Effects of Cataract Surgery on Patient’s Quality of Life
C Nanfack Ngoune1,2*, G Kagmeni1,3, AF Nomo1,2, Nzokou William4, C Donmgang Noche5 and Lucienne Assumpta Bella1,2
1Department of Ophthalmology, University of Yaounde I, Cameroon
2Ophthalmology Unit, Gyneco-Obstetric and Pediatric Hospital of Yaounde, Cameroon
3Yaounde University Teaching Hospital, Cameroon
4Ngaoundere regional Hospital, Cameroon
5Higher Institute of Health Sciences, Université des Montagnes, Cameroon
Submission: December 17, 2022;Published: January 10, 2023
*Corresponding author: Chantal Nanfack Ngoune, Department of Ophthalmology, Faculty of Medicine and Biomedical Sciences, University of Yaounde I, Cameroon
How to cite this article: C Nanfack Ngoune, G Kagmeni, AF Nomo, Nzokou William, C Donmgang N, et al. Effects of Cataract Surgery on Patient’s Quality of Life. JOJ Ophthalmol. 2023; 9(4): 555767. DOI: 10.19080/JOJO.2023.09.555767
Abstract
Background and Objective: Vision impairment caused by cataracts impacts patients’ daily activities, affecting their quality of life. This study aims to assess patients’ quality of life after cataract surgery using the National Eye Institute Visual Function Questionnaire-25 (NEI VFQ-25).
Method: Participants were patients who had undergone cataract surgery at Yaounde Gyneco-Obstetrics and Pediatrics Hospital (HGOPY) and Essos Medico-Surgical Center between September 1, 2018, and May 31, 2019. Participants were evaluated preoperatively, 14 days after cataract surgery, and one month after cataract surgery.
Results: A total of 93 patients were enrolled. Mean age was 68±12 years, ranging from 18 to 96 years old. The mean quality-of-life score varied significantly from 42.4%±21 in the preoperative period to 71.8% ±18.7 and 84.3% ±16 during evaluations at 14 days and one month postoperatively, respectively.
Conclusion: At the end of this study, it was evident that cataract surgery had a positive impact on patient quality of life. Therefore, assessment of patients’ quality of life should be considered an important element in the management and treatment of cataracts.
Keywords: Cataract surgery; Quality of life; NEI VFQ-25 questionnaire
Abbreviations: QOL: Quality of Life; VA: Visual Acuity; NEI-VFQ-25: National Eye Institute Visual Function Questionnaire; MSICS: Manual Small Incision Extra-Capsular Extraction
Introduction
Cataracts are the leading cause of blindness and low vision worldwide [1]. Visual deterioration due to cataracts negatively impacts patients’ daily activities and thus, their quality of life (QoL) [2]. QoL reflects an individual’s general well-being and ability to pursue life to its greatest fulfillment. QoL assessments in medicine evaluate how patients experience their disease and its treatments on a daily basis, providing clinicians with valuable indicators to guide patient care. Cataract treatment is surgical. It involves an extraction of the opaque crystalline lens, which is then replaced by an artificial lens, aiming to improve visual acuity (VA) and the patient QoL [2]. Cataract surgery has been the primary emphasis of QoL studies in ophthalmology. Many studies on QoL after cataract surgery have been undertaken worldwide and have found that this procedure benefits patients through visual function and QoL improvement as well as reduction of psychological distress [3-6]. The scales used to assess QoL after cataract surgery vary. For this study, we used the National Eye Institute Visual Function Questionnaire (NEI-VFQ-25) [3,7]. The aim of our study was to evaluate patient QoL after cataract surgery in Cameroonians.
Methods
This study included all consecutive patients who underwent cataract surgery at Yaounde Gyneco Obstetric and Pediatric Hospital and Essos Medico-Surgical Center between September 1, 2018 and May 31, 2019. This study was conducted in accordance with the principles presented in the Declaration of Helsinki. Written informed consent was obtained from all participants or their legal representative. The protocol was approved by the Research Ethics Committee of the HGOPY (Nr:834/CIERSH/DM/2019). All participants were invited to complete a questionnaire both preoperatively (before the installation of mydriatic drops), 14 days after cataract surgery, and one month after cataract surgery. Inclusion criteria involved adult patients with age-related cataracts without any other ocular comorbidity. Participants with cognitive impairment and those who have undergone previous cataract surgery within the past eight weeks were excluded from the study. Cognitive assessment was measured using the fouritem Abbreviated Mental Test as described by Svain DG et al. [8].
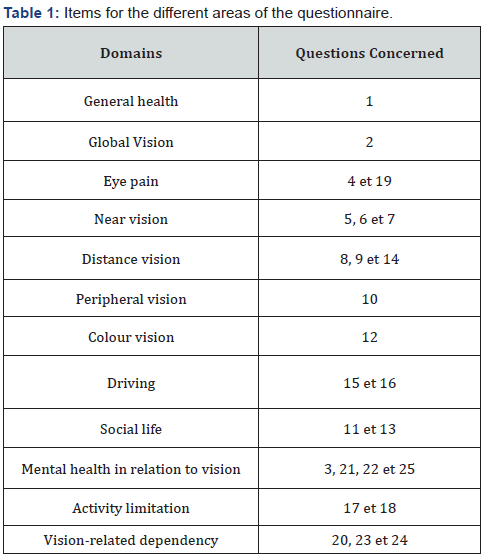
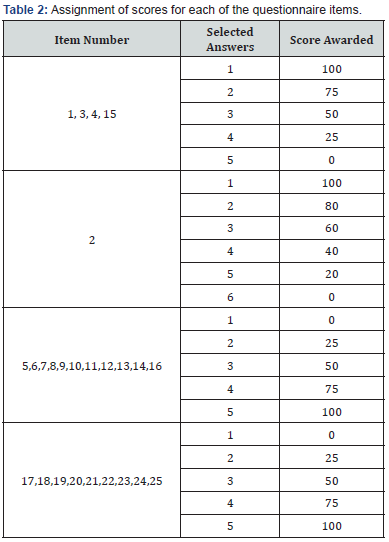
Participants with a cognitive score of <4 were excluded from the study. Analyzed parameters included socio-demographic data (i.e., age, gender, education level, and occupation) and clinical data (i.e., preoperative VA, postoperative VA, surgical technique, and surgical complications). Ocular and medical comorbidity, as well as the surgical status of the fellow eye, were also analyzed. The French version of the NEI VFQ-25 was used to evaluate QoL in our study. NEI VFQ-25 is designed as a 25-item questionnaire in which patients subjectively evaluate their ability to perform visually demanding tasks in daily life. Domains and corresponding questions are summarized in table 1. Assignment of scores for each of the questionnaire items are shown in table 2. The domain score was obtained by dividing the sum of the scores for each item by the domain and number of items.
Statistical Analysis
Qualitative variables were reported as a percentage. Quantitative variables were reported by mean ± standard deviation. Patient test results were used to compare the mean. P-values less than 0.05 were considered statistically significant.
Results
We included 93 patients who met our selection criteria, for a total of 98 eyes. Our subject pool was 50.5% male. The mean age was 68±12 years, ranging from 18 to 96 years of age. The most represented age group was over the age of 60 (80.6%). Sixty patients (64.51%) were unemployed, 10 (10.75%) had undergone cataract surgery on the contralateral eye, 23 (24.73%) were hypertensive, and five (5.37%) were both hypertensive and diabetic. Manual small incision extra-capsular extraction (MSICS) was performed on 78 patients (83.9%), and phacoemulsification was performed on 15 patients (16.1%). Preoperative corrected distance VA was less than a tenth in 65 cases (69.89%). Preoperative corrected near VA was less than Parinaud 8 in 84.9%. A progressive improvement in VA was noted in the postoperative period. Operative complications included seven posterior capsule ruptures (7.52%) and eight cornea edemas (8.6%). Data on QoL scores are summarized in table 3.
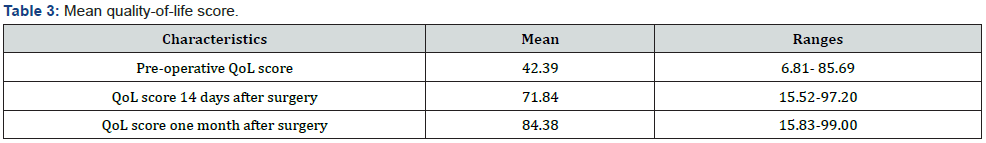
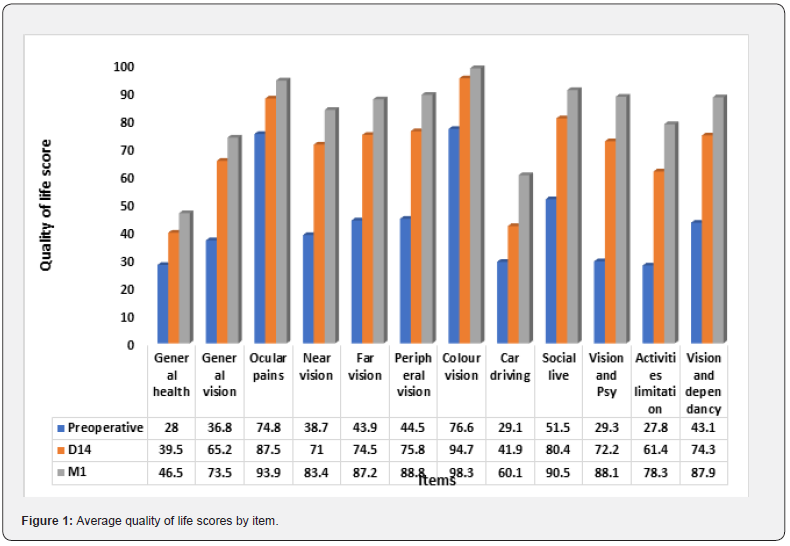
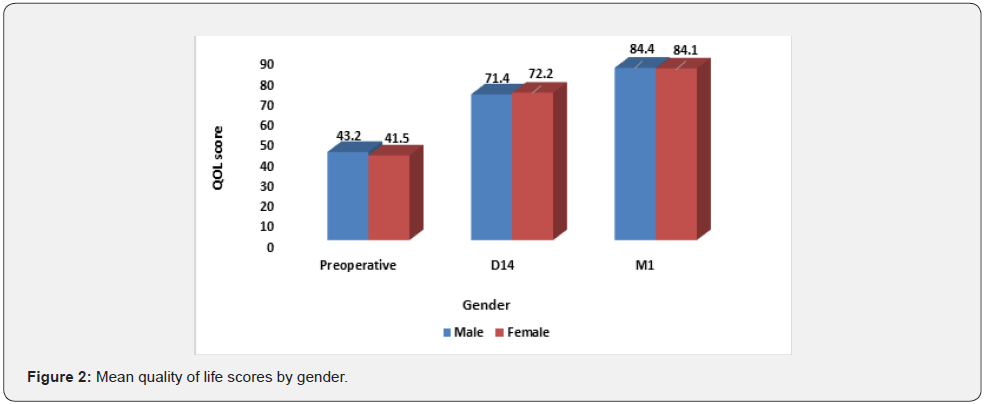
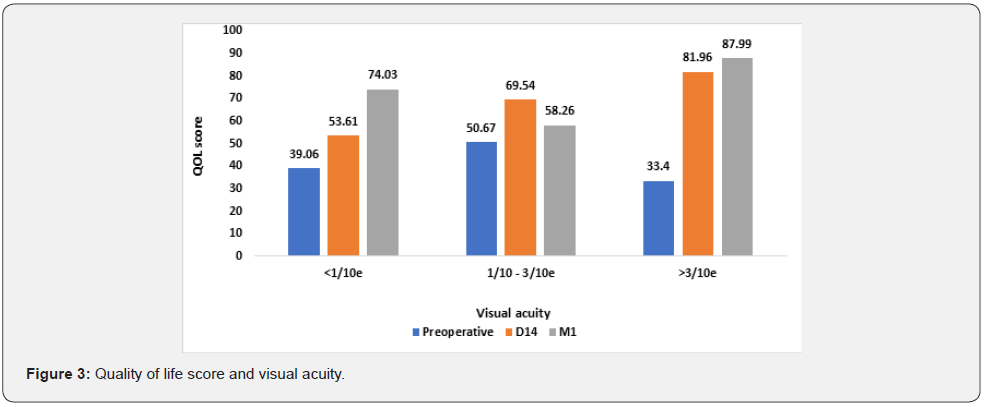
The mean QoL score increased significantly from 42.39% preoperatively to 71.84% at 14 days postoperatively (P<0.001) and to 84.38% at one month postoperatively (p<0.001). There was progressive improvement in all 12 questionnaire items representing the different domains of patient life (Figure 1). When comparing mean quality of life scores by gender, we observed no statistically significant difference (p˃0.699) prior to and after the surgery, as shown in figure 2. All age groups experienced a progressive improvement in quality of life over time. Notably, patients under 60 years of age had a higher quality of life than the elderly at any time period. This difference was not statistically significant postoperatively (p=0,2806). Preoperative quality of life was highest in patients with the best corrected VA between 1/10th and 3/10th. This score improved 14 days after surgery, regardless of visual acuity. One month after surgery, this score was still higher in patients with visual acuity less than 1/10th and greater than 3/10th, as shown in figure 3.
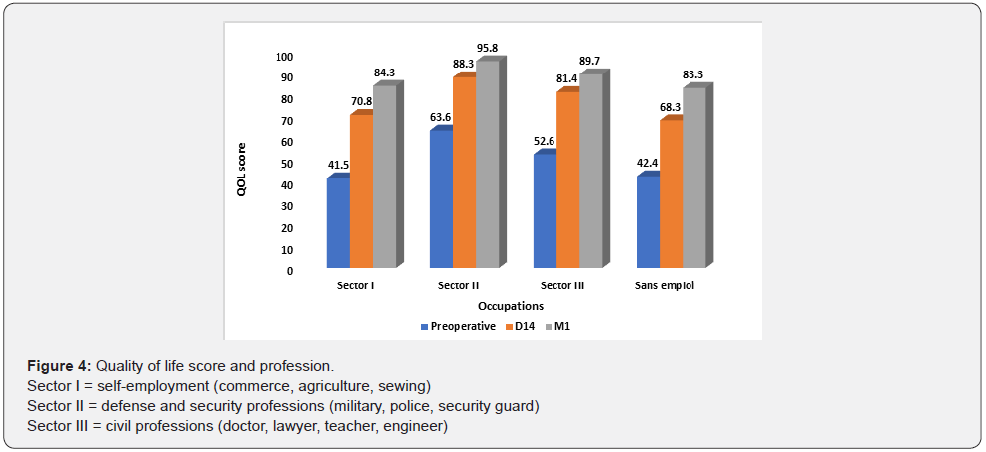
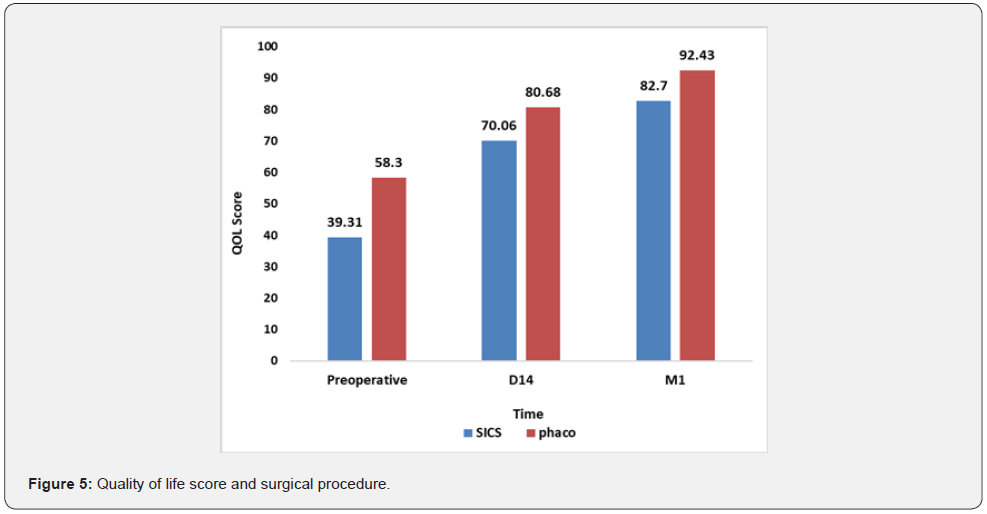
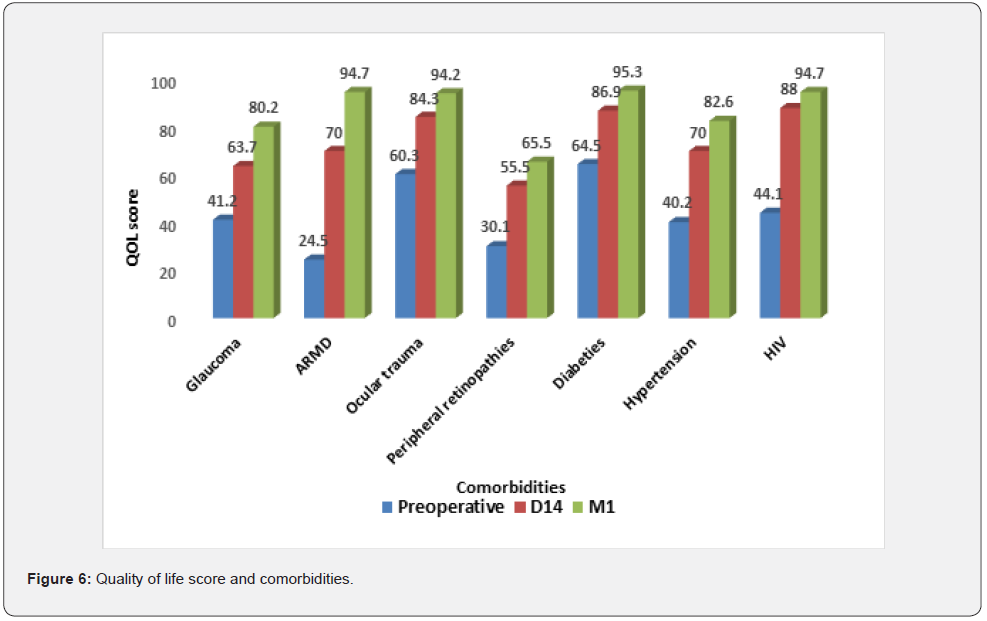
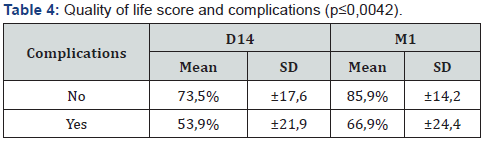
Workers in sectors II and III had the highest mean scores at M1 of 95.8% and 89.7%, respectively. This is in contrast to the unemployed, who had the lowest score (83.3%), with the difference not being statistically significant (p≥0.1815). It should be noted that regardless of occupation, QoL improved postoperatively. Postoperative QoL scores were significantly higher in patients who underwent phacoemulsification compared to Manual small incision cataract surgery (p≤0.0437). Postoperative QoL was higher in patients who had no complications, with the difference being statistically significant, as shown in table 4. We noted an improvement in patients’ QoL postoperatively despite comorbidities, the difference being statistically significant (p≤0.006) (Figure 4-6).
Discussion
A significant change in cataract patients’ daily activities and vision related QoL has been reported after modern cataract surgery. The French version of the NEI VFQ-25 was used to evaluate QoL in our study. The Visual Function Index‐14 (VF‐14) has been used in several other studies to evaluate QoL after cataract surgery [9]. We enrolled 93 patients, 50.5% of whom were men. The mean age was 68±12 years. The predominant age group (60 years and over) could be explained by the age-related cataract that is the most common in said age group [10]. In addition to cataracts, the elderly has other comorbidities, both ophthalmological (e.g., AMD, glaucoma) and general (e.g., hypertension, diabetes), which contribute to the deterioration of their QoL [11,12]. Cataract surgery in these patients would undeniably have a positive impact on their QoL [13]. In our series, about 70% of the patients were optically blind with a preoperative corrected distance VA of less than a tenth. 85% had a corrected near VA of less than Parinaud 8. This shows that the majority of patients were consulted when the cataract was in its advanced stages. The reasons for this delay in treatment include fear of surgery and poverty, but the insufficiency of qualified personnel for cataract surgery in sub- Saharan Africa is also a contributing factor.
MSICS was widely performed on our patients. This wide use of MSICS is related to the limited financial means of the patients, the high cost of phacoemulsification, and the lack of personnel qualified to administer phacoemulsification [14]. Surgical techniques used for cataract treatment have been improved over the years to reduce the risk of surgical complications. The main intraoperative complication in our research was posterior capsule rupture in 8% of patients. Guzek JP et al. [15] in Ghana reported 3% posterior capsule ruptures [15]. The main postoperative complication was corneal edemas in 8.6% of patients, as was reported in other African studies [15,16]. Corneal edema is most often caused by manipulations in the anterior chamber and especially by manual removal of the lens nucleus. These maneuvers can damage the corneal endothelium and lead to corneal edema.
In our study, we found that the mean QoL score improved over time, with a higher value at one month postoperatively. This improvement may be due to the regression of psychological and clinical signs over time and certain complications related to cataracts and surgery. The mean QoL score found in the present study is higher than that of Ka et al. [17], who reported a mean score at one month of 73.9%. However, Ni et al. [18] reported a mean score of 94.3% at one-month post operatively. This difference could be explained by the surgical techniques that were implemented. We used two techniques: small incision manual surgery and phacoemulsification. Ka et al. [17] only used conventional manual surgery for all their patients [17], while Ni et al. [18] only used phacoemulsification [18]. In the current study, the majority of items concerning the different domains of the patient’s life have improved over time, with mean QoL scores between 73% and 99% and considered satisfactory. Contrary to this, the item of general health had a final mean score of 46.5%.
This score can be explained by the advanced age of the cataract patients and the number of patients that have a history of comorbidities in this domain.
Chandrasekaran et al. did not identify a significant impact of cataract surgery on long-term changes in self-rated health. However, they found a positive impact of cataract surgery on the mental health domain and the mental component score of the short form -36 (SF- 36) health-related quality of life (HRQOL) [4], as we did in the present study with a different questionnaire. In the Blue Mountain eye study population, Chia et al. found that the mental domains were more largely affected by visual impairment than the physical domains [19,20] and that the impact of visual impairment on the mental domain was greater than that of many other medical conditions [19]. The amelioration of mental health was more than double in patients who had second eye cataract surgery compared to those who had only first eye surgery [4]. We observed that car driving scores improved from 29.1% to 60.1%. In fact, Talbot and Perkins reported an increase in older people satisfying driving license requirements from 52 to 86% after second eye surgery [21]. The improvement in daily life activities ameliorates social interactions and, thus, QoL.
The QoL of men did not differ from that of women either preoperatively or postoperatively. Similar results have also been reported by other authors despite a predominance of women in their samples [22,23]. Thus, it appears that the QoL of cataract patients is not influenced by gender. We observed a higher QoL score in younger subjects but a greater QoL improvement in older subjects. These findings were comparable to those of Lum et al. [24]. Factors that could be identified as responsible for such results were mainly related to the physiological aging of the visual system, with age and the higher prevalence of comorbidities found in elderly subjects [25].
As previously reported by OU et al. [26], we also found that patients with an occupation requiring optimal vision had a higher QoL score compared to those without a job. Indeed, due to the decrease in Income, the financial management of morbidities and the cost of cataract surgery become factors in the impairment of QoL. Patients who had a significant increase in corrected near and far vision had a higher QoL score, with a mean score at one month of 80.9%. The improvement of the visual function allowed patients to better perform their daily activities. They were more independent and had a lower risk of falling. VA, while having a positive influence on QoL, remains a necessary but not sufficient measure of QoL.
Other factors, such as peripheral vision, contrast vision, color vision, and glare sensitivity, should also be considered. Patients who underwent phacoemulsification had, postoperatively, higher QoL scores compared to those who underwent small manual incision surgery. These results could be explained by the small sample size, especially of the phacoemulsified patients, and the short postoperative follow-up. However, Chan et al. [23] did not find a significant difference in QoL scores between phacoemulsification and small manual incision assessed at a fourmonth follow-up evaluation. Other authors reported that although phacoemulsification offered a faster functional rehabilitation than the small manual incision, the final results of these two techniques were comparable [27].
Intra- and postoperative complications are responsible for visual discomfort and delayed rehabilitation. Therefore, they unquestionably have a negative impact on patient QoL. In our study, we found that QoL improved in patients with comorbidities after cataract surgery; however, their QoL was still lower than that of patients without comorbidities. Similar findings have already been reported in the literature [17]. Comorbidities have a negative influence on the QoL of cataract patients. The limitations of this study are the short duration of the follow-up because, at onemonth, postoperative care is not completed. This analysis should be done beyond three months. Additionally, the questionnaire should also be adapted to our environment.
Conclusion
The preoperative QoL of the patients was poor because of their cataracts. QoL improved considerably and progressively after surgery. Younger age, surgical technique, and postoperative visual acuity were found to be associated with a greater QoL. We suggest systematically integrating QoL evaluation in the followup of the cataract patients with a questionnaire adapted to the Cameroonian context.
References
- WHO | Cataract. WHO (2015).
- Erik J Groessl, Lin Liu, Marisa Sklar, Steven R Tally, Robert M Kaplan, et al. (2013) Measuring the Impact of Cataract Surgery on Generic and Vision-Specific Quality of Life. Qual Life Res 22(6): 1405-1414.
- JG Walker, KJ Anstey, MP Hennessy, SR Lord, C von Sanden (2006) The impact of cataract surgery on visual functioning, vision-related disability and psychological distress: a randomized controlled trial. Clinical and Experimental Ophthalmology 34(8): 734-742.
- S Chandrasekaran, JJ Wang, E Rochtchina, P Mitchell (2008) Change in health-related quality of life after cataract surgery in a population-based sample. Eye 22(4): 479-484.
- JL Helbostad, M Oedegaard, SE Lamb, K Delbaere, SR Lord, et al. (2013) Change in vision, visual disability, and health after cataract surgery. Optometry and Vision Science 90(4): 392-399.
- LB Meuleners, D Hendrie, ML Fraser, JQ Ng, N Morlet (2013) The impact of first eye cataract surgery on mental health contacts for depression and/or anxiety: a populationbased study using linked data. Acta Ophthalmologica 91(6): e445-e449.
- CM Mangione, PP Lee, PR Gutierrez, K Spritzer, S Berry, et al. (2001) Development of the 25-list-item national eye Institute visual function questionnaire. Archives of Ophthalmology 119(7): 1050-1058.
- Swain DG, O'Brien AG, Nightingale PG (1999) Cognitive assessment in elderly patients admitted to hospital: the relationship between the shortened version of the abbreviated mental test and the abbreviated mental test and mini-mental state examination. Clin Rehabil 13(6): 508-510.
- Vijaya K Gothwal, Thomas A Wright, Ecosse L Lamoureux, Konrad Pesudovs (2010) Measuring outcomes of cataract surgery using the Visual Function Index-14. J Cataract Refract Surg 36(7): 1181-1188.
- Dohvoma V, Ndongo J, Ebana MS, Mvilongo TC, Nguena M, et al. (2018) Résultats Fonctionnels de la Chirurgie de la Cataracte à l’Hôpital Central de Yaoundé par la Technique de la Petite Incision Manuelle. Health Sci. Dis 19(4): 27-30.
- Gineys R, Rohart C, Chaine G (2008) Caractéristiques socio-économiques, oculaires et systémiques des patients opérés de cataracte : particularités d’une population suburbaine en situation de précarité et mode de prise en charge en centre hospitalo-universitaire. JFO 31(1): 56-61.
- Klein BE, Klein R, Lee KE (1998) Diabetes, cardiovascular disease, selected cardiovascular risk factors and the 5-year incidence of age-related cataract and progression of lens opacities: The Beaver Dam Eye Study. Am J Ophthalmology 126(6): 782-790.
- Mozaffarieh M, Krepler K, Heinzl H, Sacu S, Wedrich A (2004) Visual Function, Quality of Life and Patient Satisfaction after Ophthalmic Surgery: A Comparative Study. Ophthalmologica 218(1): 26-30.
- Javed U, Veigh MK, Scott NW, Azuara AB (2015) Cataract extraction and patient vision related quality of life: a cohort study. Eye 29(7): 921-925.
- Guzek JP, Ching A (2003) Small-incision manual extracapsular cataract surgery in Ghana, West Africa. J Cataract Refract Surg 29(1): 57-64.
- Javaloy J, Signes-Soler I, Moya T, Litila S (2021) Cataract surgery in surgical camps: outcomes in a rural area of Cameroon. Int Ophthalmol 41(1): 283-292.
- Ka AM, Sow AS, Diagne JP, Ndoye Roth PA, Kamara K, et al. (2017)Patients' quality of life after cataract surgery. J Fr Ophtalmol 40(8): 629-635.
- Ni W, Li X, Hou Z, Zhang H, W Wang, et al. (2015) Impact of cataract surgery on vision related life performances: the usefulness of Real-Life Vision Test for cataract surgery outcomes evaluation. Eye 29(12): 1545-1554.
- Chia EM, Wang JJ, Rochtchina E, Smith W, Cumming RG, et al. (2004) Impact of bilateral visual impairment on health-related quality of life: The Blue Mountains Eye Study. Invest Ophthalmol Vis Sci 45(1): 71-76.
- Chia EM, Mitchell P, Rochtchina E, Foran S, Wang JJ (2003) Unilateral visual impairment and health related quality of life: The Blue Mountains Eye Study. Br J Ophthalmol 87(4): 392-395.
- Talbot EM, Perkins A (1998) The benefit of second eye cataract surgery. Eye 12(Part 6): 983-989.
- Lau J, Michon JJ, Chan WS, Ellwein LB (2002) Visual acuity and quality of life outcomes in cataract surgery patients in Hong Kong. Br J Ophthalmol 86(1):12-17.
- Chan CWN, Wong CCJ, Chan SKK, Wong WK, Tam CKK, et al. (2003) Evaluation of quality of life in patients with cataract in Hong Kong. J Cataract Refract Surg 29(9):1753-1760.
- F Lum , O Schein, AP Schachat, RL Abbott, HD Hoskins, et al. (2000) Initial two years of experience with the AAO National Eyecare Outcomes Network (NEON) cataract surgery database. Ophthalmology 107(4): 691-697.
- Lundström M, Stenevi U, Thorburn W (2000) Cataract surgery in the very elderly. J Cataract Refract Surg 26(3): 408-414.
- Ou F, Li K, Gao K, Liu D, Li J, et al. (2012) An urban neo-poverty population-based quality of life and related social characteristic investigations from Northeast China. Plos One 7(6): e38861.
- Oliver JE, Thulasiraj RD, Rhamathullah R, Baburajan (1998) Vision-specific function and quality of life after cataract extraction in South India. J Cataract Refract Surg 24(2): 222-229.






























