Changes in Ocular Biometric Parameters During the Menstrual Cycle-A Prospective Study
Seema Dutt Bandhu1*, Harish Chander Bandhu2, Yukta3, Sahil Garg4 and Mohammad Hifz Ur Rahman5
1MD(Ophthalmology).Professor, Department of Ophthalmology, Manipal TATA Medical College, Manipal Academy of Higher Education, Manipal, India
2MD(Obs-Gyn). Professor, Department of Obs-Gyn, Manipal TATA Medical College, Manipal Academy of Higher Education, Manipal, India
3MBBS student, Punjab Institute of Medical Sciences, Jalandhar, Punjab, India
4MBBS student, Punjab Institute of Medical Sciences, Jalandhar, Punjab, India
5PhD, Assistant Professor, department of Community Medicine, Manipal TATA Medical College, Manipal Academy of Higher Education, Manipal, India
Submission: May 2, 2023;Published: May 08, 2023
*Corresponding author: Seema Dutt Bandhu, MD(Ophthalmology), Manipal TATA Medical college, Jamshedpur, Jharkhand, India
Research A. Changes in Ocular Biometric Parameters During the Menstrual Cycle-A Prospective Study. JOJ Ophthalmol. 2023; 9(5): 555775. DOI: 10.19080/JOJO.2023.09.555775
Abstract
Introduction: The cyclic hormonal changes have a significant biological influence on the female body. Plasma estrogen levels increase during ovulation, in the luteal phase of the menstrual cycle. Since Estrogen receptors have been found in various structures of the eye, they may impact the physiology and biometric parameters of the eye.
Materials and Methods: This was a prospective study conducted on a cohort of 25 female volunteers in the reproductive age group. Corneal thickness, Anterior chamber depth, lens thickness, IOP were measured on day 2/3, day 12/13 and day 23/24 of the menstrual cycle. The results were analysed statistically.
Results: Though there were minor variations in the readings of the biometric parameters, but Paired t-test performed on all the parameters showed that there was no significant difference by days of the menstrual cycle.
Discussion: Changes in the anterior segment parameters during the menstrual cycle are referred to in the literature. Some researchers claim that these variations are significant, while others advocate that these differences are inconsiderable. The results of our study show that the changes in the biometric parameters were insignificant.
Conclusions: The ocular biometric parameters including corneal thickness, AC depth, Lens thickness, Axial length and IOP did not vary significantly during the menstrual cycle.
Keywords: Biometry; Hormones; Ocular Parameters
Introduction
Menstruation is governed by changes in the levels of ovarian estrogen and progesterone, which produce varying responses in diverse tissues and organs. The cyclic hormonal changes have a significant biological influence on the female body, both physical and emotional [1]. Plasma estrogen levels increase during ovulation, in the luteal phase of the menstrual cycle. Estrogen receptors have been found in the retina, cornea, lens, iris, ciliary body, conjunctiva, lacrimal and meibomian glands of male and female eyes across a number of species including humans, rodents and rabbits [2,3]. The oestrogen levels may impact vision through its effects on the eye, from the ocular surface to the retina [4].
Biometric measurement is important in refractive surgery calculation, in intraocular lens selection, for spectacles or contact lens prescription, etc. Changes in the anterior segment parameters during the menstrual cycle are referred to in the literature. Some researchers have shown that these hormone fluctuations show correlation with the ocular tissue variables [5,6]. On the other hand, some researchers advocate that these fluctuations do not affect ocular variability significantly [7]. We conducted the present study to find out if the ocular biometric parameters are affected during the different phases of the menstrual cycle.
Materials and Methods
This was a prospective study conducted on a cohort of 25 female volunteers in the reproductive age group were enrolled for the study after taking clearance from the ethics committee. Those with irregular menstrual cycles, on oral contraceptives and pregnant females were excluded from the study. Those with a history of ocular surgery or trauma were also excluded from the study. The study participants were sub divided into two groups Group A included 13 females of the age group 15- 25 years and group B included 12 females who were > 25 years old. Six volunteers had to be excluded from the study, 2 because of unexpected menstrual irregularity and 4 because of dropping out of the study after 1 or 2 readings. After obtaining their written informed consent, all the participants underwent a comprehensive ophthalmologic examination. Corneal thickness, Anterior chamber depth, lens thickness, IOP were measured on day 2/3, day 12/13 and day 23/24 of the menstrual cycle.
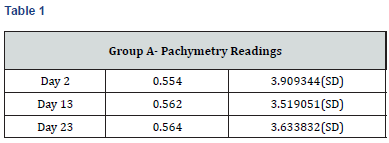
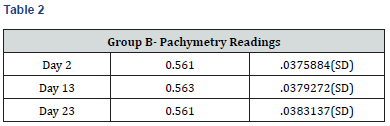
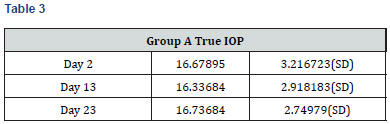
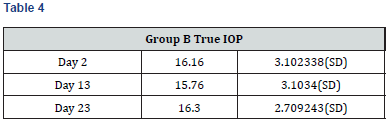
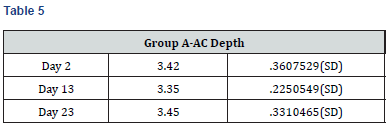
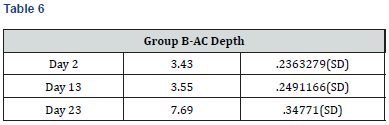
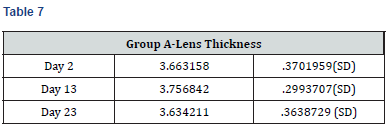
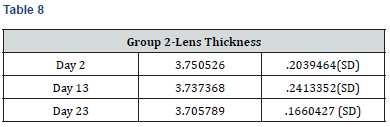
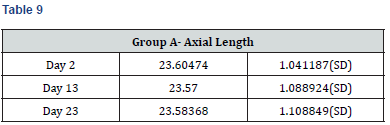
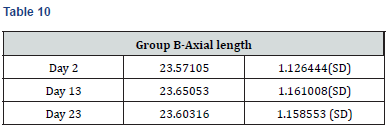
Results
Paired t-test performed on all the parameters shows that there was no significant difference in the biometric parameters by days of the menstrual cycle.
Discussion
Changes in the anterior segment parameters during the menstrual cycle are referred to in the literature. Some researchers claim that these variations are significant, while others advocate that these differences are inconsiderable. The results of the present study show that there were no significant changes in the thickness of the cornea during the different phases of the menstrual cycle. Giuffrè et al reported the cornea to be the thickest at the end of the cycle and thinnest at the beginning [8]. On the other hand, Hashemi et al investigated corneal thickness, corneal curvature, and ACD during the menstrual cycle using the Scheimpflug imaging technique found no significant difference in measurements during the menstrual cycle period [9]. Seymenoğlu, et al. determined corneal biometric properties during the menstrual cycle by using the ocular response analyzer reported that CCT was thickest at the end of the cycle and thinnest at the beginning [10]. In contrast to Goldich et al’s study, they could not find differences in corneal biomechanical properties and intraocular pressure during the menstrual cycle.
The results of the present study show that there were insignificant changes in the AC depth during the different phases of the menstrual cycle. In another study, CCT, AL, ACD, LT, and keratometric values were found to change during the menstrual cycle. Some measurements were highest at the beginning of the cycle (LT and keratometric values), some measurements were highest at the middle of the cycle (ACD), and other measurements were highest at the end of the cycle (CCT and AL). However, none of these changes was clinically or statistically significant [11]. Similar results were observed in the present study also.
The results of the present study also show that the changes in the IOP seen in the volunteers during the different phases of the menstrual cycle were insignificant as has also been reported by other studies. [10] Recent studies suggest that sex hormones, particularly estrogen, play a role in the pathogenesis of glaucoma and help explain the different distribution of this disease in the two sexes [12-14]. Growing evidence indicates that a lower estrogen level is associated with an increased risk of developing glaucoma [15-17]. From various in vitro studies, estrogens appear to exert a retinal neuroprotective action by promoting the survival of Retinal Ganglion Cells, preserving the RNFL [18] and contributing to the lowering of IOP [19].
The results of the study also show that the variations in the thickness of the lens and axial length during the different phases of the menstrual cycle were not significant as has also been reported by another researcher, but he has specifically concluded the findings for study conducted on Lenstar LS 900 and had commented in his study that some biometric measurement devices are affected by hormonal influences during the menstrual cycle [11].
Conclusions
The ocular biometric parameters including corneal thickness, AC depth, Lens thickness, Axial length and IOP did not vary significantly during the menstrual cycle.
References
- Farage MA, Neill S, MacLean AB (2009) Physiological changes associated with the menstrual cycle: a review. Obstet Gynecol Surv 64(1): 58-72.
- Wickam LA, Gao J, Toda I, Rocha EM, Ono M, et al. (2000) Identification of androgen, estrogen and progesterone receptor mRNAs in the eye. Acta Ophthalmologica Scandinavica 78(2): 146-153.
- Gupta PD, Johar K, Nagpal K, Vasavada AR (2005) Sex hormone receptors in the human eye. Survey of Ophthalmology 50(3): 274-285.
- Hutchinson CV, Walker JA, Davidson C (2014) Oestrogen, ocular function and low-level vision: a review, Journal of Endocrinology, 223(2): R9-R18.
- Versura P, Giannaccare G, Campos EC (2015) Sex-steroid imbalance in females and dry eye. Curr Eye Res 40(2): 162-175.
- Versura P, Fresina M, Campos EC (2007) Ocular surface changes over the menstrual cycle in women with and without dry eye. Gynecol Endocrinol 23(7): 385-390.
- Soni PS (1980) Effects of oral contraceptive steroids on the thickness of human cornea. Am J Optom Physiol Opt 57(11): 825-834.
- Giuffrè G, Di Rosa L, Fiorino F, Bubella DM, Lodato G (2007) Variations in central corneal thickness during the menstrual cycle in women. Cornea 26(2): 144-146.
- Hashemi H, Mehravaran S, Rezvan F (2010) Changes in corneal thickness, curvature, and anterior chamber depth during the menstrual cycle. Can J Ophthalmol 45(1): 67-70.
- Yakov Goldich, Yaniv Barkana, Eran Pras, Alexander Fish, Yossi Mandel, et al. (2011) Variations in corneal biomechanical parameters and central corneal thickness during the menstrual cycle. J Cataract Refract Surg 37(8): 1507-1511.
- Çakmak H, Taspinar A, Ozbagcivan M, Kocatürk T (2015) Ocular biometric characteristics during the menstrual cycle.Clinical Ophthalmology 9: 1177-1180.
- De Voogd S, Wolfs RCW, Jansonius NM, Uitterlinden AG, Pols HAP, et al. (2008) Estrogen receptors alpha and beta and the risk of open-angle glaucoma: The Rotterdam Study. Arch. Ophthalmol 126(1): 110-114.
- Mabuchi F, Sakurada Y, Kashiwagi K, Yamagata Z, Iijima H, et al. (2010) Estrogen receptor beta gene polymorphism and intraocular pressure elevation in female patients with primary open-angle glaucoma. Am. J. Ophthalmol 149(5): 826-830.
- Pasquale LR, Loomis SJ, Weinreb RN, Kang JH, Yaspan BL, et al. (2013) Estrogen pathway polymorphisms in relation to primary open angle glaucoma: An analysis accounting for gender from the United States. Mol Vis 19: 1471-1481.
- Feola AJ, Fu J, Allen R, Yang V, Campbell IC, et al. (2019) Menopause exacerbates visual dysfunction in experimental glaucoma. Exp. Eye Res 186: 107706.
- Lee AJ, Mitchell P, Rochtchina E, Healey PR (2003) Female reproductive factors and open angle glaucoma: The Blue Mountains Eye Study. Br J Ophthalmol 87(11): 1324-1328.
- Pasquale LR, Rosner BA, Hankinson SE, Kang JH (2007) Attributes of female reproductive aging and their relation to primary open-angle glaucoma: A prospective study. J Glaucoma 16(7): 598-605.
- Newman-Casey PA, Talwar N, Nan B, Musch DC, Pasquale LR, et al. (2014) The potential association between postmenopausal hormone use and primary open-angle glaucoma. JAMA Ophthalmol 132(2): 298-303.
- Tint NL, Alexander P, Tint KM, Vasileiadis GT, Yeung AM, et al. (2010) Hormone therapy and intraocular pressure in nonglaucomatous eyes. Menopause 17(1): 157-160.






























