Visual Outcomes after Corneal Tear Repair in Children: RGP V/S Soft Contact Lenses
Ankit S Varshney1*, Najwa Masuri2 and Vivek Reshamwala3
1Associate Professor, Department of Optometry, Shree Bharatimaiya College of Optometry & Physiotherapy, Surat, India
2Assistant Professor, Department of Optometry, Shree Bharatimaiya College of Optometry & Physiotherapy, Surat, India
3Master of Optometry student, Department of Optometry, Shree Bharatimaiya College of Optometry & Physiotherapy, Surat, India
Submission: February 13, 2024; Published: February 23, 2024
*Corresponding author: Ankit S Varshney, Associate Professor, Department of Optometry, Shree Bharatimaiya College of Optometry & Physiotherapy, Surat, India
How to cite this article: Ankit S Varshney, Najwa M, Vivek Reshamwala. Visual Outcomes after Corneal Tear Repair in Children: RGP V/S Soft Contact Lenses. JOJ Ophthalmol. 2024; 10(4): 555794. DOI: 10.19080/JOJO.2024.10.555794
Abstract
Background: This study aimed to evaluate the effects of the use of rigid gas permeable and soft contact lenses to improve the visual outcome after a repair of traumatic corneal wounds with or without surgical aphakia in the pediatric age group.
Methods: A retrospective study has been carried out and analyzed over a period of five years for children under the age of 18 who are prescribed to undergo visual rehabilitation after visual loss. In this study, two groups of patients (n=15 eyes each) suffered traumatic full thickness corneal wounds. All cases were caused by sharp objects such as knives or glass, which caused full thickness corneal wounds with or without any other associated eye injury. One group was repaired and treated medically with a rigid gas-permeable contact lens that was fitted on the cornea (RGP CL group), and the other group was repaired and treated medically with a soft contact lens that was fitted on the cornea (SCL Group) which was compared with spectacle correction. Each patient was followed up until complete healing, the sutures were removed after about 6 weeks, and the patients were followed-up for a further 6 weeks, for a complete follow-up period of 3 months, after which postoperative refraction, manifest refractive spherical equivalent, uncorrected visual acuity, and best-corrected visual acuity with spectacles and contact lenses were measured and compared between the two groups.
Results: After repair and follow-up, uncorrected visual acuity ≤0.1 (decimal visual acuity system) was achieved in 30 cases in the Corneal Tear Repair with and without Aphakia, Best-corrected visual acuity ≥0.2 was achieved with spectacles (P=0.018). Best-corrected visual acuity ≥0.6 was achieved in 15 eyes with the RGP contact lens group and ≥0.4 was achieved in 15 eyes with soft contact lens group which is statistically significant (P = 0.0047).
Conclusion: After the healing of traumatic corneal injuries, RGP contact lenses offer a useful refractive treatment alternative in traumatized eyes of children. Eyes with high degrees of astigmatism were found to benefit the most. RGP contact lenses were found to be well tolerated in this population.
Keywords: Visual Outcome ; Surgical Aphakia ; Pediatric Age Group ; Rigid Gas Permeable Contact Lenses ; Soft Contact Lenses
Abbreviations: RGP: Rigid Gas Permeable; SCL: Soft Contact Lens; MRSE: Mean Refraction Spherical Equivalent; RGP CL: Rigid Gas-Permeable Contact Lens; FML: Fluorometholone; UCVA: Uncorrected Visual Acuity; BCVA: Best-Corrected Visual Acuity; CT: Computed Tomography; MRI: Magnetic Resonance Imaging
Introduction
Serious eye injuries with ruptured eyeballs often lead to permanent vision loss. Luckily, wounds on the cornea (clear front part of the eye) have a better chance of healing well, especially if treated promptly and without other eye damage. However, delayed treatment due to late presentation increases the risk of infection and worsens the outcome [1,2]. Treating corneal wounds is complex and lacks standard guidelines. While special contact lenses are known to help heal various eye issues, this study explored their effectiveness in children (under 18) with traumatic corneal wounds [3]. The research found that hard, gas-permeable contact lenses improved vision significantly after corneal repair, especially in children with high astigmatism (blurred vision). Interestingly, factors like age, scar location, and injury severity didn't seem to affect this improvement [4,5]. Similar studies on children with more severe eye injuries suggest vision outcomes depend on initial and final vision, injury severity, and other factors [6]. Overall, both soft and hard contact lenses improve vision after corneal injury repair, with early intervention being crucial for optimal results. Additionally, children who undergo corneal transplants can also experience vision benefits, although underlying genetic conditions may affect outcomes [7]. The present study reports on the usefulness of contact lenses in decreasing the degree of induced astigmatism and improving the visual outcome after repair of traumatic corneal wounds in pediatric age group.
Materials and Methods
From August 2018 to July 2023, the ophthalmology department's emergency room at Shree K.P. the Sangvi Eye Hospital in Surat, India, admitted pediatric patients below the age of 18 years for this study. This study comprised a total of 30 children, with 20 being males and 10 being females. All cases suffered from various forms of total traumatic corneal injury caused by sharp objects such as knives or glass, as the patients stated in the history. All eyes were examined with a slit light and showed no other eye injuries other than corneal injuries. All participants received informed consent. The study was approved by the Ethics Committee.
The patients with complete corneal trauma were divided into two groups (n=15 eyes), each of which was repaired and fitted with a rigid gas-permeable contact lens on the cornea (RGP CL group), (Boston XO, United States), and the other was fitted with a soft toric contact lens after a repair (Biofinity XR toric, Cooper Vision, United States). All patients were subjected to surgical repairs under general anesthesia using nylon 10/0 sutures (Ethicon Inc., USA). After repairs with corneal sutures, all patients received broad-spectrum antibiotic treatment (Moxifloxacin; Vigamox®, Alcon, United States), Pred-Forte®, Allergan Inc., United States), and Atropine sulfate (Isopto® Atropine, Alcon, United States). After the primary repair, both groups of patients were admitted for two days and supervised. During the admission, each patient was routinely referred to corneal ultrasound to assess the posterior segment and exclude its involvement.
After 2 days of admission, all patients were discharged and instructed to come for follow-up every week. The patients were followed up for 2 weeks, after which medical treatment was stopped with the gradual withdrawal of topical steroids. After cessation of all drugs, the patients were continued on a weak topical steroid (fluorometholone; FML®, Allergan Inc.) and lubricants to improve corneal healing and decrease the density of the corneal scar. After 6 weeks of follow-up, all patients were instructed to attend the outpatient clinic for suture removal under topical anesthesia (Proparacaine 0.5%; Sunways, Inc.) after topical antibiotic (Vigamox) installation four times daily for 3 days. After suture removal, all patients were kept on fluorometholone (FML) and lubricants until they completed 3 months of follow-up. After 3 months, each patient underwent an assessment of visual function, postoperative refraction, and manifest refractive spherical equivalent (MRSE), uncorrected visual acuity (UCVA), and best-corrected visual acuity (BCVA) were measured in both groups, compared, and statistically analyzed. All parents of pediatric patients were given detailed explanations regarding the care and routine for wearing contact lenses. Additionally, they received comprehensive training on how to properly insert and remove the lenses and were advised to wear them for a duration of 8-10 hours per day. The parents were also informed about the adjustment period and were scheduled for a follow-up appointment after 6 months. The data underwent statistical analysis using the chi-square test and t-test, utilizing the Statistical Package for the Social Sciences version 20 software developed by IBM Corporation in Armonk, NY, USA. The results are presented in terms of the mean and standard deviation.
Results
The slit-lamp examination of patients in both groups demonstrated that their corneal wounds ranged in size from 3 to 9 mm in length at different locations within the cornea. Eight eyes involved both the central and peripheral parts of the cornea, five eyes were mostly peripheral (outside the center 8 mm), and seventeen eyes were central (involving the central 8 mm). In 21 cases, the right eye suffered injury, while the left eye was affected in 9 cases.
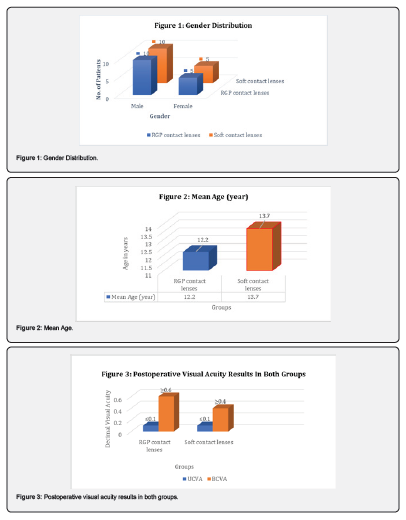
A total of 30 patients (20 males, 10 females) were included in the study, with 10 males and 5 females in each contact lens group (Figure 1). The mean patient age was 12.2 ± 3.8 years (range 7–18 years) in the RGP contact lens group compared to 13.7 ± 4.4 years (range 6–18 years) in the soft contact lens group (Figure 2). The RGP contact lens group exhibited a mean postoperative spherical error of +0.5 ± 2.55 D (range: -1.25 to +2.5 D) and a mean astigmatism of -1.5 ± 2.75 D (range: -3.5 to +2.25 D). The mean MRSE was -0.52 ± 2.64 D (range: -2.25 to +4.5 D). In comparison, the soft contact lens group showed a mean postoperative spherical error of +0.9 ± 2.44 D (range: -2.0 to + 4.75 D) and a mean astigmatism of +2.22 ± 3.43 D (range: -4.5 to +5.0 D). The mean MRSE was +1.32 ± 2.36 D (range: -4.75 to +5.25 D).
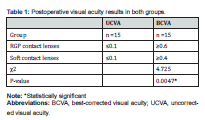
The following results were obtained from a decimal visual acuity system used to evaluate visual acuity. In 30 eyes following Corneal Tear Repair with and without aphakia, the postoperative UCVA was ≤0.1. The postoperative BCVA achieved while wearing spectacles was ≥0.2 (P=0.018). When comparing the visual acuity results between the two groups, it was observed that 15 eyes in the RGP contact lens group and 15 eyes in the soft contact lens group had best-corrected visual acuity of ≥0.6 and ≥0.4, respectively. These results are statistically significant (P = 0.0047) (Table 1) (Figure 3).
Discussion
Traumatic corneal wounds pose a significant challenge for ophthalmologists worldwide. Surgical repair remains the mainstay of treatment, as evidenced by the 3% of emergency department visits in the USA attributed to ocular trauma. Careful examination and assessment are crucial to minimize further damage and preserve vision. Particularly for open globe injuries, ruling out life-threatening associations is paramount. Detailed history-taking is essential to determine the timing, mechanism, location, and object involved. Organic materials like wood carry a higher risk of infection, while metallic objects may induce intraocular reactions like siderosis and chalcosis [8].
Following comprehensive history-taking, a meticulous and systematic ocular examination is crucial to ensure all injuries are identified. Imaging plays a vital role in revealing potential associated injuries like orbital wall fractures and intraocular foreign bodies [3]. Among imaging techniques, computed tomography (CT) offers the most valuable data, providing detailed information about both ocular and orbital structures. Plain X-rays and magnetic resonance imaging (MRI) have limited use in this context [9-11]. Ocular ultrasonography is particularly valuable, demonstrating the extent of ocular damage, presence of foreign bodies, and associated orbital injuries. One study reported a remarkable sensitivity of 100% and specificity of 97.2% for detecting ocular pathology with this technique [12,13].
Multiple factors influence final visual outcomes after ocular trauma, including the extent of damage, associated injuries, potential infections, access to specialized ophthalmologists, and the availability of well-equipped surgical facilities. This study adhered to established guidelines for managing such cases to optimize patient outcomes. Inclusion criteria for this study were restricted to patients with full-thickness corneal wounds isolated to the cornea, without any associated ocular or extraocular injuries. Cases with corneal or intraocular infections were also excluded. All repairs were performed by a highly qualified and experienced ophthalmologist. We meticulously evaluated and ruled out the potential influence of other factors known to impact the repair process, healing, and final visual outcome to ensure reliable results.
To the best of the author's knowledge, no previous reports or retrospective studies have compared the use of rigid gas-permeable (RGP) and soft contact lenses in improving visual outcomes after traumatic full-thickness corneal wound repair. This study investigated the potential benefits of both types of lenses. The authors propose that both RGP and soft contact lenses act as therapeutic molds, reshaping the cornea and minimizing surface irregularities that contribute to astigmatism and reduced vision. Specifically, they suggest that both types of lenses play a dual role: Firstly, maintaining wound apposition: The lenses help keep the wound edges aligned and close, promoting optimal healing and minimizing scarring. Secondly, providing mechanical support: The lenses offer physical protection and stability during the healing process.
This combined effect, according to the authors, leads to faster and more successful healing, ultimately resulting in a finer, less noticeable corneal scar and a greater likelihood of preserving good vision. However, they acknowledge that the final visual outcome improvement with using this strategy might be less dramatic compared to cases with more severe scarring.
This study investigated the efficacy of contact lenses in improving visual outcomes after corneal tear repair in children. The findings suggest that contact lens use can be an effective strategy for achieving positive visual outcomes in this population. The RGP contact lens group achieved a lower mean postoperative spherical error compared to the soft contact lens group (+0.5 ± 2.55 D vs. +0.9 ± 2.44 D, respectively). Astigmatism was also significantly lower in the RGP group (-1.5 ± 2.75 D) compared to the soft contact lens group (+2.22 ± 3.43 D). This is reflected in the mean MRSE, which was significantly lower in the RGP group (-0.52 ± 2.64 D) compared to the soft contact lens group (+1.32 ± 2.36 D).
Compared to the soft contact lens group, the RGP contact lens group exhibited narrower ranges for postoperative spherical error, astigmatism, and MRSE. This finding suggests potentially better healing and a more favorable anatomical and functional state of the injured cornea following repair with RGP lenses compared to soft lenses. The narrower range indicates a more consistent and controlled healing process with RGP lenses, likely due to their ability to maintain the structural integrity of the cornea more effectively.
Visual acuity assessment using a decimal system revealed promising results. Postoperative uncorrected visual acuity (UCVA) was ≤0.1 in both RGP and soft contact lens groups (30 eyes each), suggesting good initial recovery. While spectacle correction achieved a minimum best-corrected visual acuity (BCVA) of ≥0.2 in both groups, a significant difference emerged in the RGP group. Fifteen eyes in the RGP group achieved a BCVA of ≥0.6 compared to only 15 eyes reaching ≥0.4 in the soft contact lens group (p=0.0047). This statistically significant difference indicates superior visual outcomes with RGP lenses.
Several studies support the use of contact lenses for improving visual outcomes in children after corneal repair: Jain [14] reported a 68% success rate in achieving visual acuity of 6/12 or better using hard corneal lenses in children with traumatic aphakia. Yehezkeli [15] demonstrated the effectiveness of scleral lenses in aphakic children, with 76% achieving a best-corrected visual acuity of 20/40 or better. Wietharn [16] showed positive outcomes in visual function after penetrating keratoplasty with contact lenses.
Rigid Gas Permeable (RGP) lenses have also been successful in adults with post-traumatic corneas:
Kanpolat [17] reported an 82% success rate in fitting RGP lenses to these patients. Scanzera [18] found improved visual acuity in patients with corneal scarring and aphakia following open globe trauma using RGP lenses. Singh [19] observed significant visual acuity improvement in patients with corneal scars and opacities using RGP lenses (70% success rate). However, it is crucial to acknowledge potential limitations: Zheng [20] and Kanpolat [17] highlighted complications and dropout rates due to factors like age, motivation, and intolerance. Collectively, these studies suggest that contact lenses, particularly RGP lenses, can be a valuable tool for improving visual outcomes in children and adults after corneal repair. However, careful consideration of potential challenges is necessary for successful implementation. In assumption, the study's primary objective of demonstrating improved visual acuity with RGP lenses after full-thickness corneal repair was achieved. This finding suggests potential benefits of RGP lenses in optimizing visual outcomes compared to soft lenses.
Conclusion
This study investigated the use of contact lenses, particularly rigid gas permeable (RGP) lenses, as a potential alternative refractive treatment for children with scared and traumatized corneas. The findings suggest that RGP lenses offer several advantages over spectacles and soft contact lenses in this population:
Improved Visual Outcomes: Compared to spectacles and soft lenses, RGP lenses led to significantly better visual acuity, especially in children with high degrees of astigmatism. This may be due to the ability of RGP lenses to reshape the irregular corneal surface, leading to a more focused image on the retina. Enhanced Comfort: Contrary to expectations, the study found that RGP lenses were well-tolerated by most children. This is likely due to the advanced design and fitting techniques used for pediatric RGP lenses, which prioritize comfort and stability. Additional Benefits: RGP lenses can also provide other benefits for children with corneal trauma, such as protecting the fragile cornea, promoting regular wound healing, and reducing irregular astigmatism. Overall, this study suggests that RGP lenses have the potential to be a valuable alternative to spectacles and soft lenses for children with scared and traumatized corneas. However, further research and careful consideration of individual factors are needed before widespread adoption.
Limitations
While the study showed promising results, it is important to acknowledge potential limitations:
Limited Sample Size: Larger studies with more participants are needed to confirm these findings and assess the long-term effectiveness of RGP lenses in this population.
Individual Variability: The success of RGP lenses may vary depending on individual factors like age, motivation, and compliance with lens care routines.
Expertise Required: Fitting and managing RGP lenses in children requires specialized knowledge and skills, which may not be readily available in all clinics.
References
- I Rahman, A Maino, D Devadason, B Leatherbarrow (2006) Open globe injuries: factors predictive of poor outcome. Eye 20(12): 1336-1341.
- Hatton MP, Thakkar MM, Ray S (2002) Orbital and adnexal trauma associated with open globe injuries. Ophthalmol Plast Reconstr Surg 18(6): 458-461.
- Bord SP, Linden J (2008) Trauma to the globe and orbit. Emerg Med Clin N Am 26(1): 97-123.
- Kreidl K, Kim D, Mansour S (2003) Prevalence of significant intraocular sequelae in blunt ocular trauma. Am J Emerg Med. 21(7): 525-528.
- Esmaeli B, Elner SG, Schork MA, Elner VM (1995) Visual outcome and ocular survival after penetrating trauma. A clinicopathologic study. Ophthalmology 102(3): 393-400.
- Smith D, Wrenn K, Stack LB (2002) The epidemiology and diagnosis of penetrating eye injuries. Acad Emerg Med 9(3): 209-213.
- Rubinstein MP (2003) Applications of contact lens devices in the management of corneal disease. Eye 17(8): 872-876.
- Harlan JB, Pieramici DJ (2002) Evaluation of patients with ocular trauma. Ophthalmol Clin North Am 15(2): 153-161.
- Lakits A, Prokesch R, Scholda C, A Bankier (1999) Orbital helical computed tomography in the diagnosis and management of eye trauma. Ophthalmology 106(12): 2330-2335.
- Iinuma T, Hirota Y, Ishio K (1994) Orbital wall fractures. Conventional views and CT. Rhinology 32(2): 81-83.
- Eric P Holmgren, Eric J Dierks, Louis D Homer, Bryce E Potter (2004) Facial computed tomography use in trauma patients who require a head computed tomogram. J Oral Maxillofac Surg 62(8): 913-918.
- Blaivas M, Theodoro D, Sierzenski P (2002) A study of bedside ultrasonography in the emergency department. Acad Emerg Med 9(8): 791-799.
- McIlrath ST, Blaivas M, Lyon M (2005) Diagnosis of periorbital gas in ocular ultrasound after facial trauma. Am J Emerg Med 23(4): 517-520.
- I S Jain, K Mohan, A Gupta (1985) Unilateral traumatic aphakia in children: role of corneal contact lenses. Journal of pediatric ophthalmology and strabismus 22(4): 137-139.
- Veronika Yehezkeli, Ivan Hare, Elad Moisseiev, Ehud I Assia, Irit Chacham, et al. (2023) Assessment of long-term visual outcomes in aphakic children wearing scleral contact lenses. Eye 37(3): 421-426.
- Wietharn BE, William T Driebe (2004) Fitting Contact Lenses for Visual Rehabilitation After Penetrating Keratoplasty. Eye & Contact Lens: Science & Clinical Practice 30(1): 31-33.
- Kanpolat Ayfer, O U Ciftçi (1995) The use of rigid gas permeable contact lenses in scarred corneas. The CLAO journal: official publication of the Contact Lens Association of Ophthalmologists, Inc 21(1): 64-66.
- Angelica C Scanzera, Grace Dunbar, Vidhi Shah, Maria Soledad Cortina, Yannek I Leiderman, et al. (2020) Visual Rehabilitation with Contact Lenses Following Open Globe Trauma. Eye & Contact Lens: Science & Clinical Practice 47(5): 288-291.
- Kirti Singh, Divya Jain, Kunal Teli (2013) Rehabilitation of vision disabling corneal opacities: is there hope without corneal transplant? Contact lens & anterior eye: the journal of the British Contact Lens Association 36(2): 74-79.
- Bin Zheng, Lijun Shen, Maria K Walker, Zongduan Zhang, Jingwei Zheng, et al. (2015) Clinical Evaluation of Rigid Gas Permeable Contact Lenses and Visual Outcome After Repaired Corneal Laceration. Eye & Contact Lens: Science & Clinical Practice 41(1): 34-39.






























