Abstract
Purpose: To evaluate whether the use of face masks produces an alteration in the intraocular lens (IOL) calculation in patients undergoing cataract surgery.
Methods: A cross-sectional study including patients derived for cataract surgery was conducted over a period of three months during the
coronavirus disease (COVID-19) pandemic. Biometric measurements were taken using IOL Master 700 optical device (Carl Zeiss Meditec AG,
Jena, Germany). Four measurements were taken in each patient: two initial measurements with the face mask and another two measurements
after 10 minutes without wearing the mask.
Results: A total of 58 eyes of 29 subjects were included in the study with a mean age of 70.2 ± 10.5 years and 16 individuals being female
(55%). Mask wear did not show statistically significant differences in biometric values and IOL power calculation compared to the measurements
obtained without using the mask for all the parameters (p ≥ 0.05). Dahlberg´s error was usually close to 0, coefficient of variation (CV) did not
exceed 1% and intraclass correlation coefficient (ICC) was close to 1 in all cases.
Conclusions: There is a high degree of concordance between biometric measurements taken with and without the face mask, so no differences
were observed in the estimated IOL power calculation. However, it is advisable to analyses each case individually and prescribe appropriate
topical treatment if there are ocular surface symptoms related to mask use.
Keywords: Face mask; Dry eye; COVID-19; Biometry; Coronavirus Disease
Abbreviations:IOL: Intraocular lens; COVID-19: Coronavirus Disease 2019; CV: Coefficient Of Variation; ICC: Intraclass Correlation Coefficient; MADE: Mask-Associated Dry Eye; D: Diopters; AXL: Axial Length; DED: Dry Eye Disease; SD: Standard Deviation; CCT: central corneal thickness; WTW: White-To-White; IOLP: Intraocular Lens Power; K1: Keratometric Power in the Flattest Meridian; K2: Keratometric Power in the Steepest Meridian; ACD: Anterior Chamber Depth; OSD: Ocular Surface Disease.
Introduction
During the COVID-19 pandemic, the concern for reducing disease transmission led to changes in human habits, such as the widespread use of face masks [1-3]. While essential for preventing coronavirus transmission, masks also caused ocular surface changes. The tear film is a crucial barrier against pathogen invasion, but it can be compromised by mask use. There have been several reports describing ocular irritation and dryness derived from its use, which have described this condition as maskassociated dry eye (MADE) [4-7]. The exhaled air escaping upward from the edge of the mask stimulates tear film evaporation, which may lead to discomfort, inflammation and dry eye symptoms [5,8].
With the recent advances in modern optical instrument technologies and IOL design, cataract surgery is no longer a matter of replacing the natural lens with an IOL. Nowadays, patients have higher expectations for accurate refractive outcomes and excellent quality of vision after surgery. However, according to some studies, refractive errors of ± 0.5 diopters (D) or greater occur in 20% to 40% of cataract surgery cases [9-12]. Ocular biometry for IOL power calculations has become increasingly important in clinical practice to achieve preoperatively intended outcomes. Keratometry and axial length (AXL) are the main parameters for IOL power calculations.
IOL Master 700 is a non-contact biometric device based on scanning source optical coherence interferometry. Although this instrument is considered the gold standard in calculating IOL for cataract surgery [13-15], some studies have shown that an unstable tear film can produce optical aberrations, reducing the accuracy and repeatability of biometric measurements [16,17]. Inaccurate keratometric measurements lead to residual refractive errors, since the cornea is the largest refractive component of the eye, contributing 70% of its refractive power. Therefore, tear film stability is a fundamental factor in obtaining biometric measurements for calculating IOL power.
The repeatability of keratometric and anterior segment measurements has been studied and demonstrated with different devices in normal eyes and in patients with dry eye disease (DED) [16,18-20]. In individuals suffering from DED, the cornea has an irregular surface, measurements may not be as valid or reproducible, and there are no repeatability studies in association with mask wearing. During the biometric calculation in the COVID-19 period, patients did not remove their masks, and we do not know the impact this may have on IOL power calculation and the resulting refractive surprise.
Materials and Methods
Participant Selection and Recruitment
This cross-sectional study was conducted at Fundacion de Oftalmologia Medica de la Comunidad Valenciana (FOM, Valencia, Spain). Cataract patients that met inclusion/exclusion criteria were recruited over a three-month period during the COVID-19 pandemic. Written informed consent was obtained from all the patients, and they had the approval of the Clinical Research Ethics Committe at the previously mentioned hospital. The study was performed in accordance with the tenets of the Declaration of Helsinki. Inclusion criteria were individuals over 18 years old scheduled for cataract surgery for whom IOL Master 700 biometry could be performed.
Exclusion criteria were patients under 18 years old, contact lens use in the previous 7 days, prior eye surgeries, chronic dry eye treatment in the previous 14 days, ocular inflammation, allergic conjunctivitis, active eye infection, lens opacity preventing measurements with the IOL Master 700 biometer, chronic glaucoma treatment and extreme refractive errors (High myopia with AXL > 26 mm and/or > 6 D, hyperopia > 5 D, astigmatism > 3 D). The medical records of the patients were thoroughly revised to identify the selection criteria.
Study Development
The patient´s age, sex, ophthalmological history and topical treatment were noted. Every patient underwent an ophthalmic examination including best-corrected visual acuity and slit-lamp biomicroscopy to confirm the inclusion and exclusion criteria. Biometry for IOL calculation was performed on all patients in the study using the same IOL Master 700 optical biometers (Carl Zeiss Meditec AG, Jena, Germany). Each patient’s measurements were taken at two different times: at first stage with the patient wearing a surgical face mask and in a second time without the mask. Two consecutive biometric measurements were taken on each eye included in the study with the mask properly positioned, and once patients confirmed to have been wearing the mask for at least 30 minutes before the examination.
After these measurements, patients went to an internal hall where they remained for 10 minutes without the face mask. Chairs were placed in this space for the patients, maintaining social distancing and ensuring that all safety measures were followed. Once the 10-minute rest period without the surgical face mask had elapsed, the patient was called back to consultation room to repeat the two consecutive biometric measurements without the face mask. Testing was conducted under the same temperature (20°C) and humidity (40–50%) conditions, which were verified with a thermometer and hygrometer.
Sample Size Calculation
The sample size calculation was performed using GRANMO (7.2 software, Barcelona, Spain). Considering paired means (repeated within one group) and accepting an alpha risk of 0.05 and a beta risk of 0.2 in a two-tailed test, 23 subjects are required to detect a difference equal to or greater than 0.3 units. A standard deviation (SD) of 0.5 between measurements is assumed. A lossto- follow-up rate of 5%, a 95% confidence level, and a precision of 5% were estimated.
Statistical Analysis
Statistical analysis was performed using SPSS v23.0 (Armonk, NY, USA). First, the repeatability of measurements with and without the face mask was studied using Dahlberg’s error, the CV, and the ICC, as well as a descriptive of the mean difference between the two measurements. Second, the concordance between the two methods (with and without the face mask) was evaluated. The statistical indices were calculated. Given the large sample size, a parametric approach was used.
A repeated measures t-test was applied to assess the existence of possible bias between the measurements. To complete the concordance analysis, the results obtained with each pair of methods were compared using regression models. This allowed visualization of the presence and linearity of bias, as well as the variability of the measurements. 95% confidence intervals were estimated for the coefficients, and their compatibility with the concordance hypothesis was examined. The significance level used in the analyses was 5% (alpha=0.05).
Results
A total of 58 eyes of 29 subjects were included in the study with a mean age of 70.2 ± 10.5 years and 16 individuals being female (55%). Each eye underwent 4 measurements (2 with surgical face mask and 2 with no mask use). Overall, measurements taken with and without the face mask showed a high degree of concordance in our study, with no significant differences observed between them.
Analysis of Measurement Repeatability with Face Mask

K1 = keratometric power in the flattest meridian; K2 = keratometric power in the steepest meridian; AXL = axial lenght; ACD = anterior chamber depth; LT = lens thickness; WTW= white-to-white; CCT = central corneal thickness, IOLP = intraocular lens power; CV= coefficient of variation; ICC = intraclass correlation coefficient; SD = standard deviation. *p<0,05; **p<0,01; ***p<0,001.
Table 1 presents basic statistics for the difference between the two examiner measurements in the sample of 58 eyes, as well as those relating to the method error. Most of the means fall within the range of -0.05 to 0.05, so they are generally very close to 0. The difference for Central Corneal thickness (CCT) is the only one outside the range (0.328) and has the largest SD. This should be analyzed in perspective, as its scale is significantly larger than that of the other variables. All 95% confidence intervals include 0, which suggests that there are generally no differences between measurements.
When performing the student’s t-test for repeated measures, significance was reached by a narrow margin (p=0.049) for AXL. This suggests minimal bias, but despite this, the mean difference (-0.006) does not appear clinically relevant. The remaining statistics indicate that there are no overall problems for this variable. The table also shows Dahlberg’s d statistic, which typically takes values close to 0, except for CCT (4.41), where the scale appears to have a significant influence. This is an estimate of the absolute or technical measurement error. The values of Dahlberg’s d translate, in relative terms (when compared to the magnitude of what is being measured), into values for the method error (CV) that do not exceed 1%, indicating very high reproducibility.
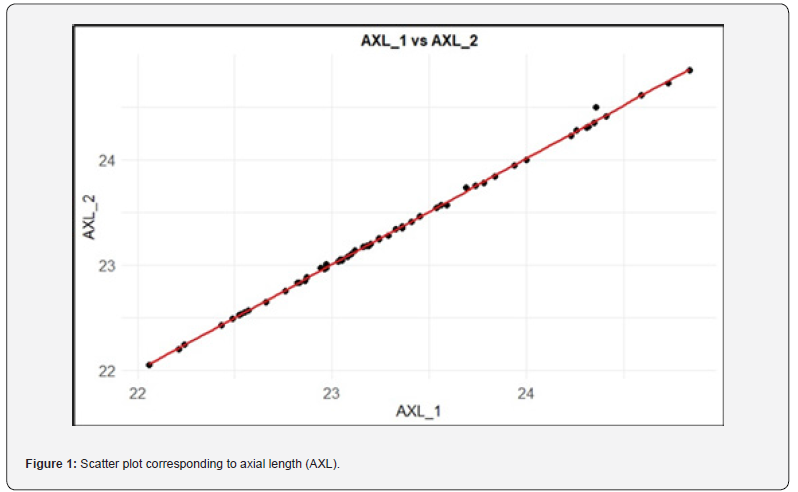
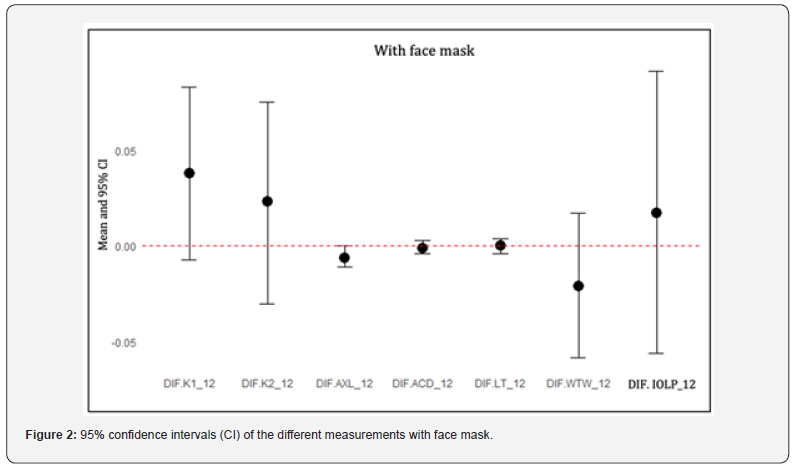
Finally, the table provides the ICC, another indicator of the degree of concordance between the two assessments, which is highly sensitive to random (non-systematic) error. Values close to 1 were obtained, so reproducibility appears to be very good. The scatter plot for AXL, for which this minimal bias was detected, is shown below (Figure 1). A discordant data point is visible. Its simple exclusion ensures a non-significant mean difference. The next graph (Figure 2) shows that all 95% confidence intervals include 0. This indicates that there are no apparent differences between measurements. Due to the difference in magnitude between variables, CCT is not included, although its interval includes 0 (-1.324: 1.979).
Analysis Of Measurement Repeatability Without the Face Mask
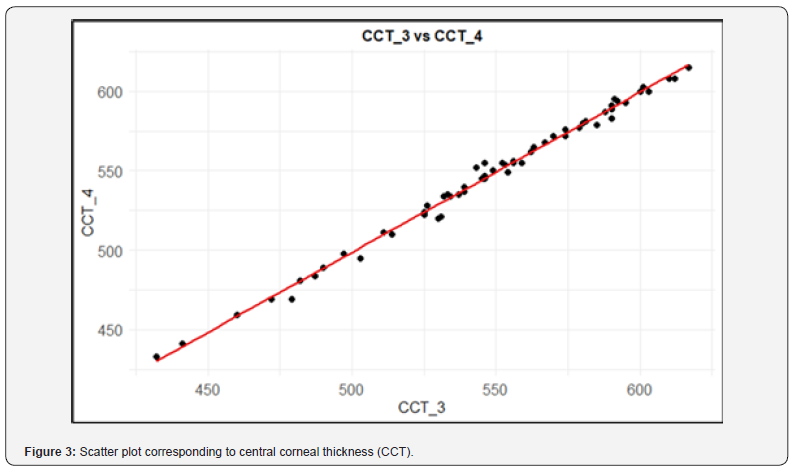
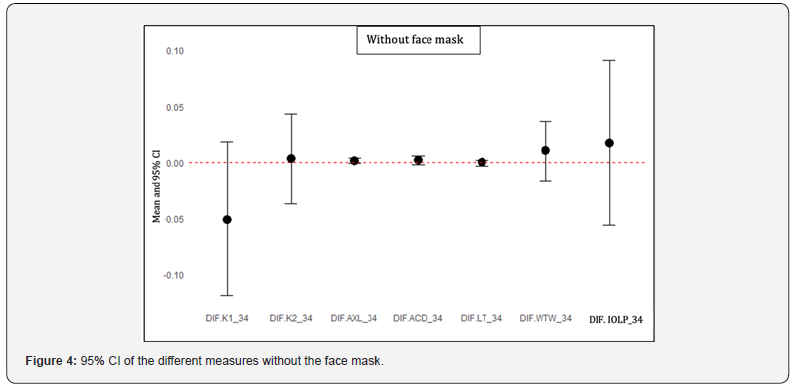
Table 2 presents basic statistics for the difference between the two measurements without the face mask in the sample of 58 eyes, as well as those relating to the method error. The t-statistics revealed a slight statistical trend in CCT without the face mask (p = 0.064), but it does not appear to have clinical relevance. The Dahlberg´s error reaches 2.66 in CCT. When it is considered in relation to the magnitude of what is being measured, relative errors (CV) below 1% are obtained in all cases, which would be interpreted as very high reproducibility. The ICC values are close to 1 in all cases, which is again interpreted as very high reproducibility. No systematic or random error pattern was detected in any case. Again, CCT was not included in the graph due to differences in measurement scale, although it includes 0 in its 95% confidence interval (-0.054, 1.882) (Figures 3 and 4).

K1 = keratometric power in the flattest meridian; K2 = keratometric power in the steepest meridian; AXL = axial lenght; ACD = anterior chamber depth; LT = lens thickness; WTW= white-to-white; CCT = central corneal thickness, IOLP = intraocular lens power; CV = coefficient of variation; ICC = intraclass correlation coefficient; SD = standard deviation. *p<0,05; **p<0,01; ***p<0,001.
Concordance Analysis Between with and without the Face Mask
Table 3 presents basic statistics for the difference between with and without the face mask in the sample of 58 eyes, as well as those relating to the method error. The mean differences are very close to 0. Even in CCT, which is of high magnitude, this difference is less than 0.5. This first detail indicates that there appears to be no difference between the measurements with and without the face mask. In fact, there are no significant results (by p-value of the t-test), only a slight trend in white-to-white distance (WTW) (p=0.095), although the other statistics show clear homogeneity between the measurements (a CV of 0.644% is very low, accompanied by an ICC of 0.952, very close to 1).
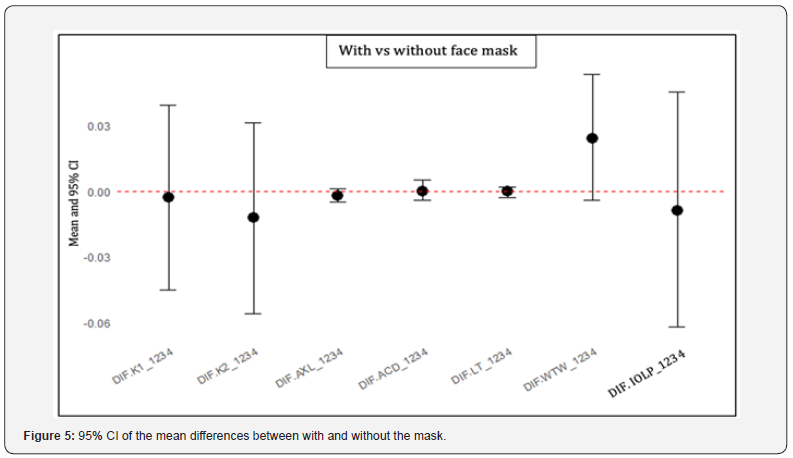
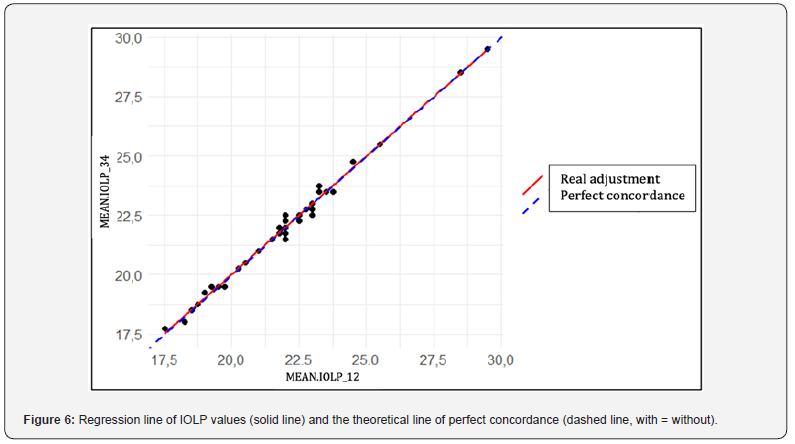
The following graph (Figure 5) represents each mean difference with its corresponding 95% confidence interval. It is clear how all parameters are unbiased and intersect the x-axis (line y=0). Table 3 shows that the d-values are very small and generally close to 0 (except for CCT, again due to its high magnitude), which suggests a small absolute error between the methods. The CV is less than 1% for all parameters and the ICCs are very close to 1, which allows us to conclude that there is a small random error. Based on the overall interpretation, all indicators point to a high level of concordance between biometric measurements with and without the face mask. Finally, the regression analysis for the comparative values between with and without face masks in the situation of intraocular lens power calculation (IOLP) (Figure 6, table 4).

K1 = keratometric power in the flattest meridian; K2 = keratometric power in the steepest meridian; AXL = axial lenght; ACD = anterior chamber depth; LT = lens thickness; WTW = white-to-white; CCT = central corneal thickness, IOLP = intraocular lens power; CV = coefficient of variation; ICC = intraclass correlation coefficient; SD = standard deviation. *p<0,05; **p<0,01; ***p<0,001.

SD = standard deviation, CI = Confidence interval. *p<0,05; **p<0,01; ***p<0,001
Discussion
This study aimed to assess whether the use of face masks produces an alteration in the IOL calculation in patients undergoing cataract surgery. Face masks were globally used during the COVID-19 pandemic, when both patients and healthcare professionals were required to wear them properly fitted [21] and there is certain evidence that during this period they contributed to increasing the prevalence of ocular discomfort symptoms [5]. Since the tear film is unstable in some of the patients wearing face masks, light reflection using the IOL Master 700 biometer may vary and lead to deterioration in measurement accuracy with their potential implications for the final refractive outcome after surgery.
It is difficult to evaluate the results in our study with those of literature because comparable studies are lacking. One of the most similar studies to ours in terms of association between ocular surface changes and IOL calculation found in the literature is that of Epitropoulos et al [16], although without correlation with the use of face masks. The purpose of their study was to evaluate the effects of tear osmolarity on the repeatability of keratometric measurements in patients undergoing cataract surgery. They observed greater variability in the mean keratometry measurement in the hyperosmolar group (i.e. DED) compared to the control group, with a difference greater than 1.0 D in corneal astigmatism. Furthermore, they described a higher percentage of eyes in the hyperosmolar group with a difference in the calculated IOLP greater than 0.5 D. All these alterations were statistically significant.
However, when the subjects were grouped by perceived dry eye symptoms, no significant differences were found. On the other hand, Hiraoka et al [18] found that the measurement repeatability of corneal curvature radius decreased in patients with DED compared to normal eyes. Moreover, shortened breakup time were correlated with a worsening in the measurement repeatability of corneal curvature radius and AXL. In this study measurements were assessed twice on the same day using IOL Master 500 and not the latest version of this device as in the present study. Burgos-Blasco et al [22] studied whether the use of a face mask influenced the measurement of keratometric parameters, in this case without looking for an association with the final IOLP calculation in patients undergoing cataract surgery. Of 35 healthy eyes analyzed with the Pentacam Scheimpflug tomograph, no differences were found in mean keratometric power in the flattest meridian (K1), the steepest meridian (K2), medium and maximal keratometry with and without the face mask. The ICC was excellent for the four parameters analyzed, although it was low when measurements with the face mask were considered. Although alterations in the tear film with mask use have been described in the literature, no significant differences were found in the topographic variables, similar to our results in this aspect. Other biometric variables apart from keratometry could be altered by using face masks, although this has not been studied in the literature. In our analysis, we correlated mask use with parameters such as anterior chamber depth (ACD), AXL, and CCT, finding no differences and a high degree of concordance between measurements taken with and without the face mask.
In the study conducted by Meyer et al [23], 97 patients with ocular surface disease (OSD) and 33 healthy individuals were studied. Corneal morphology was assessed using Scheimpflug photography, and corneal keratometry and density were analyzed in five anatomical corneal layers. Corneal density was significantly reduced in the epithelium, Bowman’s membrane, and Descemet’s membrane in patients with OSD compared to controls. Similar results regarding corneal density were obtained in the study by Wegener et al [24]. They also noted that corneal density was higher and very close to that of controls if the patient was treated with hydroxypropyl methylcellulose, which is found in tears and lubricating gels. These results show that OSD caused by face masks could affect different biometric variables, not just keratometry.
Regarding the type of face mask used, all patients in our study used surgical masks during the corresponding measurements. Therefore, a comparison with filtering facepiece or N95 respirators cannot be made in terms of the final calculation of IOLP or the alteration of keratometric parameters. However, the study conducted by Shalaby et al [25] compared the use of surgical masks and N95 respirators. In general, mask use for 60 minutes significantly worsened all tear film parameters in both groups, with greater deterioration after the use of surgical masks compared to N95 respirators. This latter finding could be due to the tighter fit provided by the N95 mask, which almost completely prevents airflow from the mask to the ocular region.
Although our research correlates face mask use with biometric measurements and compares patients who wear face masks with those who do not, it does not objectively quantify ocular surface involvement in each patient, despite many of them exhibited associated OSD symptoms during the examination. Other studies analyzed [7, 26-28] explain the results of questionnaires and tests related to associated OSD in the study group. Finally, the American Society of Cataract and Refractive Surgery Clinical Committee reported a new consensus-based practical diagnostic OSD algorithm to aid surgeons in efficiently diagnosing and treating visually significant OSD before any refractive surgery is performed [29].
The report emphasized that the importance of addressing OSD cannot be underestimated because it potentially results in different adverse surgical outcomes. So, although no objective differences were found in this research in the calculation of IOLP between mask and no mask wearing, it is necessary to consider preoperative treatment of the ocular surface in patients with symptoms of DED, not only with the aim of increasing surgical refractive accuracy, but also to reduce OSD symptoms and infections in the postoperative period, which are often exacerbated by the procedure itself.
Conclusion
Due to the recommendation and mandatory use of face masks during the COVID-19 pandemic, an increase in ocular symptoms was observed. Understanding the pathophysiological mechanisms associated with the ocular surface alteration caused by masks helps us to focus on better treatment and design prevention strategies, especially when scheduling surgery where IOL calculation becomes necessary. The increase in dry eye symptoms during the COVID-19 pandemic was multifactorial. Furthermore, face masks may have different effects on different individuals.
Multiple variables can influence the magnitude of the effects of face masks on the ocular surface, such as the severity of dry eye, air humidity, the presence of concomitant pathology, the number of hours wearing a mask, and the type of face mask. Despite the gradual reduction in mask use following the end of the pandemic, they are still widely used in healthcare facilities and public spaces. Their long-term effects on the eyes remain uncertain, as does their potential impact on visual, physical, and psychological wellbeing. According to the results of our study, there is a high degree of concordance between biometric measurements taken with and without the face mask, so no differences were observed in the estimated IOLP.
Even so, we believe it is advisable to analyze each case individually and to establish appropriate ocular surface treatment for those patients with symptoms associated with mask use. Finally, although many symptoms associated with its use have been grouped under the term MADE, the mask is a protective factor that has proven to be effective in the transmission of COVID-19 and other respiratory viruses. In fact, it is a common recommendation in ophthalmological consultations due to the proximity to the patient´s facial region during the clinical examination.
Financial Support
Project/Equipment funded by Consellería de Sanitat Universal i Salut Pública (Generalitat Valenciana, Spain) and the EU Operational Program of the European Regional Development Fund (ERDF) for the Valencian Community 2014-2020, within the framework of the REACT-EU programme, as the Union´s response to the COVID-19 pandemic.
References
- Christiane Matuschek, Friedrich Moll, Heiner Fangerau, Johannes C Fischer, Kurt Zänker, et al. (2020) Face masks: benefits and risks during the COVID-19 crisis. Eur J Med Res 25(1): 32.
- Wang Q, Yu C (2020) The role of masks and respirator protection against SARS-CoV-2. Infect Control Hosp Epidemiol 41(6): 746-747.
- Leung CC, Lam TH, Cheng KK (2020) Mass masking in the COVID-19 epidemic: people need guidance. Lancet 395 (10228): 945.
- White D (2020) Blog: Made: A new coronavirus-associated eye disease.
- Moshirfar M, West WB, Marx DP (2020) Face Mask-Associated Ocular Irritation and Dryness. Ophthalmol Ther 9(3): 397-400.
- Boccardo L (2022) Self-reported symptoms of mask-associated dry eye: A survey study of 3,605 people. Cont Lens Anterior Eye 45(2).
- Esen Baris M, Guven Yilmaz S, Palamar M (2022) Impact of prolonged face mask wearing on tear break-up time and dry eye symptoms in health care professionals. Int Ophthalmol 42(7): 2141-2144.
- Antonio Ivan Lazzarino, Andrew Steptoe, Mark Hamer, Susan Michie (2020) Covid-19: Important potential side effects of wearing face masks that we should bear in mind. BMJ 369: m2003.
- Sabite Emine Gökce, Ildamaris Montes De Oca, David L Cooke, Li Wang, Douglas D Koch, et al. (2018) Accuracy of 8 intraocular lens calculation formulas in relation to anterior chamber depth in patients with normal axial lengths. J Cataract Refract Surg 44(3): 362-368.
- Melles RB, Holladay JT, Chang WJ (2018) Accuracy of Intraocular Lens Calculation Formulas. Ophthalmology 125(2): 169-178.
- Jack X Kane, Anton Van Heerden, Alp Atik, Constantinos Petsoglou (2016) Intraocular lens power formula accuracy: Comparison of 7 formulas. J Cataract Refract Surg 42(10): 1490-1500.
- Olsen T (2007) Calculation of intraocular lens power: a review. Acta Ophthalmol Scand 85(5): 472-485.
- J Santodomingo-Rubido, EAH Mallen, B Gilmartin, JS Wolffsohn (2002) A new non-contact optical device for ocular biometry. Br J Ophthalmol 86(4): 458-462.
- Basu S (2006) Comparison of IOL power calculations by the IOLMaster vs theoretical calculations. Eye 20(1): 90-97.
- Freeman G, Pesudovs K (2005) The impact of cataract severity on measurement acquisition with the IOLMaster. Acta Ophthalmol Scand 83(4): 439-442.
- Alice T Epitropoulos, Cynthia Matossian, Gregg J Berdy, Ranjan P Malhotra, Richard Potvin (2015) Effect of tear osmolarity on repeatability of keratometry for cataract surgery planning. J Cataract Refract Surg 41(8): 1672-1677.
- Montés-Micó R (2007) Role of the tear film in the optical quality of the human eye. J Cataract Refract Surg 33(9): 1631-1635.
- Takahiro Hiraoka, Hiroki Asano, Tomohiro Ogami, Shinichiro Nakano, Yoshifumi Okamoto, et al. (2022) Influence of Dry Eye Disease on the Measurement Repeatability of Corneal Curvature Radius and Axial Length in Patients with Cataract. J Clin Med 11(3): 710.
- Christian Nilsen, Morten Gundersen, Per Graae Jensen, Kjell Gunnar Gundersen, Richard Potvin, et al. (2024) The Significance of Dry Eye Signs on Preoperative Keratometry Measurements in Patients Scheduled for Cataract Surgery. Clin Ophthalmol 18: 151-161.
- Xuemei Zhang, Kunhong Xiao, Taichen Lai, Rongyong Zhang, Mengxue Huang, et al. (2025) Reproducibility and accuracy of corneal curvature measurements in patients with and without dry eye: a device-based study. Front Med (Lausanne) 12: 1565740.
- Ji-Peng Olivia Li, Jessica Shantha, Tien Y Wong, Edmund Y Wong, Jod Mehta, et al. (2020) Preparedness among Ophthalmologists: During and Beyond the COVID-19 Pandemic. Ophthalmology 127(5): 569-572.
- Barbara Burgos-Blasco, Carlos Oribio-Quinto, Beatriz Vidal-Villegas, Mayte Ariño-Gutierrez, Jose M Benítez-Del-Castillo, et al. (2023) Effect of face mask on topographic corneal parameters in healthy individuals. Eur J Ophthalmol 33(1): 203-206.
- Meyer LM, Kronschläger M, Wegener AR (2014) Schleimpflug photography detects alterations in corneal density and thickness in patients with dry eye disease. Ophthalmologe 111(10): 914-919.
- Wegener AR, Meyer LM, Schönfeld CL (2015) Effect of Viscous Agents on Corneal Density in Dry Eye Disease. J Ocul Pharmacol Ther 31(8): 504–508.
- Shalaby HS, Eldesouky MEES (2023) Effect of facemasks on the tear film during the COVID-19 pandemic. Eur J Ophthalmol 33(1): 145-151.
- Giuseppe Giannaccare, Marco Pellegrini, Massimiliano Borselli, Carlotta Senni, Angela Bruno, et al. (2022) Diurnal changes of noninvasive parameters of ocular surface in healthy subjects before and after continuous face mask wearing during the COVID-19 pandemic. Sci Rep 12(1).
- Mana A Alanazi, Gamal A El-Hiti, Rashid Al-Tamimi, Abdullah M Bawazir, Essam S Almutleb, et al. (2022) Assessment of the Effect of Wearing a Surgical Face Mask on Tear Film in Normal Eye Subjects. J Ophthalmol 2022: 2484997.
- Shirin Hamed Azzam, Amir Nama, Hanan Badarni, Helena Asael, Wadie Abu Dahoud, Michael Mimouni, et al. (2022) Assessment of dry eye disease in N95 versus surgical face mask wearers during COVID-19. Indian J Ophthalmol 70(3): 995-999.
- Starr CE, Gupta PK, Farid M, et al. (2019) An algorithm for the preoperative diagnosis and treatment of ocular surface disorders. J Cataract Refract Surg 45(5): 669-684.






























