Strength Training Reduces Blood Pressure and Improves Lifestyle and Quality of Life Parameters in Hypertensive Woman
Nyasmin Medens Anéli, Mônica Dayane Lammers, Marcelo Decker, Gabriela Gonçalves de Oliveira, Sarah Franco Vieira de Oliveira Maciel and Andréia Machado Cardoso*
Medicine Course, Federal University of Fronteira Sul, Campus Chapeco, Brazil
Submission: April 12, 2018; Published: April 24, 2018
*Corresponding author: Andréia Machado Cardoso, Medicine Course, Federal University of Fronteira Sul, Campus Chapecó, Brazil, Tel: 49 20496507; Email: deiaa.mc@gmail.com
How to cite this article: Nyasmin M A, Monica D L, Marcelo D, Gabriela G d O, Sarah F V d O M , Andreia M C. Strength Training Reduces Blood Pressure and Improves Lifestyle and Quality of Life Parameters in Hypertensive Woman. J Phy Fit Treatment & Sports. 2018; 3(3): 555612. DOI: 10.19080/JPFMTS.2018.03.555612
Abstract
Systemic arterial hypertension is a disease intimated linked to lifestyle, and that impacts significantly in the quality of life of the patients. Strength training is currently recognized as an importante coajutant in hyptertension treatment. Thus, in this study we investigated the effect of strength training (ST) on blood pressure, life style and quality of life of hypertensive middle aged woman. Hypertensive group (n=16) and normotensive group (control group, n=11) were submitted to a six months of strength training, twice a week, at 60 to 70% of 1RM (one maximal repetition). Our results showed a significant decrease in blood pressure values in hypertensive group after 6 months of ST. Some lifestyle parameters (ingestion of fried food, sugar, depression, back pain) improved after the intervention. The participant's perception about their quality of life also improved in some parameters. In conclusion, ST acts as a great non-pharmacological treatment in hypertension, reducing blood pressure and improving lifestyle and quality of life of hypertensive population. Moreover, this study can act as an incentive for general population to adopt a healthier and more active lifestyle.
Keywords: Systemic Arterial Hypertension; Strength training; Blood pressure; Quality of life; Life style
Abbreviations: SAH: Systemic Arterial Hypertension; BP: Blood Pressure; ST: Strength Training; DASH: Dietary Approaches to Stop Hypertension; FS: Functioning of Sensory; AUT: Autonomy; PFA: Past, Present and Future Activities; SP: Social Participation; DD: Death and Dying; INT: Intimacy; SBP: Systolic Blood Pressure; DBP: Diastolic Blood Pressure; LBP: Low Back Pain; TMT: Trunk Muscle Training; QoL: Quality of Life
Introduction
Systemic Arterial Hypertension (SAH) is a chronic multifactorial non- transferable disease, characterized by high and sustained levels of blood pressure (BP). The disease is associated with functional and/or structural changes of the target organs (heart, brain, kidneys and blood vessels) as well as metabolic changes, with consequent increased risk of fatal and non-fatal cardiovascular events [1,2,3]. This pathology appears as one of the major public health problems, accounting for 13% of deaths worldwide, representing high costs for management in health [4,5]. In the last 40 years there was a decrease in the prevalence of SAH in developed countries and an increase in incidence, mainly in developing countries due to population growth and aging [5,6].
The emergence of SAH is closely related to both constitutional risk factors (age, gender, family history, race/color) and environmental (overweight/obesity, stress, alcoholism, smoking, sedentary lifestyle, use of contraceptives, Food rich in sodium and fat, diabetes) risk factor. Indeed, lifestyle, specially the sedentarism, currently has been touted as one of the main triggers of the disease [4]. This feature is related do the high prevalence of SAH as well as to the low control because pharmacological methods are insufficient when used isolated [3].
Taking this into account, non-pharmacological interventions for the treatment of SAH has emerging as very important coadjutant of the disease treatment. According to the DASH (Dietary Approaches to Stop Hypertension) guidelines, the adhesion of a healthy diet triggers a reduction in systolic blood pressure, reaching values around 11mmHg while reducing sodium intake and the practice of exercises of 90 to 150minutes per week the can cause the systolic blood pressure levels be reduced by around 5 to 8mmHg [7]. It has been many year that the regular practice of aerobic exercise is recommended as an adjunct in the treatment of HAS. However, strength training (ST), also known as weight training, has emerging as a hypertension treatment nowadays with promisor effects in reducing blood pressure. Indeed, muscle contractions during training tend to raise blood pressure more when compared with muscle movements during an aerobic exercise, both being conducted with similar intensities [8,9]. However, several studies have shown that the practice of ST is so beneficial in hypertension as aerobic exercise, and can even generate more significant changes [9]. Thus, herein we investigated the effect of resistance training on blood pressure, life style and quality of life of hypertensive middle aged woman.
Methodology
The sample of this study was constituted by twenty-seven (27) middle-aged woman, being predominantly Caucasian from different neighborhoods of the Chapeco/SC city. Participants were included in the study according to the following inclusion criteria: be resident at Chapeco-SC, aged between 50 e 60 years, sedentary, clinically diagnosed with systemic arterial hypertension or use only antihypertensive drugs for the hypertensive group. For the control group (normotensive group), participants should be normotensives without any disease and/ or medication routine. Were excluded from the study woman who practiced regularly exercise, smoke, or use any medication that alters the felt sense and physical kinetics. All volunteers underwent periodic evaluations with a cardiologist and did not present clinical contraindications to participate in the study
The participants were submitted to the application of two questionnaires: a survey about lifestyle/ life habits (EPIFLORIPA) [10] and a questionnaire about quality of life (WHOQOL-OLD) [11], before (pre-test) and after 6 months of strength training. The EPIFLORIPA questionnaire, adapted, contains questions about socioeconomic characteristics, lifestyle and general habits (ex. Food consumption) of the participants. The WHOQOL-OLD questionnaire contains questions about the functioning of Sensory (FS), autonomy (AUT), past, present and future Activities (PFA), Social participation (SP), Death and Dying (DD) and intimacy (INT), in addition to assess also the quality of life of General form. Blood pressure (BP) were measured before (pre test), after 3 months and after 6 months of exercise training program. A mercury column sphygmomanometer (Erkamater™ E300, Germany) was used for all BP measurements. The BP measurement procedures were performed according to the VII Brazilian Guidelines for Hypertension [12].
The subjects were divided into two groups, Group 1 (n=16), sedentary hypertensive woman that uses antihypertensive medication, subjected to strength training and Group 2 (n=11), sedentary and normotensive woman. Before the beginning of the ST, participants answered individually to both questionnaires, applied by students of the health area of UFFS instructed to such a process. After two groups were submitted, first, an adjustment period composed by 3 training sessions, in which individuals have performed an adaptation to the environment and to the proposed exercises motor gesture. It was subsequently applied to them the strength training protocol, in which the exercises were chosen in order to encompass the major muscle groups, being held alternately, 3 series for each exercise. Each series of 12 to 15 repetitions, with subjective perceived of effort controlled intensity of 11 to 13, according to Borg Scale [13]. The sequence of the program was composed of the following exercises: leg press, pulled low dorsal, knee extensor, flexor knee, triceps, biceps, hip adductor, calf. In addition to the realization of the ST, participants were instructed to stretch before and after the training sessions. The training program followed recommendations of ACSM (2007) and was done in partnership with the UNOCHAPECÓ institution, twice a week.
At the end of the exercise protocol, totalizing 6 months of activities, the participants answered again the quality of life and lifestyle questionnaires. Afterwards, participants' answers were computed in excel worksheets and grouped into tables for analysis. Data from the EPIFLORIPA questionnaire was analyzed by the simple percentage calculation of the participant response groups. The analysis of the WHOQOL - OLD questionnaire was performed according to its specific evaluation method, which is used to calculate the mean of the answers referring to the group of questions that represent the criteria evaluated. The data related to blood pressure measurements were analyzed using the two-way ANOVA test, considering p <0.05.
This research work was approved by the Research Ethics Committee of Federal University of Fronteira Sul (UFFS, Brazil), according to the Resolution 466/12 of the National Health Council on research involving human beings. All participants were informed about the procedures, risks and benefits of this research and signed the Informed Consent Term before the beginning of the project. Data collection was carried out by a team of academics and professors linked to the health courses from UFFS Campus Chapeco and UNOCHAPECÓ, Brazil.
Results
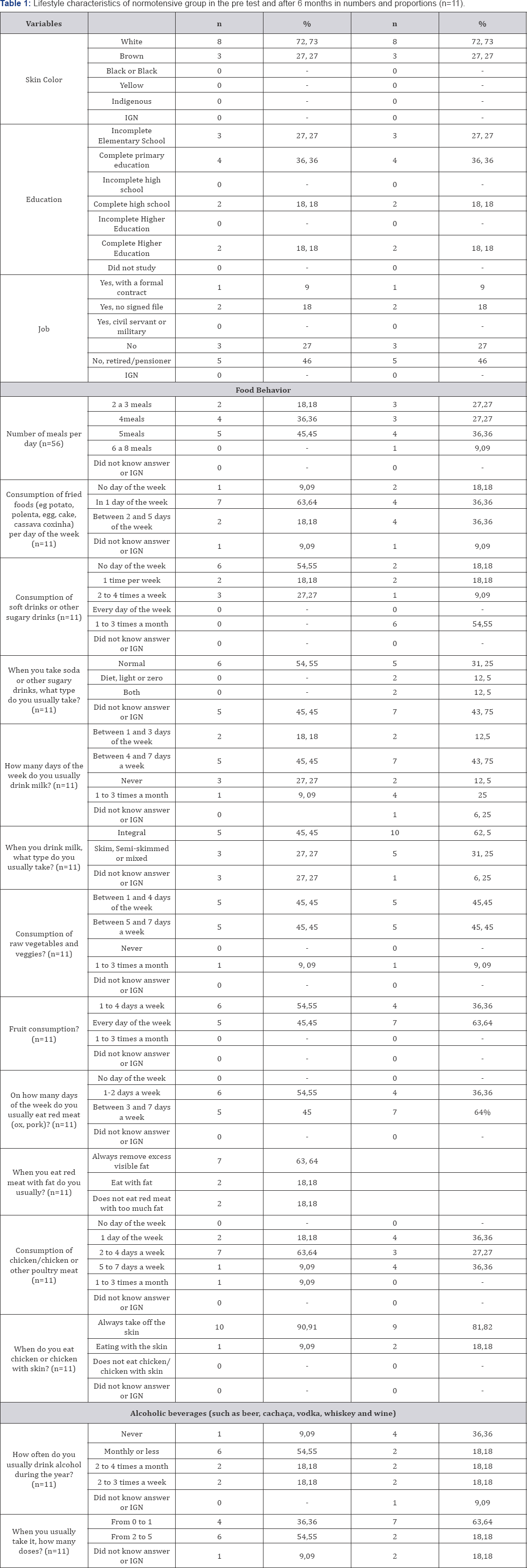
Subtitles: n: number of respondents.

Subtitles: n: number of respondents.

All data collected from the quality of life and lifestyle questionnaires are presented in Tables 1-3. The mean age of participants was 57±5 years for hypertensive group and 55±4 years for normotensive group. The most important results are presented in figures. Figure 1 shows the data referring to skin color and schooling. For skin color, the predominant was white, 87.50% of hypertensive and 72.73% of normotensive. Regarding schooling, 36.36% of the normotensive group had complete Elementary School, while in the hypertensive group the predominant schooling was incomplete Elementary School (37.50%) (Figure 1).
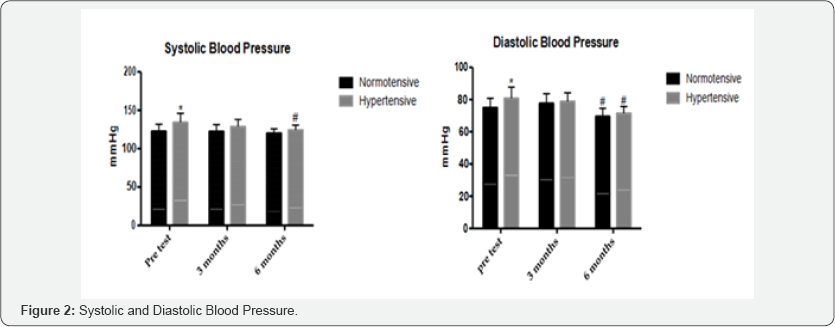
Figure 2 shows the data referring to blood pressure measurements. Blood pressure reduced significantly after 6 months of ST in the hypertensive group. Regarding to the values of systolic blood pressure (SBP) in the pre test, the normotensive group had a mean of 122.6±2.3mmHg, whereas the hypertensive group presented a mean of 134.1±2.1mmHg. In the measurement of SBP after 3 months of ST, the normotensive group presented a mean of 122.3±2.3mmHg, whereas the hypertensive group had a mean of 128.5±1.7mmHg. At the end of 6 months of ST, the group of normotensive patients presented a mean SBP of 120±1.5mmHg, while the group of hypertensive patients had a mean of 12±1.1mmHg. In the results of the diastolic blood pressure (DBP), the normotensive group had a mean of 74±1.5mmHg in the pretest, while the hypertensive group had a mean of 80.8±1.2mHg. After 3 months of ST, the group of normotensive patients had a mean PAD of 77.6±1.5mmHg, whereas the hypertensive group had a mean of 78.7±0.9mmHg. At the end of 6 months of ST the mean PAD of the normotensive group was 69.4±1.3mmHg, while in the hypertensive group the mean was 71.3±0.8mmHg.
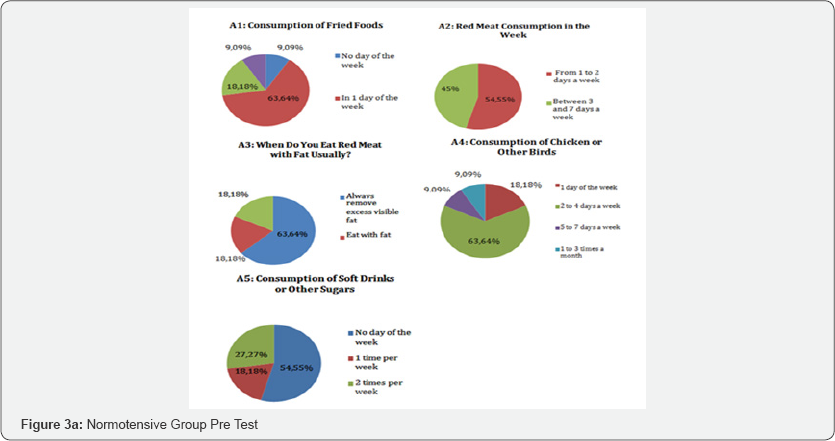
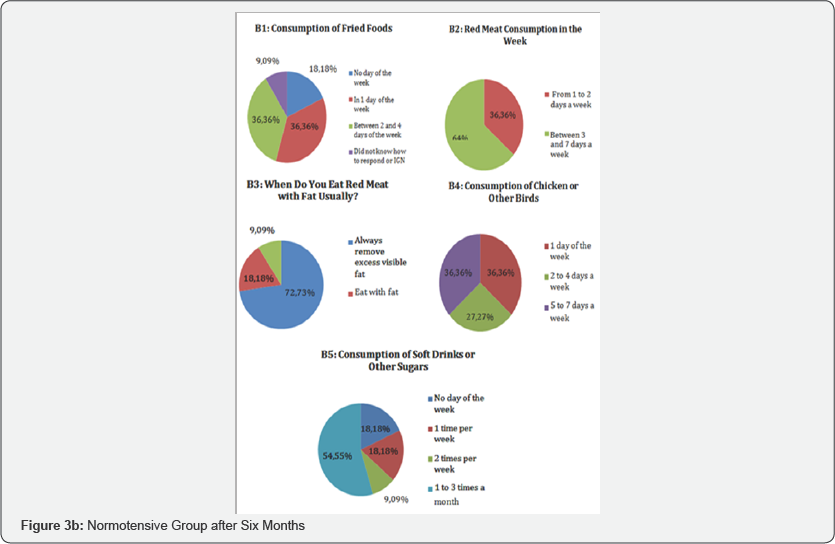
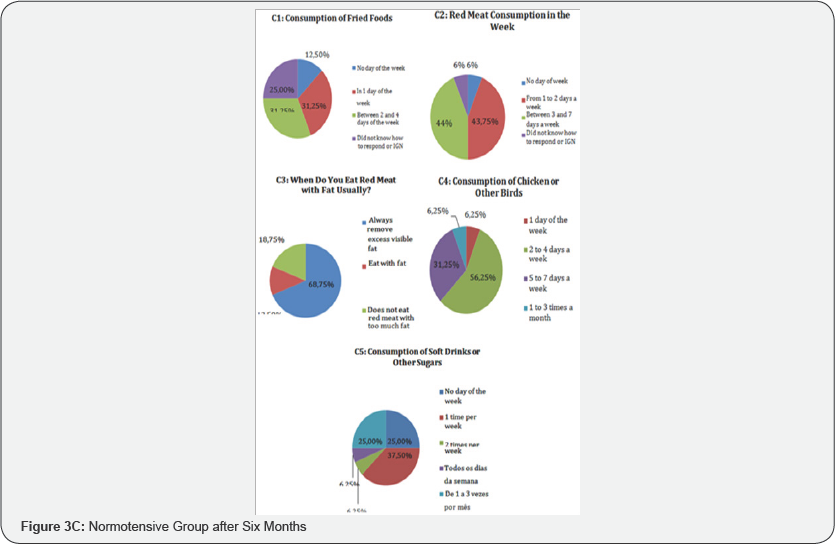
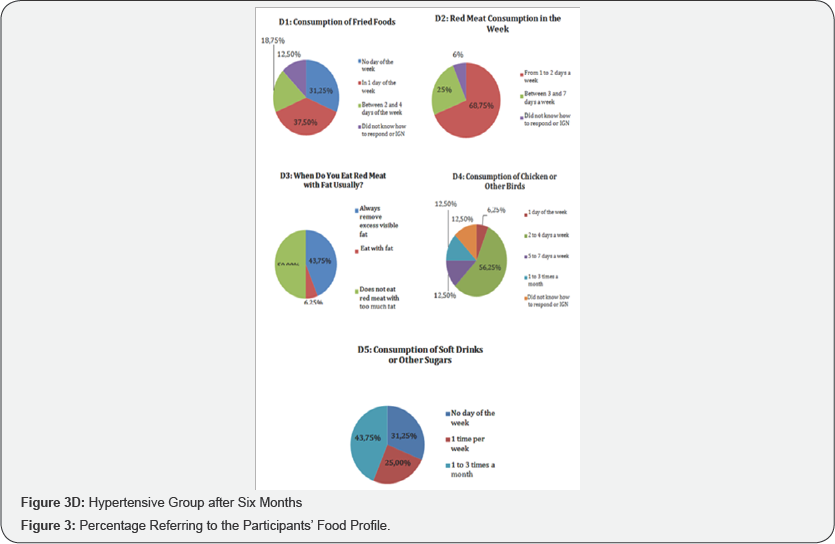

Figures 3-5 shows the results from lifestyle questionnaire. The analysis of the lifestyle responses revealed interesting data when comparing the behaviors before (pre test) and after (after six months) the practice of strength training. In the feeding profile, in the pre test, 63.64% of normotensive patients ate fried foods once a week, 18.18% between two and four days a week, 9.09% did not consume fried foods and 9.09% did not respond or did not know how to report. In hypertensive patients also in pre test, 31.25% consumed fried foods on one day of the week, 31.25% between two and four days, 12.5% on any day of the week and 25% did not respond or did not know how to respond. After six months the strength training, 36.36% of normotensive patients consumed frying on one day a week, 36.36% between 2 and 4 days a week, 18.18% on no day of the week and 9.09% did not answered or did not know how to respond. In the hypertensive groups after six months the strength training the data shows that 37.5% consumed fried foods on one day a week, 31.25% on no day of the week, 18.75% between 2 and 4 days a week, and 12.5% did not respond or did not know how to inform.
Regarding the intake of soft drinks and sugary drinks, in the pre test show that 54.55% of normotensive patients did not consume soft drinks or other sugary beverages, 27.27% consumed 2 times a week and 18.18% consumed once a week. In the pre test the date of hypertensive group show 37.5% of patients consumed soft drinks or other sugary beverages once a week, 25% did not consume such beverages on any day of the week, 25% from 1 to 3 times a month, 6.25% consume twice a week and 6.25% every day in the week. After six months the date of normotensive group shows that 54.55% of normotensive patients consumed soft drinks and sugary beverages 1-3 times a month, 18.18% did not consume such beverages, 18.18% consume those beverages one time per week and 9.09% consume twice a week. In the hypertensive group, after six months, 43.75% consume soft drinks or sugary drinks 1 to 3 times a month, 31.25% do not consume such drinks and 25% consume once a week.
Red meat consumption, before the intervention of strength training (pre test), 54.55% of the normotensive patients consumed red meat in 1 to 2 days in the week and 45% consumed between 3 to 7 days in the week. In the hypertensive group also in the pre test, 44% consumed red meat between 3 and 7 days a week, 43.75% consumed red meat in 1 to 2 days a week, 6% did not consume red meat and 6% did not respond or did not know how to report. After the strength training intervention (after six months) the data of normotensive group show 64% of the patients started consuming red meat from 3 to 7 days a week and 36.36% from 1 to 2 days a week. In the hypertensive group, also in the after six months, 68, 75% of the patients consumed red meat in 1 to 2 days in the week, 25% between 3 to 7 days in the week and 6% did not respond or did not know to inform.
As for red meat with fat, in the pre test 63,64% of the normotensive patients always took the visible excess of red meat, 18,18% of them ate meat with fat and 18,18% did not eat meat with fat. In hypertensive patients (pre test), 68.75% always removes excess visible fat from the meat, 18.75% not as meat with a lot of visible fat and 12.5% as meat with fat. After six months the strength training, 72.73% of the normotensive patients started to always remove the visible excess fat from the meat, 18.18% continue to eat meat with fat and 9.09% did not eat red meat with a lot of fat. In the hypertensive group (also after six months), the changes were even more significant: 50% of the patients did not eat red meat with a lot of visible fat, 43.75% always took away the excess visible fat and 6.25% did not eat red meat with fat.
They consumed chicken and other poultry prior to the pre test, 63.64% of normotensive patients 2 to 4 days of the week, 18.18% in one day of the week, 9.09% in 5 to 7 days in the week and 9.09% from 1 to 3 times in the month. In the date in the pre test of hypertensive patients, 56.25% of the patients consumed chicken meat from 2 to 4 days a week, 31.25% from 5 to 7 days a week, 6.25% from 1 day a week and 6.25% from 1 to 3 times a month. After six months of strength training, 36.36% of normotensive patients consumed chicken and other poultry meat in 5 to 7 days of the week, 36.36% in 1 day in the week and 27.27% in 2 4 days a week. In the hypertensive group (after six months), 56.25% of the patients consume chicken or other poultry in 2 to 4 days a week, 12.5% in 5 to 7 days in the week, 12.5% in 1 to 3 times a month, 25% consumed 1 day a week and 12.5% did not respond or did not know how to report.
Before the six-month strength training intervention (pre test), 54.55% of normotensive patients consumed alcoholic beverages monthly or less, 18.18% 2 to 4 times per month, 18.18% 2 to 3 times per week, and 9,09% never consume alcoholic beverages. In the group of hypertensive patients also in the pre test, 37.5% consume alcoholic drinks monthly or less, 37.5% never consume alcoholic beverages, 12.5% consume 2 to 4 times a month and 12.5% 2 to 3 times a week. After strength training (after six months) in the normotensive group, 36.36% of patients never consume alcoholic beverages, 18.18% consume monthly or less, 18.18% consume 2 to 4 times a month, 18.18% consume 2 to 3 times in the and 9.09% did not respond or did not know how to report. In the hypertensive group after six months the strength training, 43.75% never consume alcoholic beverages, 31.25% consumed 2 to 4 times a month, 18.75% monthly or less and 6.25% did not respond or did not know how to inform.
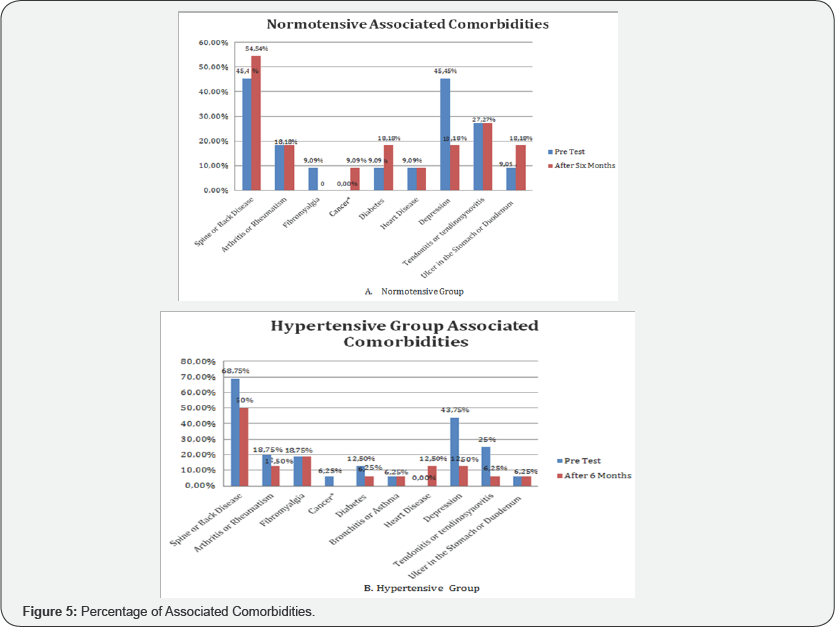
Figure 5 shows the associated comorbidities in the normotensive and hypertensive groups. Regarding to associated comorbidities, in the pre test, 45,5% the normotensive group had depression, 27,3% had tendonitis or tendinosynovitis and 45,5% had spain or back disease. In the hypertensive group (pre test), 43,7% had depression, 25% had tendonitis or tendinosynovitis and 68,7% had back pain. After 6 months of ST, in the normotensive group only 18,8% continue presenting depression, 27,2% reported tendonitis and 54,5 presented back disease. In the hypertensive group after 6 months of ST, only 12,5% continued presenting depression, 6,2% continued presenting tendonitis or tendinosynovitis and only 50% of hypertensive patients continue presenting spain or back disease.
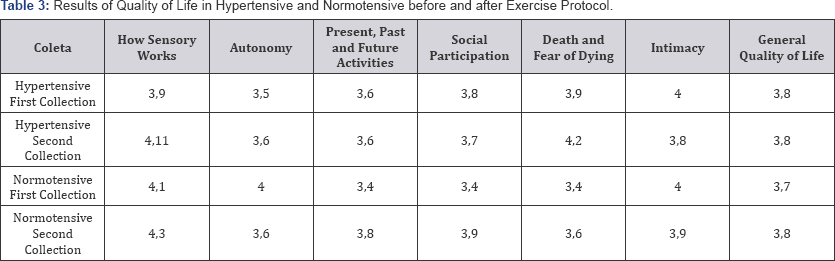
Table 3 shows the results obtained with the quality of life questionnaire. Results revealed that, when asked about death or fear of dying, before the six-month strength training intervention, hypertensive and normotensive patients rated "fear of death" or "dying" as "regular". After training, hypertensive patients assessed the fear of dying or dying as "good", while normotensive patients continued to evaluate as "regular". Already related to the functioning of the sensorium before the intervention of six months of strength training, the hypertensive patients considered the functioning of the sensorium as "regular" and the normotensive ones as "good". After training, the hypertensive and normotensive patients considered the functioning of the sensorium as "good". The other results from both questionnaires did not have significant alterations.
Discussion
Non-pharmacological treatment is increasingly being recognized as an important tool in the fight against hypertension. Although most of the literature considers aerobic exercise to reduce blood pressure levels, strength training, as performed in this protocol, is showing significant results in reducing blood pressure and improving patients' quality of life [4] and our results corroborates with the latest published papers. In this study we showed that six months of strength training were able to significantly reduce blood pressure (Figure 2). It is already known that the regular practice of physical exercise as walking is important and effective in the treatment of hypertension. However, several studies show that the practice of strength training (bodybuilding) is as beneficial in hypertension as aerobic exercise, and may even generate more significant changes [9]. A recent study also revealed that ST may be the best nondrug treatment for SAH, even acting as a substitute for drugs, as it can significantly reduce blood pressure in prehypertensive individuals without the help of medications. In addition, regular practice of TF may cause the use of antihypertensive drugs to be reduced by around 50% in hypertensive individuals [9].
Besides the reduction in blood pressure, in this study we observed changes in lifestyle parameters (Figures 3-5). For a hypertensive patient, maintaining a balanced eating habit is essential for an adequate maintenance of blood pressure levels, weight and for reduce the cardiovascular risk factors [13,14]. As observed in our results, the patients' eating habits improved after six months of intervention, mainly in the hypertensive group. Reduction in the consumption of fried foods, soft drinks and sugary drinks, red meat, red meat with fat, alcoholic beverages and the increase in the consumption of chicken meat suggest a trend of global improvement of the cardiovascular risk factors, (HDL), the decrease in triglycerides, glucose and insulin, as suggested by Fagard [15]. This, in addition to the reduction of blood pressure levels, prevents the onset of associated diseases, such as stroke, which are responsible for a greater deterioration of the quality of life of these patients. It's important to note that the modification in lifestyle verified in our study occurred spontaneously, that is, the patients were not induced by the researchers to change her habits.
These results reiterate the importance of regular practice of straight training in treating hypertension. The increasing prevalence of functionally limited hypertensive individuals emphasizes the need for interventions to reduce the burden of hypertension and maximize the chances of a healthy aging [15]. When practicing physical activities, patients feel influenced to modify their lifestyle and, as Fleischmann et al. [9] affirms, decrease body weight, BMI and active lifestyle, protecting the cardiovascular system.
Low back pain (LBP) is the most common disease in the older adult population. The LBP and others spine or back disease is increasing throughout the world, and is expected to continue growing. Trunk muscle training (TMT) has been found to be effective in reducing LBP among older adults and can be an alternative to used to against other column diseases. TMT can be used to engage the core muscles, which function as active spinal stabilizers [16,17]. In our study, the results of the exercise protocol used demonstrated an 18% reduction in back pain in hypertensive patients. This shows that the strengthening of the spinal muscles really helps to reduce this pain, which helps in the process of improving quality of life.
The results obtained with Whoqool OLD (Table 3) demonstrated that the hypertensive patients submitted to strength training improved their selves evaluations in the parameters death and fear of dying and sensorial alterations. This implies that the perception of these patients regarding to the finitude of life and its possible consequences is positive, a factor that removes possible psychological problems related to senescence such as depression [18,19]. The sensorial alterations of the aging process interfere negatively in daily activities and independence, which also influences QoL; therefore when there is improvement of these sensorial alterations, there is an improvement in the connection of the individual with his space allowing him to live longer with the freedom that is his right. Aging is a natural and progressive process that promotes physiological and psychological changes that can impair the adaptive capacity we have with the environment in which we live [20]. Thus, quality of life (QoL) becomes an important factor to be evaluated with aging, since it is a measure of the impact of this process on people's daily lives.
Depression, which is present in a significant percentage of participants, is a common disease that affects up to 17% of the population during life and is also observed as co-morbidity in various somatic diseases, such as cancer, heart disease and diabetes [21]. In addition to depressed mood, other symptoms caused by depression such as difficulty sleeping, loss of appetite, loss or significant weight gain, loss of interest or pleasure in daily activities and lack of energy, impose a hypertensive patient an additional barrier in the fight of disease control, which, as already emphasized, necessitates a lifestyle change [22]. To counteract the negative effects of depression, it is typically used pharmacotherapy and psychological interventions [23]. However, as seen with the results obtained after strength training and reinforced by Stanton, 2014, a large number of studies have confirmed the positive effect of exercise on depression. Therefore, in addition to contributing to the reduction of pressure levels and as a cardiovascular protection factor, physical exercise recovers not only the quality of life, but also the lifestyle, allowing patients with depression and, consequently, with more difficulties of routinely alter their habits in favor of their health [21-24].
The other data collected about life style and quality of life (Tables 1,2) did not change after 6 months of ST. We can infer that if the ST protocol used in this work was longer, we could have more changes in the other parameters analyzed. Fleischmann et al shows in some of his studies that after six months of intervention using physical exercise, the patients did not feel the positive effects on his quality of life [14]. Thus, we suggest for further studies a protocol using 3 times a week of ST and longer than 6 months. However, it is important to highlight that our study (only 6 months of ST) was already enough to change many aspects of quality of life and lifestyle of middle- aged woman. And, more important, was enough to significantly reduce blood pressure.
In conclusion, we verified that strength training twice a week was able to reduce blood pressure and improve lifestyle and quality of life parameters in hypertensive woman. Our results corroborate with the current literature and reinforces that for treating hypertension non pharmacological interventions need to be considered. Physical exercise and balanced diet are expedited to transform the lifestyle of patients with hypertension and, therefore, modifiable risk factors in the pathology of the disease. As we have seen through our results, physical exercise drove the volunteers to make efforts to change food habits that are linked to comorbidities associated with SAH, such as consumption of fatty foods and the use of alcoholic beverages. In addition, blood pressure values, both systemic and diastolic, had a significant reduction, mainly in the hypertensive group, showing that possibly people who practice regular ST will need low doses of anti-hypertensive drugs. In the normotensive group, the cardiovascular risk factor will be considered as a factor of cardiovascular protection in the future. Indeed, further studies are still needed to establish all the factors of strength exercise on the physiology of hypertension.
Practical Applications
The results of this study indicated that the practice of strength training influenced important changes in eating habits as well as resulted in a significant change in the systolic and diastolic blood pressure levels from hypertensive woman volunteers, further corroborating the premise that this practice serves an effective and non-pharmacological treatment. This research was conducted with middle-aged woman volunteers (a population that generally are sedentary), showing that changes in lifestyle in middle age can be decisive for prevent many diseases, specially hypertension. Moreover, this study can act as an incentive for general population to adopt a healthier and more active lifestyle, being a trigger for adhering to these practices in their routine that will probably bring them many benefits. In conclusion, current results indicate that if strength training is incorporated into the routine, it may be possible to reduce the doses of antihypertensive drugs or even replace the drugs used by this non-pharmacological treatment.
References
- Fauci AS, Braunwald E, Kasper DL, Hauser SL, Longo DL, et al. (2008) Harisson Medicina Interna. Mc Graw Hill Interamericana do Brasil, Rio de Janeiro, Brazil.
- Lloyd Jones D, Adams R, Carnethon M (2009) Heart disease and stroke statistics-2009 update. A report from the American Heart Association Statistics 119: 21-181.
- (2013) Brazil Ministry of Health. Strategies for care of the person with chronic disease: Systemic arterial hypertension, Cadernos de Atenfao Basica.
- Fleischmann EH, Friedrich A, Danzer E, Gallert K, Walter H (2004) Intensive training of patients with hypertension is effective in modifying lifestyle risk factors. Journal of human hypertension 18(2): 127-131.
- NCDRF Collaboration (2017) Worldwide trends in blood pressure from 1975 to 2015: A pooled analysis of 1479 population-based measurement studies with 19.1 million participants. Lancet 389(10064):37-55.
- Zhong Y, Rosengren A, Fu M, Welin L, Welin C (2017) Secular changes in cardiovascular risk factors in Swedish 50-year- old men over a 50-year period: The study of men born in 1913, 1923, 1933, 1943, 1953 and 1963. Eur J Prevent Cardiol 24(6): 612-620.
- Muntner P, Carey RM, Gidding S, Jones DW, Taler SJ (2018) Potential US population impact of the 2017 ACC/AHA high blood pressure guideline. Circulation 137(2): 109-118.
- Gorostegi Anduaga I, Corres P, Martinez ABA, Perez Asenjo J, Aispuru GR (2018) Effects of different aerobic exercise programmes with nutritional intervention in sedentary adults with overweight/obesity and hypertension: EXERDIET-HTA study. Eur J Prevent Cardiol 25(4): 343-353.
- Li Y, Hanssen H, Cordes M, Rossmeissl A, Endes S (2015) Aerobic, resistance and combined exercise training on arterial stiffness in normotensive and hypertensive adults: A review. Eur J Sport Sci 15(5): 443-457.
- Federal University of Santa Catarina.
- Fleck MPA, Chachamovich E, Trentini C (2003) WHOQOL-OLD project: method and results of focus groups in Brazil. Rev Saude Publica 37(6): 793-799.
- Brazilian Society of Cardiology (2016) Brazilian hypertension guideline (DBH). Brazilian archives of cardiolog 107(3): 1-103.
- Borg G (2000) Borg's scales for pain and perceived exertion.
- Borges HP, Cruz NC, Moura EC (2008) Association between arterial hypertension and overweight in adults, Belem, Para, 2005. Arq Bras Cardiol 91(2): 110-118.
- Fagard RH, Cornelissen VA (2007) Effect of exercise on blood pressure control in hypertensive patients. European Journal of Cardiovascular Prevention & Rehabilitation 14(1): 12-17.
- Coghlan S, Crowe L, McCarthypersson U, Minogue C, Caulfield B (2011) Neuromuscular electrical stimulation training results in enhanced activation of spinal stabilizing muscles during spinal loading and improvements in pain ratings. Conf Proc IEEE Engineering in Medicine and Biology Society 2011: 7622-7625.
- Hicks GE, Sions JM, Velasco TO, Manal TJ (2016) Trunk muscle training augmented with neuromuscular electrical stimulation appears to improve function in older adults with chronic low back pain: a randomized preliminary trial. The Clinical journal of pain 32(10): 898906.
- Baptista LC, Amorim AP, Valente JS, Machado RAM, Veri'ssimo MT (2018) Functional status improves in hypertensive older adults: The long-term effects of antihypertensive therapy combined with multi component exercise intervention. Aging clinical and experimental research p. 1-13.
- Tavares DMS, Matias TGC, Ferreira PCDS, Pegorari MS, Nascimento JS (2016) Quality of life and self-esteem among the elderly in the community. Cienc saude coletiva 21(11): 3557-3564.
- Burroughs H, Bartlam B, Ray M, Kingstone T, Shepherd (2018) A feasibility study for Non-Traditional providers to support the management of Elderly People with Anxiety and Depression: The NOTEPAD study Protocol. Trials 19(1): 172.
- Zhang X, Xia R, Wang S, Xue W, Yang J (2018) Relative Contributions of Different Lifestyle Factors to Health-Related Quality of Life in the Elderly. International journal of environmental research and public health 15(2): 256.
- Krogh J, Speyer H, Gluud C, Nordentoft M (2015) Exercise for patients with major depression: a protocol for a systematic review with metaanalysis and trial sequential analysis. Systematic reviews 4(1): 40.
- Zeng N, Pope Z, Lee JE, Gao Z (2018) Virtual Reality Exercise for Anxiety and Depression: A Preliminary Review of Current Research in an Emerging Field. Journal of Clinical Medicine 7(3): 42.
- Stanton R, Reaburn P (2014) Exercise and the treatment of depression: A review of the exercise program variables. Journal of Science and Medicine in Sport 17(2): 177-182.






























