An Experimental Study of Astigmatism Optical Correction on Visual Acuity Changes when being Corrected with Spherocylindrical and Spherical Equivalent Spectacle Lenses
Innocent Thawe*
Master’s Degree in Optometry and Vision Therapy, Zomba Central Hospital, Malawi
Submission: January 12, 2019; Published: February 05, 2019
*Corresponding author: Innocent Thawe, School of Advanced Education, Research and Accreditation, Master’s Degree in Optometry and Vision Therapy, Zomba Central Hospital, Zomba, Malawi
How to cite this article: Innocent T. An Experimental Study of Astigmatism Optical Correction on Visual Acuity Changes when being Corrected with Spherocylindrical and Spherical Equivalent Spectacle Lenses. JOJ Ophthal. 2019; 7(3): 555713. DOI: 10.19080/JOJO.2019.07.555713
Keywords
Keywords: Marfan’s disease; Hereditary connective tissue; Clinical polymorphism; Heart; Aorta; Eye; Skeleton; Lens ectopia; Eye manifestations; Diagnosis; Pathology; Ophthalmology clinic
Introduction
Marfan’s disease (MDM) is a hereditary connective tissue disorder transmitted in the dominant autosomal mode with variable penetrance and expressiveness. It is responsible for a clinical polymorphism, which can be life threatening (heart, aorta) and functional (eye, skeleton, ...). The lens ectopia is one of the most common eye manifestations, and represents a major criterion of diagnosis. The aim of our study was to study the ocular manifestations and to evaluate the management and evolution of this pathology through seven (07) observations made at the Ophthalmology Clinic of Aristide Le Dantec Hospital in Dakar, between January 2009 and December 2015.
Observations
Observation number 1
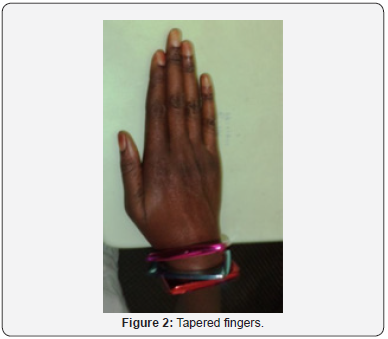
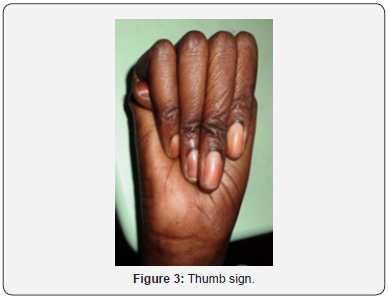
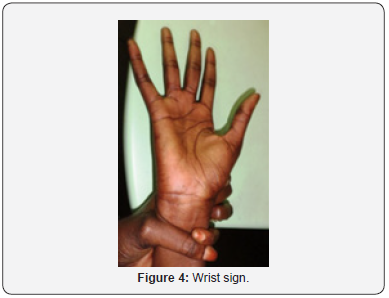
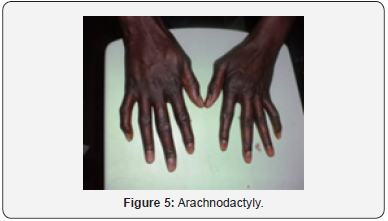
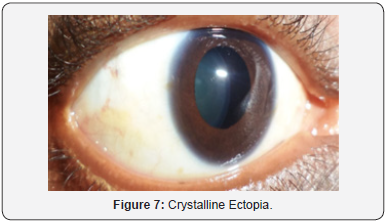
This was a 40-year-old female teacher who was screened and followed at age 17. She had a brother and a sister in the morphotype of Marfan, who died in May and December 2014 respectively of an undocumented cardiac pathology. She had consulted for a progressive BAV with both eyes evolving since the age of seven. The general examination showed a slender morphotype (size 1.90m), dolichostomelia, arachnodactyly and ligamentous hyperlaxity (Figure 1-5). AV was 1/10th at OD and CLD at 50cm at OG. In the slit lamp (LAF) there was bilateral ectopia (Figure 7) with supero-nasal displacement, cortical opacity and bilateral iridodonesis. The ocular tone was 14mmHg at ODG and the fundus revealed diffuse choroidosis. The cardiovascular examination was normal. Automatic refraction with cyclopentolate showed strong myopia with astigmatism at -18.5 (120° -12.25) at OD and -19 (60-12.5) at OG. Mean keratometry was 8.2mm at OD and 8.5mm at OG. The electrocardiographic tracing was normal and echocardiography in the TM and 2D mode revealed an undilated ascending aorta 30 mm in diameter with minimal aortic insufficiency. The diagnosis of MDM was made before ocular, morpho-skeletal, and cardiological abnormalities that met the diagnostic criteria of Ghent 2010. The indication of lens extraction and placement of an implant attached to the sclera had been proposed, but the patient had refused surgery. An optic correction was made OD : -7 (120° - 4); OG: -7 (60° - 4) and the bilateral AV was ≤ 3/10th.
Observation number 2
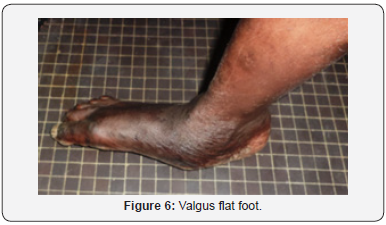
This was a 34-year-old patient, brother of patient no 1. He had come in consultation on our request for MDM screening.Examination showed a slender morphotype (size 2.02 m), dolichostomelia, arachnodactyly, dolichocephaly, ligamentous hyperlaxity and valgus flat feet (Figure 1-6). AV was 7/10th at OD, and 5/10th at OG. At the LAF, there was a bilateral ectopic lens (Figure 7) with a super-nasal direction, and a bilateral iridodonesis. The ocular tone was at 16mmHg at ODG and normal fundus. The cardiovascular examination was normal. Automatic refraction with cyclopentolate showed moderate myopia associated with astigmatism with -1.00 (177° -2.25) at OD and -1.50 (30° -3.50) at OG. Mean keratometry was 7.5mm at OD and 7.8mm at OG. The electrocardiographic tracing revealed atrioventricular block with left ventricular hypertrophy. TM and 2D echocardiography showed moderate dilatation of the aorta with minimal aortic insufficiency. Faced with family history, ocular, morpho-skeletal, and cardiological abnormalities that met the international criteria of Ghent 2010, the diagnosis of MDM was retained. The treatment consisted of a total optical correction with AV at 9 / 10th to OD, and 7/10th at OG, a bêta-blocker prescription in per os and periodic monitoring.
Observation number 3
This was a 14-year-old woman with a history of multiple lens prescription ametropia who had been referred for a progressive ODG BAV that had been on the move since the age of eight. The examination revealed an elongated morphotype (size 1.74m), dolichostomelia, arachnodactyly and ligamentous hyperlaxity Keywords: Marfan’s disease; Hereditary connective tissue; Clinical polymorphism; Heart; Aorta; Eye; Skeleton; Lens ectopia; Eye manifestations; Diagnosis; Pathology; Ophthalmology clinic (Figure 1-5). The AV was at CLD at 1m at OD and at CLD at 2m at OG. Ophthalmologic examination revealed an esotropia of OG, a crystalline ectopia (Figure 7) bilateral with supernonasal orientation. The ocular tone was at 12mmHg at OD and 14mmHg at OG. The fundus was normal. The cardiovascular examination was normal. Automatic refraction with cyclopentolate showed strong myopia associated with astigmatism in both eyes: -12 (130° -10) at OD and -14 (63°-11.25) at OG. Electrocardiographic tracing was normal, and TM and 2D echocardiography showed moderate dilatation of the aorta with minimal aortic insufficiency. MDM was found in association with ocular, morpho-skeletal and cardiological disorders that were consistent with the 2010 Ghent diagnostic criteria. The patient had scleral crystalline lens removal with optic correction of aphakia by glasses (AV at 3 / 10th ODG), oral betablocker prescription and periodic monitoring.

Observation number 4
This was a 21-year-old patient who had been seen for a progressive implantable BAV since the age of 8, and bilateral eye pain. The examination showed a slender morphotype (size 1.93m), dolichostomelia, arachnodactyly, ligamentous hyperlaxity and valgus flat feet (Figure 1-6).
Ophthalmologic examination showed CLD at 50cm ODG, stage IV keratoconus (Figure 8) and bilateral central corneal opacity. The ocular tone was 28mmHg at ODG. The fundus was normal. The cardiovascular examination was normal. Automatic refraction was impregnable at ODG. Keratometry and electrocardiogram could not be performed. Echocardiography in TM and 2D mode noted moderate dilatation of the aortic arch (37mm). The diagnosis of MDM was based on ocular, morpho-skeletal and cardiological abnormalities that met the diagnostic criteria of Ghent 2010. A medical treatment based on hypotonizing eye drops was prescribed. The patient was then lost to sight for three years. After this delay, the ophthalmological examination showed an AV at CLD less than 50cm at OD and a light perception at OG. The LAF examination was unchanged and associated with a bilateral debutative cortical cataract. The papilla was viewable without interposition of magnifying glass. The ocular tone was 12mmHg at ODG.
Observation number 5
This was a 28-year-old female patient with a history of ametropia who had been prescribed corrective lenses several times, who had been referred for an ODG progressive implant BAV that had been in the process since the age of 6, persistent despite the glasses. Examination showed a slender morphotype (size 1.85m), dolichostomelia, arachnodactyly, dolichocephaly, ligamentous hyperlaxity and dorsal kyphosis (Figure 1-5). Ophthalmologic examination revealed CLD AV at 1m ODG. LAF examination revealed a superior-temporal erythropic ectopy at ODG (Figure 7), cortical crystalline opacity, bilateral iridodonesis, and vitreous liquefaction. The ocular tone was at 14mmHg. The fundus was normal to ODG. The cardiovascular examination was normal. Automatic refraction with cyclopentolate showed strong myopia and astigmatism at -18.25 (140° -12) at OD, and -18.50 (75°-12.50) at OG. Mean keratometry was 8.3mm at OD and 8.55 mm at OG. Ocular ultrasonography in B mode showed posterior detachment of vitreous to OG. Electrocardiographic tracing demonstrated left ventricular hypertrophy and TM and 2D echocardiography showed a linear image in the lumen of the proximal aorta. The diagnosis of MDM was based on ocular, morpho-skeletal, and cardiological abnormalities that corresponded to the 2010 Ghent diagnostic criteria. A lens extraction without implant placement was proposed and performed at OG, but was refused to OD by the patient. The cardiological treatment consisted of the prescription of betablocker and periodic monitoring. The patient was regularly seen post-operatively. In the 5th month, the AV was unchanged at OD while at OG a BAV was noted with a reduced vision at PL +. FO at OG showed a retinal detachment with a tear. A strapping had been indicated and carried out without success.
Observation number 6
This was a 17-year-old patient who had been referred for an ODG progressive implant BAV that had been evolving since she was 5 years old. Examination revealed a slender morphotype (size 1.96m), dolichostomelia, arachnodactyly, ligamentous hyperlaxity, and dorsal kyphosis (Figure 1-5). Ophthalmologic examination showed 1/20 AV at ODG. LAF examination revealed bilateral posterior dislocation of the ectopic lens associated with ODG microspherophakia. The ocular tone was 6mmHg at ODG. The fundus showed a nasal retinal detachment lower than ODG. The cardiovascular examination was normal. Automatic refraction with cyclopentolate showed strong myopia associated with astigmatism with -15 (125°-10) at OD and -14 (70°-11.25) at OG. Mean keratometry was 7.8mm at OD and 7.9mm at OG. TM and 2D echocardiography revealed moderate dilatation of the aorta with minimal aortic insufficiency. The diagnosis of MDM was based on the combination of ocular, morphoskeletal, and cardiological disorders that were consistent with the 2010 Ghent diagnostic criteria. The patient had benefited from a simple extracapsular lens extraction (EEC) with ODG. Betablocker-based therapy and periodic monitoring. The patient had a post-operative AV PL + with intravitreous hemorrhage at OD and CLD at 5m to 0G.

Observation number 7
This was a 14-year-old patient with a family history of MDM who had been consulting for a 8-year progressive ODG BAV. The examination revealed a slender morphotype (size 1.75m), the fingers and toes were tapered. There was dolichostomelia, arachnodactyly, dolichocephaly and ligamentous hyperlaxity (Figure 1-5). Ophthalmologic examination revealed an AV at 2/10th at OG, and PL + at OD. The LAF examination noted a bilateral super-nasal crystalline ectopia (Figure 7). The ocular tone was at 14mmHg at ODG. The fundus showed bilateral myopic colon and temporal peripapillary chorioretinal degeneration. The cardiovascular examination was normal. Automatic refraction under cyclopentolate was not feasible. Mean keratometry was 8.2mm at OD and 8.3mm at OG. Electrocardiogram and echocardiography were requested but not done for lack of means. The diagnosis of MDM was made before eye, morpho-skeletal and cardiological abnormalities that met the diagnostic criteria of Ghent 2010. The patient was lost sight of after the first consultation.
Discussion
Marfan’s disease is rare, its frequency is estimated in the literature at 3-5 / 10000 [1], in our context its prevalence was 3/10000. Sun et al. reported a prevalence of 17.2 per 100,000 consultants in China [2]. The average age of diagnosis of the disease in our patients was 20.7 years, with extremes of 14 and 34 years. In the United States, Heur et al. [3] reported an average age of 22.3 years [3]. In France, Sultan had reported an average age of 23.9 years [4]. The diagnostic delay observed can be explained by the fact that the diagnosis is sometimes difficult, particularly in pediatrics, because of the great variability of expression of the disease, ranging from a very severe form (neonatal Marfan) to a form with a clinical expression is not very intense and because of the evolution of signs with age [5]. Neonatal MDM is considered the most severe form of type 1 fibrillinopathy. In an international series of 62 patients [6], over 80% of children died before the age of one. In the literature, Marfan’s disease affects both sexes [1]. The familial character was found in fours patients. Maumenee, noted a family history in 111 patients (69.3%), against 46 without a family history of Marfan disease [7]. Almost 25% of sporadic cases are due to new mutations in the MFS gene and the notion of family inheritance is not always a risk factor [8]. Low vision is the first reason for consultation, it is found in six (06) of our patients. Visual acuity was less than or equal to 1/10th in 11 out of 14 eyes. This is due to delayed consultation of patients who mostly reside in a rural area with low socio-economic status and lack of campaigns screening for this type of pathology. The crystalline ectopia is of great semiological value. It is a major criterion in the diagnosis of MDM. In the literature, it represents 60 to 80% [9,10]. Bilateral involvement is found in all our patients. In Norway, a study by Drolsum et al. [11] about 87 cases of MDM reported 62.1% of ectopic lens, with bilateral and symmetrical involvement [11]. The superior direction of ectopia is reported in the literature [9,10,12]. Iridodonesis is a sign often associated with ectopia [10,11]. Posterior dislocation of the ectopic lens is a complication of Marfan’s disease. It can be followed by retinal detachment [9]. Chefchaouni in Morocco reported posterior dislocation in 5 out of 38 eyes with lens ectopia [13].
Microspherophakia is described in 15% [14]. Cataract was present in 4 out of 14 eyes. In the Chefchaouni series, it has been observed in 6 out of 40 eyes. In Norway, the study by Drolsum et al. showed 20% cataract [11]. While the rate was 12% in the Konradsen et al. [8]. Myopia is the second most common ocular manifestation in Marfan’s disease with a significant incidence of strong myopia (greater than -6 diopters). In Sweden, Konradsen et al. reported 87% myopia, of which 39% had moderate myopia [15]. Maumenee revealed 16.3% of strong myopia [7]. Five patients had strong myopia, one patient had moderate myopia and. This disparity in the results can be due on the one hand to the weakness of our sample, on the other hand to the delay of consultation. This abnormality of refraction also exposes to classic retinal complications, sometimes serious, of the strong myopia. Among these complications, we can note retinal detachment and chorioretinal atrophy noted respectively in two (02) of our patients. The detachment of the retina is the main ocular complication of Marfan’s disease. Its frequency is estimated at 5 to 11%. The risk of DR is increased in case of ectopic lens or after lens extraction (8 to 38%) [16]. It usually occurs around the twenties, and mainly affects men [10]. The incidence of bilateral retinal detachment is also high and can reach 69% according to some studies [17,18]. Various factors are implicated in the etiopathogenesis of this complication, notably crystalline ectopia which exerts a continuous traction on the ora serrata, the vitreous liquefaction causing retinal traction and the coexistence of myopia and therefore of degenerative lesions of the retinal periphery. Only one case of keratoconus was recorded at an advanced stage. This manifestation is rarely linked to MDM [3]. Crystal ectopia is a relatively easy anomaly to identify when it is known, but management is a real challenge for ophthalmologists. Optical correction is one of the therapeutic means adopted when ectopia is simple, uncomplicated and without significant refractive errors. Most authors resort to surgery if any of these elements exist [9,10]
a) A bad AV not paired with glasses or contact lenses;
b) A myopia greater than 7 diopters and / or a higher astigmatism 4 diopters;
c) A cataract;
d) A glaucoma;
e) A crystalline dislocation.
The surgical procedure under the operating microscope and with maximal mydriasis consisted of a simple EEC for 4 eyes of 3 patients, with correction of aphakia by glasses for a patient. A surgical cure of retinal detachment was performed in one patient. In the Chefchaouni series, an EEC by phacophagia with anterior vitrectomy by pars plana was performed for 14 eyes. One patient had intraocular lens implantation. Three eyes underwent a retinal detachment and 9 eyes with degenerative lesions of the retinal periphery benefited from Argon laser photocoagulation. A study done in London by Hubbard et al. [19], about 30 cases of Marfan’s disease, reported an EEC by phacophagia with anterior vitrectomy by pars plana in 40 eyes. Thirty-seven eyes had a simple EEC and had been corrected by contact lenses. Three eyes benefited from implantation in the posterior chamber. Seven eyes had a retinal detachment cure. The results and the postoperative complications that the different studies show are variable. Poncophagia associated with anterior vitrectomy by pars plana remains the most used. It would decrease the risk of postoperative retinal detachment by reducing traction forces on the vitreous base [13,19]. The functional results after lens extraction were 3 / 10th improvement in AV for 2 eyes of a patient after correction of aphakia with glasses of glasses and worsening of BAV at PL + in 2 patients, due to postoperative retinal detachment and intravitreous hemorrhage. A study conducted in India by Sinha et al. [20] about 10 eyes of 5 patients who had lens-free crystalline extraction, corrected for aphakia by glasses, showed a mean postoperative AV of 0.46 ± 0.15 (preoperatively, it was 0,16 ± 0.07) [20]. The functional results of Chefchaouni, after phacophagia, without implant placement, and anterior vitrectomy reported an AV greater than or equal to 2/10th in 85% of cases. In addition, for 3 eyes having benefited from a retinal detachment cure, a retinal reapplication could be obtained in 2 cases.
Conclusion
Marfan’s disease is an inherited connective tissue disorder, transmitted in an autosomal dominant fashion with variable penetrance and expressiveness. It is often due to a mutation in the gene encoding type 1 fibrillin, located on chromosome 15 (15q21). The lens ectopia is one of the most frequent ocular manifestations, and represents a major diagnostic criterion. The management of ocular disorders remains difficult.
References
- Jondeau G, Boileau G, Chevallier B, Delorme G, Florence Arnoult, et al. (2003) Le syndrome de Marfan. Sang Thrombose Vaisseaux février 15(2): 110-115.
- Chan Y C, Ting C W, Ho P, Jensen T Poon (2008) Revue épidémiologique à dix ans des patients hospitalisés pour syndrome de Marfan. Ann Vasc Surg 22(5): 608-612.
- Heur M, Costin B, Crowe S, Grimm RA, Moran R, et al. (2008) The value of keratometry and central corneal thickness measurements in the clinical diagnosis of Marfan syndrome. Am J Ophthalmol 145(6): 997-1001.
- Sultan, Baudouin C, Auzerie O, Magdalena De Saint Jean, Marie Goldschild, et al. (2002) Cornea in Marfan Disease : Orbscan and In Vivo Confocal Microscopy Analysis. Investigative Ophthalmology & Visual Science 43(6).
- Stheneur C, Laffond C, Rioux S, G Benoist, B Chevallier, et al. (2012) Nouveautés dans le syndrome de Marfan. Archives de pédiatrie 19(5): 551–555.
- Stheneur C, Faivre L, Collod Beroud G, Gautier E, Binquet C, et al. (2011) Prognosis factors in probands with an FBN1 mutation diagnosed before the age of 1 year. Pediatr Res 69(3): 265-270.
- Maumenee I H (1981) The eye in the Marfan syndrome. Trans Am Ophthalmol Soc 79: 684-733.
- Dietz Hc, Cutting Gr, Pyeritz Re, Maslen CL, Sakai LY, et al. (1991) Marfan syndrome caused by a recurrent de novo missense mutation in the fibrillin gene. Nature 352(6333): 337-339.
- Nemet AY, Assia EI, Apple DJ, Irina S Barequet (2006) Current Concepts of Ocular Manifestations in Marfan syndrome. Elsevier Inc Surv of Ophthalmo 51(6): 561-575.
- Nahum Y, Spierer A (2008) Ocular Features of Marfan Syndrome : Diagnosis and Management. Israel Medical Association Journal 10(3): 179-181.
- Drolsum L, Rand Hendriksen S, Paus B, Geiran O R, Semb SO (2014) Ocular findings in 87 adults with Ghent-1 verified Marfan syndrome Acta Ophthalmologica 93(1): 46-53.
- Chevallier B, De Saint Jean M (2009) Le syndrome de Marfan de l’enfant et de l’adolescent La Gazette de la SOFOP 28(7).
- Chefchaouni MC, Hajji Z, El Bakkali M, A boulanouar, A Berraho (2001) Les manifestations oculaires du syndrome de Marfan a propos de 20 cas. Médecine du Maghreb 87.
- Stass Isern M, Smith LD (2010) Ophthalmologic Manifestations of Systemic Disease. International Ophthalmology Clinics 50(4): 27-43.
- Judge DP, Dietz HC (2005) Marfan’s syndrome. Lancet 366: 1965-1976.
- Mcwilliams WG, Maumenee IH (1989) Retinal detachment in the Marfan syndrome. Am J Med Genet 32: 239-251.
- Sharma T, Gopal L, Shanmugam MP, Bhende PS, Agrawal R, et al. (2002) Retinal detachment in Marfan syndrome : clinical characteristics and surgical outcome. Retina 22(4): 423-428.
- Remulla JF, Tolentino FI (2001) Retinal Detachment in Marfan’s syndrome. Int Ophthalmol Clin 41(4): 235-240.
- Hubbard AD, Charteris DG, Cooling RJ (1998) Vitreolensectomy in Marfan's syndrome. Eye (Lond) 12 : 412-416.
- Sinha R, Sharma N, Vajpayee Rb (2005) Intralenticular bimanual irrigation : Aspiration for subluxated lens in Marfan’s syndrom. J Cataract Refract Surg 31(7): 1283-1286.






























