Ulnar Nerve Reconstruction in High Level Injuries
Hosseinali Abdolrazaghi1, Javad Rahmati2 and Hojjat Molaei1,2*
1 Department of hand & reconstructive surgery, Tehran University of Medical Sciences, Iran
2 Department of plastic & reconstructive surgery, Tehran University of Medical Sciences, Iran
Submission: April 24, 2021;Published: May 17, 2021
*Corresponding author: Hojjat Molaei, Department of hand, Plastic & reconstructive surgery, Sina Hospital, medicine school, Tehran University of Medical Sciences, Tehran, Iran, Valieasr Hospital, IKHC, Bagherkhan St, Towhid Sq, Tehran, Iran
How to cite this article: Hosseinali A, Javad R, Hojjat M. Ulnar Nerve Reconstruction in High Level Injuries. JOJ Orthoped Ortho Surg. 2021; 3(1): 555603.DOI: 10.19080/JOJOOS.2021.03.555603
Abstract
Introduction: High level ulnar nerve injuries are among devastating events need more specialized corrections. As a rule, primary repair leads to better outcomes. But in case of failure, other options should be considered.
Patients and Methods: 10 patients who had unsuccessful primary repair underwent secondary nerve reconstruction with nerve graft and had hand therapy sessions. Then, selective muscle evaluations were done for each patient.
Results: Patients were young (mean age 20.9) and had their primary surgery in a few days after high level ulnar nerve trauma. Their secondary operation was about 20.66 months later. Sural nerve graft length was about 7.9 cm. Again, after approximately 6.3 months muscles` function evaluated. FCU and FDP 4,5 muscles MMT were acceptable.
Conclusion: Results of secondary ulnar nerve reconstruction with nerve graft in high injuries, is not always disappointing and good wrist flexion and grip can be expected.
Keywords: High level; Ulnar nerve injury; Reconstruction
Introduction
Upper limb injuries associated with nerve disruptions are disabling and challenging. Complete high ulnar nerve injury usually resulted in severe sequelae, such as residual sensation, loss of movement, and “claw hand” deformity, and affects fine manipulation of the hand [1]. So, high ulnar nerve injuries are often forbidden by surgeons to approach. Though, there are several interfering factors to reach acceptable outcomes, such as patient`s age, type of lesion and repair, interval between trauma and reconstruction [2], most of hand surgeons believe in disappointing serial operations in high ulnar nerve injuries. Mixture nature of ulnar nerve predisposes its repairmen more troublesome as one of most difficult issues in micro-neurosurgery, and motor and sensory function outcomes are frustrating [3]. Historical experiences in high ulnar nerve injury reconstruction, push surgeons away from high ulnar repairs, especially in brachial injuries and tempt them to sacrifice ulnar nerve as nerve graft in other nerve reconstructions. Whereas we gathered follow/up data in patients with high ulnar nerve or medial cord injuries, who underwent reconstructions and gained acceptable functions despite loss of fine hand abilities.
Patients and Methods
The study established at Sina University Hospital, Iran, between August of 2018 and August of 2019. Consecutive adult patients who were scheduled to undergo ulnar nerve reconstruction procedure in the surgical department were invited to participate in the study. Patients with a known low ulnar nerve injuries were excluded. Upon written informed consent, patients were entered the study. At last, 10 patients completed evaluation. Those are clients who had underwent secondary reconstructive operations following unsuccessful primary upper ulnar nerve repairs. All the patients received nerve grafts from sural nerve, and after recovery period, had physiotherapy cessions. Manual Muscle Testing, of involved muscles (MMT) was done and recorded accordingly. Manual muscle testing is a standard grading system to evaluate the muscle function. This descriptive information gathered and represented to demonstrate associations.
Results
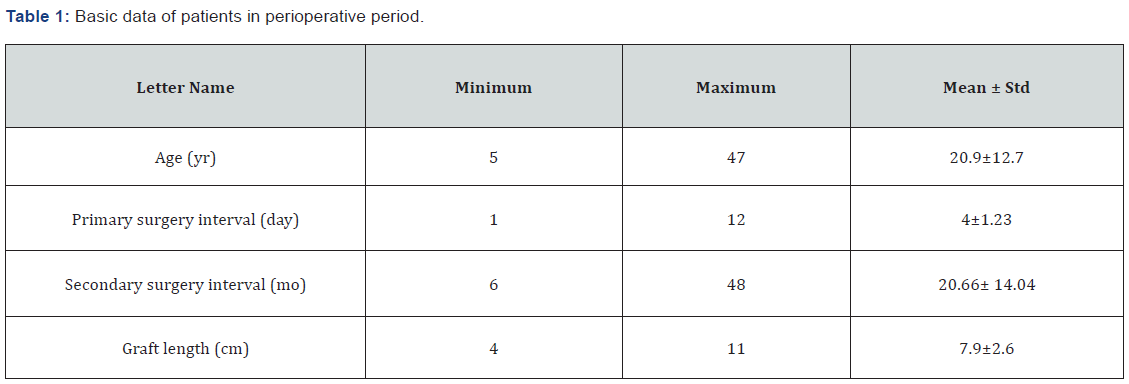
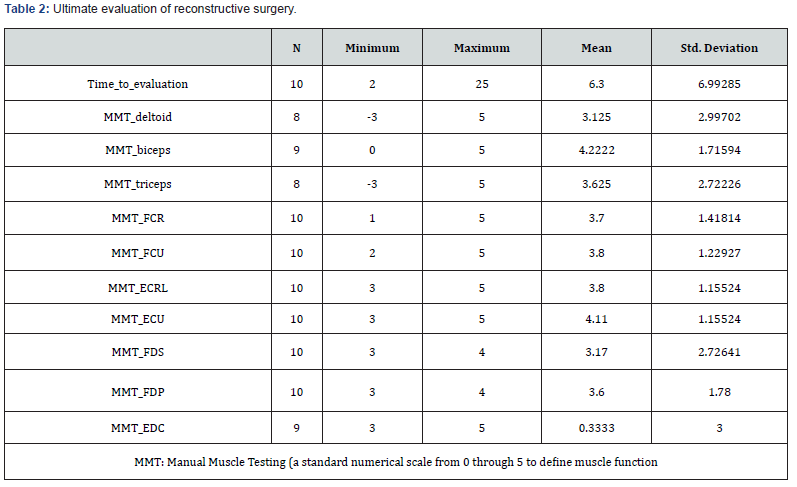
10 patients completed evaluations and questionnaire and entered the study. They are not old and the mean age was 20.9 as illustrated in Table 1. Patients had been operated one day to 12 days after injury in the primary hospital as simple nerve repair (mean 4 day ± 1.23). They had injuries in the brachial plexus or high-level injuries of ulnar branch with or without concomitant nerve or vascular injuries. Their surgery was nerve cooptation by fine sutures. All 10 patients had regular physiotherapy for months. But, when there was not acceptable progress in upper limb function, they were referred by hand therapist for more intervention. Second operations were done in our referral center, about 6 to 48 Months later (mean 20.66 ±14.04 months) according to patients` admission and surgery. During second surgery, fibrotic tissues and non-functional neural tissues were debrided and sural nerve graft was used to fill the gap. The length of graft was 7.9± 2.6 cm. after recovery period. All the patients underwent rigid hand therapy sessions and about months later (mean 6.3) were assessed as demonstrated in Table 2. Despite long distance to FCU muscle innervation, the mean MMT was 3.8 and patients had acceptable wrist flexion without radial deviation. Moreover, the mean MMT of FDP 4, 5 was 3.6± 1.78 and patients showed good pinch function. However internal hand muscle had weak functions as we expected. One of those patients who evaluated after about 6 months was shown in video 1.

Discussion
As the nerve regeneration rate is approximately 1–2 mm/d (3) and extra time is required for regeneration to reach the intrinsic muscles of the hand than proximal muscles. Thus, proximal muscle strength recovery is more significant than intrinsic muscles for fine movements is poorly recovered [1]. Though, previous studies suggested that primary epineural repair of an injured ulnar nerve has predictable function in childhood compared adults, and the level of injury has less impact upon outcome, and good intrinsic motor recovery can be expected [4]. However, generally authors believe in impact of injury level on final outcome.
Ghoraba et al. [5] presented their novel classification for ulnar nerve injuries according to zone of injury as illustrated here:
a) Zone (I): Extends distal to the proximal hiatus of Guyon’s canal.
b) Zone (II): Extends from the proximal hiatus of Guyon’s canal to the proximal border of the pronator quadratus
c) Zone (III): Extends from the proximal border of the PQ to the first motor branch of the ulnar nerve.
d) Zone (IV): Extends proximal to the first motor branch of the ulnar nerve (5) and introduced their suggestive treatment protocols. Accordingly, they recommended nerve graft plus adjuvant therapies to reach better outcomes.
Emamhadi et al. [6] in a comprehensive study on their patients confirmed advantage of primary on nerve graft and the importance of defining ulnar nerve topography in repair outcome. They considered that better outcome can be achieved for lesions in continuity compared to lesions not in continuity, and finally suggested to repair ulnar nerve injuries to have predictable results [6]. However, In order to improve outcome after various procedures for a nerve injury, especially ulnar nerve injury, care givers should be aware of the risk for severe disability and complex regional pain syndrome may happen following reconstruction and seek appropriate solutions [7]. Grinsell et al. [8] discussed on peripheral nerve reconstruction and mentioned timeframe for reinnervation of sensory receptors is much longer than that for motor nerves but earlier repair still results in better sensory outcomes [8]. Our patients waited for months even years to gain hand function, but eventually returned for more surgeries. The mean length of nerve graft in our cases was 7.9 cm, though He et al. [9] evaluated factors predicting nerve recovery following repair and concluded gaps less than 5 cm have better outcome [9]. Woo et al. [10] mentioned successful outcomes following ulnar nerve repair were defined by the recovery of M4 strength and S4 sensation and more improvement for up to 5 years due to continuing nerve regeneration and innervation and maybe psychological adaptation to the new patterns of innervation [10], an enhanced belief which admired us to keep patients as close as possible and encourage more exercises. Similarly, Barrios et al. [11] previously had pointed to the importance of nerve graft, especially in motor nerves, on final outcome and confirmed this 5 cm graft threshold [11]. So, it is noteworthy that, ulnar nerve is not ignorable in high level injuries, as some decide to sacrifice it as a graft for other nerves. Though fine hand function may compromise, but every labor with gross upper limb functions can do much compared to disabled hand and secondary reconstruction of ulnar nerve with nerve graft may reach this milestone.
Conclusion
Our restricted study on our high-level ulnar nerve injury patients who underwent reconstruction following failure of primary repair, again faded up past disappointments in this era, and suggested surgeons to consider secondary ulnar nerve reconstruction.
References
- Ding W, Li X, Pan J, Zhang P, Yin S, et al. (2020) Repair Method for Complete High Ulnar Nerve Injury Based on Nerve Magnified Regeneration. Ther Clin Risk Manag 16:155-168.
- Post R, de Boer KS, Malessy MJA (2012) Outcome following Nerve Repair of High Isolated Clean Sharp Injuries of the Ulnar Nerve. PLoS One 7(10): e47928.
- Pfaeffle HJ, Waitayawinyu T, Trumble TE (2007) Ulnar nerve laceration and repair. Hand clinics. 23(3): 291-299.
- Costales JR, Socolovsky M, Sánchez Lázaro JA, Álvarez García R (2019) Peripheral nerve injuries in the pediatric population: a review of the literature. Part I: traumatic nerve injuries. Childs Nerv Syst 35(1): 29-35.
- Ghoraba SM, Mahmoud WH, Elsergany MA, Ayad HM (2019) Ulnar Nerve Injuries (Sunderland Grade V): A Simplified Classification System and Treatment Algorithm. Plast Reconstr Surg Glob Open 7(11): e2474.
- Emamhadi M, Alijani B, Ghadarjani S (2015) Surgical Outcome of Ulnar Nerve Lesions: Not Always Disappointing. J Neurol Stroke 3(6): 00115.
- (2017) EFORT Open Rev. Originally published online at www.efortopenreviews.org
- Grinsell D, Keating CP (2014) Peripheral nerve reconstruction after injury: a review of clinical and experimental therapies. Biomed Res Int 2014: 698256.
- He B, Zhu ZW, Zhu QT, Zhou X, Zheng C, et al. (2014) Factors predicting sensory and motor recovery after the repair of upper limb peripheral nerve injuries. Neural Regen Res 9(6): 661-672.
- Woo A, Bakri K, Moran SL (2015) Management of Ulnar Nerve Injuries. J Hand Surg Am 40(1): 173-181.
- Barrios C, Amillo S,Pablos J, Cañadell J (1990) Secondary repair of ulnar nerve injury: 44 cases followed for 2 years, Acta Orthopaedica Scandinavica 61(1): 46-49.






























