Fusobacterium Necrophorum Thrombosis of Cavernous Sinus
Noemí Fàbrega Ramon1,2,3*, Eugeni Joan Paredes Costa1,2, Júlia Siscart Viladegut2,4, Rosa Plana Bolba2,3, Mònica Solanes Cabús1,2 and José María Palacín Peruga1,2
1Centre d’Atenció Primària Onze de Setembre. Gerència Territorial de Lleida, Institut Català de la Salut, Barcelona, Spain
2Fundació Institut Universitari per a la recerca a l’Atenció Primària de Salut Jordi Gol i Gurina (IDIAPJGol), Barcelona, Spain
3Hospital Universitari Arnau de Vilanova de Lleida. Institut Català de la Salut, Barcelona, Spain
4Centre d’Atenció Seròs. Gerència Territorial de Lleida, Institut Català de la Salut, Barcelona, Spain
Submission: September 13, 2022; Published: October 14, 2022
*Corresponding author: Noemí Fàbrega Ramon, Centre d’Atenció Primària Onze de Setembre. Gerència Territorial de Lleida, Institut Català de la Salut, Passeig Onze de Setembre, 10. 25005. Lleida, Barcelona, Spain
How to cite this article:Fàbrega Ramon N, Paredes Costa JE, Siscart Viladegut J, Plana Bolba R, Solanes Cabús M, Palacín Peruga JM. Fusobacterium Necrophorum Thrombosis of Cavernous Sinus. JOJ Pub Health. 2022; 7(1): 555704. DOI: 10.19080/JOJPH.2022.07.555704
Abstract
Few cases in the English literature, 136 cases, have been reported of septic dural-sinus from different institutions. Septic thrombosis most frequently involves the cavernous sinuses, 96 cases (70%). Facial or sphenoid air sinus infection often precede cavernous-sinus disease. The most common early symptom is headache, fever and periorbital edema. Also drowsiness and diplopia related to III, IV and VI nerve palsies are present. The physical findings - Ptosis, proptosis and chemosis with papilledema. Complications are frequent, just 40% have a full recovery, 30% chronic sequelae, mostly oculomotor weakness and death means near 30%. We report an unusual case of Cavernous bilateral sinus Thrombosis (CST) in a 15-year-old child, produced by Fusobacterium Necrophorum septic sinusitis, diagnosed in the hospital Arnau de Vilanova de Lleida, Spain. The patient presented fever and persistent headache with no response to oral painkillers, moreover double horizontal vision in the left eye appeared. The blood analysis revealed increased leukocytes (14.930 cells/ml), high C reactive protein (256.9 mg/dL) with high d-Dimer (1422). The cerebrospinal fluid was transparent and sterile, with increased cellularity (251 cells/ml), hypoglycorrhachia 48 mg/dL (56% of glycaemia) and normoproteinorrhachia (55 mg/dL). Fusobacterium Necrophorum infection was confirmed by blood culture and the patient was treated with metronidazole, with a partially favorable response. The patient’s thrombosis of cavernous sinus was associated with the intracranial sepsis requiring a drainage surgery of all sinuses involved in the process. This case underlines the importance of magnetic resonance imaging, when a high clinical suspicion of cavernous thrombosis with clinica of double horizontal vision with elevated d-Dimer, and the benefits of early empirical treatment.
Keywords: cavernous sinus thrombophlebitis (CST), parameningeal reaction, Fusobacterium Necrophorum, morbidity.
Introduction
Thrombophlebitis of the cavernous sinus is a rare but serious disease that most often affects young adults and children. It is associated with significant morbidity or mortality and is often related to local infections of the head. The diagnosis is based on clinical findings and is confirmed by imaging. The Clinical manifestations- headache 52% is the most common early symptom and generally precedes fever 94% and periorbital edema 75%. Drowsiness 28%. Diplopia 12%. Physical findings - Ptosis, proptosis and chemosis 95%. III, IV and VI nerve palsies 88%. Papilledema 65%. Lethargy, coma 55%. Nuchal rigidity 40%. Seizures 9%. Hemiparesia 9%. The Laboratory findings show, peripheral WBC elevated in 91% cases, in CSF parameningeal formula 55%, CSF pressure elevated 52%. Radiological signs shows, CT scan abnormal in 40% and angiogram (carotid artery) 87% abnormal. The organisms associated with septic cavernous sinus thrombosis [2] reflect the primary sites of infections. Facial infections mean the 50% of the cavernous thrombosis, those involve nasal furuncles which are caused 70% by Staphylococcus aureus and nearly 20% by methicillin-resistant S. aureus (MRSA) which is increasing in frequency. Sinusitis (ethmoid or sphenoid) means the 30% caused mostly by anaerobics. Dental-tonsillar infections 9%, less commonly results in cavernous thrombosis, which are related with Pneumococus 5%, Gram negative 5% and just 4% anaerobics (2% Bacterioides spp and 2% Fusobacterium spp. Finally, otitis media causes 7% of the cavernous thrombosis.
Case Presentation
A previously healthy 15-year-old male adolescent presented at the medical center in Lleida, Spain, with a 2- day history of high temperature 39 °C, headache, odynophagia, cough with mucus expectoration, 99% of saturation, nausea, but no vomiting neither diarrhea. He presented TAR + of covid, and initiated treatment with analgesic and antipyretic treatment, to control the symptoms. After 10-days of symptomatic treatment, due to persistence of headache he decided to consult again, in the emergencies department for persistence of the headache. Now he reported progressive holocranial headache, with no other symptomatology. Firstly, the cefalea was responding to oral painkillers but refractory after the next 5 days of receiving the symptomatic therapy. The patient reported no previous episode of otitis, no toothache, no amigdalitis, nor any lesion in the orofacial area. Physical examination on admission revealed Glasgow coma scale (GCS) at 14/15, axillary temperature 38 °C and meningeal irritation with stiff neck (meningismus: Brudzinski +, Kernig -) and an altered neurological examination with palsy of the VI cranial nerve of left eye.
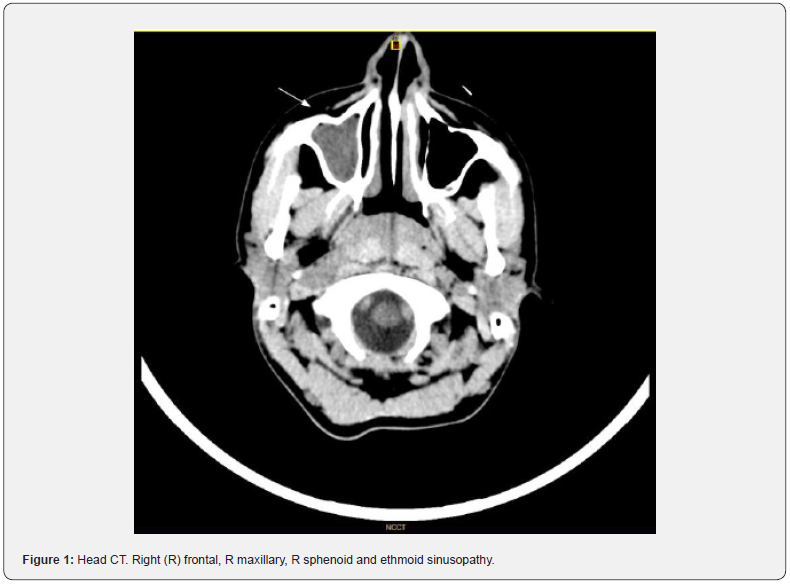
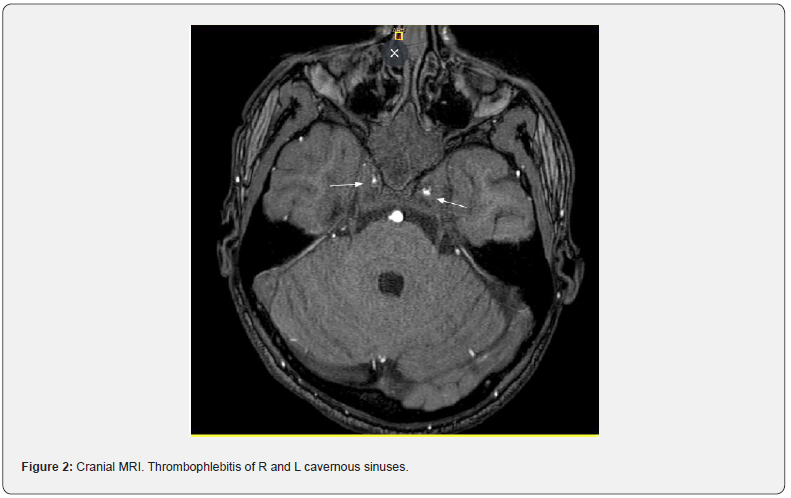
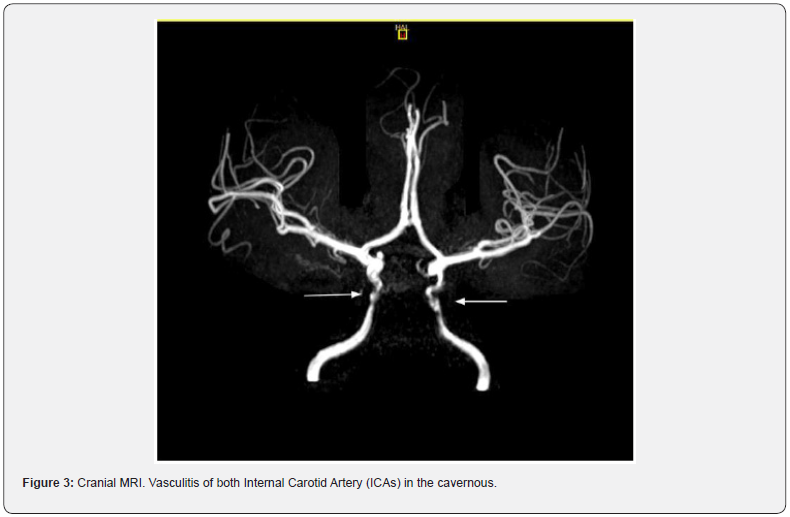
Laboratory studies showed 14.930/ml leucocytes (4500– 11000/ml), normal hemoglobin and platelet count, negative sedimentation rate and C reactive protein (256.9 mg/dL, reference value <3 mg/dL), d-Dimer 1422, no renal dysfunction and normal transaminase values. Cerebrospinal fluid (CSF) analysis showed pleocytosis (251 cells/mL with polymorphonuclear predominance; reference value <10 cells/μL), hypoglycorrhachia 48 mg/dL (56% of glycaemia, reference value ≥60% of glycaemia) and normal proteinorrhachia (55 mg/dL; reference value ≤45 mg/ dL). Multiple PCR in CSF was negative of: Toxoplasma gondii, E.coli K1, H.influenzae, L.monocytogenes, N.meningitidis, S.agalactiae, S.pneumoniae, Enterovirus, Parechovirus, Virus herpes simple 1 i 2, Virus herpes 6, Cytomegalovirus and Varicela-Zóster, DNA of M. tuberculosis complex, PCR covid test coronavirus SARS-CoV-2 (nasopharyngeal and CSF). No organism observed in the gram staining. The cultives aerobic and anaerobic of CSF were negative and Fusobacterium Necrophorum was isolated in blood cultures. Then, metronidazole lead antibioterapia was initiated. Moreover, prophylactic heparin was initiated due to an increase of d-Dimer (1843). Head CT (Figure 1) showed right frontal inflammatory sinusopathy, right maxillary, right sphenoid and right ethmoid sinusopathy. Supra aortic trunks ultrasound normal. The MRI showed right frontal and sphenoid sinusitis, associated with: Thrombophlebitis of both cavernous sinuses (Figure 2). Signs of vasculitis in the cavernous segments of both ICAs (Figure 3), with stenosis and minimal hyperacute/acute infarcts in territory of internal border and posterior right cortical border, probably secondary to hypoperfusion. Signs of leptomeningitis in the right fronto-parietal convexity, and in the parieto-occipital parasagittal right region.
The patient evolved partially favorably with metronidazole + prophylactic heparin therapy, with c-RP and DD levels going down, though fever and symptoms still persisted. The surgical drainage of sphenoid sinus infection was performed without any complication. He presented sequelae with partial diplopia of the left eye, which improved being totally recovered nowadays.
Treatment
Recommended treatment for anaerobics (Fusobacterium Necrophorum) infections is metronidazole 500 mg/6-8h during 6 weeks (2 weeks iv, later 4 weeks ov). Due to hepatotoxicity, after the 2 weeks of iv antibioterapia, it was changed to clindamycin 600mg/ 8h vo for 4 weeks more. Endoscopic nasosinual surgery bilateral with surgical drainage of sphenoid sinus infection was performed without any complication. Moreover, prophylactic dose with heparin 40.000 U. Later, the therapeutic dose 1mg/ kg/12h of heparin, which changed to oral anticoagulation therapy with anti vit. K anticoagulation (Sintrom 4 mg, 15 mg/week) during 6 months. Afterward, it was changed to acetylsalicylic acid (Adiro 100mg/24h). Double therapy with metronidazole and prophylactic heparin were ineffective as observed in this case. Triple therapy: antibiotic + anticoagulation + surgery with sinus drainage, is required.
Conclusion
Although cavernous sinus thrombophlebitis (CST) [3] tends to be increasingly rare, it remains a dramatic and lethal complication of sinusitis. Mortality from CST remains high between 20% and 30%. Early recognition and appropriate treatment is necessary to improve mortality and morbidity of this potentially fatal disease. Management of CST should include wide spectrum antibiotics and drainage of the primary site of infection. The role of anticoagulation is still debated, although some reports have shown some favorable response, mostly in one side cavernous sinus thrombophlebitis to prevent bilateral sinus thrombophlebitis.
References
- Tamayo DAA, Martín AB, Fernández DC, Dias MM, Deck M et al. (2020) Cavernous sinus syndrome secondary to thrombophlebitis due to Streptococcus intermedius complicated with vasculitis of the internal carotid artery and brain abscesses. Rev Neurol 70(1): 19-22.
- Plewa MC, Tadi P, Gupta M (2022) Cavernous Sinus Thrombosis. Stat Pearls Publishing LLC, St. Petersburg, Florida, United States.
- Mohamed B A, Shimi A, Khatouf M (2013) Cavernous sinus thrombophlebitis complicating sinusitis. Am J Case Rep 14: 99-102.






























