Complex Regional Pain Syndrome Type I Treated with Active Release Technique
Kathleen Hughes and James Mc Kivigan*
School of Physical Therapy, Touro University, USA
Submission: March 10, 2017; Published: March 28, 2017
*Corresponding author: James M McKivigan, School of Physical Therapy, Touro University Nevada, USA, 874 American Pacific Drive, Henderson, NV 89014, Tel: 702-777-3096; Email: james.mckivigan@tun.touro.edu
How to cite this article: Kathleen H, James M K. Complex Regional Pain Syndrome Type I Treated with Active Release Technique. J Phy Fit Treatment & Sports. 2017; 1(1): 555553 DOI: 10.19080/JPFMTS.2017.01.555553
Abstract
This report describes the examination, intervention, and outcome for a patient with CRPS type I treated with ART®. The patient was diagnosed with CRPS following a grade II ATFL sprain. For two months, treatment consisted of weekly 45-minute sessions including ART® in combination with self-massage, desensitization, joint mobilization, gait training, therapeutic exercise, and patient education. A brief reexamination was performed weekly. A clinically significant increase of 13 points on the LEFS was measured after eight weeks of treatment, as were improvements in quality of gait and gait distance. In addition, the patient experienced the return of ankle range of motion to normal. Throughout the treatment period, a decrease in pain and an increase in functional capacity were noted by way of patient report to supplement the objective outcome measures (which were few). CRPS continues to be a vague and complex syndrome that is difficult to treat. ART® may be an effective intervention in the physical therapy management of CRPS by way of its proposed effects of restoring optimal function and texture to the hypo mobile soft tissues as well as compromised nerves and vasculature found in patients with CRPS.
Keywords: Complex regional pain syndrome; CRPS; Active Release Techniques; Physical therapy; Soft tissue therapy; Soft tissue mobilization; Reflex sympathetic dystrophy; Case report
Abbreviations: CRPS: Complex regional pain syndrome; IASP: International Association for the Study of Pain; PT: Physical Therapists; ATFL: Anterior Talofibular Ligament; LE: Lower Extremity; MRI: Magnetic Resonance Imaging; LEFS: Lower Extremity Functional Scale; MDC: Minimal Detectable Change; AROM: Ankle Active Range of Motion; PROM: Passive Range of Motion
Introduction
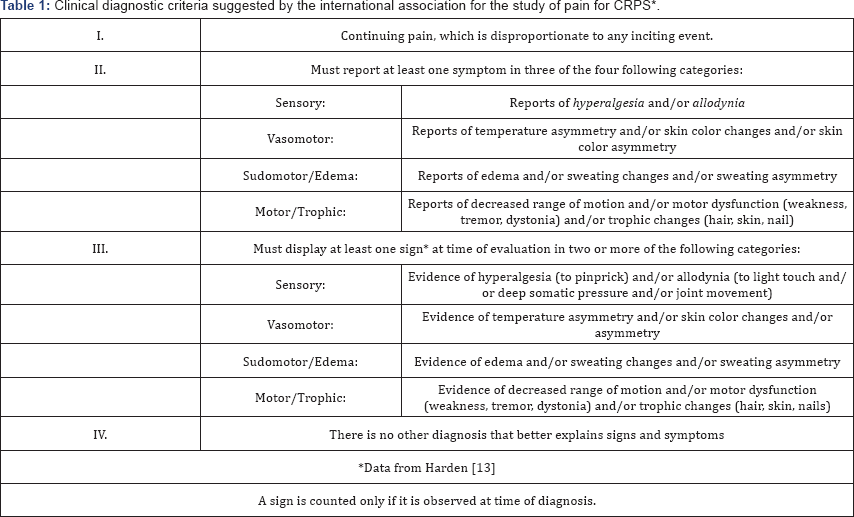
Complex regional pain syndrome type I (CRPS) is a chronic pain disorder involving the sensory, motor, and autonomic nervous systems, often leading to severe debilitation. Most commonly, a preceding limb injury catalyzes CRPS, although insidious onset has been known to occur. An estimated 60,000 Americans are affected by CRPS, including individuals between 25 and 55 years of age. CRPS is three times more likely to occur in women, although it can affect anyone [1]. Table 1 contains the CRPS clinical diagnostic criteria suggested by the International Association for the Study of Pain (IASP). Because of the poor understanding of the etiology of CRPS, its medical management is nebulous. Along with pain management, optimal treatment outcomes appear to be achieved when emphasizing functional restoration-a realm largely encompassed by physical therapists (PT). However, a review of the literature found that the term physical therapy is often used vaguely with no corresponding definition or description of procedures employed during treatment [2]. This has left PTs with a lack of guidance in treating patients with CRPS. The purpose of this case report is to describe the physical therapy management of a 38-year-old patient with CRPS developed from a chronic anterior talofibular ligament (ATFL) injury by using Active Release Techniques® (ART®) in combination with joint mobilization, gait training, therapeutic exercise, and education to document the observed clinical and functional improvements.
The theory behind ART® proposes that constant micro-trauma (small tears) among soft-tissue structures can lead to tight and weak muscles, eventually leading to chronic injury, degeneration, or inflammation [3]. During ART® therapy, deep digital tension is applied to the affected structure as it is moved from a shortened to a lengthened position [4]. The treatment goal is to improve or restore soft tissue function by reducing tissue stiffness, fibrosis, or adhesion [4]. Yet, there is a lack of high-level research to determine the efficacy of ART® more conclusively. ART® was chosen as the primary intervention in this case report because it is designed to accomplish three distinct objectives: to restore free and unrestricted motion to all soft tissues; to release entrapped nerves, vasculature, and lymphatics; and to reestablish the optimal texture, resilience, and function of soft tissues [5]. Given the significant hypomobility of soft tissue and compromised nerves and vasculature found in patients with CRPS, ART® therapy is a plausible method of restoring the function critical to achieving optimal outcomes in the management of CRPS.
Case Description
History
The patient was referred to K. Hughes 9 months after a grade II right ATFL sprain and previous failed attempts at pain control and rehabilitation through medical management. Before this injury, the patient was an active 38-year-old woman involved in snowboarding, running, hiking, and regular social pursuits. The patient also reported being diagnosed with bipolar disorder more than a decade prior. She experienced a right ATFL sprain while snowboarding and she was misdiagnosed with an Achilles tear. The day after the injury, she reported feeling an immediate coldness to the touch and numbness in the right lower extremity (LE) from the knee down.
Eight weeks after the injury, she reported her right foot became cyanotic. She visited the emergency department where a neurological exam was performed, resulting in a diagnosis of CRPS. Because of continued severe pain, the patient returned to the emergency department two weeks later (10 weeks post-injury), when a magnetic resonance imaging (MRI) scan revealed a grade II right ATFL sprain. A surgical repair was completed nearly six months post-injury. The patient was examined by this author's CI nearly four months postsurgical repair after complaints of ankle and right foot pain (in the seamaid and great toe regions); extreme difficulty with ambulation; frequent work absences due to dysfunction; and depression over her inability to participate in prior activities. She reported pain levels to be 1/10 at best, 1/7 at worst, and 3/10 at the time of the examination.
Examination
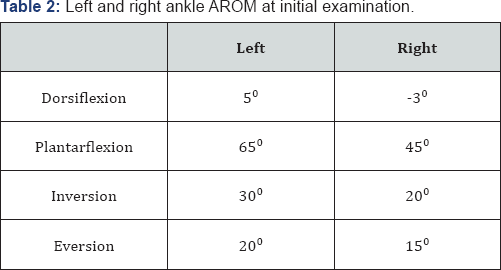
The patient presented with an antalgic gait while ambulating, secondary to a decreased right LE stance phase, and she reported using an SPC often but did not have it with her. Ambulation was limited to short distances on carpet and hard surfaces only and supplemented by several orthotic inserts in the patient's shoes. Attempts to bear weight on the right LE were very painful in the sea-maid and great toe regions with shoes on and impossible without shoes. Fear avoidance of the sea-maid and great toe regions resulted in toeing out and inversion of the right foot during gait. A non-weight bearing assessment of the right foot revealed moderate apprehension toward tactile stimuli over the sesamoid, great toe, and ATFL regions. Color and swelling symptoms of CRPS were at a minimum, but the right ankle was cold upon palpation. The patient was asked to fill out the Lower Extremity Functional Scale (LEFS) questionnaire at the beginning of the initial evaluation (Table 2), revealing a low score of 38/80.The LEFS is used to assess the impairment of a patient with an LE musculoskeletal condition or disorder. Binkley et al found the LEFS test-retest reliability and inter-rater reliability for various LE injuries to be excellent, and the minimal detectable change (MDC) was found to be nine points [6]. Ankle active range of motion (AROM) was measured by goniometry and found to have decreased on the right. A lack of passive range of motion (PROM) at the talocrural joint was found, possibly causing the patient’s metatarsal aggravation during gait. Table 3 displays the results of the goniometric measurements taken during initial examination. Goniometry has been shown to be a valid and responsive method of measuring joint ROM [7]. Whereas inter-rater reliability was found to be poor to moderate (ICC = 0.5-0.72) for goniometry, the intra-rater reliability of goniometry for ankle dorsi- and plantar flexion was found to be good to sufficient for clinical measurements (ICC = 0.86-0.91) [2].
Evaluation and diagnosis
The patient presented with signs and symptoms incompatible with those expected of a typical grade II ankle sprain; that is, they had progressively worsened and spread rather than resolved within a 2- to 4-week period, as expected [2,8]. After the patient sought further medical evaluation, she received a diagnosis of CRPS. The following results, which were found following a physical therapy examination, were correlative with the CRPS clinical diagnostic criteria outlined in Table 1.
- Continuing pain disproportionate to the inciting event
- Allodynia, color changes, color asymmetry, edema, decreased temperature, temperature asymmetry, and decreased AROM
- No other diagnosis that could better explain the signs or symptoms
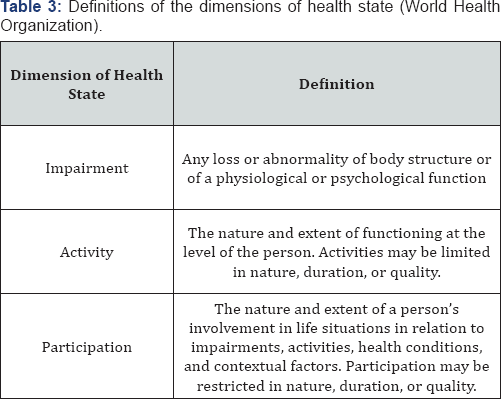
The clinical diagnostic criteria outlined in Table 1 have an established specificity of 0.69 [2]. High specificity combined with positive signs and symptoms from the clinical diagnostic criteria allowed for a confident diagnosis of CRPS for the patient in this case report. A physical therapy diagnosis was also determined, according to the terminology proposed by the World Health Organization in its International Classification for Functioning, Disability and Health, displayed in Table 4 [2]. Impairments found included ankle pain and decreased ankle AROM. The patient experienced limitations in activities and restrictions in participation, including the inability to ambulate, run, hike, snowboard, or participate in typical social activities.
Prognosis
Establishing a prognosis for a patient with CRPS is difficult for many reasons, including the great variability in signs and symptoms, the multitude of treatments used by clinicians, and the lack of unified and definitive diagnostic criteria, until recently [2]. According to the Guide to Physical Therapist Practice, 80% of individuals diagnosed with CRPS are expected to reach planned goals and outcomes in 3-36 visits [9]. However, considering the aforementioned prognostic influences, physical therapy prognosis seems largely based on expert opinion rather than researched facts. The National Institute of Neurological Disorders and Stroke [10] stated that if treatment is initiated within three months of symptom onset, remission is often achieved; if treatment is delayed, 50% of patients experience pain that persists longer than six months, possibly even years.3 Gellman and Nichols found that "prognosis is, at best, guarded," and they agree that early prognosis is of utmost importance [2].
Paice reported that if left untreated, CRPS could lead to "devastating long-term disability" [2]. Hord and Oaklander described CRPS as "disabling and difficult to treat" [2]. Hence, a consensus appears to exist-albeit not a research-based one-on the potentially crippling effects and poor prognosis for patients diagnosed with CRPS, especially when treatment is not initiated within three months of symptom onset [2]. Given the delayed diagnosis and initiation of treatment for the patient in this case report, it is reasonable to assume that the prognosis was poor. This poor prognosis could also be interpreted to suggest that a positive outcome might provide additional credibility to any positive therapeutic effects achieved through interventions described in this case report.
Intervention
For 2 months, the patient was seen once a week for 45-minute treatment sessions, including 5-10 minutes of re-examination followed by a combination of the subsequent interventions: ART®, joint mobilization, gait training, therapeutic exercise, and patient education. During initial evaluation, PROM was performed on the right ankle and gait training was implemented using several orthotic inserts in the patient's shoes. The patient was instructed to focus on ambulating without a limp and was sent home with instructions for desensitization and self- massaging the right foot and ankle. Desensitization techniques consisted of rubbing materials of varying textures, first on the left (unaffected) ankle and followed by on the right (affected) ankle. For therapeutic exercise, the patient was trained in the proper form of partial squats and sit-to-stand transfers.
During the second session, the patient reported experiencing no CRPS exacerbation from the previous session and the patient is having an "overall better week." Right ankle AROM was evaluated and found to have improved by 5° in both inversion and eversion. As well, it improved by 3° in dorsiflexion after joint mobilization was performed on the right tarsals and talocrural joint. ART® was performed on the following structures of the LE: anterior tibialis, peroneus longus, peroneus brevis, extensor hallucis longus, deltoid ligament, ATFL, gastrocnemius, soleus, calcaneofibularligament, and retinaculum. Moderate pain and tightness were found in the right calf musculature, especially in the soleus. The calcaneofibular ligament was extremely tender with manual work. Gait training focused on rocking motions with emphasis on bearing weight through the right great toe and sea-maid regions to assist with eventual progression to proper form in heel strike through toe-off, but this was limited by a worsening of pain in the associated regions. For therapeutic exercise, the patient was instructed on the following:
- Supine core activation: knees bent to 90°, feet flat on the mat, patient instructed in transversusabdominis activation
- 4-way ankle AROM: DF, PF, inversion, and eversion for 10 repetitions each
- Inversion and eversion against resistance: using a yellow Thera Band for 10 repetitions in each direction
- Bridge position with a "march": slow, gentle weight shifts from foot to foot while minimizing pelvic motion
During the third session, the patient was crying and clearly in a state of emotional distress. She reported foot soreness from excessive walking over the weekend and frustration with the chronic nature of her injury. Palpation revealed the plantar surface of the right first phalanx to be the primary source of pain, although PROM to all toes was pain-free and within normal limits. PROM of the right talocrural joint was performed as well as ART® on the following structures of the right LE: retinaculum, anterior tibialis, extensor hallucis longus, extensor digitorum longus, and extensor digitorum brevis. Modified front and side planks were added to the patient’s therapeutic exercise regimen as well as "bird dog" in a quadruped position, where the patient was asked to extend the opposite arm and leg simultaneously. Bridge position was attempted again but was limited by a worsening of pain in the great toe and sesamoid regions. During the fourth session, the patient reported increasing frustration with her lack of recovery and, though she has been trying not to limp, the excessive padding in her right shoe seemed to be causing pain in the great toe region. Adjustment of the patient's orthotic insert was made to decrease pressure over the right great toe and sesamoid regions during gait, with immediate improvement in ambulation form as well as pain level in the right foot. Gait training focused on heel strike and fully rolling through toe-off, despite the patient’s fear of bearing weight on the right great toe and sesamoid regions.
Avoidance of these regions was causing toeing out and inversion of the right foot during stride. The patient was limited by symptom onset at approximately 20 feet of gait. ART® was performed on the following structures of the right LE: retinaculum, anterior tibialis, extensor hallucis longus, anterolateral post-surgical scar tissue, posterior talofibular ligament, adductor hallucis, and abductor hallucis. No further therapeutic exercises were added to the patient's regimen. During the fifth session, the patient reported a CRPS exacerbation after the previous treatment session, with her foot remaining cold. She also reported that walking had been "really tough" due to the cold, but the orthotic adjustments have helped with the right great toe pain. The patient’s primary complaint is now regarding the ankle, particularly the anterolateral post-surgical scar tissue. Palpation revealed talocrural mobility to be improving, but decreased tendon movement under the retinaculum is limiting plantar flexion. ART® was performed on the following structures of the right LE: gastrocnemius, soleus, extensor hallucis longus, extensor digitorum longus, anterolateral post- surgical scar tissue, retinaculum, anterior tibialis, and tarsal ligaments. "Chops" and "lifts" with the patient in a half-kneeling position on an Airex pad were added to the patient's therapeutic exercise regimen as well as standing gastrocnemius and soleus stretches.
During the sixth session, the patient reported a significant decrease in pain levels with ambulation and a desire to work on strengthening, as she was feeling "so much better this week!" PROM of the right ankle and ART® were performed to the following structures of the right LE: retinaculum and posterior talofibular ligament. Core strength and stability were facilitated with bridge exercises as well as modified front and side planks. The "child’s pose" position was introduced to the therapeutic exercise regimen as a method of relaxation for the patient as well as a means of improving ankle mobility. During the seventh session, the patient reported her "body is great" but the lateral portion of her right ankle "stiffens up" after sitting all day at work. Standing calf stretches, "child’s pose" positions, and selfmassages of the right ankle and surrounding musculature were recommended to improve ankle stiffness along with regular movement. Palpation revealed improved ankle tissue texture, color, and temperature. Calcaneal mobilization and ART® were performed to the following structures of the right LE: posterior talofibular ligament, peroneus longus, peroneus brevis, and retinaculum. Tenderness and a slight color change were noted with manual work. An ankle "alphabet" was added to the patient’s therapeutic exercise regimen, where the alphabet is drawn in the air using the foot to improve ankle AROM, as well as "deadlifts" using a stick for posterior chain activation to improve strength and stability.
During the eighth session, the patient reported her foot was feeling better; she was able to wear non-cushioned sneakers rather than her normal heavily cushioned shoes during ambulation, and she no longer used an SPC. She filled out a LEFS questionnaire, revealing a significant score improvement of 51/80from 38/80 at the initial evaluation. A mottled red color was noted over the right great toe and medial arch, which spread to all toes of the right foot with manual work. PROM of the right ankle was found to have improved to within normal limits, although it was not measured. ART® was performed on the posterior talofibular ligament of the right ankle, which easily released. "Deadlifts" were practiced using small weighted kettle bells rather than the stick, first lifting from a step and progressing to lifting from the floor while maintaining a strong, straight- backed position for continued strengthening and stabilizing.
Outcomes
This author participated in and observed the physical therapy treatment of the patient for eight weeks, ending the clinical rotation in which this author was participating (as a student). The main outcome measure used was the LEFS questionnaire, which was filled out upon initial evaluation and again eight weeks later. Table 2 displays the results measured by the LEFS questionnaire, evidencing the marked score improvement and in which activities those improvements were made. Other outcome measures used to assess patient improvements were ROM, gait, use of an assistive device during gait, patient reports of pain, as well as color and temperature changes.
Although improvements in pain level and function were not noted with each session, the patient reported a steady overall improvement regarding pain and functional capacity, as evidenced by subjective reports of increased ability to participate in daily activities and ambulate without an assistive device. Along with the subjective patient reports of improved functionality and decreased pain levels, the patient’s functional capacity was objectively measured using the LEFS questionnaire. Upon re-evaluation after six weeks of treatment, right and left ankle AROMs were found to be within the normal limits. The return of normal ROM in the patient's right ankle, although not objectively measured, also appears to represent a clinically significant improvement from the measurements taken at initial evaluation, displayed in Table 3. By the eighth treatment session, the patient reported increased ambulation distances and no longer needing the use of an SPC. Upon re-examination, the patient’s right foot appeared to have improved from mottled red and cold to a nearly normal color and temperature.
Discussion
While the neurophysiological processes behind CRPS remain vague and puzzling, it is agreed to be a systemic disorder involving the entire neural system, with both central and peripheral manifestations [2]. The use of ART® in combination with the physical therapy management outlined may have assisted this 38-year-old patient in returning to a higher functional capacity after being diagnosed with CRPS. While the outcome measures are the proverbial Achilles’ heel of this case report, the 13-point change on the LEFS questionnaire achieved over eight weeks of treatment exceeded the MDC of nine points for this outcome measure [6], showing that true and meaningful change occurred. While no other outcome measures were objectively taken at eight weeks of treatment, steady improvements in gait, strength, ROM, and pain levels were noted throughout treatment. Given the patient's unsuccessful attempts at medical management and a poor prognosis at the time of physical therapy intervention due to the delay of CRPS diagnosis, it is possible that ART® influenced the clinical and functional outcomes of this case, allowing the patient to improve functional capacity and resume prior activities.
As discussed earlier, research-based information on the physical therapy management of CRPS is sparse and often conflicting, with the majority of research on the chiropractic management of CRPS. In 2013, Pain Medicine published diagnostic and treatment guidelines for CRPS based on a systematic review of the current evidence by a panel of expert practitioners in a variety of fields. They found that pain management techniques focusing on functional restoration appear to be the most effective treatment for CRPS, possibly by resetting the altered neural pathways [11]. According to the Mayo anesthesia group, "Physical therapy is the cornerstone and first line treatment for CRPS" by using gentle progressive exercises [11]. While PTs appear to be in an ideal position to treat patients with CRPS, what is lacking is a solid body of high-level research investigating the various methodologies. Further and more rigorous research into the treatment of CRPS will help reveal the most effective interventions and in what combinations they work best. Despite limited research evidence, several guidelines for the PT management of CRPS have been established, emphasizing symptomatic treatment and functional training [2]. Proposed interventions include: desensitization techniques, transcutaneous electrical nerve stimulation (TENS), joint mobilization, ROM, progressive weight bearing, strengthening, cardiovascular activities, functional training, flexibility, edema management, posture and balance training, ergonomics, and functional or vocational rehabilitation [2,12,13].
It is apparent that all of these approaches are targeting the impairments and functional limitations manifesting from CRPS rather than the underlying causes [2]. A continued effort into researching CRPS etiology is required to treat this. Nearly all patients with advanced CRPS present with myofascial pain [11], like the patient in this case report. Aggressive treatment of this symptom is a vital component of successful outcomes and chiefly the purview of the PT. Some proselytize that CRPS will often resolve once the myofascial pain has been treated. Massage and myofascial release are often used to treat pain and reduce edema, but there is a lack of formal research [11]. As indicated previously, this case report has obvious limitations. Strength measured by MMT and the state of capsular and ligament us structures was not assessed in this case, which may have provided potential clinical measures and treatment options [2]. The clinical evaluation performed included AROM measurement, subjective pain reports, observation, palpation, LE function measured by LEFS, and gait assessment. Most measures do not possess the psychometric properties required to determine an accurate physical therapy diagnosis [2]. However, they are measures prevalent in PT practice.
References
- American Society for Surgery of the Hand (2014) Complex Regional Pain Syndrome. Hand and Arm Conditions.
- Collins C (2007) Physical therapy management of complex regional pain syndrome I in a 14-year-old patient using strain counterstrain: a case report. J Man ManipTher 15(1): 25-41.
- Miners AL, Bougie TL (2011) Chronic Achilles tendinopathy: a case study of treatment incorporating active and passive tissue warm-up, Graston Technique®, ART®, eccentric exercise, and cryotherapy. J Can Chiropr Assoc 55(4): 269-279.
- system for the lower extremity. Active Release Techniques, LLC.
- Howitt S, Wong J, Zabukovec S (2006) The conservative treatment of trigger thumb using Graston Techniques and Active Release Techniques�. J Can Chiropr Assoc 50(4): 249-254.
- Binkley JM, Stratford PW (1999) The Lower Extremity Functional Scale (LEFS): Scale Development, Measurement Properties, and clinical application. Phys Ther 79(4): 371-383.
- Kersey R (2005) Measurement of Joint Motion: A Guide to Goniometry. Athletic Ther Today 10(1): 42-43.
- Patel DR, Janiski C (2005) Ankle sprains in young athletes: part I: how to evaluate: the sports injury you're most likely to see is an ankle sprain. Contemp Pediatr 22: 65-70.
- Guide to Physical Therapist Practice (2001) (2nd edn). Phys Ther 81: 9-746.
- National Institute of Neurological Disorders and Stroke (2013) Complex Regional Pain Syndrome FactSheet, USA.
- Harden R, Oaklander A, Burton AW, Costa B, Graciosa JR, et al. (2013) Complex regional pain syndrome: practical diagnostic and treatment guidelines. (4th edn), Pain Med 14(2): 180-229.
- Howitt SD (2006) Lateral epicondylosis: a case study of conservative care utilizing ART� and rehabilitation. J Can Chiropr Assoc 50(3): 182-189.
- Spina AA (2007) External coxasaltans (snapping hip) treated with active release techniques: a case report. J Can Chiropr Assoc 51(1): 23-29.






























