Severe Corynebacterium Keratitis Successfully Managed Medically: A Case Report and Review of Literature
Garima Satija*, Abhishek Dave, Arpan Gandhi, Manisha Acharya and Deepanshu Khanna
Dr Shroff’s Charity Eye Hospital, Kedarnath Lane, Daryaganj, New Delhi, Delhi, India
Submission: October 16, 2023; Published: November 02, 2023
*Corresponding author: Garima Satija, Dr Shroff’s Charity Eye Hospital, Kedarnath Lane, Daryaganj, New Delhi, Delhi, India
How to cite this article: Garima S, Abhishek D, Arpan G, Manisha A, Deepanshu K. Severe Corynebacterium Keratitis Successfully Managed Medically: A Case Report and Review of Literature. JOJ Ophthalmol. 2023; 10(3): 555787. DOI: 10.19080/JOJO.2023.10.555787
Abstract
Corynebacterium, which is a normal commensal of ocular flora is an uncommon cause of keratitis as compared to other forms of bacterial keratitis. We report a case of 59 years old North Indian male who presented to our hospital with complaints of pain, redness and diminution of vision in the right eye for the past 1 month. Right eye slit lamp bio microscopy examination showed near total full thickness corneal infiltrate, inferior descemetocele and 1mm hypopyon. Culture report of corneal scraping showed Corynebacterium. Patient was managed medically with topical antibiotics based on sensitivity report along with topical and oral steroids. The patient responded well to the treatment and healed completely with a macular grade central scar. Despite extensive corneal infiltrate which usually requires surgical intervention we could manage this case successfully with medical management.
Keywords: Corynebacterium; Keratitis
Introduction
Bacterial keratitis is a vision threatening ocular condition. The most common organisms include Staphylococci and Pseudomonas in the USA [1] while Streptococci pneumonia is the predominant organism in developing countries [2]. Corynebacterium which is the most commonly isolated bacteria from the ocular surface is an uncommon cause of ocular surface infections. Corynebacterium diphtheriae can directly penetrate an intact corneal epithelium and lead to conjunctivitis and keratitis. Corynebacterium accolens, C. jeikeium, CDC group G and Corynebacterium macginleyi are other Corynebacterium that can cause infections of the ocular surface [3]. Incidence of Corynebacterium keratitis reported in various studies is 0.3% [4], 1% [5] and 2.6% [2]. We report a case of severe Corynebacterium keratitis treated successfully with intensive medical management obviating the need for surgery.
Case Report
A 59-year-old North Indian male presented to Dr Shroff’s Charity Eye Hospital, New Delhi with complaints of pain, redness and diminution of vision in the right eye for the past 1 month. There was no previous history of ocular trauma or foreign body. There was no history of any systemic illness. At presentation patient was on topical treatment with eye drop natamycin (5%) hourly, eye drop atropine (1%) 3 times a day and tablet acyclovir (4oomg) 3 times a day. His best corrected visual acuity (BCVA) was hand movement close to face and 20/200 in the right and left eye respectively. Slit lamp biomicroscopy examination of the right eye showed congested and chemosed conjunctiva, near total full thickness corneal infiltrate with an overlying epithelial defect of 8 x 6 mm and an inferior descemetocele. Anterior chamber was formed and had a hypopyon of 1mm (Figure 1a).
The rest of the anterior and posterior segment could not be viewed. B scan ultrasonography showed normal lens echo, clear vitreous cavity and attached retina. Intraocular pressure was normal digitally. Left eye had a clear cornea and grade 2 nuclear sclerosis with a normal fundus. Lacrimal syringing was patent in both eyes. Random blood sugar was 110 mg%. Diagnostic corneal scraping of the right eye showed numerous pus cells and gram-positive rods on direct microscopy after gram staining. KOH mount revealed no organisms and appropriate culture medias were plated. The patient was started on treatment with topical moxifloxacin (0.5%) every hourly, fortified amikacin (2.5%) every hourly, homatropine hydrobromide (2%) thrice a day and tablet doxycycline (100mg) orally twice a day. A moderate growth of gram-positive rods with 'Chinese letter forms' was cultured and showed as small non-beta haemolytic colonies after 6 days of incubation on chocolate agar and blood agar plates. The biochemical characteristics of the organism were identified using in-house methods: reduced nitrate to nitrite, catalase positive, hydrolysed urea and failed to produce acid from glucose, sucrose, maltose, lactose, xylose, fructose and mannitol (Figure 2).
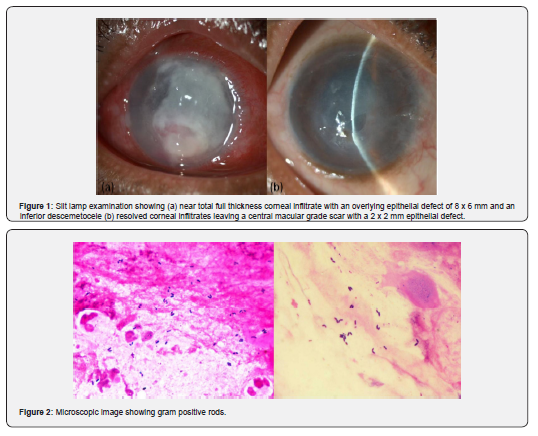
Culture depicted growth of Corynebacterium which was sensitive to the prescribed drugs. At one week follow-up the area of corneal infiltration decreased to 3x2 mm with surrounding edema. The hypopyon also reduced and the corneal clarity had improved. The conjunctival congestion and surface inflammation still persisted. Topical low dose steroid dexamethasone (0.05%) thrice a day was added, and topical antibiotics were reduced to 2 hourly dosing. Rest treatment was continued as previously. On subsequent follow up on 10th day corneal infiltrates almost resolved with a persistent epithelial defect of 6x6mm. The surface inflammation was much reduced. Intra ocular pressure was digitally low, and a micro leak was noted using fluorescien staining over inferior cornea overlying the area of descemetocele. A gentle B-scan ultrasonography showed 360-degree shallow choroidal detachment. A 14mm Acuvue Oasys bandage contact lens (BCL) was placed to seal the micro leak. Patient was started on oral tablet prednisolone 50 mg once daily day. After a week, the corneal infiltrates had resolved completely, leaving a central macular grade scar with a 2 x 2 mm epithelial defect (Figure 1b). The leak was also resolved and thus the BCL was removed. B scan ultrasonography revealed attached choroid and retina. Patient was continued on eye drop moxifloxacin (0.5%) 4 times a day and carboxy methyl cellulose (0.5%) 6 times a day. The epithelial defect eventually healed over 2 weeks. At three-month follow-up the BCVA was finger counting at 2 meters. Cornea showed a macular grade central scar with cataractous changes in lens and no recurrence of infection.
Discussion
We report a case of severe Corynebacterium keratitis which was resolved successfully with medical management. At presentation, the patient was on topical anti-fungal and oral anti-viral treatment but on diagnostic corneal scraping it showed gram positive rods on direct microscopy after gram staining. Initially because of the extensive corneal infiltration it seemed that the patient would need a therapeutic keratoplasty, but with a timely and accurate microbiological diagnosis we were able to achieve a favorable outcome for the patient.
Corynebacterium are straight or slightly curved rod-shaped bacteria which are gram-positive, non-motile, catalase positive and non-spore-forming. Their size varies from 2 to 6 mm in length and 0.5 mm in diameter. They are arranged in a characteristic 'palisades', 'V' or 'Chinese letters' pattern [6]. The most commonly isolated organisms in bacterial keratitis according to various studies include Staphylococcus epidermidis [2], Staphylococcus aureus, Streptococcus pneumoniae [4] and Pseudomonas aeruginosa [5]. Corynebacterium keratitis is an uncommon form of keratitis as compared to other forms of bacterial keratitis. Corneal infection occurs when there is a disruption of the normal defence mechanism. Under predisposing conditions such as trauma, contact lens or systemic infection the normal flora can also cause ocular infection.
Corynebacterium species which are one of the most commonly isolated bacteria from the normal ocular flora are also considered as non-pathogenic and can cause keratitis, conjunctivitis and endophthalmitis [7]. Corynebacterium species reported to cause keratitis include C. macginleyi, C. amycolatum, C. pseudodiphtheriticum, C. striatum, C. xerosis and C. propinquum [8]. In a study done by Das S et al on Corynebacterium spp as causative agents of microbial keratitis ocular predisposing factor was present in 63.6% eyes, trauma in 27.2% eyes and surgical intervention was required in 54.5% patients [7]. In our patient Corynebacterium keratitis occurred without any predisposing factor which is unusual as compared to the previous reports.
Corynebacterium are usually susceptible to a wide range of antibiotics such as fluoroquinolones, gentamicin, penicillin's, rifampicin and macrolides while 11 out of 16 C. macginleyi ophthalmic organisms showed fluoroquinolones resistance in a recent study from Japan [9]. In this case report also, Corynebacterium was sensitive to fluoroquinolone and aminoglycosides and responded well to the treatment.
Literature Search
We performed a PubMed search in May 2020 for English language results using following terms: Corynebacterium and keratitis.
Conclusion
Corynebacterium are normal commensal bacteria in conjunctival sac and thus it becomes difficult to assign a pathogenic role to the organisms in causation of ocular infections. This case demonstrates that Corynebacterium are capable of causing infectious keratitis and timely diagnosis and appropriate management can prevent surgical intervention even in severe cases.
References
- Lin A, Rhee MK, Akpek EK, G Amescua, M Farid, et al. (2019) Bacterial Keratitis Preferred Practice Pattern®. Ophthalmology 126(1): P1‐P55.
- M Jayahar Bharathi, R Ramakrishnan, R Meenakshi, S Padmavathy, C Shivakumar, et al. (2007) Microbial keratitis in South India: influence of risk factors, climate, and geographical variation. Ophthalmic Epidemiol 14(2): 61‐69.
- Riegel P, Ruimy R, Christen R, Monteil H (1996) Species identities and antimicrobial susceptibilities of corynebacteria isolated from various clinical sources. Eur J Clin Microbiol Infect Dis 15(8): 657‐662.
- Jayaraman K, Catti Muniswamy K, Pragya P, Christadas ANJ, Philip AT (2013) Spectrum of bacterial keratitis at a tertiary eye care centre in India. Biomed Res Int 2013: 181564.
- Schaefer F, Bruttin O, Zografos L, Guex-Crosier Y (2001) Bacterial keratitis: a prospective clinical and microbiological study. Br J Ophthalmol 85(7): 842‐847.
- Murphy JR (1996) Corynebacterium Diphtheriae. In: Baron S, editor. Medical Microbiology. 4th Galveston (TX): University of Texas Medical Branch at Galveston Chapter 32, USA.
- Das S, Rao AS, Sahu SK, Sharma S (2016) Corynebacterium spp as causative agents of microbial keratitis. Br J Ophthalmol 100(7): 939‐943.
- Daisuke T, Hiroshi E, Norihiro Y, Hirotake S, Ryuichi H, et al. (2015) Contact Lens-Related Infectious Keratitis with White Plaque Formation Caused by Corynebacterium propinquum. J Clin Microbiol 53(9): 3092‐3095.
- Kathryn LR, Christine MTK, Muthiah S, Prajna L, Nisha RA, et al. (2010) Corynebacterium macginleyi isolated from a corneal ulcer. Infect Dis Rep 2(1): e3.






























