Comparison of Age-Appropriate Visual Acuity Tests Based on Preferential Looking Principles in Infants with Retinopathy of Prematurity
Puja Sarbajna1*, Anand Vinekar2, Prithwis Manna1, Tos Berendschot3, Carroll AB Webers3, Rohit Shetty4 and Sourav Karmakar5
1Senior Consultant Optometrist, Narayana Nethralaya, Bengaluru, India
2Head, Department of Paediatric Retina, Narayana Nethralaya, Bengaluru, India
3Department of Ophthalmology, Maastricht University of Health Sciences, Netherlands, Europe
4Head, Department of Cornea and Refractive Surgery, Narayana Nethralaya, Bengaluru, India
5Assistant Professor, Department of Optometry and Vision Science, Amity University, Amity Education Valley Campus, Manesar, Gurgaon, Haryana, India
Submission: January 11, 2024; Published: January 18, 2024
*Corresponding author: Puja Sarbajna, Senior Consultant Optometrist, Narayana Nethralaya, Bengaluru, India
How to cite this article: Puja S, Anand V, Prithwis M, Tos B, Carroll AB W, et al. Comparison of Age-Appropriate Visual Acuity Tests Based on Preferential Looking Principles in Infants with Retinopathy of Prematurity. JOJ Ophthalmol. 2024; 10(3): 555790. DOI: 10.19080/JOJO.2024.10.555790
Abstract
Purpose: This study aimed to predict age-normal visual acuity scores and agreement between the TAC, the LGP, and the BGC for ROP infants.
Methods: The prospective observational study recruited 150 infants aged 3 to 12 months. Infants with ROP types I and II (study group) and without ROP (control group) were divided into three age groups: 3-5 months, 6-9 months, and 10-12 months. On days 1, 4, and 7, a single observer randomly measured monocular and binocular acuity using the TAC, the LGP, and the BGC. The mean acuity scores were analysed.
Result: The visual acuity of ROP infants improves significantly with age. Binocular acuity ranged from 3.00 (SD = 1.05) CPD to 8.13 (SD = 2.55) CPD using the TAC, from 2.66 (SD = 0.95) CPD to 7.41 (SD = 2.37) CPD using the LGP, and from 1.80 (SD = 0.83) up to 1.96 (SD = 0.80) CPD using the BGC. The TAC and LGP did not significantly differ (3-5 months, p = 0.086, 5–6 months, p = 0.765, and 10–12 months, p = 0.154). The mean acuity, however, was marginally lower than that of the control group. Intergroup comparisons demonstrated that the TAC and LGP measurements were consistent and interchangeable across all age groups.
Conclusion: The TAC, LGP, and BGC are reliable acuity tests. However, BGC is not interchangeable with TAC or LGP. More studies with larger sample sizes are essential to determine more exact age standards and whether various testers may attain equal acuity ratings.
Keywords: Preferential Looking Tests; Grating Acuity, Teller Acuity Card; LEA Grating Paddle; Brown’s Grating Card; Age-Normal Visual Acuity; Retinopathy of Prematurity
Abbreviations: TAC: Tellers Acuity Card; LGP: LEA Grating Paddle; BGC: Brown’s Grating Card; ROP: Retinopathy of Prematurity; SD: Standard Deviation; CPD: Cycles Per Degree; PFL: Preferential Looking Test; OD: Ocular Dexter / Right Eye; OS: Ocular Sinister/ Left Eye; OU: Ocular Uterque/ Both Eye.
Introduction
In India, Retinopathy of Prematurity (ROP) is an emerging preventable form of childhood blindness affecting preterm infants [1-3]. The reported incidence rates range from 38% to 51.9% [4]. Therefore, it is essential to combine ROP services with national child health services to safeguard the safe survival of premature infants. All premature infants admitted to special newborn care units must undergo a retinal examination due to vision-threatening ROP. Consequently, laser treatment becomes necessary to preserve patient’s eyesight [5]. Therefore, periodic visual acuity evaluations should be included in regular assessments and follow-up programs. However, evaluating visual acuity in this population is a formidable challenge. Fantz et al. devised the Forced Choice Preferential Looking (FPL) method to understand the constraints associated with studying the visual abilities of nonverbal infants. The method helps provide valuable insights into the developing brain from birth to six months [6-8]. Later, the introduction of the Tellers Acuity Card (TAC) procedure aided in the rapid assessment of infants' visual acuity. The procedure depends on the adult observer's subjective judgment of the minor stimuli an infant can detect [9]. Moreover, FPL and acuity card procedures share the same variability [10-12]. Therefore, the Tellers Acuity Card (TAC) has become the standard diagnostic instrument for evaluating visual acuity [13]. The LEA Grating Paddle (LGP) and Brown's Grating Card (BGC) are the other two visual acuity tests that measure the visual acuity of preverbal children using the PFL method [14,15]. Several studies have analyzed the performance of the TAC [10,11,16,17] and LGP [14,18,19] in normal infants and determined the average visual acuity scores based on age. Consequently, a hypothesis assumes that all three acuity tests based on the PFL are efficacious at assessing the visual acuity of newborns with ROP and can generate precise and dependable outcomes. Therefore, the primary aim of this study was to evaluate the predictive visual acuity of infants with ROP and the agreement between the three visual acuity tests. If this hypothesis is confirmed, PFL-based acuity tests will aid in the early identification and management of visual challenges in ROP infants.
Patients and Methods
This prospective, observational study was directed at a tertiary eye care centre in Bengaluru, India, between January 202 and August 2023 after obtaining clearance from the Institutional Review Board and following the tenets of the Declaration of Helsinki. After the study’s goal was explained, the infant's parents signed the informed consent form.
Patient Selection
The study included infants born normally without ROP, with ROP type I or type II, and who underwent laser treatment. The study excluded infants with a history of ocular surgery, untreated type II ROP, untreated type III ROP, or a loss to follow-up. At the outset of the study, 210 infants were included, both with and without ROP. After recording the ocular history, 25 infants were considered ineligible because of an absence of follow-up; 5 infants were diagnosed with type II ROP but did not receive laser treatment; 28 infants were fussy and unresponsive during evaluation, and two infants were diagnosed later with type III ROP. A total of 150 infants aged between 3 and 12 months were ultimately included in the study. The age limit was set up based on developmental milestones. At three months, the infant develops the ability to shift their visual focus from one object to another and to follow moving objects with their eyes. In addition, by 12 months, infants gain increased senses and learn to coordinate their vision with their body movements [20]. Among the 150 infants, 75 were born normal, healthy, or without ROP; these patients composed the "control group." The 75 infants included had type I and type II ROP treated with laser radiation and composed the experimental group, represented as "with ROP."
Setup for Evaluation
The study ensured that the illumination of the examination room was within the standard range of 150-300 lx and that the background was uniformly grey to prevent distraction. A single observer with extensive training conducted the monocular and binocular visual acuity tests using the TAC, LGP, and BGC. The infant's mother held the infant at a consistent distance during the test following the procedure reference for accurate results. In addition, the observer ensured that the infants were awake and coherent by displaying low spatial frequency gratings. The three visual acuity tests were performed monocularly and then binocularly in a random order on days 1, 4, and 7 of the study to reduce the possibility of bias.
Procedures
During the Tellers Acuity Card™ II (TAC) test, infants aged 3 to 5 months and infants aged 6 to 12 months were positioned 38 cm and 55 cm behind the stage, respectively. For the visual acuity evaluation, the observer used seventeen sets of 25.5 x 55.5 cm cards with black and white gratings painted on one side of each card. Early after the commencement of the exam, the cards were stacked facing down. On the reverse of each card, the grating size was written down in cycles per centimeter (CPCM). The observer selected the first card for the presentation based on the infant's abilities and age group. The observer then progressively enhanced the complexity of the gratings by selecting cards with increasing CPCM values. After the test, the scores were converted to CPD values using the formula [(test distance/55) x CPCM]. As the test progressed, this allowed for a more accurate assessment of the infant's visual acuity and ability to perceive finer details. Through the peephole, the observer viewed the infant's eye movements. If the observer found that the infant distinguished the gratings presented until the infant showed no evidence of resolving the stripes. Each card was presented twice before determining whether the infant could resolve the gratings [21,22]. During the LEA Grating Paddle #253300 (LGP) test, the observer kept the appropriate distance. 28 centimeters for infants aged 3 to 5 months, 57 centimeters for those aged 6 to 9 months, and 85 centimeters for those aged 10 to 12 months.
The test employs four paddles measuring 31 cm in height and 19.5 cm in diameter. The observer always began the evaluation with the coarsest grating, followed by the second grating. The observer then sees the infant's eye movements when presented with the gratings. The observer presented increasingly fine gratings until the observer found that the infant could not detect the grating patterns. At that point, acuity scores were recorded. Afterward, using the formula [test distance/57.2) x CPCM], the acuity scores recorded in CPCM were converted to CPD [18,23]. The observer ensured that the test distance was 36 cm for all age categories when conducting visual acuity tests with a Brown Grating Card (BGC). The test consisted of six sets of 35 x 36 cm cards and a 12 x 14 cm rectangular grating window in the centre. The observer presented the infant with the coarser gratings first, followed by the finer gratings, until the observer found that the infant could not distinguish the stripes. The observer moved each card 20 centimeters to the right or left and held it still for several seconds while continuing to see the infants. Through the 2-millimeter-diameter peephole, the observer observed the eye movements of the infants. After using the formula [(test distance/55) x CPCM], the acuity score measured in CPCM was converted to CPD [15].
Statistical Analysis
The statistical information is presented as the mean and standard deviation (SD). Three visual acuity scores of each acuity test were stored using Microsoft Office Excel 365 and the average visual acuity was calculated. The mean score data were then used for the analysis. The normality of the data was calculated using the Kolmogorov-Smirnov test. The Wilcoxon signed-rank test was used to compare the mean visual acuity scores between the age groups and study groups. The analysis was conducted using the IBM Statistical Package for the Social Sciences (version 27.0). A p-value of 0.05 or less was considered to indicate statistical significance.
Results
The study involved 150 infants aged 3 to 12 months, 80 of whom were male and 70 of whom were female. The average age of the infants was 7.48 (SD = 3.17) months. On average, the infants in the control group were a few days older than those with ROP were. Table 1 presents the average age of the two groups. For statistical analysis, there were 25 infants in each of the three age categories (3-5 months, 6-9 months, and 10–12 months). Table 2 shows the initial mean visual acuity standard (CPD) and standard deviation (SD) for each age group. There was a steady increase in the visual acuity scores with increasing age when measured using the TAC and the LGP, compared to the BGC. The acuity scores prove that infant visual acuity improves with age, regardless of the presence or absence of ROP. The Wilcoxon signed rank test was used to compare visual acuity and agreement within and between the different age groups. The findings of these tests are presented in Tables 3 and 4, respectively. Figure 1 represents the monocular and binocular visual acuity scores of infants aged 3-5 months according to the using the TAC, LGP, and BGC. In both the control and ROP groups, the mean scores for TAC (control: OD: 3.59 CPD, OS: 3.55 CPD, OU: 3.59 CPD; ROP: OD: 2.78 CPD, OS: 2.75 CPD, OU: 3.00 CPD) and LGP (control: OD: 3.09 CPD, OS: 3.09 CPD, OU: 3.09 CPD; ROP: OD: 2.58 CPD, OS: 2.58 CPD, OU: 2.66 CPD) were comparable, with the control group having slightly better visual acuity. However, the mean scores continued to decrease when evaluated using BGC (control: OD: 1.80 CPD, OS: 1.75 CPD, OU: 1.81 CPD; ROP: OD: 1.74 CPD, OS: 1.60 CPD, OU: 1.80 CPD). The Wilcoxon signed rank test revealed no significant difference between TAC and LGP (control: OD: p = 0.077, OS: p = 0.164, OU: p = 0.77; ROP: OD: p = 0.366, OS: p = 0.365, OU: p = 0.086). The TAC and BGC differed significantly (p = 0.001), as shown by the LGP and BGC (p = 0.001) for both the control and ROP groups (Table 4).
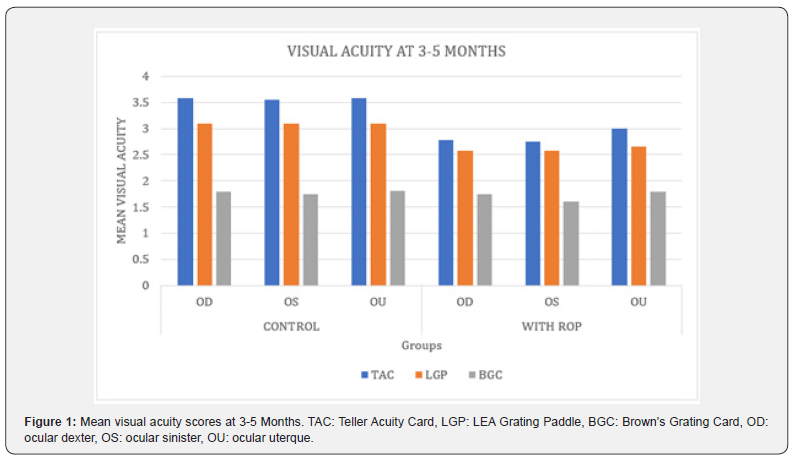
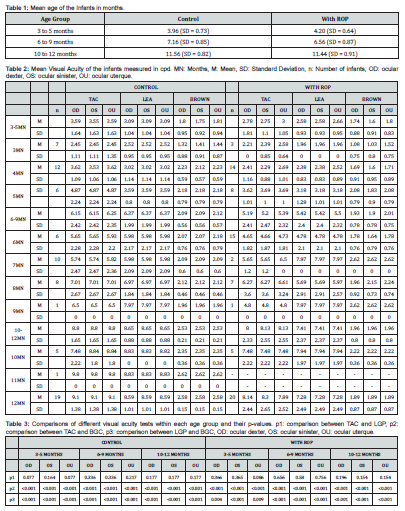

Figure 2 shows the monocular and binocular visual acuity scores of the TAC, LGP, and BGC at 6–9 months. Mean visual acuity increased rapidly with TAC (control: OD: 6.50 CPD, OS: 6.56 CPD, OU: 6.60 CPD; ROP: OD: 4.97 CPD, OS: 4.97 CPD, OU: 5.14 CPD), and LGP (control: OD: 6.53 CPD, OS: 6.53 CPD, OU: 6.53 CPD; ROP: OD: 5.26 CPD, OS: 5.26 CPD, OU: 5.23 CPD). With BGC, however, the mean visual acuity score remained lower (Control: OD: 2.09 CPD, OS: 2.09 CPD, OU: 2.12 CPD; ROP: OD: 1.93 CPD, OS: 1.90 CPD, OU: 2.01 CPD). A comparison of the TAC and LGP using the Wilcoxon signed rank test yielded inconclusive results (Control: OD: p = 0.336, OS: p = 0.336, OU: p = 0.217; with ROP: OD: p = 0.656, OS: p = 0.580, OU: p = 0.756). When comparing the control group and the ROP group, significant differences were detected between the TAC and BGC groups (p = 0.001) and between the LGP and BGC groups (p = 0.001).

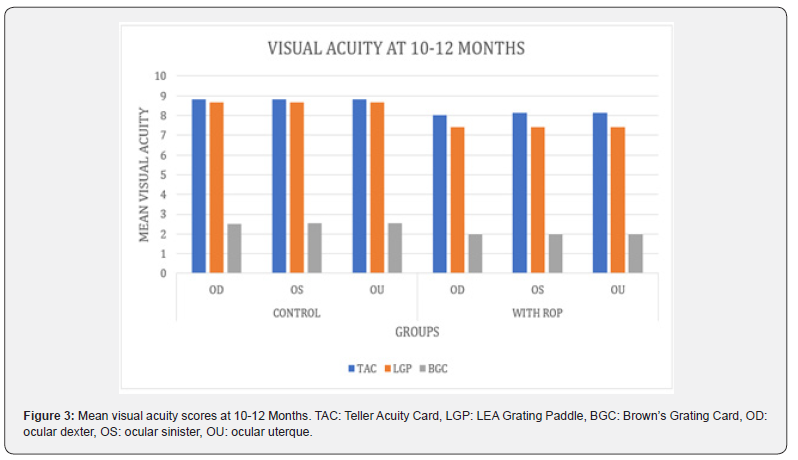
The Wilcoxon signed rank test revealed no significant difference between the TAC and LGP in the 10–12 months age group (control: OD, OS, and OU: p = 0.177; ROP: OD: p = 0.196; OS: p = 0.154; OU: p = 0.154). TAC and BGC had a statistically significant different (p < 0.001), as was the LGP and BGC (p < 0.001). The mean visual acuity scores associated with TAC (control: OD: 8.80 CPD; OS: 8.80 CPD; OU: 8.80 CPD; ROP: OD: 8.00 CPD; OS: 8.13 CPD; OU: 8.13 CPD); LGP (control: OD: 8.30 CPD; OS: 8.30 CPD; OU: 8.65 CPD; ROP: OD: 7.41 CPD; OS: 7.41 CPD; OU: 7.41 CPD), and BGC (control: OD: 2.53 CPD; OS: 2.53 CPD; OU: 2.53 CPD; ROP: OD: 1.96 CPD; OS: 1.96 CPD; OU: 1.96 CPD) are presented in Figure 3.
The Wilcoxon signed rank test was used to compare the visual acuity scores between the two study groups. The results indicated that the TAC maintained agreement (OD: p = 0.078, OS: p = 0.073, OU: p = 0.113). The statistical analysis showed that the TAC is a viable option for assessing infants' visual acuity at this age in both groups. When compared between each eye, the LGP was more reliable across the tests (3-5 months: OD: p = 0.075, OS: p = 0.075, OU: p = 0.960; 6–9 months: OD: p = 0.051, OS: p = 0.051, OU: p = 0.064; 10–12 months: OD, OS, and OU, p = 0.086). There was no statistically significant difference in age according to the BGC test (OD: p = 0.227, OS: p = 0.139, OU: p = 0.352, and 6–9 months: OD: p = 0.264, OS: p = 0.264, OU: p = 0.564). Figure 4 graphically stands for the comparison between the two groups. Considering these results, the TAC may not be as dependable as the LGP in assessing infants' visual acuity at different ages. However, when comparing results across age groups, the LGP appears to be the most exact and reliable indicator of infant visual acuity. The results suggest that TAC and LGP interventions positively affect visual acuity scores, with a significant increase observed in the group with ROP compared to the control group. Nevertheless, the BGC intervention did not result in the same improvement in visual acuity scores, indicating a potential limitation or lesser effectiveness of this intervention in improving visual acuity in this population.
Discussion
The present study employed the three-grating acuity card procedure to assess visual acuity, both monocularly and binocularly, a method based on preferential looking. One study indicated that infants born with ROP had lower mean visual acuity scores than infants without ROP [15,24]. Nevertheless, it is worth noting that both groups showed significant and swift improvements in their visual acuity scores during the study period, which extended from 3 to 12 months. The potential adverse effects of ROP could explain the disparity in acuity scores, primarily due to the proliferation of retinal blood vessels [25]. Regardless of the disparity, the rapid improvement in visual acuity substantiates the developmental progression of the retina alongside the increased concentration and arrangement of cone photoreceptors [18,26]. The study assessed the visual acuity scores of infants categorized as "controls" or "with ROP" using TAC. The binocular visual acuity scores ranged from 2.45 CPD at three months to 9.10 CPD at 12 months for the "control" group and from 2.58 CPD at three months to 7.89 CPD at 12 months for the "with ROP" group. The LGP acuity score ranged from 2.52 CPD at three months to 8.59 CPD at 12 months for the control infants. In contrast, for infants with ROP, the score was 1.96 CPD at three months and 7.28 CPD at 12 months. In addition, the BGC acuity score seen at three months for the control infants was 1.44 CPD, which improved to 2.58 CPD by the time the infants reached 12 months of age. The acuity score for infants with ROP varies from 1.03 CPD at three months to 1.89 CPD at 12 months. Vision assessment with the TAC remains the primary diagnostic instrument for evaluating visual acuity in preverbal children [13]. The visual acuity score obtained in the present study was not directly comparable to that of earlier studies due to variations in sample sizes and methodological approaches employed in both studies. However, the measured visual acuity documented in this study exhibits like the findings reported by Courage and Adams. The author reported the mean acuity score of 20 infants in each age group as 2.6 CPD at the three-month mark, 5.9 CPD at the six-month mark, and 9.6 CPD at the 12-month mark [27]. In other previous investigations, the observed visual acuity varied, exhibiting either lower [17] or higher [11] values.

Based on our literature search, three studies have documented the use of the LGP to assess age-normal visual acuity. The visual acuity score observed in this study is like that reported by Yudcovitch et al. (4 CPD at 0-4 months; 9.3 CPD at 12-16 months) [28] and lower than that reported by Elgohary et al. [18]. In addition, a single study utilized the BGC to evaluate visual acuity in infants born full-term or preterm [15], which resulted in significantly lower visual acuity measurements than did the present study. The consistent and comparable outcomes demonstrated the proficiency of the single observer [12,29,30] in conducting the three assessments, irrespective of the infant's condition, whether it was normal or affected by ROP. Therefore, the visual acuity scores of the infants diagnosed with ROP in this study are dependable and indicative of their first age-appropriate visual acuity within the 3 to 12-month range, as assessed through the three administered tests.
This study analyzed the data obtained from each acuity test. The present study revealed significant relationships and agreement between the acuity scores of the individuals in the control group (p = 0.077 at 3-5 months, p = 0.217 at 6-9 months, and p = 0.177 at 10–12 months) and those of the ROP group (p = 0.152 at 3-5 months, p = 0.756 at 6–9 months, and p = 0.154 at 10–12 months). This finding is consistent with the research conducted by Yudcovitch et al. The author observed no statistically significant variation (p = 0.7516) across the different age groups, ranging from 0 to 4 months to 12 to 16 months [28]. Nevertheless, this study did not reveal any significant correlation between the TAC and BGC or between the LGP and BGC. The strong association observed between TAC and LGP in ROP infants shows the dependability of both test scores, rendering them interchangeable within clinical contexts.
According to the intergroup comparison in this study, neither TAC ( at 3-5 months, p = 0.113; at 6-9 months, p = 0.189; at 10-12 months, p = 0.053, for OU) nor LGP ( at 3-5 months, p = 0.960; at 6-9 months, p = 0.174; at 10–12 months, p = 0.086, for OU) showed a statistically significant difference in the acuity scores obtained for controlled or ROP infants in all age groups. Even though the BGC had a similar result until the age group of 6-9 months (p = 0.564), the study showed a significant difference beyond 10-12 months (p = 0.003). Therefore, the findings of this study suggest that the acuity scores of infants with ROP are marginally lower. However, this difference was not statistically significant when the TAC or the LGP were used. Across all age groups, the difference in TAC was significantly greater than that in LGP, except for in the 10–12-month age group, during which the difference in LGP was significant (p = 0.086) (p =0.053). One probable explanation is that infants display diminished interest in simple and similar grid stimuli. Compared with the enclosed stage used to present the TAC, infants exhibit greater interest in the observer, the stimuli presented by the observer, and the surrounding environment [31]. Therefore, the LGP appears to be more convenient and straightforward for evaluating visual acuity. Compared to TAC, LGP is also lightweight, low-cost, and portable, making it easy to evaluate in every available situation and test site [23,28]. Despite its advantages, the LGP does not allow "blind testing," as both sides of the paddle have the gratings painted. Therefore, the examiner is aware of their acuity when they are present. Both the LGP and BGC are portable grating acuity cards. Nevertheless, the acuity scores generated by the BGC exhibited a notable difference (p < 0.001) from those generated by the TAC and LGP. One crucial constraint in this study is the consistent testing distance employed across all age groups [15]. Both tests have a restricted quantity of acuity scorecards, six for the BGC and four for the LGP [15,23]. However, based on the infant's performance, the variable test distance makes the LGP more dependable and advantageous than the BGC. BGC, as a standalone tool, is limited by its ability to rapidly assess visual acuity [15] and cannot be directly compared to the effectiveness of TAC and LGP.
Conclusion
In summary, the TAC, LGP, and BGC acuity card procedures, which use the preferential-looking technique, offer reliable and effective behavioural assessments of an infant's visual acuity in a clinical setting, both for healthy infants and those with ROP. The efficiency of the BGC was not comparable or interchangeable. This study presents initial findings on age norms for ROP that agree with earlier age norm studies. However, additional investigations are needed to establish more extensive and standardized age norms for these evaluations. The study thus suggested the use of larger sample sizes and the assessment of the repeatability of acuity scores across multiple testers. Furthermore, this study proposes the utilization of LGP as a choice for assessing visual acuity in infants diagnosed with ROP, particularly in situations where financial limitations are present and across different testing locations and distances.
References
- Jefferies AL (2016) Retinopathy of prematurity: An update on screening and management. Paediatrics & child health 21(2): 101-104.
- Sanghi G, Mangat RD, Deeksha K, Amod G (2014) Aggressive posterior retinopathy of prematurity in infants≥ 1500 g birth weight. Indian J Ophthalmol 62(2): 254-247.
- Vinekar A, Chaitra J, Siddesh K, Shwetha M, Mangat Ram D, et al. (2016) Impact of improved neonatal care on the profile of retinopathy of prematurity in rural neonatal centers in India over a 4-year period. Eye and Brain 8: 45-53.
- Kaul S, Renu M, Madhuvanthi M, Divya M, Chirag S, et al. (2021) Prevalence and risk factors of retinopathy of prematurity inWestern Maharashtra. Indian J Clin Experiment Ophthalmol 7: 224-228.
- Shukla R, Murthy GVS, Clare G, Bala V, Sridivya M (2020) Operational guidelines for ROP in India: a summary. Indian J Ophthalmol 68(Suppl 1): S108-S114.
- Fantz RL (1965) Visual perception from birth as shown by pattern selectivity. Ann N Y Acad Sci 118(21): 793-814.
- Fantz RL, Ordy J (1959) Visual acuity test for infants under six months of age. The Psychological Record 9: 159.
- Frantz RL, Ordy J, Udelf M (1962) Maturation of pattern vision in infants during the first six months. J Comparative Physiological Psychol 55(6): 907.
- Chandna A, Pearson C, Doran R (1988) Preferential looking in clinical practice: a year's experience. Eye 2(5): 488-495.
- McDonald M, Sebris SL, Mohn G, Teller DY, Dobson V (1986) Monocular acuity in normal infants: the acuity card procedure. Am J Optom Physiol Opt 63(2): 127-134.
- Mayer DL, Beiser AS, Warner AF, Pratt EM, Raye KN, et al. (1995) Monocular acuity norms for the Teller Acuity Cards between ages one month and four years. Invest Ophthalmol & Visual Sci 36(3): 671-685.
- Atkinson J, Braddick O, Pimm-Smith E (1982) Preferential looking'for monocular and binocular acuity testing of infants. Br J Ophthalmol 66(4): 264-268.
- Sturm V, Cassel D, Eizenman M (2011) Objective estimation of visual acuity with preferential looking. Inves Ophthalmol Visual Sci 52(2): 708-713.
- Deshmukh AV, Uppal Vipul G, Ashik M, Akshay B, Ramesh K (2020) Interobserver variability for measurement of grating acuity in preverbal and nonverbal children using lea grating paddles. J Pediatr Ophthalmol Strabismus 57(5): 305-308.
- Brown AM, Yamamoto M (1986) Visual acuity in newborn and preterm infants measured with grating acuity cards. Am J Ophthalmol 102(2): 245-253.
- Clifford-Donaldson CE, Haynes BM, Dobson V (2006) Teller Acuity Card norms with and without use of a testing stage. J AAPOS 10(6): 547-551.
- Salomao SR, Ventura DF (1995) Large sample population age norms for visual acuities obtained with Vistech-Teller Acuity Cards. Investigative Ophthalmol Visual Sci 36(3): 657-670.
- Elgohary AA, Abuelela MH, Eldin AA (2017) Age norms for grating acuity and contrast sensitivity measured by Lea tests in the first three years of life. Int J Ophthalmol 10(7): 1150-1153.
- Mody KH, Mihir TK, Aparna S, Preeti D, Jaydeep AW, et al. (2012) Comparison of lea gratings with cardiff acuity cards for vision testing of preverbal children. Indian J Ophthalmol 60(6): 541.
- Boyd K (2022) Vision Development: Newborn to 12 Months.
- Davida Y Teller VD, Luisa Mayer D (2023) Teller Acuity Cards®.
- Quinn GE, Berlin JA, James M (1993) The Teller acuity card procedure: three testers in a clinical setting. Ophthalmol 100(4): 488-494.
- Hyvarinen L (2023) LEA Gratings.
- Van Hof-van Duin J, Mohn G (1986) The development of visual acuity in normal fullterm and preterm infants. Vis Res 26(6): 909-916.
- Strube YNJ, Wright KW (2022) Pathophysiology of retinopathy of prematurity. Saudi J Ophthalmol 36(3): 239-242.
- Berezovsky A, Nilva Simeren BM, Steven N, Solange RS (2003) Standard full-field electroretinography in healthy preterm infants. Documenta Ophthalmologica 107: 243-249.
- Courage ML, Adams RJ (1990) Visual acuity assessment from birth to three years using the acuity card procedure: cross-sectional and longitudinal samples. Optom Vis Sci 67(9): 713-718.
- Yudcovitch L, Maeda J, Verma N (2004) An Evaluation of Infant Visual Acuity Using Lea Grating Paddles and Teller Acuity Cards. J Optom Vis Dev, pp. 35.
- Spierer A, Royzman Z, Kuint J (2004) Visual acuity in premature infants. Ophthalmologica 218(6): 397-401.
- Xiang Y, Erping L, Zhenzhen L, Xiaoyan L, Zhuoling L, et al. (2021) Study to establish visual acuity norms with Teller Acuity Cards II for infants from southern China. Eye 35(10): 2787-2792.
- Kohl P, Roled RD, Bedford AK, Samek M, Stern N (1986) Refractive error and preferential looking visual acuity in human infants: a pilot study. J Am Optom Assoc 57(4): 290-296.






























