Baseline HIV Stigma Index Survey for St. Kitts and Nevis
Adegbenro Omotuyi John Fakoya1*, Angel M. Matos Lugo1, David Adeiza Otohinoyi2 and Ann Celestine1
1University of Medicine and Health Sciences, Basseterre, St. Kitts and Nevis
2Louisiana State University, New Orleans, USA
Submission: October 22, 2022; Published: November 18, 2022
*Corresponding author: Adegbenro Omotuyi John Fakoya, University of Medicine and Health Sciences, Basseterre, St. Kitts and Nevis
How to cite this article:Adegbenro Omotuyi John F, Angel M. Matos L, David Adeiza O, Ann C. Baseline HIV Stigma Index Survey for St. Kitts and Nevis. JOJ Pub Health. 2022; 7(2): 555707. DOI: 10.19080/JOJPH.2022.07.555707
Abstract
The stigma associated with AIDS is a setback for HIV/AIDS prevention, care, and treatment. Persons living with HIV/AIDS (PLWH), and those that fear they might be HIV-infected, fear judgment and discrimination from within their community, and more especially from their health care services. Thus, this study seeks to establish a baseline index of the stigma level for HIV in Saint Kitts and Nevis (SKN), as well as estimate this level among local health care providers (HCP). A total of 88 participants volunteered for the study, consisting of 43 PLWH and 45 HCP. Data from the PLWH was collected by trained physicians, while the HCP collected their data via a self-administered questionnaire. The results of the study reveal that the majority of PLWH had experienced stigmatization due to their health condition, either externally or internally, or both. The study revealed deficiencies in HIV-patient counseling and possible breaches of confidentiality regarding HIV status disclosure. However, the results of the study statistically showed an occupational bias concerning potential confidentiality breaches, as none of the skilled participants had their status revealed without their permission. This differed for the semi-skilled and unskilled participants. Amongst the HCP, the study revealed both passive and active displays of HIV stigma, attributed mainly to insufficient training. The study also revealed that HCP’s perception of their work environment in terms of safety negatively impacted their interaction with the PLWH. The results of this study underline the need for active participation from the SKN Community and Government, to ensure the quality of life for PLWH, as this could have a boomeranging effect on the health of the society as a whole.
Introduction
Human immunodeficiency virus (HIV) infection is classified as one of the world’s most significant public health challenges [1]. Globally, reliable data from the World Health Organization (WHO) and the joint United Nations Programme on HIV/AIDS (UNAIDS) have estimated a total of 31.1 – 43.9 million people living with HIV (PLWH). The Caribbean classified as the second most-affected region in the world after Africa, with an HIV prevalence of 1.6% [1,2]. As per a 2017 report from the Pan Caribbean Partnership against HIV/AIDS (PANCAP), the HIV epidemic in the Caribbean has been stable over the last 10 years, with a prevalence of 1.3% and an HIV incidence rate of 0.82 per 1000 population (PANCAP, 2018)[3]. Among the Caribbean nations, Haiti (48%), Dominican Republic (22%), Jamaica (10%), Cuba (8%), and Trinidad and Tobago (4%) account for 92% of HIV infections, with the other nations accounting for the remaining 8% [3].
There has been an impressive global commitment to both stopping new HIV infections, and to ensuring that PLWH have readily available access to treatment [2]. Although the global community has been focused on ensuring the availability of the needed antiretroviral drugs for an improved standard of living of PLWH, the detrimental effect of the associated stigma on PLWH also plays a significant role in their lifestyle [4].
Defined by Herek and Capitanio [5], HIV stigma is “the prejudice, discounting, discrediting and discrimination directed at people perceived to have AIDS or HIV, their loved ones and associates, and the groups and communities with which they are affiliated.” HIV stigma has a direct negative effect on the lifestyle of PLWH, especially when it concerns social interaction [6]. It can also affect their access to health care services when perpetrated by health care providers [4]. Studies have shown that HIV stigma from health care workers affected access by PLWH to antiretroviral drugs [7,8]. Studies completed in Grenada and Trinidad and Tobago, showed that stigma from health care providers resulted in marginal institutional practices to safeguard patient confidentiality [9].
HIV stigma can either be internally or externally perceived and experienced by PLWH or HIV-negative individuals [4]. Aside from that, the social understanding of individuals residing in the same community with PLWH also plays a significant role in the conceptualization of HIV stigma [5]. HIV stigma can be described in two major categories: felt and enacted stigmatization. Generally, enacted HIV stigma is classified as incidents of discrimination against PLWH; while felt stigma is the fear, real or imagined, of encountering enacted stigma [10]. It is generally accepted that enacted stigma may have a significant impact on felt stigma, yet felt stigma, although prevalent according to reports, can be premature and thus misleading for PLWH [11].
Synopsis of the Psychological Construct of HIV Stigmatization
The nature of the human mind is such that its development relies on the social stimuli it obtains, either through the discernment of societal attitudes or through personal experiences [5]. As a result, this can influence how individuals’ value, or devalue, an attribute or trait. Relegating conditions, such as HIV infection, to a devalued status has been observed as the primary source of negatively valenced beliefs [12]. Such views may affect an individual’s demeanor to the point of prompting them to discriminate against PLWH.
To fully conceptualize HIV stigma, a multidimensional approach is warranted. However, in this study, we will stick to a generally accepted point of view. Link and Phelan [13] described social context in four acts that could lead to the creation of stigma: labeling, stereotyping, grouping of individuals with a trait or attribute, and discrimination. The authors emphasized that the labeling of individuals most often arises due to societal influences, such as religion and culture, that are reinforced by formal and informal power structures. This, in turn, can induce stereotyping along the lines of the perceived differences. Devaluation thus spawns an out-grouping of PLWH from other members of the community. This will eventually lead to negatively valenced beliefs and attitudes, creating distance from the devalued characteristics of PLWH. Consequently, these out-grouped individuals are subject to stigma enactment through discrimination.
The caribbean context of HIV and HIV stigma
Little research has been done on the HIV stigma index in the Caribbean, with the majority of the studies restricted to the Windward Islands of the eastern Caribbean, such as Barbados, Grenada, and Trinidad and Tobago. However, there are a considerable number of studies focusing on the prevalence of HIV infection in the Caribbean.
The Caribbean consists of more than 40 million people spread over thousands of islands, thus rendering HIV/AIDS surveillance difficult [14]. With various degrees of postcolonial autonomy, and with African and East Indian influences spread across the Caribbean, the primary factor that maintains the region’s social conservatism is ‘religion.’ Religion is dominated in the area by Christianity, with other sizeable populations of Muslim, African spirituality, Judaism and Hinduism [15]. Pan American Health Organization (PAHO) reports indicating that HIV transmission is predominantly among heterosexuals [14]. However, social conservatism, largely facilitated by the role of religion, has resulted in widespread homophobia, the criminalization of homosexuality in the Caribbean, and even anti-gay violence. [16,17]. Consequently, it is believed that the data for HIV transmission among male homosexuals is underestimated.
The HIV stigma in the Caribbean has been classified similar to research done by Goffman (1963), where individuals with disabilities were ‘marked’ and given a ‘spoiled’ identity. In the Caribbean, PLWH are made to feel like ‘biohazards,’ contaminated, and untouchable. The influence from religion, coupled with the society proposes to the Caribbean communities that PLWH do not deserve care and compassion because they “brought the disease upon themselves” [17,18]. These predominant social attitudes have led to structural influences, further reinforcing the cultural responses, thus worsening the discrimination of PLWH [14].
HIV Stigma among health care providers in the caribbean
Health care providers (HCP) are responsible for the prevention and therapeutic management program for HIV infection. They are thereby in a position to significantly influence the increase or decrease of the social discourse about HIV/AIDS [19]. Therefore, the management of the HIV stigma index among HCP is essential to improving the standard of living of PLWH. Studies done between 1996 and 2001 showed that the HIV stigma level among HCP was high and could have impeded the availability of treatment [9]. Studies in Barbados, Grenada, and Trinidad and Tobago in 2007 showed that HCP directed most discrimination towards men who have sex with men (MSM) and intravenous drug users (IDU). Also, HCP who had to touch PLWH were more uncomfortable than HCP, who had direct contact with PLWH [9]. Another study carried out in Barbados showed that physicians who graduated from medical school before 1984 had fewer HIV/AIDS patients. They admitted having poor knowledge of the disease and were likely to carry out HIV testing without consent [20]. Similar studies done in Grenada, and Trinidad and Tobago, also revealed that efforts by HCP to safeguard patient confidentiality were not satisfactory [14].
With limited studies done on the HIV stigma index in the Caribbean, it is difficult to estimate the current level of stigmatization PLWH encounters. HIV stigma could lead to perceived low self-worth among PLWH, which could progress to depression. It could also lead to mental health issues, as well as problems with medication adherence, the latter being essential in PLWH. Anticipated stigma by PLWH may also affect social relationships leading to isolation and reduced social support participation. Overall, HIV stigma can negatively impact the standard of living for PLWH and even reduce their life expectancy [21,22]. Currently, there is no scientific report on the HIV stigma index for Saint Kitts and Nevis. This study aims to begin to fill that gap by conducting a baseline stigma index among people living with HIV, along with selected healthcare workers, in Saint Kitts and Nevis.
Material and Method
Sample Population
Saint Kitts and Nevis are a twin-island federation in the West Indies located, 17 20 degrees north, 62 45 degrees west. The islands have a combined area of 261 sq km (St Kitts 168 sq km, Nevis 93 sq km), and a tropical climate that is tempered with the constant sea breeze. As of July 2018, the islands have a total estimated population of 53,094. The religious distribution was estimated in 2001 to be: Protestant 74.4% (includes Anglican 20.6%, Methodist 19.1%, Pentecostal 8.2%, Church of God 6.8%, Moravian 5.5%, Baptist 4.8%, Seventh Day Adventist 4.7%, Evangelical 2.6%, Brethren 1.8%, other 0.3%), Roman Catholic 6.7%, Rastafarian 1.7%, Jehovah’s Witness 1.3%, other 7.6%, none 5.2%, unspecified 3.2%. The ethic composed (2001) is: African origin (92.5%), mixed (3%), white (2.1%), East Indian (1.5%), other (0.6%), unspecified (0.3%) [23].
Ethical Approval and Considerations
All portions of this study were approved by Saint Kitts and Nevis Interim Ethics Review Committee. To ensure the confidentiality of every participant, no information classified to be identifiable to anyone was asked. To maintain a high level of comfort in every participant, a guideline which provided consistency and minimized sensitivity feeling, was utilized.
Participant, Sampling and Procedure
In this cross-sectional study, HIV positive patients were enrolled from all the parishes on the main island and Nevis. To ensure accurate data collection, the inclusion criteria for participating physicians was: 1) sufficient information and practice in HIV/AIDS, 2) adequate understanding for filling out questionnaires, 3) responsibility, and 4) no substance addiction. These trained physicians assisted with data collection from the PLWH under the supervision of the principal investigator. Access to the primary care physicians of PLWH was approved and provided by the Ministry of Health for St. Kitts and Nevis. Patients considered for the study were those who had received HIV treatment from a Ministry of Health certified HCP. Also, the patient-inclusion criteria for the survey requested consent from the participants, determined adequate cooperation and understanding of the questionnaire, and specified the patient to be at least 18 years of age. In cases where patients could not physically appear, conversations with the physician via phone were adopted as the alternative means for data collection.
Unlike the approach for enrolling PLWH in the study, HCPs were recruited from the JNF General Hospital and other approved healthcare facilities. Formal approval was obtained from the hospital “Head of Operations” to administer the questionnaires to the HCP in the hospital. This enhanced smooth contact with the physicians, nurses and other socio-professional cadres. Participants were recruited via targeted enrolment methods, such as focused memos and broadcasted emails to HCP over the hospital email servers. Inclusion criteria for each volunteer HCP participant focused on those who were functionally providing care for PLWH, and other patients in general. Participants were then presented with a comprehensive self-administered questionnaire.
Measurement
To ensure each aspect of HIV stigma was captured, questions were grouped around each of the significant factors. These factors were defined as: experiences of stigma and discrimination and their causes, access to work, health and education services, internal stigma, rights, laws, and policies, effecting change, HIV testing and diagnosis, disclosure and confidentiality, treatment, and challenges. The questions were also verified by experienced physicians to ensure that each aspect of HIV stigma was screened. To measure the stigma level in the various sections of questions, we decided that if a patient experienced at least one of the questions asked in the external stigma section, it would be considered positive. Similar policy was applied to the questions in the internal stigma section. We also felt that due to the sensitive nature of the study we needed to provide a guide for our interviewers for consistency and confidentiality during data acquisition.
To further facilitate accurate data capture, several similar modalities were employed. The methodology used by Rutledge et al. [14] was reviewed and duplicated in our study with modifications. Our approach to assessing HIV stigma among HCP involved the combination of a mindfulness model of stigma with the component of Link and Phelan’s stereotyping, out-grouping (a combination of loss of status and separation) and discriminating. The questionnaire also captured prejudicial attitudes.
Data Analysis
We analyzed our data using STATA software package version 15 (Texas, US). Statistical significance cut-off was set at P ≤ 0.05. First, descriptive analyses were used to characterize the frequency with which participants reported a range of stigmarelated experiences. For descriptive purposes, items were coded as “agreed” or “yes” if responses were 3 (often) or 4 (sometimes). Second, Pearson’s chi-square analyses were used to identify health history and demographic variables associated with stigmarelated experiences. Also, the Kruskal–Wallis test (non-parametric method for testing) was used to compare as potential correlations between dependent and non-dependent variables.
Results
Baseline Characteristics on HIV Patients
In total, 43 HIV positive patients filled out the Stigma Index questionnaire through interviews. The participants were primarily male (Table 1). The predominant age groups were 31 - 35 years (15%) and 46 – 50 years (15%), while the mean age for the participants was 46 ± 13.6 years. Baseline analysis was performed for proper data interpretation (Table 1). The majority of the participants were employed full-time, 24 (58.5%). None of the participants were illiterate; most had high school diplomas, 25 (59.5%); others had an elementary school, 4 (9.5%); and a number had university degree certificates, 13 (40%). The dominant religion was Anglican and Methodist, 15 (37.5%). Among the participants who were homosexual or bisexual (Table 1), 100% were males, p=0.003.
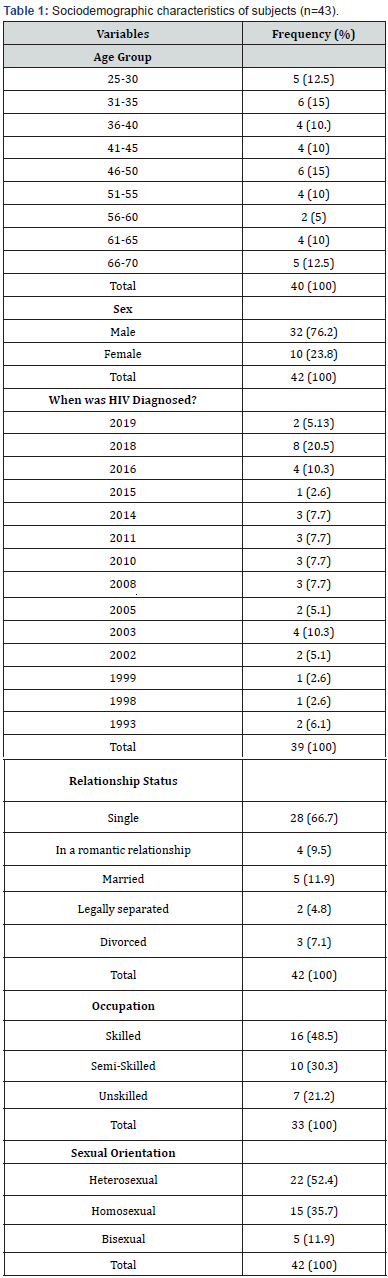
Baseline Characteristics on HIV Patients
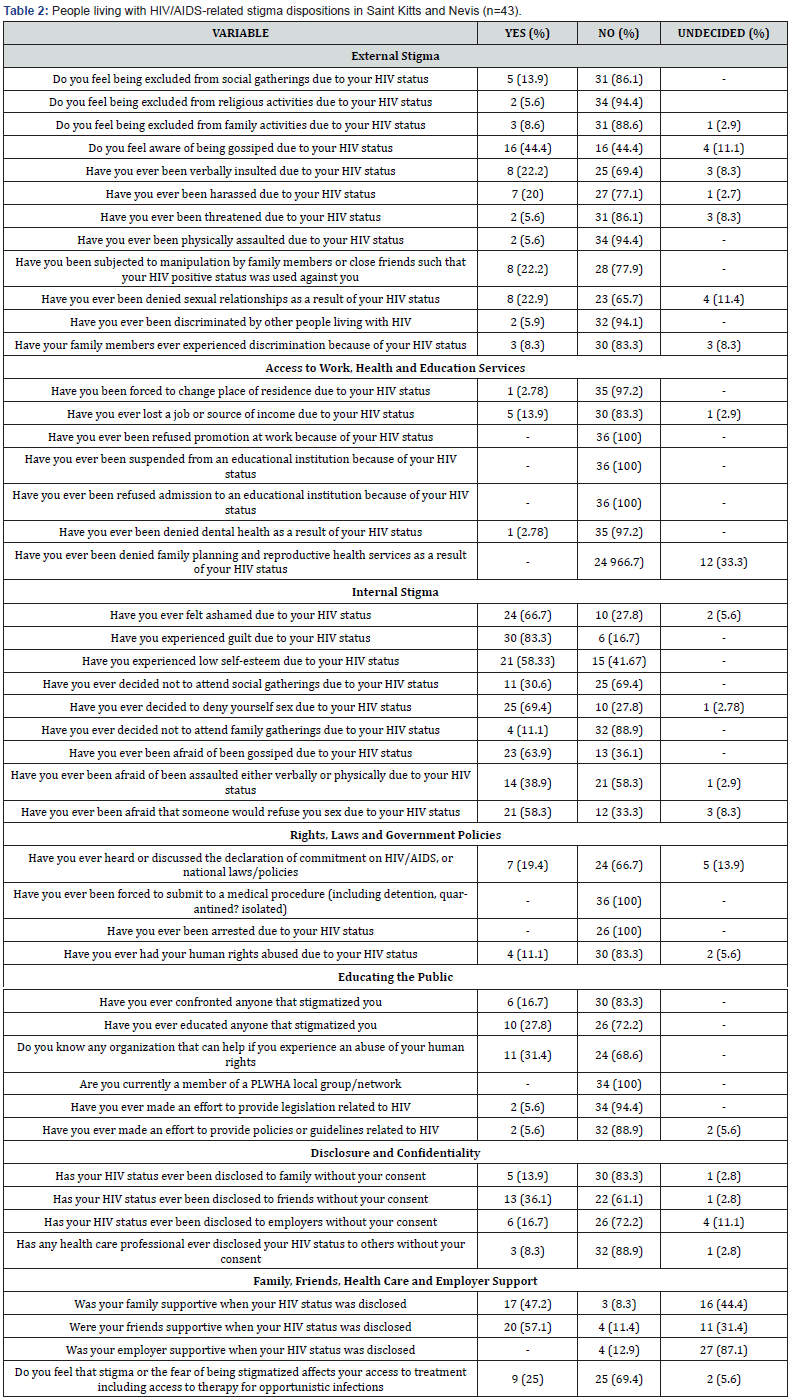
When asked why they were tested for HIV, 1 (2.6%) mentioned due to pregnancy, 16 (42.1%) were due to HIV like symptoms, 15 (39.5%) just wanted to know their HIV status, 4 (10.5%) were because their partner had tested positive to HIV, and 2 (5.3%) were due to incarceration. The majority, 33 (82.5%) stated they were tested voluntarily, while 4 (10%) reported they were pressured. A further 2 (5%) were forced, and 1 (2.5%) did not know they had been tested. Among these HIV positive patients participating in the survey, 20 (50%) had pre-and-post HIV Test counseling, 7 (17.5%) had only post, and 13 (32.5%) had no counseling. In order to have a good idea of the stigma index of the participants the questionnaire aimed to assess and tabulate the following: external stigma, issues with access to work and educational service, internal stigma, rights, laws and policies interaction, how PLWHA educate people, testing and diagnosis, and confidentiality (Table 2). A Kruskal-Wallis H Test showed a statistical significance between the participant’s occupation and those who had their HIV status revealed to friends without their permission, χ2(2) = 17.115, p = 0.0002. It showed that none of the skilled participants had their status revealed without their permission, while the opposite was exact for the semi-skilled and unskilled participants (p<0.05). Correlating access to healthcare with occupation was not statistically significant (p>0.05).
.
Baseline Characteristics on Health Care Providers
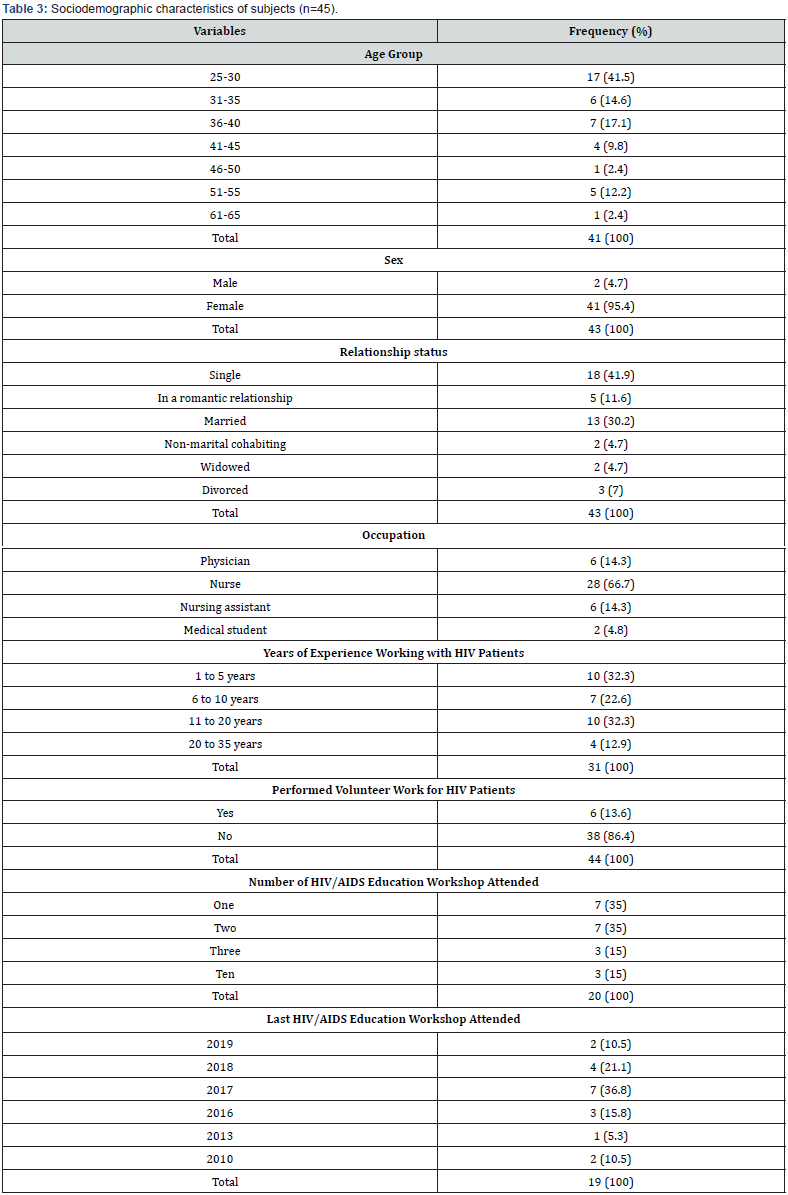
A total of 45 health care workers participated in the survey. The bulk of the respondents were within the age group of 25- 30 (41.5%) with a mean age of 35 ± 10 years. The demographic analysis was done to display the baseline characteristics of the respondents (Table 3). Among the participants, 43 (95.6%) were full-time employees, and 2 (4.4%) were unemployed. The majority of the participants acknowledged to be heterosexual, 36 (85.7%), while 1 (2.4%) classified as homosexual, 4 (9.5%) as bisexual, and 1 (2.4%) claimed celibacy. The predominant religions among the participants were Pentecostal/Evangelical, 13 (31%), and Anglican, 9 (21.4%). Another religion noted in the survey was Roman Catholic, 4 (9.5%), while 4 (9.5%) persons claimed no religion.
HIV Stigma Index among HCP
Only 29 (64.4%) claimed to have educated both HIV/AIDS patients and non-HIV/AIDS patients about HIV/AIDS. HIV/AIDSrelated stigma attitudinal profiles and item factor loading to assess the stigma index was tabulated for ideal data presentation (Table 4). Among the 20 participants that attended workshop training on HIV/AIDS, only 5 (25%) acknowledged performing volunteer work for HIV patients (p=0.04). Most of the participants that had 11 to 35 years of experience working with HIV patients had only gone for HIV/AIDS training once, p>0.05. A Kruskal-Wallis H test was, however, statistical significance for health care workers who were afraid to manage HIV patients and those who felt they were not trained to handle HIV patients, χ2(2) = 7.269, p = 0.0264. Nurses were the predominant group claiming insufficient training to manage HIV patients (p>0.05).
Discussion
HIV/AIDS is classified as one of the diseases that plague its host with both the ailment and the stigma. PLWH occasionally experience individual and institutional judgment, as well as a loss of status. The discrimination usually arises from multiple sources, such as neighbors, service providers, and religious leaders [13].
Since HIV stigma can afflict the standard of living of PLWH and reduce their life expectancy [21,22], our study was focused on identifying the stigma experienced by PLWH, and similarly assessing the HIV stigma that exists among HCP. A study done in Grenada and Trinidad and Tobago had revealed that HCP was judgmental towards PLWH, causing individuals to avoid testing or seeking medical treatment [14]. This study showed that 41% of HCP admitted their colleagues discriminated against PLWH, while 25% of PLWH reported that their fear of discrimination from HCP impacted their access to health care. This is a significant issue for the Caribbean [14,24,25]. Recommendations aimed at curbing this situation have revolved around the provision of proper training for HCP. In our study, 46% of HCP accepted not having enough training to handle PLWH, with 12% stating they were afraid to manage HIV patients.
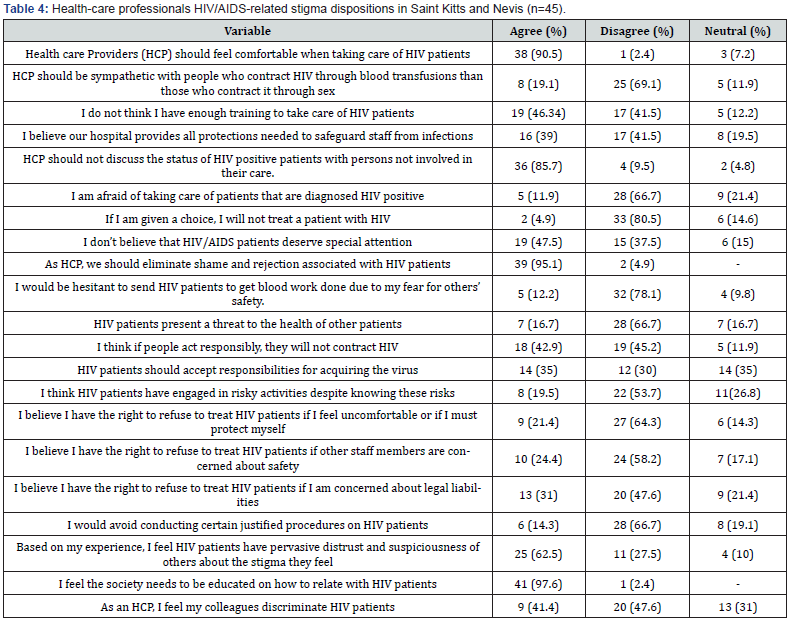
Our study also revealed that external (enacted) and internal (felt) stigma was 15% and 53%, respectively, among PLWH’s screened, thus positive in Saint Kitts and Nevis (Table 1). This finding is similar to other studies that have shown external and internal stigma affect how PLWH disclose their diagnosis for fear of resulting discrimination, thus impeding efforts to curb the spread of the disease [26]. Individual HCP efforts to curb the “non-disclosure-infection-spread” cycle could have led to some of the confidentiality breaches demonstrated in our study, wherein 18.8% acknowledged disclosure of their status without their consent. It has been shown that PLWH who do not inform their sexual partners and coworkers, end up creating an environment with an elevated risk of infection [14]. Of note, however, the Kruskal-Wallis Test revealed an occupational bias in the disclosure of patient HIV status. It showed that while none of the skilled participants had their status disclosed without their permission, this differed markedly for the semi-skilled and unskilled participants.
Our study also revealed that PLWH are not adequately informed on the commitment of the government to ensure an optimal standard of living for PLWH, amounting to an abuse of their human rights. This finding conforms with studies that showed PLWH frequently had their human rights violated by limiting their access to health care, healthy living, job employment, and other necessities [27]. A comparable study in Jamaica, reported in “Human Rights Watch,” was emphatic that the government should not remain silent about the prejudice that continues to weaken their legal policies designed for the expressed purpose of improving the standard of living of PLWH [28].
Studies investigating the mode of transmission have always identified homosexuals as being the predominant party responsible for disease transference [24]. Within the Caribbean nations, there has been a predominant incline in the number of HIV diagnoses among “men who have sex with men” (MSM). In our study, all reported homosexuals were men with no record of women, conforming with other studies done within the region [25]. A study done in Chicago showed that MSM, who were HIV positive experienced higher levels of discrimination. Considering the homophobic nature of most Caribbean nations, it will be expected that MSM will face an even higher degree of stigma here. It was further observed that MSM were more prone to sue individuals or organization in the event they felt their rights were violated [9,29].
Another issue affecting the stigma level experienced by PLWH is the lack of adequate and recommended counseling for patients. In this study, 32% of PLWH did not receive counseling, and 17.5% received only post-test counseling. This means that approximately 50% of the PLWH in care did not receive the recommended counseling. A significant reported hindrance to counseling is illiteracy [30]. Nevertheless, among the participants in our study none were illiterate, with the lowest level of schooling attained by the few with elementary education. HCP are required to deliver this recommended counseling. A primary reason why most HCP fail to fulfill this counseling obligation is due to their inadequate training on HIV/AIDS and HIV stigma. The counseling period provides the opportune time to introduce the patient to support groups and educate them about organizations that are available to assist them with HIV related stigma.
Consequently, our study revealed that about 69% were unaware of any organization that helped with HIV stigma, and a full 100% of PLWH screened in this study did not belong to any support group. As with any other chronic disease, the importance of a support group cannot be overemphasized. Mutual help and support among peers have been proven invaluable in facing and overcoming challenges related to the share condition. Hence, optimal and continuous counseling through the management phase is an effective and proven tool for assisting any patient that has tested positive for HIV.
Our study also disclosed that some of the PLWH were themselves trying to educate people about their condition to minimize discrimination, demonstrating how society still conceptualizes PLWH. This report was further confirmed with 97.6% of HCP attesting to the dire need for societal education about HIV and the repercussions of meted stigma on PLWH, as well as the consequential boomeranging societal health effect. The power held by religious leaders has been shown to have a significant impact on how the Caribbean society interacts with PLWH [9]. Across the geographical region, the peoples of the Caribbean are predominantly considered to adhere firmly to their religious convictions. Some religious leaders emphasize HIV/AIDS as “chastisement meted out by God.” Such edification can affect the public including HCP, and consequently how they interact with PLWH. The use of mass media interventions remains one of the leading solutions for reducing stigma on a large scale, suggesting that this mode of intervention targets behavior and social attitude. The use of electronic mass communication media, broadcasting new and up-to-date information on HIV/AIDS, can potentially be both efficient and effective due to scope and the repetitive, ongoing scale of the messaging. Also, personal experiences shared over mass media can impact the social behavior of people by educating them and instilling sympathy.
The HCP screened during the study, despite the majority possessing decades of experience working with HIV patients, acknowledged attending only one workshop on HIV/AIDS. Yet, routine training is a vital component for all HCP involved in the health services of PLWH, as is training on the emotional aspects of working with PLWH [20]. HCP need to understand the prejudices that affect PLWH as this impacts their relationship. Furthermore, with 39% of HCP stating the Hospital/VCT Center is ill-equipped to handle HIV patients, it stands to reason why some HCP remain fearful of working with PLWH, as shown by our study. These findings are consistent with other studies in revealing that the majority of HCP most often describe their place of work as unequipped to manage HIV patients [31,32]. In light of these findings, the government and community must commit to upgrading their healthcare facilities to ensure an ideal work environment for staff that makes possible the delivery of quality health care for all patients, regardless of their health status.
Study Limitations
The sample size in our study was small. Continuing the study over a longer period may have increased the sample size, but funding restraints made this impossible. Thorough, one-onone interviews may have afforded more in-depth exploration, nevertheless the study was constrained by the limited time for data collection. Focus groups and group dialogues, arguably ideal for acquiring data, were restricted due to stigma and confidentiality issues.
Conclusion/Recommendations
HIV infection remains a significant public health challenge. Attempts to improve the lives of PLWH are usually undermined by HIV stigma. HIV stigma erodes the standard of living of PLWH and potentially leads to further complications such as depression, low self-esteem, and avoidance of medical services. Studies done across the Caribbean have described a pronounced stigma index. With no previous report on the stigma index of Saint Kitts and Nevis, our survey was able to fill this gap by providing detailed information on the topic. Our study results underline the crucial and urgent need to manage HIV stigma among PLWH. Measures, such as setting up local support groups/networks, ensuring optimal HIV patient counseling, educating PLWH about laws protecting their rights, and sensitizing the public about HIV, should all be employed. Also, HCP requires routine training on how to manage and interact with HIV patients, which includes non-biased HIV status disclosure. Health care facilities should also be well equipped with materials for optimal patient care and safety. Additionally, the questionnaire reveals that a forum will be required to allow discussion around the term “special treatment” for PLWH, to allow debate on how to address potentially irresponsible activities that may fuel the spread of the virus, and to detail the rights of the HCP as relating to the management of PLWH.
Acknowledgment
The investigators would like to extend their appreciation to the initiators of this project, the Pan Caribbean Partnership Against HIV/AIDS (PANCAP) and the National Justice for All Programme, St. Kitts and Nevis. We acknowledge the valuable support of the Director of PANCAP, Mr. Dereck Springer, as well as the CMO, Ministry of Health, St. Kitts and Nevis, Dr. Hazel Laws. Thanks also for the assistance of Ms. Chereca Weaver, Dr. K. Liddie, Dr. M.G. Alexander, Dr. C. Kelsick-Hobson, Dr. B. Udo, Dr. O’Loughlin, Dr. M. Grant-Tate, Dr. B. Sahely, Dr. T. Drew, Dr. L. Richardson, Dr. J. Woodley, Dr. D. Archibald, and Dr. C. Franks. With special thanks going to Dr. K. Allen-Ferdinand, Dr. J. Nisbett, Dr. M. Laws, and their team, for their immense contribution. We appreciate the technical assistance provided by Antonio Grant, Charnelle McMaster, and Rochelle Harris of the University of Medicine and Health Sciences, St. Kitts and Nevis; Londyna Lennon, M & E, and Surveillance officer, St. Kitts and Nevis; the Head of operations, JNF Hospital, Dr. Cameron Wilkinson; and the Head of Nursing, JNF Hospital, Matron Sonia Daley.
Funding
This study was funded by grants provided by the PANCAP/ Global funds National Justice for All Programme and the Ministry of Health, St. Kitts, and Nevis. Contract number: CCS/OGC// PAN/2019/5/87.
Conflict of Interest
The authors declare no conflict of interest.
References
- UNAIDS (2018) Global HIV & AIDS statistics - 2018 fact sheet.
- WHO (2019) HIV/AIDS.
- PANCAP (2018) HIV and AIDS in the Caribbean – PANCAP.
- Wagner A, Hart T, McShane K, Margolese S, Girard T (2014) Health Care Provider Attitudes and Beliefs About People Living with HIV: Initial Validation of the Health Care Provider HIV/AIDS Stigma Scale (HPASS). AIDS Behav 18(12): 2397-2408.
- Herek G, Capitanio J (1998) Symbolic Prejudice or Fear of Infection? A Functional Analysis of AIDS-Related Stigma Among Heterosexual Adults. Basic And Applied Social Psychology 20(3): 230-241.
- Emlet C (2006) An Examination of the Social Networks and Social Isolation in Older and Younger Adults Living with HIV/AIDS. Health Soc Work 31(4): 299-308.
- Dong X, Yang J, Peng L, Pang M, Zhang J, et al. (2018) HIV-related stigma and discrimination amongst healthcare providers in Guangzhou, China. BMC Public Health 18(1): 738.
- Stringer K, Turan B, McCormick L, Durojaiye M, Nyblade L, et al. (2015) HIV-Related Stigma Among Healthcare Providers in the Deep South. AIDS Behav 20(1): 115-125.
- Abell N, Rutledge S, McCann, T, Padmore J (2007) Examining HIV/AIDS provider stigma: assessing regional concerns in the islands of the Eastern Caribbean. AIDS Care 19(2): 242-247.
- Lekas H, Siegel K, Leider J (2011) Felt and Enacted Stigma Among HIV/HCV-Coinfected Adults. Qual Health Res 21(9): 1205-1219.
- Henkel K, Brown K, Kalichman S (2008) AIDS-Related Stigma in Individuals with Other Stigmatized Identities in the USA: A Review of Layered Stigmas. Social And Personality Psychology Compass 2(4): 1586-1599.
- Berger B, Ferrans C, Lashley F (2001) Measuring stigma in people with HIV: Psychometric assessment of the HIV stigma scale. Res Nurs Health 24(6): 518-529.
- Link B, Phelan J (2001) Conceptualizing Stigma. Annual Review of Sociology 27(1): 363-385.
- Rutledge S, Abell N, Padmore J, McCann T (2009) AIDS stigma in health services in the Eastern Caribbean. Sociol Health Illn 31(1): 17-34.
- Inciardi J, Syvertsen J, Surratt H (2005) HIV/AIDS in the Caribbean Basin. AIDS Care 17(sup1): S9-25.
- Schleifer R (2004) Hated to death: homophobia, violence and Jamaica’s HIV/AIDS epidemic. Human Rights Watch 16(6): 1-79.
- Carr R (2003) On ‘judgment’: poverty, sexuality-based violence, and human rights in 21st century Jamaica. Caribbean Journal of Social Work 2: 71-87.
- Goffman E (1986) Stigma. New Jersey, United States: Penguin.
- Kang E, Rapkin B, DeAlmeida C (2006) Are psychological consequences of stigma enduring or transitory? A longitudinal study of HIV stigma and distress among Asians and Pacific Islanders living with HIV illness. AIDS Patient Care STDS 20(10): 712-723.
- Massiah E, Roach T, Jacobs C, St. John A, Inniss V, et al. (2004) Stigma, discrimination, and HIV/AIDS knowledge among physicians in Barbados. Rev Panam Salud Publica 16(6): 295-401.
- Turan B, Budhwani H, Fazeli P, Browning W, Raper J, et al. (2017) How Does Stigma Affect People Living with HIV? The Mediating Roles of Internalized and Anticipated HIV Stigma in the Effects of Perceived Community Stigma on Health and Psychosocial Outcomes. AIDS Behav 21(1): 283-291.
- Saki M, Kermanshahi MKS, Mohammadi E, Mohraz M (2015) Perception of Patients With HIV/AIDS From Stigma and Discrimination. Iran Red Crescent Med J 17(6): e23638.
- CIA (2019) Central America: Saint Kitts and Nevis -The World Factbook - Central Intelligence Agency.
- Figueroa J (2008) The HIV epidemic in the Caribbean: meeting the challenges of achieving universal access to prevention, treatment, and care. West Indian Med J 57(3): 195-203.
- Figueroa J (2014) Review of HIV in the Caribbean: Significant Progress and Outstanding Challenges. Curr HIV/AIDS Rep 11(2): 158-167.
- SeyedAlinaghi S, Paydary K, Afsar Kazerooni P, Hosseini M, Sedaghat A, et al. (2013) Evaluation of Stigma Index Among People Living With HIV/AIDS (PLWHA) in Six Cities in Iran. Thrita Journal of Medical Sciences 2(4): 69-75.
- Kohi T, Makoae L, Chirwa M, Holzemer W, RenéPhetlhu D, et al. (2006) HIV and AIDS Stigma Violates Human Rights in Five African Countries. Nurs Ethics 13(4): 404-415.
- Schleifer (2019) Hated to death: homophobia violence and Jamaica’s HIV/AIDS epidemic.
- Dowshen N, Binns H, Garofalo R (2009) Experiences of HIV-Related Stigma Among Young Men Who Have Sex with Men. AIDS Patient Care STDS 23(5): 371-376.
- Kontomanolis EN, Michalopoulos S, Gkasdaris G, Fasoulakis Z (2017) The social stigma of HIV-AIDS: society’s role. HIV AIDS (Auckl) 9: 111-118.
- Crowley T, Stellenberg E (2014) Integrating HIV care and treatment into primary healthcare: Are clinics equipped? Afr J Prim Health Care Fam Med 6(1): E1-7.
- Landis R, Abayomi E, Bain B, Greene E, Janossy G, et al. (2018) Shifting the HIV Paradigm from Care to Cure: Proceedings from the Caribbean Expert Summit in Barbados, August 2017. AIDS Res Hum Retroviruses 34(7): 561-569.






























