Proportion of Dual Protection use at a Time to Prevent Unwanted Pregnancy and HIV/AIDS/Sexually Transmitted Infections and Its Predictors among Human Immunodeficiency Virus (HIV) Positive Women attending Anti Retro Viral Therapy (ART) Clinic Hosanna Hospital, Southern Ethiopia; Institution Based Cross Sectional Study
Markos Selamu Jifar1* and Tilahun Beyene Handiso2
1College of Health science, Dembi Dolo University, Morsito, Ethiopia
2 Department of Epidemiology and Biostatics, University school of Public Health, Wolaita Sodo, Ethiopia
Submission: May 15, 2019; Published: July 01, 2019
*Corresponding author: Tilahun Beyene Handiso, Department of Epidemiology and Biostatics, University school of Public Health, Wolaita Sodo, Ethiopia
How to cite this article:Markos S J, Tilahun B H. Proportion of Dual Protection use at a Time to Prevent Unwanted Pregnancy and HIV/AIDS/Sexually Transmitted Infections and Its Predictors among Human Immunodeficiency Virus (HIV) Positive Women attending Anti Retro Viral Therapy (ART) Clinic Hosanna Hospital, Southern Ethiopia; Institution Based Cross Sectional Study. JOJ Pub Health. 2019; 4(5): 555649. DOI: 10.19080/JOJPH.2019.04.555649
Abstract
Background: Dual protection is a strategy that prevents both unwanted pregnancy and sexually transmitted infections, including human immune deficiency virus. Reasons for using and for not using are not well known.M
Objectives: To assess dual contraceptive utilization and associated factors among pre-ART and ART women living with human immune deficiency virus.
Methods: Institution based cross-sectional study was conducted. Data were collected through interview using structured questionnaires. Participants were selected by using simple random sampling technique from patient registration book. Bivariate and multivariable analysis was performed using logistic regression on SPSS version 20.0. Adjusted odds ratio with 95%CI was used.
Results: The prevalence of dual contraceptive utilization of women living with human immune deficiency virus in the Hospital was 28.3% (95% CI: 23.8, 33.7) and significantly associated with receiving follow up counseling (AOR: 6.05; 95% CI: 2.46, 14.83), starting ART(AOR: 0.21; CI: 0.07, 0.64), had no child (AOR: 0.19; 95% CI: 0.06, 0.57), supporting to use (AOR: 6.36; 95% CI: 2.49, 16.28).
Conclusion: Dual contraception utilization was less than one-third and having no child; receiving follow up counseling in the last 3 months; starting antiretroviral treatment; supporting to use were significantly associated with dual contraceptive utilization. It needs governmental and non-governmental organizations, other professionals and researcher’s involvement to improve dual contraceptive utilization.
Keywords:Dual protection; HIV/AIDS; Hosanna Hospital; sexually transmitted infections
Abbreviations: AIDS: Acquired Immune Deficiency Syndrome; AOR: Adjusted Odds Ratio; ART: Anti-Retroviral Therapy; CD4: Cluster of differentiation / Cell differentiation; CPR: Contraceptive Prevalence Rate; CSA: Central Statistical Agency; EDHS: Ethiopian Demographic and Health Survey; HAART: Highly Active Antiretroviral Therapy; HAPCO: HIV/AIDS Prevention and Control Office; HIV: Human Immune Deficiency Virus; IUD: Intrauterine Device; MOH: Ministry of Health; PMTCT: Prevention of Mother to Child HIV Transmission; REC: Research & Ethical Committee; SPSS: Statistical Package for Social Science; STI: Sexually Transmitted Infection; UNAID: United Nations Program on IV/AIDS; WHO: World Health Organization; PCA: principal component analysis; NEMMH: Nigist Ellen Mohammed Memorial Hospital
Introduction
Dual contraceptive utilization refers to the use of a barrier contraceptive (i.e., condoms), which can reduce transmission of many STIs, plus another effective family planning method that can prevent pregnancy as recommended by the World Health Organization (WHO) [1]. The co-occurrence of HIV and unintended pregnancy has prompted a relatively recent body of work on dual protection, the simultaneous protection against STIs and unintended pregnancy [2]. Some studies that have considered the benefits of dual protection for people living with HIV show that dual protection can be an effective strategy to prevent HIV transmission to partners and to promote safe childbearing; but little of it is known in our country [3,4]. Increase of contraceptive prevalence rate (CPR) in Sub-Saharan Africa with corresponding reduction in primary HIV infections and unintended pregnancies in HIV infected women has potential to decrease the proportion of infants infected with HIV by 35-55% [5].
Ethiopia is one of the countries’ most severely hit by the HIV epidemic. The dominant heterosexual transmission, the vertical virus transmission from mother to child accounts for more than 90% of HIV/AIDS infection [6]. The World Health Organization (WHO) recommends that women living with HIV use dual contraceptive methods or dual protection to prevent unintended pregnancies and STIs [7]. In some cases, women living with HIV-infection continued to have unprotected sex with their partner, even though they were aware of the risk of infecting their partner, rather than begin using condoms, and have their partner discover their HIV-positive status. The burden of unintended pregnancy and STIs was greater among younger and economically disadvantaged men and women [8]. There were few studies done on dual contraceptive utilization and Reason to use among HIV positive reproductive age women in Ethiopia [9].
Materials and Methods
Study area and study period
The study was conducted among ART & pre-ART user in Hosanna Hospital, Hadiya zone, South Nation Nationalities and Peoples Regional State (SNNPR), Southern Ethiopia; which is located 232km far from south of Addis Ababa, the capital city of Ethiopia and 174 km far from north of Hawassa, capital city of SNNPR. ART clinic provides free services for patients for routine testing and counseling services, comprehensive HIV/ AIDS prevention, treatment and care interventions. According to institutional report the number of people living with HIV ever enrolled ART/Pre-ART was 3,155 on chronic care registration log book among those currently active on ART and Pre-ART are 966 and 386 respectively while 692 HIV positive reproductive age women. The study was conducted from to March 12 to April 13, 2016.Facility based cross-sectional study was employed.
Inclusion criteria
HIV positive reproductive aged women attend chronic HIV/ AIDS care clinic HIV positive reproductive aged women at least one visit attended before this study.
Exclusion criteria
Unable to communicate verbally/seriously ill at time of data collection Pregnant women at the time of data collection
Sample size and sampling technique/sampling procedure
The required sample size was calculated using a single population proportion formula as follows
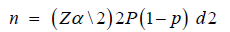
Where: n = sample required; Zα \ 2 = the critical values at 95% confidence level of certainty =1.96; P=19.8% (Proportion of dual contraceptive use from previous study; d= margin of error = 5%. After adjustment for non-response 10%; the total sample size required 269. For the second objective the required sample size was calculated by using Epi-Info software version 7.0 stat calc program. The variables associated with dual contraceptive utilization: residence (27.9%), CD4 count (29.6%), counseling about family planning (10.1%) with confidence interval 95%, power 80% assumption; Ratio (No of outcome in unexposed: No of outcome exposed). Sample size was calculated for the second objective from previous study using odds ratio effect measure.10The second objective calculated sample size was 252, 62 and 253 respectively, but 269 maximum sample size was taken
Sampling Procedure /Techniques
Computer generated simple random sampling technique using Excel sheet to select study respondents by using their ART & Pre-ARTHIMS registration numbers. During the one -month study period; 258 HIV positive women were recruited from sample frame. Respondents, who were not obtained at appointment date, were revisited the whole data collection period. The HIV positive women visit the Hospital at least once in a month. During one-month data collection period, there was possible condition to get the study participants.
Data collection tool
Structured questionnaire was used to collect data which were adapted from different relevant literatures and modified to the local context. The questionnaire was designed to obtain information on study variables (dependent and independent Variables). The questionnaire was prepared in English and translated to Amharic & local language (Hadiyigna) and back retranslated to English to check its consistency. Translator to Amharic and back translated to English by independent translators to keep the consistency of the questionnaires.
Data collectors
Data were collected by three diploma nurses who were recruited from Hossana health center & one supervisor degree holder nurse from Nigist Ellen Mohammed Memorial Hospital. Data were collected by face to face interview using structured Amharic and local language (Hadiyigna) questionnaires. No compensation was given to participants. The data on dual contraceptive use was collected by oral report of mothers but some other independent variables like CD4 from oral report and registration book.
Data quality assurance/control
To ensure data quality, data collectors and supervisor were trained by the principal investigator for two days on purpose of the study, on data collection tools, research ethical issues & confidentiality prior to data collection. Pre-test was done on 5% of the sample of HIV positive women in Homacho district Hospital to identify any inconsistency, skips patterns and acceptability of questionnaire, and then necessary corrections was made before the actual data collection. Supervisor closely followed the data collection throughout the data collection period along with the principal investigator. After data collection, each questionnaire was checked for completeness and code was given before data entry. The data were cleaned and carefully entered into Epidata version 3.1 & exported to SPSS version 20.0 for analysis
Data processing and analysis
Descriptive statistics was done to describe the data by using frequency, tables, percentages etc. leanalysiswasperforme dusinglogisticregres siononSPSSversion 20.0 software in order to determine factors associated with dual contraceptive utilization with statistically significant level of p<0.05 and CI of 95%. Independent variables with p-value of less than 0.25 was candidate variables to multivariable logistic regression for controlling the possible effect of confounders and finally the variables which has significant association with dual contraceptive utilization was identified on the basis of adjusted odds ratios (AOR), with corresponding 95% CI were used to quantify the degrees of association between independent variables & dual contraceptive utilization. Goodness of fit of the final model was checked using Hosmer & Leesha test considering good fit at P-value=0. 065.Multicollinearity among independently associated variables was checked using variance inflator factor (VIF), standard error) and correlation coefficient. The Bartlett test of sphericity is statistically significant at p<0.05 conducted on analysis. The Kaiser-Meyer-Olkin (KMO) measure of sampling adequacy (MSA) greater than 0.5 for individual as well as the full set of items was used to check the appropriateness of the PCA [10,11]. Internal consistency of PCA were checked.
Operational Definition & Terms
Dual contraceptive utilization: in this study it refers to the HIV positive women who used two methods of contraception simultaneously, a barrier method (male/female condom use in every sexual encounter in the last six months preceding the study) &other modern/hormonal/ contraceptive methods.
Accessibility of family planning service: it refers to the distance from client’s residence to the health institution took 5km or ≤30 minutes walking time considered as accessible [12].
Knowledge of contraceptive use: in this study refers to from total of five dichotomized questions, 0 for incorrect answer and 1 for correct answer about contraceptive use, women who answered median score& above, considered as good knowledge and below median score considered as poor knowledge
Pregnant woman: refers to woman who reported she was pregnant or her husband who reported his wife pregnant Reproductive aged women: in this study refers HIV positive women whose age 18-49 years attend chronic HIV/AIDS care clinic.
Ethical Approval
Ethical clearance & official letter approved from College of Jimma University School of public health & Health Research Ethical committee (REC). Written consent was obtained from medical director of NEMMH. Verbal informed consent for participation obtained from each study participant. The confidentiality of clients’ information was ensured, as names or any identifiers of study participants were not be included in the data sheet. The discussions between the data collectors and the respondents were taken place privately and individually. All individuals and institutions mentioned in this study are asked and they were agreed.
Result
From the total of 269 sample size, response rate of 258 (95.9%) were included in this study. The non-response rate was due to 5 refusals, 4 discarded due to incomplete data, 2 unable to get in follow up. Regarding Socio demographic characteristics more than half (52.3%) of the participants were in age group of 30-39 years. Hadiya account 52.7%, protestant 33.7%, nearly one-third of the participants completed primary education, 34.9% merchants, urban residents were 76.4% and 21.3% of the participants were in medium wealth index (Table 1).
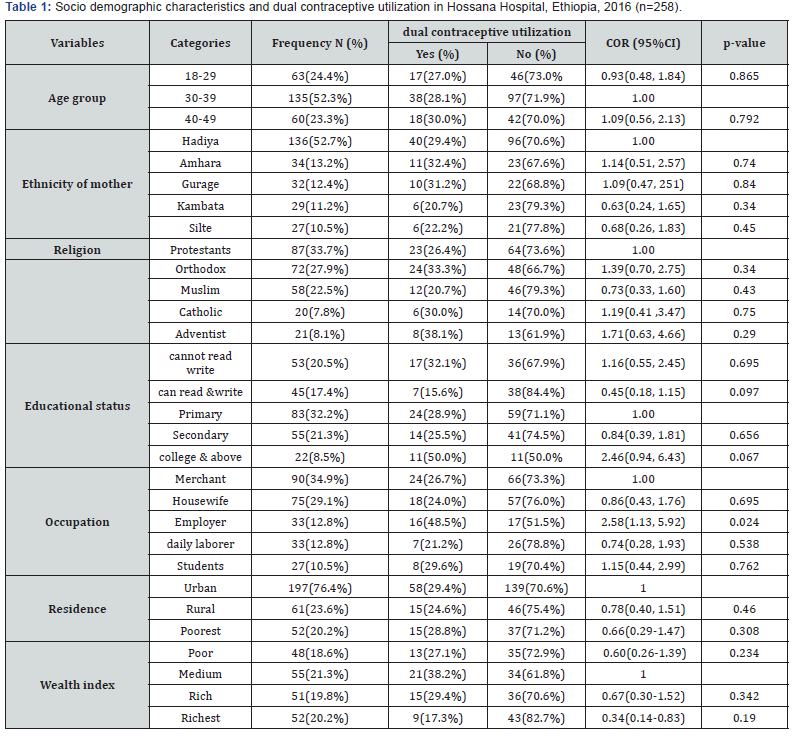
Dual Contraceptive utilization and Reasons to use
The use of dual contraceptive utilization of HIV positive women in NEMMH was 73(28.3%). This means 28.3% of the study participants used condom and other method of contraceptive simultaneously. The most common reason for using dual contraception is fear of STIs followed by to prevent pregnancy. The most common reasons for not using were childbearing desire followed by fear of side effect (Table 2).

Sexual and reproductive related factors & dual contraceptive utilization by HIV positive women on ART and follow up care
Out of the respondents (93.4%) had sexual intercourse within last six months: among those (84.9%) had sex with regular partner and (8.9%) were had multiple sexual partners (Table 3).
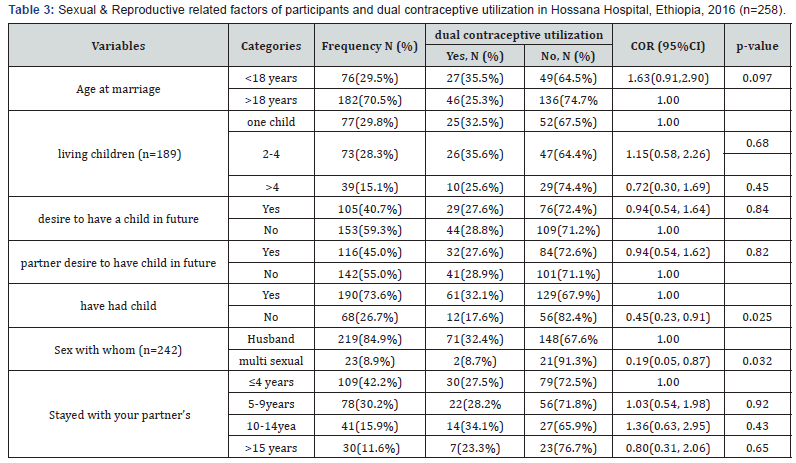
Service-related factors & socio-cultural factors and use dual contraceptive utilization on ART and follow up care
Concerning about time to reach health institution (80.2%) was reported that it takes ≤ 30 minutes to reach the health institution from their residence. The majority of respondents (95.0%) were reported that services utilized in the health institution. The majority (93.4%) of respondents there is no cultural practice in their community that prevents from dual contraceptive utilization (Table 4).
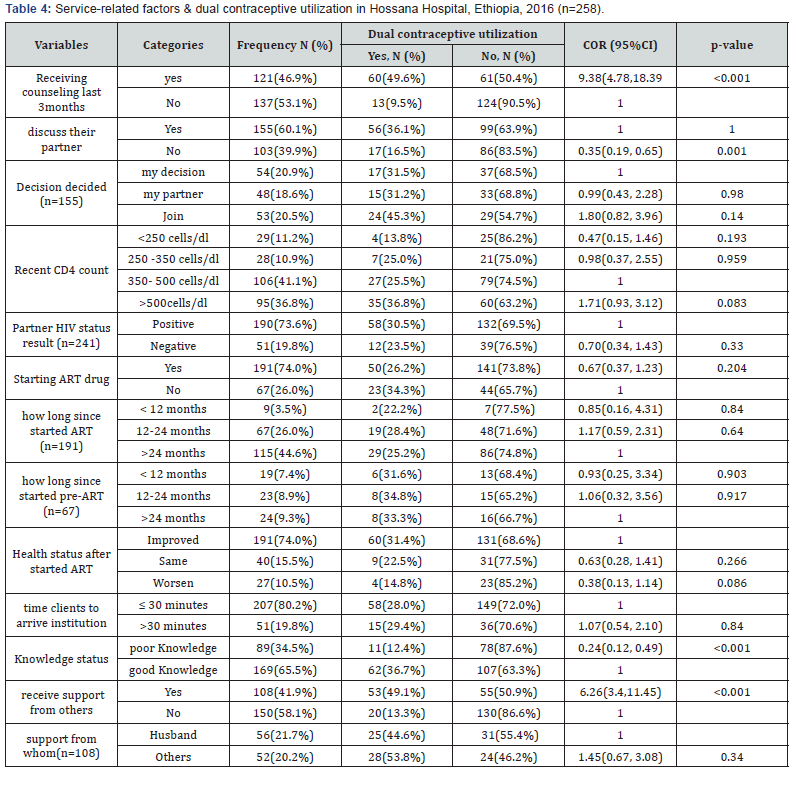
Factors independently associated with dual contraceptive utilization
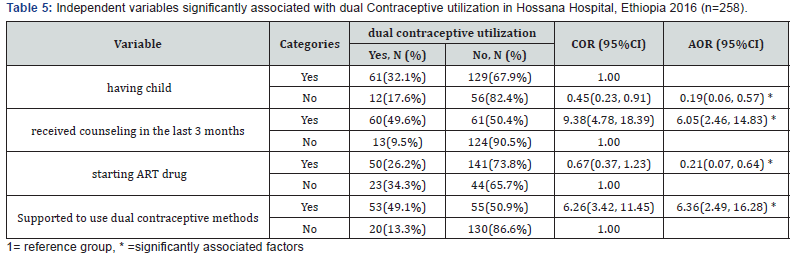
In multivariable analysis the following factors were independent predictors of dual contraceptive utilization with p-value <0.05. In this study variables associated with dual contraceptive use: have had child, receiving follow up counseling in the last 3 months, starting ART drug and supporting to use dual contraceptive methods. The participants who had no child less likely to utilized dual contraceptive utilization as compared to have had living children with (AOR: 0.19; CI: 0.06, 0.57)& Participants who receiving follow up counseling in the last three months more likely use dual contraceptive methods than those who did not receive follow up counseling in the last three months with(AOR: 6.05; CI: 2.46, 14.83).With regarding to start ARV therapy, starting ART treatment less likely to utilized dual contraceptive methods as compared to did not start ART treatment with (AOR: 0.21;CI: 0.07, 0.64). Supporting to use dual contraceptive utilization more likely to use dual contraceptive utilization than those who did not receive support to use dual contraceptive utilization with (AOR: 6.36; CI: 2.49, 16.28) (Table 5)
Discussion and conclusion
This study attempts to assess dual contraceptive utilization and associated factors among HIV positive reproductive age women. This study revealed that, the use of dual contraceptive utilization of HIV-positive women in NEMMH was 28.3% (95%CI: 23.8-33.7%). This implies that less than one-third of the study participants used condom and other contraceptive method simultaneously, which is important in preventing pregnancy and STIs including viral load. This figure is high when compared to the cross-sectional study conducted in Gebretsadik Shawo Hospital on HIV-positive women which is (19.8%) [10]. Reasons for this variation might be due to study setting, age group & time of contraceptive utilization. But, similar with study conducted in Fitch Hospital Oromia region on people living with HIV finding showed that (32%) [13]. And also, study conducted in western Ethiopia on modern contraceptive utilization among reproductive age group female attend ART clinic finding showed that (30%) use dual contraceptive utilization [14] The most common reason identified by this study to use dual contraceptive was to prevent STIs and avoid unwanted pregnancy. Whereas the main reasons not to use were desire to bear child and fear of side effect were identified.
Factor like have had no child, receiving follow up counseling in the last 3 months, starting ART drug &supporting to use dual contraceptive utilization were significantly associated with dual contraceptive utilization. In this study HIV positive women who had no living children were 81%less likely to utilized dual contraceptive utilization as compared to who have had living children with (AOR: 0.19;95% CI: 0.06, 0.57), this finding was similar with study conducted in Fitch Hospital Oromia region on people living with HIV [13]. According this study HIV positive women who receiving follow up counseling in the last three months six times more likely use dual contraceptive than those who did not receive follow up counseling in the last three months with (AOR: 6.05;95% CI: 2.46, 14.83).This finding was similar with finding from the cross sectional study done in Geektastic Shaw Hospital, Ethiopia [10].
Regarding to ARV therapy, those who starting ART treatment were less likely to utilized dual contraceptive methods as compared to who did not start ART treatment with (AOR: 0.21; 95% CI: 0.07, 0.64). This finding was similar with study done gimbie town, western Ethiopia on modern contraceptive utilization among female attend ART clinics [14]. Reasons for non uses of dual contraceptives might be fear of contraception related complication with ART drugs. Study participants who supported to use dual contraceptive were 6.36 times more likely to use dual contraceptive than those who did not support to use dual contraceptive (AOR: 6.36; 95%CI: 2.49, 16.28).This finding similar with study finding from the cross sectional study done in Gebretsadik Shawo Hospital, Ethiopia on HIV positive women.10 Also, this finding similar with study conducted in Uganda on utilization of family planning services among HIV positive women [15]. According to study conducted in Gebretsadik Shawo Hospital, Bonga, SNNPR, Ethiopia educational status, occupational status, decision with their partners, recent CD4 count, were the significantly associated. But these variables were not significant in this study. Possible reasons for this variation might be due to age group, geographical variations, economic status &patient status /stages/. Even if study conducted on facility based primary data were used. A set of reliability and validation rules were applied. This study had a few limitations: Cause and effect relation not assured. Dual contraceptive utilization &wealth index were assessed based on self-reported information which is subjected to socially desirability bias and recall bias.
Conclusion
In this study level of dual contraceptive utilization was low. Factors likes to have had child, receiving follow up counseling in the last 3 months, starting ART treatment & supporting to use contraceptive were significantly associated with dual contraceptive utilization. Modern contraceptive method uses other than condoms was low (no one use permanent, implant).
Recommendation
Health professionals working in ART clinics should consider and plan to increases number of dual contraceptive users among HIV positive women in NEMMH. It needs intervention by involving woreda, zonal health office, NEMMH &other concerned stakeholders towards the increment of coverage of family planning in the NEMMH for HIV positive women.
References
- Wilson TE, Koenig LJ, Walter E, Fernandez I, Ethier K: Perinatal Guidelines Evaluation Project (2003) Dual contraceptive method use for pregnancy and disease prevention among HIV-infected and HIV-uninfected women: the importance of an event-level focus for promoting safer sexual behavior. Sex Transm Dis 30(11): 809-812.
- Berer M (2006) Dual protection: more needed than practiced or understood. Reproductive Health Matters 14(28): 162-170.
- Ngure K, Heffron R, Mugo N, Irungu E, Celum C, Baeten JM (2009) Successful increase in contraceptive uptake among Kenyan HIV-1-serodiscordant couples enrolled in an HIV-1 prevention trial.” AIDS 23(1): S89-95.
- Heffron R, Were E, Celum C, Mugo N, Ngure K, et al. (2010) A prospective study of contraceptive use among African women in HIV-1 serodiscordant partnerships.” Sexually Transmitted Diseases 37(10): 621-628.
- Barbara N, Sandra C, Christopher G, Jaya E (2011) Family planning among people living with HIV in post-conflict Northern Uganda. Makerer University 5(18): 1-12.
- (2011) Federal Ministry of Health Guidelines for Prevention of Mother-to-Child Transmission of HIV in Ethiopia Pp. 1-224.
- Munsakul W, Lolekha R, Kowadisaiburana B, Roongpisuthipong A, Jirajariyavej S, et al. (2016) Dual contraceptive method use and pregnancy intention among people living with HIV receiving HIV care at six hospitalsin Thailand. Reproductive Health 13: 8.
- Atlanta G (2010) Sexually Transmitted Disease Surveillance 2009, Centers for Disease Control and Prevention.
- Myer L, Mathews C, Little F (2002) Dual method use in South Africa. Internet Fam Plann Perspect 28(2): 119-221.
- Meseret W M (2015) Dual-Contraceptive Method Utilization and Associated Factors among HIV Positive Women Attending Art Clinic in Gebretsadik Shawo Hospital, SNNPR, South West Ethiopia. Women’s Health Care 4: 6.
- Dingeta T, Oljira L, Assefa N (2012) Patterns of sexual risk behavior among undergraduate university students in Ethiopia: a cross-sectional study. Pan African Medical 12(33): 82-86.
- Hasan A (2007) Patient satisfaction with Maternal and Child Health services among mothers attending the Maternal and Child Health Training Institute in Dhaka, Bangladesh. MAHIDOL. satisfaction with Maternal and Child Health p. 1-66.
- Abdissa D (2015) Dual Contraceptive Utilization and Associated Factors among People Living with HIV Attending ART Clinic in Fitche Hospital, Ethiopia. Health, Medicine and Nursing 20: 25-33.
- Polisi A, Gebrehanna E, Tesfaye G, Asefa F (2014) Modern contraceptive utilization among female ART attendees in health facilities of Gimbie town, West Ethiopia. Reproductive Health 11: 30.
- Joseph (2010) utilization of family planning services among sexually active people living with hiv/aids in taso tororo p.11-75.






























