Epidemiological, Microbiological Profiles and Treatment Outcome of Patients Suffering of Corneal Ulcers in Magrabi Ico Cameroon Eye Institute
Jibia G*, Yande J, Afetane TG, Tchouyo M, Helles G, Tchuindem S, Signe JA, Emade N and Nkumbe HE
Magrabi ICO Cameroon Eye Institute, Cameroon
Submission: May 06, 2024; Published: June 05, 2024
*Corresponding author: Jibia Gaëlle, Ophthalmologist, Magrabi ICO Cameroon Eye Institute, Cameroon
How to cite this article: Jibia G*, Yande J, Afetane TG, Tchouyo M, Helles G, Tchuindem S, Signe JA, Emade N and Nkumbe HE. Epidemiological, Microbiological Profiles and Treatment Outcome of Patients Suffering of Corneal Ulcers in Magrabi Ico Cameroon Eye Institute. JOJ Ophthalmol. 2024; 11(1): 555804. DOI: 10.19080/JOJO.2024.11.555804
Abstract
Objective: To present epidemiological and microbiological profiles, antibiotic and antifungal susceptibility patterns and treatment outcome in patients with corneal ulcers in Cameroon.
Design of the study: this is a retrospective study of 5 years ((1st January 2017- 30th November 2022) based on files of patients diagnosed with a corneal ulcer who had undergone a cornea scrapping.
Setting: Magrabi ICO Cameroon Eye Institute (MICEI).
Materials and Methods: The historical aspects including the systemic and local predisposing factors, results of culture for which material was taken by scraping of the ulcer or conjunctiva swabs, and its sensitivity pattern, type of management, and its outcome, were noted and the results were interpreted.
Results: 151 patients (151 eyes) were included in the study. 51% of patients were males with a mean age of 49.95 ± 17.52 years. Housewives 57 (37.7%), merchants 21 (13.9%) and farmers 19 (12.6%) were the main professions represented. 93.37% (141/151) of cases showed positive culture of which 76.8% (116/151)were bacteria (Staphylococcus 73% (84/116) and streptococcus 26.1% (30/116)) and 34.4% (52/151) were fungal isolates (mainly Aspergillus 45/52 (86.5%)). 27(17.9%) presented a co-infection. Bacterial strains were susceptible to quinolones as ciprofloxacin 105/113 (92.9%) and aminosides as gentamycin 108/115 (93.9%). Fungal species were sensitive to triazoles as Econazole 49/52 (94.2%) (p=0.00). 73 eyes/ 131 (70.9%) received an initial dual therapy with econazole and ciprofloxacin (p=0, 00). 71.5% of ulcers healed with a scar after treatment while 8.6% encountered an evisceration. As local predisposing factors, 57 (45.2%) were post traumatic (p=0.067) and 32 (25.4%) cases used traditional medicine (p=0,00).
Conclusion: corneal ulcers are frequent amongst middle aged male Cameroonians doing manual work. The main germs in causes are Staphylococcus spp, streptococcus pneumonia and Aspergillus responding very well to quinolones and econazole.
Keywords: Corneal ulcer; Epidemiology; Antibacterial sensitivity; Antifungal sensitivity; Cameroon; MICEI
Introduction
Keratitis is an important cause of ocular morbidity worldwide, the outcome of which depends on early diagnosis, prompt and effective treatment and various host and agent factors [1]. Their incidence varies from 11/ 100000 persons in USA to 799 / 100000 persons in Nepal [2]. In Africa and specifically in Cameroon, cornea ulcers represent a real challenge for clinicians whose limited diagnostic and therapeutic means are crowned by disappointing results with frequent functional and/or organic loss. Some of the common causes of infectious keratitis include bacterial, fungal, viral, and protozoan, the diagnosis of which is made on clinical examination aided by microbiological demonstration in smears or cultures from corneal tissues. Empirical treatment with broad spectrum anti-microbial medication based on the microbiological profile of each particular region is a frequent practice, supported by the finding that 96% of isolated microorganisms are sensitive to empirical therapy [3]. This practice provides favorable results in the majority of cases, but when therapy fails, occasionally, due to increased resistance of microorganisms to empirical therapy, identification becomes mandatory. The aim of this study was to present the epidemiological and microbiological profiles, antibiotic and antifungal susceptibility patterns and treatment outcome in patients with corneal ulcers in Magrabi ICO Cameroon Eye Institute (MICEI) in order to improve their management in our setting.
Material and Methods
This is a cross-sectional, retrospective and monocentric study of 5 years duration (1st January 2017- 30th November 2022) based on the files of 151 patients with a diagnosis of corneal ulcers who received a sample with microbiological analysis in MICEI. Viral keratitis, Mooren’s ulcers, posttraumatic perforations and other degenerative conditions of cornea were not included in the study. The samples collected by the different ophthalmologists by corneal scrapings and/or conjunctiva swabs in all age groups were inoculated in different culture media (Blood agar, Chocolate agar and Sabouraud dextrose agar) and subjected for microscopic examination as KOH wet mount. The antibiotic discs used were ofloxacin (5μg), rifampicin (5μg), levofloxacin (5μg), ciprofloxacin (5μg), nalixidic acid (30μg), gentamycin (10μg), cefixim (5μg), cloxacin (5μg), norfloxacin (10μg), tobramycin (10μg) vancomycin (30μg), azithromycin (15μg) and metronidazole (50μg). The antifungal dics used were fluconazole (10μg), nystatin (100μg), amphotericin B (100μg), itraconazole (50μg), miconazole (10μg), econazole (10μg). .Bacterial growth in culture media was considered significant if it was observed in two solid phase media or confluent growth in one media. Fungal isolation in SDA (sabaurauds dextrose agar) or observation of hyphal filaments in KOH smear was considered sufficient for diagnosis.
Data Management and Analysis
The data collected (age, sex, place of residence, profession, date of consultation, ophthalmological and general history, microbiological results, antimicrobial sensitivity, treatment received, treatment results) were analyzed by Epi Info version 7.1.2. Frequency and percentages were calculated and twotailed Pearson’s Chi-square test was used to test the significance of attributes between study variables. The p-value < 0.05 was considered statistically significant.
Results
Epidemiologic Profile
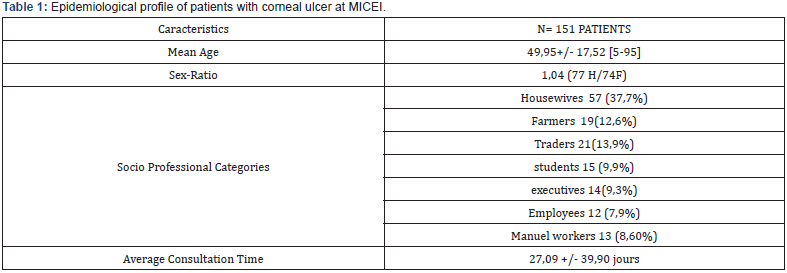
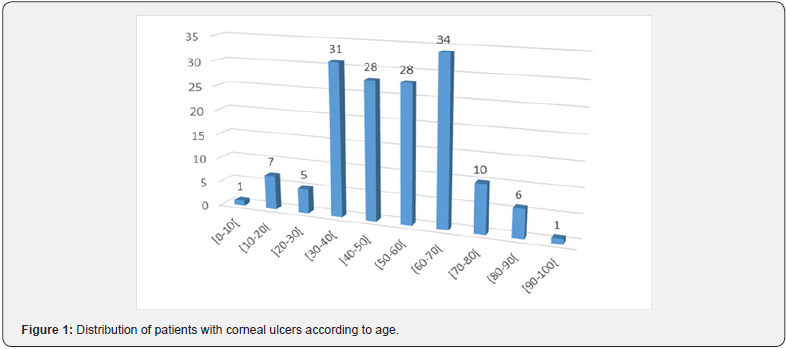
151 patients were included in the study giving an incidence rate of 8.32/10000 (151/181399 consultations ) .The average age was 49.95 +/- 17 years, affecting more frequently the age groups of 30-40 and 60-70 years (Table 1, Figure 1); the sex ratio was slightly in favor of men. Housewives, farmers and traders were the most affected social categories. 81(53.6%) of patients were coming from an urban area (Yaoundé and nearby suburbs).
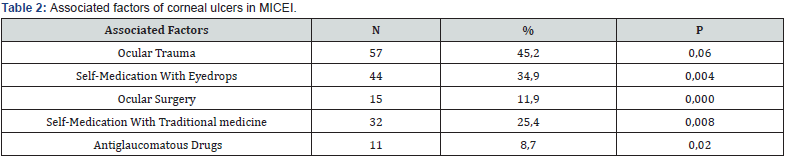
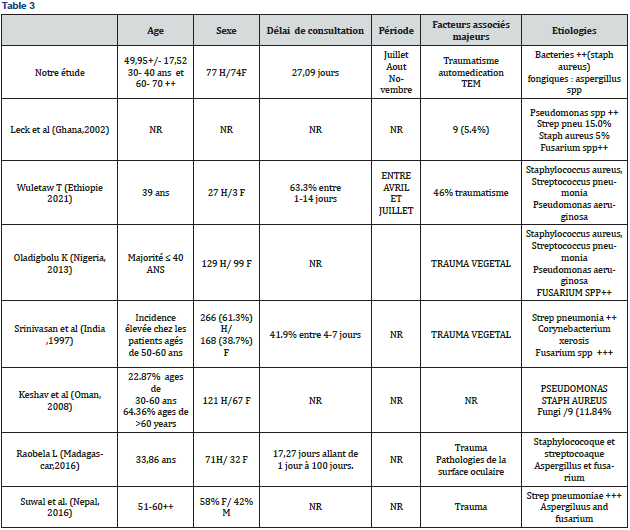
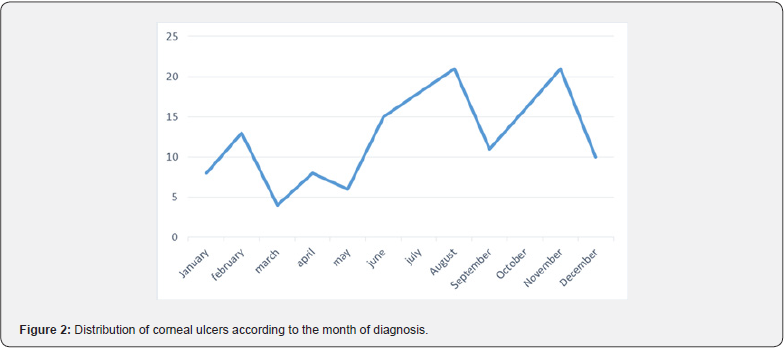
The average consultation time was 27 +/- 39 days and diagnostic peaks were noted during the months of July, August and October (Figure 2). Main associated factors were trauma, selfmedication, and history of eye surgery or long-term antiglaucoma treatment as seen in Table 2, 3.
Microbiologic Profile
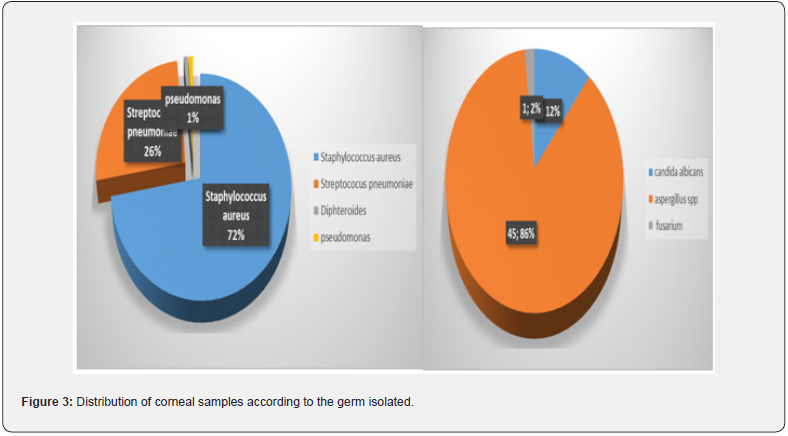
On the 151 samples collected, 141 (93.37%) were positive to the culture and 10(6,6%) sterile that is 116 (76.8%) bacteria and 52 (34.4%) fungal; 28 eyes (18.6%) had a co-infection. (27 bacterial-fungal co-infection, 1 polybacterial eye). Staphylococcus aureus represented 72% of the isolated bacterias and Aspergillus was the most frequent fungal germ seen as shown in Figure 3. The bacterial strains were more sensitive to antibiotics of the quinolone, aminoglycoside and rifamycin family and a little less to cephalosporins and beta lactamines. Mycotic strains were more sensitive to triazoles (econazole and miconazole) and resistant to amphotericin B , nystatin and ketoconazole as seen in figure 3.
Treatment and Evolution
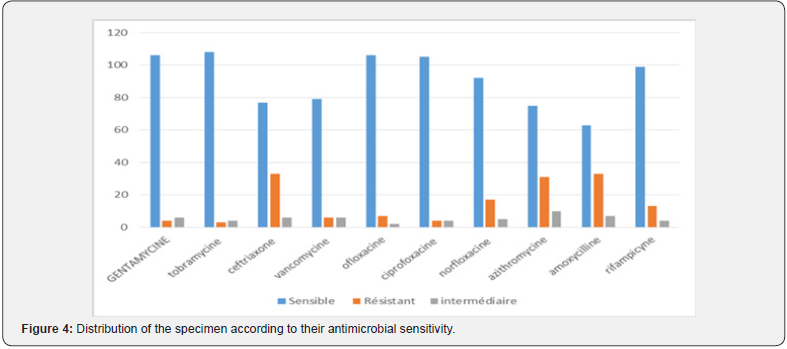
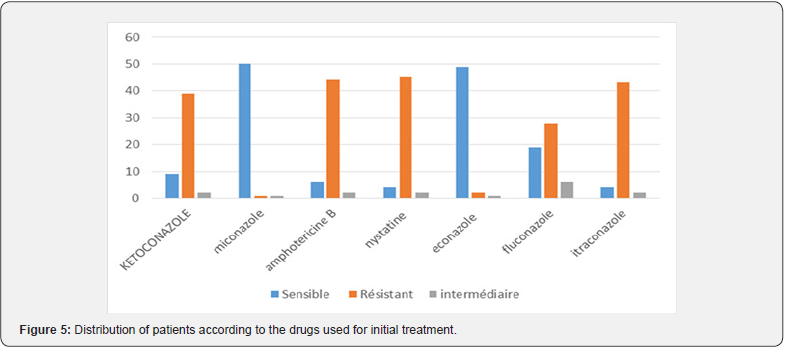
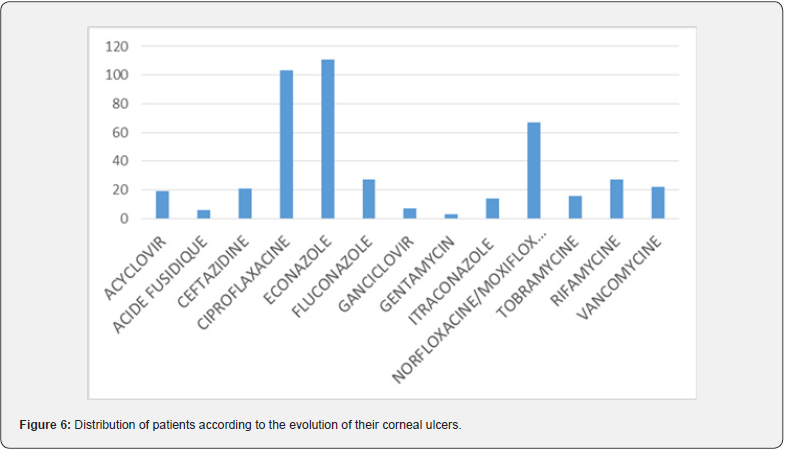
Ciprofloxacine and econazole were the principal drugs used for the treatment of patients as seen in Figure 4. An initial dual therapy based on this two molecules has been done in 71% of cases. Fortified eyedrops were not commonly used. Evolution was favorable in more than 70% of case with a formation of a scar and 9% of the eyes were eviscerated (Figure 5).
Discussion
Incidence
In our study, the incidence of corneal ulcers was 8.32/10000 patients seen. This number can be underestimated given the fact that we only considered the patients who had undergone corneal scrapping. This is similar to the reports of other low-income countries like Madagascar ( 0,76 per 1000 consultations), South India (113 per 100,000 population-year) and Nepal (799 per 100,000 population-year) but still very high compared to the reports in USA ( 2.5-27.6 per 100,000 population-year) and UK (34.7 per 100,000 population-year in Nottingham UK, between 2007 and 2019) or Australia ( 6.6 per 100,000 population-year during the period of 2005-2015) [4]. The epidemiological profile of corneal ulcers varies given the geographical region. The higher incidence observed in low-income countries was primarily attributable to the poorer environmental and personal hygiene, lower level of education, agricultural industry, increased risk to work-related corneal trauma and poorer access to sanitation and healthcare facility [4]. However, these results show the persistent burden of infectious keratitis worldwide , highlighting the importance of sensitization for prevention when possible.
Age and Sex
The average age was 49.95 +/- 17 years even though it touches all ages meaning that corneal ulcers mainly affect the working population of our country as it has been remarked by Ting et al in his study [4]. Also, a majority (34 patients) of them were over 60 years of age. The Madurai [5] and Keshav [6] studies conclude the same. For the latest [6], it can be explained by the plethora of predisposing factors like CDK, dryness, cataract surgery, glaucomatous patients on medications, and lid deformities due to trachomatous scarring which probably predisposed this age group to corneal ulceration more than the other age groups.
We noticed a big lag of time before consultation, longer than the one reported by Raobela L [7] in Madagascar (15 days) or Srinivasan L [5] in South India (1 week) ; this can be explained by the fact that many patients go first for self-medication either with eye drops or traditional treatment, and /or other nearby centers before coming to MICEI considered like a referral center. Also, there is a lack of good transportation means from other towns to MICEI which reduces accessibility to proper healthcare. Ocular trauma was the main associated factor in our series (45.2%) followed by self-medication as seen in several other studies [3-7]. As explained by Raobela L [7], corneal trauma acts by modifying the epithelial barrier, which promotes the adhesion of saprophytic or exogenous flora germs to the injured epithelial surface. Corneal trauma is a risk factor predisposing to corneal abscesses in young active subjects, with a frequency of 15 to 70%. Self-medication with eye drops or traditional medications is a real challenge, very often complicating the patient’s very mild initial picture. This attitude tends to be cultural in southern Africa as reported by some studies in Nigeria or Malawi [4] where the population believes that the application of breast milk or some plant essence will heal the abcess of which this actually worsen their keratitis [4]. In addition, patients who had prior use of traditional eye medicine tended to present later to the eye care professionals, resulting in delayed treatment and poorer visual outcome. The high peak of corneal ulcers during the months of July, August and October can be explained by the fact that this period corresponds to the rainy seasons with a huge load of farm work leading to ocular trauma [8].
Microbiologic Profile
Microorganisms were isolated in 141 (93.37%) of samples which is comparable with the 80% figure in Nepal by Upadhyay [9] or 81.7% in Bangladesh by Dunlop [10]. The proximity of the laboratory and a good method of scrapping can explain the up said results. 76.8% (116) of all corneal ulcers with positive cultures were bacterial in origin. Bacterial keratitis represents the most common type of IK in most regions, including the UK (91-93%), North America (86-92%) , South America (79-88%) , Middle East (91.8%) , and Australasia (93-100%) [4]. The specific germs isolated that is S. aureus (72%), Streptococci spp. (26%), Pseudomonas aeruginosa (1%) seem to corroborate the literatures [3-8]. Staphylococcus aureus represented 72% of bacterial isolates; our results are similar to the results in Abubakar in northern Nigeria [11] but different from the ones reported by Srinivisan et al. [5] in her study where streptoccocus pneumoniae was the main cause of bacterial ulcers. Therefore, we can say that a bacterial ulcer in cameroonians should be considered of staphylococcal or streptococcal origin and treated as one until it is proven otherwise.
52 eyes (34.4%) were positive to fungal culture mainly from the Aspergillus family. Our results differ from the ones reported by Srinivisan [5,12,13] in South India (47.1% Fusarium spp, 16.1% Aspergillus spp), Liesegang and Forster from Ghana in south Florida [14] (61%. Fusarium spp) and Hagan et al [15] in Ghana (52% Fusarium spp). For Dóczi [16], the differences in climates can explain this presentation. In fact, in agriculture based geographical regions with hot, humid, tropical or sub-tropical climates like Ghana, Floride or South India, Fusarium keratitis is predominant. The particularity of the climate of Yaounde and his subburns (tropical wet and dry/ savanna climate) which is more temperate than others zones in Cameroon like Douala, can explain the predominance of Aspergillus spp or candida spp infections in our study. Nevertheless, fungal keratitis seems to be an enormous public health problem in Cameroon. The big prevalence of these infections can also be explained by the use of traditional medicine by the patients that are from vegetable origin.
The bacterial strains were more sensitive to antibiotics of the quinolone, aminoglycoside and rifamycin family and a little less to cephalosporins and beta lactamines. Our results are similar to the ones of Abubakar in Nigeria [11] or Erzoudi in Greece [17] (100% sensitivity to ciprofloxacie for gramm negative and positive bacterias). A previous study done in Ethiopia [18] showed also a big resistance of Gram-positive cocci (57% ) to Penicillin and Amoxicillin. For Wuletaw T [7], this resistance can be explained by their frequent use by the patients both with and without prescription. The high sensitivity of mycotic strains to triazoles (econazole and miconazole) seems to corroborate the literature [19]. Many authors recommend topical natamycin as first choice of treatment in fungal keratitis, although topical amphotericin B is the best choice for Aspergillus and Candida keratitis [19,20]. More to that Amphotericin is a very expensive drug in our context and so difficult to afford for many patients.
Ciprofloxacine and econazole were the principal topical drugs used for the treatment of patients. This can be explained by the availability of these molecules in our structure. An initial dual therapy based on this two molecules has been done in 71% of cases and seems to be efficient as an empiric treatment when cornea sampling can’t be done; in fact, we notice a high rate of favorable evolution and a reduced number of eviscerations done. Ghokale [20] did a comparison between fortified drugs and fluoroquinolones and found that they have equivalent efficacity and therefore recommend 4th generation quinolones as first line treatment for bacterial corneal ulcers because of their affordability and less toxicity on that organ.
Conclusion
For the best of our knowledge, this study is one of the first of his kind in Cameroon. Corneal ulcers are frequent amongst middle aged male Cameroonians doing manual work. The main germs in causes are Staphylococcus spp, streptococcus pneumonia and Aspergillus responding very well to quinolones and econazole. As for Srinivisan [6], this knowledge is essential, firstly, to define the magnitude of the problem in terms of health care costs, human costs, and the economic burden of blindness and, secondly, to design an efficient public health programme for the rapid referral, diagnosis, treatment, and ultimately the prevention of corneal ulceration in the population at risk. It will also help to guide Cameroonian eye care pratitionners in the management of corneal ulcers in some remote areas where sampling is not possible. This approach has important public health implications for the treatment and prevention of corneal ulceration in the developing world.
*This article was the subject of an oral communication at the 126th congress of the French society of ophthalmology and at the 28th congress of the Cameroonian society of ophthalmology.
Acknowledgement
To all the medical staff of Magrabi ICO Cameroon Eye Institute.
References
- Vemuganti GK, Murthy SI, Das S (2011) Update on pathologic diagnosis of corneal infections and inflammations. Middle East Afr J Ophthalmol 18: 277-284.
- Bakayoko S, Elien Gagnan Yan Zaou RR, Kole Sidibe M, Dicko M, et al. (2020) Épidémiologie des Abcès Graves de la Cornée au Centre Hospitalier et Universitaire IOTA. Health Sci Dis 21(7): 1-4.
- Zemba M, Dumitrescu OM, Dimirache AE, Branisteanu DC, Balta F, et al. (2022) Diagnostic methods for the etiological assessment of infectious corneal pathology (Review). Exp Ther Med 23(2): 137.
- Ting DSJ, Ho CS, Deshmukh R, Dalia GS, Harminder SD (2021) Infectious keratitis: an update on epidemiology, causative microorganisms, risk factors, and antimicrobial resistance. Eye 35(4): 1084-1101.
- Srinivasan M, Gonzales CA, George C, Cevallos V, Mascarenhas JM, et al. (1997) Epidemiology and aetiological diagnosis of corneal ulceration in Madurai, south India. Br J Ophthalmol 81(11): 965-971.
- Keshav BR, Zacheria G, Ideculla T, Bhat V, Joseph M (2008) Epidemiological characteristics of corneal ulcers in South sharqiya region. Oman Med J 23(1): 34-39.
- Raobela L, Ralibert JN, Andriatsilavo RR , Randrianarisoa HL, Volamarina RF, et al. (2015) Les abcès cornéens graves présumés d’origine bactérienne vus au Centre Hospitalier Universitaire d’ Rev. anesth.-réanim. Med Urgence 7(1): 10-14.
- Tarekegn W, Mekuanint G, Adane B, Wossen M, Baye G (2021) Clinical and Microbiological Profile of Bacterial and Fungal Suspected Corneal Ulcer at University of Gondar Tertiary Eye Care and Training Centre, Northwest Ethiopia. J Ophthalmology 2021: 9.
- Upadhyay MP, Rai NC, Brandt F, Shrestha RB (1982) Corneal ulcers in Nepal. Graefes Arch Clin Exp Ophthalmol 219(2): 55-59.
- Dunlop AA, Wright ED, Howlader SA, Nazrul I, Husain R, et al. (1994) Suppurative corneal ulceration in Bangladesh. A study of 142 cases examining the microbiological diagnosis, clinical and epidemiological features of bacterial and fungal keratitis. Aust N Z J Ophthalmol 22(2): 105-110.
- Abubakar UM, Lawan A, Muhammad I (2018) Clinical pattern and antibiotic sensitivity of bacterial corneal ulcers in Kano, Northern Nigeria. Ann Afr Med 17(3): 151-155.
- Gonzales CA, Srinivasan M, Whitcher JP, Smolin G (1996) Incidence of corneal ulceration in Madurai district, South India. Ophthalmic Epidemiol 3(3): 159-166.
- Ting DSJ, Ho CS, Cairns J, Elsahn A, Al-Aqaba M, et al. (2021) 12-year analysis of incidence, microbiological profiles and in vitro antimicrobial susceptibility of infectious keratitis: the Nottingham Infectious Keratitis Study. Br J Ophthalmol 105(3): 328-333.
- Liesegang TJ, Forster RK (1980) Spectrum of microbial keratitis in South Florida. Am J Ophthalmol 90(1): 38.
- Leck AK, Thomas PA, Hagan M, Kaliamurthy J, Ackuaku E, et al. (2002) Aetiology of suppurative corneal ulcers in Ghana and south India, and epidemiology of fungal keratitis. Br J Ophthalmol 86(11): 1211-1215.
- Dóczi I, Gyetvai T, Kredics L, Nagy E (2004) Involvement of Fusarium spp. in fungal keratitis. Clin Microbiol Infect 10(9): 773-776.
- Erzidou C, Dalianis G, Brozou CG, Nektarios M, Stamatina G (2016) Corneal ulcer: analysis of isolated bacteria and antibiotics sensitivity in the urban region of Attica, Greece. Adv Ophthalmol Vis Syst 5(3): 251-254.
- Siraj M, Teklebirhan G, Bitew A (2018) Clinical and microbiological profile of keratitis in menelik II memorial hospital, Addis Ababa, Ethiopia. Microbiol 14(4): 173-180.
- Mahmoudi S, Masoomi A, Ahmadikia K, Seyed AT, Mohammad S, et al. (2018) Fungal keratitis: An overview of clinical and laboratory aspects. Mycoses 61(12): 916-930.
- Gokhale NS (2008) Medical management approach to infectious keratitis. Indian J Ophthalmol 56(3): 215-220.






























