Free Groin Flap for Soft Tissue Coverage of the Lower Legin Oncological Surgery: A Case Report
*Veena Singh
Assistant Professor, All India Institute of Medical Sciences Patna, India
Submission: April 14, 2017; Published: May 02, 2017
*Corresponding author: Veena Singh, Assistant Professor, All India Institute of Medical Sciences, Patna, Bihar, India, Email: drsveena@gmail.com
How to cite this article: Veena S. Free Groin Flap for Soft Tissue Coverage of the Lower Legin Oncological Surgery: A Case Report. JOJ Orthoped Ortho Surg. 2017; 1(1): 555554. DOI: 10.19080/JOJOOS.2017.01.555554
Abstract
The treatment of lower limb tumours has been shifted from limb amputation to limb salvage by advancements in adjuvant treatment protocols and microsurgical reconstruction. Standard approaches include oncological surgery by a multidisciplinary team in terms of limb sparing followed by soft tissue reconstruction and adjuvant therapy when indicated. For the development of a comprehensive surgical plan, the identity of the tumour should first be determined by histology after biopsy. Then the surgical goal and comprehensive treatment concept should be developed by a multidisciplinary tumour board and combined with soft tissue reconstruction. In this article, we present the reconstruction of soft tissue of lower third of the leg with free groin flap after oncological resection of squamous cell carcinoma (SCC).
Keywords: Free groin flap; Lower leg; SCC; Oncological
Introduction
A meticulous surgical technique is crucial to ensure an optimal oncological and functional outcome for the patient. Successful limb-sparing surgery consists of three interdependent stages performed in sequence as follows: tumour resection with appropriate oncological margins, reconstruction and stabilization of the involved bone and joints, and restoration of soft tissue envelope and restoration of function. After tumour resection of the lower extremity complex, defects are anticipated and multiple variables must be considered for soft tissue reconstruction. A large number of details must be taken into consideration when planning a reconstruction, especially after oncological surgery. One must consider the timing of reconstruction, size and location of the defect, involvement of neurovascular structures, and exposure or resection of bone, tendons, and nerves. Donor site morbidity, disease prognosis, and the patient's previous level of function and expectations of restored function must be evaluated as well. Reconstructive options for the lower leg with regard to local flaps are limited particularly for the lower third can be challenging, thus free flaps are often required.
Since first described by McGregor and Jackson in 1972 [1], the groin flap has been widely used in the field of reconstructive surgery. Numerous surgical techniques that use the pedicled [2,3] or free groin flap as a means of dealing with complex soft tissue injuries of the head and neck [4,5], as well as the extremities [5,6], have been described. The groin flap is an axial pattern flap based on the superficial circumflex iliac artery. This relatively constant vascular supply forms a cartwheel of anastomosing vessels that encompass a large area of the groin and hypogastrium, thereby allowing for a substantial amount of tissue to be utilized. We present a case report outlining an alternate use for this versatile flap.
Case Report
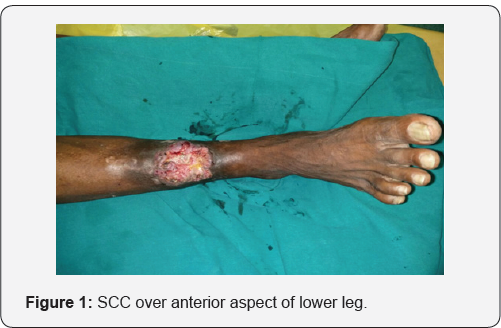
A 53-year old male presented with a fungating lesion of approximately 8 x 6 cms. Over the anterior aspect of lower third of right leg for last 2 months (Figure 1). There was no neurovascular deficit and not restriction in ankle movements. A biopsy was done which came out to be moderately differentiated squamous cell carcinoma. MRI was done which showed that the tibia was free. Hence, a plan was made for wide local excision (WLE) and cover of soft tissue defect with free groin flap.
Harvest of Free Groin Flap
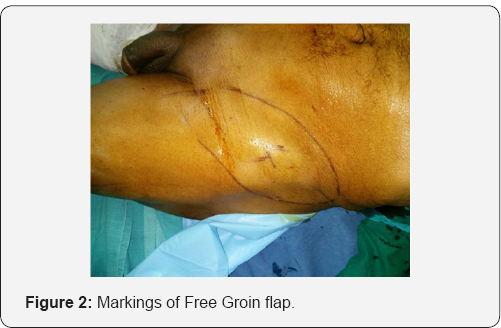
After the defect was measured, markings for groin flap were made according to standard recommendations (Figure 2). In this patient, groin flap was harvested from the contra lateral side for ease of two-team approach. In contrast to the conventional technique where the flap is elevated from medial to lateral, we start elevating the flap from lateral to medial. As the flap is raised from lateral side, the perforator to the skin is identified (Figure 3). This perforator is then skeletonised to its origin. Thus, it does not make any difference whether the perforator is from the superficial or the deep vascular system and the problem of the variability of the pedicle is solved. The perforator thus isolated is dissected distally in a plane between the superficial and deep layers of fat. This dissection is a little tedious and is done under an operating microscope. With this technique, we obtain a pedicle length of 5-7 cm which is sufficient in most cases.

Vascular Anastomosis
Recipient artery included the anterior tibial artery. Two venous anastomoses were performed in this patient, one to the great saphenous vein and other to the venae comitantes at the recipient sites. The donor site was closed primarily without complication. Good position and colour of flap inset was noted at the conclusion of the procedure (Figure 4).

Discussion
The aim of lower-extremity reconstruction has focused on wound coverage and functional recovery. The pedicled groin flap has long been accepted as a safe, easy and reliable option for the reconstruction of soft tissue defects [7]. The free flap has been successfully used for lower extremity reconstruction for the past many years. The selection of appropriate recipient vessels is an essential element for achieving successful treatment outcomes in the reconstruction of lower extremity defects using free flap [8]. The groin flap is based on the superficial circumflex iliac artery, which is supplied from the superficial femoral artery at the level of the inguinal ligament and drains into the saphenous system. The groin flap has several advantages including adequate skin thickness and minimal donor site morbidity, making it the most useable free flap for soft tissue coverage of the hand and forearm [1,9]. The disadvantages of the flap include the short pedicle and that the artery size can be small [1,9].
The authors stress that strict preparation as well as the appropriate selection of the recipient vessel which led to good results. As mentioned before, two anastomosis were performed for all of the veins. For the recipient vein, we tried to use one superficial vein and one deep vein whenever possible. Our aim in doing so was to drain the venous drainage of the flap to different sites. We selected the superficial veins whose ends were not exposed to the defect site whenever possible; however, as most deep veins were exposed to the defect site along with the recipient artery, we expected the deep veins to have been damaged along with the artery and applied a strict reference point for the intact vessel, as was done for arterial preparation.
References
- McGregor IA, Jackson IT (1972) The groin flap. Br J Plast Surg 25(1): 3-16.
- Arner M, Moller K (1994) Morbidity of the pedicled groin flap. A retrospective study of 44 cases. Scand J Plast Reconstr Surg Hand Surg 28(2): 143-146.
- Buchman SJ, Eglseder WA, Robertson BC (2002) Pedicled groin flaps for upper-extremity reconstruction in the elderly: A report of 4 cases. Arch Phys Med Rehabil 83(6): 850-854.
- Inigo F, Jimenez Murat Y, Arroyo O, Martinez BA, Ysunza A (2000) Free flaps for head and neck reconstruction in non-oncological patients: experience of 200 cases. Microsurgery 20: 186-192.
- Hough M, Fenn C, Kay SP (2004) The use of free groin flaps in children. Plast Reconstr Surg 113(4): 1161-1166.
- Barfred T (1976) The Shaw abdominal flap. Scand J Plast Reconstr Surg 10(1): 56-58.
- Chuang DC, Colony LH, Chen HC, Wei FC (1989) Groin flap design and versatility. Plast Reconstr Surg 84(1): 100-107.
- Basheer MH, Wilson SM, Lewis H, K Herbert (2008) Microvascular free tissue transfer in reconstruction of the lower limb. J Plast Reconstr Aesthet Surg 61(5): 525-528.
- Lutz BS, Wei FC, Chang SC, Yang KH, Chen IH (1999) Donor site morbidity after suprafascial elevation of the radial forearm flap a prospective study in 95 consecutive cases. Plast Reconstr Surg 103(1): 132-137.






























