Assessment of Patient Empowerment in Type 2 Diabetic Patients in Turkey
Murat Yildiz and Ersin Akpinar*
Cukurova University Family Medicine Department, Adana-Turkey
Submission:January 14, 2021;Published: February 22, 2021
*Corresponding author: Ersin Akpinar, Cukurova University Family Medicine Department, Adana-Turkey
How to cite this article: Murat Y, Ersin A. Assessment of Patient Empowerment in Type 2 Diabetic Patients in Turkey. Nov Appro Drug Des Dev. 2021; 5(5): 555671. DOI: 10.19080/NAPDD.2021.05.555671
Abstract
Aim: Empowering patients means providing them with the opportunities and the environment to develop the skills, confidence and knowledge to move from being a passive recipient of care to an active partner in their health care. Patient empowerment is gaining greater international importance in healthcare, but uncertainty remains about the best way to define and measure it. The purpose of the study was to assess the factors influencing patient empowerment in patients with type 2 diabetes.
Material and Method: The participants of the study were 125 diabetic patients in Çukurova University Outpatient Clinic. A sociodemographic questionnaire and the Diabetes Empowerment Scale (DES) were used. Adherence to medications, diet, and exercise and the numbers of diabetes consultations were asked. Statistical analysis was used to determine any relationship with the above-mentioned variables to the DES ratings.
Results: The mean age was 55,1±9,7 years (range=25-77). Of the patients, 24,8% were male, 81,6% were married, and 93,6% had education level of diploma and higher. The mean duration of diabetes was 9,56±7,98 years. Diabetes Empowerment Scale has three conceptual domains of ‘Managing the psychosocial aspect of diabetes’, ‘Assessing dissatisfaction and readiness to change’ and ‘Setting and achieving diabetes goal’. The mean score of each domain was 23,6±3,8, 24,4±3,7, and 34,4±6,1, respectively. It was found that age, gender, marital, educational, work, and socioeconomic status, dietary status, state of being educated about the illness, psychological support received, level of knowledge about the illness, and length of time after diagnosis have influence on the illness perception in diabetes. Partial correlation analyses failed to show any statistically significant relationship between patient empowerment and glycemic control or other diabetes management variables (HbA1c, p=0,229; HDL, p=0,492; LDL, p=0,977; TC, p=0,873; triglycerides, p=0,893). Logistic regression analysis confirmed that patient empowerment score was not a significant predictor of glycemic control. The mean total empowerment score was 82,4 (SD=11,4) indicating a moderate-to-high level of self-management in diabetes.
Conclusion: Combining family medicine-based approaches with culturally competent diabetes care may improve knowledge, attitudes, perceptions and self-care practices of and collaborative care for people with diabetes. Empowering the patients encourages interaction of communities, health care professionals, policy makers and all other civil society actors with respect to health and well-being of individuals. Patient empowerment programs have been shown to improve mental health, doctor-patient communication, healthy eating, and patient self-efficacy, although the capacity of existing outcome measures to capture the patient benefits of these programs has been questioned.
Keywords: Patient empowerment; Type 2 diabetes; Primary care; Family medicine
Abbreviations: DES: Diabetes Empowerment Scale; WHO: World Health Organization; IDF: International Diabetes Federation; DM: Diabetes Mellitus
Introduction
Empowerment of the patient is defined as a process that will assist the patient in learning and developing the individual capacity that he / she has in charge of his / her own life [1].
The World Health Organization (WHO) defined the concept of empowerment in 1998 as the process of gaining greater control over decisions and actions that affect people’s own health [2]. The International Diabetes Federation (IDF) defines the process in which patients learn to cope and manage their illness as “empowering” [3].
Diabetes mellitus (DM) is a major public health problem, affecting people of all ages worldwide. It is resulting in increased mortality, morbidity and important reduction in quality of life especially in industrialised countries where risk factors such as obesity and unhealthy eating habits are more common [4]. The International Diabetes Federation (IDF) estimated there were 451 m people with DM worldwide in 2017 and that number will increase to 693 m by 2045 [5].
Different methods have been developed for the management of chronic diseases such as diabetes. One of these models is the “patient-centered approach”. The patient-centered approach is one of the basic competencies of family medicine [6]. Family physicians provide comprehensive and continuous care to every individual seeking medical care, regardless of age, gender and illness. They evaluate the physical, spiritual, social, cultural and existential factors together by using the knowledge and trust generated by repeated contact while discussing the management of their illnesses with their patients.
Material and Methods
125 patients who were admitted to the Çukurova University Polyclinics who were diagnosed with diabetes for at least six months and signed the informed consent form were included in the study. The questionnaires used in the study were administered through face-to-face interviews.
Inclusion criteria of the patients are as follows:
• Having Type 2 Diabetes Mellitus,
• Being over 18 years old,
• DM having been diagnosed for at least six months,
• Not having sight-hearing problems and being able to communicate verbally,
• Not being diagnosed with depression and / or not currently receiving treatment for depression.
Procedures
Patients with type 2 diabetes included in our study were examined for fasting blood glucose, HbA1C, total cholesterol, HDL-cholesterol, LDL-cholesterol, triglyceride, urea, creatinine, and complete urine tests. The patient’s duration of diabetes, the medications used, diabetes education status, and the medications used for other chronic diseases, if any, were questioned. Diabetes Empowerment Scale (DES) was applied to the patients [7].
Evaluation of Data
A biostatistical digital program was used for the statistical analysis of the study. A p <0.05 was determined to be significant.
Results
The mean age was 55,1±9,7 years (range=25-77). Of the patients, 24,8% were male, 81,6% were married, and 93,6% had education level of diploma and higher. The mean duration of diabetes was 9,56±7,98 years. Diabetes Empowerment Scale has three conceptual domains of ‘Managing the psychosocial aspect of diabetes’, ‘Assessing dissatisfaction and readiness to change’ and ‘Setting and achieving diabetes goal’. The mean score of each domain was 23,6±3,8, 24,4±3,7, and 34,4±6,1, respectively. DES total score of the patients was calculated as 82,4 ± 11,4.
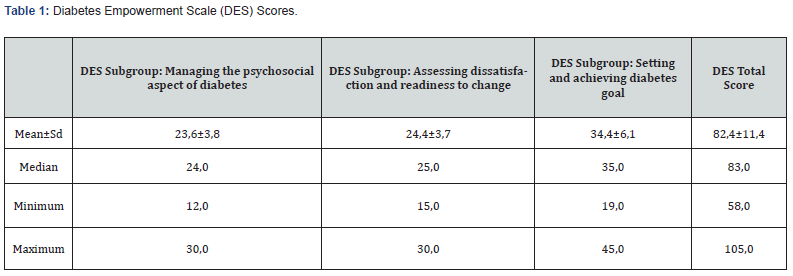
“How many points would you give when you think about your health in general?” and 85,6% of patients gave 5 points to their health. “How would you rate your regular use of your diabetes medication?” for the question, the average was found to be 8,7 ± 2,1 and 84% of the patients gave ≥7 points. “How do you adapt to your recommended diabetes diet?” and 81,6% of the patients gave a score of 5 for the question. “How is your sex life in your opinion?” and 27,4% of the patients stated that they did not have an active sexual life, 81,6% of them gave a score of ≥5 (Table 1).
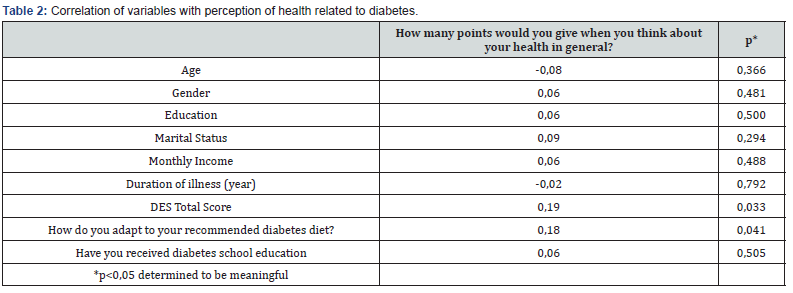
It was found that there was no correlation between age, gender, marital status, education level, employment status, socioeconomic status, dietary status, education about the disease, and the length of time passed after the diagnosis of diabetes (Table 2).
Partial correlation analyses failed to show any statistically significant relationship between patient empowerment and glycemic control or other diabetes management variables (HbA1c, p=0,229; HDL, p=0,492; LDL, p=0,977; TC, p=0,873; triglycerides, p=0,893). Logistic regression analysis confirmed that patient empowerment score was not a significant predictor of glycemic control. The mean total empowerment score was 82,4 (SD=11,4) indicating a moderate-to-high level of self-management in diabetes.
Discussion
When the education status of the patients is examined, it is seen that 56,8% of them have a primary education or less, and 6,4% are illiterate. Looking at the literature; In our country, there are studies supporting that the education level of people with diabetes is mostly primary school, literate and illiterate [7-11]. In the study of Chen et al., 25,6% of the patients living in China were secondary school graduates, and 73% were university graduates in the study of Anderson et al. [12, 13], our findings related to the education of the patients was consistent with the literature does not comply with international studies in Turkey. A statistically significant difference was found between the education level and the DES total scale score and the DES diabetes-related goals subgroup score. It was found that this difference was between the total DES scale score of the illiterate group and the DES diabetesrelated goals sub-group score. In a similar study conducted by Tol et al. with 688 type 2 diabetic patients published in 2013, the effect of diabetes-related factors on strengthening was investigated using the Diabetes Empowerment Scale (DES-28), and statistically significant increases in the mean scores of all DES subgroups as the education level increased. It has been stated that patients with type 2 diabetes with a high level of education have higher selfmanagement and self-empowerment abilities.
Conclusion
Strengthening was found to be low in patients with low education level. Education has been found to be an important parameter in diabetes management. It has been found that TYPE 2 diabetes patients have low compliance with medical nutrition therapy and do not exercise regularly. In our study, it was determined that most type 2 diabetes patients did not receive diabetes education. When DES scores were compared by gender, no statistically significant result was found. It has been found that glycemic control is insufficient in diabetic patients. The active role of family physicians in the care of diabetic patients and patient education can be increased and empowering patients can be supported.
Combining family medicine-based approaches with culturally competent diabetes care may improve knowledge, attitudes, perceptions and self-care practices of and collaborative care for people with diabetes. Empowering the patients encourages interaction of communities, health care professionals, policy makers and all other civil society actors with respect to health and well-being of individuals. Patient empowerment programs have been shown to improve mental health, doctor-patient communication, healthy eating, and patient self-efficacy, although the capacity of existing outcome measures to capture the patient benefits of these programs has been questioned.
References
- Funnell MM, Anderson RM, Arnold MS, Barr PA, Donnelly M, et al. (1991) Empowerment: An idea whose time has come in diabetes education. Diabetes Educ 17(1): 37-41.
- Kan E, Shiu A, Wong R (2006) Empowerment Approach to Diabetes Education Promises and Challenges. Hong Kong Society for Nursing Education.
- International Diabetes Federation. International Curr iculum for Diabetes Health Professional Education. http://www.idf.org/webdata/docs/Curriculum_Final20041108_EN.pdf, 2014.
- Zimmet P, Alberti KG, Magliano DJ, Bennett PH (2016) Diabetes mellitus statistics on prevalence and mortality: Facts and fallacies. Nat Rev Endocrinol 12(10): 616-622.
- International Diabetes Federation. Diabetes atlas-eighth edition 2017, https://www.diabetesatlas.org (Accessed 11 May 2020).
- Commission of the WONCA European Council. The European Definition of General Practice/Family Medicine Wonca Europe 2011 edition. Barcelona: The European Society of General Practice/ Family Medicine; 2011. http://www.woncaeurope.org.
- Uçan Ö, Ovayol N, Torun S (2007) Determination of Information on Blood Sugar Control and Insulin Use of Patients with Diabetes Mellitus. Atatürk University School of Nursing Journal 10(1): 89-96.
- Güneş Z, Körükçü Ö, Özdemir G (2009) Determination of Sleep Quality in Diabetic Patients. Journal of Atatürk University School of Nursing 12(2): 10-28.
- Türten T (2011) Determination of Psychosocial Adjustment to Disease in Individuals with Diabetes, Hacettepe University, Master's Thesis, Ankara.
- Ünsal E, Kızılcı S (2009) The Relationship Between the Knowledge Level of Individuals with Diabetes, Self-Care Ability and A1c Level. Dokuz Eylul University School of Nursing Electronic Journal 2(2): 16-26.
- Anderson RM, Fitzgerald JM, Funnell MM, Marrero DG (2000) The Diabetes Empowerment Scale, A measure of Psychosocial Self-Efficacy. Diabetes Care 23(6): 739-743.
- Chen MF, Wang RH, Cheng CP, ChinCC, Stocker J, Tang SM, Chen SW (2010) Diabetes Empowerment Process Scale: Development and Psychometric Testing of Chinese Version. Journal of Advanced Nursing 67(1): 204-214.
- Tol A, Baghbanian A, Mohebbi B, Shojaeizadeh D, Azam K, et al. (2013) Empowerment assessment and influential factors among patients with type 2 Journal of Diabetes & Metabolic Disorders 12(1): 6.






























