Perspectives on Collaboration and Community Partnership in Improving Health Outcomes
Diane Smith* and Maureen Pettitt
Washington State University, Burlington
Submission: January 08, 2022; Published: January 21, 2022
*Corresponding author: Diane Smith, Washington State University, Burlington
How to cite this article:Diane S, Maureen P. Perspectives on Collaboration and Community Partnership in Improving Health Outcomes. JOJ Pub Health. 2022; 6(4): 555692. DOI: 10.19080/JOJPH.2022.06.555692
Abstract
People working together in effective collaboration is necessary to realize improvements in today’s rapidly changing health care landscape. In Skagit County, the Population Health Trust (PHT) was established through an intentional process of building a coalition of community members, agencies, and public health with a shared vision and commitment to improve community health. The perspective presented in this review describes best practices followed in building a collaboration to move the dial on community health beyond clinical care to address determinates of health. Next steps in the process are informed by PHT member feedback and lessons learned.
Keywords: Availability; Accessibility; Communicable Diseases; Prevention Health Care Services; Sustainable Development Goal 3; Utilization
Abbreviations: Collaboration; Culture of Health; Health Care Access; Social Determinates of Health; Community Partnership
Introduction
The Population Health Trust (PHT) is a board of community leaders with a shared commitment to improve the quality of life for everyone in Skagit County. This partnership, referred to as PHT members, was formalized by the Skagit County Board of Health to advise on issues that can improve the health and wellness of all. The PHT followed an intentional process of building a coalition of community partners with the shared commitment to improved health, and to rethink and reshape the traditional perspectives of community health. This cross-collaboration exemplifies an evolutionary shift from clinical care to a more comprehensive view of community health which includes the social determinants of health. Determinates of health include a range of personal, social, economic, and environmental factors within the community with the recognition that only a small percentage of personal health and well-being is related to clinical care [1]. This paper describes the origins of the organization, the role of community collaborations, the organizational and assessment processes followed by the PHT, and how the organization has evolved to be more effective based on member feedback and lessons learned.
Skagit County, Washington
Skagit County is a rural community located in the northwest corner of Washington State. Situated between the Puget Sound and the Cascade Mountains, County residents enjoy a bucolic setting framed by an agriculture corridor and blessed with an abundance of outdoor activities. While best known for its agriculture, manufacturing accounts for one-third of the County’s GDP. Of the 123,700 residents, 20% are over 65 years, 22% are under 18 years, and 18% identify themselves as Hispanic or Latino. An estimated 15% of the county’s residents live in poverty [2]. The quality of life in Skagit, as measured by health outcomes in the Robert Wood Johnson Health Rankings, reflects a community ripe for initiating health improvement strategies. Since 2010, Skagit County has consistently ranked between 9th to 16th among the overall health outcomes of length of life and quality of life among the 39 counties in Washington. However, Skagit County has ranked between 17th and 23rd in overall health factors social and economic factors, physical environment, clinical care and health behaviors among Washington counties [3].
Collaborations: Definition and Models
Cross-sector collaborations offer greater potential for collective impact through maximizing resources, developing sustainable outcomes, and engaging a wider community ownership and commitment [4-6]. Posited that it is critical for collaborative efforts to move from problem driven to vision driven, from muddled roles and responsibilities to defined relationships. In particular, moving from problem-driven activities to vision-driven solutions offers greater potential for maximizing resources, developing sustainable outcomes and greater community ownership, and commitment to courses of action [7]. Defined collaboration as “a mutually beneficial and well-defined relationship entered into by two or more organizations to achieve common goals. The relationship includes a commitment to mutual relationships and goals; a jointly developed structure and shared responsibility; mutual authority and accountability for success; and sharing of resources and rewards” (p. 39). The authors identified factors, grouped into six categories membership, process and structure, communications, environment, purpose, and resources that influence the success of collaborations. These factors provide the framework for our discussion of the current PHT structure and efforts in Collaboration Success Factors section below.
Emergence of the Population Health Trust
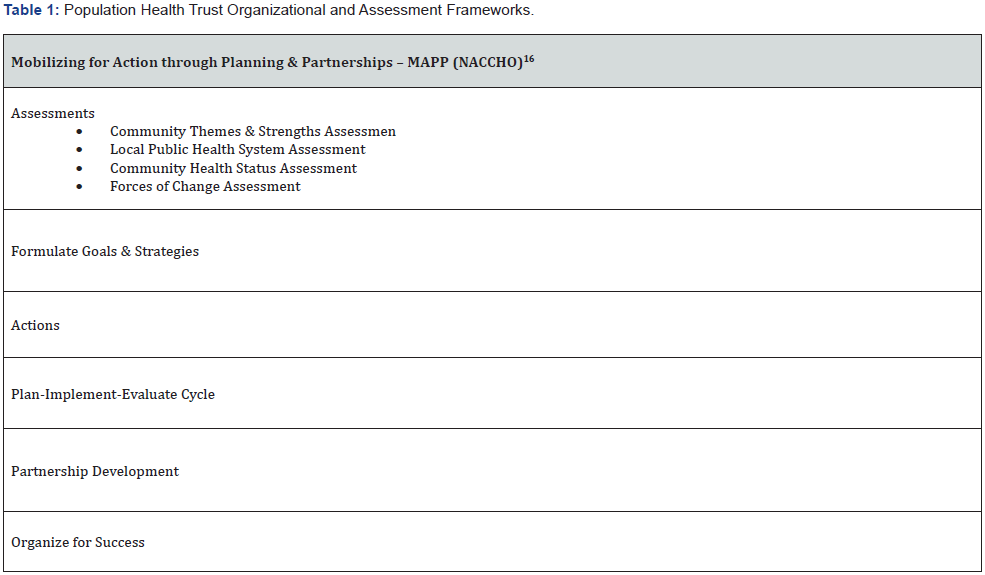
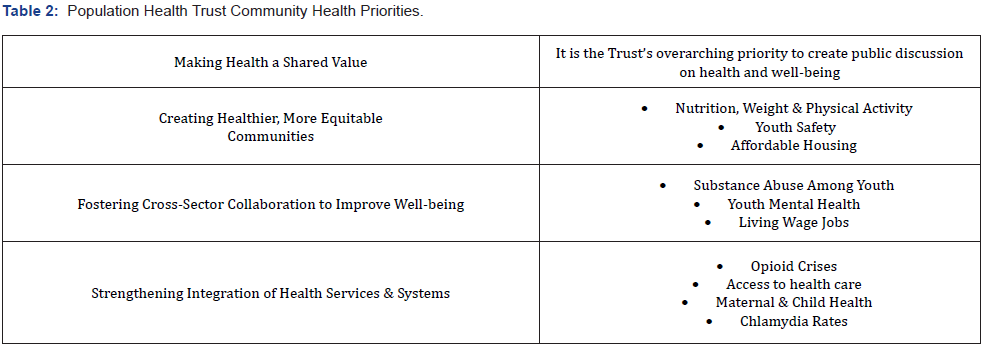
In the two years prior to the creation of the PHT, there were two community partnerships with a vested interest in population health in Skagit County: the Skagit County Alliance for Healthcare Access (SCAHA) and One Community, One Voice (OCOV). SCAHA was a group representing health and social services organizations with the stated purpose to “facilitate processes that enable Skagit County residents to access appropriate and effective health care services” [8]. OCOV was formed to explore ways to break the cycle of poverty using local, collective action. The significant community capital created by the work of SCAHA and OCOV led to a “perfect storm” and readiness for the creation of the PHT [9-11]. Both SCAHA and OCOV helped create networks and relationships with a common focus on community health. The social capital generated from the groups fostered networks in the community built on the sense of belonging, while the political capital that resulted from connections to people in power gave legitimacy to the newly formed PHT. A corresponding shift in the role and focus of Skagit County Public Health (SCPH) from providers of clinical care to promoting health through assessment and policy development was being implemented. Two outside factors the Affordable Care Act which was impacting the financing and availability of health care [12-14]. and the Regional Accountable Communities for Health initiative [15]. an innovative approach to harnessing the collective efforts of health stakeholders provided Skagit County a means to promote and fund population health improvement and health equity. In the four years since its creation, the PHT has concentrated on organizational formation and assessment and planning activities. The PHT members, under the leadership of the PHT Health Analyst, evaluated models for building community health collaborations and frameworks for assessing population health. The National Association for County and City Health Organizations (NACCHO) model for Mobilizing for Action through Planning and Partnerships (MAPP) [16,17] aligned best with the vision of the PHT. (Table 1) presents the model adopted to support PHT organizational and assessment efforts. PHT members worked together in the design and completion of a community health survey, presentation of a data carousel highlighting survey results, and hosting community listening sessions. Community survey results identified areas of need while the listening sessions identified problems that the community had highest priority. From this work, 13 priorities were identified, which have evolved into the categories and priorities described in (Table 2).
The PHT members determined that the first work group would focus on the emerging opioid epidemic a priority that emerged from the community listening sessions. At the time the data carousel was conducted, there was little opioid-related data available. As a result, this topic was not included in that event. However, it became clear from the community listening sessions that while there might be a dearth of data on the topic, opioid use was a significant and critical health issue for the community. A cross-sectional representation of community stakeholders engaged in various aspects of substance use disorder prevention, treatment, and recovery. In concert with PHT members, stakeholders met to create an action plan that encompassed policy, system, and environmental change. An estimated 700 volunteer work hours were committed by PHT members and community stakeholders in the development of the opioid action plan [18]. And subsequent report. The collective impact of this effort is seen in the policy changes for county-wide reporting of opioid-related deaths and the creation and implementation of a prescriptiontake back program. A second work group focused on Maternal, and Child Health was established to address the gaps suggested by the data and develop a plan with an emphasis on prenatal care and the first 1,000 days of life. A comprehensive plan has been completed and reviewed by the PHT. PHT members have also indicated how they and/or their organization can contribute to meeting the goals of the First 1000 Days Action Plan.
Member Survey Methodology
In summer 2017, SCPH sought information about how the PHT organization and processes were working after two years in operation. In response, a web-based survey was developed informed largely by the framework developed by [7]. The survey included questions related to the community health assessments; identification of community health goals, priorities and common measures; and the degree to which the PHT organization and structure was engaging members and promoting successful outcomes. The last three questions asked respondents to describe how the PHT encourages and strengthen partnerships and communications. This survey was exempted by the Washington State University Institutional Review Board for the Protection of Human Subjects. There were twenty-one survey responses, representing 62% of the PHT membership. The responses were downloaded into SPSS and analyzed. A report was submitted to the PHT membership with the frequency distribution of the closed-ended questions and a complete list of the responses to open-ended questions. The results and implications were discussed at a subsequent PHT meeting. Selected survey results are provided below, as appropriate, to provide further insight into the PHT.
Collaboration Success Factors
The categories developed by [7]. serve as a framework for analyzing the organization and collective impact efforts of the PHT. Each of these elements, along with lessons learned from the PHT experience, are described below.
Environment
Environmental characteristics comprise the geographic location as well as the social context within which the collaborative group exists. As described by [19]. geography plays a role in assessment methods, priority selection, stakeholders available to support implementation, and participation in activities. Skagit County is a rural community with small population centers with a commitment to create both community and economic vitality. The PHT benefitted from the foundational work of SCAHA and OCOV in establishing relationships that created mutual respect, understanding and trust. This allowed the PHT to progress more rapidly to the implementation stage [20]. These factors reinforced the value of the social capital built through prior relationships and enabled the group to readily trust the process. Further, the “Forces of Change” [21]. presentations, a MAPP [14]. Element encouraged PHT members to share current activities, challenges and opportunities within their sector, and reveal potential connections among members.
Membership
Sustainability of the PHT was predicated on wide representation from cross-section of public and private entities with a mission that align with stated goals of the PHT. Thirty-two (32) individuals representing 29 organizations in Skagit County are members of the PHT. A robust vetting process which included nominations of and interviews with potential advocates, health care providers and local jurisdictions was implemented and continues to be used. Members are sought out purposefully with invitations and selections based not only the skills and attitudes, but on the desire to establish an inclusive membership. A list of organizations representing a cross-section of stakeholders is used to identify sectors and organizations for representation on the PHT. Members commit to a two-year term. As a result, the membership has benefitted from depth of experience, historical and new perspectives, and voices from education, agriculture, Hispanic and Native American communities, hospitals, pharmacy and clinical care providers, academic faculty, non-profit organizations, and relevant public health sectors. Most members participate as part of their employment and identifying resources to engage volunteers from the community has been a challenge. The importance of an inclusive and diverse membership was echoed in the member survey. One member noted that the PHT members “continue to question themselves on inclusivity of appropriate partners in moving our mission forward.” Another stated that the PHT continues to work “to maintain a PHT that is diverse and representative of the community.” The academic community (i.e., Washington State University, Eastern Washington University, and Skagit Valley College) provided research and literature reviews to help the PHT identify models and frameworks to inform PHT strategies. Academic representatives contributed to survey development, data collection and analysis, and led stakeholder focus groups resulting in agreed-upon metrics listed on Skagit County Trends [22]. Website They presented at a national Community Health conference on lessons learned based on the PHT collaboration and initiated the writing of this manuscript.
Process and structure
Acknowledging that the sense of “ownership” of both the way the group works, and the products of its work are hallmarks of successful collaborations, considerable effort has been put into promoting meaningful involvement in a variety way, including monthly meetings and discussion, voting, and committee work. In addition, PHT members jointly established consistently referenced meeting norms and a charter that includes topics such as operating values, planning process principles, and member roles and expectations [22]. Recognizing the contribution of inkind time and materials, as well as financial support to augment the SCPH budget, has reinforced the level of commitment and PHT structure. A Steering Committee was established to guide PHT work with PHT members self-selecting to serve on this oversite body. The variety of ideas and suggestions that emerge from monthly PHT meetings are discussed by the Steering Committee and used to plan for the next PHT meeting to ensure that the work of the PHT is focused and relevant. As one PHT member put it: “I feel everyone has a voice and, therefore, buy-in for the tasks at hand.”
Communications
Effective and continuous communication strategies keep the community informed of the PHT’s work and progress. When the PHT was established, a communication system was also established using electronic mail (email), webpage, and Facebook. All meeting notes are posted on the PHT webpage, part of the SCPH website, for easy access. Monthly meetings are held with an agenda and prior meeting minutes distributed by email. Oral and written reports are shared openly to avoid the conflicts which could occur with selective distribution. In the survey, PHT members characterize this approach as resulting in “a well-organized system of disseminating information” and “strong and frequent inclusive communications.” An important aspect of communications is the members’ connections to the community. As one PHT member observed in the PHT member survey: “The PHT is providing a link and/or networking for the community” about population health. The local newspaper has published articles about PHT activities and posts announcements for upcoming PHT events to keep the general public informed. The Skagit County Trends [23]. Website provides a comprehensive, shared set of data points for easy access and interpretation that can be used by the PHT members and stakeholders.
Purpose
This factor refers to agreement and understanding about the reason for developing a collaborative effort. The Skagit County Board of Health authorized the PHT through Proclamation [24]. To guide health improvement efforts and develop a community health plan. The PHT members met to create a shared mission, objectives, and strategies which are revisited often to reinforce this shared purpose. An important lesson learned was demonstrated at a recent meeting. When asked to describe the work of the PHT for an “elevator speech,” members, not surprisingly, expressed a variety of different strengths related to the PHT and its efforts. It became apparent that time spent crafting an “elevator speech,” with contributions from all members, was of value not only in articulating the PHT mission to the public, but to solidify the shared vision and unique contribution of each sector. This process provided clarity about the PHT purpose, reinforced commitment, and allowed for a robust conversation that highlighted differing perspectives from the various sectors represented by PHT members. The final verbiage was agreed to by all the PHT members as a way to describe the purpose and work of the PHT to community members.
Resources
Both financial and human “input” are necessary to develop and sustain a collaborative group. Sufficient funds and a skilled convener are equally important in a successful collaboration. Serving as the backbone organization, the SCPH hired a highly skilled individual to convene the PHT. In the nearly four years since the PHT was established, he has demonstrated the organizational and interpersonal skills necessary to lead the group effectively. He carries out his responsibilities as organizer and facilitator in a fair and respectful manner which in turn has generated “legitimacy” and respect from the collaborative partnerships. While the financial base for PHT came from the SCPH and Board of Health, PHT members and their organizations provided additional funds needed to establish and maintain the Skagit County Trends [23]. website, increasing the sense of ownership in this valuable resource. Sharing the financial support across agencies sustains the work and creates a valued investment across PHT members. Discussions about supplemental funding are open and candid but no one is pressured. Indeed, volunteer time and in-kind contributions are valued equally with dollars to support projects.
Recommendations for Future Partnerships
We offer the collaborative processes employed by the PHT not as a perfect example of planning, engagement and implementation at the local level, but rather as a multifaceted collective impact model that was adopted and adapted to improve community health outcomes. The research conducted about the PHT—the literature review, interviews, and surveys served not only as the basis for our observations but also resulted in the identification of several lessons learned. These lessons learned are critical to the continued improvement and sustainability of the organization and might prove useful to those engaged in similar efforts: 1) patience with the process is essential. Building collaborations can be complicated and frustratingly non-linear. Despite the fact that many of the 32 PHT members had successfully worked together in the past, it still required time and attention to build strong relationships and trust; 2) consistent with the literature on collaborative efforts [25]. the presence of a backbone organization—providing materials, web support, and a skilled, committed staff—has been essential to the forward movement of the PHT; 3) effective communications should be a priority. Good communications ensure that all members have access to important information and, equally important, help identify and acknowledge differing perceptions among members and promote resolutions to conflict; 4) including representatives from the range of community sectors is indispensable for hearing multiple perspectives and getting results that do, in fact, produce collective impact. At the recent annual retreat, PHT members reflected on work accomplished and the work yet to be achieved. This day-long activity led to the identification of goals and research priorities for the coming year, with an eye to collective impact. Developing a formal communications plan and engaging PHT members in equity activities are priority goals. Research priorities include engaging stakeholders in a new cycle of community health assessments and updating the Skagit County Trends [23]. Data the PHT members support a culture of health that encompasses all aspects of community health and health equity, from access to clinical care to social determinants of health. While the PHT has its challenges, the collaborative is also highly adaptive and inherently creative. The PHT has a strong foundation of respect and trust among its members, and will, no doubt, build on that foundation to make substantial and sustainable progress in community health.
References
- Disease Prevention and Health Promotion. U S Department of Health and Human Services.
- Quick Facts. U S Census Bureau.
- (2018) County Health Rankings and Roadmaps. Robert Wood Johnson Foundation.
- Bryson J, Crosby B, Stone M (2015) Designing and implementing cross‐sector collaborations Needed and challenging. Public Administration Review 75(5): 647-663.
- Henig JR, Riehl CJ, Houston DM, Rebell MA, Wolff JR (2016) Collective Impact and the New Generation of Cross-Sector Collaborations for Education A Nationwide Scan. Teachers College, Columbia University 35(23): 5.
- Hogue T Community-based collaboration Community wellness multiplied. Oregon Center for Community Leadership.
- Mattessich PW, Monsey BR (1992) Collaboration what makes it work A review of research literature on factors influencing successful collaboration. Amherst H Wilder Foundation.
- Webster J Skagit County Alliance for Healthcare Access. Community Assessment Report.
- Emery, Mary, Cornelia Flora (2006) Spiraling Up Mapping Community Transformation with Community Capitals Framework. Community Development 37(1): 19-35.
- Jacobs C (2011) Measuring Success in Communities the Community Capitals Framework. Extension Extra.
- Bartol KM, Zhang X (2007) Networks and leadership development Building linkages for capacity acquisition and capital accrual. Human Resource Management Review 17(4): 388-401.
- Levesque JF, Harris MF, Russell G (2013) Patient centered access to health care conceptualizing access at the interface of health systems and populations. International journal for equity in health 12(1): 18.
- Buck JA (2001) The looming expansion and transformation of public substance abuse treatment under the Affordable Care Act. Health Affairs 30(8): 1402-1410.
- Huntington WV, Covington LA, Center PP, Covington LA, Manchikanti L (2011) Patient Protection and Affordable Care Act of 2010: reforming the health care reform for the new decade. Pain Physician 14(1): E35-E67.
- Haar WL, Cantor J (2016) Accountable Communities for Health A ‘Portfolio of Strategies’ Approach to Improving Population Health. Prevention Institute & JSI Research & Training Institute.
- (2019) Mobilizing for Action through Planning and Partnerships (MAPP). National Association of County and City Health Officials.
- Jacobs LM, Elligers JJ (2009) The MAPP approach: using community health status assessment for performance improvement. Journal of Public Health Management and Practice 15(1): 79-81.
- Skagit County Population Health Trust. Opioid Workgroup Leadership Team 2016 Summary Report and Recommendations.
- Kegler MC, Rigler J, Honeycutt S (2011) The role of community context in planning and implementing community-based health promotion projects. Evaluation and Program Planning 34(3): 246-253.
- Butterfoss FD, Gilmore LA, Krieger JW, Lachance LL, Lara M, et al. (2006) From formation to action: How allies against asthma coalitions are getting the job done. Health Promotion Practice 7(2): 345-435.
- Erwin P (2015) Forces of Change. American Journal of Public Health 105(5): 836.
- Population Health Trust Meeting Information and Archives.
- Skagit County Trends. EWU Institute for Public Policy and Economic Analysis.
- (2015) Skagit County Board of Health. Proclamation Creating the Population Health Trust.
- Kania J, Kramer M (2011) Collective Impact. Stanford Social Innovation Review.






























