Post-Traumatic Carotid-Cavernous Fistula: About A Case
Diagne JP, Gaye SS, Ka AM, Sy EM, Aw A, Diallo HM, Samra A, Mbaye S and Ndiaye PA
Ophthalmological Clinic Abass Ndao Hospital Center, Avenue Cheikh Anta Diop Dakar, Senegal
Submission: October 10, 2023; Published: November 14, 2023
*Corresponding author: Diagne JP, Ophthalmological Clinic Abass Ndao Hospital Center, Avenue Cheikh Anta Diop Dakar, Senegal
How to cite this article: Diagne JP, Gaye SS, Ka AM, Sy EM, Aw A, et al. Post-Traumatic Carotid-Cavernous Fistula: About A Case. JOJ Ophthalmol. 2023; 10(3): 555788. DOI: 10.19080/JOJO.2023.10.555788
Summary
Purpose: to show the clinical and paraclinical particularities of post-traumatic carotid-cavernous fistulas, through a case and to review the literature.
Observation: This was a 35-year- old patient , seen for a protrusion of the left eye (LE) and reduced visual acuity in both eyes. This symptomatology dates back 10 months after multiple trauma following a public road accident. Ophthalmological examination revealed corrected visual acuity limited to seeing hand movement in the right eye and 4/10 in the left eye. On the LE we noted exophthalmos lateralized outwards and downwards, reducible, pulsatile with murmur and dilated episcleral vessels in the head of a jellyfish. The ocular tone was normal in both eyes. Optic atrophy was noted as total on the right eye (RE) and partial on the LE. An orbito-cerebral CT angio -CT a few days after the trauma concluded to a carotid-cavernous fistula (CCF) and grade 3 left exophthalmos. The more recent angio-MRI confirms the CCF and the left exophthalmos. Faced with this table, the patient was referred to a neurosurgery department where monitoring was indicated because they did not have a raised table. With a follow-up of two months, the examination remains stationary.
Conclusion: CCF is a neurosurgical emergency that must be systematically considered when pulsatile exophthalmos appears following craniofacial trauma. Endovascular treatment is now a routine technique used in neuroradiology.
Keywords: Emergency; Internal Carotid; Cavernous Sinus; Fistula; Prognosis
Abbreviations: LE: left Eye; RE: Right Eye; CCF: Carotid-Cavernous Fistula
Introduction
Carotid-cavernous fistula (CCF) is a shunt abnormal arterio venous between the carotid system and the cavernous sinus. It can be spontaneous or post-traumatic. The traumatic form is described as a communication between the internal carotid in its intracavernous portion and the cavernous sinus resulting from a tear in the arterial wall. This is a diagnostic and therapeutic emergency that can be life-threatening and functional. The diagnosis is clinical and confirmed by imaging. Management must be multidisciplinary [1]. Our objective was to show the clinical and paraclinical particularities of post-traumatic CCF, through a case diagnosed in our department and to review the literature.
Observation
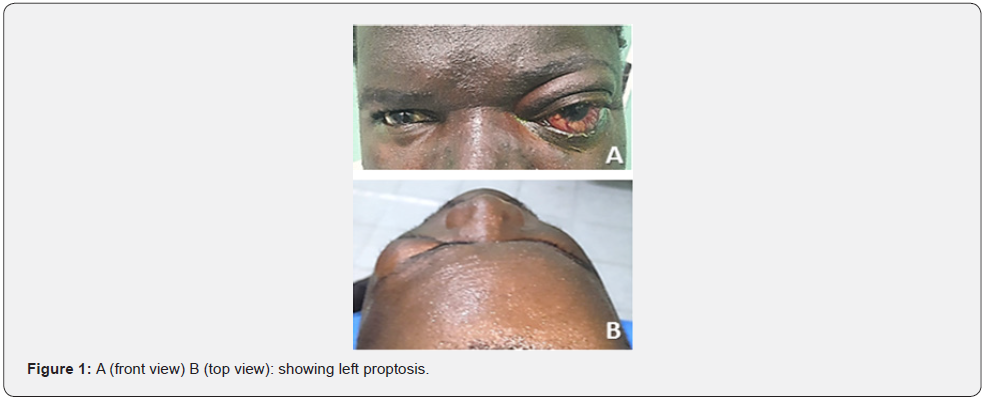
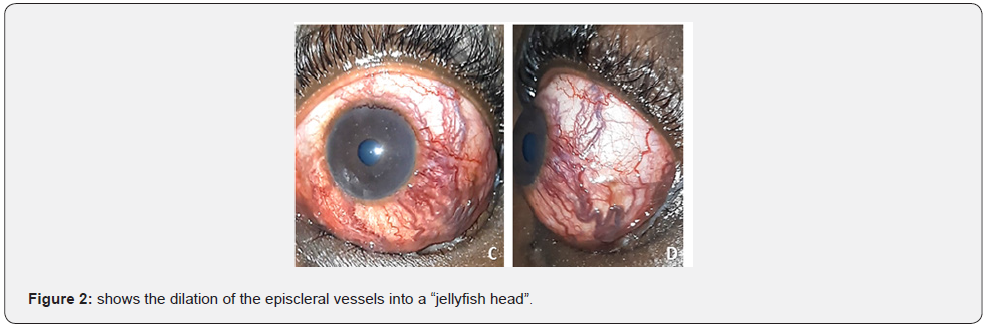
This was a 35-year- old patient , seen for a protrusion of the left eye (LE) and a reduction in visual acuity in both eyes, which had been ongoing for 10 months following a road accident. public causing polytrauma . Following the accident, the patient had initial loss of consciousness and multiple fractures (right arm) and left hemiparesis. These multiple lesions were treated in a trauma department. After vital stabilization, the patient was lost to follow-up. On admission, the ophthalmological examination found corrected visual acuity limited to seeing hand movement in the RE and 4/10 in the LE . We note at the LE a lateralized exophthalmos outwards and downwards, reducible, painless, pulsatile with murmur and dilated episcleral vessels in the head of a jellyfish (Figure 1 and 2). The ocular tone was normal in both eyes. Optical atrophy was noted, total in the RE and partial in the LE .
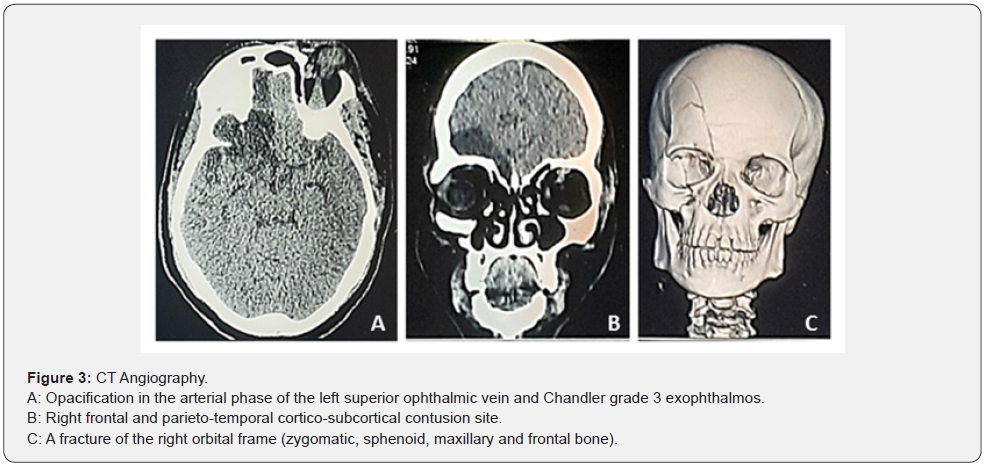
Angio- CT a few days after the trauma showed opacification in the arterial phase of the left superior ophthalmic vein and Chandler grade 3 exophthalmos, a fracture of the right orbital frame (zygomatic, sphenoid, maxillary and frontal bone). and a right frontal and parieto-temporal cortico-subcortical contusion focus (Figure 3). The more recent angio-MRI confirmed CCF and grade 3 exophthalmos on the left, the presence of two right frontoparietal proencephalic cavities measuring 40 x 70 mm and the white matter of the right semi-oval center measuring 39 x 10 mm, associated with peri-lesional gliosis , without mass effect on the median structures , sequelae of hemorrhage (Figure 4).

The diagnosis of CCF in the left eye and compressive optic neuropathy in the RE, post-traumatic, were retained. The patient was referred to a neurosurgery department where the indication for endovascular treatment of CCF was made. Given the low plateau and the patient’s lack of resources, they opted for monitoring. With a follow-up of two months, the examination remains stationary.
Discussion
The CCF direct (following craniofacial trauma or neurosurgical intervention) represents 70-90% of all FCCs [2]. They are most often high flow and classified type A according to Barrow [3]. There are indirect, spontaneous, low-flow forms occurring most often in young women. The latter develop on pre-existing lesions, congenital or acquired (hypertension, pregnancy, hereditary diseases of elastic tissue) [4]. Our patient was presented with type A post-traumatic FCC.
The diagnosis time varies from a few weeks to a few months depending on the symptoms . In the study carried out by Desal et al., the time for symptoms to appear was less than 15 days in 75% of cases. [5]. In our patient the diagnosis was early, but the patient was lost to follow-up.
The clinical picture may inconsistently associate signs related to orbital venous stasis, namely proptosis, dilation of the episcleral vessels, ocular hypertonia and papilledema [6]. Less suggestive signs can also be present: oculomotor paralysis which can be complete in 30% of cases or incomplete with a predominance of damage affecting the III, IV and VI [1] a Claude Bernard Horner syndrome is present in 4% of cases due to sympathetic plexus involvement, facial dysesthesia due to trigeminal involvement and in very rare cases a non-specific intracranial syndrome [7]. The symptomatology of direct forms is noisy unlike indirect forms which are progressive and chronic, explaining their often-late diagnosis [8]. Our case presented a noisy form. Optical atrophy in the right eye is believed to be due to post-traumatic orbital hematoma.
Direct forms occur in 0.2% of head trauma and in 4% if skull base fractures are associated [9]. They mainly affect young men; their number tends to decrease due to the wearing of seat belts and the generalization of airbags [10]. As in our case, young subject, male and following a public road accident leading to polytrauma with cranio-facial waiting and initial loss of consciousness. A case following ballistic head trauma is described [11].
The CT angiogram mainly shows indirect signs such as exophthalmos and dilation of the superior ophthalmic vein. But angio-MRI, thanks to the “time of flight” sequence, can objectify the CCF with a sensitivity of 83% and a specificity of 100% , by showing abnormal and early hyper flow in the cavernous sinus . According to certain authors, Angio-CT remains as reliable as Angio-MRI for the diagnosis of CCF [12]. The diagnosis was precise with these two examinations. Color Doppler ultrasound directly visualizes the fistula with a sensitivity of 95%. The definitive diagnosis is only made by bilateral internal external carotid angiography and remains the gold standard directly objectifying the fistula.
Current treatment of CCF is based on interventional neuroradiology. Its principle is based on the occlusion of the fistula by detachable intravascular balloons or metal turns (coils) while respecting the permeability of the carotid axis. The approach can be done by arterial route (lower and posterior fistula) or by retrograde venous route (upper and anterior fistula). Anticoagulant treatment with hypocoagulant aim with subcutaneous injection of heparin proves effective [13].
Spontaneous healing is exceptional, due to cavernous sinus thrombosis, and is observed in certain low-flow fistulas (5 to 10% of cases in the series by Debrun et al [14]. If left untreated, ophthalmologic complications may occur such as anterior or posterior ischemic optic neuropathy, glaucoma, venous or arterial occlusion, choroidal detachments or hematomas, and corneal complications related to proptosis. The vital prognosis can be compromised by the occurrence of subarachnoid hemorrhage, cerebral thrombophlebitis or an ischemic or hemorrhagic stroke related to posterior drainage [15]. Due to lack of resources, the neurosurgical team opted for surveillance.
Conclusion
Post-traumatic CCF is a neurosurgical emergency which must be systematically considered when faced with the appearance of pulsatile exophthalmos following craniofacial trauma. Cerebral arteriography is the test of certainty. Emergency endovascular embolization helps avoid the serious complications it could cause but remains a treatment available in our regions due to lack of technical support.
References
- Sellam M, Milazzo M, Deramond H (2005) Traumatic carotid-cavernous fistula. J.Fr. Ophthalmol 7(28): e1.
- Koenigsberg RA. Carotid cavernous fistula.
- Barrow DL, Spector RH, Bram IF, Londman JA, Tindall SC, et al. (1985) Classification and treatment of spontaneous carotid cavernous sinus fistula.J Neurosurg 62(2): 248-256.
- Levasseur F, Toussaint P, Milazzo S (1992) Ophthalmological manifestations of dural fistulas of the cavernous sinus. Bull soc opht France 10: 893-900.
- Graf CJ (1965) Spontaneous carotid cavernous fistula. Ehlers - Danlos syndrome and related syndrome and related conditions - Arch. Neurol 13(6): 662-672.
- Balayre S, Gicquel JJ, Merrie M, Dighiero P (2004) Orbital extension of a secondary sinus plasmacytoma transformed into multiple myeloma. J Fr Ophtalmo 27(1): 67-71.
- Fantin J (1968) Glaucoma and pulsatile exophthalmos - Nice Méd 65: 15.
- Bonnin N, Bacin F, Gabrillargues J, Chiam Barreta F (2013) Carotid-cavernous fistula: comparison of clinical and neuroradiological aspects pre and post embolization. J.Fr. Ophthalmol 36(10): 862-827.
- Liang W, Xiafeng Y, Weiguo L, Wusiq G (2007) About traumatic carotid cavernous fistula. J trauma 63: 1014-1020.
- Ellis JA, Goldstein H, Meyer PM, E Sander Connolly (2019) Carotid cavernous fistula. Neurosurg FO 32(5): E9.
- Aissa A, Arous A, Alouini R, Taktak J, Alloni M (2012) Ballistic trauma causing a carotid cavernous fistula. J Fr Ophthalmol 35(9): 722.e1-722.e4.
- Chen CC, Chang PC, Shy CG, Chen WS, Hao-Chun Hung (2005) CT Angiography and MR angiography in the evaluation of carotid cavernous sinus fistul prior to embolization: a comparison of technique. Am J. Neur radiol 26(9): 2349-2356.
- Moreau Gandy Vv, Lefournier V, Descour F, Bessou P, Vosdey A, et al. (2009) Dural carotid cavernous fistula: progression in therapeutic massage from 1989 to 2004, A report of ten cases. J.Fr Ophthalmol 32(6): 404-410.
- Debrun GM, Vinuela F, Fox AJ, Davis KR, Ahn HS (1988) Indications for treatment and classification of 132 carotid-cavernous fistulas. Neurosurgery 22(2): 285-289.
- Milbouw G et al. (1986) Head trauma, arteriovenous shunt, limit of brain CT scan. Neurochir 32: 254-257.






























