [37] in conjunction with knee osteoarthritis, regardless of whether trait or state anxiety was assessed.
Ellis [38] who examined 154 indigent knee arthroplasty surgery cases found 11% has presurgical anxiety, but data presented by Jacobs et al. [39] who followed 1020 knee arthroplasty surgery cases for 2 years showed 41.9% of less severe cases, reported anxiety, and this subgroup was more dissatisfied than more severe cases.
In sum, anxiety when assessed seems to occur alone or in combination with depression in a modest percentage of knee osteoarthritis cases, and can influence the extent to which treatment is perceived as efficacious or not, a conclusion supported by Stubbs et al. [40].
Depression, anxiety, and pain
Studies examining the nature of the linkage between depression, anxiety, and pain among knee osteoarthritis cases, generally show pain, the symptom of most concern to knee osteoarthritis patients, can both mask depression, exacerbate depression, and/or anxiety, thus intensifying the pain experience. Ghandi et al. [24] found subjects with osteoarthritis who reported six or more painful joints including the hips and knees, had a 2.5 fold or greater odds of depression when compared to those whose symptoms were limited to a single surgical joint. Moreover, Holla et al. [41] found depression was independently associated with knee pain and activity limitations in people with knee osteoarthritis, and Aflaki et al. [42] reported a linear correlation between depression severity and pain, stiffness and function in knee osteoarthritis cases.
Axford et al. [36] too found that greater pain was associated with greater depression in cases with knee osteoarthritis. Similarly, Hirshmann et al. [43] found individuals with higher levels of psychological distress to be at higher risk for experiencing more pain and more disabling disease before and after knee surgery than those with no such problems.
Depression in turn, contributes to the osteoarthritis pain cycle [42], as well as pain and disability [43], and Zullig et al. [44] found depressive symptoms were associated with worse pain. Depression is also a risk factor for post surgical pain [45,46] and worse function over a 1-year period [47], as well as pain, but not necessarily for radiographic disease severity within a 3-4 year follow up period [48]. Wylde et al. [49] however, found that the presence of severe persistent pain at 3 or 4 years after total knee replacement was significantly related to major depression, as well as number of pain problems at other body sites. Bierke et al. [50] similarly found depressive symptoms affected the course of pain one year after uncomplicated total knee replacement surgery in that more depressed patients had higher pain scores post operatively, as did anxious patients. Salaffi et al. [51] who examined the relationship between disability and psychological variables of anxiety and depression among 61 women with symptomatic knee osteoarthritis using an anxiety inventory, and a pain index found pain correlated with the degree of psychological involvement.
Likewise, Smith and Zautra [52] who examined the effects of anxiety on pain in women with osteoarthritis and rheumatoid arthritis found anxiety was related to elevations in current and forthcoming pain estimates. In particular, when studying the differential effects of depression and anxiety on pain, it was noted that the effects were nearly twice as large for anxiety compared to depression, suggesting the mechanism of action is unique.
These data were further substantiated by Sinikallio et al. [53], who examined cases with knee osteoarthritis and found elevated anxiety was associated with pain, and that the osteoarthritis cases reported high levels of anxiety. Earlier, Somers et al. [54] noted osteoarthritis cases with higher levels of depression tended to be more prone to report increased osteoarthritis pain, and depressed patients tended to report more pain than those who were not depressed after total knee arthroplasty [55]. Similarly, Zautra and Smith who found elevations in depression correlated with pain elevations among cases with osteoarthritis [56], Dekker et al. [57] found pain and anxiety were correlated in osteoarthritis [57], and Schiphof et al. [58] showed depression yielded significant interactions with knee pain in cases without osteoarthritis. Earlier work by Salaffi et al. [58] did show osteoarthritis pain was highly impacted by psychological factors, that depressive symptoms in turn, can impair the ability to detect the origin of knee pain complaints [59].
In sum, psychological factors are prevalent among cases diagnosed as having knee osteoarthritis, and these problems impact pain or are impacted by unrelenting pain [60,61]. In particular, Smith & Zautra [62] who examined 88 cases of women with osteoarthritis using 19 items from the Mental health Inventory found depression predicted elevations in current and anticipated pain in the next week. Van Baar et al. [63,64] too, found that regardless of the importance of systemic or mechanical mechanisms affecting osteoarthritic pain, factors such as depression can predict the extent of the disease impact more strongly than the apparent extent of visible joint damage. In addition, Ahn et al. [65] noted higher levels of depression may contribute to greater clinical pain in knee osteoarthritis cases, as did Rathburn et al. [66], and Jung found an association between osteoarthritis, high stress levels, depression and suicidal ideation [67]. Earlier, Summers et al. [19] found that even after controlling for disease severity, psychological variables including depression remain strong predictors of individual differences in pain among adults with knee osteoarthritis, a finding supported by Okma-Keulen & Hopman-Rock [64].
Clinical implications
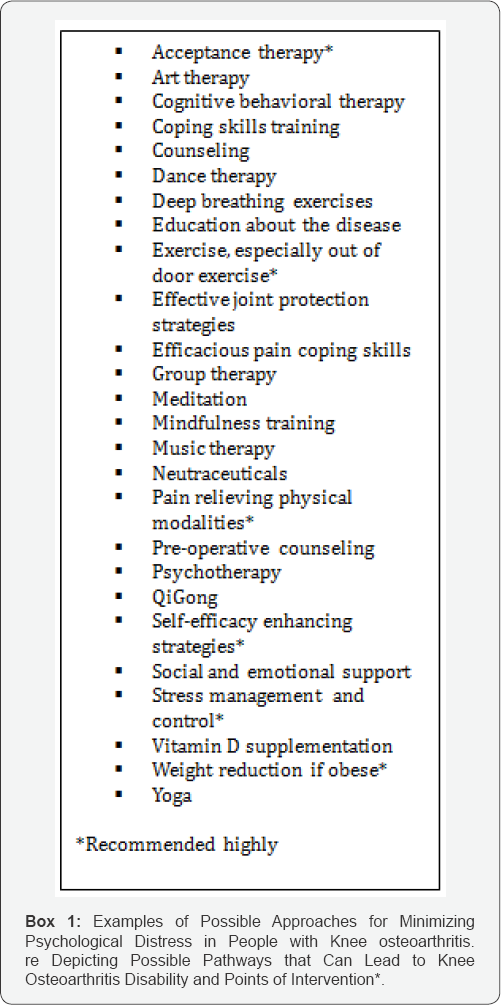
To improve the outlook for people with knee osteoarthritis, efforts to routinely assess the patient's psychological status, followed by treatment, as required, are clearly indicated. However, because a one size fits all approach is unlikely to be efficacious, a well designed tailored set of strategies to minimize any prevailing psychological distress is recommended. These strategies may include, but are not limited to items listed in Box 1.
Discussion
Osteoarthritis, the most common joint disease causes appreciable disability in a high percentage of older individuals. A health condition with no known cure, factors contributing to the disease process have been the subject of study for more than 30 years with much attention being devoted to uncovering the physical mechanisms underlying this disease, which involves significant damage to bone and articular cartilage of one or more joints. More recently, however, in efforts to better understand all factors contributing to its pathogenesis [68], in addition to examining the physical correlates of osteoarthritis disability, emphasis has been placed on examining the psychological correlates of osteoarthritis disability, such as depression, Because osteoarthritis is the major cause of constant pain among older populations [69], a group with a high prevalence of depression [70], and disability [69], it was consequently deemed beneficial to examine the related literature in this area in the hope of identifying if psychological correlates, which are potentially modifiable, are implicated in the pathway from osteoarthritis pathology to disability [9], or in mediating or moderating the extent of osteoarthritis-related pain and disability [71-73].
Unfortunately, despite its prevalence, there is a very limited body of definitive information on this aforementioned aspect of health in the context of osteoarthritis [71], even though Maisiak [74] reported the presence of a depressive affect was three times more likely to occur among individuals with osteoarthritis than among nonarthritic individuals.
As well, even though osteoarthritis is said to be syndrome associated with depression [69], and this population may suffer from depression to a greater extent than healthy controls [47], the related literature on osteoarthritis is often hard to interpret because other conditions such as rheumatoid arthritis are often studied simultaneously [9]. Even when osteoarthritis alone is studied, the fact that mixed samples are studied, makes it challenging to identify the role of either anxiety or depression in knee osteoarthritis specifically. Hence the prevalence of these psychological correlates, and their unique or specific impact either as pre-existing or as reactive conditions remains unclear. It was also evident that despite the potential benefits of identifying and treating depression and anxiety [28,39], in addition to treating osteoarthritic pain, depression, anxiety, and its consequences, these are frequently omitted topics in publications designed to highlight available treatment options for this cohort (e.g. [8]).
Moreover, most commonly, depression or anxiety are not actually measured, cut-off scores for depressive/anxiety symptoms vary, as do survey related tools designed to measure depression and anxiety.
Thus even though the present work sought to examine what is known about the prevalence and impact of co-occurring or reactive depression/anxiety among cases with the most common form of osteoarthritis, namely, knee osteoarthritis, nothing definitive can be said. A further analysis to examine the link between pain and affective changes among patients with knee osteoarthritis did seem to indicate this is however, a very important topic to pursue in the future and is one with immense clinical implications atall stages of the disease process.
Consequently, even though neither Creamer et al. [75] or Scopaz et al. [76], nor Maly et al. [77] found depression of clinical relevance in the context of knee osteoarthritis, the current findings showed others have observed substantive rates of depression in cases with knee osteoarthritis [33,78], and that where present, the presence of depressive symptoms can have profound health implications [79] for pain and disability outcomes as outlined by Rosemann et al. [80] and Ghandi et al. [24]. At the same time, a reasonable number of people with diagnoses of both knee joint osteoarthritis and depression may receive no depression treatment [81], even though research shows cases with knee osteoarthritis are more likely to be classified as being depressed than adults with similar characteristics, but no evidence of osteoarthritis [70]. Similar arguments can be applied to anxiety even though Singh and Lwellyn [82] found anxiety was associated with 1.4 higher odds (95% CI 1.0, 2.0) of moderate to severe index knee pain at 2 years; at 5 years and anxiety contributes to physical functioning [83] and worse outcomes after joint replacement surgery [84].
Given that individuals with knee osteoarthritis and co existing depression and /or anxiety symptoms are more likely to experience functional limitations and severe pain than those who are mentally healthy, failure to identify and treat these comorbid conditions may be expected to produce less than optimal health outcomes, including, greater levels of pain. Conversely, those patients who exhibit depressive and/or anxiety symptoms and who do receive appropriate treatments and treatment recommendations may be expected to experience more optimal outcomes than those who do not [43].
In addition to having a negative impact on conservative management approaches commonly applied to help manage osteoarthritis disability, the failure to identify and treat depression or anxiety, where they exist - may clearly have an equally deleterious effect on surgical treatments, and recovery rates following surgery as outlined by Possley et al. [85]. Ample research shows moreover, that the failure to apply appropriately timed and targeted interventions that also address psychological correlates and their presence as comorbid and/or reactive aspect of the condition can adversely heighten pain in general [86], plus the presence of excess or persistent pain following joint replacement surgery [49,84,82,87,88].
Sale et al. [89] found having a depressed mood was also influential in explaining the extent to which older adults experienced fatigue, stress, and perceptions that their coping strategies were unsuccessful, even though these cases used more coping strategies than those without depressive symptoms. Consequently, this group suggested individuals treating people with painful knee osteoarthritis consider the possibility that both conditions, that is, osteoarthritis and depression may readily coexist especially among older individuals with high rates of radiographic pathology [90,91]. Since both pain and disability in osteoarthritis of the knee are positively related to depression and anxiety scores, minimizing the extent of any depressive or anxiety related symptoms is arguably essential for allaying the onset and progression of pain, as well as for improving osteoarthritis treatment outcomes in general, and especially for better post-operative results if this is indicated. Alternately, an individual with osteoarthritis who feels anxious or depressed because no one is responding to their situation adequately may experience greater levels of disability or rates of joint deterioration especially if they are not motivated towards self-care or instructed to do this, regardless of actual pathology status [92,93]. They are also likely to use more pain medication than those without concomitant depression [94], to exhibit higher health utilization rates [94], and to display less adherence to treatment regimens [85,94], and lower forms of social functioning [86].
In addition, they may be less active physically [89], as well as less able to control their weight, given that depressive symptoms are common in overweight cases of osteoarthritis as observed by Possley et al. [82] and Rosemann et al. [90]. Since knee osteoarthritis cases who are depressed also tend to be heavier than those who are not [80,87], this situation may not only place excess stress on their already damaged joints, but may exacerbate pain directly [91] as a result of complex metabolic and inflammatory responses. Since weight gain can ensue not only through the excess inactivity that can arise as a result of the presence of co-existing depression and increased pain, reduced motivation for physical and social activity, plus self-efficacy for physical activity [77], and a sense of perceived failure to cope with their difficulties [85], it appears more needs to be done to identify and address these highly salient overlapping health outcome determinants of knee osteoarthritis [16]. In particular, in order to minimize the possibility of excess weight gain and excessive knee joint deterioration [88,92] due to anti depressants, the importance of minimizing depression safely without side effects cannot be overestimated in the context of both weight control, as well as pain control.
In sum, because both comorbid as well as reactive depression and anxiety may co exist in adults with knee osteoarthritis, and there is an association between these psychological factors and risk of osteoarthritic pain flares [93], numbers of affected lower limb joints including the knee [95], and life quality [96], strategies to treat or minimize depression or anxiety among this population are highly indicated. In this respect, more efforts to screen for anxiety and depression, plus specific exploration of desirable assessment approaches, followed by carefully construed intervention [s] may lead to better treatments and referrals [97]. To this end, outcomes examined among knee osteoarthritis samples with and without such interventions at different disease stages may help us to better discern the importance of identifying and treating evidence of co existing clinical depression and anxiety as well as symptomatic depression or anxiety and their typologies. Examining what types of pain are implicated in these situations in the specific case of this form of osteoarthritis is also strongly indicated as suggested by Veronese et al. [95] and Kim et al. [96].
In short, notwithstanding the widespread myth that osteoarthritis is inevitable and irreversible [94] and that it is therefore futile to try and prevent this problem, along with societal mores that demand stoicism and the belief pain and aging are synonymous, more proactive screening for depression and anxiety followed by appropriate treatments in the adult population is surely likely to be especially advantageous [97]. Bearing in mind that the depressive phenotype found in knee osteoarthritis showed higher pain levels and more severe activity limitations than three other phenotypes, with the exception of the obese/weak phenotype [98,99], detection of this serious comorbidity is likely to be highly influential clinically as well as functionally [96].
Indeed, efforts to minimize cognitions that involve negative associations or experiences may not only strengthen the patient's ability to overcome the tendency to avoid physical and social activities that can lead to muscle weakness, joint instability, excess pain and severe disability [97,100], increased rates of sleep fragmentation or sleep disturbances [93], excess body mass [98], the development of disability and longer term worse pain [99], and increased risk of participation restriction [100], but may enable surgery outcomes to be maximized or surgery to be averted, and ultimately to foster a high rather than a low life quality, regardless of intervention mode [88].
To accurately establish whether or not persons with knee osteoarthritis are depressed or anxious or both, given the variety of instruments and measures reported for this purpose in the related literature, more comparative studies to identify the most sensitive and responsive instruments for identifying and following up on both depression and anxiety in a variety of samples at different disease stages is especially indicated. However, in the event of time constraints, simply asking patients about any symptoms of depression or anxiety is also advocated [21], as outlined by Ghandi et al. [24] who found this measure correlated well with actual treatments for depression. Valid and timely assessments followed by carefully construed psychological treatment strategies may be highly effective for reversing or attenuating the extent of disability shown in Figure 1 [100,101] and should be subjected to careful scrutiny in order to advance evidence based practices for knee osteoarthritis [102-110].
Conclusion
As outlined above, knee osteoarthritis, a chronic degenerative joint disease of unknown cause produces high degrees of pain and disability among older adults. Among the specific disease consequences evidence reveals:
a. Psychological correlates of depression and anxiety highly implicated in the pain disability cycle [28] are often overlooked as a predictors of symptoms and dysfunction in persons with knee osteoarthritis [25, 27], but do appear to prevail in a fair percentage of patients [39].
b. Correlated with pain, treatment of depression and anxiety is predicted to improve knee osteoarthritis outcomes, especially pain, regardless of stage of disease.
c. In contrast, failure to acknowledge the presence of psychological distress among cases with knee osteoarthritis is likely to produce less than optimal clinical and surgical outcomes, regardless of disease status, even if these correlates do not alter radiographic severity [48].
More work is needed however, to examine both these psychological correlates and how they contribute to the pain cycle in well-defined knee osteoarthritis samples, and whether those treated appropriately are likely to experience significantly lower degrees of pain and disability than those with undiagnosed depressive or anxiety symptoms. Comparative studies to establish the degree to which depression and anxiety are causative factors, or reactive disease correlates in the knee osteoarthritis pain cycle are especially recommended.
References
- Zhang Y, Jordan JM (2010) Epidemiology of osteoarthritis. Clin Geriatr Med 26(3): 355-369.
- Kwok WY, Vliet Vlieland TP, Rosendaal FR, Huizinga TW, Kloppenburg M (2011) Limitations in daily activities are the major determinant of reduced health-related quality of life in patients with hand osteoarthritis. Ann Rheum Dis 70(2): 334-336.
- Murphy L, Helmick CG (2012) The impact of osteoarthritis in the United States: a population-health perspective: a population-based review of the fourth most common cause of hospitalization in US adults. Orthop Nurs 31(2): 85-91.
- Moskowitz RW (2009) The burden of osteoarthritis: clinical and quality-of-life issues. Am J Manag Care 15(8): S223-S229.
- Swift A (2012) Osteoarthritis 1: Physiology, risk factors and causes of pain. Nurs Times 108(7): 12-15.
- Martel-Pelletier J, Boileau C, Pelletier JP, Roughley PJ (2008) Cartilage in normal and osteoarthritis conditions. Best Pract Res Clin Rheumatol 22(9): 351-384.
- Kubota M, Ishijima M, Kurosawa H, Liu L, Ikeda H, et al. (2010) A longitudinal study of the relationship between the status of bone marrow abnormalities and progression of knee osteoarthritis. J Orthop Sci 15(5): 641-646.
- Sinusas K (2012) Osteoarthritis: diagnosis and treatment. Am Fam Physician 85(1): 49-56.
- McDonough CM, Jette AM (2010) The contribution of osteoarthritis to functional limitations and disability. Clin Geriatr Med 26(3): 387-399.
- Edwards RR, Calahan C, Mensing G, Smith M, Haythornthwaite JA (2011) Pain, catastrophizing, and depression in the rheumatic diseases. Nat Rev Rheumatol 7(4): 216-224.
- Griffin MR, Brandt KD, Liang MH, Pincus T, Ray WA (1995) Practical management of osteoarthritis. Integration of pharmacologic and nonpharmacolic measures. Arch Fam Med 4(12): 1049-1055.
- Hochberg MC, Lawrence RC, Everett DF, Cornoni-Huntley J (1989) Epidemiologic associations of pain in osteoarthritis of the knee: Data from the National Health and Nutrition Examination Survey and the National Health and Nutrition Examination-I Epidemiologic follow-up survey. Semin Arthritis Rheum 18(4 suppl 2): 4-9.
- Briggs A, Scott E, Steele K (1999) Impact of osteoarthritis and analgesic treatment on quality of life of an elderly population. Ann Pharmacother 33(11): 1154-1159.
- Jackson DW, Simon TM, Aberman HM (2001) Symptomatic articular cartilage degeneration: the impact in the new millennium. Clin Orthop Rel Res 391(Suppl): S14-S25.
- Kuller LH (1984) The epidemiology of osteoarthritis. In: Lawrence RC, Shulman LE (Eds). Epidemiology of the Rheumatic Diseases: Proceedings of the Fourth International Conference. New York, Gower, USA, pp. 282-289.
- Creamer P, Hochberg MC (1998) The relationship between psychosocial variables and pain reporting in osteoarthritis of the knee. Arthritis Care Res 11(1): 60-65.
- Woolf CJ (1989) Recent advances in the pathophysiology of acute pain. Br J Anaesth 63(2): 139-146.
- Wilcox S, Brenes GA, Levine D, Sevick MA, Shumaker SA, Craven T (2000) Factors related to sleep disturbance in older adults experiencing knee pain or knee pain with radiographic evidence of knee osteoarthritis. J Am Geriatr Soc 48(10): 1241-1251.
- Summers MN, Haley WE, Reveille JD, Alarcon GS (1988) Radiographic assessment and psychological variables as predictors of pain and functional impairment in osteoarthritis of the knee or hip. Arthritis Rheum 31(2): 204-209.
- Keefe FJ, Caldwell DS, Queen KT, Gil KM, Martinez S, et al. (1987) Pain coping strategies in osteoarthritis patients. J Consult Clin Psychol 55(2): 208-212.
- Keefe FJ, Caldwell DS, Queen KT, Gil K, Martinez S, et al. (1987) Osteoarthritic knee pain: a behavioral analysis. Pain 28(3): 309-321.
- Axford JS, Ross F, Triggs E, Victor C (2000) Osteoarthritis of the knee causes appreciable disability in females associated with depression and inability to cope. Arthritis Rheum 43: S927.
- Zautra AJ, Smith BW (2001) Depression and reactivity to stress in older women with rheumatoid arthritis and osteoarthritis. Psychosom Med 63(4): 687-696.
- Gandhi R, Zywiel MG, Mahomed NN, Perruccio AV (2015) Depression and the overall burden of painful joints: an examination among individuals undergoing hip and knee replacement for osteoarthritis. Arthritis 2015(2015): 327161.
- Wong LY, Yiu RL, Chiu CK, Lee WK, Lee YL, et al. (2015) Prevalence of psychiatric morbidity in Chinese subjects with knee osteoarthritis in a Hong Kong orthopaedic clinic. East Asian Arch Psychiatry 25(4): 150-158.
- Smith TO, Penny F, Fleetcroft R (2016) Medical morbidities in people following hip and knee arthroplasty: data from the Osteoarthritis Initiative. Eur J Orthop Surg Traumatol 26(1): 99-106.
- Khatib Y, Jenkin D, Naylor JM, Harris IA (2016) Psychological traits in patients waiting for total knee arthroplasty. a cross-sectional study. J Arthroplasty 31(8): 161-166.
- Castaño Carou A, Pita Fernández S, Pértega Díaz S, de Toro Santos FJ, Grupo de estudio EvalÚa (2015) Clinical profile, level of affection and therapeutic management of patients with osteoarthritis in primary care: The Spanish multicenter study EVALÚA. Reumatol Clin 11(6): 353-360.
- Howard KJ, Ellis HB, Khaleel MA, Gatchel RJ, Bucholz R (2011) Psychosocial profiles of indigent patients with severe osteoarthritis requiring arthroplasty. J Arthroplasty 26(2): 244-249.
- Cremeans-Smith JK, Greene K, Delahanty DL (2011) Symptoms of postsurgical distress following total knee replacement and their relationship to recovery outcomes. J Psychosom Res 71(1): 55-57.
- Tonelli SM, Rakel BA, Cooper NA, Angstom WL, Sluka KA (2011) Women with knee osteoarthritis have more pain and poorer function than men, but similar physical activity prior to total knee replacement. Biol Sex Differ 2: 12.
- das Nair R, Anderson P, Clarke S, Leighton P, Lincoln NB, et al. (2016) Home-administered pre-surgical psychological intervention for knee osteoarthritis (HAPPiKNEES): study protocol for a randomised controlled trial. Trials 17: 54.
- Marks R (2007) Physical and psychological correlates of disability among a cohort of individuals with knee osteoarthritis. Can J Aging 26(4): 367-377.
- Duivenvoorden T, Vissers MM, Verhaar JA, Busschbach JJ, Gosens T, et al. (2013) Anxiety and depressive symptoms before and after total hip and knee arthroplasty: a prospective multicentre study. Osteoarthritis Cartilage 21(12): 1834-1840.
- Ferreira AH, Godoy PB, Oliveira NR, Diniz RA, Diniz RE, et al. (2016) Investigation of epression, anxiety and quality of life in patients with knee osteoarthritis: a comparative study. Rev Bras Reumatol 55(5): 434-438.
- Axford J, Butt A, Heron C, Hammond J, Morgan J, et al. (2010) Prevalence of anxiety and depression in osteoarthritis: use of the Hospital Anxiety and Depression Scale as a screening tool. Clin Rheumatol 29(11): 1277-1283.
- Ellis HB, Howard KJ, Khaleel MA, Bucholz R (2012) Effect of psychopathology on patient-perceived outcomes of total knee arthroplasty within an indigent population. J Bone Joint Surg Am 94: e84.
- Jacobs CA, Christensen CP, Karthikeyan T (2015) Chronic non- orthopedic conditions more common in patients with less severe degenerative changes that have elected to undergo total knee arthroplasty. J Arthroplasty 30(7): 1146-1149.
- Stubbs B, Aluko Y, Myint Pk, Smith TO (2016) Prevalence of depressive symptoms and anxiety in osteoarthritis: a systematic review and metaanalysis. Age and Aging 45(2): 228-235.
- Holla JF, van der Leeden M, Knol DL, Peter WF, Roorda LD, et al. (2012) Avoidance of activities in early symptomatic knee osteoarthritis: results from the CHECK Cohort. Ann Behav Med 44(1): 33-42.
- Hirschmann MT, Testa E, Amsler F, Friederich NF (2013) The unhappy total knee arthroplasty (TKA) patient: higher WOMAC and lower KSS in depressed patients prior and after TKA. Knee Surg Sports Traumatol Arthrosc 21(10): 2405-2411.
- Parmelee PA, Tighe CA, Dautovich ND (2014) Sleep disturbance in osteoarthritis: linkages with pain, disability and depressive symptoms. Arthritis Care Res 67(3): 358-365.
- Parmelee PA, Harralson TL, McPherron JA, Schumacher HR (2013) The structure of affective symptomatology in older adults with osteoarthritis. Int J Geriatr Psychiatry 28(4): 393-401.
- Zullig LL, Bosworth HB, Jeffreys AS, Corsino L, Coffman CJ, et al. (2015) The association of comorbid conditions with patient-reported outcomes in Veterans with hip and knee osteoarthritis. Clin Rheumatol 34(8): 1435-1441.
- Valdes AM, Doherty SA, Zhang W, Muir KR, Maciewicz RA, et al. (2012) Inverse relationship between preoperative radiographic severity and postoperative pain in patients with osteoarthritis who have undergone total joint arthroplasty. Semin Arthritis Rheum 41(4): 568-575.
- Riddle DL, Kong X, Fitzgerald GK (2011) Psychological health impact on 2-year changes in pain and function in persons with knee pain: data from the Osteoarthritis Initiative. Osteoarthritis Cartilage 19(9): 10951101.
- Lindberg MF, Miaskowski C, Rusteon T, Rosseland LA, Cooper BA, et al. (2016) Factors that can predict pain with walking: 12 months after total knee arthroplasty. A trajectory analysis of 202 patients. Acta Orthop 87(6): 600-606.
- Rathburn AM, Yau MS, Shardell M, Stuart EA, Hochberg MC (2017) Depressive symptoms and structural disease progression in osteoarthritis: data from the Osteoarthritis Initiative. Clin Rheumatol 36(1): 155-163.
- Wylde V, Hewlett S, Learmonth ID, Dieppe P (2011) Persistent pain after joint replacement: prevalence, sensory qualities, and postoperative determinants. Pain 152(3): 566-572.
- Bierke S, Haner M, Petersen W (2016) Influence of somatization and depressive symptoms on the course of pain within the first year after uncomplicated total knee replacement: a prospective study. Int Orthop 40(7): 1353-1360.
- Salaffi F, Cavaliera F, Nolli M, Ferracciolo G (1991) Analysis of disability in knee osteoarthritis: relationship with age and psychological variables but not with radiographic score. J Rheumatol 18(10): 15811586.
- Smith BW, Zautra AJ (2008) The effects of anxiety and depression on weekly pain in women with arthritis. Pain 138(2): 354-361.
- Sinikallio SH, Helminen EE, Valjakka AL, Vaisanen-Rouvali RH, Arokoski JP (2014) Multiple psychological factors are associated with poorer functioning in a sample of community-dwelling knee osteoarthritis patients. J Clin Rheumatol 20(5): 261-267.
- Somers TJ, Keefe FJ, Godiwala N, Hoyler GH (2009) Psychosocial factors and the pain experience of osteoarthritis patients: new findings and new directions. Curr Opin Rheumatol 21(5): 501-506.
- Torres-Claramunt R, Hinarejos P, Arnestoy J, Leal J, Sanchez-Soler J, et al. (2017) Depressed patients feel more pain in the short term after total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc doi: 10.1007/s00167-016-4418-1.
- Zautra AJ, Smith BW (2001) Depression and reactivity to stress in older women with rheumatoid arthritis and osteoarthritis. Psychosom Med 63: 687-696.
- Dekker J, Boot B, van der Woude LHV, Bijlsma JWJ (1992) Pain and disability in osteoarthritis patients: a review of biobehavioral mechanism. J Behav Med15(2): 189-214.
- Schiphof D, Krkhof HJ, demen J, de Klerk BM, Hofman A, et al. (2013) Factors for pain in patients with different grades of knee osteoarthritis. Arthritis Care Res (Hoboken) 65(5): 695-702.
- Pereira D, Severo M, Barros H, Branco J, Santos RA, et al. (2013) The effect of depressive symptoms on the association between radiographic osteoarthritis and knee pain: a cross-sectional study. BMC Musculoskelet Disord 14: 214.
- Edwards RR, Cahalan C, Mensing G, Smith M, Haythornthwaite JA (2011) Pain, catastrophizing, and depression in the rheumatic diseases. Nat Rev Rheumatol 7(4): 216-224.
- Aflaki E, Parang A, Ghanizadeh A (2010) Depression in patients with hand and knee osteoarthritis. Int J Rheum Dis 113(Suppl 1): 163.
- Smith BW, Zautra AJ. The effects of anxiety and depression on weekly pain in women with arthritis. Pain 138(2): 354-361.
- van Baar ME, Dekker J, Lemmens JA, Oostendorp RA, Bijlsma JW (1998) Pain and disability in patients with osteoarthritis of hip or knee: the relationship with articular, kinesiological, and psychological characteristics. J Rheumatol 25(1): 125-133.
- Okma-Keulen P, Hopman-Rock M (2001) The onset of generalized osteoarthritis in older women: a qualitative approach. Arthritis Care Res 45(2): 183-190.
- Rathburn AM, Stuart EA, Shardell M, Yau M, Baumgarten M, et al. (2017) Dynamic effects of depressive symptoms on knee osteoarthritis pain. Arthritis Care Res doi: 10.1002/acr.23239.
- Ahn H, Weaver m, Lyon D, Choi E, Fillingim RB (2017) Depression and pain in asian Americans and Whites with knee osteoarthritis, J Pain S1526-5900(17): 30613-30622.
- Jung JH, Seok J-H, Song GG, Choi SJ (2017) Association between osteoarthritis and mental health in a Korean population: a nationwide study. Int J Rheum Dis doi: 10.1111/1756-185X.13098.
- Lin EH, Katon W, Von Korff M, Tang L, Williams JW Jr, et al. (2003) Effect of improving depression care on pain and functional outcomes among older adults with arthritis: a randomized controlled trial. JAMA 290(18): 2428-2429.
- Wenham CYJ, Conaghan PG (2010) Optimising pain control in osteoarthritis. Practitioner 254(1735): 23-26.
- Leite AA, Costa AJ, de Lima, BDAM, Padila A, et al. (2011) Comorbidities in patients with osteoarthritis: frequency and impact on pain and function. Rev Bras Rheumatol 51(2): 113-123.
- Veenhof C, Huisman PA, Barten JA, Takken T, Pisters MF (2012) Factors associated with physical activity in patients with osteoarthritis of the hip or knee: a systematic review. Osteoarthritis Cartilage 20(1): 6-12.
- Giraudet-Le Quintrec JS, Coste J, Vastel L, Pacualt V, Jeanne L, et al. Positive effect of patient education for hip surgery: a randomized trial. Clin Orthop Rel Res 414: 112-120.
- Rosemann T, Kuehlein T, Laux G, Scecsenyi J (2008) Factors associated with physical activity of patients with osteoarthritis of the lower limb. J Eval Clin Pract 14(12): 288-293.
- Maisaik R (1990) Arthritis and risk of depression: an epidemiological case control study. Arthritis Care Res 3: C36
- Creamer P, Lethbridge-Cejku M, Hochberg MC (2000) Factors associated with functional impairment in symptomatic knee osteoarthritis. Rheumatol 39(5): 490-496.
- Scopaz KA, Piva SR, Wisniewski S, Fitzgerald GK (2009) Relationships of fear, anxiety, and depression with physical function in patients with knee osteoarthritis. Arch Phys Med Rehabil 90(11): 1866-1873.
- Maly MR, Costigan PA, Olney SJ (2005) Contribution of psychosocial and mechanical variables to physical performance measures in knee osteoarthritis. Phys Ther 85(12): 1318-1328.
- Dieppe P, Cushnaghan J, Tucker M, Browning S, Shepstone L (2000) The Bristol 'OA500 study': progression and impact of the disease after 8 years. Osteoarthritis Cart 8(2): 63-68.
- Colbert CJ, Song J, Dunlop D, Chmiel JS, Hayes KW, et al. (2011) Knee confidence as it relates to physical function outcome in persons with or at higher risk for knee osteoarthritis in the osteoarthritis initiative. Arthritis Rheum 64(5): 1437-1446.
- Rosemann T, Backenstrass M, Joest K, Rosemann A, Szecsenyi J, et al. (2007) Predictors of depression in a sample of 1,021 primary care patients with osteoarthritis. Arthritis Rheum 57(3): 415-422.
- Agarwal P, Pan X, Sambamoorthi U (2013) Depression treatment patterns among individuals with osteoarthritis: a cross sectional study BMC Psychiatr 13(1): 121.
- Possley D, Rudiman-Mak E, O'Connell S, Jelinek C, Collins EG (2009) Relationship between depression and functional measures in overweight and obese persons with knee osteoarthritis of the knee. J Rehabil Res Dev 46: 1091-1098.
- Jinks C, Jordan KP, Blagojevic M, Croft P (2008) Predictors of onset and progression of knee pain in adults living in the community. A prospective study. Rheumatol 47(3): 368-374.
- Schwartz FH, Lange J (2017) Factors that affect outcome following total joint arthroplasty: a review of the recent literature. Curr Rev Musculoskelet Med.
- Sale JE, Gignac M, Hawker G (2008) The relationship between disease symptoms, life events, coping and treatment, and depression among older adults with osteoarthritis. J Rheumatol 35(2): 335-342.
- Bookwala J, Harralson TL, Parmalee PA (2003) Effect of pain and functioning and well-being in older adults with osteoarthritis of the knee. Psychol Aging 18(4): 844-850.
- Marks R (2009) Comorbid depression and anxiety impact hip osteoarthritis disability. Disabil & Hlth 2(1): 27-35.
- Peters TJ, Sanders C, Dieppe P, Donovan J (2005) Factors associated with change in pain and disability over time: a community-based prospective observational study of hip and knee osteoarthritis. Br J Gen Pract 55(512): 205-211.
- De Rooij M, Steultjens M, Dekker J (2013) Restrictions and contraindications for exercise therapy in patients with hip and knee osteoarthritis and comorbidity. Phys Ther Rev 18: 101-111.
- Rosemann T, Laux G, Szecsenyi J (2007) Osteoarthritis: quality of life, comorbidities, medication and health service utilization assessed in a large sample of primary care patients. J Orthop Surg Res 2: 12.
- Jinks C, Jordan KP, Blagojevic M, Croft P (2008) Predictors of onset and progression of knee pain in adults living in the community. A prospective study. Rheumatol 47(3): 368-374.
- Bookwala J, Harralson TL, Parmalee PA (2003) Effect of pain and functioning and well-being in older adults with osteoarthritis of the knee. Psychol Aging 18(4): 844-850.
- Wise BL, Niu J, Zhang Y, Wang N, Jordan JM, Choy E, Hunter DJ (2010) Psychological factors and their relation to osteoarthritis pain. Osteoarthritis Cartilage 18(7): 883-887.
- Marks R (2008) Impact of age, gender, disease, and health status on physical and psychological correlates of knee osteoarthritis disability. Open Longevity Sci 2: 49-57.
- Veronese N, Stubbs B, Solmi M, Smith TO, Noale M, et al. (2016) Association between lower limb osteoarthritis and incidence of depressive symptoms: data from the osteoarthritis initiative. Age Ageing.
- Kim KW, Han JW, Cho HJ, Chang CB, Park JH, et al. (2011) Association between comorbid depression and osteoarthritis symptom severity in patients with knee osteoarthritis. J Bone Joint Surg Am 93(6): 556-563.
- Scott KM, Von Korff M, Alonso J, Angermeyer MC, Bromet E, et al. (2009) Mental-physical co -morbidity and its relationship with disability: results from the World Mental Health Surveys. Psychol Med 39: 33-43.
- Marks R (2010) Gender differences in hip osteoarthritis. Health 2: 696-704.
- Helminen EE, Sinikallio SH, Valjakka AL, Vaisanen-Rouvali RH, Arokoski JP (2016) Determinants of pain and functioning in knee osteoarthritis: a one-year prospective study. Clin Rehabil 30(9): 890900.?
- Vaughan MW, LaValley MP, Felson DT, Orsmond GI, Niu J, et al. (2017) Affect and incident participation restriction in adults with knee osteoarthritis: the MOST study. Arthritis Care Res doi: 10.1002/ acr.23308.
- Singh JA, Lewallen DG (2013) Medical and psychological comorbidity predicts poor pain outcomes after total knee arthroplasty. Rheumatol 52(5): 916-923.
- Nur H, Sertkaya BS, Tuncer T (2017) Determinants of physical functioning in women with knee osteoarthritis. Aging Clin Exp Res.
- Schwartz FH, Lange J (2017) Factors that affect outcome following total joint arthroplasty: a review of the recent literature. Curr Rev Musculoskelet Med.
- Knoop J, van der Leeden M, Thorstensson CA, Roorda LD, Lems WF, et al. (2011) Identification of phenotypes with different clinical outcomes in knee osteoarthritis: data from the Osteoarthritis Initiative. Arthritis Care Res 63(11): 1535-1542.
- Ozcetin A, Ataoglu S, Kocer E, Yazici S, Yildiz O, et al. (2007) Effects of depression and anxiety on quality of life of patients with rheumatoid arthritis, knee osteoarthritis and fibromyalgia syndrome. West Indian Med J 56(2): 122-129.
- De Vellis B (1993) Depression in rheumatogical diseases. Ballieres Clin Rheumatol 7: 241-257.
- Margaretten ME, Katz P, Schmajuk G, Yelin E (2013) Missed opportunities for depression screening in patients with arthritis in the United States. J Gen Intern Med 28(12): 1637-1642.
- Paker, Bugdayci D, Dere D (2011) Determinants of quality of life in women with symptomatic knee osteoarthritis: the role of functional and emotional states. Turkish J Geriatr 14: 14-18.
- Ozcakir S, Raif SL, Sivrioglu K, Kucukcakir N (2011) Relationship between radiological severity and clinical and psychological factors in knee osteoarthritis. Clin Rheumatol 30(12): 1521-1526.
- Sullivan M, Tanzer M, Stanish W, Fallaha M, Keefe FJ, et al. (2009) Psychological determinants of problematic outcomes following total knee arthroplasty. Pain 143(1-2): 123-129.






























