Obturator to Femoral Nerve Transfer for Femoral Nerve Palsy Using a Modified Technique
*David Graham and Richard Lawson
Department of Hand and Peripheral Nerve Surgery, Royal North Shore Hospital, Australia
Submission: April 25, 2017; Published: May 11, 2017
*Corresponding author: David Graham, Department of Hand and Peripheral Nerve Surgery, Royal North Shore Hospital, Reserve Rd, St Leonards 2065, NSW Australia, Email: davidgraham80@gmail.com
How to cite this article: David Graham and Richard Lawson . Obturator to Femoral Nerve Transfer for Femoral Nerve Palsy Using a Modified Technique. JOJ Orthoped Ortho Surg. 2017; 1(2): 555556. DOI: 10.19080/JOJOOS.2017.01.555556
Introduction
Though uncommon, femoral nerve palsies are potentially devastating injuries which can occur as a result of penetrating trauma or malignancies, however the most common cause is inadvertent iatrogenic injury following intra abdominal surgery such as gynaecological/vascular surgery or total hip replacement [1]. We present a case of iatrogenic femoral nerve injury with a delayed presentation resulting in an 8.5cm nerve defect, which was managed with both traditional cable grafting and a contemporary nerve transfer utilising a modification of an existing technique.
Case Report
In September 2015 a 49 year old female presented to our institution 6 months following a laparoscopic inguinal hernia repair which had resulted in a complete transection of the right femoral nerve. There was a 6 month delay in diagnosis of the iatrogenic injury. The patient had an extraperitoneal exploration of the right groin which confirmed the diagnosis, and an 8.5cm nerve defect at the level of the inguinal ligament was cable grafted with 4 cables sural nerve grafts. After discussion with the patient and appropriate review of the literature and cadaver dissection, the patient had a nerve transfer procedure 3 weeks following the cable grafting.
Procedure 1
In conjunction with General Surgical colleagues a supra- inguinal extraperitoneal approach was performed exposing the femoral neurovascular bundle in the right iliac fossa. This incision was then extended distally and the inguinal ligament was divided and later repaired for exposure of the nerve. A prominent neuroma was identified where the nerve was divided, associated with mesh and metallic tacs from the hernia. Ipsilateral sural nerve was harvested and a reversed cable graft using four 8.5cm cables was used to close the defect.
Procedure 2
Nineteen days after the first operation an obturator to femoral nerve transfer was performed. An anterior longitudinal incision incorporating the existing scar was used to expose the distal end of the cable graft, the distal femoral nerve and its terminal branches. The medial sensory branch and the branches to the rectus femoris and vastus lateralis were identified and the latter two confirmed to be non functional with electrical stimulation. The anterior branch of the obturator nerve was identified and traced distally to identify the branch entering gracilis. The nerve to gracilis was transected distally and passed over the adductor longus muscle to reach the femoral nerve. It was then redirected sub muscularly under the adductor longus muscle (Figure 1). With this more direct route, the end of the gracilis branch was able to reach four centimetres more distally. The nerve to gracilis was then neurotised to the femoral nerve branch to rectus femoris. The neurotisation was undertaken under microscope magnification with 9-0 S&T sutures (Insert Trade Details) and reinforced with Tiseel™ fibrin glue (Baxter pharmaceuticals).
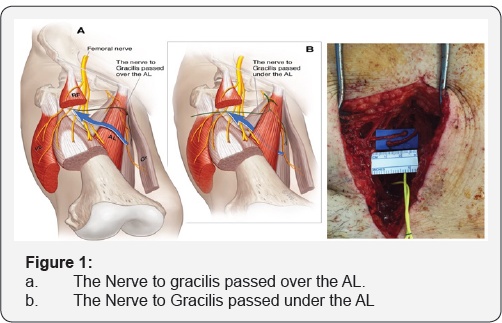
Discussion
Complete femoral nerve injuries are uncommon and usually leave the patient with significant morbidity, requiring orthoses for simple mobility. Traditionally a nerve defect of this size would be managed with autologous cable grafting as initially performed. The large size of the nerve defect and also the significant distance from the distal end of the graft to the neuromuscular junction result in a poor prognosis for functional recovery. Whilst tendon transfers provide a good reconstructive option for some neurological injuries, (example radial nerve palsy), there are few satisfactory options available for femoral nerve palsy. Fischer et al. [2] reported on a hamstring transfer after soft tissue sarcoma resection with significant complications and modest results of extension force.
Nerve transfers have been well described in the literature for upper limb reconstruction [3]. There is in contrast a paucity of reconstruction options in lower limb nerve injury. Nerve transfers provide an attractive option, as performing the neurotisation distally minimises the distance and hence time required for neural regeneration and ultimately functional recovery. Motor end plates are known to undergo extensive change post denervation and functional reinnervation is unlikely beyond 18 months due to progressive fibrosis [4]. This case also posed further time pressure as referral to our institution was delayed by 6 months since the nerve injury. By performing the second procedure of the obturator to femoral transfer, viable axons were delivered approximately 13cm closer to the neuromuscular junctions providing greater potential for reinnervation prior to loss of the motor end plates.
The pattern of the femoral nerve branching pattern has been previously described in a cadaver dissection by Tung et al. [3]. There have only been two previous papers in the literature discussing case reports of 3 similar procedures. Campbell et al. [5] reported a single case of total obturator to femoral nerve transfer 3 months post schwannoma resection with good functional result. This was performed above the inguinal ligament. Goubier et al. [6] conducted a cadaveric feasibility study in 2012 confirming the possibility of performing a subcutaneous transfer of two obturator motor branches to the femoral nerve in the thigh.
Tung et al. [3] reported on 2 cases of a subcutaneous obturator to femoral nerve transfer for complete femoral nerve injury- 1 performed acutely and the other 5 months post injury. The second patient was also supplemented with a superior gluteal nerve transfer after the first patient had incomplete recovery and an inability to climb stairs. This showed encouraging results. In our patient we have combined the existing obturator to femoral nerve transfer and added a cable graft in an attempt to provide a belt and braces reconstruction. We also determined that directing the gracilis branch deep to adductor longus rather than superficial to this muscle provides an increase in effective length of the nerve, allowing a more distal nerve repair, which is theoretically beneficial.
Iorio et al. [7] noted the proximity and potential of the anterior branch of the obturator nerve to gracilis in femoral nerve injuries. In their cadaveric study they proposed using this nerve for a donor for cable grafting, hypothesising that a motor nerve may maximise functional outcomes. They also noted that the average donor length was 11.4cm. The anterior branch of the obturator nerve has also been considered for restoring other neurological losses. In a cadaveric study in 2014, Houdek et al. [8] deemed it feasible to transfer the anterior branch of the obturator nerve to pelvic nerves in order to restore bowel and bladder function. Interestingly Spiliopoulos et al. [9] published a case report of the reverse nerve transfer - femoral branch to obturator to restore adduction following another iatrogenic injury. They reported a good outcome with full power and normal gait.
Conclusion
We present a novel 'belt and braces' approach for managing this unusual injury, using a modification of a nerve transfer which has only been reported in the literature three times previously to our knowledge.
References
- Kim DH, Murovic JA, Tiel RL, Kline DG (2004) Intrapelvic and thigh level femoral nerve lesions: Management and outcome in 119 surgical treated cases. J Neurosurg 100(6): 989-996.
- Fischer S, Soimaru S, Hirsch T, Kueckelhaus M, Seitz C, et al. (2015) Local tendon transfer for knee extensor mechanism reconstruction after soft tissue sarcoma resection. J Plast Reconstr Aesthet Surg 68(5): 729-735.
- Tung TH, Chao A, Moore AM (2012) Obturator nerve transfer for femoral nerve reconstruction: anatomic study and clinical application. Plast Reconstr Surg 130(5): 1066-1074.
- Lee SK, Wolfe SW (2000) Peripheral nerve injury and repair. JAAOS 8(4): 243-252.
- Campbell AA, Eckhauser FE, Belzberg A, Campbell JN (2010) Obturator nerve transfer as an option for femoral nerve repair: case report. Neurosurgery 66(6): 375.
- Goubier JN1, Teboul F, Yeo S (2012) Transfer of two motor branches of the anterior obturator nerve to the motor portion of the femoral nerve: an anatomical feasibility study. Microsurgery. 32(6): 463-465.
- Iorio ML, Felder JM, Ducic I (2011) Anterior branch of the obturator nerve: a novel motor autograft for complex peripheral nerve reconstruction. Ann Plast Surg 67(3): 260-262.
- Houdek MT, Wagner ER, Wyles CC, Moran SL (2014) Anatomical feasibility of the anterior obturator nerve transfer to restore bowel and bladder function. Microsurgery 34(6): 459-463.
- Spiliopoulos K, Williams Z (2011) Femoral branch to obturator nerve transfer for restoration of thigh adduction following iatrogenic injury. J Neurosurg 114(6): 1529-1533.






























