Isolation, Identification and Antibiotic Resistance of Pathogenic Bacteria Responsible for Childhood Pharyngo-Tonsillitis in Benin
Pamphile Aguessy1, SM Ismaël Hoteyi2, Durand Dah Nouvlessounon1, Victorien Dougnon3, Christine N’tcha1, Wassiyath Mousse1, Haziz Sina1, Adolphe Adjanohoun4, Lamine Baba-Moussa1*
1Laboratory of Biology and Molecular Typing in Microbiology, Department of Biochemistry and Cell Biology, Faculty of Science and Technology, University of Abomey-Calavi, 05 BP 1604, Cotonou, Benin
2Centre Béninois de la Recherche Scientifique et de l’Innovation (CBRSI), Cotonou, Benin
3Research Unit in Applied Microbiology and Pharmacology of Natural Substances, Research Laboratory in Applied Biology, Polytechnic School of Abomey-Calavi, University of Abomey-Calavi, Cotonou BP 526, Benin
4Institut National des Recherches Agricoles du Bénin (INRAB), Cotonou 01 BP 284, Benin
Submission: September 29, 2023; Published: October 12, 2023
*Corresponding author: Lamine Baba Moussa, Laboratory of Biology and Molecular Typing in Microbiology, Department of Biochemistry and Cell Biology, Faculty of Science and Technology, University of Abomey-Calavi, 05 BP 1604, Cotonou, Benin
How to cite this article:Pamphile A, Ismaël MS H, Durand Dah N, Victorien D, Christine N, et al. Isolation, Identification and Antibiotic Resistance of Pathogenic Bacteria Responsible for Childhood Pharyngo-Tonsillitis in Benin. JOJ Pub Health. 2023; 8(2): 555733. DOI: 10.19080/JOJPH.2023.08.555733
Abstract
Introduction: The term pharyngo-tonsillitis refers to inflammation and infection of the mucosa and lymphatic elements of the oropharynx: lymphoid structures and tonsils. It is common, especially in children. This work aimed to isolate, identify, evaluate the antibiotic resistance of pathogenic bacteria responsible for tonsillitis in children at the Padre Pio Humanitarian Health Center (CSVH) in Cotonou and at the Vallée de Grace Medical Clinic in Abomey-Calavi (CMVG).
Methods: To achieve the objective of this work, a prospective analytical and descriptive study was carried out at the CSVH and the CVGAB over a period of 12 months (July 2022 to June 2023). It included children aged 0-15 years old in whom the diagnosis of pharyngo-tonsillitis was made and the bacterial etiology confirmed after a throat swab were considered in this study. The variables age, sex, months, clinical signs, bacterial and fungal culture, antibiogram and treatment were considered.
Results: In total, 203 cases of pharyngo-tonsillitis out of 1206 consultations in pediatrics and ENT in the health facilities serving as the framework for the study, representing a prevalence of of 16.83%. Among the 203 cases of pharyngo-tonsillitis, the bacterial origin was confirmed with 99 cases, representing a proportion of 48.77%. The bacteria involved were: S. pyogenes (45.54%), S. aureus (21.78%), S. viridans (10.89%), S. pneumoniae (9.90%). The isolated bacteria were sensitive mainly to antibiotics in varying proportions: Ceftriaxone (70.43%), Cefixime (66.34%), Cefuroxime (57.43%) and Amoxicillin clavulanic acid (53.47%) and resistant to Erythromycin (60.40%). Antibiotic therapy was dominated by amoxicillin + clavulanic acid (29.91%) followed by the 3rd generation cephalosporins cefixime (29.91%) and cefuroxime (13.08%).
Conclusion: Bacterial origin represents 48.77% of pharyngo-tonsillitis with a predominance of S. pyogenes (45.54%) in Benin; this high rate is compatible with the probabilistic antibiotic therapy commonly used for pharyngo-tonsillitis in clinical practice where cytobacteriological examination is not easy.
Introduction
The term pharyngo-tonsillitis refers to inflammation and infection of the mucosa and lymphatic elements of the entire oropharynx: lymphoid structures and tonsils. That of tonsillitis considers inflammation localized at the level of the tonsils, pharyngeal, palatine and lingual [1-3]. Acute angina is one of the most common upper respiratory tract infections [4]. In Benin, the frequency of angina in children was 7.53% [5]. In Mali, pharyngo-tonsillitis represents 1.8% of pathologies encountered in ENT and constitutes the 3rd ENT infectious pathology after nasopharyngitis and otitis. This pharyngo-tonsillitis can generate complications which can be locoregional and/or general [6,7]. They are common among school-age children and young adults. The etiological diagnosis of angina is difficult based on clinical findings alone. Bacteriological examinations, in particular the culture of the throat swab, are necessary for a definitive diagnosis [8,9].
Pharyngo-tonsillitis is usually caused by viruses or bacteria; but the bacterial etiology is formidable due to its potentially serious complications (post-streptococcal syndromes: acute rheumatic fever (AAR), acute glomerulonephritis (AGN), and locoregional septic complications whose prevention justifies the implementation of antibiotic therapy usually probabilistic. They can be acute or chronic. They constitute a public health problem, due to their frequency, their recurrence, and their socio-professional and economic impact [10,11]. Pharyngotonsillitis has been the subject of little work in Benin. It is in this context that we decided to carry out our research work on the theme: bacteriological characteristics of pharyngo-tonsillitis, the objective of which was to isolate, identify, evaluate the antibiotic resistance of pathogenic bacteria responsible for childhood pharyngo-tonsillitis at the Padre Pio Humanitarian Health Center (CSVH) in Cotonou and at the Vallée de Grace Medical Clinic in Abomey-Calavi.
Material and Methods
Study centers
The study was carried out in three centers: The Vallée de Grâce Medical Clinic, the Padre Pio Humanitarian Health Center (CSVH) and the Laboratory of Biology and Molecular Typing in Microbiology.
Vallée de Grâce Medical Clinic (CMVG)
It is located in the Aidignon district, district of Togba, in the commune of Abomey Calavi, in the department of Atlantique in Benin. It is organized into several sections: reception, pharmacy, consultation rooms, hospitalization rooms, room, Maternity department, pediatric department, otorhinolaryngology and the laboratory. The laboratory has several units including Bacteriology/Parasitology, Serology, Biochemistry and Immunology.
Padre Pio Humanitarian Health Center (CSVH)
The CSVH Padre Pio is in the 6th arrondissement of Cotonou in the Akpakpa Dodomè district, Coastal Department. It is organized into several sections: reception, pharmacy, consultation rooms, hospitalization rooms, treatment room, sampling room, the Hepato-gastroenterology service, the pediatric services, Medicine, endocrinology, maternity, cardiology, obstetrics and gynecology, otolaryngology (ENT) and the laboratory. The laboratory also has several units including Bacteriology/Parasitology, Serology, Biochemistry and Immunology.
Laboratory of Biology and Molecular Typing in Microbiology
Located in the Department of Biochemistry and Cellular Biology of the Faculty of Science and Technology of the University of Abomey-Calavi, it is a research laboratory in Microbiology (clinical and food), Biochemistry, Molecular Biology and pharmacology of natural substances.
Methods
Prospective analytical and descriptive study was carried out for 12 months (from July 2, 2022 to June 31, 2023).
Sampling and variables analyzed
The patients who were sampled are children aged 0-15 years old in whom the diagnosis of pharyngo-tonsillitis was made in the ENT and pediatric departments of the sturdy health centers on the clinical arguments (fever, odynophagia dysphagia, hypertrophy and redness palatine tonsils and pharyngeal inflammatory signs, earache, and digestive signs) and the bacterial etiology confirmed after a cytobacteriological examination of the throat swab. Variables such as age, sex, months, clinical signs, bacterial characteristics and prescribed antibiotic treatment were studied.
Samples, cytobacteriological examination and identification
Throat swabs were taken by swabbing two tonsillar compartments and the posterior wall of the pharynx, using two swabs from patients diagnosed with pharyngo-tonsillitis in the study centers. The discharge was carried out in 2 ml of physiological water. The fresh state of the first slide covered with coverslip was carried out under a microscope, at low magnification (X10 and X40) to identify and quantify the represented elements (bacteria and leukocytes, red blood cells, yeasts). The Gram stain was read under a microscope using an X100 objective with immersion oil. The culture was carried out by inoculating each sample on Chapman agar, Muller Hinton agar, Eosin Methylene Blue agar and Blood Agar after having identified with the marker the petrie dish concerning these agars and incubating at 37°C. A staining of the Gram control was performed on isolated colonies. Then the identification was carried out using biochemical tests (catalase and cytochrome oxidase) or the LEMINOR gallery.
Susceptibility of Bacterial Isolates to Tested Antibiotic
To assess the antibiotic susceptibility of the isolated strains, we utilized the disc diffusion method, per the guidelines set forth by the Antibiogram Committee of the French Society of Microbiology. We utilized a range of antibiotics from Oxoid®, including Cefuroxime (CXM 30μg), Céfime (FIX 30μg), Erythromycin (ERY 30μg), Ceftriaxone (CRO 30μg); Amoxicillin + clavulanic acid (AMG 30μg)
Ethical aspects
This research protocol was approved by the Scientific Ethics Committee of the Doctoral School (Life Sciences) of the University of Abomey Calavi (UAC), Benin under number UAC/FAST/ EDSV/1562003 in accordance with national and local regulations. Likewise, all patients or their first-degree parents gave informed consent by verbal or written agreement and confidentiality was respected.
Data processing and analysis
Microsoft Excel 2019 spreadsheet was used for data processing and then subjected to a univariate or multivariate analysis of variance (ANOVA) using STATA 3 version 11.0 software.
Results
Patients sociodemographic characteristics
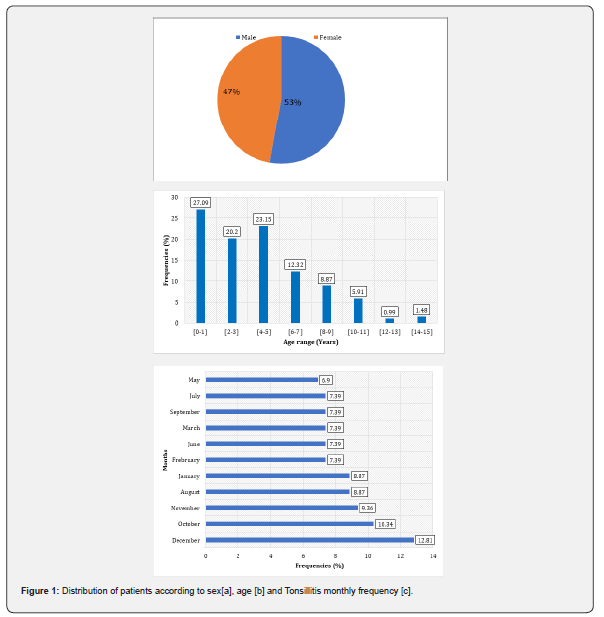
Information relating to sex and age was collected from 203 patients. Average rate of 47% are women compared to 53% men Figure 1a with a sex ratio of 1.11 in favor of the male sex. They belonged to age bracket from 3 months and 15 years with 7.24 ± 3 years as average age. The age group from 0 to 1 year is the most affected with 55 cases out of 203 representing the proportion of 27.09% Figure 1b. Regarding the engines frequency, pharyngotonsillitis is more frequent in December and October respective proportions of 12.81% and 10.34% Figure 1c.
Epidemiological and clinical and paraclinical aspects
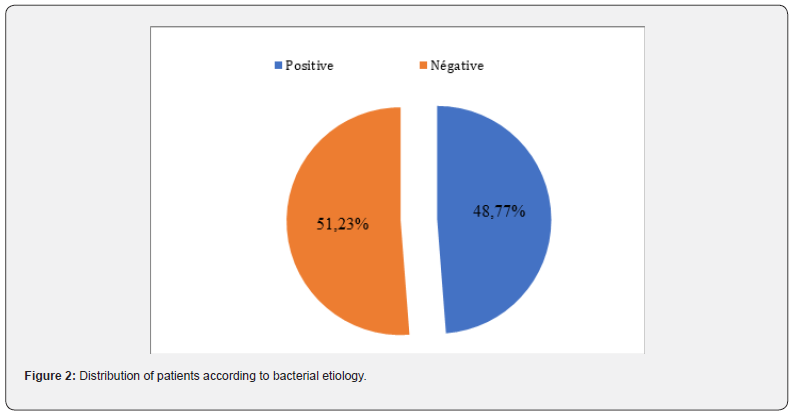
A total of 203 cases of childhood pharyngo-tonsillitis were recorded out of 1806 pediatric and ENT consultations in the study health centers, representing prevalence of 11.24%. Among the 203 cases of pharyngo-tonsillitis, the bacterial origin was confirmed in 99 cases, with a proportion of 48.77% Figure 2.
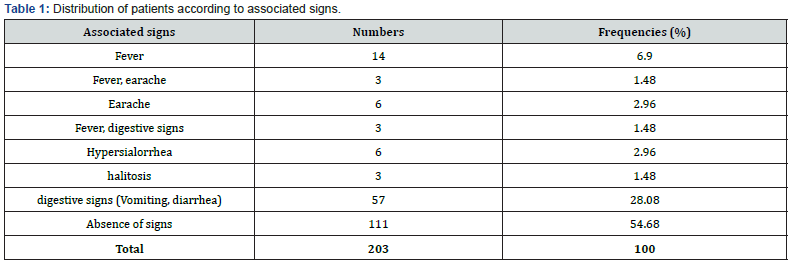
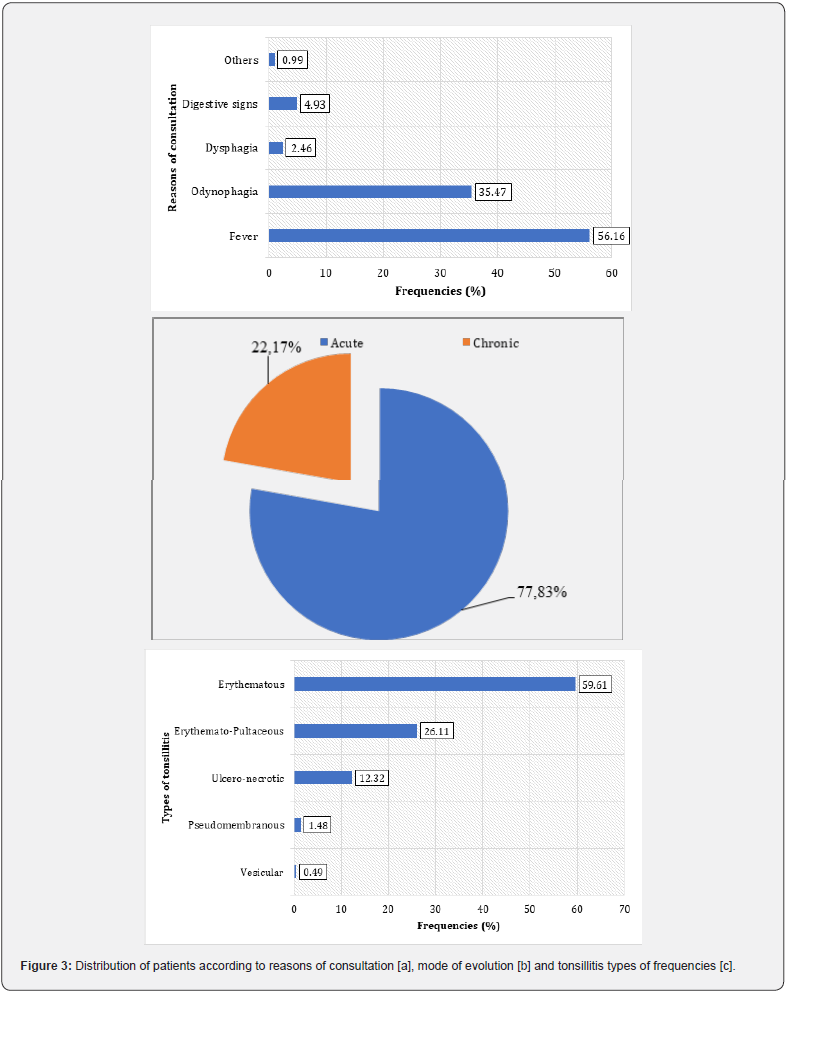
Regarding the reasons or clinical signs which accompany these cases of pharyngo-tonsillitis, we note that fever and odynophagia are the most frequent reasons of consultation with the proportions of 56.16% and 35.47% respectively Figure 3a. Furthermore, In addition to the reasons of consultation of pharyngo-tonsillitis, several signs have been identified with the patients. These signs include fever, earache, hypersialorrhea and halitosis individually or in combination. Indeed, digestive signs are the most representative (29.56%) of the associated signs followed by fever (9.86%) and earache (4.44%) Table 1.
Childhood pharyngo-tonsillitis can progress from acute to chronic form. The distribution of patients according to the mode of development shows that acute tonsillitis was observed with 158 patients, representing a proportion of 77.83% compared to 22.17% of chronic tonsillitis with 45 patients Figure 3b. Likewise among bacterial tonsillitis, several types have been identified in patients). Erythematous tonsillitis are predominant (59.61%), followed by erythematous-pultaceous (26.11%), ulcero-necrotic (12.32%) and vesicular in a small proportion (0.49%) Figure 3c.
Etiologically, several groups of bacteria involved in childhood tonsillitis were isolated and identified in varying proportions after cytobacteriological examination and culture of the patients’ throat swabs. These are S. pyogenes (45.54%), S. aureus (21.78%), S. viridans (10.89%), S. pneumoniae (9.90%), H. influenzae (7.92%), E. coli (2.97%) and K.. pneumoniae (0.99%) Figure 4a, 4b shows the resistance profile of the childhood tonsillitis isolated bacteria to the antibiotics used for the antibiogram. It should be noted a high resistance (60.40%) to erythromycin. The tonsillitis isolated bacteria were sensitive mainly to the following antibiotics: Ceftriaxone (70.43%), Cefixime (66.34%), Cefuroxime (57.43%) and Amoxicillin + clavulanic acid (53.47%).

Therapeutic aspects
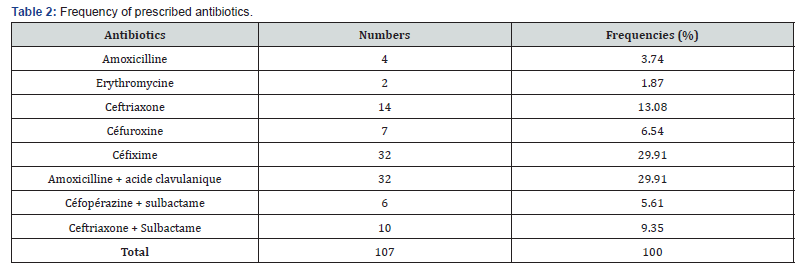
In the treatment of childhood pharyngo-tonsillitis, antibiotics are prescribed in 107 cases (52.71%) out of the 203 Table 2. The evolution was favorable towards clinical cure at the control on the 7th day in 92 cases out of 99 cases of bacterial pharyngo-tonsillitis or 92.92%. A 100% cure was obtained at the 14th day control under dual therapy.
Discussion
Epidemiological data of pharyngo-tonsillitis
Pharyngo-tonsillitis constitutes one of the main reasons for consultations in pediatrics and ENT in the health centers serving as the setting for the study with a prevalence of 11.24% and a bacterial proportion of 48.77% [5] found a prevalence of 7.53% among children aged 0 to 15 [12] had found a prevalence of 11% in India among children aged 0 to 5 years [13] in Mbouda found a prevalence of 9.84%. We note an increase in the frequency of childhood angina compared to the results of [5] in 2012 in Benin, which could be due to the ease of access to peripheral health centers. The frequency of 11.24% in our study is close to the work of [5,12-15] in Mbouda found bacterial etiologies of 38%, 44.59% respectively. 52.35% and 66.67%.
It appears that the high proportion of 48.77% for the bacterial origin of pharyno-tonsillitis in our study is compatible with the results of the aforementioned researchers. The climate of tropical regions like ours favors the development of bacteria. In our study, the sex ratio was 1.11 in favor of the male sex. Our result is compatible with those of [13] who reported a sex ratio of 1.14 with male predominance and [5] who also reported a sex ratio of 1.09 with male predominance. The average age was 7.24 years ± 3 with extremes between 3 months and 15 years. The age group of 0 to 1 year is the most affected with 55 cases out of 203, or a proportion of 27.09%. Children aged 0 to 5 years old were 70.44% in our study. The high representation of children aged 0 to 5 years is similar to the results of [5] who reported 57.86% for children aged 0 to 5 years in Cotonou.
Clinical aspects of pharyngo-tonsillitis
Acute tonsillitis was common (77.83%), this frequency is close to that of and [13] who found 75% and 80% of acute forms respectively. This frequency is higher than that of [5] who reported 45.99% of acute tonsillitis. Fever and odynophagia were the most frequent reasons for consultation with the proportions of 56.16% and 35.47% respectively. The proportion 35.47% for odynophagia is close to the 31.88% found by [5] and lower than the 100% of [13]. Erythematous tonsillitis (59.61%) was predominant, followed by erythematous-pultaceous (26.11%) and ulcero-necrotic (12.32%). [5] found 12.02% of erythematous tonsillitis and 33.44% of erythematous-pultaceous tonsillitis. Our frequency is higher for erythematous forms and close for erythemato-pultaceous forms to the results of [5].
Bacteriological aspects of tonsillitis
After cytobacteriological examination and culture of the throat swab, the bacteria isolated were: S. pyogenes (45.54%), S. aureus (21.78%), S. viridans (10.89%), S. pneumoniae (9.90%), H. influenzae (7.92%) E. coli (2.97%) and K. pneumoniae (0.99%). Therefore, S. pyogenes pharyngo-tonsillitis occupies first place among bacterial pharyngo-tonsillitis with a frequency of 45.54%. The frequency of E. coli (2.97%) in our study is lower than those of 6.66% and 10% found respectively by [5,16] in Cotonou. It should be noted that the frequency of Hemophilus influenzae (7.92%) is very close to that reported by [5]. The predominance of S. pyogenes (45.54%) is similar to the results of [13], with 45% and 43% respectively.
The predominances of S. pyogenes (45.54%) and S. aureus (21.78%) were also observed by Maachou et al. [16] who reported that the bacterial origin of pharyngo-tonsillitis was mainly due to 𝛽-hemolitic streptococci (43.3%) and staphilococcus (37.77%), Enterobecter (4.44%), and E. coli (6.66%), Enterococus (1.11%), streptococci pneumonia and 𝛼-hemolitic in the same percentage (2.22%). This study allowed us to differentiate the germs causing this disease in children in the Médéa region. Our results are similar in terms of types of bacteria isolated but different in proportion compared to the work of [5] who found Pneumococcus (28%), beta-hemolytic streptococcus (24%), Escherichia coli in the lead. (10%) and Pseudomonas aeruginosa (10%) and finally Hemophilus influenzae (8%).
Resistance profil of isolated bacteria
The isolated bacteria showed different degrees of sensitivity to beta lactams and macrolides. The isolated bacteria were sensitive to beta lactams (61.91%) mainly to the following antibiotics Ceftriaxone (70.43%), Cefixime (66.34%), Cefuroxime (57.43%) and Amoxicillin clavulanic acid (53.47%). It should be noted a strong resistance to erythromycin 60.40%. Our results are close to those of [13] who reported a sensitivity of 70% to beta lactams and in particular the association Amoxicillin with clavulanic acid 56 cases (93.33%), Cefotaxime (76.66%), Cefixime (73.33%) and Cefuroxime (70%). we also note a drop in the sensitivity of bacteria to Céfixime and Céfuroxime in our study compared to that of [13] in Mbouda in Cameroon.
Therapeutic aspects
In our study, the antibiotic prescription rate was 107 cases out of 203 or 52.71% for all forms of pharyngo-tonsillitis tonsillitis. The antibiotic therapy prescribed was dominated by amoxicillin + clavulanic acid (29.91%) and 3rd generation cephalosporins cefixime (29.91%) and cefuroxime (13.08). The results of [17] gave an antibiotic prescription rate of 72% for all forms of tonsillitis, therefore higher than ours. Our prescription rate (52.71% is close to the rate of 40% found by [13] lower than that of [17]. Systematic antibiotic therapy is questionable in regions where diagnostic tests Rapid tests are not available for consultation. This questionable attitude would favor the selection of new multiresistant bacterial strains..
Our results are close to those of [18-22] with respectively 31% and 26% prescription of amoxicillin clavulanic acid and far from the results of [13,15] for the same association. The evolution was favorable towards recovery in 92.92% of cases. This result is close to the 95% obtained by [13] and far from the 84.46% found by [5].
Conclusion
Pharyngo-tonsillitis has a prevalence of 11.24% and a bacterial proportion of 48.77%. The bacteria S. pyogenes (45.54%), S. aureus (21.78%) is the most prevalent. The bacteria involved are sensitive to beta-lactams and resistant to erythromycin. The cure rate was 92.92% for bacterial pharyngo-tonsillitis. Probabilistic antibiotic therapy is justified but questionable in view of inappropriate antibiotic prescriptions. In our context, etiological research by cytobacteriological examination of the throat swab must be carried out with the aim of limiting the selection of multiresistant bacterial strains.
Acknowledgement
We thank the patients and all other people encountered during this study for their openness and collaboration.
Conflicts of Interest
The authors declare that they have no conflict of interest.
References
- Berezin A (1980) Angines aigues. EMC Paris Oto-rhino-Laryngol 20500 AI0: 9:14.
- Strunski V (1993) Angines, Etiologies, diagnostic, Evolution, traitement. Rev Prat Paris 43: 2417-2420.
- Woolford TJ (2000) Spontaneous resolution of tonsillitis in children on the waiting list for tonsillectomy Clinical Otolaryngology 25(5): 428-430.
- Bingen E (2005). Résistance du streptocoque du groupe A aux macrolides. J Pediatr Puericult 18: 349–353.
- Chobl M, Yehouessi Vignikin B, Zoumenou E, Mensah E, Lawson LA, et al. (2012) Prise en charge des angines de l’enfant au CNHU de Cotonou RAMUR 17: 1-12.
- Diop M, Barry A, Camara E, Diallo M, Bangoura M, et al. (2020) Frequency of Group A Beta-Hemolytic Streptococcal Angina in Children in the Department of Pediatrics of Donka National Hospital Open J Pediatr 10(4): 610-616.
- Timbo SK, Keita MA, Togola FK, Traoré L, Mohamed AG (2006) Aspects Epidemiologiques de l’angine a Bamko. Mali Médical 4: 1-3.
- AFSS (1999) Agence Française de Sécurité Sanitaire des Produits de Santé. Angine aiguë. Med Mal Infect 29: 227–36.
- Kaplan EL, Top FH, Dudding BA, Wannamaker LW (2001) Diagnosis of streptococcal pharyngitis: differentiation of active infection from the carrier state in the symptomatic child J Infect Dis 123(5): 490-501.
- Bingen E (2005) Résistance du streptocoque du groupe A aux macrolides. J Pediatr Puericult 18: 349-353.
- Spilf HAS (2022) Haute Autorité de Santé et la Société de Pathologie Infectieuse de Langue Française.
- Vijayashree MS, Viswanatha B, Sambamurthy BN (2014) Clinical and Bacteriological Study of Acute Tonsillitis. IOSR Journal of Dental and Medical Sciences Volume 13(1): 37-43.
- Njifou AN, Zounon S, Ngaba GP, Vodouhé UB, Fedjo GT, et al. (2020) Les Angines Bactériennes à Mbouda: Aspects Cliniques et Thé Health Sci Dis 21(8): 72-75.
- Gehanno P, Portier H, Longuet P (1992): Le point actuel sur l'épidémiologie des angines aiguës et des syndromes post-streptococciques. Rev Prat Paris 42: 284-287.
- Haidara A (2014) Les amygdalites et leurs complications: aspect épidémiologique, clinique et thé Thèse de doctorat en médecine; Université des sciences des techniques des technologies de Bamako, Mali pp: 216.
- Maachou M, Seddar M, Telaidji M, Zergoug A (2022) Microbiologie Appliquée. Etude de l’Antibiorésistance des Germes Pathogènes Responsables des Angines Infantiles.
- Grijalva Cg, Nuorti Jp, Griffin Mr (2009) Antibiotic prescription rates for acute respiratory tract infections in US ambulatory settings. JAMA 302(7): 758-766.
- Bourrous M, Tassi N, Bouskraoui M (2009) Antibiotherapie des angines de l’ Esper med 16: 269-277.
- Romicka AM (2009) Streptococcal infection and antistreptolisine O Przegl Lek 66(1-2): 76-77.
- Maizia A, Letrilliart L, Colin C (2012) Stratégies de diagnostic de l'angine aiguë en France: une étude coût-efficacité. Presse Médicale 41:195-203.
- Cohen J, Levy C, Chalumeau M, Bidet Ph, Cohen R (2014) Rapid antigen detection tests for group A streptococcus in children with pharyngitis. Arch Pediatr 21(2): S78-S83.
- Maizia A, Letrilliart L, Colin C (2012) Stratégies de diagnostic de l'angine aiguë en France: une étude coût-efficacité. Presse Médicale 41: 195-203.






























