Problem of Diagnosis and Management of Choroidal Hemangioma: About Two Cases
El Hadji Malick SY*, Aissatou AW, Aly Mbara KA, Jean Pierre Diagne, Soda Mbaye, Ousmane Ndiaga Senghor, Serigne Sohibou Gaye and Papa Amadou Ndiaye
Abass Ndao Hospital Eye Center, Cheikh Anta University of Dakar, Senegal
Submission: June 20, 2023; Published: July 15, 2023
*Corresponding author: El Hadji Malick SY, Abass Ndao Hospital Eye Center, Cheikh Anta University of Dakar, Senegal
How to cite this article: El Hadji Malick S, Aissatou A, Aly Mbara K, Jean Pierre D, Soda M. Problem of Diagnosis and Management of Choroidal Hemangioma: About Two Cases. JOJ Ophthalmol. 2023; 10(2): 555782. DOI: 10.19080/JOJO.2023.10.555782
Abstract
Introduction: Choroidal hemangiomas are the most common benign uveal vascular tumors. They are usually diagnosed at the complication stage. We report two atypical cases of choroidal hemangioma discovered on pathological examination.
Observation: These were two patients aged 50 and 49, respectively, with poorly monitored hypertension, whose left eye (LE) had been non-functional for a few years. One had consulted for a sudden decrease in visual acuity of the right eye (RE). Examination of this eye found visual acuity (VA) reduced to light perception, an annexal inflammatory syndrome, a normal ocular tone and a fundus showing a greyish choroidal mass at the posterior pole of about 5 papillary diameters with a lower choroidal lift. The other had consulted for pain associated with spontaneous left eye bleeding. On examination the visual acuity was reduced to a lack of light perception, a perforation with result of the ocular contents was noted. Orbit and cerebral imaging performed in them showed an intraocular tumor process with signs of malignancies. After multidisciplinary consultation, the exenteration of the eyes concerned was indicated and carried out. The pathological examination of the surgical parts was in favor of choroidal hemangioma.
Conclusion: Choroidal hemangiomas are rare benign tumors. They can be problematic in their management because they can mimic choroidal melanomas.
Keywords: Perforation; Neuroimaging; Exenteration; Hemangioma; Melanoma
Abbreviations: LE: Left Eye; RE: Right Eye; VA: Visual Acuity; CH: Choroidal Hemangioma; CCH: Circumscribed Choroidal Hemangioma; DCD: Diffuse Choroidal Hemangiom; CMM: Choroid Malignant Melanoma; LP: Light Perception; RD: Retinal Detachment; MRI: Magnetic Resonance Imaging; FA: Fluorescence Angiography; ICG: Indocyanine Green Angiography; PDT: Photodynamic Therapy
Introduction
Choroidal hemangioma (CH) is a choroidal tumor that occurs in two forms: circumscribed «circumscribed choroidal hemangioma (CCH)» or more rarely diffuse «diffuse choroidal hemangioma (DCD)». These choroidal tumors are both rare and very diverse, their diagnosis is complex and is generally limited to highly specialized centers [1]. CH can mimic other intraocular tumors in particular, choroid malignant melanoma (CMM), especially in its achromal form or in isolated metastasis [2]. The management of choroidal hemangioma has undergone considerable development in recent years [3]. The purpose of this work is to highlight the diagnostic and therapeutic aspects of choroidal hemangioma through two cases observed in our service.
Observations
Case 1
She was a 50-year-old woman who had been hypertensive for 10 years for a decrease in sudden visual acuity (VA) in her right eye that had been developing for 13 days. Examination of the right eye (RE) showed a distance visual acuity reduced to light perception (LP+), a stage 1 pterygium, hypothalamic, semi-mydriasis areflexic and cortical cataract. The ocular tone was 18 mm Hg and the fundus showed inferior retinal bleeding in the layer, dilation of the retinal vessels, a pearly white appearance and a discrete inferior temporal bulge associated with choroidal uplift of the entire lower retinal hemifield and massive detachment of the retina. The left eyeball had an absence of light perception with a phthisis eye and an inaccessible fundus. The cause of this monophtalmy has not been found. The locoregional examination (ENT, neurological) associated with that of the other organs was without particularity.
Mode B ocular ultrasound (Figure 1,2) showed on the right a single choroidal mass, temporo-inferior associated with a massive retinal detachment (RD) and on the left a vitreo-retinal rework with a total RD.
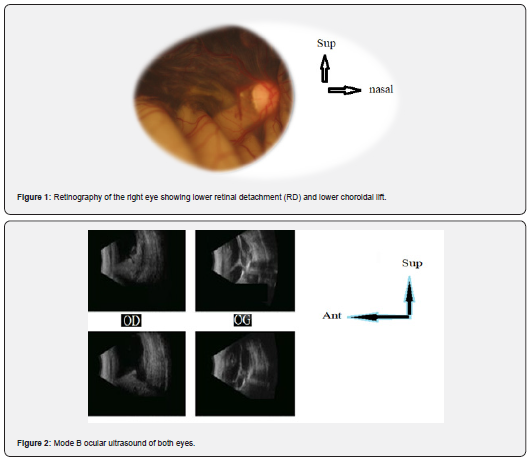
Magnetic resonance imaging (MRI) of the brain was performed without and with contrast injection at arterial and venous times (Figure 3). It showed an intracavitary mass in the right eye of about 1cm in diameter, with hyper-intense contours in T1 and iso-intense in T2 with contrast taking making suspect a choroidal or retinal tumor. Sclerotia, was healthy with no sign of invading intraconic and extraconic fat. In front of the strong suspicion of choroidal melanoma, we had achieved an extension balance that had returned normal. After a multidisciplinary consultation meeting, an enucleation of the right eye was indicated and carried out. Anatomopathological examination of the operating room indicated a circumscribed choroidal hemangioma (Figure 4). The surgical suites were simple, and an ocular prosthesis had been placed in the right eye.
Case 2
This is a 50-year-old, poorly monitored hypertensive patient whose left eye had been non-functional for 2 years with an unknown cause of monophtalmy. She was urgently recuperated for left ocular bleeding associated with pain and progressive redness within two days. On examination, the visual acuity on the left was reduced to a lack of light perception and there was a perforation of the globe resulting from spontaneous ocular contents (Figure 5). The examination of the right eye was without distinction. An emergency orbit and cerebral CT scan showed a left intraocular tumour with no secondary localizations (Figures 6,7). After a multidisciplinary consultation meeting, the exenteration of the left eye with eyelid preservation was indicated and carried out. Pathological examination of the operating room confirmed circumscribed choroidal hemangioma. The surgical suites were simple, and a prosthesis had been placed in our patient’s home.
Discussion
Circumscribed choroidal hemangioma is defined as a benign choroidal vascular tumor, orange red in colour and preferentially localized to the posterior pole [3]. It is a rare tumour whose prevalence is difficult to establish due to the existence of many asymptomatic cases, however it is estimated to be between 0.1 and 0.2 cases per 1 million population (Table 1) [4-6]. The rarity of this condition explains the importance of eliminating choroid melanoma, which is the most common primary ocular malignant lesion in the elderly person, 15 times more than CCH [3,7]. These are the first cases reported in our service. The diagnosis of a choroidal hemangioma is relatively easy in the context of Sturge-Weber syndrome, where a choroidal hemangioma must be systematically searched before a hemiface angioma. It is also less easy when the latter is isolated and circumscribed [8].
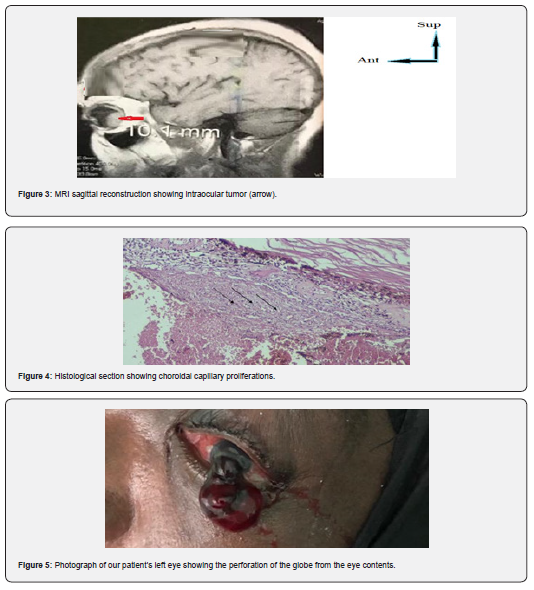
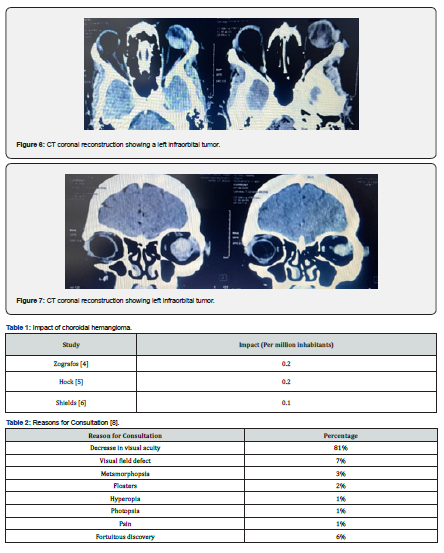
Usually asymptomatic, the signs begin to appear between the fourth and sixth decade. Decreased visual acuity is the main symptom (41%) associated with visual field amputation (7%) suggesting the occurrence of a complication of which the most common is retinal detachment (RD) [8] (Table 2). This detachment when it is formed, can often mask the choroidal mass at the fundus of the eye as was the case in our 1st case which presented at admission a massive RD. The location of the mass in our patient in the temporal quadrant and near the macular region was the most common topography found in the Krohn series [9] or 66% with an associated impairment of the upper hemisphere.
Before intraocular tumors, ocular ultrasound is of considerable contribution for the diagnosis. It allowed us in our first case to highlight the dome appearance of the choroidal mass, reflectivity and echogenicity similar to the choroid surrounding the tumor on the A-scan and B-scan. The hyperintense aspect in T1 and isointense in T2 with contrast enhancement of the endocavity mass found at our patient’s MRI, was also in favor of a choroidal tumor [8,10]. Fluorescence angiography (FA) and indocyanine green angiography (ICG) would play an important role in the diagnosis of choroidal hemangiomas in the absence of any complications [6,10]. In our patients, they could not be performed.
Verteporfin photodynamic therapy (PDT) and proton therapy have revolutionized the management of choroidal tumours. They are nowadays the conservative treatment of choice for symptomatic tumors because they are very radiosensitive tumors [4]. Their indication remains essentially focused on preserving visual functional structures, in the absence of major complications such as retinal detachment [3]. However, in our patients faced with the diagnostic delay and lack of certainty about the benign or malignant nature of the tumor, a radical treatment was indicated after a multidisciplinary consultation meeting. Radical treatment is indicated to preserve the vital prognosis to the detriment of functional prognosis in case of doubt. In our patients the pathological examinations of the surgical parts of our patients both came back in favor of an CH. This has also been reported in some series where about 5-10% of the eyes enucleated for a suspicion of choroidal melanoma were actually a CH [11,12]. Moreover, with the benign nature of the tumor found, the vital prognosis was not engaged in our patients. Aesthetically, patients received eye prosthesis and, clinically, regular follow-up without noted complications.
Conclusion
The discovery at the back of the eye of a choroidal mass is not uncommon however it is less easy to differentiate choroidal hemangioma from choroidal melanoma. The circumscribed choroidal hemangioma is a vascular tumor, benign, rare and mainly asymptomatic diagnosis mainly clinical confirmed by ultrasound and in the absence of posterior pole complication by fluorescence angiography (FA) and indocyanine green angiography (ICG). Its current treatment is essentially conservative with verteporfin photodynamic therapy (PDT) and proton therapy. Moreover, a problem in the choice of the best indication arises in case of diagnostic doubt. Its management must be multidisciplinary with close collaboration between general oncologists and specialists.
References
- Camila JM, Lorenzo D, Arias L, Catala-Mora J, Filloy A, et al. (2017) Tumeurs choroidiennes. Elsevier 17: 307-348.
- Campagnoli TR, Médine CA, Singh AD (2016) Choroidal melanoma initially treated as hemangioma: diagnostic and therapeutic considerations. Retin Cases Brief Rep 10(2): 175-182.
- Cassoux N, Desjardins L, Levy-Gabriel C, Lumbroso-Le Rouic L (2022) Oncologie oculaire, rapport Société Française d’Ophtalmologie. Elsevier, Paris, Pp. 433.
- Zografos L, Uffer S (2004) Tumors of the choroid. EMC Ophthalmology. Elsevier, pp. 39-61.
- Jarrett WH, Hagler WS, Larose JH, Boucliers JA (1976) Clinical experience with presumed hemangioma of the choroid: Radioactive phosphorus uptake studies as an aid in differential diagnosis. Trans Sect Ophthalmol Am Acad Ophthalmol Otolaryngol 81: 862-870.
- Shields CL, Shields JA, Nicol E, Geoffrey P, Sara E (1997) Survey of 520 uveal metastases. American Academy of Ophthalmology 104(8):1265-1276.
- Cassoux N (2015) Pronostic des mélanomes de la choroïde : nouveautés, Images en Ophtalmologie 9(1): 16.
- Mrittika S, Santosh GH (2019) Circumscribed choroidal hemangioma: an overview of clinical manifestation, diagnosis and management. Indian J Ophtalmol 67(12): 1965-1973.
- Krohn J, Rishi P, Froystein T, Singh AD (2019) Circumscribed choroidal haemangioma: clinical and topographical features. BJ Ophthalmol 103(10): 1448-52.
- Shields CL, Honavar SG, Shields JA, Carter J, Demerci H (2001) Circumscribed choroidal hemangioma: Clinical manifestations and factors predictive of visual outcome in 200 consecutive cases. American Academy of Ophthalmology 108(12): 2237-2248.
- Ferry AP (1964) Lesions mistaken for malignant melanoma of the posterior uvea. A clinicopathologic analysis of 100 cases with ophthalmoscopically visible lesions. Arch Ophthalmol 72(4): 463-469.
- Shields JA, Zimmerman LE (1973) Lesions simulating malignant melanoma of posterior uvea. Arch Ophthalmol 89(6): 466-471.






























