The Gray Frosted Branch Sign in Central Retinal Artery Occlusion
Fubin Wang*
Shanghai Bright Eye Hospital, 899 Maotai Road, Changning District, Shanghai 200336, Shanghai, China
Submission: June 07, 2023; Published: June 20, 2023
*Corresponding author: Fubin Wang, Shanghai Bright Eye Hospital, 899 Maotai Road, Changning District, Shanghai 200336, Shanghai, China
How to cite this article: Fubin W. The Gray Frosted Branch Sign in Central Retinal Artery Occlusion. JOJ Ophthalmol. 2023; 10(2): 555781. DOI: 10.19080/JOJO.2023.10.555781
Abstract
Aim: To describe a gray frosted branch sign in CRAO.
Methods: A 44-year-old male patient with no previous medical history first visited ophthalmologic department with amaurosis fugax for about one week and persistent visual impairment of left eye. The best corrected visual acuity showed that visual accuracy of the left eye was count fingers and the right eye was normal 1.0. The Pupillary light reflex test showed a relative afferent pupillary defect of the left eye. Based on the clinical presentation, CRAO was diagnosed in the left eye.
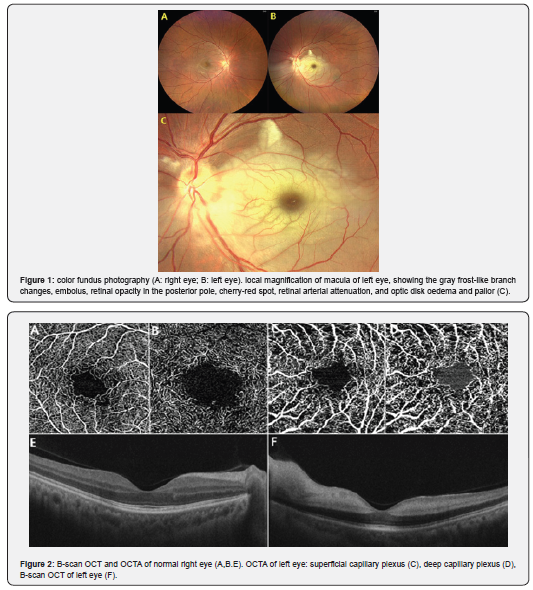
Results: The color fundus photography of the left eye showed the following results: retinal opacity in the posterior pole, cherry-red spot, retinal arterial attenuation, and optic disk oedema and pallor. The embolus was found. In the macular area especially, the gray frost-like branch changes appeared around the arterioles with irregular edges. Optical coherence tomography with B-scan in the macula showed the disorganized hyperreflective ischemic inner retinal layers and the inner retinal layers thickened with the hyporeflective outer retinal layers. OCT angiography images showed decreased vascular density and the disruption of the superficial and deep capillary plexus was noted with decreased vascular perfusion.
Conclusion: It is speculated that this gray frosted branch sign may be related to the paCFZ stress response during CRAO.
Keywords: Central Retinal Artery Occlusion; Gray Frosted Branch Sign; Periarterial Capillary-Free Zone; OCT; Color Fundus Photography
Abbreviations: CRAO: Central Retinal Artery Occlusion; CF: Count Fingers; BCVA: Best Corrected Visual Acuity; CFP: Color Fundus Photography; RAPD: Relative Afferent Pupillary Defect; OCTA: OCT Angiography; OCT: Optical Coherence Tomography; FBA: Frosted Branch Angiitis
Introduction
Central retinal artery occlusion (CRAO) has been known as a clinical entity since 1859, when von Graefe first described CRAO due to embolism. After that, Schweigger [in 1864 described it on ophthalmoscopy. It is an ophthalmic emergency because of instant, massive visual loss [1].
Here, a case of CRAO is reported which showed a novel image.
Case report
A 44-year-old male patient with no previous medical history first visited ophthalmologic department with amaurosis fugax for about one week and persistent visual impairment of left eye. The best corrected visual acuity (BCVA) showed that visual accuracy of the left eye was count fingers (CF) and the right eye was normal 1.0. The Pupillary light reflex test showed relative afferent pupillary defect (RAPD) of the left eye. Based on the clinical presentation, CRAO was diagnosed in the left eye. The color fundus photography (CFP) (Clarus 500, Carl Zeiss Meditec, Inc) of the left eye showed the following results: retinal opacity in the posterior pole, cherry-red spot, retinal arterial attenuation, and optic disk oedema and pallor. The embolus was found. In the macular area especially, the gray frost-like branch changes appeared around the arterioles with irregular edges. These gray frost-like branch changes appeared to correspond to the periarterial capillary-free zone(paCFZ) (Figure 1).
Optical coherence tomography (OCT) (Cirrus HD-OCT 5000, Carl Zeiss Meditec, Inc) with B-scan in the macula showed the disorganized hyperreflective ischemic inner retinal layers and the inner retinal layers was thickened with the hyporeflective outer retinal layers. OCT angiography (OCTA) was performed in macula and 3 × 3 and 6 × 6 mm images of central macular area were acquired. OCTA scans of the superficial and deep capillary plexuses were generated separately using the automated software algorithm. OCT angiography images showed decreased vascular density and the disruption of the superficial and deep capillary plexus was noted with decreased vascular perfusion. The superficial retinal plexus was more compromised. (Figure 2) Institutional review board approval and informed consent from patients was obtained.
Discussion
Central retinal artery occlusion (CRAO) is a rare but blinding disorder characterized by an obstruction of retinal blood flow that may be due to an embolus, thrombus, vasculitis, traumatic vessel wall damage or spasm [2]. The gray frost-like changes around the arterioles in CRAO are different from Frosted branch angiitis (FBA). Frosted branch angiitis is a relatively rare form of pan retinal perivasculitis, characterized by widespread, severe sheathing of the retinal vessels and mild to moderate anterior uveitis. Although initially described as affecting both arteries and veins, particularly in younger patients, it predominantly involves the veins [3,4]. Frosted branch angiitis is the clinical appearance of sheathing of retinal vessels, resembling frost on a tree branch [5]. The clinical presentation of frosted branch angiitis does not correlate with any single etiology. Rather FBA can be considered a clinical sign [6].
In this case, the gray frost-like change is due to CRAO. It is speculated that this change may be a compensatory response to the periarterial capillary-free zone. The periarterial capillary-free zone is an area of physiological vascularization surrounding the retinal arteries in which no efferent vessels emerge directly from the walls, and it was first identified by His in 1880 [7]. It is thought to develop during embryogenesis along human retinal arteries confined to the plane of the superficial plexus [8]. Therefore, it is speculated that this gray frosted branch sign may be related to the paCFZ stress response during CRAO. As the transmural oxygen diffusion from the retinal artery can meet the metabolic demands of the nearby cells, the need for vessels in this area is mitigated, and the paCFZ develops. The paCFZ may expand or converge in concert with changes in the retinal oxygen saturation in many retinal vascular disorders and is an important indirect index of the intravascular oxygen partial pressure [9,10].
References
- Sohan Singh Hayreh (2018) Central retinal artery occlusion. Indian J Ophthalmol 66(12): 1684-1694.
- Rita Serras-Pereira, Diogo Hipolito-Fernandes, Luísa Azevedo, Luísa Vieira (2020) Central retinal artery occlusion from Streptococcus gallolyticus endocarditis. BMJ Case Rep 13(9): e235763.
- Kleiner RC, Kaplan HJ, Shakin JL, Yannuzzi LA, Crosswell HH, et al. (1988) Acute frosted retinal peri phlebitis. Am J Ophthalmol 106(1): 27‐34.
- Ayliffe W (2002) Diagnosis and Treatment of Uveitis. (In: Stephen Foster C, Vitale AT, Eds.) Diagnosis and Treatment of Uveitis. WB Saunders Company, USA, pp. 827.
- Ito Y, Nakano M, Kyu N, Takeuchi M (1976) Frosted branch angiitis in a child. Jpn J Clin Ophthalmol 30: 797-803.
- Kristen Collistera, Sam S Dahra (2022) Frosted branch angiitis after smallpox vaccination. Am J Ophthalmol Case Rep 27: 101622.
- Wenyi Tang, Jingli Guo, Xiaonan Zhuang, Ting Zhang, Ling Wang, et al. (2021) Wide-Field Swept-Source Optical Coherence Tomography Angiography Analysis of the Periarterial Capillary-Free Zone in Branch Retinal Vein Occlusion. Transl Vis Sci Technol 10(2): 9.
- Hughes S, Yang H, Chan-Ling T (2000) Vascularization of the human fetal retina: roles of vasculogenesis and angiogenesis. Invest Ophthalmol Vis Sci 41(5): 1217-1228.
- Mase T, Ishibazawa A, Nagaoka T, Yokota H, Yoshida A (2016) Radial peripapillary capillary network visualized using wide-field montage optical coherence tomography angiography. Invest Ophthalmol Vis Sci 57(9): 504-510.
- Phelps DL (1990) Oxygen and developmental retinal capillary remodeling in the kitten. Invest Ophthalmol Vis Sci 31(10): 2194-2200.






























