Need for Sustained Donor Funds to Maintain Health Services in Afghanistan
Najibullah Safi1*, Palwasha Anwari2 and Helah Safi3
1The University of Suffolk, Ipswich, the United Kingdom
2London School of Hygiene and Tropical Medicine, London, the United Kingdom
3CDC Foundation, Atlanta, USA
Submission: September 21, 2022; Published: September 26, 2022
*Corresponding author: The University of Suffolk, Ipswich, the United Kingdom
How to cite this article:Najibullah S, Palwasha A, Helah S. Need for Sustained Donor Funds to Maintain Health Services in Afghanistan. JOJ Pub Health. 2022; 7(1): 555703. DOI: 10.19080/JOJPH.2022.07.555703
Introduction
Afghanistan is a landlocked country located in South Asia and has a population of approximately 38 million [1]. Traditional medicine has an ancient history and it was the only treatment practice until the early 20th century [2,3]. The first group of Afghan doctors was trained in Turkey in the 1920s [4]. The physician assistant program and the first medical college were established in 1931 and 1932, respectively [5]. Throughout the 1960s, the health system was limited to a few hospitals in large urban areas. After the Ex-Soviet Union invasion in 1979, non-governmental organizations (NGOs) initiated cross-border activities in rural areas. Overall, the country had a fragmented health system until 2001.
After the fall of the Taliban in 2001, the government of Afghanistan introduced a new health care delivery model with financial support from United State Agency for International Development (USAID), European Union (EU), and the World Bank (WB) [6]. The Basic Package of Health Services (BPHS) and the Essential Package of Hospital Services (EPHS) were developed in 2003 and 2005, respectively. The BPHS provides primary healthcare and preventive health services, whereas the EPHS consists of hospital-level services and provides referral support to BPHS facilities [7,8]. Health services are provided through a network of around 3,500 health facilities, which include sub-health centers, basic health centers, comprehensive health centers, and district and provincial hospitals. District hospitals have the elements of both categories of services. Besides these two packages, there is another group of national hospitals for specialized tertiary care and training of medical doctors through different residency programs. In 2019, the country spent 2.8 billion dollars on health, out of which 20% was provided by key donors, 77% out-of-pocket expenditures by people at the point of service delivery, and only 3% by the government [9].
The health services are contracted out to NGOs, and there are eleven indicators linked with the payments of NGOs. In this brief review, we are only focusing on the impact of recent political transition on these eleven key performance indicators [10].
After the collapse of the government on August 15, 2021, the key donors of the health system paused their funding to Afghanistan. The sudden halt of health services, one of the basic human rights, exposed Afghans to extreme vulnerability [11]. Following Taliban takeover, they declared that women were not allowed to travel more than forty-five miles without a mahram (unmarriageable male kin or husband). Such restrictions on the movements of women created excessive barriers to access and utilize health services for females and children, as over 10% of the population had to travel more than two hours, and another half of them had to travel over 30 minutes to reach a health facility [12].
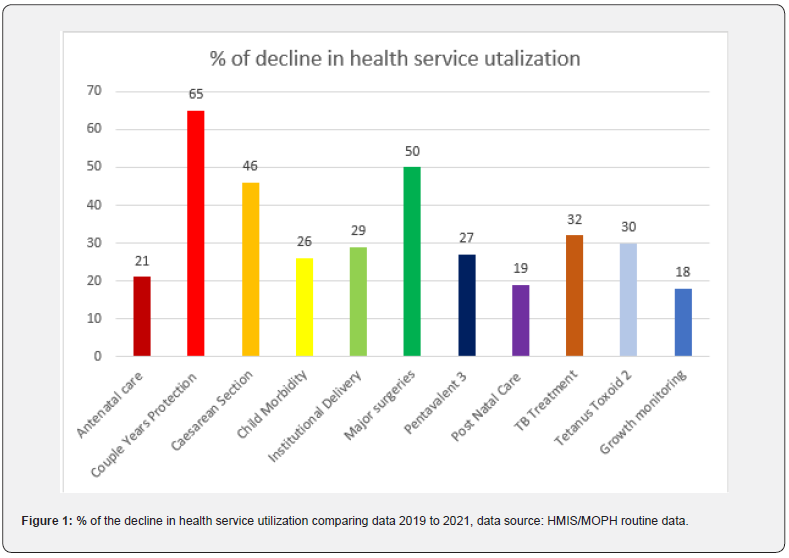
We compare the data for the same period of 4 months (July - October) over three years (2019-2021). The data is collected by NGOs and complied by the Ministry of Public Health (MoPH) using the DHIS2 platform (Figure 1).
The comparison of key indicators confirms that the recent political changes affected the health of women and children. However, the situation improved after bridging funds by the Global Fund to Fight HIV/AIDS, TB, and Malaria (GFATM), and United Nations (UN), and WB.
In October 2021, we proposed an alternative model for health services delivery in Afghanistan. The major purpose was to sustain basic health care, prevent catastrophic disasters due to outbreaks of communicable diseases, and ensure access to quality care across the country [11]. At the same time, our model proposed an alternate financing arrangement to align with the ban on the access of de-facto authorities to health funds. However, all funds to finance BPHS and EPHS were channeled through the government of Afghanistan before August 15, 2021. We proposed the establishment of project management units in WHO and UNICEF, to manage donor funds and ensure continuity of health services with adequate transparency and accountability. Fortunately, the WB agreed to support an emergency health program for 24 months through UNICEF [13]. In addition, the EU, USAID, the Asian Development Bank (ADB), and other key donors reinitiated their support for the health system through UN agencies and a few international NGOs. All the activities related to health services provision are coordinated with de-facto authorities at national and sub-national levels. All these arrangements will help in sustaining the health care delivery in Afghanistan. However, restrictions on the movement of women will negatively affect the health of mothers and children across the country [14].
Considering the ongoing sanctions on the country, growing restrictions on women’s mobility, education, constant brain drains of health professionals, growing unemployment, cash flow crisis due to restrictions on the banking system, and increasing poverty, it is crucial to ensure donor support for the continuation of health services in Afghanistan for coming years. Leaving these services neglected leads to unforeseen consequences, not only for Afghans but also for the region and the rest of the world.
References
- Afghanistan-Statistical-Yearbook-first-Version.
- COUNTRY PROFILE: AFGHANISTAN. 46f9133b0.pdf.
- Research Publications. Afghanistan Research and Evaluation Unit Organization. 2020.
- Najibullah Safi Afghanistan health care system.
- History of KUMS | KUMS.
- Acerra JR, Iskyan K, Qureshi ZA, Sharma RK (2009) Rebuilding the health care system in Afghanistan: an overview of primary care and emergency services. Int J Emerg Med 2(2): 77-82.
- Newbrander W, Ickx P, Feroz F, Stanekzai H (2014) Afghanistan’s Basic Package of Health Services: Its development and effects on rebuilding the health system. Glob Public Health 9 suppl (Suppl 1): S6-28.
- The Essential Package of Hospital Services for Afghanistan.
- Afghanistan National Health Accounts with Disease Account 2019.
- Sehatmandi Project | Ministry of Public Health.
- Safi N, Singh LS, Naseri S, Anwari P (2021) An alternative model for health service delivery in Afghanistan. Lancet 398(10310): 1481-1482.
- Chantelle Lee. What is the status of healthcare for women in Afghanistan under the Taliban? Frontline Newsletter August 2022.
- Afghanistan Health Emergency Response (HER) Project.
- Anwari P (2022) A year on from the Taliban takeover, what is the state of the health system in Afghanistan?






























