Oral Ivermectin for the Treatment of Rosacea-Associated Blepharitis: Case Report
Aleksandra L Lindgren1, Kathleen M Welsh2 and Andrea Hui Austin2,3*
1University of Queensland, Ochsner Clinical School, USA
2Bay Area Cosmetic Dermatology, USA
3Department of Dermatology, State University of New York Downstate Medical Center, USA
Submission: June 26, 2022;Published: July 15, 2022
*Corresponding author: Andrea Hui Austin, Bay Area Cosmetic Dermatology, 2299 Post St., #312, San Francisco, CA 94115, USA
How to cite this article: Aleksandra L L, Kathleen M W, Andrea Hui A. Oral Ivermectin for the Treatment of Rosacea-Associated Blepharitis: Case Report. JOJ Ophthalmol. 2022; 9(2): 555759. DOI: 10.19080/JOJO.2022.09.555759
Abstract
Blepharitis is an inflammatory condition of the eyelids managed by primary care providers, ophthalmologists, and dermatologists. It can be associated with allergies, infections, seborrheic dermatitis, rosacea, eczema, and psoriasis. In both cutaneous and ocular rosacea, overgrowth of Demodex has been implicated as a causative factor. We present a case of recalcitrant rosacea-associated blepharitis treated successfully with oral ivermectin. Oral ivermectin can be an advantageous option for rosacea-associated blepharitis resistant to other treatment options due to its targeted action, once-a-day dosing and minimal adverse effects.
Keywords: Ivermectin; Rosacea; Blepharitis
Introduction
Rosacea is a chronic, inflammatory skin disease that manifests as erythema, pustules, telangiectasias, and flushing of the face [1]. It is more common in women and fair-skinned persons but can affect all demographics [1]. Rosacea is divided into erythematotelangiectatic, papulopustular, rhinophymatous, and ocular subtypes, but exact classification is complicated by progression of one subtype to another or multiple subtypes presenting simultaneously [1,2]. Cutaneous rosacea management is multifaceted and includes gentle skincare, lifestyle changes, vascular laser treatments, topical medications, and oral medications [1,3].
Ocular rosacea is estimated to occur in 50% or more of patients with diagnosed cutaneous rosacea and limited studies indicate ocular manifestations are seen before cutaneous symptoms in 20% of rosacea patients [2,3]. Ocular rosacea is thought to be underdiagnosed so exact prevalence is unknown [2,3]. It has varied presentations and can be difficult to distinguish from other eye pathologies. Mild ocular rosacea can present with keratoconjunctivitis sicca, pruritis, conjunctivitis, photophobia, or epiphora while moderate to severe cases can include vision changes, foreign-body sensations, chalazion and hordeolum formation, blepharitis, and keratitis [1,4]. Rarely, untreated ocular rosacea can result in complete vision loss [3,5]. Despite many options to manage cutaneous rosacea, treatments for ocular rosacea only include topical azithromycin, topical tacrolimus, and topical or oral cyclosporin, along with eyelash hygiene [3]. This case report presents a patient with cutaneous and ocular rosacea successfully treated with oral ivermectin.
Case Report
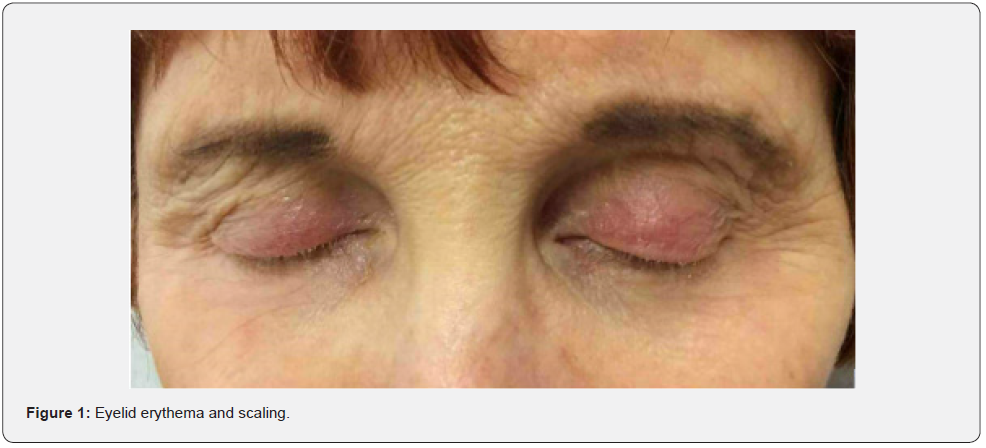
A 73-year-old woman presented with multiple years of facial papulopustular erythema and concomitant itching and irritation of bilateral eyelids. Her lash-crusting, keratoconjunctivitis sicca, and hordeola were especially bothersome (Figure 1). She carried an ophthalmological diagnosis of blepharitis and used warm compresses and over-the-counter lubricating eye drops as needed per instructions but stated these interventions had not alleviated her eye symptoms.
On exam, symptoms of papulopustular rosacea, including facial erythema, pustules, and papules on her bilateral cheeks and nose, were visualized. Crusting and erythema of the eyelash bases on bilateral upper and lower eyelids were also present. We diagnosed her with cutaneous rosacea with concomitant ocular rosacea. The patient was educated on rosacea triggers, started on oral ivermectin 3 mg/day, and given skincare recommendations. She was also instructed to continue following her ophthalmologist’s recommendations.
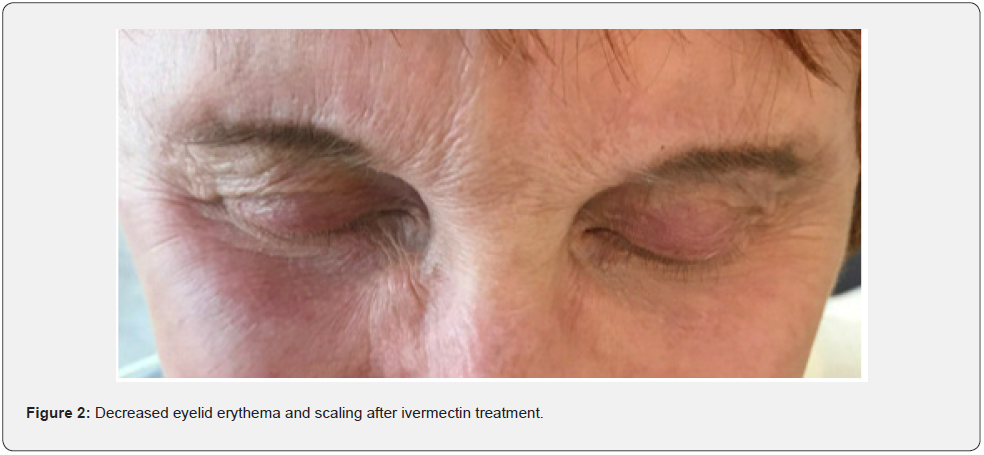
Six months later, the patient returned with marked improvement of her symptoms. There were no visible signs of inflammation on her cheeks, nose, or eyelids (Figure 2). An appointment with her ophthalmologist supported this finding. She reported improvement in her quality of life and no adverse effects to the ivermectin. We tapered the ivermectin to a dose of 0.2mg/kg/month and recommended follow-up if symptoms recurred on the maintenance dose.
Discussion
Blepharitis is an inflammatory condition of the eyelids commonly associated with infections, seborrheic dermatitis, rosacea, eczema, and psoriasis [6]. It affects individuals of all demographics and is one of the most common ocular conditions encountered by primary care and ophthalmic practices. Blepharitis can present with ocular pruritis, epiphora, conjunctivitis, and lid margin erythema and irritation. [6] Blepharitis can be classified as anterior involving outer eyelid margin at the eyelash base and posterior affecting the inner eyelid margins and meibomian glands. If untreated, keratitis, corneal erosions, skin lesions, and trichiasis can occur. Standard management includes optimizing eyelid hygiene, corticosteroid eyedrops, topical antibiotic ointments, and systemic tetracycline antibiotics [7].
Demodex, a microscopic mite, is a common etiology of blepharitis. [6] Demodex folliculorum inhabits eyelash follicles causing anterior blepharitis while Demodex brevis resides in meibomian and sebaceous glands causing posterior blepharitis and meibomian gland dysfunction. [8] Waste, debris, and eggs produced by these mites can accumulate at lash roots forming cylindrical dandruff and irregular lash growth also causing ocular discomfort. [8,9] Studies have found significant correlations between facial rosacea, eyelid inflammation, and Demodex infestations. [10,11] These studies provide some answers but leave the question of whether targeted treatment of Demodex would improve the disease course of cutaneous and ocular manifestations of rosacea.
There is a plethora of treatment options for rosacea and blepharitis but many of them have bothersome side effects or they fail to target the correct disease etiology. From an ophthalmological perspective, blepharitis management includes warm compresses, eyelid massage, and eyelid scrubs. [7] Various classes of eyedrops and ointments are also utilized but patients can be susceptible to local and systemic adverse effects due to ocular drainage and subsequent absorption into the bloodstream. [12] An example is corticosteroid drops which reduce ocular inflammation but can cause elevated intraocular pressure, cataracts, hyperglycemia, and systemic toxicity. [12] Antibiotic ointments are used to treat blepharitis with staphylococcal or seborrheic etiologies, but side effects include irritation and pruritis of the eye and surrounding skin. [7,12] Systemic therapy, such as oral tetracyclines, are used to treat posterior blepharitis and moderate to severe rosacea but this treatment is limited by common side effects such as diarrhea, nausea, headache, and photosensitization and is contraindicated in children and during pregnancy. [3,7] These conventional treatments are ineffective for Demodex blepharitis and rosacea, and other options are needed [10].
The best treatment for Demodex blepharitis remains controversial. Ivermectin is an antiparasitic drug found to effectively treat Demodex blepharitis with sustained results and minimal side effects as seen in our patient and other case reports. [6,13-16] Its labeled indications are for onchocerciasis and intestinal strongyloidiasis but has been used off-label for other infectious etiologies such as scabies. [17] Ivermectin is also known to have anti-inflammatory effects by blocking nuclear factor-kB pathways and suppressing inflammatory cytokine production. [18] Advantages of oral ivermectin include small tablet size, oncea- day dosing, minimal adverse effects, and no chronic monitoring parameters. [17] For those without known nematode infection, there is a 1-4% risk of tachycardia, peripheral edema, dizziness, altered blood cell counts, diarrhea, and nausea [17].
Conclusion
We report this case to provide further support for oral ivermectin as a treatment option for rosacea-associated blepharitis, especially for refractory cases or with known Demodex infestations. Rosacea proves to be a risk factor for Demodex-induced blepharitis so in patients with chronic blepharitis, we suggest asking about concurrent cutaneous symptoms and conversely, in patients with chronic rosacea, we suggest asking about ocular symptoms. We also stress the importance of recommending early ophthalmic involvement and follow-up to all patients with ocular symptoms to prevent worsening or new rosacea-associated eye complications.
Declaration
Author contributions: All authors made substantial contributions to the concept of this article; the acquisition and interpretation of information for this article; and the drafting of this article. All authors reviewed and approved the final manuscript.
Consent for Publication
Informed, voluntary consent was obtained from the included patient for use of the information and materials (such as photograph) included in this article.
References
- Van Zuuren EJ, Fedorowicz Z, Carter B, Mireille M D van der Linden, Lyn Charland ( 2015) Interventions for rosacea. Cochrane Database Syst Rev 2015(4): CD003262.
- Wilkin J, Dahl M, Detmar M, Drake L, Feinsteinet A at el. (2002) Standard classification of rosacea: Report of the National Rosacea Society Expert Committee on the Classification and Staging of Rosacea. J Am Acad Dermatol 46(4): 584-587.
- Thiboutot D, Anderson R, Cook-Bolden F, Draelos Z, Gallo LR, et al. (2020) Standard management options for rosacea: the 2019 update by the National Rosacea Society Expert Committee. J Am Acad Dermatol 82(6): 1501-1510.
- Rainer BM, Kang S, Chien AL (2017 ) Rosacea: epidemiology, pathogenesis, and treatment. Dermatoendocrinol 9(1): e1361574.
- Subashini K, Pushpa G, Venugopal V, Murali N (2012) Rosacea with severe ophthalmic involvement and blindness - a rare occurrence. Int J Dermatol. 51(10): 1271-1273.
- Putnam CM (2016) Diagnosis and management of blepharitis: an optometrist's perspective. Clin Optom (Auckl) 8: 71-78.
- Lindsley K, Matsumura S, Hatef E, Akpek EK (2012) Interventions for chronic blepharitis. Cochrane Database Syst Rev (5): CD005556.
- Gao YY, Di Pascuale MA, Li W, Liu DTS, Baradaran-Rafii A, et al. (2005) High prevalence of Demodex in eyelashes with cylindrical dandruff. Invest Ophthalmol Vis Sci 46(9): 3089-3094.
- Liu J, Sheha H, Tseng SCG (2010) Pathogenic role of Demodex mites in blepharitis. Curr Opin Allergy Clin Immunol 10: 505-510.
- Li J, O'Reilly N, Sheha H, et al. (2010) Correlation between ocular Demodex infestation and serum immunoreactivity to Bacillus proteins in patients with Facial rosacea. Ophthalmology 117(5): 870-877.
- Gonzalez-Hinojosa D, Jaime-Villalonga A, Aguilar-Montes G, Lammoglia-Ordiales L (2018) Demodex and rosacea: Is there a relationship? Indian J Ophthalmol. 66(1): 36-38.
- Farkouh A, Frigo P, Czejka M (2016) Systemic side effects of eye drops: a pharmacokinetic perspective. Clin Ophthalmol 10: 2433-2441.
- Forstinger C, Kittler H, Binder M (1999) Treatment of rosacea-like demodicidosis with oral ivermectin and topical permethrin cream. J Am Acad Dermatol. 41(5 Pt 1): 775-777.
- Holzchuh FG, Hida RY, Moscovici BK, Villa Albers BA, Santo RM, et al. (2011) Clinical treatment of ocular Demodex folliculorum by systemic ivermectin. Am J Ophthalmol 151(6): 1030-1034.
- Brown M, Hernández-Martín A, Clement A, Colmenero I, Torrelo A, et al. (2014) Severe demodexfolliculorum-associated oculocutaneous rosacea in a girl successfully treated with ivermectin. JAMA Dermatol 150(1): 61-63.
- Hernández-Martín Á (2017) Tratamiento con ivermectina oral en un paciente inmunocompetente con rosácea pápulo-pustulosa. Actas Dermosifiliogr. 108(7): 685-686.
- Ivermectin (Systemic): Drug Information (2021).
- Zhang X, Song Y, Ci X, N An, Y Ju, et al. (2008) Ivermectin inhibits LPS-induced production of inflammatory cytokines and improves LPS-induced survival in mice. Inflamm Res 57(11): 524-529.






























