Irrational Use of Three Antibiotics in Khartoum, Sudan: A Cross-Sectional Study
Azhari Elnour Haj Elamin 1,2*, Habab A Mohamed Saleh3, Walaa Saadeldin3, Eman Abualgasim3, Lina Ali3 and Emad M Abdallah4
1Department of Clinical Pharmacy and Pharmacy Practice - Karary University,Sudan.
2Khartoum University and Military Hospital, Sudan
3Department of Clinical Pharmacy, Faculty of pharmacy, Alneelain University, Khartoum, Sudan
4Department of Science Laboratories, College of Science and Arts, Qassim University, Ar Rass, 51921 Saudi Arabia
Submission: January 3, 2021; Published: January 18, 2022
*Corresponding author: Azhari Elnour H Elamin, Department of Clinical Pharmacy and Pharmacy Practice - Karary University, Sudan
How to cite this article: Walaa S, Eman A, Lina A, Azhari E H E, Emad M A. Irrational Use of Three Antibiotics in Khartoum, Sudan: A Cross-Sectional Study. Nov Appro Drug Des Dev. 2022; 6(2): 555685. DOI: 10.19080/NAPDD.2022.06.555685
Abstract
Antibiotic resistance may develop in a wide variety of pathogens as a result of irrational usage. This study aimed to investigate the irrational use of three antibiotics (oral macrolides, third generation cephalosporin injection, and amoxiclav) in Khartoum hospitals and its consequences. A cross-sectional cohort study in Khartoum hospitals over an 8-month period was conducted on a sample size of 300 patients who were undergoing antibiotic treatment by either oral macrolides, third generation cephalosporin injection, or amoxiclav. These patients completed the questionnaire, and the results were then gathered and analyzed using SPSS program. Results showed that the majority of patients (39%) used macrolide (azithromycin) in treatment and 23% used co-amoxiclav. When the same symptoms recurred, 56% of respondents re-used the same antibiotic without a prescription. The most common reasons for hospitalization were gastrointestinal tract infections and upper respiratory tract infections.
In conclusion, this study’s results indicate that antibiotic usage in some Khartoum state hospitals is often not based on acceptable therapeutic principles. Inadequate awareness about antibiotic usage contributes significantly to irrational antibiotic use.
Keywords: Antibiotics; Macrolides; Cephalosporin; Amoxiclav; Infections; Sudan
Introduction
Antibiotics are truly miracles of modern medicine, having been discovered around the turn of the twentieth century. Penicillin was the first drug discovered for the treatment of tuberculosis, and its development included the first use of clinical trials. The first compound with antimicrobial activity was introduced in 1911 by Erlich, who focused his research on the discovery of a “magic bullet” to treat syphilis [1]. Physicians and scientists were so ecstatic with their early success in combating infections that the US Surgeon General declared in 1970 that the battle against pestilence had been won [2]. Unfortunately, time has proved that they were overoptimistic. Nobody could anticipate the wide variety of mechanisms the bacteria use to evolve, especially their amazing ability of interchanging genes and this unexpected capacity of microorganisms is the reason why, in spite of the success of antibiotics in curing a considerable number of infectious diseases, the emergence of multidrug-resistant bacteria is currently a major worldwide concern, because it is the major cause of treatment failure against many pathogens [3].
Resistance in bacteria is often induced by self-medication, genetic variances, or mutations in bacteria, as well as phenotypic variation involving beta-lactams. Because antibiotics are target- specific, bacteria release enzymes that break chemical bonds within the antibiotic structure. Additionally, changes in membrane permeability, antibiotic target modification in bacteria, and resistant gene transmission to subsequent generations all contribute to antibiotic resistance, and as a result, bacteria have developed resistance and are now capable of causing devastating infections in humans [4]. Moreover, while there is a rising demand for novel antibiotics, there is a large and ongoing cost barrier to their development. The issue derives from the widely held belief that a “market” is required to stimulate commercial antibiotic research [5].
A more comprehensive approach for improved antibiotic usage is critical for sustaining the medicines’ substantial value. There is a definite need to advance scientific knowledge of the variables related with antibiotic usage in particular. Historically, the majority of attempts to regulate antibiotic usage have been focused at prescribers: recommendations, national and international antibiotic regulations, and instructional initiatives. However, since little is known about the extent to which patients contribute to antibiotic usage, no solid approach for public education has been created [6]. Therefore, the aim of the present study was to investigate the irrational usage of three antibiotics (oral macrolides, third generation cephalosporin, and amoxiclav) in Khartoum hospitals amongst patients.
Methodology
Study design
A descriptive cross-sectional survey was used in this study to confirm and/or refute assumptions of the attitude of the patients treated at Khartoum hospitals with three different types of antibiotics and to evaluate the results in order to comprehend and resolve the study’s issue using a well-designed questionnaire.
Study area
The investigation was carried in three emergency clinics in Khartoum, Sudan’s capital: the Military hospital, the Khartoum teaching hospital, and the Royal care hospital.
Study duration
Between July 2018 and February 2019, the following surveys were conducted to collect data using a questionnaire:
(i) During the first two months, data collected amounted for 25% of the total sample size;
(ii) Within the next two months, the remaining 25% (total 50%);
(iii) Within the next two months, the remaining 25% (total 75 %); and
(iv) The remaining data was obtained throughout the preceding two months (total 100 %).
Data collection
Prior to conducting a survey, the sample size was determined to be 300. The questionnaire was anonymous, and the age group examined spanned from 18 to above. It has twelve questions, eleven of which are closed-ended and one of which is openended. The questionnaire elicited information on the antibiotics prescribed to patients under treatment guidelines. The disease or condition that needs hospitalization. Antibiotic therapy duration. Adherence to getting medications on time. The patient’s conduct when he or she misses a dosage and complains of the same symptoms after antibiotic use. When a patient discontinues the use of an antibiotic recommended by a physician and experiences relief from their symptoms. If the medicine did not work or did not cure the infection, the patient’s interpretation.
Ethical approval statement
The study was performed in a cross-sectional approach. The protocol for the research was approved by the ethics committee of the Faculty of Pharmacy, Alneelain University, Khartoum, Sudan, in line with the Helsinki Declaration for the conduct of human experimentation. After obtaining a comprehensive verbal overview of the procedure, each participant signed an informed consent form.
Statistical analysis
SPSS was used to analyze, classify, and analyze data. Tables and figures were used to display the descriptive statistics and the outcomes. The chi-square test is used to compare and correlate variables.
Results and Discussion
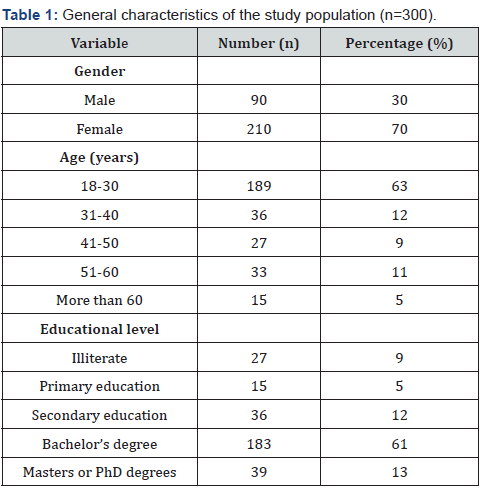
This cross-sectional research aimed to determine the current situation of irrational antibiotic usage and its repercussions in Khartoum state. It included 300 patients; the general characteristics of the study population are shown in (Table 1), The majority of patients (70%) were females, their ages varied between 18 and 30, and most of them had education level of bachelor’s degree (61%). Association between education level amongst youth age and the use antibiotic at specific time was significant (P-value <0.05).
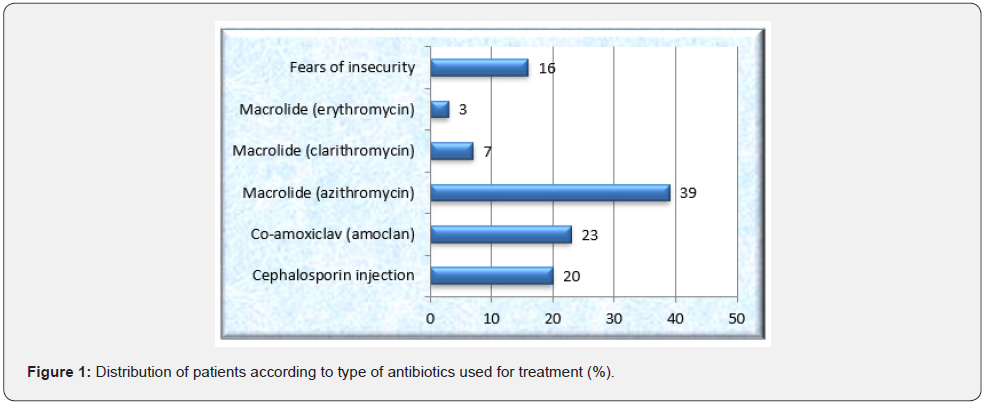
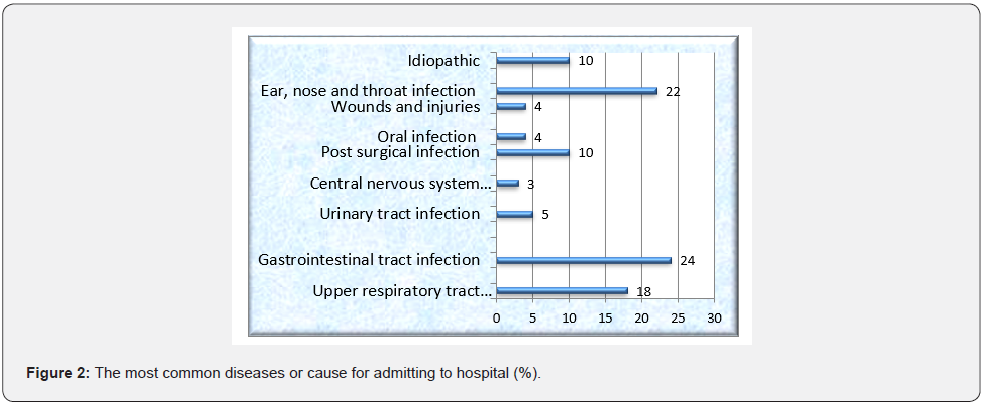
As seen in (Figure 1), the majority of patients (39%) had previously taken Azithromycin. Whereas the most often seen illnesses or reasons for hospitalization were gastrointestinal tract infections (24%); ear, nose, and throat infections (22%); and upper respiratory tract infections (18%), respectively (Figure 2).
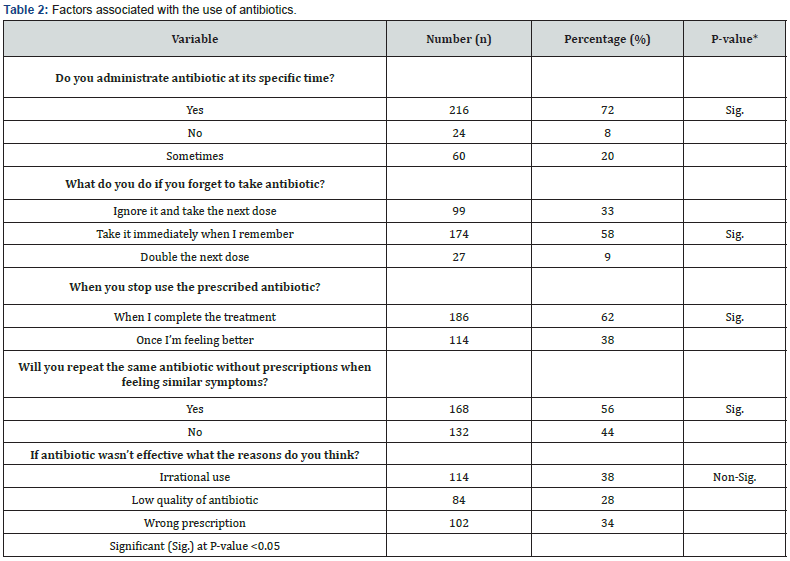
The factors behind the irrational use of antibiotics in certain Khartoum hospitals are outlined in Table 2. 72 percent of patients administer antibiotics at the prescribed time, while 58 percent of patients who forget to take antibiotics do so soon upon recall. Interestingly, 56% of patients repeat the same antibiotic without a prescription when they have identical symptoms, which is the most irrational usage and may result in serious medical consequences. According to the questionnaire responses, patients are unaware of the specific cause for antibiotic inefficiency. 38% believe it is due to irrational usage, 34% believe it is due to incorrect prescription, and 28% believe it is due to low quality of antibiotic. According to the majority of patients, irrational usage was the primary cause for treatment failure. The chi-square correlation test revealed that depending on the p-value = 0.000 (P-value <0.05). Additionally, statistical research revealed substantial connections between irrational antibiotic usage and confounding variables (gender, age, education level, etc.). Therefore, in the studied Khartoum hospitals, antibiotics were used irrationally.
In general, published reports about the irrational use of antibiotics in Sudan are scant. All of the data demonstrated that the primary reasons of antibiotic resistance in Sudan are multifaceted, since they were given from a variety of perspectives. The inappropriate use of antibiotics by doctors, pharmacists, and the general public complicates the matter. Additionally, lack of public knowledge is a well-recognized factor contributing significantly to the spread of drug-resistant pathogens and irrational use of antibiotics in Sudan [7]. Respiratory infections in Sudan recorded a high level of resistance to antibiotics and this is attributed to the irrational use of antibiotics [8]. Adult self-medication with antibiotics is extremely widespread in our country (Sudan). On the one hand, medical stores sell antibiotics without a prescription, while on the other side, physicians prescribe antibiotics with inadequate follow-up or awareness, this This issue is particularly acute in developing countries as it was reported extensively in many developing countries, like Pakistan [9], India [10], Nigeria [11], Egypt [12], and many countries in African, Latin American and south-eastern Europe regions [13]. Among the general public, major factors contributing to antibiotic resistance are a lack of knowledge and awareness, access to antibiotics without a prescription and leftover antibiotics, and the knowledge, attitude, and perception of prescribers and dispensers. Among healthcare providers, major factors contributing to antibiotic resistance include insufficient medical training, pharmaceutical promotion, a lack of rapid and sufficient diagnostic tests, and patient– doctor interaction [14]. Global and regional guidelines currently call for the establishment of a government structure devoted to monitoring and improving the use of antibiotics, as well as the conduct of a national situation analysis in order to design a roadmap for action. The WHO Regional Office for South-East Asia is currently conducting national situational studies upon request from countries in order to assist them in developing coordinated action plans [15]. We hope that the same is implemented expeditiously in Sudan, and that Sudanese health authorities pay more attention to the rising phenomena of antibiotic-resistant infections and irrational antibiotic use.
Limitation
We did not conduct a cohort study and follow-up; the sample size was small and certain patients were uncooperative.
Conclusion
The questionnaire findings revealed that antibiotic usage in some Khartoum state hospitals is often not based on solid therapeutic principles. Certain patients did not recover after treatment with the three kinds of antibiotics studied in this study, due to patient discomfort, side effects, or ineffectiveness. Furthermore, the majority of patients self-administer the same antibiotic after experiencing a comparable illness. Antibiotic misuse is quite widespread in this population. Antibiotics are most often used without a prescription. Insufficient information about antibiotic usage contributes significantly to irrational antibiotic use. Low education was substantially connected with irrational antibiotic usage. There is a need to evaluate antibiotic accessibility in local retail pharmacies.
References
- Zaffiri L, J Gardner, LH Toledo-Pereyra (2012) History of antibiotics. From salvarsan to cephalosporins. Journal of Investigative Surgery 25(2): 67-77.
- Anker MS, W H Organization (2001) WHO report on global surveillance of epidemic-prone infectious diseases.
- Couce A, J Blazquez (2009) Side effects of antibiotics on genetic variability. FEMS microbiology reviews 33(3): 531-538.
- Naveed M (2020) Antibiotics resistance mechanism, in Antibiotics and Antimicrobial Resistance Genes in the Environment. pp. 292-312.
- Klug DM, Idiris FIM, Mark AT, Frank VD, Dowson CG, et al. (2021) There is no market for new antibiotics: this allows an open approach to research and development. Wellcome Open Research 6(146): 146.
- Pechere JC (2001) Patients' interviews and misuse of antibiotics. Clinical infectious diseases 33(Supplement_3): S170-S173.
- Abdulgader NEA, Galil RKA, Tagwa MAO, Shahd YMNS, Sahar GE, et al. (2021) Irrational use of antibiotics with representation of antimicrobial resistance patterns in Sudan: a narrative review: 43-47.
- Ahmed SMA-Z (2018) Etiological trends and patterns of antimicrobial resistance in respiratory infections. The Open Microbiology Journal 12: 34.
- Hameed A (2016) Irrational use of antibiotics. Different Age Groups of Karachi: a wakeup calls for antibiotic resistance and future infections. J Bioequiv Availab 8: 242-245.
- Kotwani, A, C Wattal, PC Jhoshi, K Holloway (2012) Irrational use of antibiotics and role of the pharmacist: an insight from a qualitative study in New Delhi, India. Journal of clinical pharmacy and therapeutics 37(3): 308-312.
- Akinyandenu O, A Akinyandenu (2014) Irrational use and non-prescription sale of antibiotics in Nigeria, a need for change. J Sci Innov Res 3(2): 251-7.
- Maraghy DAE, AM Younis, N Abbas (2016) Survey on the irrational use of antibiotics among adults in Egyptian community. Int J Pharmacol Pharm Sci 3: 6-9.
- Bbosa GS (2014) Effects of intervention measures on irrational antibiotics/antibacterial drug use in developing countries.
- Machowska A, C Stålsby Lundborg (2019) Drivers of irrational use of antibiotics in Europe. International journal of environmental research and public health 16(1): 27.
- Holloway KA (2011) Promoting the rational use of antibiotics. in Regional Health Forum.






























