Introduction
Sleep plays a foundational role in physical and mental health, with insufficient sleep linked to cardiovascular disease, diabetes, depression, cognitive decline, and mortality [1-3]. Despite strong evidence, sleep is rarely assessed as a routine vital sign in healthcare [4]. To address this gap, we developed the Sleep Quality Screener (SQS)—a brief, plain-language, eight-item self-assessment tool designed to measure key dimensions of sleep health as a ‘Lifestyle Vital Sign.’ This paper describes the conceptual foundation, item development, scoring, and applications of the SQS within public health and clinical settings. The screener aligns with research on multidimensional sleep health and the RU-SATED framework, while emphasizing readability, behavioral feedback, and healthliteracy accessibility [5].
National surveillance data confirm that inadequate sleep is a major public health concern. The Centers for Disease Control and Prevention (CDC) reports that only about two-thirds of U.S. adults regularly achieve seven or more hours of sleep per night, with notable disparities by race, socioeconomic status, and geography [6,7]. Short sleep duration has been associated with frequent mental distress and chronic disease risk, emphasizing the importance of population-level interventions that promote sleep awareness and self-monitoring [8].
Sleep health is a multidimensional construct including duration, efficiency, timing, and alertness [2]. Population data indicate widespread insufficient sleep and disparities across populations [3]. Meta-analyses show strong relationships between sleep and both mortality and mental health outcomes [4]. These findings underscore the bidirectional nature of sleep and mental health, as supported by evidence that interventions improving sleep quality yield substantial gains in psychological well-being [3]. Collectively, this growing body of research supports calls to elevate sleep to the status of a clinical and public health vital sign [4]. Embedding short, literacy-appropriate tools such as the Sleep Quality Screener into clinical and community settings operationalizes this vision by translating complex science into accessible, actionable feedback that can improve individual and population-level health outcomes.
Conceptual Framework
The Sleep Quality Screener (SQS) was developed to address a critical gap in sleep health assessment: the lack of brief, integrated, and accessible tools suitable for real-world use. Despite growing recognition of sleep as a key determinant of health, existing instruments are often lengthy, disorder-specific, or not designed for rapid screening in clinical or community settings. Few tools are grounded in behavioral theory while also prioritizing health literacy and user engagement [9,10].
To address this gap, the SQS was developed based on four
guiding principles for effective lifestyle assessment tools:
1. Tools should support both assessment and behavior
change
2. Tools should be brief (ideally completed in under three
minutes)
3. Tools should be grounded in public health guidelines
and behavioral theory
4. Tools should be written in plain language to enhance
accessibility
Without brief and user-friendly screening tools, healthcare professionals and educators miss valuable opportunities to assess lifestyle behaviors holistically, deliver brief interventions, and track progress over time. Rapid assessment tools can enhance patient engagement, guide goal setting, and support populationlevel monitoring of behavioral risk factors. These approaches also align with national priorities such as the Healthy People 2030 objective on organizational health literacy, which emphasizes ensuring that individuals can understand and use health information effectively [11].
Within this framework, the SQS was designed as part of a broader Lifestyle Vital Signs approach, representing a scalable strategy to integrate lifestyle medicine into clinical care, education, and community health practice.

Methods—Item Development
The Sleep Quality Screener (SQS) consists of eight items that assess key behavioral and experiential dimensions of sleep health (Figure 1). The items were selected to reflect both established sleep science and practical, modifiable behaviors. The ordering of items was intentionally designed to enhance usability, comprehension, and response accuracy. Questions are sequenced to follow a logical progression from nighttime sleep behaviors to daytime functioning, mirroring how individuals naturally think about their sleep experience. The screener begins with concrete, easily observable behaviors (e.g., falling asleep, staying asleep), which are cognitively simple to recall and help build respondent confidence. It then transitions to duration and routine-based behaviors, followed by environmental and behavioral sleep hygiene practices. The final items assess subjective sleep quality and daytime alertness, allowing respondents to reflect on the outcomes of their sleep patterns. This structured flow reduces cognitive burden, minimizes response fatigue, and supports more accurate self-assessment, particularly in low-literacy or timeconstrained settings.
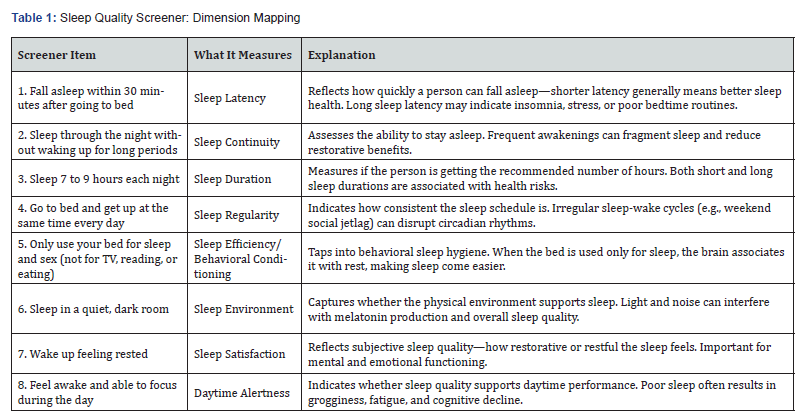
Items 1 and 2 assess sleep onset and continuity, including the ability to fall asleep within 30 minutes and remain asleep without prolonged awakenings (Table 1). These are widely recognized indicators of sleep efficiency and are commonly used in both clinical and research settings to identify sleep disturbances. Item 3 evaluates sleep duration, asking whether individuals obtain 7 to 9 hours of sleep per night, consistent with national recommendations from the Centers for Disease Control and Prevention and the American Academy of Sleep Medicine. Items 4 through 6 focus on sleep hygiene and environmental factors, including maintaining a consistent sleep schedule, reserving the bed for sleep-related activities, and sleeping in a quiet, dark environment. These behaviors are associated with improved circadian regulation and reduced sleep latency. Items 7 and 8 assess subjective sleep quality and daytime functioning, including feeling rested upon waking and maintaining alertness and focus during the day. These indicators reflect restorative sleep and are strongly associated with cognitive performance, mood, and overall health.
Summary of Dimensions: The Sleep Quality Screener measures all six major dimensions of sleep health:
• Regularity →Item 4
• Satisfaction →Item 7
• Alertness →Item 8
• Timing/Latency →Item 1
• Efficiency/Continuity →Items 2 & 5
• Duration →Item 3
It also includes behavioral / environmental measures via Item 6 (environmental control) and Item 5 (sleep hygiene practices), providing extra
clinical relevance.
The Sleep Quality Screener (SQS) incorporates a simple selfscoring system designed to facilitate immediate interpretation and user engagement. Each item is scored on a three-point scale (0=Never/Rarely, 1=Sometimes, 2=Often/Always), with total scores ranging from 0 to 16. Higher scores indicate more consistent engagement in health-promoting sleep behaviors. To enhance usability, the screener includes step-by-step scoring instructions that guide users to first total responses within each column and then calculate an overall score. This structured approach reduces confusion, supports accuracy, and allows individuals to independently complete the assessment without assistance, making the tool suitable for both clinical and community settings.
Score ranges are categorized into three intuitive levels: Poor Sleep (0-6), Fair Sleep (7-12), and Great Sleep (13-16). These categories provide immediate, easy-to-understand feedback that helps users contextualize their results without requiring clinical interpretation. In addition to numeric scoring, the screener includes brief, plain-language educational messaging (e.g., “Sleep Quality Matters”) that reinforces the importance of sleep for overall health. These messages are intentionally framed to promote self-efficacy and encourage small, achievable behavior changes. Rather than focusing on deficits, the feedback emphasizes that even modest improvements in sleep habits can lead to meaningful health benefits. This combination of self-scoring and supportive messaging transforms the SQS from a passive assessment tool into an active behavior change prompt. By providing immediate feedback and reinforcing key health concepts, the screener aligns with principles of the Health Belief Model and Self-Determination Theory, supporting awareness, motivation, and autonomy in health decision-making. This design allows the SQS to function as both a screening tool and a micro-intervention, bridging the gap between assessment and behavior change in real-world settings.
Tool Design and Usability
The SQS is designed for rapid administration, requiring fewer than three minutes to complete. Its low respondent burden makes it suitable for use in clinical waiting rooms, community health settings, and educational environments where time constraints are significant. The screener uses a simple response format and scoring system to facilitate immediate interpretation and feedback.
The tool is grounded in both public health guidance and behavioral theory. It reflects evidence-based sleep recommendations and aligns with constructs from the Health Belief Model, by increasing awareness of perceived risk and benefits, and Self-Determination Theory, by promoting autonomy and intrinsic motivation through self-assessment and personalized feedback. To support health literacy, all items are written in plain language using familiar terms (e.g., “fall asleep,” “wake up rested,” “quiet, dark room”). Supporting instructions and feedback messaging (e.g., “Sleep Quality Matters”) are designed to enhance understanding and empower individuals to make small, meaningful changes in their sleep behaviors.
Discussion
The SQS advances the concept of sleep as a lifestyle vital sign—a quick, universal assessment that makes sleep health visible in everyday practice. Like the RU-SATED, it prioritizes multidimensionality and patient-centered communication but uniquely integrates behavioral and environmental items suitable for population screening. In public health and clinical settings, the SQS can be used as a first pass sleep health check that can prompt deeper evaluation, within community wellness programs, or as part of behavior-change counseling to guide small, evidence-based actions (e.g., maintaining regular bedtimes, improving environment). Addressing disparities in sleep health— particularly among racial and socioeconomic groups—is a public health imperative. By being brief, free, and literacy-adapted, the SQS reduces barriers to assessment in underserved populations and aligns with Healthy People 2030’s Organizational Health Literacy objective [11]. A key strength of the SQS is its ability to function as both a screening tool and a micro-intervention, reducing reliance on clinician time while prompting immediate reflection and behavior change.
Implications for Practice and Public Health
The findings of this study have important implications for both clinical practice and public health. As highlighted in the Discussion, the Sleep Quality Screener (SQS) offers a practical approach to making sleep health visible and actionable within routine care and community settings. By combining brief assessment, immediate scoring, and plain-language feedback, the SQS enables healthcare professionals, educators, and public health practitioners to efficiently identify sleep-related behaviors and initiate meaningful conversations about sleep health.
In clinical and community environments, the SQS can be integrated into workflows as a first-pass screening tool that supports brief intervention and referral when appropriate. Its brevity and ease of use make it particularly well-suited for high-throughput settings such as primary care clinics, college health services, and community wellness programs, where time constraints often limit the ability to assess lifestyle behaviors comprehensively. As noted in the Discussion, this approach enhances opportunities to address sleep as a modifiable health behavior alongside other lifestyle factor.
From a public health perspective, the SQS supports broader efforts to address sleep as a determinant of chronic disease and overall well-being. Its standardized format allows for consistent measurement of sleep behaviors across populations, making it a useful tool for screening, program evaluation, and populationlevel surveillance. In addition, its emphasis on plain language and self-assessment aligns with national priorities such as the Healthy People 2030 objective on organizational health literacy, ensuring that individuals can understand and act on health information.
Importantly, the SQS extends beyond assessment by functioning as a brief, embedded intervention. As described in the Methods, the combination of self-scoring and supportive messaging encourages individuals to reflect on their sleep habits and consider small, achievable changes. This positions the SQS as a bridge between measurement and action, reinforcing its role as both a screening tool and a micro-intervention. By embedding behavior change principles directly into the assessment process, the SQS offers a scalable strategy to promote sleep health across clinical, educational, and community contexts.
Conclusion
The Sleep Quality Screener offers a practical, theory-based, and health-literate way to integrate sleep assessment into both public health and clinical practice. It operationalizes the call to treat sleep as a measurable, actionable vital sign—promoting awareness, prevention, and self-care across populations [4]. Future research will report on its psychometric properties against other sleep screeners and responsiveness to intervention [12].
Conclusion
Despite these potential limitations, the present authors believe that this research still has much to offer regarding the subject of being a “newbie” when it comes to living fulltime as a member of one’s affirmed gender. This study has demonstrated that being new to living full-time as a member of one’s affirmed gender is associated with higher levels of psychological distress and an increased risk for experiencing suicidal ideation compared to persons who have been living for a longer period of time as a member of their affirmed gender. While the finding for psychological distress was not robust enough to sustain in a multivariate analysis controlling for the effects of other key variables, the finding for suicidal ideation was robust. Structural equation analysis confirmed that the relationship between being a “newbie” and experiencing an elevated risk for suicidal ideation was a direct one. Importantly, this relationship remained significant even when controlling for the effects of other independent variables, including age. The main implication of this finding is that transgender people who are new or relatively new to living full-time as a member of their affirmed gender are at elevated risk for experiencing poor mental health outcomes and, therefore, constitute a group that is in need of targeted intervention and support efforts that can make their transition to be a smoother one.
References
- Buysse DJ (2014) Sleep health: Can we define it? Does it matter? Sleep 37(1): 9-17.
- Cappuccio FP, D Elia L, Strazzullo P, Miller MA (2010) Sleep duration and all-cause mortality: A systematic review and meta-analysis of prospective studies. Sleep 33 (5): 585-592.
- Scott AJ, Webb TL, Martyn St James M, Rowse G, Weich S (2021) Improving sleep quality leads to better mental health: A meta-analysis of randomised controlled trials. Sleep Medicine Reviews 60: 1-19.
- Hirschtritt ME, Walker MP, Krystal AD (2023) Sleep as a vital sign. Sleep Science and Practice 7(3): 1-5.
- Ravyts SG, Dzierzewski JM, Perez E, Donovan EK, Dautovich ND (2019) Sleep health as measured by RU-SATED: A psychometric evaluation. Sleep Health 5(4): 339-346.
- Centers for Disease Control and Prevention (2016) Prevalence of healthy sleep duration among adults—United States, 2014. MMWR Morbidity and Mortality Weekly Report 65(6): 137-141.
- Centers for Disease Control and Prevention (2021) Effect of inadequate sleep on frequent mental distress—United States, 2018. Preventing Chronic Disease 18.
- Centers for Disease Control and Prevention (2023) Prevalence and geographic patterns of self-reported short sleep duration among U.S. adults, 2020. Preventing Chronic Disease 20.
- Coelho J, et al. (2021) The RU-SATED is a short practical self-reported symptom scale that is a reliable valid tool for the rapid evaluation of sleep health. Sleep Medicine 90: 214-220.
- Li XL, Wei J, Zhang XY, Meng Z, Zhu W (2023) Relationship between night-sleep duration and risk for depression among middle-aged and older people: A dose response meta-analysis. Frontiers in Physiology 14: 1-10.
- Office of Disease Prevention and Health Promotion (2020) Healthy People 2030: Organizational Health Literacy. U.S. Department of Health and Human Services.
- Kotecki JE, Greene MA. Psychometric properties of the Sleep Quality Screener (Manuscript under review).






























