Outbreak of Chikungunya Fever in Sudan, 2018-2019
Seid Ali Mohammed1* and Yaregal Animut2
1Oda buldiglu district, Assosa zone, Benishangul Gumuz Region, Western Ethiopia
2 Department of Biostatistics and Epidemiology, Institute of Public Health, College of Medicine and Health Sciences University of Gondar College of Medicine and Health
Submission: March 3, 2019; Published: June 13, 2019
*Corresponding author: Seid Ali Mohammed, Department of Biostatistics and Epidemiology, University of Gondar, Gondar, Ethiopia
How to cite this article:Seid Ali Md, Yaregal A. Rubella Outbreak Investigation and response in Oda buldiglu District of Assosa zone, Benishangul Gumuz Region, Western Ethiopia, 2018.JOJ Pub Health. 2019; 4(4): 55564. DOI: 10.19080/JOJPH.2019.04.555645
Abstract
Introduction:Rubella is an acute and contagious disease caused by the Rubella virus. It is also called German measles. Rubella usually have milled illness, it presents with low-grade fever and maculopapular rash that start on the face and spreads to the rest of the body. Pregnant women who contracts rubella are at risk for miscarriage or stillbirth, and their babies are at risk for severe birth defect known as congenital rubella syndrome (CRS). Little is known about rubella epidemiology and the incidence of CRS in Africa. At present Rubella vaccine is not included in any vaccination program in Ethiopia. Suspected Rubella cases were reported from Jun 9 to 22/2018 from oda buldiglu Woreda, BGR of western Ethiopia. We investigated to confirm the etiology, identify potential risk factors and suggest control measures.
Methods:A line list was prepared to describe the outbreak by place, person and time. Un Mach Case control study was used with ratio of 1to 2. Fifty-seven suspected cases and 114 controls were enrolled in the study. Cases are defined as an illness characterized by acute onset of maculopapular rash, fever, arthralgia, lymphadenopathy, conjunctivitis with positive serologic test for rubella immunoglobulin M (IgM) antibody in the blood specimen. Data was obtained from parents or care takers by face to face interview with structured questionnaire.
Results: A total of 57 suspected Rubella cases with zero death were line listed during the outbreak. The mean age of the case was 3years and 6months with the median age of 2years. The overall attack rate of this outbreak was 76 per 100,000 populations with zero case fatality rate. The attack rate was highest among less than five years age group (390 per 100,000 pop). Based on a case control finding poor knowledge on rubella mode of transmission (AOR=3.688, 95% CI=1.328-10.238); having contact with a person who had sign and symptoms of Rubella (AOR: 2.791, 95% CI=1.181-6.597); living in unventilated house (AOR=5.436, 95% CI: 2.167-13.634) were found to be significantly associated with rubella infection..
Conclusion: we verified the existence of Rubella outbreak in the district. Having Poor knowledge on rubella mode of transmission, housing condition with poor ventilation, having contact with a person with rubella, was significantly associated with rubella outbreak.
Keywords:Rubella; Outbreak; Benishangul Gumuz Region; Ethiopia
Introduction
Rubella is an acute and contagious disease caused by rubella virus; it also called German measles. Rubella virus is classified as a toga virus, genus rub virus and may be prevented through vaccination [1-3]. Rubella virus is transmitted from person to person through direct or droplet contact from nasopharyngeal secretions of an infected person in the air from the person with rubella coughing, sneezing or laughing or urine of an infant with CRS [4]. Persons with rubella are most infectious when rash is erupting, but they can shed virus from 7 days before to 7 days after rash onset. The disease has an incubation period of 12–23 days, more commonly 14 to 18 days [5,6]. The disease is characterized by a rose-coloured maculopapular rash and followed by other mild symptoms, such as low-grade fever, conjunctivitis, headache, mild Coryza, malaise, arthralgia and lymphadenopathy. The rash usually lasts from one to four days, it starts on the face and then progresses to other part of the body. The Symptoms are often mild in children and adults, up to 50% of infections may be subclinical or in apparent. The maculopapular rash first appears on the face and spreads rapidly to the chest, limbs, and abdomen, which lasts from one to four days. It is most common among teenagers and young adults [1,2,7]. Pregnant women who contracts rubella virus during the first trimester of pregnancy, are at risk for miscarriage or stillbirth, and their babies are at risk for developing severe birth defect associated with congenital rubella syndrome (CRS) up to 90%. The most common congenital defects associated with CRS are deafness, blindness, heart defects, and brain damage. Rubella also can cause serious complications in children and adults, such as a low platelet count or encephalitis [7-9]. Immunity following natural infection or vaccination is life-long [10].
Rubella occurs worldwide; a total of 22,361 rubella cases and 319 CRS were reported to world health organization in 2016 from different country of the world. It shows 76% decrease from 94,277 cases reported in 2012. Globally approximately 100,000 cases of congenital rubella syndrome estimated to occur each year [11]. The world health organization estimates that, each year’s more than 110,000 cases of congenital rubella syndrome reported from developing countries of the world [12]. In Africa 17,338 cases with the incidence rate of 2.11 per 100,000 populations were reported
Information is limited on the epidemiology of rubella and CRS in Ethiopia. From a total of 28,284 suspected measles cases reported through the measles case-based surveillance system between 2009 to 2015 and 11,151 (39.4%) were positive for measles IgM and 17,066 were negative for measles IgM, from this negative case 2615 (15.3%) were positive for rubella virus IgM during the same period [13,14]. The distribution of confirmed Rubella cases in Ethiopia from 2009-2015 was 2009 (83cases), 2010 (131 cases), 2011 (198 cases), 2012 (806 cases), 2013 (856 cases), 2014 (222 cases) and 2015 (319 cases) [14].
Rubella is a leading vaccine-preventable cause of birth defects. Preventing these adverse pregnancy outcomes is the focus of rubella vaccination programs. The US childhood rubella vaccination program was started in 1969; however, many other countries do not have, or have recently implemented, rubella vaccination programs [9]. In 2000, just over half of 99(51%) countries had introduced RCV into their immunization schedule; by the end of 2012, more than two thirds 132 (68%) of countries were using RCV. Global coverage with RCV increased from 21% in 2000 to 40% in 2012 and to 47% in 2016 [6,10]. The countries that have already started immunization against rubella should integrate rubella surveillance with measles surveillance. This will help to ensure that all potential rubella cases and outbreaks are investigated and quantify the impact of rubella immunization [6]. Rubella and CRS surveillance are necessary to assess disease burden before RCV introduction, to monitor disease burden and epidemiology after introduction, to identify pregnant women infected with rubella virus who require follow-up to assess pregnancy outcomes, and to identify, diagnose, and manage CRSaffected infants [11].
In African countries, including Ethiopia, CRS is widely under-recognized as a public health problem, and information on rubella and CRS epidemiology is very limited. Surveillance for rubella or CRS does not exist in Ethiopia; however, the measles case-based surveillance system, established in 2004, includes laboratory testing for the detection of measles and rubella-specific antibodies. The measles and rubella case-based surveillance system has helped greatly in terms of documenting the epidemiology of measles and rubella in Ethiopia. However, little is known about the magnitude and distribution of Rubella cases in Ethiopia. Therefore, this study aimed to determine the magnitude of the outbreak and identify risk factors associated with Rubella outbreak in oda buldiglu district of Benishangul Gumuz region, western Ethiopia. The findings of this investigation may help to facilitate rapid implementation of control measures to reduce disease burden associated with morbidity and mortality of rubella disease and to interrupt virus transmission as soon as possible. The findings of this investigation may also help to Monitoring the changing epidemiology of rubella and identifying high-risk population that call for targeted immunization strategies and help to plan for introduction of the rubella vaccine to prevent future outbreaks. Help to inform the government and other stakeholder for the necessary of rubella surveillances in the country.
Methods
Study Area
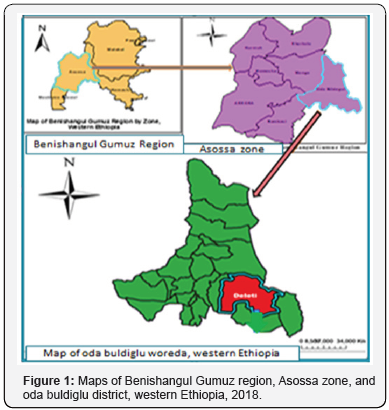
An outbreak investigation was carried out in oda buldiglu Woreda.it is one of the seven woreda found in Asossa zone of benishangul Gumuz region of Ethiopia. It is located 661 Km away from Addis Ababa; and 173 km far from Asossa town. The district is bordered with Asossa woreda in the North-West; Menge woreda in the west; stedal woreda in north-East and Mensibu (Oromia region) woreda in South. The Woreda has 23 rural and 2 urban Kebeles with the total population 74999 in 2017/2018. There were three Health Centre and twenty health Posts. Based on the physical health facility counting the Potential Health Service Coverage of the district was 92%. There was a sudden increase of suspected measele cases in the district on WHO Epidemiological week 19 which was later confirmed to Rubella Igm posetive. The outbreak was detected only from one kebele of the Woreda which is called daleti. Based on 2017/18 population projection estimation the kebele has 11057 population in 2017/2018 from this 5527 were male and 1794 were under five children. The major ethnic groups in the kebele were Oromo. They are agriculturalist and live across the border on Oromia region (Figure 1).
Study Design and Period
Both descriptive and Analytical unmatched Case- control study was used. The study was conducted from 9th June to 22th June 2018. Line listing of suspected cases was used to describe the outbreak by place, person and time.
Population
Source population: All People who reside in oda buldiglu woreda of Asossa zone of Benishangul Gumuz regional state.
Study population: All peoples who live in daleti kebele the district.
Study unit: Selected individuals (cases and controls) who live in the selected household of daleti kebele
Sample Size
Atotal of 57cases and 114 controls with 1:2 case control ratios were used to investigate potential risk factors for this outbreak
Cases Definition
Probable cases: In the absence of a more likely diagnosis, any person with generalized rash illness of acute onset that does not meet the criteria for suspected or confirmed rubella or any other illness
Suspected Cases: Any person with signs and symptoms consistent with rubella clinical criteria (Generalized maculopapular rash; Fever; arthralgia; arthritis; lymphadenopathy; or conjunctivitis) and lack of epidemiologic linkage to a laboratory-confirmed case of rubella; and no serologic or virologic tests [4]. Confirmed Case definition:
A suspected case which has laboratory evidence of rubella infection confirmed by one or more of the following laboratory tests: isolation of rubella virus; or detection of rubellavirus specific nucleic acid by polymerase chain reaction; or significant rise between acute- and convalescent-phase titers in serum rubella immunoglobulin G antibody level by any standard serologic assay; or positive serologic test for rubella immunoglobulin M (IgM) antibody [3].
Epidemiologic linkage case: A suspected case which has not been adequately tested by laboratory or a suspected case who has close contact with an individual positive serologic test for rubella immunoglobulin M (IgM) in proximity for a prolonged time period [3].
Epidemic Threshold
Confirmed Rubella outbreak
The epidemic threshold for this outbreak is defined as the occurrence of three or more confirmed rubella cases (at least two of which should be laboratory confirmed; IgM positive) within one-month period per kebele/ health facility/ Woreda [12].
Suspected Rubella Outbreaks
defined as the occurrence of five or more suspected Rubella cases in one month in a defined geographic area such as a kebele, Woreda or health facility catchment [12].Mixed Outbreak
If at least one case is positive for measles and at least one case is positive for rubella, the outbreak is designated to be mixed outbreak.
Surveillance and Response
The district health office reported suspected Measles/ Rubella cases on Jun 2/ 2018 to zonal health department. On the same days Asossa zone health department also verified and report the cases to Regional health bureau public health emergency management through a weekly aggregated report on WHO epidemic week 19; than we communicate with concerned bodies for the verification of suspected outbreak. Having concerned problem Benishangul Gumuz Regional Health Bureau PHEM field base had sent field epidemiology residents to the outbreak site for further investigation. The team was mobilized to the area and directly contact with Woreda Health office vice head and PHEM focal person about the root cause, aggravating factors relating to the outbreak and the response under action. After dealing some issue about the cause and early preparedness and response. We also directly discussed with Woreda RRT about the causes and how we proceed the way of the outbreak investigation. Team were established for further control of the outbreak in the Woreda and mobilized to the affected Kebele.
Laboratory Investigation
To identify the etiologic agent of the outbreak five blood samples were collected and sent to Ethiopian Health and Nutrition Research Institute (EHNRI) for laboratory confirmation. After a week, the report revealed two out of five samples were positive for measles IgM with the Positivity rate was 40%. Line list was also created to collect information about cases and was maintained throughout the outbreak.
Operational Definition
House ventilation
A living house consist at least one functional window for air ventilation.
Knowing modes of transmission
A person responds the mode transmission of measles disease from infected person to the uninfected individual via droplet (sneezing, cough).
Nutritional status
Nutritional status of children aged 6-59 months was determined by measuring the middle upper arm circumference (less than 12 cm is taken as malnutrition).
Data Collection Procedure
Semi structured questionnaire was prepared based on basic epidemiological information, sign and symptoms, rash onset, medical care and possible risk factors for rubella outbreak and transmission. The information on potential risk factors was collected from the caregivers of cases and controls in the community. Line list were also created to collect information about cases and was maintained throughout the outbreak.
Data Analysis
All the quantitative data from questionnaires and line list were entered on a computer and analyzed using a computerized data base Epi info 7, Microsoft office excel 2010 and SPSS version 20. Arc GIS was also used to indicate the spatial distribution of the diseases. Descriptive statistics and odds ratios (OR) with 95% confidence intervals (CI) were calculated to compare risk factors among cases and controls.
Ethical Consideration
The study was conducted after taking Permission from Benishangul Gumuz Regional Health Bureau. After discussing the purpose and method of the study with woreda health office head and PHEM Focal person, they were convinced to write a letter to selected kebele Written informed consent was obtained from study participants.
Result
Descriptive epidemiology
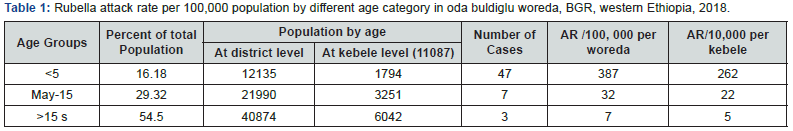
A total of 57 suspected rubella Cases and zero death were reported from June 9-22/2018. The case was reported only from one kebeles of the district. Throughout the outbreak the overall attack rate (AR) of rubella was 76 per 100, 000 populations, with zero case fatality rate. The attack rate was highest (390 cases per 100,000 populations) among less than five years age group. Secondary attack rate was 52/100,000 population. At Kebele level (daleti) the attack rate (AR) of rubella was 514 per 100,000 populations. The index case was a 3 years old male patient and he was registered at health facility on Jun nine, 2018, but he reported that sign and symptoms of the disease started on June five/2018. The index case had travel history to Asossa woreda with his family two weeks before (on May 23/2018) the onset of rash and contact with his relative who came from Menge woreda Keshaf kebele, who had probable signs and symptoms of measles. He returned to daleti kebele on May 29/2018. The dates of exposure are to be expected from May 23-29/2018.The average incubation period for rubella was expected to be 17 day (12-22day). The district reports the outbreak when the case riches at maximum level.
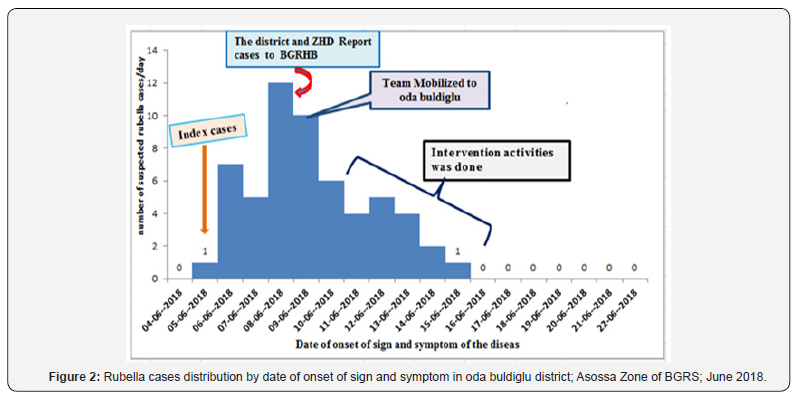
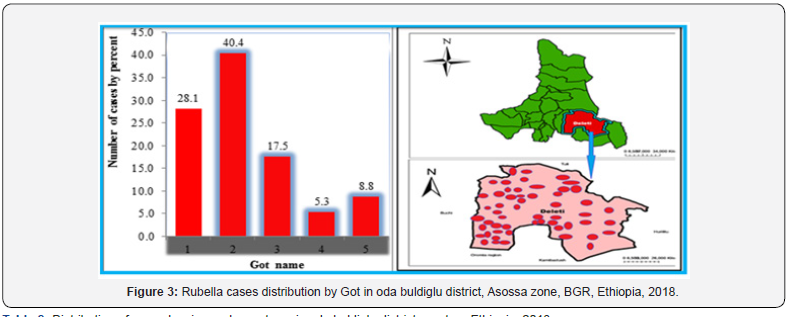
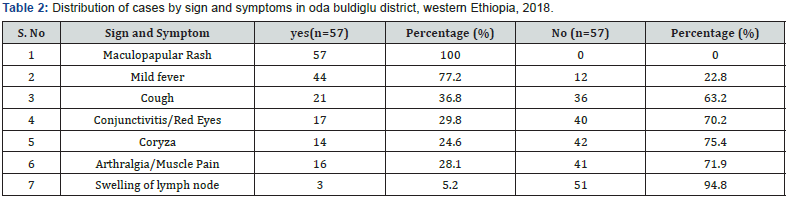
The case builds up gradually to reach its peak on June 8, 2018.The overall shape of the outbreak suggested propagated type of outbreak (Figure 2). From a total of fifty-seven suspected rubella cases registered on the line list, 34(60%) were females. The age range of cases was from 6 months to 26 years with the median age of 2 years. The mean age of the case was 3years and 6 months. Higher proportion of the cases 47(82.5%) were in the age category of under five years. Rubella outbreak was occurred only one kebele of the district; which is called daleti. The kebele has five gots. From this got two (40.4%) and got one (28.1%) were mostly affected area of the kebele. The rest three got of the kebeles have accounted only 31.6% of cases (Table 1). (Figure 3) Concerning to the clinical signs and symptoms, majority of the cases present with rash and milled fever. While other signs and symptoms like, cough, Coryza, conjunctivitis and swelling of lymph node also present in some patients. All ceases were cured after managed with appropriate antibiotics like vit A; TTC eye ointments; and amoxicillin. During the outbreak period there was no reported complications due to Rubella infection (Table 2).
Analytical Epidemiology
We compared 57 rubella cases with 114 community controls unmatched by sex, age and Place of residence. From this 23(40.3%) cases and 69(60.5%) of controls were male. Two third (64.3%) of participants were found less than five years age group. A total of 48(84.2%) cases and 94(82.5%) had a recent history of measles vaccination while All cases and controls did not get rubella vaccine. Descriptive statistics and odds ratios with 95% confidence intervals were calculated to compare risk factors among cases and controls. In the bivariate analysis; having poor knowledge on rubella mode of transmission (COR=2.787, 95% CI=1.247- 6.229), having contact with a person who had sign and symptoms of Rubella (COR: 10.18, 95% CI: 4.868 -21.30) and living in unventilated house (COR=4.455, 95%CI: 2.114-9.388) were significantly associated with this rubella outbreak (Table 3).
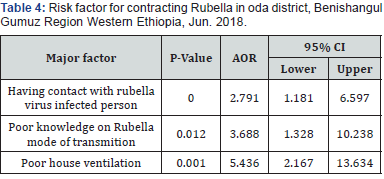
The above variables which showed a statistically significant association in the binary logistic regression model and variable having p value less than 0.3 in binary logistic regression model were entered into multiple logistic regression analyses models to assess their independent effect on the use of antenatal care services. However, on the multiple logistic analysis; having contact with a person with active rubella cases (AOR: 2.791; 95%CI: 1.181-6.597), having Poor knowledge on Rubella mode of transmition (AOR: 3.688; 95%CI: 1.328-10.238) and Poor house ventilation (AOR: 5.436; 95% CI: 2.167-13.634) had significantly associated with this rubella outbreak (Table 4).

The following activities were done in order to control the rubella outbreak: - Sensitization of Health Workers, Village Health Workers, and the community at large; active case search, contact tracing and line listing of cases were done in the community. Cases were managed with appropriate supportive medication like Vit A, antibiotics and TTC aye ointment. Isolation of rubella case was done both at home and school until he/she recovers. Daily situation monitoring, assessing risk factors and case management were strengthened. Intensive health education on Measles and rubella were given at school and community level.
Discussion
Several factors may have contributed for the occurrence of this outbreak. The results of the investigation revealed that all (100%) had never been vaccinated against rubella infection. This result is similar with study conducted tin Bambasi, and Sherkole district of the region, which indicates that 100% had never been vaccinated against rubella infection [15,16]. It is also Similar with rubella outbreak investigation conducted in Miyo Woreda of Borena zone in Oromia Region also indicate 100% of the cases had never vaccinated rubella vaccine [17]. This might be one of the risk factors contributing for the occurrence of the outbreak. Rubella vaccination plays a major role in the prevention of rubella by offering lifelong immunity; However, Ethiopia did not introduce rubella vaccine yet. This might be due to uncommon Rubella outbreak in Ethiopia and the disease is not targeted as priority disease and there is no set of prevention and control strategy.
The index cases had history had travel history to other area with his family 1 to 2 weeks before onset of rash and he had been in contact with persons who came from other area with active Rubella outbreak (Keshaf kebele of Menge district). This might imply that the outbreak came from Menge woreda Keshaf kebele and spread within the community. Rubella infection showed a clear seasonal pattern, higher in the hot dry season of the region (February to June) reaching a peak in March. This seasonal pattern was similar to findings from previous studies conducted from different country of the world [14-18]. Most rubella outbreaks occurred in dry season of the country. Majority of the cases (94.7%) occur under fifteen years old. This might be one of the risk factors contributing for the occurrence of the outbreak. This result is also similar with other study conducted from different part of the country [16,17,19]. This might be due to those age groups are mostly affected by nutritional problems and intestinal parasitic diseases than other age groups of the population.
The study showed that poor ventilation of the house was significantly contributed for the occurrence of the outbreak. Persons who live in unventilated house were five times more likely attacked by rubella than persons who live in ventilated house. Which is Similarly with rubella outbreak conducted in Oromia region, it documented that poorer ventilation was a stronger risk factor for gaining of rubella [18]. This might be due to spreading of the rubella infection to others through sneezing and coughing in unventilated house was high. This finding is also biologically plausible considering that rubella is spread through respiratory secretions.
Contact with rubella vires infected person was a significant risk factor for contracting rubella outbreak in oda buldiglu Woreda. The study verifies that persons who have contact with rubella vires infected persons were two times more likely attacked by rubella than who had no contact with infected person. Children contracted rubella from their relatives at school and home during contact with infected person. This implies that isolation at home could have stopped the spread of rubella to non-school going children. This was consistent with the study done in pastoralist community of the Ethio-Kenyan Boarder of Miyo district; Kafta Hummera district of Tigray region and study conduct in Bambasi district [16-18]. In the outbreak situation, isolation of infected person with Rubella virus is the major prevention and control mechanism.
Care givers perceived rubella as measles which are almost similar in terms of signs and symptoms. Where there was significant difference in knowledge of rubella mode of transmission between cases and controls. The result of the study shows persons who have Poor knowledge on rubella mode of transmission were three times more likely attacked by rubella and it has significant associated with this outbreak, this finding is also similar to case control study conducted in Zimbabwe, which shows persons who have poor knowledge on rubella mode of transmission were more likely attacked by rubella disease than who have good knowledge on mode of transmission [19]. This might be due to Knowing mode of rubella transmission might help the caregivers to protect their children from contact with infected person.
Limitation of the study
These results are subject to few limitations. Many individuals with rubella cases may not have any significant fever, and some individuals with rubella cases may present without a rash or have subclinical illness. The sensitivity of this case definition is likely not high enough to identify all rubella cases.it may lead to Selection bias on controls selection.
Conclusion
We investigate rubella outbreak in oda buldiglu Woreda in Asossa zone of benishangul guz region of Ethiopia. The district health offices detect and report the outbreak when it reaches at maximum level or lat. The index cases had travel history and had contact with a person who came from an area where cases of Rubella were reported. Rubella infection showed a clear seasonal pattern, higher in the hot dry season of the region (February to June) reaching a peak in March. Rubella infection is predominantly found in those who are younger than 15 years old. Respondent’s poor knowledge on rubella mode of transmission, having contact with rubella infected person and housing condition with poor ventilation were significantly associated with this rubella outbreak. Case - contact tracing and case management was good in the district. The investigation team recommends to the Regional Health Bureau in collaboration with the FMOH together to plan towards the introduction of rubella vaccine in to the country’s immunization programme for the sustainable prevention and control of the cases. The surveillance system should be strengthening at all level in order to detect case early as much as possible. The investigation team also recommends the district health office to Restocking emergency drugs and supplies that are running out; to strength and Continues Health Education of the community on Ways of transmissions and prevention activities; to strengthen Sensitization of health workers to improve the awareness of the community towards rubella infection.
Acknowledgment
I would like to thank all that participated in the process of Measles and Rubella surveillance in the Region, particularly surveillance officers working on detection, investigation, and outbreak management at all levels. Our appreciation also goes to health workers and the community at various levels who directly or indirectly supported and contributed for outbreak investigation in the district. Last but not least i would like to acknowledge my adviser and mentors Mr. Yaregal Animut, Mr. Getachew Abebe, Mr. Fikadu Ayalewu and Mr. Gizachew Yaregal for their overall support throughout my work.
References
- WHO (2018) Global Measles and Rubella Strategic Plan from 2012 to 2020.
- (2013) Missouri Department of Health and Senior Services Communicable Disease Investigation Reference Manual, Rubella and Congenital Rubella Syndrome.
- Eliminating Measles, Rubella & Congenital Rubella Syndrome (CRS) Worldwide, CDC, Global Health.
- WHO (2014) Recommended surveillance standard of rubella and congenital rubella syndrome.
- WHO (2013) Guidelines on Measles and Rubella Surveillance and Outbreak Investigation and response in the WHO European region.
- The immuniation advisory center (2017) Fact sheeton Rubella (German measles).
- South MA, Sever JL (1985) Teratogen update: the congenital rubella syndrome. Teratology 31(2): 297-307.
- Miller E, Cradock-Watson JE, Pollock TM (1982) Consequences of confirmed maternal rubella at successive stages of pregnancy Lancet 2(8302): 781-784.
- Gavin B. Grant (2017) US Department of Health and Human Services/Centers for Disease Control and Prevention Progress, in Rubella and Congenital Rubella Syndrome Control and Elimination-Worldwide 66(45): 1256–1260.
- Upreti SR, Thapa K, Pradhan YV, Shakya G, Sapkota YD, et al. (2011) Developing Rubella Vaccination Policy in Nepal-Results from Rubella Surveillance and Seroprevalence and Congenital Rubella Syndrome studies , Rubella Vaccination Policy in Nepal. J Infect Dis 1: S433-8.
- Danovaro H et al (2003) American Journal of Public Health. Peer Reviewed Research and Practice 93(2): 289.
- N, et al. (2016) Worldwide Epidemiology and Current Control, Elimination and Eradication Policies, Lancet. Author manuscript.
- M, et_al. (2011) Epidemiology of rubella diseases in ethiopia data from the measel case based survelance system and progress in measel mortality redaction in ethiopia from 2002-2009.
- Mekonen G, Berhane B, Kathleen G, Ayesheshem A, Birke T, et_al. (2016) Epidemiology of rubella virus cases in the pre-vaccination era of Ethiopia, 2009–2015 BMC Public
- Gizachew Y Taye (2017) Rubella Outbreak Investigation in Sherkole Woreda of Assosa Zone: Benishangul Gumuz Regional State: Western Ethiopia, AAU.
- Sharewu S Rubella Outbreak Investigation in bambasi Woreda of Assosa Zone: Benishangul Gumuz Regional State: Western, Ethiopia.
- Birhanu KS (2013) Rubella outbreak investigation in Miyo Woreda of Borena zone in Oromia Region, AAU.
- Alefech A (2013) Rubella outbreak investigation Kafta Hummera District, western zone of Tigray Region; AAU.
- Makoni AC, Chemhuru M, Bangure D, Gombe NT, Tshimanga M, et_al. (2015) Rubella outbreak investigation, Gokwe North District, Midlands province, Zimbabwe, 2014 - a case control study. pan African medical journal 22: 60.






























